Abstract
Isolated fallopian tube torsion (IFTT) is clinically rare, particularly in adolescents. Misdiagnosis or a missed diagnosis can lead to serious consequences. Early and thorough awareness of the risk factors and imaging features of IFTT is essential for an accurate diagnosis. The case report involves an 18-year-old girl who presented with the atypical symptom of dull pain in the right lower quadrant. The sonogram indicated that a right-lower-quadrant mass existed, with an uncertain relationship to the appendix. At gynecologic surgery, the diagnosis was confirmed as a hydrosalpinx torsion with seven twists, accompanied by an elongated fallopian tube. This case underscores the importance of recognizing classic sonographic signs and identifying torsion-related precipitating factors and risk factors, in the diagnosis of IFTT.
Isolated fallopian tube torsion (IFTT) is a rare abdominal clinical gynecological emergency, with a reported prevalence of one in 1.5 million.1,2 The main risk factors for its onset include endometriosis, pelvic surgery, inflammatory adhesions, hydrosalpinx, mesosalpinx cysts, and congenital developmental anomalies.2,3 For adolescent patients, preserving the adnexa and normal fertility through adnexal repositioning is a major concern. This means that establishing an accurate diagnosis in the early stages of torsion and ischemia is crucial.4,5 This case study provides the imaging data and treatment process of an 18-year-old girl, with hydrosalpinx and IFTT.
The release of this case was approved by the ethics committee of a tertiary-grade A hospital. All procedures and reporting were done in accordance with the 1964 Declaration of Helsinki and later amendments. 6
Case Report
An 18-year-old girl with a 3-day history of right lower abdominal pain reported for care. Her pain was intermittent and dull, without progression or migration. She was afebrile and had no chills, nausea, vomiting, or diarrhea, and no history of pelvic disease. Since the onset of illness, her mental status, appetite, sleep, and bowel and urinary habits had all remained normal. Her menstrual cycles were irregular, with normal menstrual flow and no reported dysmenorrhea. The last menstrual period occurred 26 days before the date of consultation, with no sexual or surgical history.
The patient’s vital signs were normal. Abdominal palpation revealed a soft abdomen with tenderness in the right lower quadrant, accompanied by rebound tenderness. There was no tenderness in the left lower quadrant, but mild rebound tenderness was noted. A gynecologic examination showed normal external genitalia. No internal examination was performed due to the lack of sexual history. Digital rectal examination revealed a normal-sized uterus with tenderness. A mass the size of an egg was palpable in the right adnexal region, with significant tenderness and poor mobility. No mass was palpable in the left adnexal region, but tenderness was present. Laboratory tests showed a hypersensitive C-reactive protein level of 7.5 mg/L (i.e., normal range: 1.0–3.0 mg/L). The patient’s complete blood count, coagulation function, and urinalysis were all within normal limits.
A transabdominal gynecologic sonogram revealed a 5.4 cm × 3.5 cm complex, mixed-echogenicity mass in the right lower quadrant. The lesion contained both tubular and anechoic cystic structures, with “cord-like” and “whirlpool” patterns observed at the affected site. Color Doppler demonstrated punctate blood flow within the whirlpool-like structure and the adjacent ovarian structures are clearly visualized, appearing morphologically normal. There were no obvious abnormalities sonographically detected in the left uterus or ovary. The sonographer reported a cystic lesion of the right adnexa with torsion (See Figure 1). The sonogram indicated the lesion was located in the right lower quadrant, but the appendix could not be visualized. For added caution, a computed tomogram (CT) was completed and demonstrated a complex mass in the right lower quadrant. The mass was lying adjacent but separate from a structurally intact and well-defined appendix (See Figure 2). These diagnostic findings suggested an adnexal origin of the lesion.
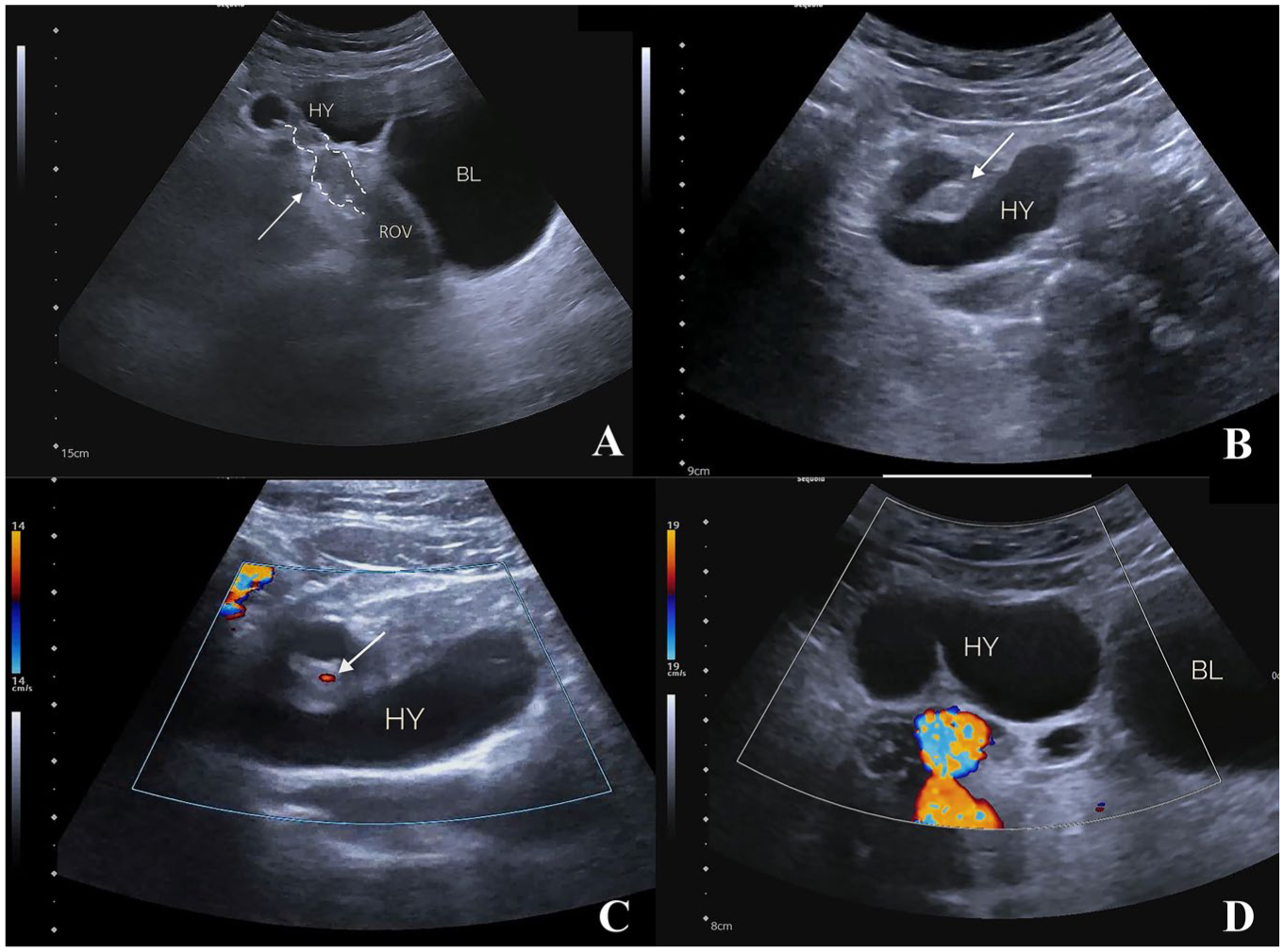
A series of sonographic images demonstrated a suspected isolated fallopian tube torsion (IFTT). (A) This sonogram shows the torsed and thickened fallopian tube forming a cord-like, isoechoic structure (arrow), continuous at both ends with the ipsilateral ovary (ROV) and the cystic fluid collection (HY). (B) The sonogram demonstrates the “whirlpool sign” (arrow), surrounded by a dilated cystic structure (HY). (C) Doppler reveals punctate blood flow within the whirlpool-like structure (arrow), whereas no flow is detected in the surrounding cystic structure (HY). (D) Doppler displays a “lotus-root segment” cystic structure (HY).
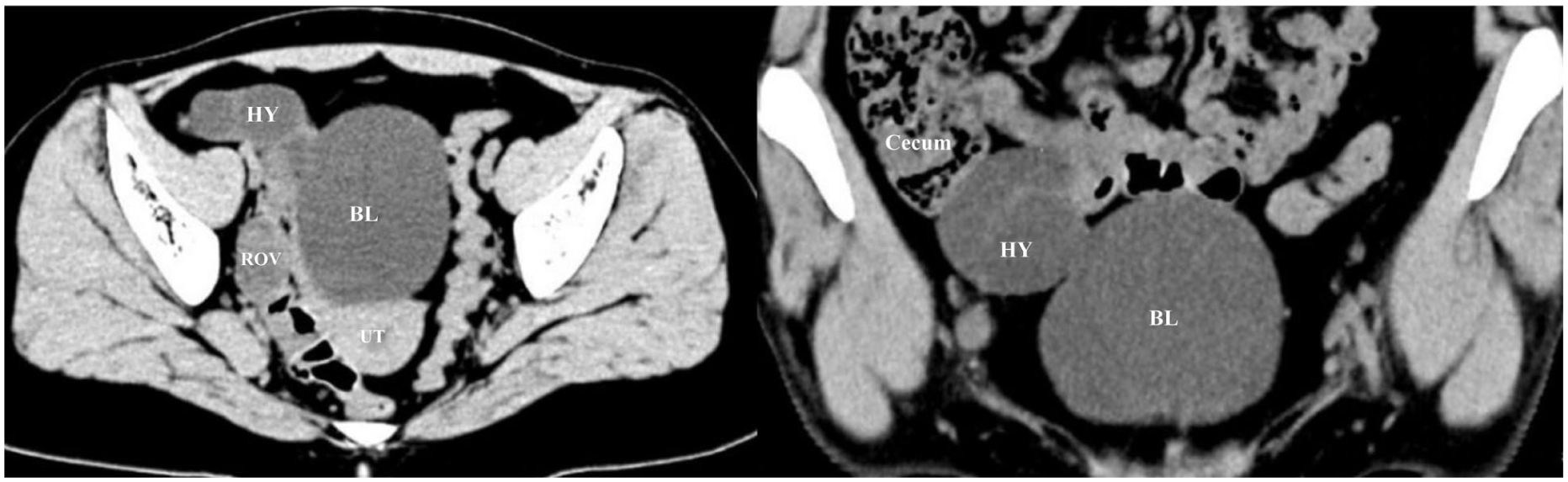
A set of computed tomographic images provided additional evidence of an isolated fallopian tube torsion (IFTT).
The patient’s pain involved persistent and progressively worsened without relief, which prompted an emergency diagnostic laparoscopy, in the department of obstetrics and gynecology. The uterus appeared normal in size, the right fallopian tube was markedly distended by a hydrosalpinx, dusky-blue and purple, measuring approximately 8.0 cm × 5.0 cm. It appeared to be twisted seven times (See Figure 3). The right tube itself was about 20 cm long, while both ovaries appeared macroscopically normal. Given evidence of ischemic necrosis, a right salpingectomy was performed. The postoperative histopathological examination results were consistent with the intraoperative diagnosis. The patient had an uneventful recovery and was discharged on the fourth postoperative day.
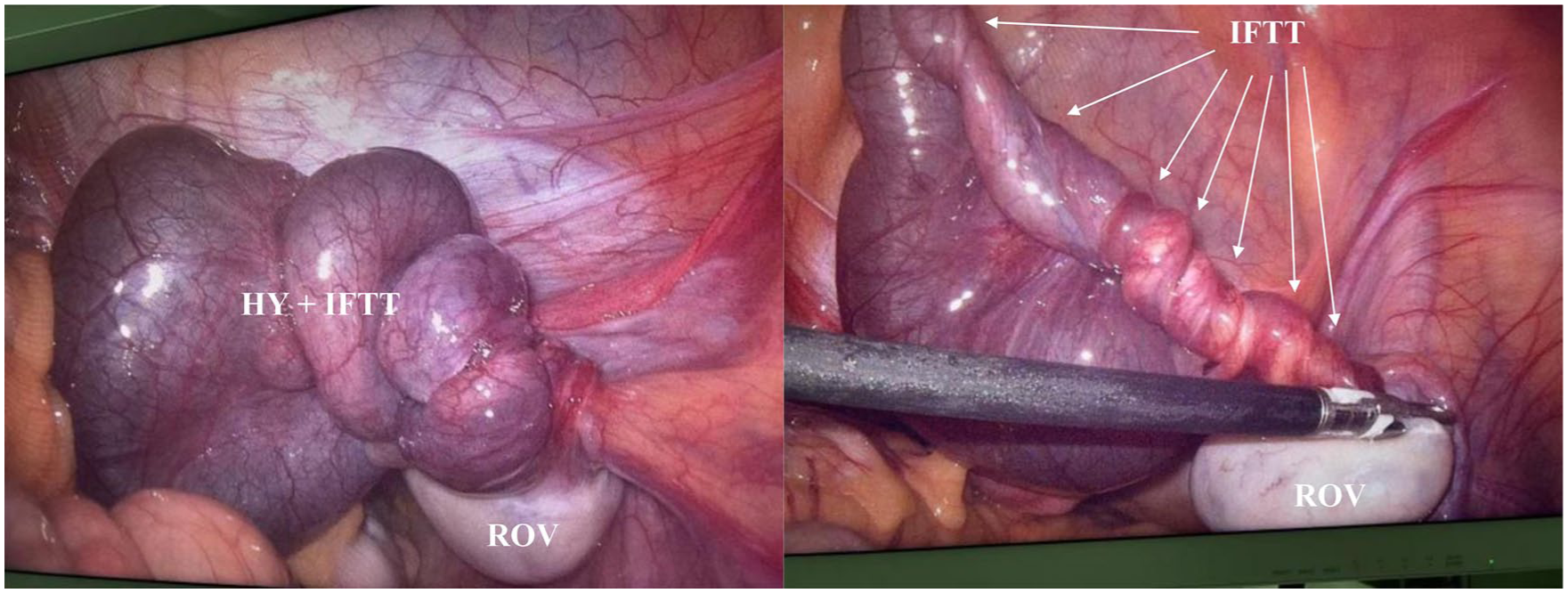
Images are provided of the intraoperative documentation of an isolated fallopian tube torsion (IFTT).
Discussion
Isolated fallopian tube torsion is rarely encountered in clinical practice, and timely diagnosis and treatment are crucial. Isolated fallopian tube torsion is characterized by rotation of the fallopian tube on its mesenteric axis, without concomitant ovarian involvement.1,2 After an IFTT occurs, venous and lymphatic drainage are first obstructed, leading to congestion, edema, and transudation of the distal fallopian tube. If the torsion persists, arterial inflow diminishes and eventually results in tubal necrosis and gangrene. The first 24 hours are regarded as the primary opportunity for salvaging the fallopian tube. 7
This patient had no history of surgery or related pelvic diseases. The clinical symptoms were atypical but exhibited the classic features of IFTT. Interference from bowel gas limited the sonographic visualization of the appendix. The dominant lesion being situated in the right lower quadrant, therefore, posed a diagnostic challenge. It is noteworthy that the case had an elongated fallopian tube, resulting in an altered position, compared with normal anatomy. This abnormal positional shift indirectly corroborates the presence of a congenital developmental anomaly, which can be an independent risk factor for IFTT.2,8 Another risk factor was a hydrosalpinx (See Figure 1A–1D). In this patient case, severe hydrosalpinx appeared on the sonogram as cystic and tubular anechoic structures, accompanied by the “waist sign” 9 (See Figure 1D). With seven complete torsions, the fallopian tube, in this case, readily displayed the characteristic sonographic patterns of a “cable sign” (See Figure 1A) and a “whirlpool sign” (See Figure 1B and 1C) produced by the twisting. 10 Intense physical activity is also regarded as an important risk for IFTT, 11 and the patient’s history of professional dancing may have influenced the development of IFTT.
Isolated fallopian tube torsion symptoms are usually nonspecific, and acute lower abdominal pain with nausea and vomiting is the most consistent presentation. 12 This pathology must be distinguished from acute appendicitis, in which migratory right-lower-quadrant pain is characteristic. Sonography is still the primary imaging technique, due to its convenience, nonionizing radiation, and Doppler, which allows real-time assessment of blood flow. An adnexal mass, or the “whirlpool sign” of a twisted tube may suggest IFTT, yet the accuracy of sonography is heavily dependent on the skill of the sonographer and is highly patient-dependent. The overall diagnostic accuracy of sonography to detect an adnexal torsion is 79%. 13 Computed tomography has low diagnostic sensitivity for detecting IFTT; however, it is superior in imaging the appendix and bowel, which makes it important in the overall diagnosis. The use of magnetic resonance imaging (MRI) is more expensive, although excellent for lesion characterization and is usually reserved for complex diagnostic cases (i.e., to determine malignancy). 14 Management of IFTT must be individualized, considering the patient’s age, fertility, clinical presentation, and medical history. 15 The longer the interval between symptom onset and operative intervention, the greater the likelihood of irreversible tubal damage. Therefore, emergency surgical exploration is recommended, as soon as IFTT is diagnosed or strongly suspected.
Conclusion
The diagnosis of IFTT is challenging. In an adolescent female presenting with lower abdominal pain, a detailed medical history and physical examination are essential. Sonography is often pivotal; an adnexal mass and the “whirlpool sign” are classic features of IFTT, while also recognizing risk factors such as hydrosalpinx, elongated fallopian tubes, and mesosalpingeal cysts. A definitive diagnosis still relies on surgical exploration and histopathological confirmation.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval for this study was obtained from the ethics committee of Tianyou Hospital Affiliated to Wuhan University of Science and Technology (Approval Number: LL2025-08-19-02).
Informed Consent
Verbal informed consent (verbal assent) was obtained from the subjects before the release of the report for review.
