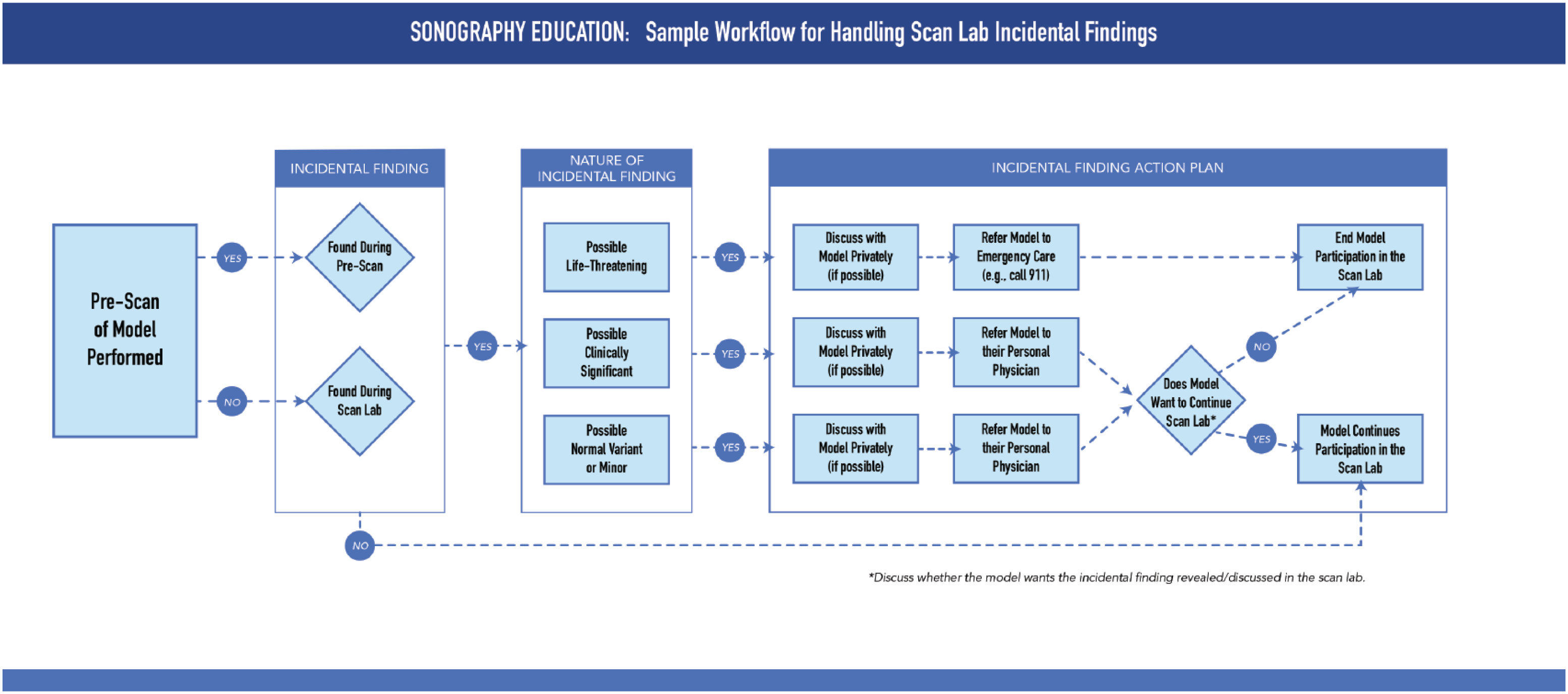
Abstract

Introduction
Diagnostic medical sonography educational programs (“sonography program[s]”) commonly use student volunteers, outside volunteers, and standardized patients (“model[s]”) during hands-on sonography training sessions (“scan lab[s]”) to practice sonographic procedures and techniques. This approach provides sonography students with the opportunity to practice on and interact with a variety of simulated patients as well as perfect their clinical scanning skills in a semi-structured educational environment. Utilizing student volunteers and outside volunteers may also reduce the expense associated with hiring trained, standardized patients and purchasing simulation phantoms.
Sonography Program Scan Labs
Provide scheduled and required experiences;
Provide student scanning exercises in a controlled laboratory setting;
May occur in a classroom setting or in a clinical setting;
May utilize paid or volunteer models, such as other students;
Should occur under the personal supervision of qualified and appropriately credentialed faculty;
Should occur in accordance with written policies, procedures, and disclosures to ensure that each model understands the purpose of the scan lab is educational, and not for diagnostic purposes;
Should occur in accordance with all applicable infection control and disinfection standards; and
Should not take the place of clinical education in a hospital or office setting on actual patients but can enhance scanning experience in certain limited settings.
Adapted from: Policies & Procedures, Joint Review Committee on Education in Diagnostic Medical Sonography, May 2018, available at: http://www.jrcdms.org/policies.htm. Accessed August 26, 2018.
Sonography Program Scan Labs
Sonography Educational Program Accreditation
While this white paper discusses one important aspect of the operation of sonography educational programs, such programs are advised to refer to the current Commission on Accreditation of Allied Health Education Programs’ (CAAHEP) Standards and Guidelines and the applicable Joint Review Committee/Committee on Accreditation’s policies and procedures. Questions about their requirements should be directed to CAAHEP or the applicable Joint Review Committee/Committee on Accreditation.
CAAHEP Standards and Guidelines https://www.caahep.org/Program-Directors/Standards.aspx
− Committee on Accreditation for Advanced Cardiovascular Sonography (COA-ACS) https://www.caahep.org/About-CAAHEP/Committees-on-Accreditation/Advanced-Cardiovascular-Sonography.aspx
− Joint Review Committee on Education in Cardiovascular Technology (JRC-CVT) http://jrccvt.org/policies%20&%20procedures.htm
− Joint Review Committee on Education in Diagnostic Medical Sonography (JRC-DMS) http://www.jrcdms.org/policies.htm
Sonography students, particularly incoming students, receive benefits from volunteering as a model such as:
Exposure to the scan lab setting;
Introduction to sonographic principles;
Observation of the sonography student learning process and faculty teaching methodology; and
With an educational scan lab, there is the possibility of uncovering an unexpected or “incidental finding”.1-8 An incidental finding is the identification of a sonographic finding or medical condition that was previously unknown to the model. Incidental findings can range from normal anatomical or physiologic variation (e.g., functional cardiac murmur, etc.) or other minor findings to possible clinically significant or life-threatening pathologies (e.g., ventral septal defect, vascular occlusion, suspected malignancy. etc.). 2
The published literature on incidental findings primarily relates to clinical skills training in medical students. Pols et al, estimated the incidence of an incidental finding in medical students during practical or clinical skills training activities to be 1.5%. 2 Other studies found a high likelihood of unexpected findings during medical school training sessions. 4 Mills et al reported the rate to be up to 9.1%. 11
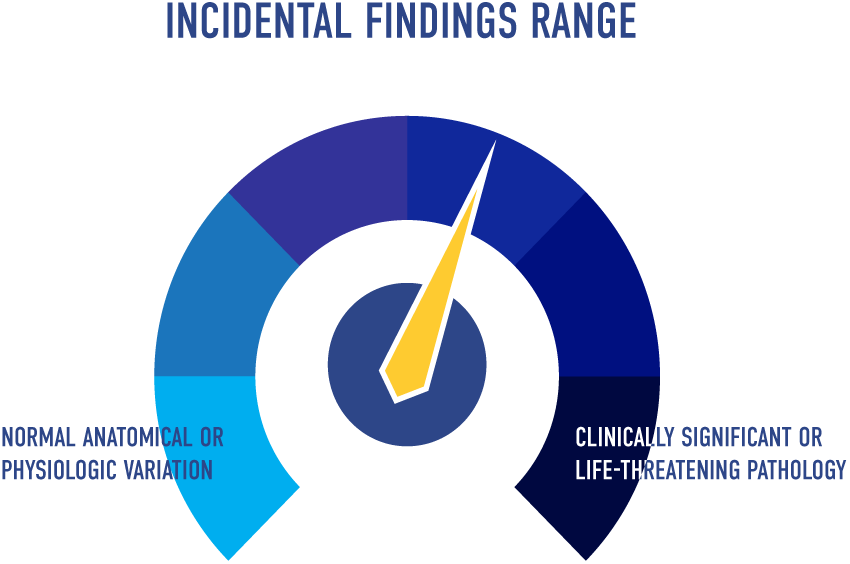
Incidental findings can range from minor to possibly life-threatening.
The literature does not currently report the number of incidental findings discovered during sonography program scan labs. However, anecdotal information may suggest the number of incidental findings is rising. Possible reasons may include:
Instructors teaching more scanning skills in the scan lab setting to help ensure students have fully developed the necessary skills and techniques for the clinical setting; and
An increase in the number of sonography programs and number of students enrolled.
The discovery of an incidental finding has the potential to impact not only the model, but also the student performing the sonographic procedure, the scan lab instructor, other students in the scan lab, and the sonography program.1-8 Because a number of legal and ethical issues can arise from the discovery and handling of an incidental finding during a simulated patient experience, the sonography program’s written incidental finding policy and procedures, as well as model disclosure and HIPAA authorization forms, can help the sonography program deal with incidental finding appropriately and consistently.
Today, sonography programs may or may not have policies and procedures in place that address handling an incidental finding in the scan lab setting. The Commission on Accreditation of Allied Health Education Programs (CAAHEP), which accredits diagnostic medical sonography, cardiovascular technology, and advanced cardiovascular sonography educational programs in the United States, does not have a specific accreditation standard regarding the handling of incidental findings in the scan lab or clinical training environments. 10
The sonography program’s written policy and procedures should guide the response when a student or instructor discovers an incidental finding in a scan lab model. At least annually (or whenever updated), the sonography program should require all models (including student volunteers) to complete and sign the sonography program’s written consent, HIPAA authorization, and medical history forms. Since student volunteers and other models may not expect or recognize that the risk for incidental findings exist, the sonography program should also provide models with the sonography program’s written incidental finding policy and procedures and give them the opportunity to ask questions about these documents.1-8 The sonography program should encourage models with questions about personal or confidential matters to meet with the program director or scan lab instructor privately (ideally before the scheduled scan lab).
Students and Incidental Findings in a Clinical Setting
If an incidental finding is discovered by a sonography student while scanning a patient at a sonography program’s clinical site (e.g., hospital, clinic, etc.), the student should discuss the possible incidental finding with their clinical site’s clinical instructor or supervising sonographer (outside the patient’s presence, if possible) and defer to the clinical site’s staff and policies and procedures to handle the possible incidental finding.
The following table describes the various documents and forms that a scan lab may use. Although listed separately here, the sonography program could combine the forms into one or more forms.
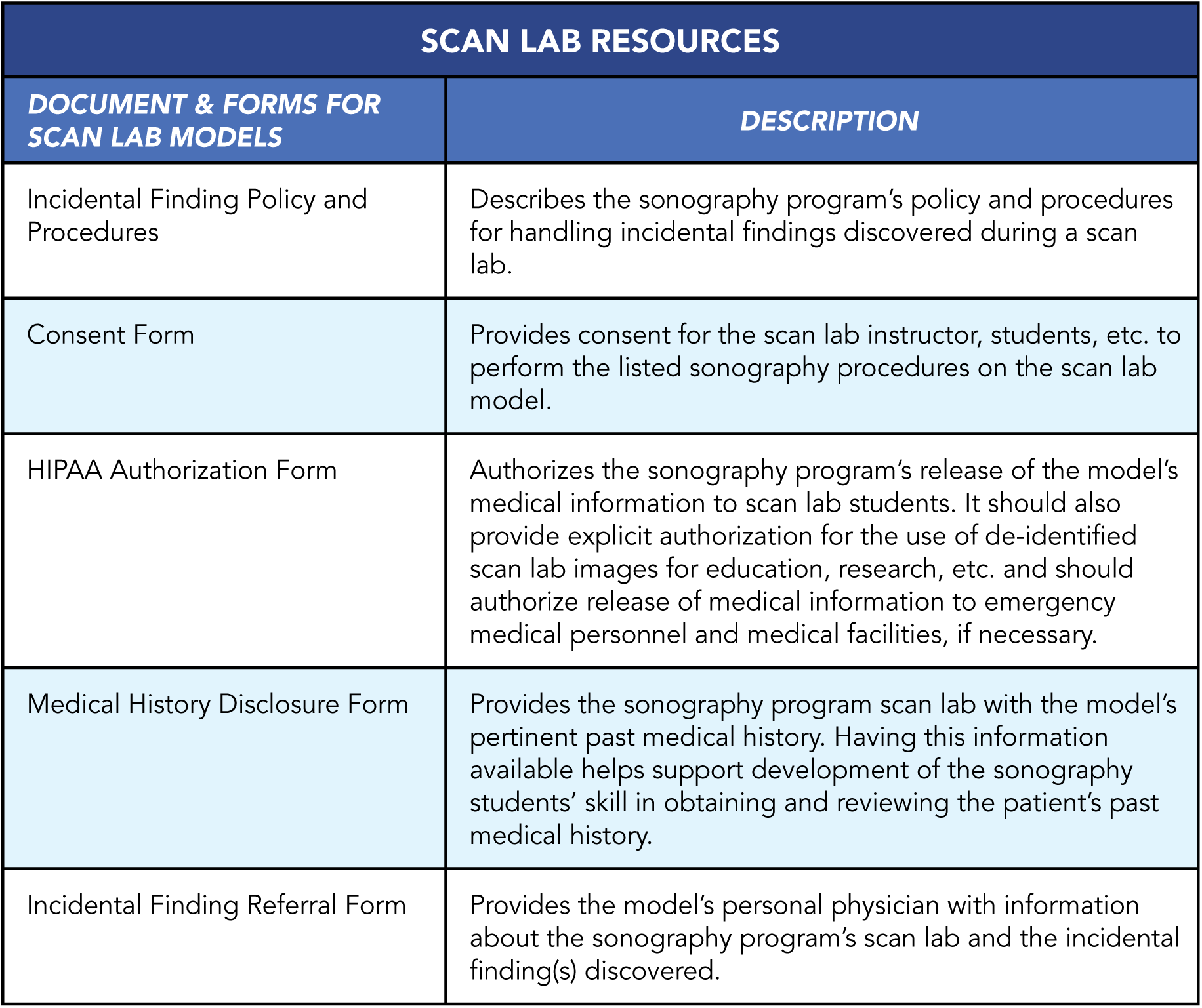
Scan Lab Resources
Strategies for Development of an Effective Incidental Finding Policy & Procedures
Although the discovery of an incidental finding during the sonography scan lab environment could be life-altering or even life-saving, legal or ethical issues could also arise from incidental findings. If a student or scan lab instructor provides the model with what appears to be a medical diagnosis or inappropriately discloses the model’s personal health information, the sonography program may be in violation of state or federal laws and regulations. Making a diagnosis or disclosure of incorrect information could also result in unnecessary anxiety and unnecessary care or medical costs for the model.
To help avoid issues resulting from the discovery of an incidental finding, a sonography program should have a written policy and procedures in place before they need them. For the policy and procedures to be most effective, the sonography program should strive to involve key personnel in their development and implementation. Key personnel may include, but is not limited to the:
Program director;
Program medical advisor or director (“medical advisor”);
Program faculty, including the scan lab instructor(s), clinical coordinator(s) or instructor(s), etc.;
Risk management staff; and
Legal counsel.
It is important to remember that sonography students (and sonographers) cannot diagnose in either a clinical or an academic environment. Everyone involved with the sonography program, including all models, should understand that only a qualified physician can make a medical diagnosis, including when an exam during a scan lab uncovers an incidental finding. If available, the sonography program’s medical advisor could speak with the model about the incidental finding. However, in many cases, the scan lab instructor or program director is the one who will disclose the incidental finding to the model.
“During the scan lab, the sonographic examination appeared to be different than expected. I cannot be sure if it is significant or not. You should consult your personal physician or other healthcare provider (e.g., physician’s assistant, nurse practitioner, etc.) and tell them you were participating as a model in a non-diagnostic sonography scan lab and the sonographic examination appeared to be different than expected. Your personal physician will decide whether you should have a diagnostic sonographic examination performed. If you don’t have a personal physician, I can provide you with a list of physicians in the area who you may wish to contact for follow-up. If you are a student, you may wish to contact your school’s student health services.”
Upon discovery of an incidental finding, the medical advisor, scan lab instructor or program director should disclose the incidental finding to the model.
The sonography program should review the written incidental finding policy and procedures periodically (e.g., annually) and obtain the feedback and approval of the sonography program’s key personnel. The sonography program’s faculty, administrative staff, clinical coordinator(s), or instructor(s) should fully understand the incidental finding policy, how to respond to questions about the policy, and the procedures to follow if they or a student discovers an incidental finding during a preliminary scan (“pre-scan[s]”) or a scan lab.
The policy and procedures should address handling a range of possible incidental findings – from normal anatomical or physiologic variations or other minor findings to possible clinically significant or life-threatening conditions. There is no “bright line” or “easy button” as every incidental finding situation will be somewhat different, and no policy can specifically address the entire range of possible incidental findings. If a student or instructor discovers a possible clinically significant or life-threatening condition in the scan lab setting, it is generally better to err on the side of caution and to ensure the model understands the scope of the incidental finding and has access to any needed medical care.
Some clinical findings in models will provide students with a unique opportunity to identify and differentiate between normal, normal variation, and abnormal anatomy and physiology. The lab instructor must carefully weigh the model’s privacy and the value of a teachable moment in the scan lab setting. If the scan lab instructor has conducted a pre-scan and discussed the pertinent findings with the model in private, the model can make an informed decision in advance of the scan lab about whether they want to serve as a model and if so, what information they are comfortable with the instructor sharing with the students. Seeing an incidental finding in scan labs may also provide students with vital experience since they will most likely encounter incidental findings in the clinical setting.
The sonography program’s policy and procedures should identify how, when, and whom reveals incidental findings to the model and to the participants in the scan lab. Ideally, the lab instructor will have completed a pre-scan and the model will have authorized the sharing of information with students and faculty. If the lab instructor has not completed a pre-scan, including all body organs or areas to be covered in the scan lab, or a student discovers a new incidental finding during the scan lab, the lab instructor could:
Pull the model aside and share information about the incidental finding;
Switch models without drawing attention; or
Take a break and discuss the incidental finding with the model.
Whenever possible, the lab instructor should avoid last minute or spur-of-the moment changes in models since doing so could make it difficult to conduct a pre-scan and as a result may significantly complicate the scan lab if a student uncovers an incidental finding.
Due to the nature of the educational setting, it is often difficult to maintain a model’s privacy during a scan lab. Students and instructors will discuss the model’s medical history, anatomy, or physiology, as well as sonographic technique, sonographic images, etc. during the scan lab. Additionally, other models in the scan lab may overhear these discussions. Lab instructors should require and maintain a professional atmosphere in the scan lab. They should stress to student sonographers that the scan lab is not a casual environment and should be treated as a simulated real-life experience (i.e., a sonographer would not blurt out what they see while scanning a patient in a clinical setting and they should not do so in the scan lab). Lab instructors should also remind students that information about any model regardless of the source (i.e., provided by the model, obtained by a lab instructor or student, or discussed during the scan lab) is strictly confidential and should not be discussed outside of the scan lab or classroom setting. Discussions outside of the scan lab setting could be particularly problematic if the model is also a student in the sonography program.
Consent Form Considerations
From a medico-legal perspective, a consent form used in a clinical setting discloses information to a patient about the applicable benefits, risks, and alternatives for a diagnostic test or a medical procedure or treatment. The provision of this information and the person’s understanding of this information form the basis for the patient’s “informed consent.” It also documents the person’s authorization to perform the specific diagnostic test, medical procedure or treatment, or to share patient information (e.g., with family members, personal physicians, other healthcare providers, insurance companies, etc.).
While a sonography program’s scan lab does not set forth the expectation that it is for diagnostic purposes and no medical treatment is expected to result, it is still important that the model understand what to expect during the sonographic procedure and what will happen if an incidental finding is discovered during the scan lab. The sonography program’s consent form for models can help answer many questions and address issues related to incidental findings before they arise.
A sonography program’s staff (e.g., program director) typically develop the consent form for models and the sonography program’s medical advisor, risk management staff, legal counsel, etc. should approve it. The sonography program staff should review the model’s completed consent form with each model and answer any questions. The sonography program should store the signed and dated consent form as it would store any other documents containing confidential information (i.e., with access restricted to only those staff who need access to the consent form). Ideally, a model would sign a new consent form on an annual basis and provide in writing a revocation of consent to serve as a model. However, if a model only provides verbal revocation, the sonography program staff should document the verbal revocation in writing.
Development and Implementation of an Incidental Findings Policy & Procedures and Related Forms
While the actual content and format of a sonography program’s incidental findings policy and procedures and related forms will vary, sonography programs should consider the following elements:
Disclose the non-medical purpose of the sonographic procedure(s).
Explain the prudent use of ultrasound and the
List the minimum age required for participation as a model.
Explain that participation is voluntary, and the model can stop at any time.
Request that the model disclose past pertinent medical history including known pathologies, past imaging studies, etc.
Obtain the name, address, and telephone number for the model’s personal physician (if applicable).
Obtain written consent for the performance of sonography procedure(s).
Document and store each model’s written consent or revocation of consent.
Obtain a signed Health Insurance Portability and Accountability Act of 1996 (“HIPAA”) authorization form.
Perform a pre-scan on the model (whenever feasible).
Identify the body organs/areas, the sonographic procedures the scan lab instructor and students will perform, and the estimated amount of time the scan lab will take.
List obstetrical scan lab requirements and restrictions (e.g., prior medical sonogram, no first trimester models, no more than one scan lab per month, no color doppler, etc.).
Provide the incidental findings policy and procedures and all related forms to models, students, and staff.
Ensure the scan lab is appropriately supervised when models (including students) are scanned.
Provide procedures or a referral form for the referral of a model with a possible clinically significant or life-threatening incidental finding to their personal physician (or emergency personnel, if applicable).
List who the sonography program should notify for each type of incidental finding (i.e., normal variation versus possible clinically significant or life-threatening).
Describe how to handle emergency (life-threatening) situations that may arise in a scan lab setting.
List the contact person(s) (e.g., Program Director) including contact information for questions about incidental findings policy and procedures or related forms.
NOTE: Sonography programs may include some of the elements listed above in both the incidental findings policy and procedures and related forms for models. See below for additional discussion of each element.
If a student discovers a possible clinically significant incidental finding during the scan lab, the instructor should attempt to keep the incidental finding confidential and to discretely change models or temporarily stop the scan lab activity so they can speak with the model in private. The instructor should not point out this type of incidental finding to the rest of the class. 4 Once aware of the incidental finding, the model can decide whether to continue serving as a model and whether to share the incidental finding with the rest of the class. In rare cases where the scan lab instructor believes the incidental finding is of an emergent nature (e.g., sonographically appears to be a possible dissecting aortic aneurysm), the scan lab instructor should ensure appropriate medical care is available (e.g., call 911).
For a model who is also a student in the program, notification of the program director allows the program director to prepare for additional questions from the student, offer suggestions for follow up, and in severe cases, prepare for the possibility of a medical leave of absence or withdrawal from the sonography program. 6 If the incidental finding was noted by other scan lab participants or observers, the program director may need to provide assurance that the appropriate procedures are in place and remind everyone to respect the affected student’s privacy. The discovery of an incidental finding may also cause students to question their future participation as a model. Individualized counseling may be necessary if a fellow student discovered the significant pathology.
The program director should also debrief with the scan lab instructor. This allows the instructor to process emotions, which they may have held in check while attending to the model, the student sonographer, and the class. It is also an opportune time to reflect on the scan lab policies and procedures and adjust them as neccessary.3,10
If the incidental finding is not a normal anatomical or physiologic variation or a minor incidental finding, the scan lab instructor should inform the model in a private setting that an incidental finding was found during the non-diagnostic sonographic procedure, including a brief description of the incidental finding in neutral terms without attempting to make a diagnosis. When discussing the incidental finding, it is important to remember to treat each situation seriously and respectfully as this news may be confusing or upsetting for the model.2,3 Some models may view an incidental finding in a positive light and appreciate knowing and being able to take appropriate action. Others may have a neutral reaction and need time to process the information. Still others may view the information in a negative light due to the added worry, time, and possible expense to their life. 2 The scan lab instructor should encourage the model to see their personal physician for follow up and possibly obtain a diagnostic sonography examination.
Many sonography programs do not store the non-diagnostic images generated from a scan lab. However, if the sonography program’s policies and procedures include saving and providing any sonographic images from the pre-scan or scan lab to the model’s personal physician, the sonography program should clearly mark the images that they are solely for educational, non-diagnostic purposes. In addition, the sonographic images and any related documents should be stored in compliance with the sonography program’s policies and procedures. 1
To avoid any confusion, sonography programs may include a note in their forms and policies and procedures clarifying that the sonography program is not responsible or liable for any costs or results (e.g., diagnostic testing, treatment, mental anguish, etc.) associated with a model seeking medical evaluation or care based on the referral.
Conclusion
Sonography programs use a variety of models in their scan labs to give students the opportunity to practice and hone their skills and techniques. There is always a possibility that a student or scan lab instructor will identify an unexpected or unknown finding in a model. Sonography students and the sonography program models and staff should be aware of this possibility.
Incidental findings in scan lab models may range from normal anatomical or physiologic variation or minor findings to possibly clinically significant or life-threatening pathologies. Standardizing the process that the sonography program uses to handle possible clinically significant or life-threatening incidental findings (e.g., provide an “Incidental Finding Referral Form” to the model, notify the Program’s medical advisor, etc.) and ensuring that all involved follow the policy and procedures can help avoid medical, legal, and ethical issues that could arise from the identification of incidental findings in a scan lab setting. The sonography program should proactively involve their medical advisor and other key personnel or departments in the development of the incidental finding policy and procedures, as well as the forms used by the sonography program.
Best Practices Summary
Case Studies
Case Study #1
An instructor scheduled a renal scan lab during the first months of a sonography program’s curriculum. The scan lab involved each student scanning the right kidney of a model. While a student was scanning through the kidney, the scan lab instructor observed a possible, subtle hyperechoic mass in the model’s liver. With only two more students left to scan the model, the instructor continued with the scan lab. At the end of the scan lab, the instructor discretely asked the model to stay behind. Upon scanning the liver more thoroughly, the instructor found a 2.0 cm hyperechoic mass in the right lobe of the liver. The instructor told the model that he noticed something unusual or unexpected (an incidental finding) and encouraged her to follow up with her personal physician. Later, the model participated in another scan lab activity where she reported that her personal physician had ordered a complete abdominal ultrasound examination and diagnosed her with a hepatic hemangioma.
Discussion: This case study demonstrates how the instructor maintained the confidentiality of the model by not pointing out the possible incidental finding to the class and properly disclosed the finding to the model. If the scan lab instructor had discovered the incidental finding during a pre-scan, it could have been addressed prior to the scan lab. Now that a physician has diagnosed the model with a hepatic hemangioma, the scan lab instructor could ask the model for their consent to reveal the diagnosis and offer the scan lab students an opportunity to scan the hepatic hemangioma.
Case Study #2
As a visiting instructor, I taught a neonatal spine sonography lecture and scan lab. The scan lab included live scanning on a neonatal scan model who was only weeks old and a relative of a scan lab participant. The neonate’s parent signed a consent form. As soon as I placed the transducer on the spine, I noticed an abnormality. The abnormality went undetected by the students, who were new to spine sonography. While I continued to scan, my mind was racing 100 mph trying to formulate a plan. During a break, I called an attending radiologist to discuss the case, who recommended I counsel the parents to contact their pediatrician for follow-up diagnostic imaging.
Discussion: This case study supports the recommended use of a consent form for models and an incidental findings policy and procedures, with physician involvement when warranted. In this case study, the sonography program obtained the consent of the neonate’s parent before performing the sonographic procedure in the scan lab setting. It is unknown whether the sonography program incidental findings policy and procedures specifically authorized the scan lab instructor to contact an attending radiologist for consultation. A pre-scan of the neonate by the scan lab instructor could have identified the abnormality prior to the scan lab and avoided potential issues resulting from the incidental finding.
Case Study #3
As a sonography student, I had a personal experience with an incidental finding. During my second month of school, my instructor was demonstrating to the class how to image the iliac arteries and veins. While she was teaching the scanning technique, I noticed she repeatedly scanned through my left lower quadrant. I thought she was looking at my ovary, so I disclosed my history of polycystic ovarian syndrome. I also commented that my mom had a dermoid cyst removed in the past. It was then that she pointed out a mass-like area that was concerning. My instructor did not tell me what she thought it might be but recommended that I follow up with my family doctor or Student Health. After seeing my doctor and having a diagnostic sonographic examination, he diagnosed me with a 9.0 cm left ovarian dermoid cyst.
Discussion: This case study demonstrates the need for volunteers to disclose any known pathologies prior to serving as a model. Other unique factors about this case were the student’s disclosure of her medical history to her instructor and classmates in the scan lab. Reviewing the model’s medical history with the model during a pre-scan could have helped to better manage the incidental finding in a private setting. Now that a physician has diagnosed the model with a dermoid cyst, the scan lab instructor could ask the model for their consent to reveal the diagnosis and offer the scan lab students an opportunity to scan the dermoid cyst.
Case Study #4
Unbeknownst to us, we recently had a student bring her under-age sister into the scan lab to act as a model. The consent form was completed and signed in the scan lab, but the student didn’t consider that the sister was under-age or that the student was supposed to be supervised for any sonography procedures performed on a model. The faculty member had unlocked the scan lab door because the student indicated she would be practicing scans using a phantom. We disciplined the student for this after we discovered she had logged her sister’s name as a model. We thought we had this tightly controlled. What a learning experience!
Discussion: This case study demonstrates the need to have consent forms for models and to ensure both students and staff understand and follow the sonography program’s policies and procedures, including scan lab requirements or restrictions.