Abstract
Primary signet ring cell carcinoma of the appendix is a very rare neoplasm that usually presents with signs and symptoms of acute appendicitis and in particular with a right lower abdominal pain. Preoperative imaging detection of appendiceal adenocarcinoma has an important value because it may result in an appropriate surgical procedure. We report a rare case of primary signet ring cell carcinoma of the vermiform appendix in an 80-year-old man who was misdiagnosed on computed tomography (CT) scan as acute appendicitis.
Primary adenocarcinoma of the vermiform appendix is a rare neoplasm of the gastrointestinal tract that occurs in approximately 0.5% of appendectomies and generally affects adults (1) Moreover, a primary signet ring cell carcinoma of the appendix is an exceedingly rare entity, comprising only 4% of all appendiceal neoplasms (2). These tumors usually present with signs and symptoms of acute appendicitis and in particular with a right lower abdominal pain, which may lead to cross-sectional imaging. When found in asymptomatic patients, these neoplasms are often found incidentally on imaging for other purposes. Preoperative detection of appendiceal adenocarcinoma has an important value because it may result in an appropriate surgical procedure, leading to right hemicolectomy instead of appendectomy (1).
Signet ring cell carcinoma is considered as an aggressive type of cancer. In 93% of cases, metastases to adjacent organs, lymph nodes, or to the peritoneal cavity are often present at the time of diagnosis (3). In this report, we describe a rare case of primary signet ring cell carcinoma of the vermiform appendix in an 80-year-old man who was misdiagnosed on computed tomography (CT) scan as acute appendicitis.
Case report
An 80-year-old man presented to the Emergency Department in May 2009 with persistent right lower quadrant abdominal pain. Baseline blood tests showed neutrophilic leukocytosis. Preoperative contrast-enhanced CT scan (Figs. 1 and 2) showed a wide and severe thickening of the appendiceal walls with extensive soft-tissue stranding and inflammation of the peri-appendicular fat. Loculated fluid and lymphadenopathy adjacent to the appendix were also detected on the CT examination.
Axial post-contrast CT image showed an enlarged appendix, with severe peri-appendiceal and peri-cecal inflammation and associated fat stranding (white arrows)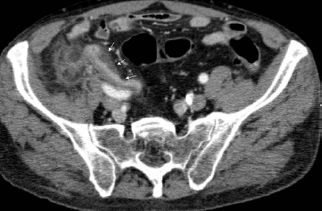
Coronal CT multiplanar reconstruction confirms the presence of an enlarged appendix with severe peri-appendiceal and peri-cecal inflammation and fat stranding and associated intra-mural air (white arrows)
The patient underwent an appendectomy. At laparotomy the appendix appeared severely inflamed with an associated abscess at its apex. The inflammatory process also involved the first part of the cecum, making it difficult for the identification of the ceco-appendiceal junction. The final histological diagnosis was consistent with well-differentiated infiltrating adenocarcinoma of the appendix with mucinous and “signet ring cells” appearance, with signs of infiltration of peri-appendicular fat and a peritoneal abscess (Fig. 3).
Low-power view of mucinous and “signet ring cells” adenocarcinoma in the wall of the appendix with lakes of mucin. Normal glands and lymphoid tissue are present (arrow) (HE, x 40). Inset: High-power view of the signet ring cells that penetrated the peri-appendiceal fatty tissue. (HE, x400)
The patient underwent colonoscopy for the evaluation of synchronous disease, which was negative. Neoplastic markers were negative as well.
The patient subsequently underwent right hemicolectomy and no residual carcinoma with negative lymph nodes was found. The patient was discharged from the hospital 10 days later and had an uneventful postoperative course.
Discussion
Only few cases of appendiceal adenocarcinomas have been described in the literature showing different CT imaging findings, depending on the histological type. Mucinous epithelial neoplasms appear on CT like a mucocele, with a grossly distended appendix. In less than 50% of cases, curvilinear mural calcification might be present, which are highly suggestive of the diagnosis and also visible on plain abdominal film (4). Other CT signs are soft-tissue thickening, irregularity of the mucocele wall, and presence of lymph nodes in the surrounding fat (5). Non-mucinous or colonic-type epithelial neoplasms rarely occur in the appendix and appear at CT like a focal soft-tissue mass that involves the appendix without mucocele formation. Carcinoid tumors represent up to 80% of appendiceal neoplasms and are usually small, confined to the distal appendix and with a low complication rate. Because of the small size it is difficult to detect these lesions by CT examination. Globet cell carcinoid tumors are unusual and appear on CT imaging with an infiltrative pattern and diffuse mural thickening and a propensity to metastasize to the ovaries and peritoneum. Appendicular mucocele is rare and usually presenting as an irregular soft-tissue mass near the root of the mesentery. Non-Hodgkin's lymphoma might involve the appendix, which appears enlarged causing a diffuse mural thickening with dilation of the appendiceal lumen. Signet ring cell carcinoma is the rarest of the appendiceal cancers and, as the others, the clinical presentation is usually non-specific. The most common symptom of these tumors is a right lower quadrant abdominal pain indistinguishable from acute appendicitis. Therefore, it is invariably difficult to diagnose primary signet ring cell carcinoma of the appendix preoperatively. There are no specific CT findings useful to distinguish a signet ring cell carcinoma from other histological types, except from the spread to adjacent organs (76%) at presentation compared with mucinous (63%) and colonic type (37%) cancers (6). Because of the poor prognosis some authors consider these neoplasms separately from other appendiceal malignancies (7). Usually the diagnosis is not made until after histologic examination of a surgically removed inflamed appendix (8).
Preoperative diagnosis of an appendiceal neoplasm is important with regard to surgical planning in patients presenting with symptoms of acute appendicitis (9), but it is difficult due to the absence of specific imaging findings. As appendiceal adenocarcinomas can present with signs and symptoms of acute appendicitis, it may often be misdiagnosed (6). The presence of a non-homogeneous mass in the appendicular area with enhancing wall and stranding of peri-appendicular fat suggests the possibility of adenocarcinoma. These findings along with the presence of surrounding lymph nodes may be suggestive of a malignant lesion and should be carefully evaluated as an aid in the differential diagnosis with a non-neoplastic disease (4). Localized ascites is also frequently seen adjacent to the inflammatory lesions as are appendicoliths, intramural air, and focal cecal apical thickening; these findings are nearly 100% specific for acute appendicitis (7). In addition, patients with advanced age at presentation appear to be another indicator for the possibility of an underlying neoplasm (1). The treatment of appendiceal carcinoma is controversial. Some authors reports that appendectomy is a curative procedure for mucosal lesions and recommends right hemicolectomy only for advanced stages of appendiceal carcinomas (9). Secondary right hemicolectomy with lymph node dissection should be considered in patients presenting with undifferentiated adenocarcinoma, in those with lymphatic invasion and with significant invasion of the sub-mucosa (10).
In conclusion, patients with a non-specific clinical presentation and right lower quadrant abdominal pain, should be always carefully examined to correctly differentiate between acute appendicitis and appendiceal carcinoma, because subsequently planning, is crucial for the most appropriate surgical treatment.
