Abstract
Summary
Objectives
To determine how many General Practice (GP) Registrars in the London Deanery taught medical students during their final year of training. For those who did teach, to evaluate their experiences and for those who did not, to identify perceived barriers to teaching.
Design
Cross sectional survey of GP Registrars in the London Deanery completing their training in August 2010.
Setting
Online survey of GP Registrars sent after completion of training via the London Deanery GP Vocational Training Scheme (VTS) programme administrators.
Participants
GP Registrars in the London Deanery completing their training in August 2010.
Main outcome measure
The proportion of London Deanery GP registrars completing training in August 2010 who taught medical students during their registrar year.
Results
Over half of respondents were involved in some form of medical student teaching during their registrar year. Most of those who taught felt it enhanced their training, and the majority of those who did not teach would have liked to. Commonly cited barriers to teaching were: students not attached to the practice; not being given the opportunity to teach; and not having time to teach.
Conclusions
This evaluation demonstrated that GP registrars are either already involved with undergraduate teaching or want to get involved and the majority who teach feel that it enhances their training. A UK-wide study investigating the experiences and views of both GP registrars and GP trainers is warranted and qualitative work using focus groups or semistructured interviews would be valuable to develop the questionnaire for wider dissemination.
DECLARATIONS
The authors teach medical students as part of their work both at the Department of Primary Care & Public Health at Imperial College and in clinical practice and have a keen interest in the involvement of junior doctors in Medical Education
Both Bronwen Williams and Cressida Amiel hold Academic GP ST4 posts at Imperial College, funded by the London Deanery. The Department of Primary Care & Public Health at Imperial College is grateful for support from the NIHR North West London CLAHRC Scheme, the NIHR Biomedical Research Centre scheme, and the Imperial Centre for Patient Safety and Service Quality.
This was an evaluation of current practice rather than new research and ethical approval was therefore not sought.
BW and CA
Dr Paul Booton (Director of medical education, Imperial College Department of Primary Care and Public Health) conceived the study. CA and BW wrote and disseminated the questionnaire, performed the analysis and wrote the manuscript.
Joe Rosenthal
Introduction
Teaching medical students and junior doctors is part of the established tradition of medical practice. This has received recent endorsement in the General Medical Council's Tomorrow's Doctors, which states that graduates should be able to ‘reflect, learn and teach others' 1 and Good Medical Practice, which recognizes that ‘teaching, training, appraising and assessing doctors and students are important for the care of patients now and in the future’. 2
In the United Kingdom, curriculums for both Foundation doctors and General Practice trainees identify teaching as a core competency. The Royal College of General Practitioners GP Curriculum includes a detailed list of learning outcomes relating to teaching, which include designing, planning, structuring and facilitating teaching episodes in both small group and one-to-one settings. 3
Many GP registrars will have been involved in undergraduate teaching during their hospital placements. In the hospital setting, junior doctors contribute significantly to medical student teaching and in some situations are perceived by students to be their ‘most important clinical trainers’. 4 Students may feel more able to ask questions from doctors who are closer to them in age and experience; and junior doctors can relate to students more easily, and share learning and exam techniques from their own experience. 5 Less experienced doctors are still learning the process of clinical reasoning themselves and may therefore work through problems in logical steps that are accessible to students. In this way, junior doctors can ‘complement rather than duplicate the contributions’ made by more senior colleagues. 5 Furthermore, junior doctors enjoy teaching, consider it important, and feel that it improves their clinical knowledge and skills, and encourages self-directed learning. 6 However, despite the extensive (and often positive) involvement of junior hospital doctors in undergraduate teaching, there is often a lack of training, feedback or supervision. 7
Traditionally, medical student placements in general practice were short, and teaching was usually undertaken by experienced GPs. However, the proportion of community-based undergraduate teaching is increasing. There are some practical and logistical reasons for this, such as a reduction in hospital beds, shorter hospital stays and transfer of services to community practitioners, which result in fewer learning opportunities for medical students in hospitals. However, this has also been a positive educational choice, supported by Tomorrow's Doctors, 1 which provides students with the opportunity to see and manage common problems and chronic diseases, see preventative healthcare and public health interventions in practice and see patients in the context of their social and family environment. The shift in undergraduate education policy, which has occurred alongside the changing structure of primary care organizations, has necessitated a rise in teaching capacity in general practice, and newly qualified GPs and GP registrars are becoming increasingly involved.
A literature review published in 2010 8 identified three research papers specifically relating to this topic, all from Australia. One study involved surveys and qualitative interviews with both GP trainers and registrars. The study found that whilst GP registrars were both enthusiastic and confident about becoming involved in teaching, GP trainers had concerns (including funding, time, patient load, training and physical space in the surgery). 9 In another study, a survey was sent to GP registrars asking about their teaching experience and previous training in teaching skills and identified that only 9% of respondents had received any training in teaching. 10 Finally, a focus group study involving GP trainers and registrars reported that GP registrars expressed concerns about renumeration and that teaching may slow their consultation rate, and that both groups felt the need for training in teaching and supervision of teaching. 11
The literature review did not identify any UK based research looking at GP registrar involvement in undergraduate teaching and concludes that ‘there is a lack of research into the feasibility and acceptability for, and barriers to, UK GP registrars taking on more formal teaching roles’. 8 Because of the lack of UK-based research, we carried out an evaluation of current practice by investigating the teaching experiences of GP registrars who had recently completed their registrar year in the London Deanery, with the aim that this could inform future research in this area.
Aims
To identify the proportion of GP registrars in the London Deanery who were involved in medical student teaching during their registrar year;
To evaluate the experiences of those who did teach, in terms of the type and amount of teaching they were involved in, any training or supervision that they may have had and their opinion on the impact of medical student teaching on their GP training;
To explore whether those who did not teach would have liked to, and the potential barriers to GP registrars teaching medical students.
Methods
As no suitable questionnaire or validated scales existed, we developed a new, structured, online questionnaire tool, hosted by the online survey website www.surveymonkey.com. This allowed access to the trainees within the time and financial constraints of the evaluation project. Initial drafts were piloted with a GP registrar and the final tool was reviewed by the undergraduate teaching staff at the Department of Primary Care & Public Health at Imperial College to increase content validity.
Owing to data protection constraints, we were not able to obtain the individual email addresses of each GP registrar. Instead, we contacted each GP Vocational Training Scheme (VTS) programme administrator in the London Deanery, with a request to forward the online questionnaire to GP registrars who had completed their training in August 2010. An initial email was sent to programme administrators in September 2010 with the hope that experiences of teaching would be fresh in the minds of newly qualified GPs. This was followed by four reminder emails between September and October 2010. Programme administrators were asked to confirm how many GP registrars the online questionnaire had been sent to. Figure 1 summarizes the data collection process and numbers involved.

Data collection process
Results
1. What proportion of GP registrars were involved in medical student teaching?
A total of 40 out of 65 (62%) GP registrars reported being involved in some form of medical student teaching during their GP registrar year.
2. What type of medical student teaching were GP registrars involved in?
Figure 2 illustrates the different types of medical student teaching undertaken by GP registrars.

Type of medical student teaching undertaken by GP registrars (GPRs)
One-to-one teaching in surgery n = 32 (80%)
The majority of GP registrars who taught were involved in this type of teaching. From the free-text responses, generally one-to-one teaching in surgery was done on an ad hoc and unplanned basis. The following quote from one of the GP registrars reflects some of the concern felt about this:
‘Would be useful to have some sessions on it in VTS and get prior notice of students coming, rather than another GP just asking at the last minute’
Within this category, the individual GP registrar experiences varied considerably: some reported being observed themselves, some observing medical students in surgery and then critiquing their performance. Some GP registrars reported taking medical students on home visits, teaching about prescriptions and pharmacology, aiding with patient projects and undertaking formal one-to-one teaching of clinical skills.
Small group teaching as part of their undergraduate course n = 16 (40%)
GP registrars reported teaching small groups of between 4 to 6 students in a variety of medical student year groups (1-5) on a range of teaching topics. Examples included clinical methods teaching for Year 3, facilitating problem based learning sessions for Year 2 and small group teaching of final year students to prepare for end-of-year examinations. One GP registrar helped to organize a teaching module for final year students based in General Practice. Some GP registrars reported teaching other topics in small groups such as obstetrics and gynaecology and public health, from a primary care perspective.
Large group lectures or presentations n = 3 (7.5%)
These 3 GP registrars reported giving introductory lectures on general practice, giving lectures on dermatology, paediatrics and psychiatry, and also grand round teaching and presentations in a hospital environment. However, it was unclear whether the latter was done during their GP registrar year or during the trainee's hospital posts.
3. How much time did GP registrars spend preparing to teach and teaching medical students during their registrar year?
Figure 3 illustrates that half of GP registrars did not prepare for teaching medical students during their registrar year, which correlates with the ‘ad hoc’ nature of the one-to-one teaching in surgery that the majority GP registrars reported involved in. Most registrars taught students for between 2 to 5 hours during their entire registrar year. However, 10 registrars (25%) were involved in greater than 10 hours teaching over the year.
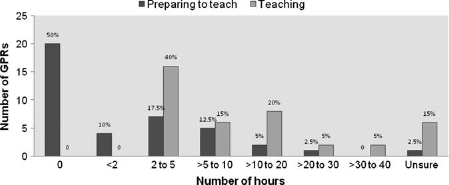
Hours spent preparing to teach and teaching during GPR year
4. Did GP registrars receive any training or supervision for their medical student teaching?
Figure 4 illustrates that the majority of GP registrars (60%) did not receive any training or supervision for their medical student teaching. In terms of supervision, surprisingly, the GP registrars who were involved in an extensive amount of teaching, including small group teaching lectures or presentations often did not receive any supervision.

Number of GPRs receiving training or supervision
5. What impact did GP registrars feel medical student teaching had on their GP training?
GP registrars were asked to rate what effect teaching medical students had on their GP training overall. Figure 5 illustrates that the overwhelming majority felt it enhanced their training. Indeed, only one registrar felt teaching hindered their training, citing lack of time for medical student teaching as the reason for this.

Overall effect of medical student teaching on GP training
6. What proportion of GP registrars did not teach?
25 out of 65 (38%) GP registrars were not involved in medical student teaching during their registrar year. 22 of the 25 (88%) reported they would have liked to have been involved teaching.
7. What barriers to teaching medical students can be identified?
The following barriers were identified from the GP registrars free-text responses, supported with some quotes:
No medical students attached to training practice (42%) n = 11
‘We did not have medical students at our practice. It would be great to have the option, even if it's a session at another practice.’
‘Medical students not welcome at my practice.’
No opportunity to teach during GP registrar year (31%) n = 8
‘Really enjoy teaching but wasn't given any opportunity for developing this during my ST3 year… It's likely we're all going to have some teaching role as GPs, and learning how to do this from an early stage would have been really beneficial’.
‘Medical students taught by another partner in the practice. Lack of opportunity to help’
No time to teach during GP registrar year (23%) n = 6
‘I would not have had enough time to plan and teach medical students, even though I think this would have been a very interesting experience.’
‘I did not have the opportunity [to teach]. There did not seem to be any time available to prioritize teaching during the already very busy ST3 year.’
‘Too time consuming. Would have had to do in own time rather than surgery time.’
Feeling inexperienced and not qualified to teach (8%) n = 2
‘Medical student teaching is ok if you are nearing the end of registrar year but can be stressful if you're not sure what you're doing yourself, never mind teaching someone else!’
‘Nervous about not having experience.’
GP trainer not keen on GP registrar teaching (4%) n = 1
‘In-spite of my previous teaching experience and presence of students in the practice, my trainer was not keen for teaching by registrars.’
Unsure how to get involved in teaching (4%) n = 1
‘No students at my practice and I wasn't sure how to do teaching with the university.’
Discussion
Nearly two thirds (62%) of London Deanery GP registrars who completed the questionnaire were involved in some sort of medical student teaching during their registrar year. The individual experiences of these registrars appear to be varied in terms of the type of teaching undertaken, and the amount of time dedicated to teaching and preparing for it. The majority of registrars were involved in one-to-one teaching in surgery (82%), taught for 5 hours or less for the entire registrar year, without prior preparation and did not receive supervision or training. This last point is consistent with previous research in both primary and secondary care settings.7,10 Despite this, the majority (75%) felt that overall their teaching experiences enhanced their GP training which reflects previous research showing that junior doctors enjoy teaching and consider it important for their clinical development. 6 Of those GP registrars who were not involved in teaching (38%), a significant majority would have liked to have been involved (88%). The main barriers to teaching identified were not having medical students attached to the practice, not being given the ‘opportunity’ to teach and lack of time to dedicate to teaching during the GP registrar year. Similar concerns were raised in two of the Australian studies in this area,9,11 as discussed previously.
This was a small evaluation of GP registrars’ experiences of undergraduate teaching, with the aim of informing new research in this area in the future. The questionnaire was only sent to GPs who had trained in the London Deanery area and therefore may not be representative of the UK as a whole. Despite four reminder emails, the response rate was 38%, which resulted in a relatively low number of questionnaires (n = 65) being completed. This may be explained by the mode of administering the questionnaire (via email) and because we were unable to access the GP registrars directly. This response rate can be compared with the previous survey-based research in this area as follows: Usherwood et al. received a 52% response rate for their survey regarding GP registrars’ experience of teaching, but this resulted in a sample size of only 22 trainees. 10 Dodd et al. 9 received a survey response rate of 62.2% from GP registrars (n = 84) but were able to offer a book token as an incentive to complete the survey, which was unfortunately not possible in our study due to financial constraints. These relatively small sample sizes highlight the limited extent of research that has taken place to date, and the need for larger scale studies to investigate this area further. As with all surveys of this nature, there may have been an element of selection bias, with registrars who had a very positive or very negative experience of undergraduate teaching being more likely to respond.
Teaching medical students and junior doctors is a core competency of GP registrars, endorsed by both the General Medical Council and Royal College of General Practitioners. This evaluation has demonstrated that GP registrars who were given the opportunity to teach value their experiences, and feel that they have enhanced their GP training. Specifically, those registrars who were able to undertake small group teaching sessions with adequate time for preparation appeared to derive the most benefit. However, currently the teaching experiences of GP registrars in the London Deanery appear to be diverse and lack uniformity. Formally incorporating medical student teaching into GP VTS sessions and providing them with at least one opportunity to put this into practice in a formal teaching setting, might be a way of exposing all GP trainees to teaching methods, without adding undue burden to their busy registrar year. In addition, trainees undertaking four year VTS programmes could be further involved in undergraduate teaching through affiliation with an academic department.
Conclusions
GP registrars in the London Deanery are keen to teach medical students, but currently their experiences are haphazard and lack standardization. Although nearly two thirds have had some teaching involvement during their registrar year, for the most part this was ‘ad hoc‘ teaching in surgery with no preparation, training or supervision. GP registrars have raised concerns about lack of opportunity for teaching, lack of adequate time to dedicate to teaching during the registrar year and lack of experience in this area. An increasing proportion of undergraduate education is taking place in primary care which has resulted in increasing involvement of GP registrars and newly qualified GPs in teaching. This further emphasizes the value of obtaining teaching experience at an early stage of training.
This UK-based evaluation has highlighted a number of issues that need further exploration. In addition, the lack of UK based research in this area suggests that a UK wide study investigating the experiences and views of both GP registrars and GP trainers would be warranted. It would be beneficial to do some preliminary qualitative work in the form of focus groups or semistructured interviews to develop the questionnaire for wider dissemination.
Footnotes
Acknowledgements
We would like to thank Dr Paul Booton, Dr Graham Easton, Dr Anuradha Arasu and Professor Azeem Majeed for their assistance and advice, the London Deanery VTS programme administrators for disseminating the questionnaire and the GP registrars who took the time to respond.
Appendix
GPR experiences of medical student teaching questionnaire
