Abstract
The bipolar radiofrequency endometrial ablation system (NovaSure™) has been developed to treat women suffering from menorrhagia due to dysfunctional uterine bleeding. This technology allows for a customized, controlled, contoured endometrial ablation, without the need for hysteroscopic visualization and endometrial pretreatment. Average treatment time is 90 s. Active bleeding, at the time of treatment, is not found to be a limiting factor for the use of this technology. Technical aspects of the bipolar radiofrequency ablation procedure are described and summarized in this article. The safety features employed, combined with a high level of effectiveness and patient satisfaction, qualifies this system for consideration as a logical alternative to hysterectomy as well as an alternative to hysteroscopic endometrial ablation.
Hysterectomy is currently the leading treatment method for patients symptomatic for menorrhagia. Over 600,000 hysterectomies are performed every year in the USA alone. This surgical method of treatment was found to be efficacious, although it is associated with a number of well known and analyzed serious disadvantages. Hysterectomy has a relatively high morbidity and mortality rate, and direct and indirect costs associated with the procedure are also quite significant [1]. Ablation of the endometrial lining of the uterus as an alternative to hysterectomy was found to be a less invasive and aggressive method [2]. A large number of clinical trials, as well as retrospective analysis of clinical and financial data, has shown that endometrial ablation allows for a lower morbidity and mortality rate and significantly lower procedure costs [3]. Worldwide, endometrial ablation is increasingly being adopted by the gynecological community [4]. The risks associated with the hysteroscopic approach are well known and include uterine wall perforation, intravasation of fluid distention media, hyponatremia, encephalopathy and death [5–8]. Technical challenges, the need for well developed hand–eye–foot coordination, potential risks and other drawbacks of this treatment modality do not allow for a successful adoption of this procedure by the vast majority of gynecologists. In fact, only 15% of practicing gynecologists in the USA offer this treatment method [9].
This fact, and the alarming rate of hysterectomies performed, triggered the development of other, less challenging methods of endometrial ablation.
A variety of methods were and are continuously developed. Most of them are found to be quite effective, such as heated balloons (Thermachoice™ and Cavaterm™), heated free circulating saline (HTA™), cryoablation (Her Option™) and microwave energy (MEA™). Randomized, controlled studies have been and are continuously conducted to evaluate the safety and effectiveness of each treatment modality. Nevertheless, most of these methods cannot be used when the patient is actively bleeding, which results in a logistical problem with respect to scheduling. Hence, these technologies require some form of pretreatment with drugs or dilation and curretage (D&C). Intra- and postoperative pain can be quite significant, partly owing to the duration of the procedure; therefore, compatibility with the office setting remains questionable. Moreover, most of these technologies are lacking a reliable safety mechanism that would prevent energy delivery in the event of a perforation of the uterus. The bipolar radiofrequency (RF) endometrial ablation system (NovaSure™, Cytyc Surgical products, CA, USA) successfully addresses many of these drawbacks.
Technology
The bipolar RF system (Figure 1) consists of a single-use, 3D bipolar ablation device and RF controller that enables a controlled endometrial ablation in an average of 90 s without the need for concomitant hysteroscopic visualization. Endometrial pretreatment of any kind (mechanical, hormonal or cycle timing) is not required when using the bipolar RF system. The technology is easily employed in the actively bleeding patient.
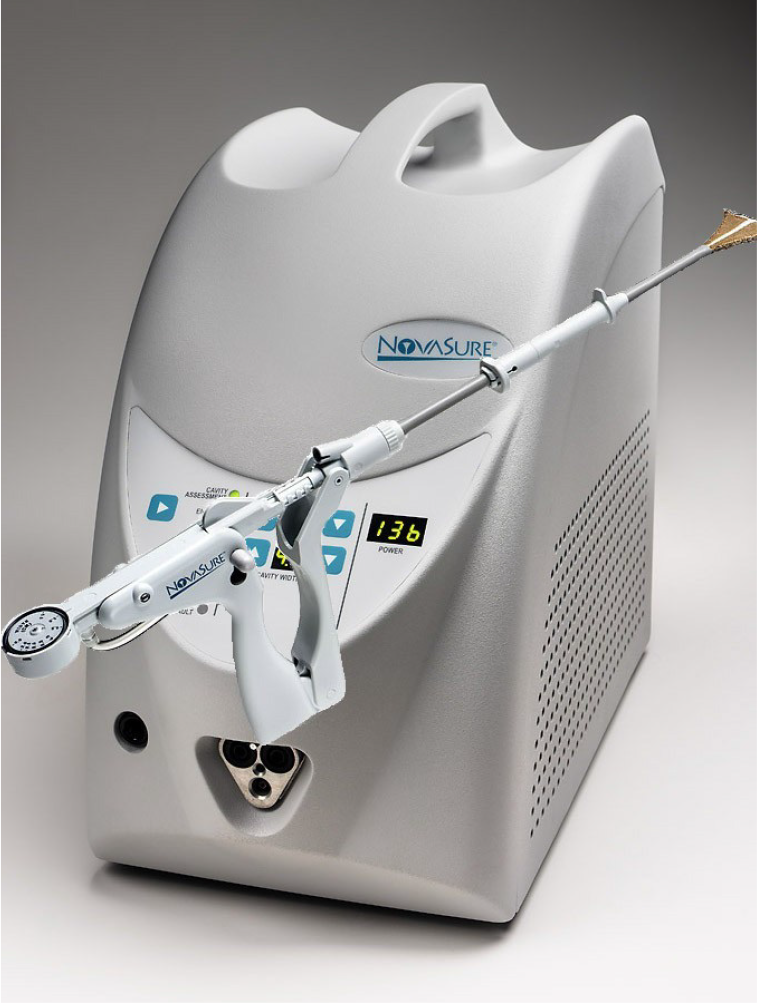
NovaSure™ controller and disposable applicator.
The bipolar RF disposable ablation device consists of a conformable, bipolar, gold-plated, porous, fabric mesh, mounted on an expandable metal frame. Integral to the hand-held device is the Intrauterine Measuring System (IMD) used to determine uterine cavity width (cornu-to-cornu distance). The particular geometry of the electrode enables a controlled depth of ablation. It is characterized by a more shallow depth of myometrial penetration (2 mm) at the cornu and lower uterine segment, and a deeper (5 mm) ablation in the mid-body of the uterus. The bipolar RF device can treat uteri with sounding lengths up to 12 cm. During insertion into the uterine cavity, the ablation electrode is housed in a protective sheath (similar to an intrauterine device) with an outside diameter of 7.2 mm. During electrode deployment, the sheath is withdrawn into the endocervical canal, allowing for full and proper intrauterine deployment of the fan-shaped bipolar electrode. During the ablation procedure, the protective sheath occupies the full length of the cervical canal, assuring an effective protection of the endocervix from thermal injury.
The bipolar RF controller contains a constant power output generator with a maximum power delivery of 180 W. Measurement of uterine cavity length (determined during sounding and cervical dilation) and width (measured by the disposable device at the time of device deployment) are entered into the controller, which automatically calculates the unique power output required to ensure an optimal, confluent endomyometrial ablation. Throughout the short procedure, the depth of ablation is continuously controlled by monitoring tissue impedance (resistance). Vaporization of the endometrial layer is a low-impedance process owing to a high concentration of conductive liquid (electrolytes) present in the endometrial tissue. As a result, the endometrial tissue is not slowly ablated, but vaporized instead. The vaporization front continuously moves deeper and closer to the edge of the myometrium. Once the ablation process reaches the myometrial layer, the saline content of these cells becomes significantly lower. Tissue impedance (resistance) rises rapidly during myometrial tissue desiccation process and reaches 50 Ohms, which is equivalent to the impedance of the ablated superficial myometrium. This signals the bipolar RF generator to automatically terminate the ablation process. With the bipolar RF system, the ablation process is based, not on temperature and time, but on specific, well-analyzed physical characteristics (electrical conductivity) of tissues that are continuously changing during the ablation process. This approach allows for an effective ablation that is independent of the endometrial layer thickness. Treatment time equates to the length of time that is necessary to vaporize an endometrial layer of a certain thickness. The ablation procedure is usually longer in patients with thick endometrium (100–120 s) and shorter in patients with thin endometrium (30–100 s). This unique approach allows for a well-controlled, tailored, consistent and rapid ablation process.
An important component, unique to the bipolar RF system, is a vacuum pump, contained within the RF controller. This pump provides continuous suction during the procedure, thus allowing for the removal of steam, blood and other by-products of ablation from the cavity. Another valuable aspect of the bipolar RF system is its portability and light weight, allowing the system to be stored easily in an office cabinet.
Safety
Safety begins with proper patient selection. Contraindications for this procedure include:
Patients who are pregnant or want to become pregnant in the future;
Patients with known or suspected endometrial carcinoma or premalignant change of the endometrium, such as unresolved adenomatous hyperplasia;
Patients with anatomical or pathological conditions in which weakness of the myometrium could exist, such as history of previous classical caesarean section or transmural myomectomy;
Patients with active genital or urinary tract infection at the time of the procedure;
Patients with intrauterine devices currently in place;
Patients with uterine sound measurement greater than 12 cm;
Patients on medications that could thin the myometrial muscle, such as long-term steroid use;
Patients with an abnormal uterine cavity, such as malformation, fibroids greater than 2 cm or polyps that distort the cavity.
There are two types of safety mechanisms in most of the new global endometrial ablation systems: preventive safety measures and corrective safety measures. In the latter, if there is a problem (e.g., a uterine perforation), the system will recognize this and either shut down the energy delivery or inform the physician through an alarm. Thus, it may stop delivering energy once it has recognized the perforation, although damage to adjacent organs may still have occurred. Conversely, preventive safety measures mean that the system uses safety checks first and will not allow energy delivery unless these have been passed. In my view, this type of safety mechanism is much more efficient in terms of protecting patients against injury. The bipolar RF controller includes a cavity integrity assessment system (perforation detection system) that is an integral part of the bipolar RF System. This automatic safety feature assists the physician in the timely detection of a uterine perforation and prevents energy delivery in such cases. The cavity integrity assessment system uses the same technology employed by conventional hystero-flators, in which there is an inverse relationship between flow rate and pressure. CO2 is delivered into the uterine cavity at a safe flow rate (100 cc/min maximum) and pressure (100 mmHg maximum). The goal is to generate and maintain an intrauterine pressure of 50 mmHg for a period of 4 s. The pressure of 50 mmHg was chosen in order to avoid false-positive results due to leakage of CO2 through the fallopian tubes (cracking pressure of the fallopian tube is 75–80 mmHg). Once the controller determines that this pressure is maintained, thus confirming uterine wall integrity, it signals the generator to proceed with the ablation process.
Another very helpful safety feature of the bipolar RF system is the device position feedback system. This system was designed and implemented to enable the physician to track and control the process of opening of the device electrode in the uterine cavity. It will also prevent RF energy delivery in the event of inadvertent placement of the device into a false passage. In this case, proper deployment of the array is not possible due to the resistance of the surrounding myometrium. This incomplete deployment of the array enables some of the electrodes to be in contact with each other, causing an electrical shortage or direct current (DC) short. This is recognized by the generator, which does not allow energy to be delivered.
Based on extensive clinical data (~350,000 patients treated worldwide since 2001), it was found that the procedure is easy to perform, does not require special skills and has a very short (one or two clinical cases) learning curve. Only knowledge and experience with intrauterine manipulations (i.e., D&C or IUD insertion) is required.
In a summary of safety and effectiveness data (SSED) obtained from the US FDA, Cooper and Gimpelson found that, in a large, multicenter, prospective, randomized trial performed with the bipolar RF system, there were no significant intraoperative adverse events, and there was a 4% minor adverse event rate in the first 24 h, mainly pelvic pain and cramping. Although this paper was not intended to be a head-to-head comparison, the incidence of adverse events was less than with other global endometrial ablation techniques [10].
SSED provides detailed treatment protocols and objective data sources for evaluating a range of performance parameters when assessing these technologies and can be useful for validating marketing claims. The Manufacturer and User Facility Device Experience (MAUDE) database, another source of information on the internet, allows for review of adverse events reported during commercial use [101]. Although a valuable tool, MAUDE was found to have significant limitations and pitfalls if used to compare various technologies (i.e., occasional duplicate reporting or underreporting, inability to assess the true rate of adverse events without knowing the total number of cases performed [denominator], and description of events was often subjective). Clinical results reported in the SSED are credible but should only be expected if there was strict adherence to the protocol described. There have been a few reports of complications using the bipolar RF system, as with any other endometrial ablation system. However, these rare unfortunate events occurred essentially as a result of protocol violation. Either the patient was not a suitable candidate for this procedure, such as the presence of a large submucous fibroid (confirming the need for adequate patient selection that ideally would include hysteroscopy), or the physician did not proceed according to the manufacturer's instructions. Therefore, one should exercise caution in the interpretation of information from the MAUDE database. As with any disposable device, there can be an occasional device failure. However, with more than 350,000 cases performed worldwide, bipolar RF endometrial ablation has shown a very good safety profile, even with minimal physician training.
Efficacy
In this type of procedure, efficacy can be determined in many different ways since endometrial ablation is aimed at curing menorrhagia as a dysfunctional condition. Depending on the study protocol, efficacy as an end point may vary from ‘decreased menstrual bleeding below normal value’ or ‘amenorrhea with or without spotting’ to ‘strictamenorrhea’ (Table 1) [15]. It may also be defined as an impact on the quality of life or the avoidance of additional surgery, namely hysterectomy [16]. To date, there are four prospective, single-arm, observational studies published [11–14], one of which describes the results of a 3-year follow-up [13]. In 2002, Gallinat was the first to publish a series of 107 patients on which he performed endometrial ablation with the bipolar RF system [11]. There were no operative complications and the strict amenorrhea rate was 58% at 1 year with a persistent menorrhagia rate of 3.9%. Subsequently, these women were followed for up to 3 years to observe an increase in the amenorrhea rate to 65% and the avoidance of hysterectomy in 97.2% of patients treated with the bipolar RF system [13]. Baskett obtained data on 146 women followed for 1–4 years. The strict amenorrhea rate was 43% and hysterectomy was eventually required in only ten of the 146 women [14]. Perhaps the most significant manuscript published thus far, in terms of quality of the data, was the outcome of a prospective, randomized, multicenter trial between the bipolar RF system and rollerball endometrial ablation, published by the late Jay Cooper and colleagues [15]. First, performing randomization avoids selection bias that may occur in prospective, observational, single-arm studies. Second, the design of this particular study allowed not only a comparison with the traditional gold standard of hysteroscopic endometrial ablation, but also considered operator variability, since it was performed by nine different physicians and therefore much closer to the reality of practice in the community.
Bipolar radiofrequency endometrial ablation: summary of efficacy after 12 months.
Reduced bleeding refers to amenorrhea, spotting and hypomenorrhea combined. NA: Not available.
In this study performed by Cooper, a total of 265 premenopausal patients were enrolled at nine study centers; 175 patients were randomized to the bipolar RF system group and 90 to the rollerball group. No significant differences were observed between the investigational and control groups with respect to age, race, baseline pictorial blood loss assessment chart (PBLAC) score, uterine cavity length, body mass index, number of prior pregnancies or number of full-term deliveries. In addition, there were no significant differences among these variables for either treatment group across the nine sites, which allowed for pooling of the data from all study centers. When these study parameters were compared between treatment groups for those patients completing 1 year of follow-up, there were no observed differences. Furthermore, the demographic and gynecological history variables were equivalent for patients aged under 40 years when compared with patients aged 40 years and older.
Anesthesia and/or analgesia for the ablation procedure were delivered at the discretion of the investigator and the attending anesthesiologist. For the patients randomized to the bipolar RF group, 73% (127 out of 174) had the procedure performed under local and/or intravenous intravenous sedation, with the anesthesia regimen not reported for one patient. In the rollerball group, only 18% (16 out of 90) were treated under local and/or intravenous sedation. The increased use of general anesthesia in the rollerball group versus the bipolar RF group was statistically significant (Fischer's Exact Test; p < 0.0001).
The procedure time was defined, recorded and reported as the time from device insertion to device removal. The mean procedure time for the bipolar RF patients was 4.2 (± 3.5) min, which was statistically significantly less than the 24.2 (± 11.4) min required to perform the rollerball ablation (Student's t-test; p < 0.0001). There were a total of seven intraoperative adverse events, one (0.6%) of the 175 bipolar RF randomized patients, and six (6.7%) of the 90 women randomized to the rollerball group. One patient in the bipolar RF group experienced bradycardia after device insertion. After the patient was stabilized, the procedure was performed with no further complications.
Including six initially aborted cases, there were a total of 27 (10.2%) patients discontinued from the trial prior to the 12-month visit: 19 (10.8%) in the bipolar RF group and eight (8.9%) in the rollerball group. Five of these patients had a hysterectomy; three (1.7%) in the bipolar RF group and two (2.2%) from the rollerball group. Six additional patients reported persistent menorrhagia and sought additional treatment: four (2.3%) in the bipolar RF group and two (2.2%) in the rollerball group. Of these, three bipolar RF patients and one rollerball patient had a repeat ablation procedure with the rollerball device, and the two remaining patients with continued bleeding, one from each treatment group, requested medical therapy. The remaining discontinued patients consisted of eight lost to follow-up, six (3.4%) bipolar RF and two (2.2%) rollerball.
Treatment effectiveness was evaluated using PBLAC scores reported at the patient's 12-month follow-up visit. A total of 154 of the 175 patients randomized to the bipolar RF procedure and 82 of the 90 rollerball patients completed this follow-up period. A 90% or greater reduction in bleeding was achieved in 84.4% (130 out of 154) of the patients in the bipolar RF group and 76.8% (63 out of 82) of the patients in the rollerball group.
Study success, defined as a PBLAC score of 75 or less, was observed in 88.3% (136 out of 154) of the bipolar RF patients and 81.7% (67 out of 82) of the rollerball patients. A PBLAC score of 1–10 equated with spotting and a PBLAC score of 0 defined amenorrhea. A total of 40.9% (63 out of 154) of the bipolar RF group and 35.4% (29 out of 82) of the rollerball patients reported amenorrhea at 12-month follow-up.
The postoperative PBLAC scores, and therefore success rates, were stable over time. A separate analysis, comparing PBLAC scores for the first five patients undergoing the bipolar RF procedure, were compared with those of the remaining bipolar RF patients at each investigational site. No significant difference was found, thus indicating a negligible learning curve.
Prior to undergoing treatment, slightly over half of the patients in both treatment groups (56%) experienced dysmenorrhea (pain with menses). However, at 6 and 12 months posttreatment, there was a significant reduction in pain associated with menstruation. The difference between treatment groups at 12 months was statistically significant (Χ2; p = 0.02) with a greater number of rollerball patients than bipolar RF patients experiencing dysmenorrhea. There was also a significant reduction in premenstrual syndrome (PMS) symptoms postprocedure. Approximately two-thirds of the patients in both groups experienced premenstrual symptoms before treatment, while a little over a third experienced PMS at 6–12 months following treatment.
The responses to the Quality of Life and Menstrual Impact questionnaires provided a secondary measure of procedure success. Patients responded to a series of questions regarding the impact of monthly menstruation. When asked at 12 months post-treatment, 92.8% of the bipolar RF group and 93.9% of the rollerball group responded that they were satisfied or very satisfied with the outcome of the procedure. At the 12-month visit, 96.7 and 95.9% of the bipolar RF and rollerball groups, respectively, responded that they would, or probably would, recommend the procedure to a friend or relative.
In addition, two other randomized trials comparing bipolar RF impedance-controlled ablation with other global endometrial ablation systems were published. In the first study, Abbott and colleagues proceeded to perform 18 cases of endometrial ablation with a thermal balloon (Cavaterm) system and 37 with the bipolar RF system [16]. Amenorrhea rates at 12 months were 11% in the thermal balloon group and 43% in the bipolar RF group, a rate that is consistent with the other aforementioned prospective studies mentioned in this review. In the second randomized trial, Bongers and colleagues performed 83 cases of bipolar RF and 43 cases of thermal balloon ablation (Thermachoice™) and followed these patients for 1 year [17]. Amenorrhea rates were 43% in the bipolar RF group and only 8% in the thermal balloon group. Patients' satisfaction was recorded to be 90% in the bipolar RF group compared with 79% in the thermal balloon group, and this difference was statistically significant. However, both techniques significantly improved health-related quality of life [18].
Finally, compatibility with office or outpatient setting is an important aspect of this procedure and pain management is at the center of its feasibility. In a prospective, multicenter, double-arm study, we assessed intra- and postoperative pain associated with bipolar RF and thermal balloon (Thermachoice) endometrial ablation systems performed on 67 women in the office setting [19]. All patients were administered a paracervical block and mild intravenous sedation. Bipolar RF impedance-controlled ablation was associated with a statistically significant reduction of intra-and postoperative pain compared with balloon ablation. Reasons postulated for this observation include shorter procedure time, absence of uterine distension with the bipolar RF system and, possibly, a reduced liberation of by-products of the ablation into the bloodstream, notably prostaglandin F2α (PGF2α), which can cause uterine cramping.
Conclusions
The technology of RF impedance-controlled bipolar energy used to develop the NovaSure system provides physicians with a very quick, safe and easy-to-perform surgical procedure that gives consistent satisfactory results and can be performed readily in the office. A number of well designed, prospective studies published in peer-reviewed journals by gynecologists from eight different countries support these findings. Women with dysfunctional uterine bleeding resistant to medical treatment should be offered this treatment modality instead of hysterectomy or hysteroscopic endometrial ablation.
Future perspective
The underlying characteristics of the bipolar RF impedance-controlled ablation system are based on physical properties of tissues and, therefore, the ability to control the depth of tissue destruction to within a half millimeter will surely find additional applications in other fields of minimally invasive surgery. There is also a growing interest in the gynecological community to be able to offer patients concommittant hysteroscopic tubal sterilization at the time of endometrial ablation of any kind, and this should stimulate new research in the years to come.
Executive summary
The single-use bipolar disposable device, along with the portable radiofrequency (RF) controller, make up the NovaSure™ system, which provides endometrial ablation in an average of 90 s without the need for pretreatment. In can be used at any time during the menstrual cycle, even when the patient is actively bleeding.
The system uses bipolar RF and measures tissue impedance throughout the short procedure, which allows for a precise depth of ablation adapted to each uterine cavity, regardless of endometrial thickness.
Features built into the controller and device that improve safety are: the device insertion feedback and perforation detection systems, which will detect false passage or uterine perforation and prevent energy delivery; and an automatic shut-off mechanism when the ablation is terminated based on issue impedance.
Based on published data and extensive clinical experience worldwide, the risk of complications is decreased compared with hysteroscopic endometrial ablation.
This system has shown excellent results in randomized trials compared with hysteroscopic ablation and other global ablation devices, such as the thermal balloon. It has also been demonstrated to be faster and less painful than thermal balloon ablation, making it a prime choice for office use. 3-year follow-up data also confirms its long-term effectiveness.
