Abstract

DECLARATIONS
None declared
None
Written informed consent was obtained from the patient or next of kin
ZC
ZC was involved in conception, drafting the article, and critical revision of the article. HJ critically reviewed the article
Tricuspid regurgitation is a common abnormality, which is often only diagnosed on echocardiography and not on clinical examination. This case report describes the rare presentation of eyeball pulsation seen in a patient with tricuspid regurgitation, presenting with severe congestive cardiac failure. The eyeball pulsation diminished after treatment with diuretics, synchronously with a lowered jugular venous pressure. Given the proposed mechanism behind eyeball pulsation, this sign is likely to have high specificity for tricuspid regurgitation and clinical progression in fluid overload. We propose that clinicians should routinely or at least be alert to looking for eyeball pulsation in the clinical examination.
Introduction
A range of clinical signs including pulsatile hepatomegaly, Rivero-Carvallo sign, and distended venous pressure are specific to tricuspid regurgitation. 1 Tricuspid regurgitation is, in turn, related to right heart failure. We describe the case of a patient presenting with severe congestive cardiac failure (New York Heart Association Class IV) 2 associated with tricuspid regurgitation, and eyeball pulsations as a result of markedly elevated venous pressure. Eyeball pulsation is not well described in tricuspid regurgitation. We discuss the need to look for eyeball pulsation in the bedside clinical examination and its significance in offering clues to a possible diagnosis.
Case report
A 74-year-old lady presented to our Medical Assessment Unit with two weeks’ history of increasing orthopnoea, ankle swelling and abdominal distension. Past medical history included ischaemic heart disease and atrial fibrillation. She also had a history of normocytic normochromic anaemia of unknown cause. Her regular medications included aspirin 75 mg (once daily); simvastatin 40 mg (once per night); Sotalol 160 mg (once daily); doxazosin 4 mg (once daily); and lisinopril 20 mg (once daily).
On examination, her pulse was 80 per minute, irregularly irregular and blood pressure was 180/80 mmHg. Normal heart sounds were heard throughout the praecordium. The jugular venous pressure 0VP) was grossly elevated up to the ear-lobes causing them to pulsate with an indiscernible waveform, even with the patient sitting fully upright. The external jugular veins were filled, consistent with increased venous pressure. There was pitting ankle and sacral oedema. Diffuse crackles were heard throughout both lungs. There was gross, tense ascites, but no signs of chronic liver disease. Neurological examination was normal. On fundoscopy the optic discs appeared normal with characteristic venous pulsation.
Of note, there was bilateral forward systolic eyeball displacement of up to 5 mm at all angles of incline of the patient when viewed from the side (Figure 1). There was no visual disturbance associated with the pulsation. The patient was asymptomatic and was not aware of any orbital movement.
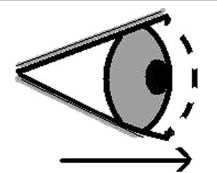
Schematic representation of eyeball pulsation from a sideways view. The dotted line and arrow show the forward propulsion of the eyeball
The admission electrocardiogram showed atrial fibrillation. A chest X-ray showed cardiomegaly, alveolar oedema and bilateral pleural effusions. Admission bloods revealed a normocytic anaemia with low white cell count but a normal platelet count. Urea and electrolytes, liver function tests and bone profile were unremarkable.
The clinical impression at this stage was that of congestive cardiac failure with severe venous hypertension. The increasing ascites and generalized pitting oedema was likely to be secondary to congestive cardiac failure, on a background of ischaemic heart disease.
Clinical progression
The patient was given 80 mg furosemide intravenously, with a daily per oral regimen of 25 mg spironolactone once per day and 80 mg furosemide twice daily.
A subsequent echocardiogram revealed severe tricuspid regurgitation. After two days of diuretic treatment, the patient improved clinically. The JVP descended in height and revealed visible prominent v-waves, indicative of tricuspid regurgitation. The eyeball pulsation had resolved. The previous severity of the congestive cardiac failure on presentation was such that v-waves were not detected clinically.
Discussion
A variety of specific signs are often present in tricuspid regurgitation. 1 A pansystolic murmur can be heard in a third of patients, and two-thirds of patients have pulsatile hepatomegaly. 3 In our case, there were no well-known signs to suggest tricuspid regurgitation on admission, although the prominent v-waves and echocardiogram confirmed this diagnosis later on. Orbital pulsation is also not mentioned in the common textbooks as a sign in tricuspid regurgitation. We discuss the importance of these pulsations in aiding the clinician in the diagnostic process.
On review of the literature, eyeball pulsation in tricuspid regurgitation has been reported only in five cases in two reports dating from 1970 and 1985.1,4 In these cases, the diagnosis of tricuspid regurgitation was not confirmed by echocardiography, as in our case. Furthermore, well-known and unequivocal signs were present in previous cases such as a characteristic pansystolic murmur to identify tricuspid regurgitation. In our case, eyeball pulsation is the only clinical finding present at the time of presentation to suggest a diagnosis of tricuspid regurgitation.
In this case, the symmetrical forward displacement of the eyeballs was synchronous with earlobe thrusting, which moved with the raised venous pressure in the internal jugular vein. Examination of the JVP is an essential part of the bedside cardiovascular assessment. The distended JVP has been shown to be a sensitive and specific sign, indicating raised left and right ventricular pressures in patients with congestive cardiac failure. 5 An elevated JVP acts as an independent indicator for adverse progression of cardiac failure.5,6 The eyeball propulsions were best noted from the side with the patient looking in the forward direction and visible at every angle of inclination. We were unable to discern the jugular venous waveform because of the JVP height. Therefore, in cases of severe congestive cardiac failure, it may be favourable to look for bilateral pulsations of the eyeballs when the waveform of the elevated JVP is not so easily discerned. This sign may be used to alert clinicians to a diagnosis of tricuspid regurgitation.
The mechanism for systolic eyeball pulsation in tricuspid regurgitation is likely to reflect similar pathways behind pulsation of the liver and previously described arm vein pulsation 4 and varicose vein pulsation. 7 A fistula between the carotid artery and the cavernous sinus may also produce eyeball pulsation but is usually unilateral with local symptoms of pain and progressive visual loss.8,9 In our case, the eyeball pulsation was asymptomatic. The eyeball pulsation in tricuspid regurgitation is a result of transmission of raised right ventricle pressures to the cavernous sinus into the internal jugular vein during right ventricular systole.
Such bilateral eyeball pulsations may be an indication to arrange for an echocardiogram to detect the underlying cardiac pathology. As seen here, eyeball pulsation correlates to fluid overload and changes with the patient's clinical progression, given that it disappeared with diuretic treatment. Therefore, eyeball pulsation may be a useful, although rare, marker of fluid overload in tricuspid regurgitation, helpful in both the diagnosis and monitoring of treatment.
The presence of eyeball pulsation only occurs in raised right ventricular pressures coexisting with tricuspid regurgitation. Eyeball pulsation is not well recognized; thus, inspection of the orbits laterally is seldom carried out routinely. Furthermore, clinicians now have the ready availability of an echocardiogram diagnosis. These factors may all account for the phenomenon being noted infrequently.
Conclusion
We propose that eyeball pulsation is a useful, albeit rare, sign in diagnosing the relatively common tricuspid regurgitation on a background of congestive cardiac failure. In cases such as the one we presented, where there are no other signs to suggest a diagnosis of tricuspid regurgitation, the clinician may be aided by looking out for eyeball pulsation. The presence of eyeball pulsation may serve as a useful distinguishing feature in patients presenting with severe fluid overload, indicating right ventricular high pressures and tricuspid regurgitation.
