Abstract
Internal jugular vein (IJV) phlebectasia is a rare, benign venous anomaly characterized by fusiform dilatation of the vessel without tortuosity. It is more frequently reported in children, with adult-onset presentations being uncommon. The condition is often asymptomatic, manifesting as a soft, compressible swelling in the neck that becomes prominent during activities increasing intrathoracic pressure. A case is presented of a 41-year-old man who had an enlarged right-sided neck swelling for 6 months, which became more pronounced during speaking and the Valsalva maneuver. Clinical evaluation and high-resolution ultrasonography with color Doppler were used to evaluate the patient. Sonography revealed fusiform dilatation of the right IJV along its course to the subclavian vein, with a maximal diameter of 15 mm at rest and further dilatation during the Valsalva maneuver. No intraluminal filling defect or cervical lymphadenopathy was observed. Based on clinical and imaging findings, a diagnosis of right IJV phlebectasia was established. Since the patient had no symptoms or problems, the patient was managed conservatively with advice for periodic follow-up. In adults with intermittent neck swelling, this simple vascular anomaly should be considered as a possible causative factor, especially in regions with limited reporting.
Internal jugular vein (IJV) phlebectasia is a rare but harmless vascular condition in which the IJV becomes abnormally widened in a smooth, spindle-like (fusiform) shape, without twisting or the structural changes seen in a true aneurysms. 1 The condition is generally unilateral, with a strong predilection for the right side attributed to anatomical and hemodynamic differences, including the shorter and more direct course of the right brachiocephalic vein, into the superior vena cava and a larger right IJV bulb.2,3
A 2019 systematic review article documented approximately 247 cases of IJV phlebectasia that had been reported in the literature, both in pediatric and adult patient populations. 4 While the condition has been documented across multiple regions, reports from the Middle East remain rare or underreported.
Clinically, IJV phlebectasia presents as a soft, compressible, and non-tender swelling in the lateral neck. 5 It is more noticeable during any activity that puts pressure on the chest, like coughing or speaking. It becomes less obvious or disappears completely when the patient is relaxed and resting. 6 Although it is a benign and often asymptomatic condition, its dynamic presentation can mimic other cervical swellings, including laryngocele, branchial cyst, cystic hygroma, lymphadenopathy, or venous aneurysm, making accurate diagnosis crucial to avoid unnecessary invasive interventions. 7
Sonography with color Doppler is considered the diagnostic imaging technique of choice. It allows real-time visualization of venous dilatation, demonstrates dynamic changes during a Valsalva maneuver, and excludes intraluminal thrombus or extrinsic compression. 8 Other diagnostic imaging techniques, such as computed tomographic (CT) angiography or magnetic resonance (MR) venography, can be employed for further anatomical assessment, as indicated. 9 Standardized criteria for measuring the size of the IJV are important for accurate diagnosis and consistent comparisons across studies. In normal adults, the mean anteroposterior diameter of the IJV, at rest, is approximately 4 to 7 mm, with the diameter increasing to about 10 to 12 mm, during a Valsalva maneuver. 10
The patient case presented is of a 41-year-old Yemeni male presenting with right IJV phlebectasia, which was confirmed by sonographic and Doppler examination. This case report emphasizes the importance of recognizing this rare entity in adults, particularly in underreported regions, to prevent misdiagnosis and unnecessary surgical exploration.
Case Report
A 41-year-old Yemeni male presented to an outpatient clinic with a complaint of a swelling in the right side of his neck, over the past 6 months. The swelling was first noticed during prolonged speaking and gradually increased in size over time. The patient reported that the swelling became more prominent during talking or straining and reduced at rest. There was no history of pain, tenderness, fever, weight loss, hoarseness of voice, dysphagia, or respiratory distress. The patient’s past medical, surgical, and family history were unremarkable. There was no history of neck trauma, surgery, or exposure to chronic infections. He denied smoking, alcohol use, or any occupational exposure that might predispose to neck masses.
On examination, a soft tissue swelling was noted on the neck, located anterior to the sternocleidomastoid muscle. The swelling was elongated, non-pulsatile, and non-tender. It was compressible upon palpation and diminished with gentle pressure. The swelling became more prominent during speech and the Valsalva maneuver. There was no overlying skin change, bruit, or thrill. No cervical lymphadenopathy was manually appreciated.
A sonographic examination was performed on the neck with the patient in a supine position and slight head rotation to the contralateral side. The examination was conducted using an Acuson (Siemens, Munich, Germany) ultrasound equipment system with a high-frequency linear transducer, operating at 7 MHz. Dynamic evaluation was performed both at rest and during the Valsalva maneuver, to assess changes in the IJV diameter. Care was taken to avoid excessive transducer pressure that could artificially compress the vein. Imaging revealed a fusiform dilatation of the right IJV along its course, to its termination at the right subclavian vein, with a maximal diameter of 15 mm at rest. The dilatation increased when the patient did the Valsalva maneuver. No intraluminal filling defect or evidence of thrombus was detected. Both subclavian veins were normal in caliber and compressibility, and there was no sonographic evidence of enlarged cervical lymph nodes (See Figure 1). A contrast-enhanced CT of the neck was subsequently performed using a 64-slice Somatom (Siemens, Munich, Germany) unit, which demonstrated aneurysmal dilatation of the right internal jugular vein with a maximal diameter of 26 mm, thereby confirming the sonographic diagnosis of phlebectasia (See Figure 2). Based on these findings, a diagnosis of right IJV phlebectasia was established, and given the benign and asymptomatic nature of the lesion, the patient was counseled for conservative management with periodic surveillance.
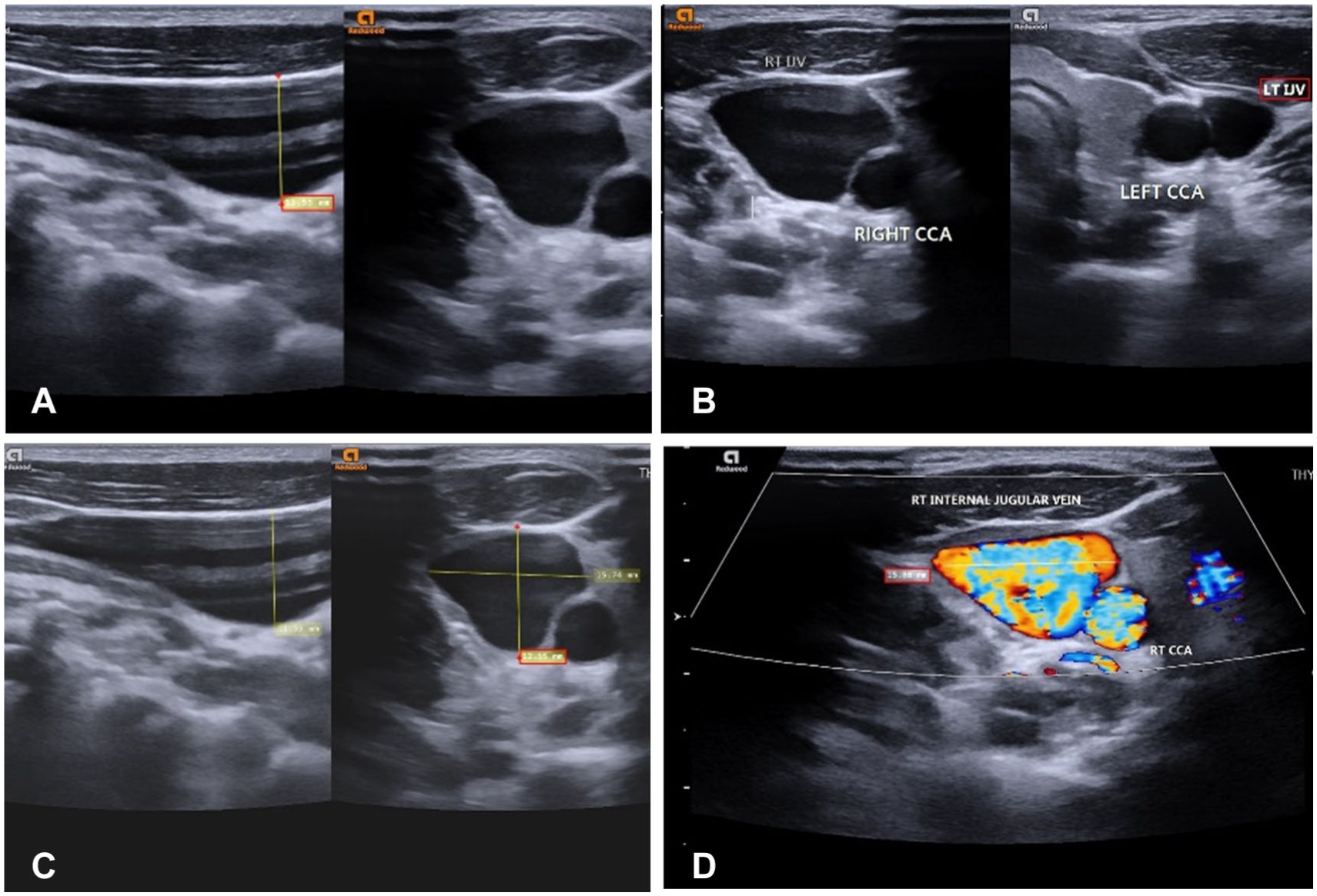
(A) Dual longitudinal and transverse gray-scale sonographic images of the right internal jugular vein (IJV) are captured at rest. (B) Dual longitudinal (11.55 mm) and transverse (12.55 mm) diameters were taken of the right IJV, at rest. These measurements increased to 15 mm, during the Valsalva maneuver. (C) Dual sonograms provide a comparison of right and left IJV diameters, showing enlargement of the right IJV consistent with phlebectasia. (D) A transverse color Doppler image is captured of the right IJV, which demonstrated patent flow.
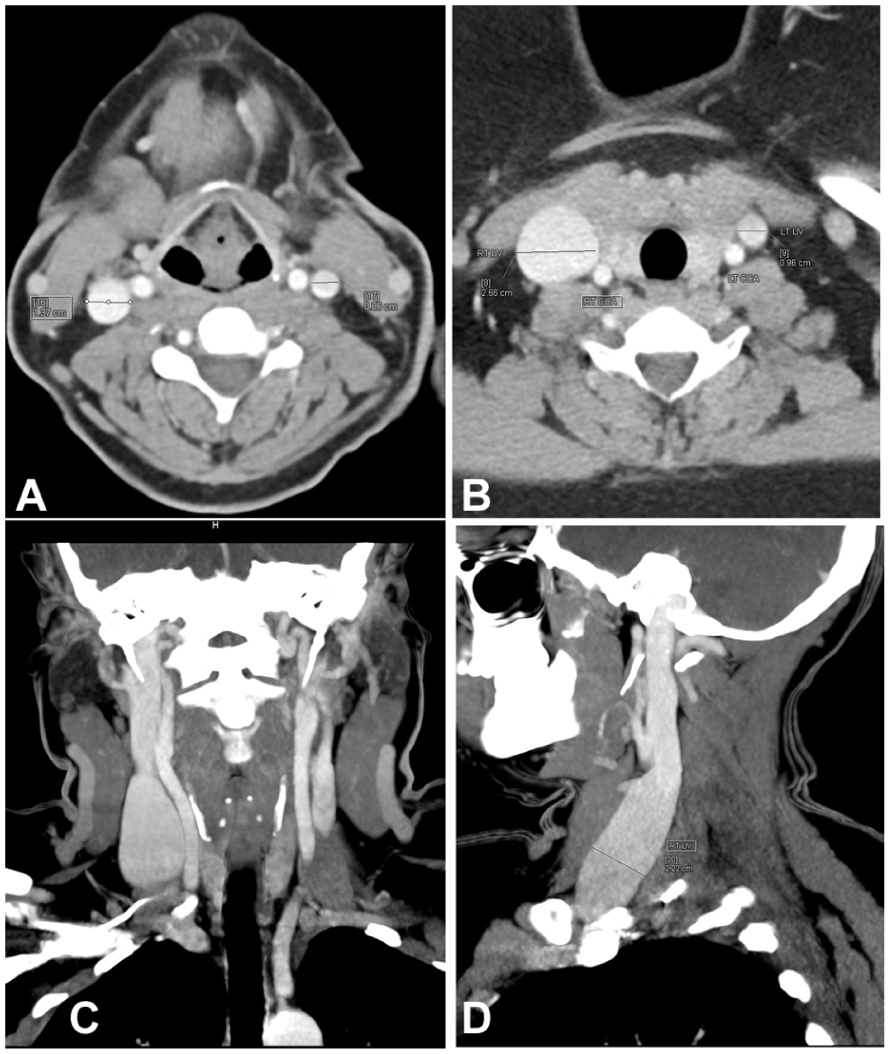
A series of computed tomographic (CT) contrast-enhanced images of the neck demonstrated a fusiform aneurysmal dilatation of the right internal jugular vein (IJV). (A, B) Axial CT sections demonstrated the dilated right IJV, with a maximum diameter of 26 mm, confirming phlebectasia. (C) A CT coronal view reformatted image shows the full extent of the dilated right IJV, from the jugular bulb to its junction with the subclavian vein. (D) A CT sagittal view reformatted image depicts smooth, fusiform dilatation without intraluminal thrombus or external compression, consistent with right IJV phlebectasia.
Discussion
This case report described a 41-year-old Yemeni male with right IJV phlebectasia. The patient’s presentation was a gradually enlarging, soft, compressible neck swelling becoming more prominent during speaking and the Valsalva maneuver. This was consistent with previous descriptions of this rare vascular anomaly. The diagnosis was established noninvasively, and the patient was managed conservatively given the absence of symptoms and complications. Based on a limited review of the literature, this may be the first reported case of adult IJV phlebectasia from Yemen, adding limited evidence to the available literature from the Middle East.
Internal jugular vein phlebectasia is a rare vascular abnormality. It can occur in both children and adults, though pediatric cases are more frequently documented. 11 The condition is often unilateral, with the right side affected in up to 70% of cases attributed to the direct drainage of the right brachiocephalic vein into the superior vena cava and the larger caliber of the right IJV bulb. 12 There is no clear sex predilection in adults, though some pediatric studies suggest a slight male predominance. As stated, reports from the Middle East are sparse and only isolated adult cases from Saudi Arabia and neighboring countries have been published. To date, only one case has been reported of a 61-year-old woman, living in Saudi Arabia, with internal jugular phlebectasia. The patient presented with neck swelling that had been noticed for 4 years, initially enlarging before reaching a stable size. 13
Clinically, the most common presentation is a soft, fusiform neck swelling that becomes prominent during straining, coughing, or the Valsalva maneuver. 14 This finding is usually asymptomatic and often brought to medical attention due to cosmetic concerns, especially in children. Infrequently, patients may complain of mild discomfort or pain in the neck, while rare manifestations include hoarseness of voice, dysphagia, or respiratory difficulty due to compression of adjacent structures. Even less commonly, complications such as intraluminal thrombosis, hemorrhage following trauma, or airway compromise have been reported. 15
Internal jugular vein phlebectasia is generally benign but can lead to rare complications such as Horner’s syndrome from nerve compression, thrombosis, congestive heart failure, and life-threatening hemorrhage due to trauma-induced vessel rupture. 16 Spontaneous rupture is not reported, but trauma remains a serious risk. Some cases suggest possible intracranial extension and an association with Menkes disease, which may cause neurological issues. 17 Increased intracranial pressure is theoretically possible in severe cases but is very rare. The exact etiology of IJV phlebectasia remains unclear. Proposed mechanisms include congenital weakness of the venous wall, absence or incompetence of venous valves, and elevated intrathoracic pressure causing focal venous dilatation.14,18 Some authors have suggested that anatomical variations, particularly on the right side, predispose individuals to this condition.19,20 Secondary causes such as thoracic outlet syndrome, mediastinal masses, or increased central venous pressure should be excluded through clinical and imaging evaluation. 21 Histopathological studies have shown thinning of the elastic and muscular layers of the venous wall in some cases, supporting a congenital structural defect hypothesis. 22
Sonography with color Doppler is the preferred diagnostic imaging tool for IJV phlebectasia, due to its noninvasive nature, availability, and dynamic imaging capabilities. It can confirm venous dilatation, demonstrate changes in diameter during Valsalva, and exclude intraluminal thrombus. Computed tomographic angiography and MR venography can be used for further anatomical delineation, particularly when surgical intervention is considered or when secondary causes are suspected. In the current study patient, sonography alone was sufficient to establish the diagnosis, as there were no signs of complications or underlying pathology. While sonography can confirm venous dilatation and valve function effectively, CT and MR provide complementary high-resolution visualization of deeper structures and complex anatomy that sonography may not fully capture, thereby strengthening diagnostic confidence in such atypical or complicated cases.
Management of IJV phlebectasia depends on symptoms, cosmetic concerns, and the presence of complications. In asymptomatic cases, conservative management with observation as the standard approach, as the condition is benign and the risk of complications is low. Surgical intervention (such as excision of the dilated segment or ligation of the IJV) is generally reserved for patients with significant cosmetic deformity, thrombus formation, or rare compressive symptoms. 23 Prognosis is excellent, with most conservatively managed cases showing no progression or adverse outcomes during long-term surveillance.24,25
Conclusion
Internal jugular vein phlebectasia is a rare, benign vascular anomaly that should be considered in the differential diagnosis of dynamic neck swellings, particularly those that enlarge during Valsalva. Although most described in children, it can also present in adults, as in the present patient case. Sonography with color Doppler remains the diagnostic modality of choice, allowing confirmation of venous origin, assessment of dynamic changes, and exclusion of thrombus or extrinsic compression. Given its characteristically asymptomatic nature and favorable long-term outlook, a conservative approach involving periodic observation is the recommended management strategy for most patients; surgical intervention is indicated only for significant cosmetic deformity or the development of complications. The significance of this patient case lies in its status as the first reported instance of right IJV phlebectasia in a Yemeni adult. This contribution to the limited regional literature underscores the necessity for clinician familiarity with this entity to preclude unnecessary and invasive diagnostic interventions.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Verbal informed consent was obtained from the subject before the release of the report for review.
Ethics Approval
Ethical approval was not sought for the present study because all patient information was de-identified.
