Abstract

DECLARATIONS
None declared
Shanghai Committee of Science and Technology, China (grant no. 09140902300)
Written consent to publication was obtained from the patient or next of kin
BS
All authors contributed equally
John Ajo and Gareth Morris-Stiff
We report a case of a 64-year-old man who presented with liquefying panniculitis associated with intraductal papillary mucinous neoplasm (IPMN) after the Whipple operation.
Case report
A 64-year-old man presented with a weight loss of 10 kg over 1 year and insomnia. CT scan revealed an approximate 3.0 cm homogeneous low-density mass in the head of pancreas.
Tumor markers including CEA, CA125, AFP and CA199 were not elevated. The patient's serum levels of amylase, lipase and calcium were normal. The patient received the pancreatoduodenectomy on 3 March 2010 and the postoperative pathology gave a definite diagnosis of IPMN of the pancreas (Figure 1).
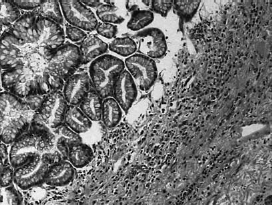
The photomicrograph of a resected specimen showing dilation of the pancreatic duct and ductal epithelial papillary hyperplasia, without obvious atypical and invasive growth(H&E, x100)
0.1 mg of octreotide injected subcutaneously every 8 h was postoperatively administered to suppress pancreatic secretion and decrease the risk of pancreatic fistula. On postoperative day 2, on the right lower limb skin a localized erythema appeared which slowly became larger, but the subcutaneous lesion did not bulge onto the surface of the skin. Subsequently the localized red-brown erythema was present over the right upper leg and knee joint. On postoperative day 5, the examination showed multiple subcutaneous inflammatory nodules on the legs and the buttock. (Figure 2).
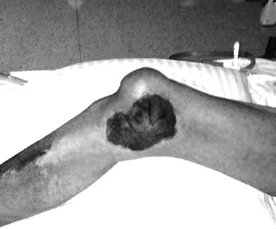
The photograph showing a large area of the skin lesions on the right lower limber leg and knee joint, respectively
Some of the larger lesions were necrotic and exuded a viscous fatty material, accompanied by general malaise. On postoperative day 7, we invited the dermatologist to examine the patient and made a diagnosis of liquefying panniculitis.
According to the report from the former literature, the octreotide was effective to liquefying panniculitis.1,2 We increased octreotide intravenous infusion to 0.6 mg every day and simultaneously used the Medrol (glucocorticoid, 20 mg/24h), 2 Ulinastatin (protease inhibitors) and antibiotics. No new nodules appeared and the original nodules did not change. However, the patient appeared anastomotic leakages and the wound grew worse. Drainage pipes discharged some yellow oily mucus substance. The patient had to receive the second operation on 1 April 2010. Introperatively, we found the pelvic cavity filled with brown oily necrotic liquids of about 50 mL. The postoperative pathology showed the necrosis of omental fat tissue. Unfortunately, several days later, new erythemas spread and scattered over his right thigh and right hand wrist. The former nodules grew larger again. The patient died of multiple organ failure on 27 April 2010.
Discussion
Panniculitis has rarely been reported in the world since the first report of Weber in 1935.1–6 Most of them were associated with pancreatitis or pancreatic carcinomas and had poor prognosis.1––5 In 2006, Gahr et al presented the first case of intraductal papillary mucinous adenoma of the pancreas associated with lobular panniculitis. 7 Hereon, we presented a case of liquefying panniculitis associated with IPMN. Liquefying panniculitis (Rothman's panniculitis) is a special type of nodular panniculitis (Weber-Christian disease). 6 In the past 20 years, one case of liquefying panniculitis has been reported in China. 2 Compared with domestic cases, there are more foreign cases reported. Most of them associated with pancreatic diseases have poor prognosis. In our case, the retinal tissue is involved 8 and anastomotic leakages appear which lead to a fatal outcome. The pathogenesis of pancreatic panniculitis is still unknown. The pancreatic enzymes, such as trypsin, may increase the permeability of the microcirculation and are involved in the process of fat degradation, which produces more free fatty acids combining with calcium to form soap. 5 However, cases of fat necrosis with normal serum lipase levels have also been described. 6 These reports suggest that there must be some other factors which allow the pancreatic enzymes to escape from the circulation and act on the subcutaneous fat. Deficiency of the alpha-1-antitrypsin (AAT) was also mentioned as a cause of pancreatic panniculitis. 9 According to the literature, octreotide and methylprednisolone can only slow down the progress of the disease.1,2 The patient's only preoperative symptom is the insomnia which has developed on him for many years, 10 so the study on whether the insomnia is associated with liquefying panniculitis becomes crucial, which may offer evidence for the early diagnosis of the panniculitis. In this case, skin lesions appeared postoperative and the operation may also be a predisposing risky factor for liquefying panniculitis and the exact mechanism needs to be further explored.
Footnotes
Acknowledgements
The authors thank Xiao-chun Wang for the pathological pictures and Wang Hui for his help
