Abstract
Introduction
Sterile fluid shortages have become a pervasive threat in the United States health care system. There were 37 documented sterile fluid shortages from 2001 to 2017, with 12 new shortages reported in 2017 alone. 1 Often, these shortages are the result of manufacturing delays, natural disasters, and quality control issues. Such supply chain disruptions compromise patient safety, especially when intravenous (IV) fluids are urgently needed for drug administration and fluid resuscitation. This adds further strain to inpatient systems already burdened by limited resources. 2 This crisis reached a peak in 2017 in the aftermath of Hurricane Maria, which devastated Puerto Rico, where 44% of IV fluid bag manufacturing in the United States occurs. 3
Hurricane Maria made landfall in Puerto Rico as a Category 4 storm in September of 2017, causing a major natural and humanitarian crisis that reverberated throughout the United States, the effects of which were felt until 2018. 4 The storm devastated a Baxter International IV fluid manufacturing plant, one of the suppliers of IV fluid bags, leading to major shortages across the United States.5,6 As a result, many first-line clinical practices were altered to attempt to accommodate the shortage. This national vulnerability was further underscored by the impact of Hurricane Helene in September of 2024 as another Baxter International facility was decimated in western North Carolina, resulting in many of the same shortages experienced during Hurricane Maria. 7
Febrile neutropenia is a life-threatening emergency that requires immediate clinical intervention via the use of broad-spectrum antibiotics and IV fluid administration. 2 Timely antibiotic use is critical for treatment to prevent disseminated and often lethal infection. Thus, delays in antibiotic administration have been associated with significantly increased mortality rates. 8 Current ASCO/IDSA guidelines recommend initial antibiotic administration within 1 hour of triage in the setting of febrile neutropenia, due to the rapid rate at which the condition may advance to sepsis or septic shock, with mortality rates approaching 50% in severe cases. 2 Furthermore, fluid resuscitation is often essential in maintaining adequate perfusion and organ function in these patients. Rapid availability of IV antibiotics, which can be prepared in fluids such as normal saline, and fluids for resuscitation are critical for the treatment of this high-risk condition, thus emphasizing the need for evaluation of the potential impacts of fluid shortages on patient outcomes. This study aimed to evaluate the impact of a normal saline shortage on in-hospital mortality and the length of stay (LOS) among adults with febrile neutropenia.
Methods
This retrospective cohort study used data from the Healthcare Cost and Utilization Project (HCUP) National Inpatient Sample (NIS) claims database. The NIS is the largest publicly available all-payer inpatient health care database in the United States, providing regional and national estimates related to inpatient utilization, access, costs, quality, and outcomes. It includes information on approximately 7 million hospital stays annually. Our project was submitted to our institutional review board (IRB) as non-human subjects for research and was acknowledged by the IRB as meeting criteria for this categorization.
We identified adult encounters experiencing febrile neutropenia using methods adapted from those described by Li and colleagues. 9 To be included, patients had to have an ICD-10-CM diagnostic code indicating neutropenia (ie, D70.X) in combination with an ICD-10-CM diagnostic code indicating either fever or infection. Identified encounters were used to create 2 cohorts. The first cohort represented the normal saline shortage caused by Hurricane Maria and included all identified encounters between November 2017 and March 2018. 10 The second cohort represented the same time period in the year prior to the shortage to account for seasonality and included all encounters between November 2016 and March 2017.
Comparisons of categorical variables between cohorts were conducted using chi-square or Fisher’s exact tests. Continuous variables were analyzed using independent t-tests. In-hospital mortality, the primary outcome of interest, was assessed through adjusted logistic regression models. Adjusted comparisons of LOS, the secondary outcome of interest, were performed using generalized linear regression with a gamma distribution and log-link function. All statistical analyses were carried out using SPSS version 30 (IBM Corp., Armonk, NY), with P-values <0.05 considered significant.
Results
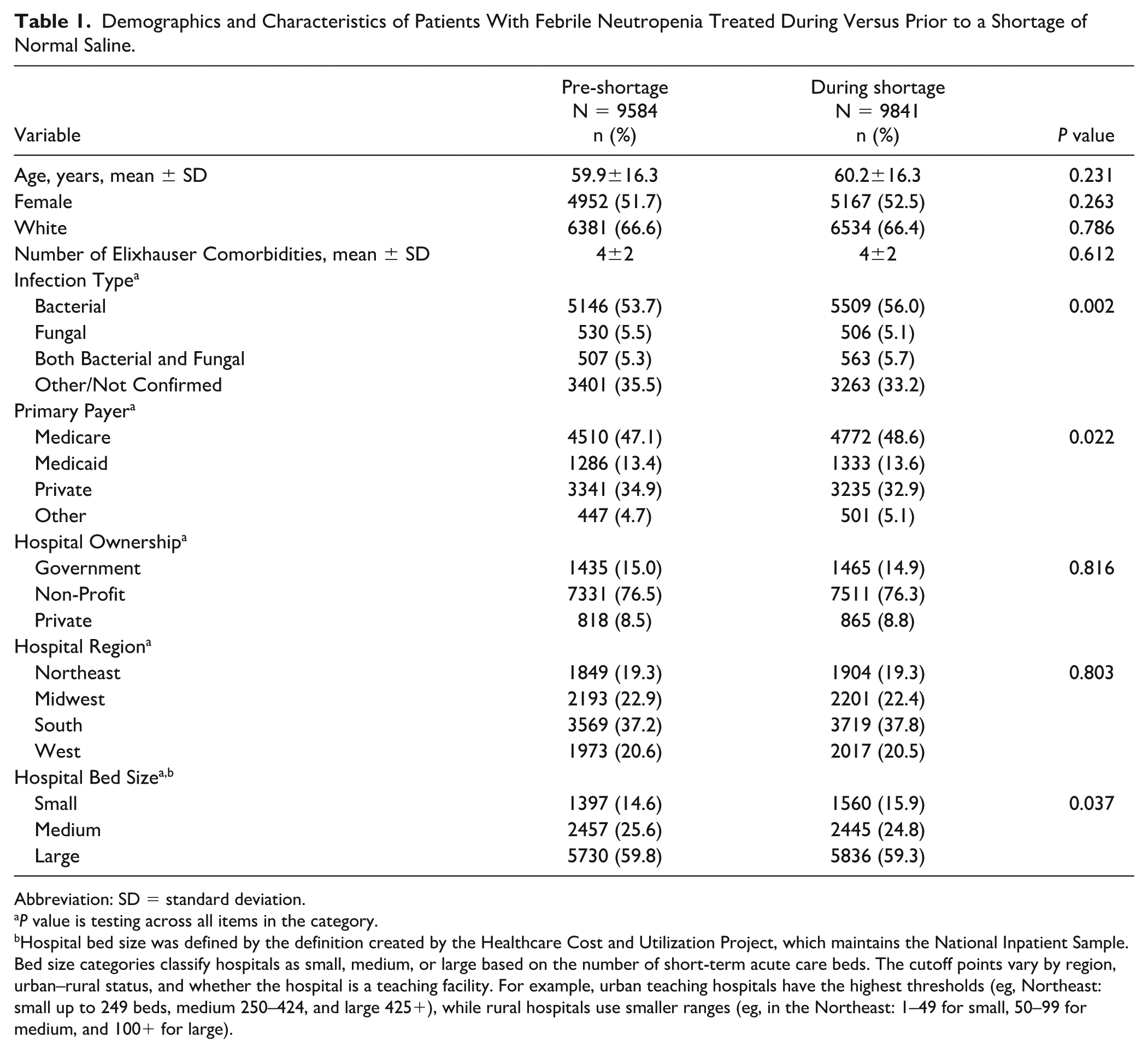
There were 19 425 encounters for febrile neutropenia that were identified in the dataset. Of these, 9584 occurred between November 2016 and March 2017, prior to a national normal saline shortage, while 9841 occurred during a shortage period of November 2017 to March 2018 (Table 1). The mean age of the patients treated during the shortage was comparable to those treated pre-shortage (60.2 ± 16.3 vs 59.9 ± 16.3 years, P = 0.231), more than half of the patients in both cohorts were female (53.5% during vs 52.7% pre-shortage, P = 0.263), and nearly two-thirds of those studied in each cohort were White (66.4% during vs 66.6% pre-shortage, P = 0.786). The average number of comorbidities was similar between cohorts.
Demographics and Characteristics of Patients With Febrile Neutropenia Treated During Versus Prior to a Shortage of Normal Saline.
Abbreviation: SD = standard deviation.
P value is testing across all items in the category.
Hospital bed size was defined by the definition created by the Healthcare Cost and Utilization Project, which maintains the National Inpatient Sample. Bed size categories classify hospitals as small, medium, or large based on the number of short-term acute care beds. The cutoff points vary by region, urban–rural status, and whether the hospital is a teaching facility. For example, urban teaching hospitals have the highest thresholds (eg, Northeast: small up to 249 beds, medium 250–424, and large 425+), while rural hospitals use smaller ranges (eg, in the Northeast: 1–49 for small, 50–99 for medium, and 100+ for large).
Primary payer distribution differences were small, yet statistically significant (P = 0.022). Patients that were treated during the shortage were more likely to be covered by Medicare (48.6% during vs 47.1% pre-shortage), Medicaid (13.6% during vs 13.4% pre-shortage), and other primary payers (5.1% during vs 4.7% pre-shortage) and less likely to be covered by private insurance (32.9% during vs 34.9% pre-shortage). Hospital ownership and regional distribution were consistent across both periods, with most patients receiving care at non-profit institutions (76.3% during vs 76.5% pre-shortage, P = 0.816). Care was also consistently distributed across US regions throughout the pre-shortage and shortage periods (P = 0.803). The distribution of hospital bed size displayed a small but statistically significant shift between the pre-shortage and shortage periods (P = 0.037). Patients treated during the shortage were more likely to be treated at small hospitals (15.9% during vs 14.6% pre-shortage) and less likely to be treated at medium (24.8% during vs 25.6% pre-shortage) or large hospitals (59.3% during vs 59.8% pre-shortage) as compared with the pre-shortage period. Small but statistically significant differences were also observed in infection type (P = 0.002). In the pre-shortage period, patients were less likely to have bacterial infections (56.0% during vs 53.7% pre-shortage) and more likely to have fungal infections (5.1% during vs 5.5% pre-shortage).
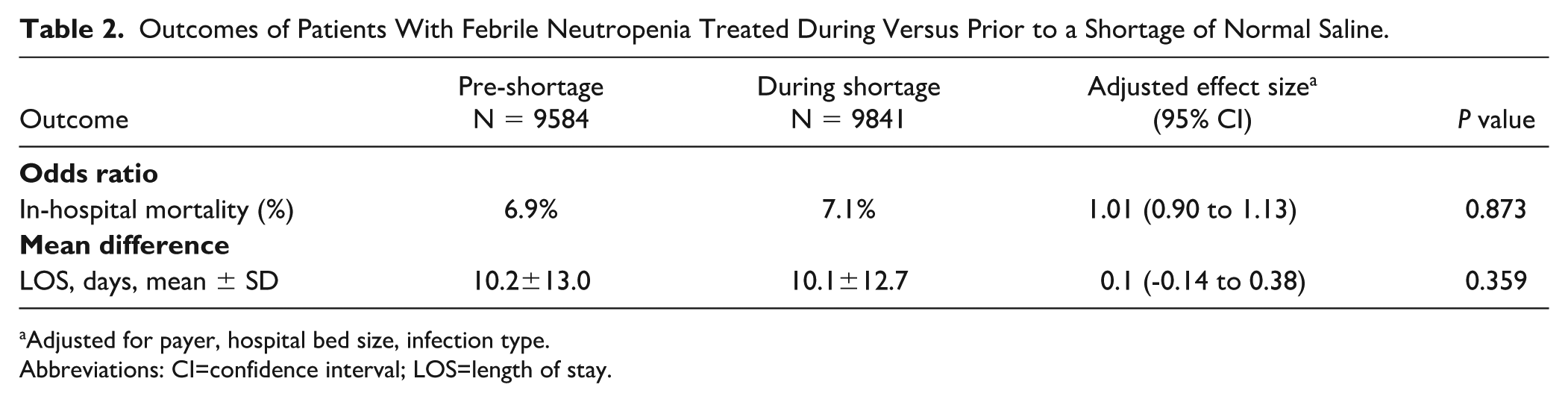
Treatment outcomes among patients with febrile neutropenia were similar before and during the normal saline shortage (Table 2). In-hospital mortality rates before the shortage were 6.9%, with a slight increase to 7.1% during the shortage. After adjustments were made for payer, infection type, and hospital bed size, no significant difference was observed in in-hospital mortality (adjusted odds ratio = 1.01; 95% confidence interval [CI] = 0.90 to 1.13). In addition, hospital LOS was similar between the groups. The mean LOS was 10.2 ± 13.0 days in the pre-shortage cohort and 10.1 ± 12.7 days during the shortage. The adjusted mean difference in LOS was 0.1 days (95% CI = −0.14 to 0.38).
Outcomes of Patients With Febrile Neutropenia Treated During Versus Prior to a Shortage of Normal Saline.
Adjusted for payer, hospital bed size, infection type.
Abbreviations: CI=confidence interval; LOS=length of stay.
Discussion
In this retrospective analysis of 19 425 febrile neutropenia encounters, no significant difference in in-hospital outcomes among pre-shortage and shortage patient groups was observed. Patient demographics of age, sex, and race were comparable across groups. However, small yet significantly significant differences in primary payer and hospital bed size did exist, reflecting a reduction in hospital size and an increase in Medicare and Medicaid coverage. No differences were found in in-hospital mortality or LOS. These findings were similar in adjusted analyses, which showed no significant difference in in-hospital mortality and an adjusted mean difference in LOS of just 0.1 days (95% CI 0 –0.14 to 0.38). These results suggest that despite valid concerns surrounding national normal saline shortages, patient outcomes for those hospitalized with febrile neutropenia remained stable during this period despite shifts toward smaller, resource-limited hospitals and older Medicare populations.
Previous studies have analyzed the impact of the 2017 NS shortage on process-based outcomes as opposed to clinical outcomes. Elgersma and colleagues evaluated how NS shortages impacted antibiotic administration for patients with febrile neutropenia. 8 This revealed a significant decrease in timely antibiotic administration in the shortage period, with successful administration within 60 minutes dropping from 93.8% to 33.3% (P = 0.0002). This is of major concern given the fact that delayed antibiotic administration is associated with increased mortality for patients with Febrile neutropenia. 8 During normal saline shortages, institutions have reported implementing intravenous push (IVP) routes of administration for select antibiotics, demonstrated improvements in workflow efficiency, and found mechanisms for preserving saline resources. 6 However, these reports were not focused on presenting patient morality or other final health outcome data.
Other studies have focused on the implementation of oral rehydration strategies to reduce reliance on IV fluids for mild dehydration. 3 For example, one study found this led to a 30% reduction in IV fluid use within 1 week and a 15% decrease in IV fluid orders in the emergency department over the course of 3 weeks. While these studies demonstrate creative responses to supply shortages, the emphasis was mainly on workflow modifications, cost, and time metrics, with minimal focus on clinical outcomes.
While IV fluid shortages directly impact health care delivery and may pose a threat to patient outcomes, our findings may reflect the resiliency of the health care system and the adaptability of health care providers. While many of the studies cite significant challenges to standard protocols in the treatment of febrile neutropenia due to these shortages, our analysis suggests that there was no change in final health outcomes.3,6,8 Several avenues may have served to mitigate the impact of the shortage on patient outcomes, especially among those that were critically ill. The flexibility of front-line health care professionals likely played a crucial role in minimizing the effects of the shortage via the development of effective oral rehydration strategies and the administration of IV push antibiotics in lieu of IV infusions when possible.3,6 Unfortunately, subsequent shortages have continued to occur. 7 These recurrences emphasize the need for an evaluation of IV fluid shortages on patient outcomes.
Study Limitations
This study has several limitations. First, the data utilized from the HCUP NIS database does not include information about the time to antibiotic or fluid administration, preventing evaluation of any nationwide impacts on this measure. Rapid administration of antibiotics and often fluids is a key treatment strategy in the setting of febrile neutropenia and is correlated with improved mortality outcomes.2,8 While our study shows no statistically significant impact on mortality, large studies specifically including an evaluation of time to antibiotic administration may be warranted. In addition, the database lacks data on chemotherapy regimens and degree of immunosuppression, granular data on cancer type, ICU admission data, and specific medications administered, which limits further risk stratification. Furthermore, the dataset lacked information on the duration of IV antimicrobial therapy. The assessment of sepsis criteria or illness severity at presentation was limited due to a lack of vital sign data in the NIS. The etiology of febrile neutropenia cannot be determined in the dataset. In addition, there is a lack of data on adjuvant interventions, including discontinuation of chemotherapy or other offending agents. Furthermore, potential changes in clinical practice during the study period cannot be evaluated. The NIS does not contain data on anticipated LOS; thus, this also could not be evaluated in our study and compared with actual LOS. Moreover, the database did not include information on hospital specific metrics or strategies to address the shortage (eg, conservation techniques, average supply per hospital site, if drug reconstitutions were adjusted to alternative fluids) or health system relationships; thus, these could not be summarized in our study.
Conclusion
In this retrospective analysis comparing outcomes in patients with febrile neutropenia during a national IV saline shortage to those of patients prior to the shortage, in-hospital mortality and LOS did not significantly vary between the study periods. While IV fluid shortages negatively impact health care processes, our study did not find meaningful negative impacts on patient outcomes in those presenting with febrile neutropenia. Further large-scale studies investigating time to antibiotic administration during NS shortages are warranted to elucidate the impact of resource limitations on timely care delivery and to guide the development of evidence-based contingency plans that preserve treatment quality.
Footnotes
Acknowledgements
None.
Authors’ Note
The findings of this research article were previously presented as a poster at the 2025 School of Medicine Greenville Annual Research Symposium.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
