Abstract
Holoprosencephaly (HPE) is a complex brain malformation caused by incomplete fusion of cleavage of the cerebral hemispheres and deep brain structures affecting 6 to 12:10,000 live-born infants. There are three categories of HPE ranging in severity, with alobar holoprosencephaly being the most severe, followed by semilobar holoprosencephaly, and lobar holoprosencephaly being the mildest form. Facial anomalies as well as chromosome anomalies are often associated with HPE. This case study describes a transabdominal sonographic diagnosis of alobar HPE with cebocephaly originally found at 27 weeks 3 days on a patient with no prenatal care.
Embryologically, primary neuralation is responsible for forming the neural tube. The neural tube forms three important structures: the forebrain, midbrain, and hindbrain. 1 Holoprosencephaly (HPE) results from incomplete separation of the forebrain into the right and left hemispheres, which occurs between days 18 and 28 of gestation.2,3 Depending on the location and lack of cleavage, HPE is categorized into three main categories and a variant: alobar, semilobar, lobar, and the most recently described middle interhemispheric variant of HPE (MIH).1,4 Alobar is the most severe, followed by semilobar and then lobar. MIH is somewhere in middle of these classifications, closer to lobar than alobar. In alobar, semilobar, and lobar HPE, the incomplete cleavage is in the basal forebrain1,5; however, the MIH variant consists of a fusion of the cerebral hemispheres in the posterior frontal and parietal lobes.1,5–7
In lobar HPE, the brain forms only a partial frontal horn, an absent corpus callosum, and a normal third ventricle. 8 In semilobar HPE, there is partial formation of the interhemispheric fissures and the falx cerebri with complete fusion of the anterior brain. 8 “In alobar HPE there is limited formation of the anterior portion of the brain. The infants also lack a falx cerebri, an interhemispheric fissure and a corpus collosum.” 8 In this severe form of HPE, there is no third ventricle and the thalami are fused. The partially formed cerebrum is found in the rostral calavarium. 8 A dorsal cyst is almost always found in alobar HPE (92%), which correlates with thalamic fusion. A dorsal cyst is found less frequently with semilobar HPE (28%) and occasionally with lobar HPE (9%). 1
In addition to the brain anomalies, craniofacial findings may also be present. These may include ocular hypotelorism (decrease distance between eyes), cyclopia (single, midline, fused eye exists in a single orbit below a proboscis), proboscis (nose-like appendage), ethmocephaly (proboscis separating ocular hypotelorism), cebocephaly (ocular hypotelorism with a single nostril nose), single nostril, or cleft lip and/or palate. 9
With recent advancements and improvements of high-resolution sonography, early diagnosis of HPE is possible. Excellent sonographic images help to predict the severity of craniomaxillofacial anomalies as well as cephalic anomalies. There are at least two case reports diagnosing HPE before 10 weeks menstrual age and many more case reports detecting HPE between 10 and 14 weeks. At this early age, sonography detects abnormal facial morphology and the absence of the “butterfly” sign.1,10,11 “The butterfly sign is demonstrated in the first trimester because the choroid plexus is narrow in the middle but thicker at both ends. In the first trimester, the choroids are side by side and this creates an image of a butterfly. If sonographers are unable to demonstrate this butterfly image, HPE is highly suggestive.”1,11
The incidence of HPE is about 6 to 12:10,000 live-born infants and 40:10,000 in embryos and is found more often in females than males. 12 The definitive cause of holoprosencephaly is unknown in many cases. However, 40% of live births have a chromosomal abnormality, with trisomy 13 accounting for half of the chromosomal abnormalities. It can also be caused by maternal infections, such as cytomegalovirus and toxoplasmosis. It can also be attributed to environmental factors, such as maternal diabetes, infections during pregnancy, drugs taken during pregnancy, and low cholesterol levels. 13 Although many are born with a chromosomal abnormality, normal karyotypes are also found with HPE. HPE can be recessive or autosomal. 9
Depending on which classification an infant is diagnosed with, HPE may be fatal or debilitating. In a study performed by Stashinko et al. 14 involving 104 children, approximately 50% of the children with alobar HPE died within five months, and of those surviving, approximately 30% lived beyond one year; however, none of the surviving children could sit independently or speak.1,15 More than 50% of children with lobar HPE are able to walk (some with assistance), have normal to impaired hand function, and can speak single words (some could put a multiword sentence together).1,16 MIH children can often walk with assistance and talk and function with minimal impairment.1,17 A study by Wenghoefer et al. 18 that involved 51 children reported only one survivor, with this child having both motor and mental weaknesses.
Case Report
A young woman, gravida 3, para 1, presented to the Labor and Delivery clinical unit with complaints of abdominal pain. Upon receiving a complete assessment by the obstetrician, a sonogram was ordered for fetal well-being, insufficient prenatal care, fetal measurements, and abdominal pain. The sonogram revealed a singleton female fetus with the biometry measurements indicating the pregnancy at 27 weeks 3 days. The abdominal circumference (AC) measurements and femur length (FL) measurements were symmetrical; however, the biparietal diameter (BPD) and head circumference (HC) measured markedly smaller, lagging more than four weeks. Evaluation of the brain discovered a monoventricle, no separation of the cerebellar hemispheres (Figure 1), and a prominent cystic area in the posterior fossa (Figure 2). Spine, heart, and face could not be well assessed; however, midline facial anomalies were suspected, possibly cebocephaly (Figures 3 and 4) and proboscis (Figure 5). A biophysical profile was performed two days later, and the fetus scored 2 for amniotic fluid, 2 for gross movement, 2 for tone, and 2 for breathing for a score of 8/8 with resistive indices being normal. The patient was released, and follow-up care was recommended by a specialty obstetrical physician due to the severity of anomalies.
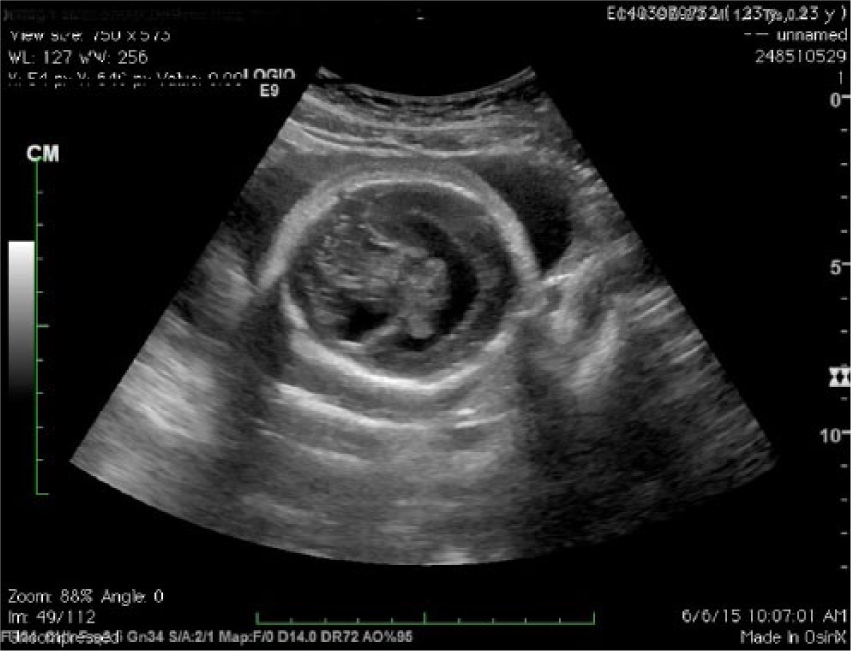
Image showing monoventricle and no separation of the cerebral hemispheres.
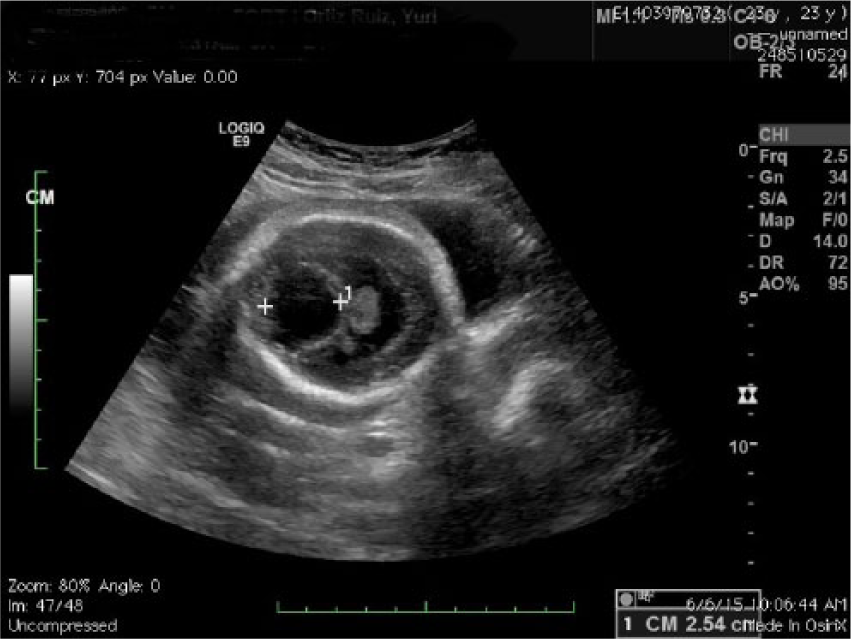
Transverse image of the head with prominent cystic area in the posterior fossa.
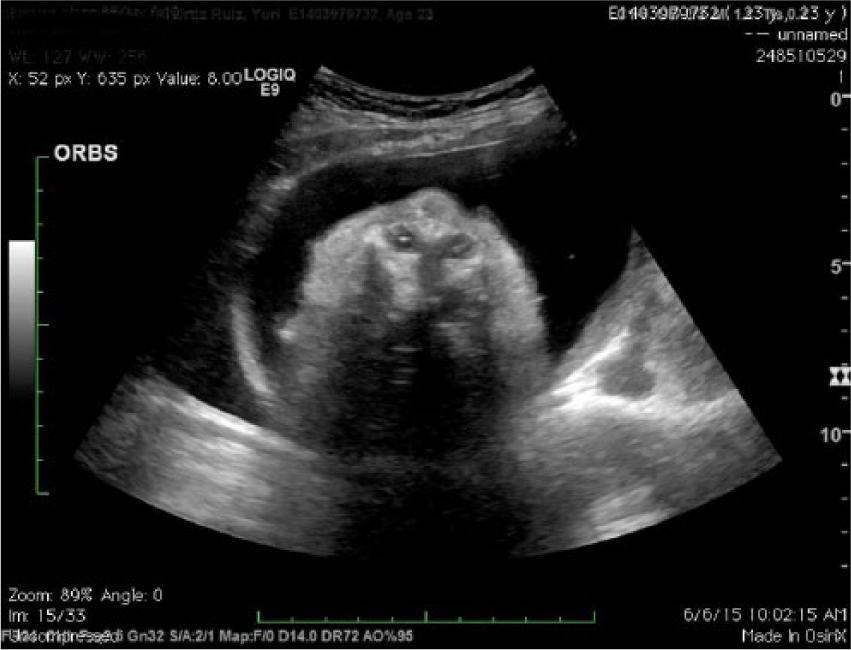
Hypotelorism on 27-week sonogram.
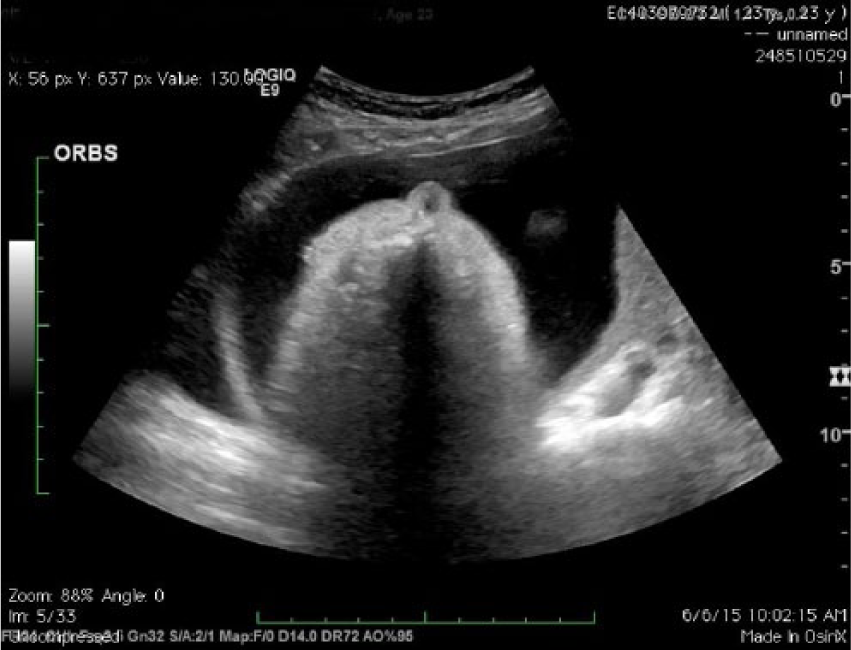
Cebcephaly on 27-week sonogram.
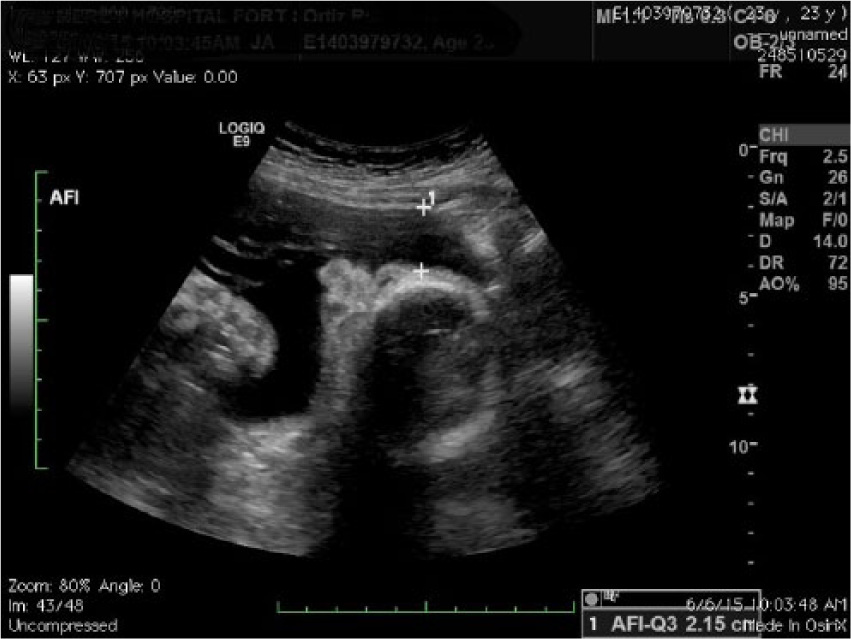
Possible proboscis with an amniotic fluid index (AFI) measurement.
Follow-up examinations were performed two and three months later. The fetal head was microcephalic with the BPD and HC continuing to fall behind the AC and FL measurements. On the final sonographic examination, the BPD and HC measured less than the fifth percentile (eight weeks behind all other biometry). A single ventricle with a fused thalamus was noted. Fetal face was dictated as abnormal, with the midface demonstrating a pedunculated nose suggestive of a proboscis. The fetus was diagnosed with alobar HPE.
Discussion
HPE is a severe congenital brain malformation causing a wide variety of congenital brain anomalies and facial deformities. Sonography is a good modality for prenatal diagnosis of HPE and its associated anomalies; therefore, a careful sonographic examination of the fetal head and face should be performed preferably during the early second trimester of pregnancy.
Alobar HPE can be characterized by a varied amount of residual holospheric mantle and can be referred to with these graphic labels: pancake (remnants of brain tissue against the frontal base of the skull), bowl (brain tissue that is only a peel of frontal cerebrum), and ball (complete parenchymal lining of the holosphere without a dorsal pouch). 19 Based on these labels and sonographic images, this case appears to be most aligned with the bowl appearance. This rare case of alobar HPE is also presented to illustrate the importance of early screening biometry measurements. It also points to the need to carefully review these measurements for discordance and the possible diagnoses of the associated outcomes.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
