Abstract
Although the nephropathy of visceral leishmaniasis (VL) is known both in humans and dogs, histopathologic alterations have not been thoroughly studied. We examined renal alterations in 55 dogs with naturally acquired VL compared with five noninfected dogs from an endemic area in northeastern Brazil. Glomerulonephritis was found in 55 dogs, interstitial alterations in 53 dogs, and tubular changes in 43 dogs with VL. The glomerular alterations found were minor glomerular abnormalities (n = 8, 14.5%), focal segmental glomerulosclerosis (n = 10, 18.2%), mesangial proliferative glomerulonephritis (n = 17, 32.7%), membrano-proliferative glomerulonephritis ,(n = 18, 30.9%), crescentic glomerulonephritis (n = 1, 1.8%), and chronic glomerulonephritis (n = 1, 1.8%). Morphometric and ultrastructural studies complemented the analysis. The five control animals exhibited no glomerular alterations. The glomerular lesions were related to functional alterations. Considering that the alterations of canine and human nephropathy in VL are very similar, the data obtained in this study constitute an important contribution to the understanding of canine and human VL nephropathy.
Canine visceral leishmaniasis (VL) is a highly prevalent infection encountered throughout the world. In Brazil, VL results from infection by the protozoan Leishmania (Leishmania) chagasi, which occurs in 18 of 27 Brazilian states. 20,22,26 VL is endemic to northeastern Brazil, and in Teresina, in the State of Piaui, some 1,600 dogs presenting naturally acquired VL were known when this study was initiated. At present, VL is also spreading to other urban areas in the southern and southeast regions, where the disease was not previously endemic. 31 In the infectious cycle of VL, the dog is the most important domestic reservoir and exhibits chronic evolution of the disease. 1,8,21
Leishmania is an obligatory intracellular parasite of mononuclear phagocytes. During infection, various host organs are affected including the kidney. Although VL-related nephropathy is known both in humans and dogs, the histopathologic patterns of the lesions present in VL have not been clearly established because most studies are based on very few cases and mainly because well-defined, lesion classification criteria were not used. 3,4,9,10,24,37,38 In human VL, glomerulosclerosis, mesangial cell proliferation, and interstitial nephritis have been reported. 3,9,10,16,18,38
Renal involvement in canine VL is also frequent, and the renal changes are similar to those seen in humans. 2,5,8,23,32 This similarity renders the study of canine VL nephropathy of interest with regard to human pathology. The renal lesion itself does not lead to renal insufficiency. However, when moderate or severe renal lesions are present, VL patients with systemic complications such as secondary infections, sepsis, and hypotension do develop renal insufficiency. 16 Furthermore, glomerular lesions apparently reflect the severity of the disease because the survival of dogs receiving treatment has been related to kidney function. 36
To aid in comprehending the pathogenesis of VL, we studied renal alterations in dogs with naturally acquired VL from the city of Teresina to establish the morphologic patterns of the lesions and to evaluate correlations with clinical and laboratory findings.
Materials and Methods
Animals and VL diagnosis
The animals studied included both privately owned and stray dogs. The dogs were serologically tested for leishmaniasis (mandatory in areas endemic for leishmaniasis) in a survey performed by the Center for Zoonosis Control of Teresina city, Piaui State, Brazil. The animals showing positive serology were initially selected, and 55, male and female, adult dogs of different ages and breeds were chosen randomly from this population from May 1996 through May 1998. The diagnosis of VL was confirmed by detection of anti-Leishmania antibodies in the sera by an indirect immunofluorescence assay and enzyme-linked immunosorbent assay, by detection of Leishmania in smears of skin, spleen, and popliteal lymph nodes, or by culture of material from sternal bone marrow, spleen, or popliteal lymph nodes (or all). Parasite identification as L. (L.) chagasi was performed at the Instituto Evandro Chagas, in Belém, Para State, Brazil, in samples from two dogs, using species-specific monoclonal antibodies. Five dogs without VL from the same endemic region were used as controls. Urine and blood samples were obtained in the morning. Dogs were handled and sacrificed under general anesthesia using 25 mg/kg i.v. thiopental sodium (Sigma-Aldrich, St. Louis, MO). 14,25 All Leishmania-infected dogs were routinely sacrificed by the Center for Zoonosis Control to avoid VL transmission. The noninfected control animals were stray dogs, captured to be sacrificed for rabies control. All procedures involving animals were performed according to the Brazilian guide for care and use of laboratory animals (Projeto de lei 3.964/97—www.planalto.gov.br), and all experimental protocols used were previously approved by the Ethics Committee of the Federal University of Piaui.
Biochemical analyses of serum and urine
Total serum protein (catalog # 18), albumin (catalog # 19), and globulin concentrations were measured in 38 dogs using LABTEST Kit (Labtest Diagnóstica S.A., Lagoa Santa, MG, Brazil) and analyzed according to the methods of Coles 12 and Duncan and Prasse. 17 Estimation of the protein-creatinine ratio in isolated urine samples was performed according to Grauer et al. 19 in 11 dogs. Urine protein concentration was estimated using modified Bradford method. 7 Serum creatinine (catalog # 35), serum cholesterol (catalog # 60), and urine creatinine (catalog # 35) concentrations were measured by LABTEST Kit.
Histopathologic analysis of the kidney
Under anesthesia, the dogs were perfused with 0.01 M, pH 7.4, phosphate-buffered 10% formalin (buffered formalin) through the carotid artery for 12–15 minutes. The kidneys were removed, and the renal tissues were fixed in buffered formalin. Kidney samples were embedded in paraffin, and 3-µm-thick sections were deparaffinized in xylene and dehydrated in increasing concentrations of alcohol. Sections were stained by hematoxylin and eosin (HE), periodic acid–Schiff (PAS reaction), Masson's trichrome, periodic acid–methenamine silver (PAMS), or Congo red. The sections were analyzed by light microscopy (Axiolab, Carl Zeiss, Germany), and the renal changes were classified according to the criteria of the World Health Organization for classification of the morphologic pattern of glomerulonephritis. 11 Lesion intensity was classified semiquantitatively on a scale from 0 to 4, where 0 = normal, 0.5 = minimal or doubtful; 1 = medium; 2 = moderate; 3 = moderately severe; and 4 = severe, according to Tisher and Brenner. 30
Electron microscopy
Renal tissue was fixed in 2.0% glutaraldehyde in 0.1 M phosphate buffer, pH 7.4, postfixed in 1.0% osmium tetroxide, washed in saline, and incubated overnight in 0.5% aqueous uranyl acetate. Samples were dehydrated in increasing acetone concentrations and embedded in Araldite 502 (Polysciences, Warrington, PA). Ultrathin sections were stained with lead citrate and uranyl acetate for analysis by transmission electron microscopy (Philips, Model E.M. 201).
Detection of Leishmania antigen in renal tissue
Formalin-fixed, paraffin-embedded kidney sections were deparaffinized in xylene, rehydrated in decreasing alcohol concentrations, and then incubated with 0.03% hydrogen peroxide in methanol solution for 30 minutes in the dark to block endogenous peroxide activity. Antigen retrieval was performed using Tris-HCl (1.2 mg/ml), pH 1.0, in a microwave oven (Sanyo, Brazil), under maximum potency in consecutive cycles of 10 and 5 minutes. After washing in 0.01 M phosphate-buffered saline (PBS), pH 7.2, the sections were treated using a Blocking Kit (Vector Laboratories, Inc., Burlingame, CA) and a Protein Block (Dako Corporation, Carpinteria, CA). The tissues were then incubated with mouse, polyclonal, anti-Leishmania amazonensis antibody diluted 1 : 1,600 (vol/vol) in PBS overnight at 4 C in a humid atmosphere. 15 The reaction proceeded using a catalyzed signal amplification system—peroxidase (Dako Corporation) following protocols provided by the manufacturer, and the reaction was developed using 0.06% hydrogen peroxide and 0.3 mg/ml 3,3′-diaminobenzidine (Sigma Chemical Co., St. Louis, MO) in PBS. Counterstaining was performed with Harry's hematoxylin (Sigma).
Morphometry
Morphometric analyses were performed on some of the sections from samples stained with HE and on those stained for Leishmania antigen by immunohistochemistry using an automatic image analyzer using the Bioscan Optimas software (Version 4.10) (Optimas, Edmonds, CA). The following parameters were measured: glomerular area, total number of cells per glomerulus, total number of cells positive for Leishmania antigen per glomerulus, and total number of cells per glomerular unit in a total of 50 glomeruli per animal.
Statistical analyses
The morphometric parameters were analyzed using Kruskal-Wallis or Dunn test to compare multiple groups and the Mann-Whitney or Student's t-test to compare two groups, using Sigma Stat software (Jandel Corporation, San Raphael, CA).
Results
Clinical and laboratory findings
According to the classification modified by Pozio et al. 33 of 55 Leishmania-infected dogs, 13 were asymptomatic, 33 were symptomatic showing cutaneous lesions (alopecia, furfuraceous eczema, periorbital depilation, ulcers), keratoconjunctivitis, onychogryphosis, and nine were oligosymptomatic showing only lymph node enlargement, weight loss, and slight splenomegaly. Anti-Leishmania antibodies were detected in all infected animals, the titer ranging from 1 : 40 through 1 : 1,280. Parasites were detected in all animals in spleen, popliteal lymph node, or bone marrow samples under direct microscopic exam of smears or after culture. Biochemical parameters were examined in 49 dogs: serum protein levels were elevated in 22, hypergammaglobulinemia was present in 21, and hypoalbuminemia was found in 30.
Renal histopathologic changes
Glomerular alterations were present in all 55 naturally infected dogs. Fifty-three dogs showed tubular changes, and 43 of these also presented interstitial nephritis. The five control animals showed no histopathologic glomerular changes. The glomerular changes were classified as minor glomerular abnormalities, focal segmental glomerulosclerosis, diffuse mesangial proliferative glomerulonephritis, diffuse membranoproliferative glomerulonephritis, crescentic glomerulonephritis, and chronic glomerulonephritis as described below.
Glomerular alterations in Leishmania-infected animals
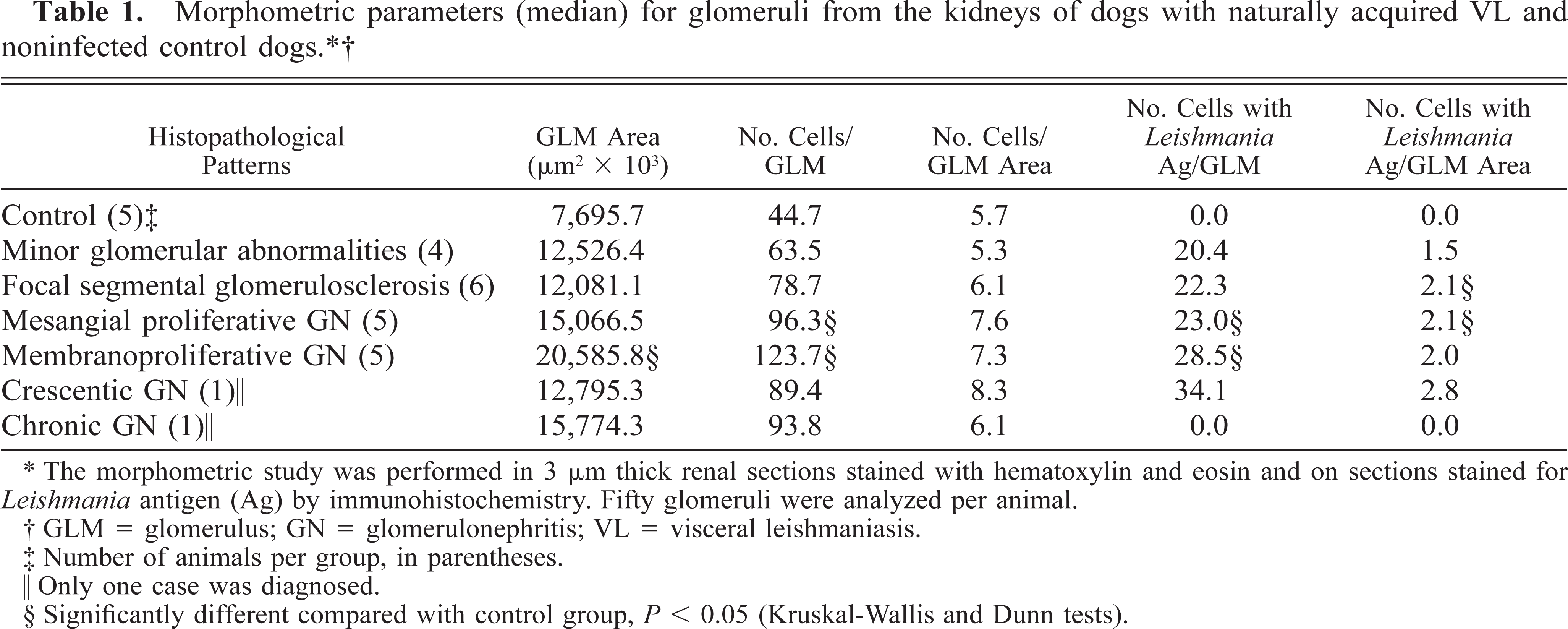
Minor glomerular abnormalities were present in eight dogs (14.5%). The glomeruli were normal in size with a slight increase in cellularity under light microscopy, and capillary walls were not thickened. In rare cases, a slight widening of the mesangium was observed. Ultrastructural analysis showed a loss or effacement of the epithelial cell foot processes (Fig. 1). Visceral epithelial cells showed degeneration with cytoplasmic vacuolation and protein droplets (Fig. 1).
Kidney; pattern of glomerulonephritis in dogs with naturally acquired VL. Histopathology (light microscopy) and ultrastructure.
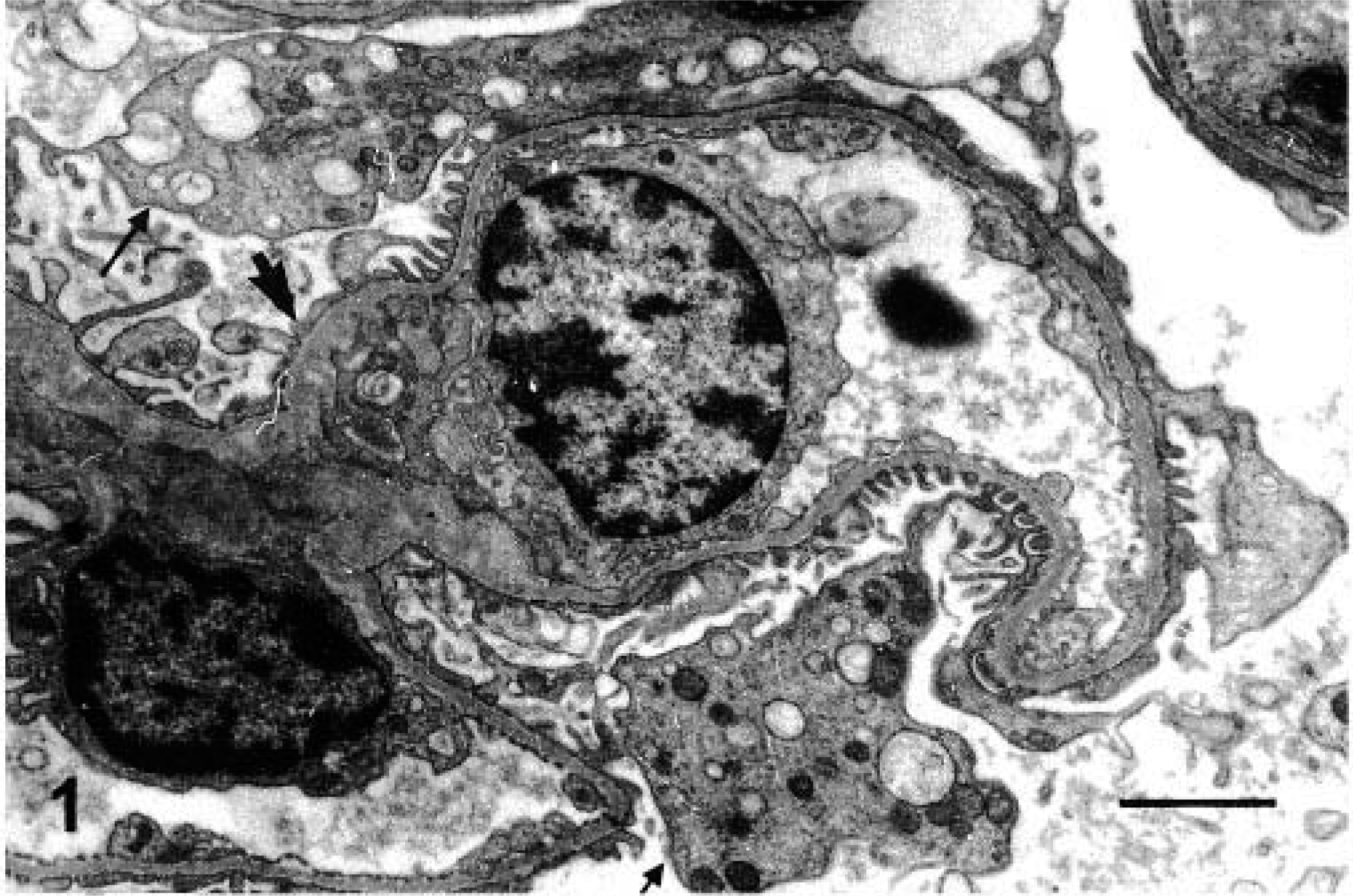
Focal segmental glomerulosclerosis was observed in 10 dogs (18.2%). The alteration was focal and segmental in distribution and characterized by sclerosis of part of the glomerular tuft, mainly in the juxtamedullary zone, close to areas with collapsed capillary lumens. In some cases, a hypercellular cap of swollen, visceral epithelial cells, sometimes containing PAS-positive protein droplets within the cytoplasm, was observed at the periphery of the sclerotic area. Ultrastructural examination revealed swelling and effacement of visceral epithelial cell foot processes (Fig. 2), pyknotic nuclei, and protein droplets in the cytoplasm of the podocytes that sometimes detached from the underlying glomerular capillary wall. The sclerotic regions exhibited collagen fibrils in proliferation. Electron-dense deposits were absent from the glomerular capillary basement membrane.
Focal, segmental glomerulosclerosis. Swelling and effacement of visceral and epithelial cell foot processes. Absence of electron-dense particles from the glomerular capillary basement membrane. EM. Bar = 2,170 µm.
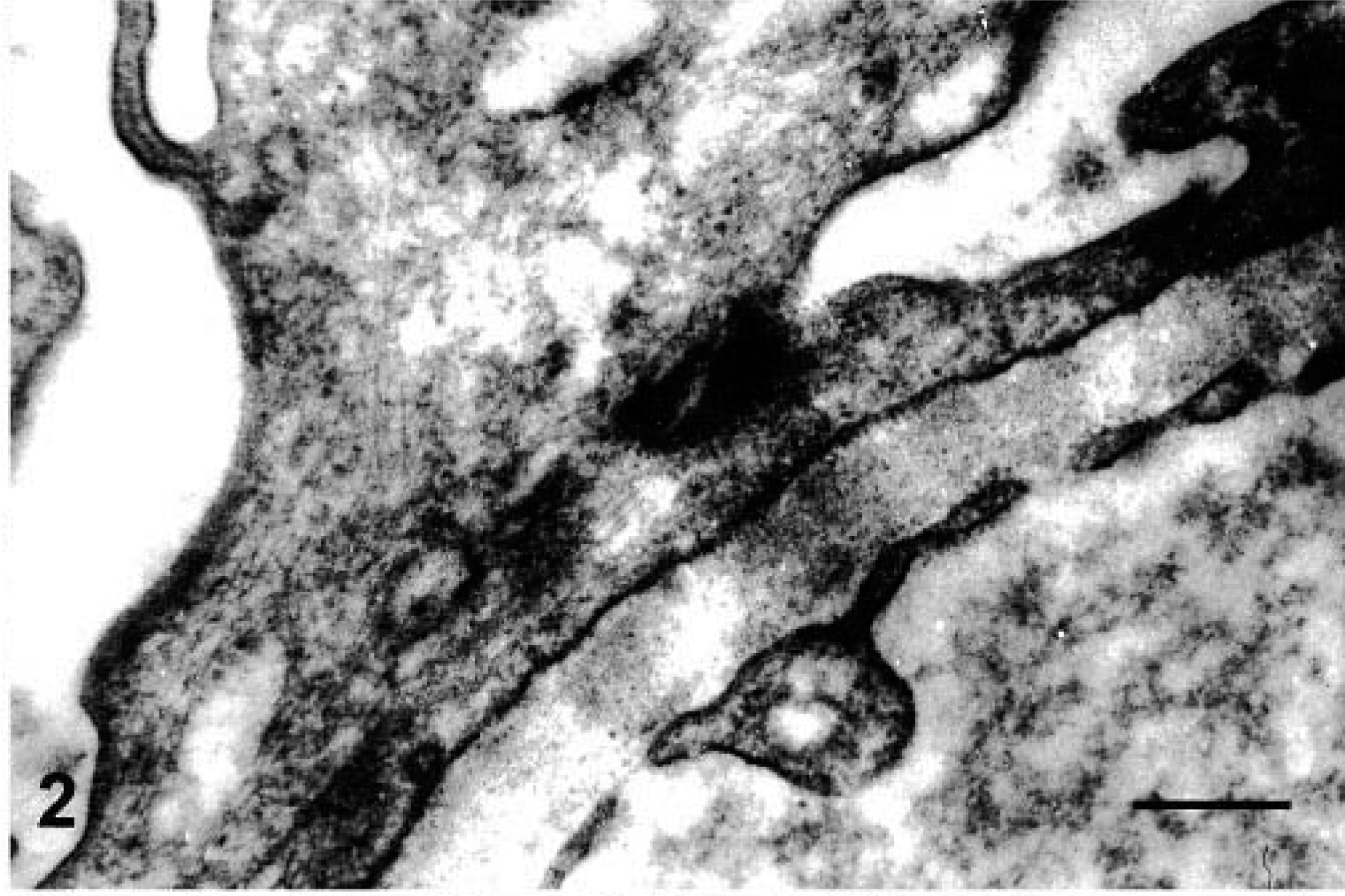
Diffuse membranoproliferative glomerulonephritis was seen in 18 dogs (32.7%). The glomerular tuft showing a patent lobular pattern was enlarged, often filling the entire Bowman's space. The mesangium was expanded, capillary lumen was narrowed, and segmental thickening and duplication of the peripheral capillary wall were present (Fig. 3). In some sections, protein deposits were evident on the capillary wall.
Diffuse, membranoproliferative glomerulonephritis. Segmental thickening and duplication of the peripheral glomerular capillary wall. PAMS. Bar = 25 µm.
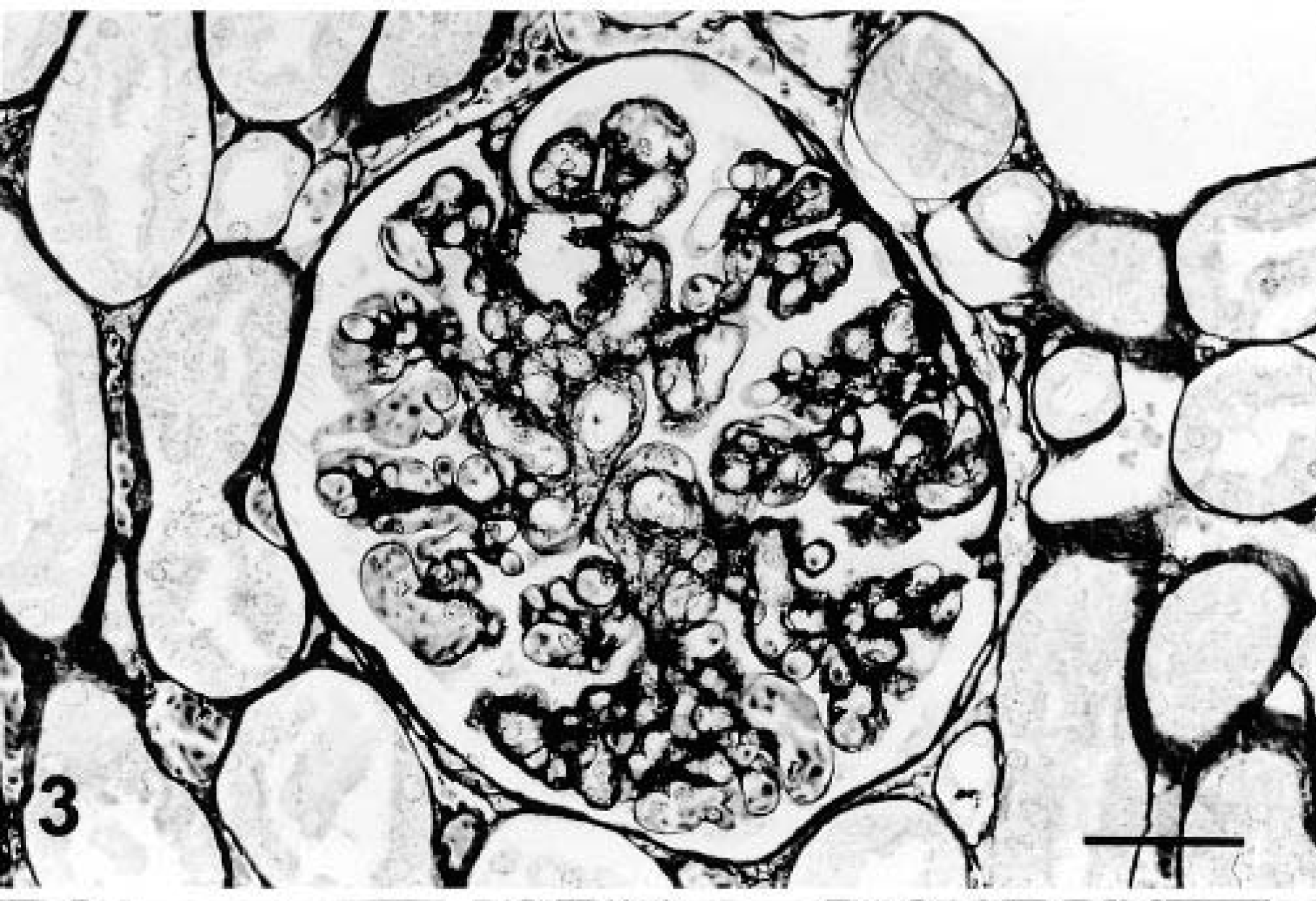
Diffuse mesangial proliferative glomerulonephritis was observed in 17 animals (30.9%). The mesangium showed global and diffuse proliferation of mononuclear cells, and the Bowman's space was nearly completely filled by the glomerular tuft. The proliferating cells formed clusters of three or more cells per mesangial area. The mesangial matrix was expanded and increased with little or no alteration of the capillary lumina; the glomerular capillary wall was normal (Fig. 4). Ultrastructural examination showed that the width and morphology of the glomerular basement membrane were normal. Electron-dense deposits were absent.
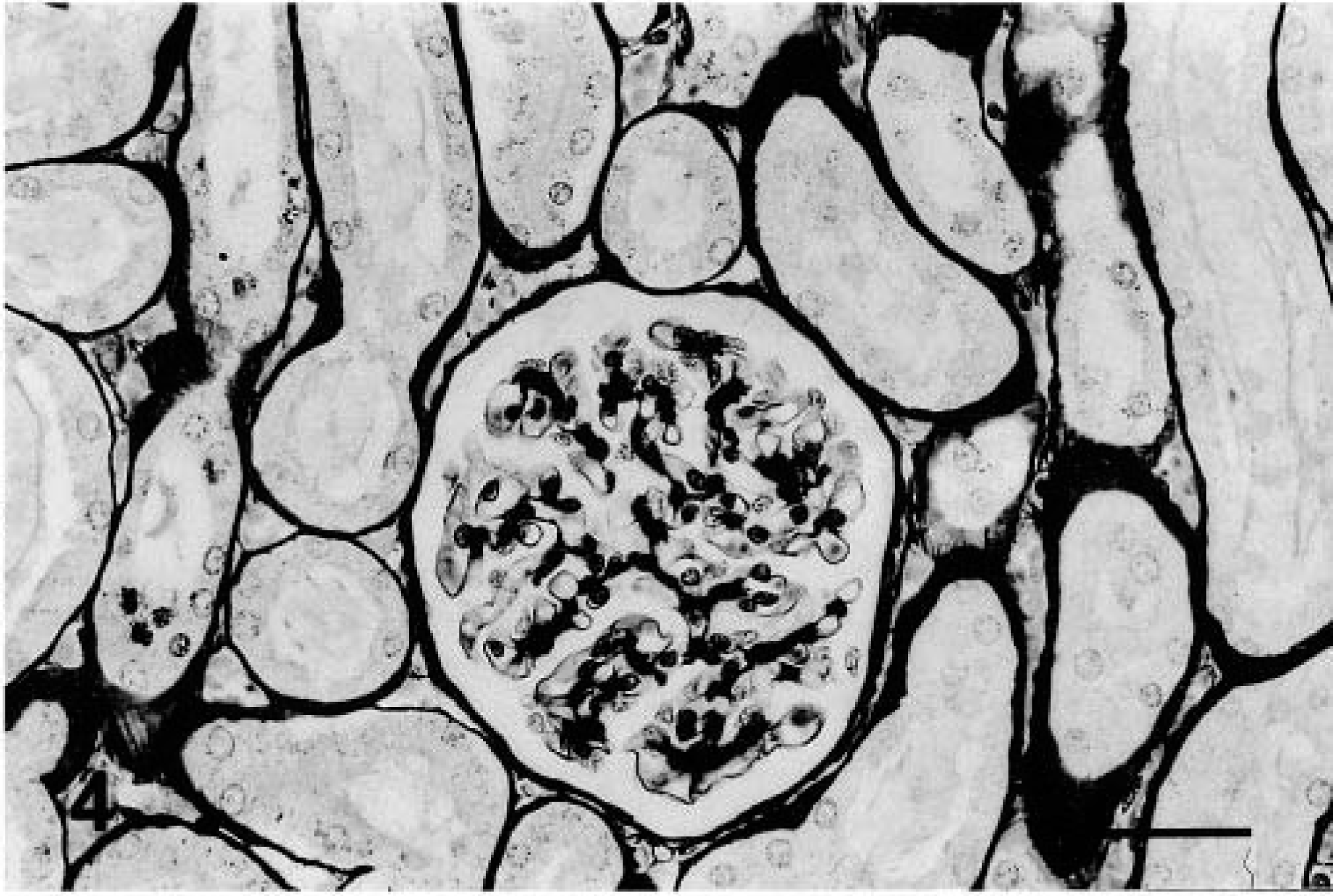
Diffuse, mesangial proliferative glomerulonephritis. Normal glomerular capillary wall. PAMS. Bar = 25 µm.
Crescentic glomerulonephritis was present in a single animal (1.8%), in which crescents were found in 43% of the glomeruli. A discrete fibrocellular or fibrous proliferation, mainly segmental (Fig. 5) but occasionally focal or rarely circumferential, filling part of the Bowman's space was present. Hyaline material was frequently deposited in the mesangium, and a duplicated basement membrane present as double contour was found. Some glomeruli exhibited mesangial centrilobular sclerosis, and a few neutrophils were present in the glomerular capillaries (less than three per glomerulus).
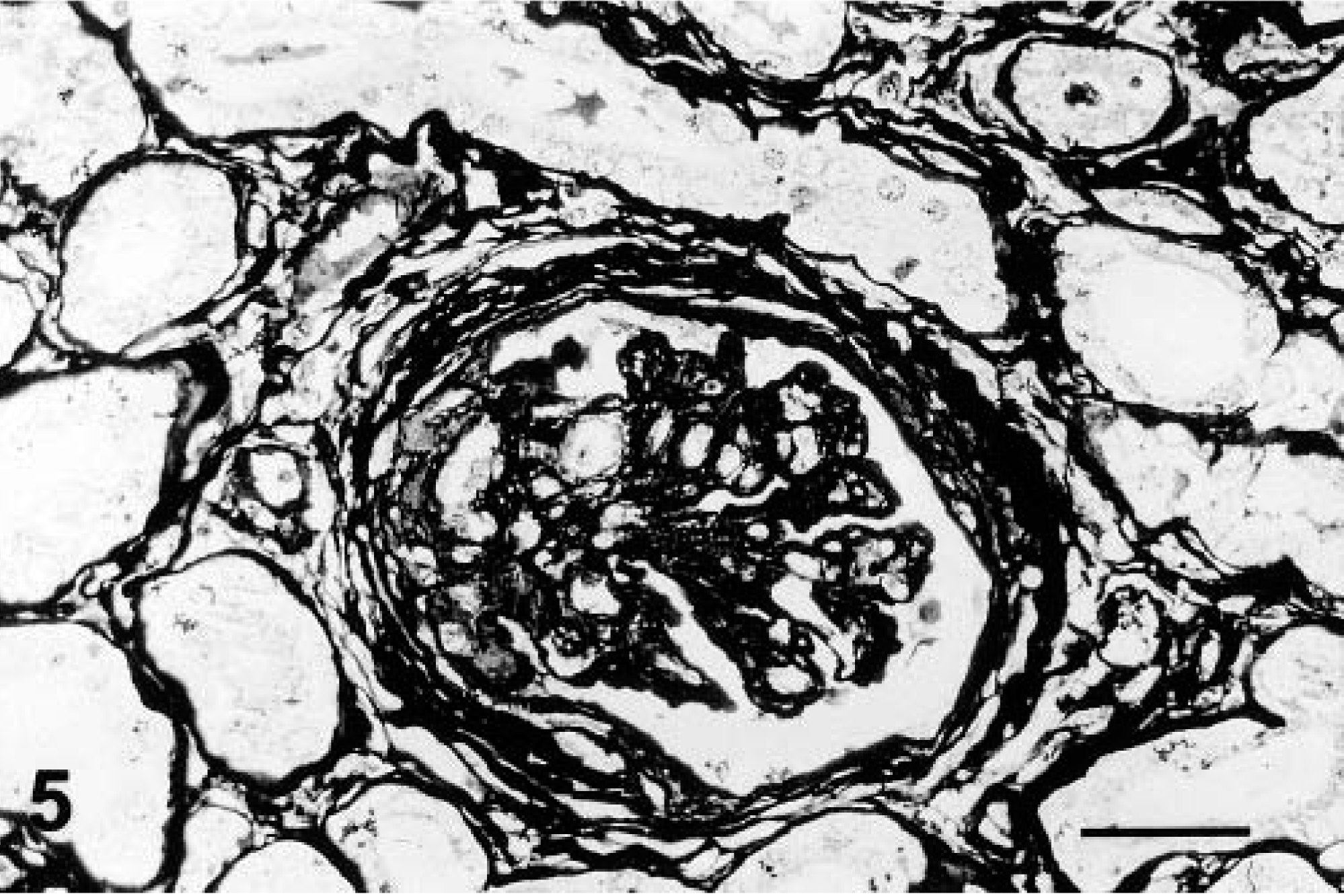
Crescentic glomerulonephritis. Fibrocellular or fibrous proliferation occupying part of the Bowman's space. PAMS. Bar = 25 µm.
Chronic glomerulonephritis was found in one animal (1.8%). Nearly all glomeruli exhibited intense proliferation of the mesangial matrix and obstruction of the capillary lumen (glomerular sclerosis), transforming the glomerular tuft into an amorphous, atrophic, hypocellular or acellular mass. Fibrosis, tubular atrophy, and severe interstitial infiltration of mononuclear cells were present. Transmission electron microscopy revealed intense fibroblast activity, collagen proliferation, and cellular remnants in the interstitial space (Fig. 6).
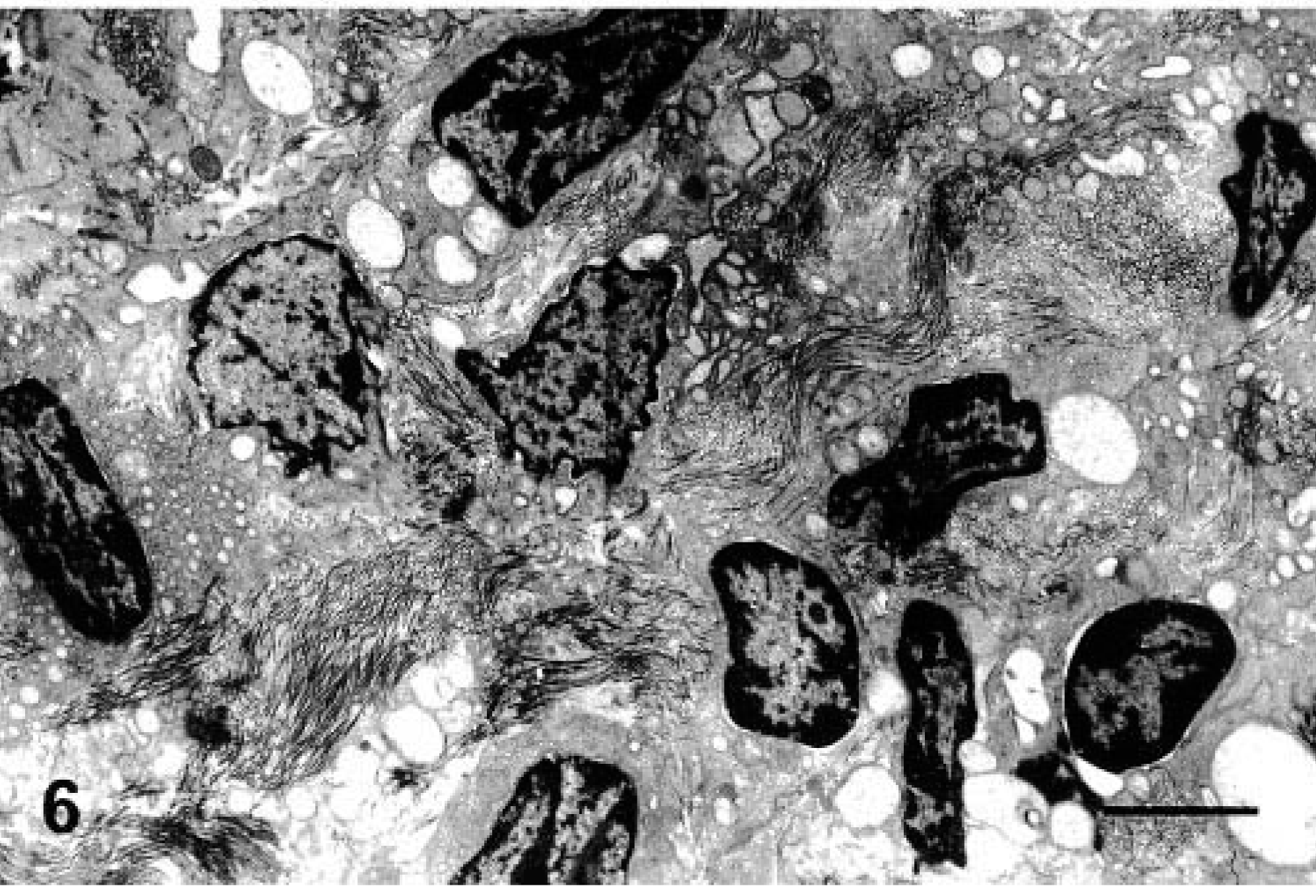
Chronic glomerulonephritis. Intense activity of fibroblasts, collagen proliferation, and cell remnants in interstitial space. Bar = 350 µm.
Morphometric studies revealed 44.7 (median) cells per glomerulus in the noninfected control dogs (Table 1). A significant increase was observed in glomerular area (Fig. 7)(P < 0.001, Mann-Whitney test) and cell number per glomerulus (Fig. 8)(P < 0.001, Mann-Whitney test) in the infected animals when compared with the noninfected control dogs. However, considering the histopathologic pattern, the glomerular area was significantly greater only in the dogs showing membranoproliferative glomerulonephritis compared with the control group (P < 0.05, Kruskal-Wallis and Dunn tests) (Table 1). Cell number per glomerulus was greater in the groups showing mesangial proliferative glomerulonephritis and membranoproliferative glomerulonephritis compared with the control group (P < 0.05, Kruskal-Wallis and Dunn tests) (Table 1).
∗ The morphometric study was performed in 3 μm thick renal sections stained with hematoxylin and eosin and on sections stained for Leishmania antigen (Ag) by immunohistochemistry. Fifty glomeruli were analyzed per animal.
† GLM = glomerulus; GN = glomerulonephritis; VL = visceral leishmaniasis.
‡ Number of animals per group in parentheses.
‖ Only one case was diagnosed.
§ Significantly different compared with control group, P < 0.05 (Kruskal-Wallis and Dunn tests).
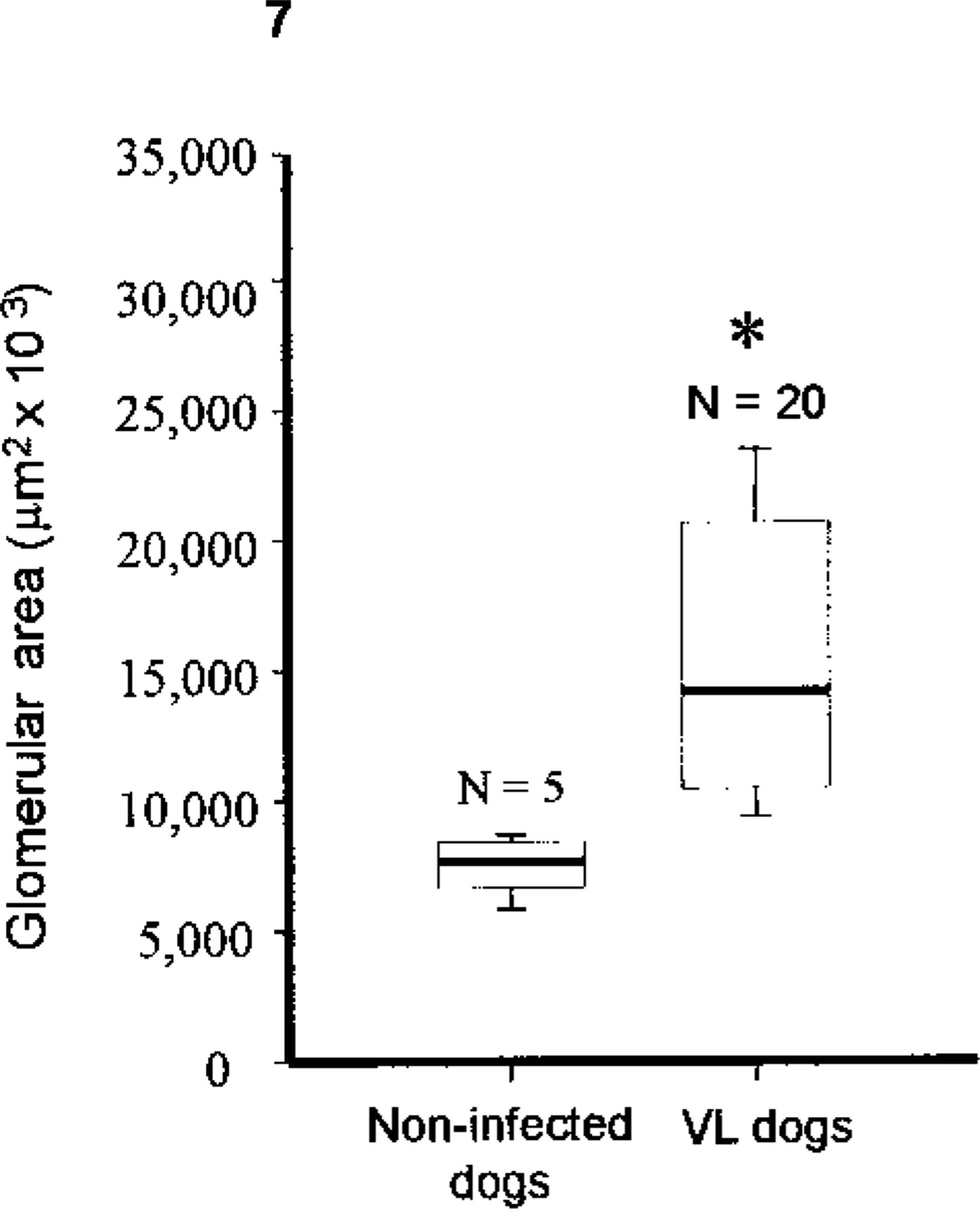
Kidney; dogs with naturally acquired VL. Morphometric parameters (median and 25–75 percentile intervals) for glomeruli from the kidneys of dogs naturally infected with, Leishmania (Leishmania) chagasi and noninfected control dogs. Glomerular area.
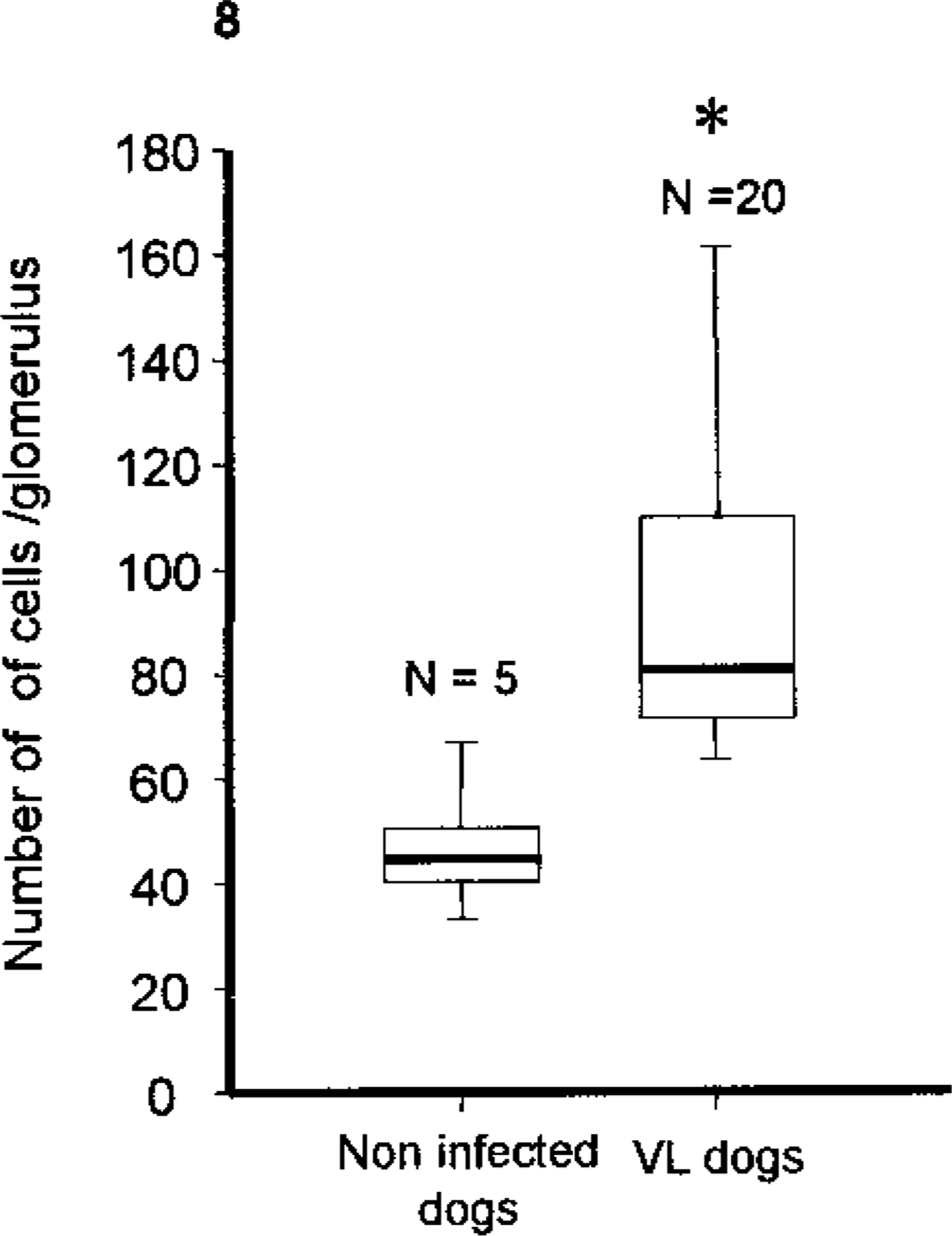
Kidney; dogs with naturally acquired VL. Morphometric parameters (median and 25–75 percentile intervals) for glomeruli from the kidneys of dogs naturally infected with, Leishmania (Leishmania) chagasi and noninfected control dogs. Cell number per glomerulus. ∗ = P < 0.05 (Mann-Whitney test).
Interstitial changes
In 43 (78.2%) of the 55 infected dogs, interstitial nephritis was present and more prominent in the renal cortex. Only 13 animals (23.6%) exhibited an inflammatory infiltrate in the medulla. In these cases, the lesions were also more severe in the cortex. The inflammation in the cortex was organized into foci and constituted primarily by lymphocytes and plasma cells, although scarce histiocytes and polymorphonuclear neutrophils were also present. In a few cases, the inflammatory infiltrate was severe and diffuse, occasionally localized in intertubular cords, in small clusters or even as massive foci, spreading in areas of fibrosis. Where the alterations were less conspicuous, the inflammatory infiltrate was localized in peritubular, intertubular, and perivascular areas. In more intense cases, a very well-defined periglomerular organization forming a circle around the Bowman's capsule was present. The inflammatory infiltration in the medulla was less conspicuous, present as multiple foci, and localized below the corticomedullary region. The most frequent tubular change was vacuolar and hyaline degeneration, also present in cases without interstitial inflammatory infiltration and atrophy. Necrosis was found in isolated tubules when more conspicuous inflammatory foci were present.
Detection of Leishmania antigen
In 50 infected dogs (90.9%), Leishmania antigen was revealed in the glomeruli; in 34 (61.8%), antigen was also observed in the interstitial inflammatory infiltrate. Intensity ranged from minimal to severe. The antigen was detected in a cellular pattern in phagocytic cells of the glomeruli, in the interstitial mononuclear cell infiltrate, and seldom in the form of particulate extracellular material as previously seen. 13 The antigen was also detected in tubular epithelial cells, even in apparently normal tubules. The whole parasite was not detected in any case. Leishmania antigen was not detected in the renal tissue of the five control animals.
Morphometric analysis revealed more cells with antigen per glomerulus in cases showing mesangial proliferative glomerulonephritis and membranoproliferative glomerulonephritis compared with the control group (P < 0.05, Kruskal-Wallis and Dunn tests) (Table 1). When the number of cells showing Leishmania antigens per glomerular area was analyzed, a significant difference (P > 0.05, Kruskal-Wallis and Dunn tests) was found between the control group and those exhibiting focal segmental glomerulosclerosis and mesangial proliferative glomerulonephritis (Table 1). Leishmania antigens were not seen in the only case of chronic glomerulonephritis.
Correlation of pathologic, clinical, and laboratory findings
In 11 animals, blood and urine samples were obtained concomitantly to evaluate renal function. Six dogs presented proteinuria (i.e., urine protein-creatinine ratio > 1.0), three showed increased creatinemia (serum creatinine > 1.0 mg/dl), and only two animals showed increased cholesterol level (serum cholesterol > 210.0 mg/dl). Proteinuria and increased serum creatinine and cholesterol levels were observed only in the cases presenting glomerulonephritis, except for minor glomerular abnormalities and concomitant, interstitial nephritis (Table 2).
Pathologic, clinical, and laboratory findings in 11 dogs with naturally acquired VL. ∗
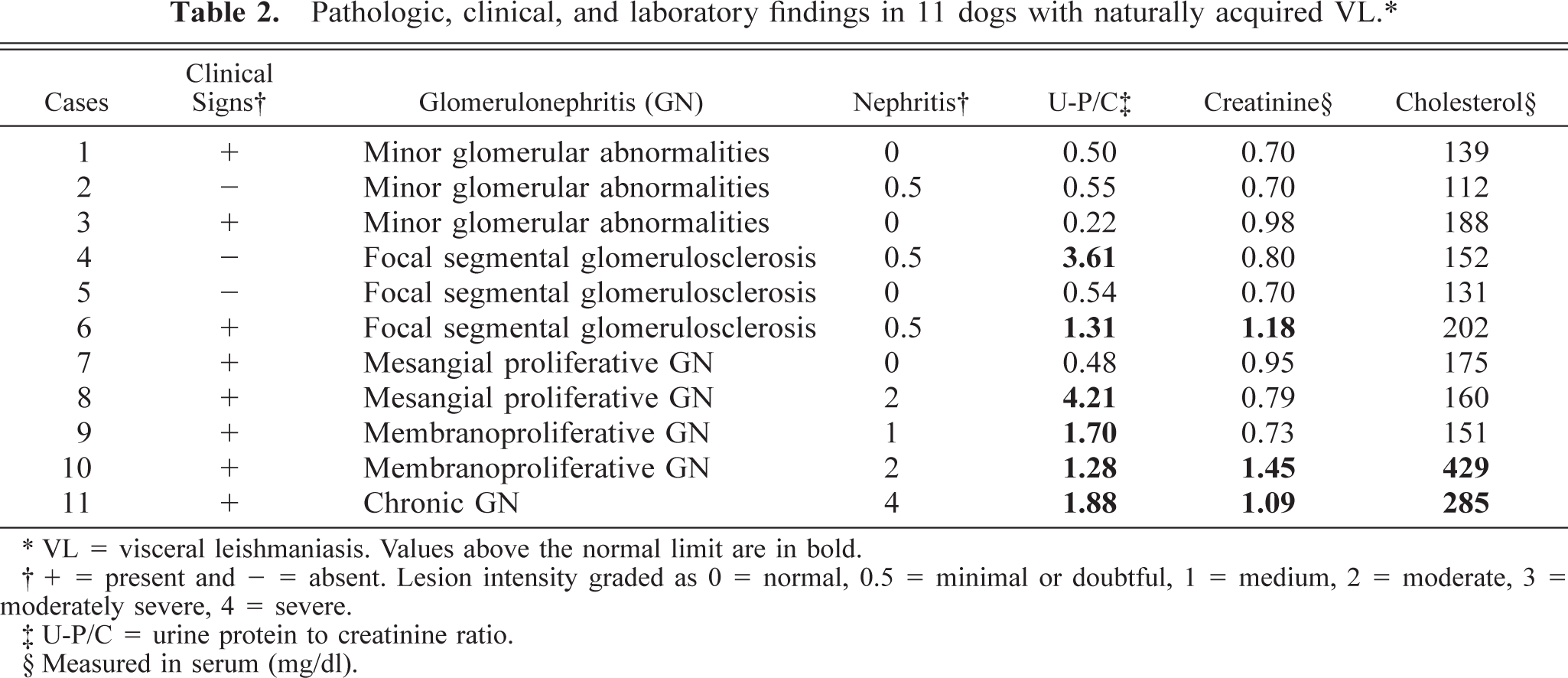
∗ VL = visceral leishmaniasis. Values above the normal limit are in bold.
† + = present and — = absent. Lesion intensity graded as 0 = normal, 0.5 = minimal or doubtful, 1 = medium, 2 = moderate, 3 = moderately severe, 4 = severe.
‡ U-P/C = urine protein to creatinine ratio.
§ Measured in serum (mg/dl).
Discussion
A high frequency of interstitial nephritis (78.2%) and glomerulonephritis (100.0%) was found in 55 dogs with naturally acquired VL. In most cases, the Leishmania antigen was detected, indicating that the lesions were related to VL. Clinical and necropsy examinations in these animals showed no alterations suggestive of other diseases, and the dogs had not been submitted to potentially nephrotoxic drug treatments. Noninfected animals from the same area showed no glomerular changes or Leishmania antigens in the kidney.
In this study, we observed a wide variety of patterns of glomerular lesion not previously reported. In canine VL in France and Spain, diffuse membranoproliferative glomerulonephritis was the only pattern found in naturally infected dogs. 5,27 In another study of naturally acquired VL in Italy, diffuse membranoproliferative glomerulonephritis and diffuse mesangial proliferative glomerulonephritis were diagnosed. 32 These two patterns were also those most frequently seen in our study. The absence of other patterns in other studies may be because of the small number of animals used or because of the different species of Leishmania involved.
In human VL, the most frequently described alterations are glomerular sclerosis and proliferation of the mesangial cells. 3,9,38 We also encountered a relatively high frequency of focal segmental glomerulosclerosis in this study, the diagnosis of this pattern being reinforced by ultrastructural data showing fusion of podocyte pediceles. Another pattern seen in human VL is minor glomerular abnormalities, also frequent in our study. 18 In these cases, although the histopathology was considered normal and high proteinuria was absent, ultrastructural data showed fusion of podocyte pediceles in some areas and glomerular, visceral, and epithelial cell vacuolization and protein droplets in the cytoplasm of the podocytes.
Crescentic glomerulonephritis and chronic glomerulonephritis have not been described in either natural or experimental VL. In this study, the Leishmania antigen was not found in chronic glomerulonephritis, and thus we cannot assume that the renal lesions resulted from Leishmania infection. However, chronic glomerulonephritis represents the final outcome of several types of glomerulonephritis, and it is likely that the antigen had already been eliminated from the tissue.
The predominance of proliferative glomerulonephritis in parasitic diseases is not restricted to VL, and this pattern has been observed in human schistosomiasis. 28 This may be attributed to a chronic antigenemia present both in VL and schistosomiasis. Although the patterns found in this study extend over a wide range of alterations, the amyloidosis often described in experimental VL in the hamster was not encountered. 15,29,35
Interstitial nephritis and glomerular alterations in canine VL were mainly localized in the cortical region as also seen in human VL. 16 Although glomerular involvement in human VL is less frequently reported than interstitial nephritis, it was diagnosed in all our animals as also observed by Poli et al. 32 in canine VL and possibly related to the usually longer evolution of the disease in dogs. 16
The renal lesions found in this study comprised not only of interstitial nephritis and glomerulonephritis but also hyaline degeneration, vacuolar degeneration, tubular atrophy, and fibrosis that may cause alterations in renal function and may affect the evolution of the disease. The symptoms recorded in this study in 33 animals were compatible with those described in the literature, and in 80% of these symptomatic cases, proliferative glomerulonephritis also was seen (data not shown). 33 Poli et al. 32 found a significant correlation between the presence of diffuse proliferative and membranoproliferative glomerulonephritis and oligosymptomatic and symptomatic dogs.
When renal function was evaluated, the frequency and intensity of proteinuria in this study were greater than the 30–35% observed in other studies. 27,32 Variation in creatinine level was variable in other studies, which showed higher or lower levels than those obtained in this study. 5,34 Like human VL cases, proteinuria and increased levels of serum creatinine and cholesterol were observed only in cases concomitantly presenting interstitial nephritis and glomerulonephritis but minor glomerular abnormalities. 16 Alterations in serum creatinine have been more related to tubulointerstitial alterations than to the severity of glomerular lesions. 6 However, in the present study, proteinuria, increased creatinemia, and hypercholesterolemia were absent in cases showing minor glomerular abnormalities, suggesting an important contribution of glomerular lesions to functional alterations, which may be related to the severity or chronicity of the lesions.
Our findings suggest that VL in dogs causes both glomerular and interstitial lesions that are related to functional alterations. In addition to certain differences attributed to the peculiarity of the host, and to the usually longer evolution of the disease in dogs, the nephropathies present in canine and human VL are very similar. We consider the data from this study to be very relevant to comprehending both canine and human VL nephropathy. Further studies are in progress to analyze the pathogenesis of the disease.
Footnotes
Acknowledgements
We thank Dr. S. M. L. T. Hidd of the Department of Biochemistry and Pharmacology, Universidade Federal do Piauí, for biochemical analyses of serum and urine, and the Histopathology Laboratory of the Department of Pathology, Faculdade de Medicina, and Faculdade de Medicina Veterinária e Zootecnia, Universidade de São Paulo, for histopathologic preparations. This study was supported by FAPESP (98/10364–8), CAPES (scholarship to FALC), CNPQ (fellowship to HG and JLG), and LIM-38 HC/FMUSP.