Abstract
Objective:
This review evaluated the impact of a digitized computerized prescriber order entry (CPOE) system and described barriers and facilitators for introducing a digitized system.
Data Sources:
A systematic literature search was conducted in PubMed, Medline, and CINAHL using keywords. Articles in English during the last 10 years were included.
Study Selection and Data Extraction:
Study selection was presented using a PRISMA flow diagram. Forty-eight studies were included. Data from the articles were presented to address each of the three objectives.
Data Synthesis:
CPOE systems improved the quality of care provided but also introduced new types of errors. Facilitating factors for implementation included leadership, stakeholder engagement, training, and user-centered design. Inadequate training, software design, changes in workload, and workflow disruptions were identified as barriers. Recommendations for implementation included dedicated training of users, user-centered design, a backup for system downtimes, and stakeholder engagement.
Conclusion:
Application of knowledge of the facilitators and barriers for the introduction of a CPOE system supports this change-management process within the specific context and augurs for more successful implementation.
Introduction
A computerized prescriber order entry (CPOE) system is a type of automation machinery specifically designed to assist prescribers in the ordering of medicines or patient services, and for providing instructions via a predefined set of rules.1,2 The literature showed that the implementation of a CPOE system resulted in a reduction in prescription and transcription errors, and enhanced real-time reactions to medication-related problems through an alert system. 3 Moreover, using a CPOE system minimized medication errors (MEs) by a maximum of 75% and adverse drug events (ADEs) by 80%, with an error severity between 97% and 100%. 4 CPOE systems resulted in rework reductions, a decreased incidence of MEs that cause harm of 2.2% and 0.1% compared with 30.6% and 4.2% for handwritten orders, 5 and reduced duplication of work by staff. 6
Digitization or digital technology is the procedural change from physical information to electronic. Digitalization encompasses the entire process. The introduction of new technologies, including the digitalization of new processes, brings about change, and such change needs to be managed. 7 This change involves the need for the relevant stakeholders to alter their processes and interact in relation to the digitized systems implemented. The theories of implementation focus on giving a reason and explaining why and in what way an implementation succeeds or fails. Implementation theory includes describing the process model, implementation assessments, and evaluating the outcomes of an implementation. 8 Whenever a new system or process is implemented in an organization, inevitably it brings about change. An innovation may not always be adopted because change may not be accepted due to barriers.
Rationale
This literature review evaluated what change models were used to support the implementation of a digitalized CPOE system in health, the impact of a digitized CPOE system, and described the barriers and motivators for introducing a digitized system. For the purpose of this publication, the focus will be on the impacts, barriers, and facilitators.
Methodology
A protocol was developed to conduct a systematic literature search. Questions were formulated and eligibility criteria were set to identify the relevant studies based on the population, concept, and context. Google Scholar was used to pretest words and help generate keywords. The following keywords/combinations were used: (1) “change management”; (2) “change management model” or “change management framework” or “change model” or “change framework”; (3) “e-readiness” or “information systems” or “HIS” or “health information technology” or “HIT” or “information technology” or “health technology” or “e-health” or “digit*”; (4) “computerized provider order entry” or “CPOE”; (5) “barrier*” or “resistance” or “readiness” or “facilitator*.”
A systematic literature search was conducted using the following databases: PubMed, Medline, and CINAHL. The information on the identified articles was presented using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram, 9 and the results were reported (Figure 1).

Prisma flow diagram.
The main inclusion criteria considered were articles in English during the last 10 years. The removal of duplicates from the three databases was done electronically using RefWorks. Forty-eight articles were identified in the study. Details of these articles are presented in Appendix I. These studies were mainly case studies (48%), systematic reviews (16.7%), literature reviews (10.4%), and cross-sectional studies (8.3%). The remaining studies (16.6%) consisted of retrospective, qualitative, and longitudinal studies and reports. The studies were carried out in various countries spanning different continents: Asia (22.9%), Australia (2.1%), Europe (14.6%), Canada and North America (58.3%), and South America (2.1%).
Findings
Impact of Digitalization on the Process/System
From the studies identified in the literature review, 32 articles addressed the impact of CPOE on the process/system (Table 1).
Studies on the impact of CPOE systems on the process/system.
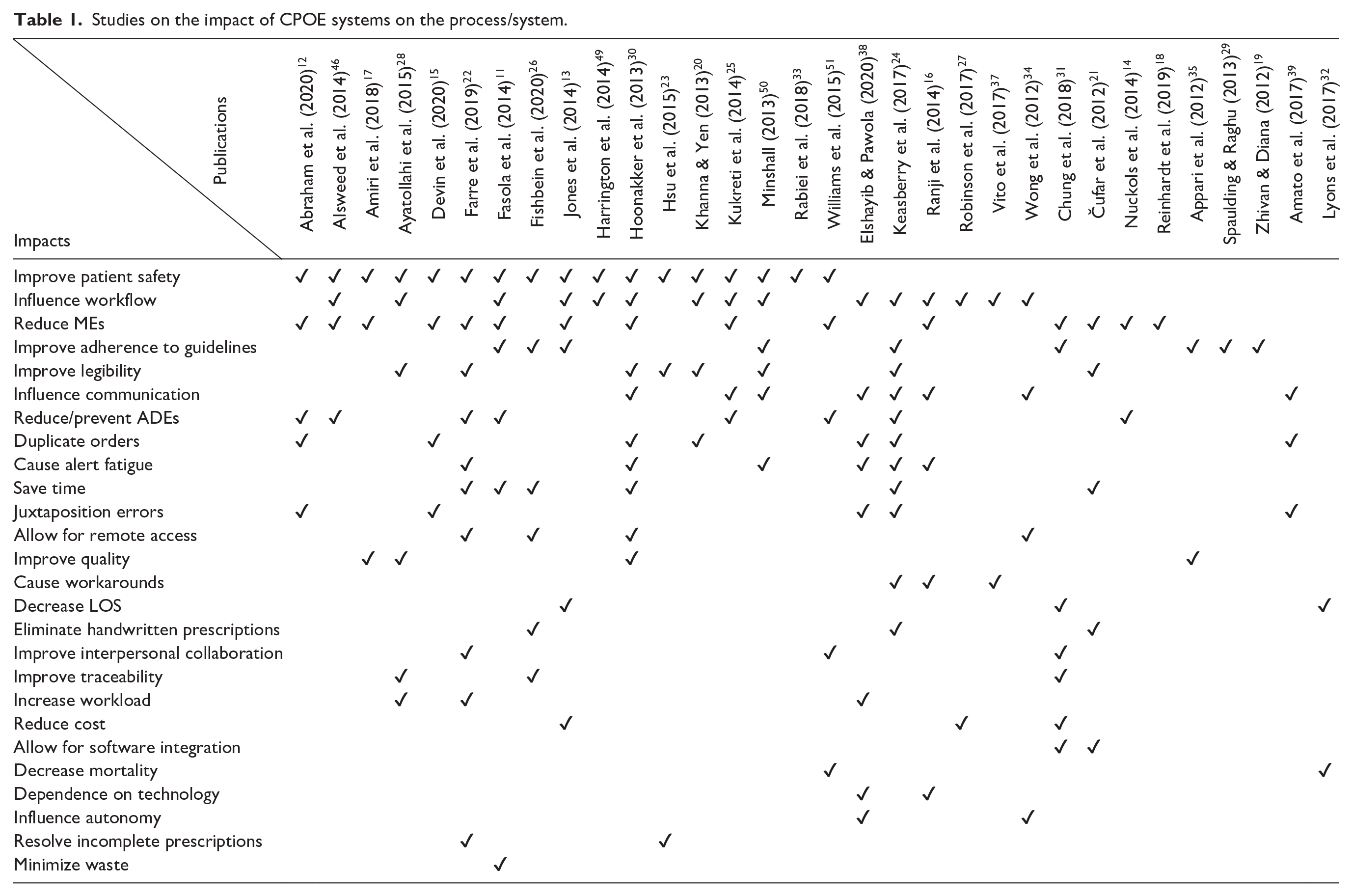
Using a multidisciplinary approach for the planning and decision making was a crucial step for strategic development because it ensured all the aspects of the workflow. 10 A properly developed health information technology ensured a better managed service, saved time, and reduced costs. A CPOE system that is paired with a drug-processing unit allowed for reduced waste and substantial cost savings. At the pharmacy level, a CPOE allowed for a higher number of orders processed per hour, leading to improved workflow and a better allocation of pharmacists. 11
Advantages of a CPOE System for the Process/System
The literature indicated that the introduction of a CPOE system decreases MEs by 75% 4 through medication ordering 12 and automated dose calculations resulting in a reduction in errors by 37% to 80%. 13 Systematic reviews found a significant reduction in ADEs with a relative risk reduction of between 35% and 53%. 12 Nuckols et al. 14 showed that a CPOE system would reduce preventable ADEs by half when compared with manual systems. A systematic review by Devin et al. 15 found that implementing a CPOE system resulted in a reduction in prescription errors, but a narrative review by Ranji et al. 16 reported that ADEs were not affected.
CPOE systems were shown to improve the quality of care provided.14,17 –19 Findings from a case study suggested that CPOE systems are aligned toward improving the quality of care, whereas electronic medical record (EMR) systems are more appropriate for improving inefficient systems. 19 Other studies indicated that CPOE systems improved legibility due to the removal of handwritten orders,20,21 ensured that prescriptions were complete,13,22 –24 and improved the quality of patient care. 25 Following research on physician perspectives, Fishbein et al. 26 showed that there was a positive impact on workflow mainly due to efficiency when placing orders, accessibility, and a greater adherence to guidelines.
CPOE systems reduced cost by minimizing waste, 11 by decreasing the number of labor hours, 27 and by reducing duplication. 28 Moreover, CPOE systems were associated with increased process compliance, 29 facilitated traceability by enabling easier access to patient information, 30 increased adherence to guidelines, 24 improved communication between stakeholders, 31 and minimization of legal issues. 23 The results related to length of stay (LOS) were inconsistent. A CPOE system was found to decrease the LOS by 0.92 days 32 ; in contrast, a systematic review by Keasberry et al. 24 found that a CPOE system would not reduce LOS. The results related to mortality also were contrasting. A CPOE system was found to decrease mortality by 1.75% 32 ; in contrast, a systematic review by Keasberry et al. 24 found that a CPOE system would not reduce mortality. A systematic review by Abraham et al. 12 found a variety of results in mortality ranging from no significant change to different decreases with use of CPOE systems. Unless adequately designed, a CPOE system could increase LOS, MEs, and costs. 33
A CPOE system could reduce manual tasks by half 21 and enable prescriptions to be accessed remotely, 22 allowing the physicians to avoid returning to a patient’s bedside to discover any new information. 15 In addition, a CPOE system enables the use of a barcode system, thus reducing the need for transcribing and minimizing the workload. 21 This integration also enables result monitoring and data sharing between users. 11
Disadvantages of a CPOE System
The weaknesses of a CPOE system were categorized as being an increased workload for both nurses and physicians and interface problems that resulted in inefficiencies due to the complexity of the software to complete prescriptions, thus increasing the time required throughout all phases of the medication process22,28,30 and increasing physician responsibilities. 20 The average time to fill a prescription on a CPOE system was longer than manually prescribing it, with a statistically significant increase in time of 5.14 minutes. 25 Wong et al. 34 reported that although there was an increase in time, this allowed for time savings during medication reviews, which could be allocated to training and teaching.
A retrospective study by Appari et al. 35 suggested that hospitals that adopted a CPOE system alone had no significant difference regarding adherence to medication administration when compared with hospitals that did not adopt a CPOE system. Inefficiencies in a process can lead to workarounds whereby personnel compensate for lack of resources by bypassing the steps they consider as obstacles. 36 Integrating a CPOE system with an EMR system resulted in staff developing workarounds due to workflow implications. 37
Introducing a CPOE system would bring new kinds of errors, and the impact would be an increase in workload, process inconsistencies, ongoing support systems, a reduction in autonomy, 34 and greater dependence on technology. 38 Following an assessment of 2522 MEs, the study by Amato et al. 39 found that the most common errors with the CPOE ordering system included communication errors, wrong medication dosages, and duplicate orders. The reasons for such errors were attributed to five categories of problems: (1) system issues, (2) lack of adherence to policies, (3) lack of communication, (4) inadequate medication reconciliation, and (5) the clinical decision support system not being integrated into the CPOE system. Another problem with CPOE systems is juxtaposition errors, which consist of selecting the wrong patient, drug, or dose when entering orders.24,38 A cross-sectional study by Hoonakker et al. 30 indicated that a CPOE system decreased communication between physicians and nurses because when physicians wrote orders, they no longer communicate them directly to nurses.
Barriers and Motivators for Introduction of a CPOE System
Fourteen of the articles included in this study addressed this question. Barriers and motivators for introducing a digitized system were grouped separately, and recommendations were established.
Motivators
Motivators are defined as factors that facilitate the implementation of change. The most common motivators for successful implementation of a digitized system were governance, stakeholder engagement, training, and having a user-centered design (Table 2).
Motivators of a CPOE system.

Perceived usefulness and perceived ease of use are two factors required for adopting and using a system. When stakeholders perceive a system as useful, they are more inclined to adopt and use it.40,41 The perceived usefulness would improve the user’s insight into the importance of using it, whereas the perceived ease of use would impact their behavioral intention to use it.40,42,43
Engagement should start with the planning and move through implementation and also must include training. 44 Piloting before implementing the system allows for an improved transition and identifies system errors, but this carries the risk of having two systems running simultaneously. However, this can minimize the transition. 22 User engagement allows for tailoring of the system according to users’ needs and minimizes workarounds. 45 For users to use a CPOE system successfully, adequate training is required. Proper training of healthcare professionals (HCPs) on the use of CPOE systems influenced various aspects of clinical work, including a reduction of MEs with a standard deviation of 2.58 ± 0.55 and improved nursing workflow, enabling more time for patient care, 46 thus improving patient safety. In addition, having continued training allows one to develop and improve new skills by having champions within the organization who can help their colleagues 45 and bridge information flow with the supplier. 38 Training helps in building good relationships within the organization by identifying and anticipating problems, resulting in better resource estimating and the setting of time frames. 22 Effective communication from the management to the involved stakeholders on digitized interventions should be presented in a nonthreatening environment, and the impacts would be reduced resistance and greater buy-in. 44
Barriers
Barriers are defined as the factors that prevent the implementation of change. The most common barriers to a digitized system are presented in Table 3 and included the training provided, software design, and the change in workload.
Barriers of a CPOE System.

Certain factors were found to contribute to CPOE system–related medication errors. These included flaws in the interface design, issues with alerts, and loss of orders. 38 Stakeholders resist new technologies when they are perceived to negatively influence patient safety or increase their workload. 45
Lin et al. 41 found that perceived threat is considered a key inhibitor in the adoption of technology. A longer time requirement when using a CPOE system compared with a manual system was identified to be the greatest barrier. 10 Lack of resources during the implementation was found to be a potential barrier that could be counteracted by proactive planning and tailoring of workflows. 10 The literature review by Fasola et al. 11 did not conclude whether use of health information technology is timesaving.
System crashes resulted in all unsaved data being lost and having physicians redo the work, therefore increasing the work. 43 When a digitized system is implemented, software stability must be considered. Having complex systems requires excessive changes in workflow, and stakeholders perceive this as a hindrance. 40 Lacking the required knowledge and experience results in underestimating the resources required to implement a system.10,47
Proposals and implementation of change lead to extra work and other problems for relevant stakeholders, and this brings about resistance from those concerned. If the digitized system is incompatible with current practices, the change can be perceived negatively. 41
Delays in implementation can be the result of internal factors (e.g., lack of planning, poor training, and shortage of human resources) and external factors (e.g., supplier obligations and organizational structure). 47 Workflow interruptions cause inconvenience. Thus, management should ensure that unnecessary steps are removed for stakeholders to minimize resistance and allow them to adopt the change. 22 The absence of an information technology infrastructure would result in workflow disruptions due to the lack of system interoperability, work duplication, and information transfer. 22 Workflow disruption may result in changes in administration practices and an increased number of requests received by the pharmacy. This would lead to an increase in workload and reduced pharmacy clinical practice. 10 Software stringency is another barrier that users identified as a limiting factor. 44 Requiring the supplier to customize the interface to be compatible with current systems could cause delays in implementation. 47
Physicians resist adopting digitized systems because they perceive the change to increase their costs, workload, and liabilities while minimizing their privacy. 42 Age was identified as a barrier because older physicians required a longer time to become accustomed to the system, complaining that the system was too complex 44 or that the provided training was not tailored to seniors. 43
If management does not have a comprehensive project plan, the result would be an inaccurate implementation timeline. 47 Communication has been found to influence adoption, and when management does not use appropriate methods for effective communication, physicians may resist adopting the system. 44
Recommendations for Implementation of a CPOE System
By tackling the potential barriers to a CPOE system, a healthcare organization is in a better position to achieve success and support from stakeholders during implementation. 2 A user-centered design should be adopted to meet stakeholders’ needs, avoid delays and resistance, and increase system interactivity.38,42 Stakeholder engagement enables the detection of users’ needs, and steps could be taken to address them, thus increasing acceptance. 38 A strategy to overcome implementation barriers is required. This should assess the hardware and software requirements and evaluate the process workflow to design and customize them in accordance with those processes. 10 Because excessive alerts lead to fatigue, a continuous process redesign of existing CPOE systems is required to minimize such alerts and improve the integration into physician workflows. 48
If a system were perceived by HCPs to positively influence workflow and patient safety, there would be a higher degree of acceptance. Similarly, if a system were perceived by HCPs to negatively influence workflow and patient safety, resistance would occur. 45 As a result, it is recommended that user engagement and a user-centered design be developed to strategically create a system to give users a sense of ownership.
For any implementation, management support is needed.22,42 Implementing a user-centered design software can enable the system to have improved specificity, thus reducing alert fatigue. 38 Having software flexibility allows for adoption in accordance with users’ needs. 43 Governance should involve the creation of a committee or a stakeholder group and should consist of a team of multidisciplinary stakeholders. 49 Committees allow for pathway development and ensure that users’ needs are met.10,22 The pathway development should consist of a roadmap for the implementation to go according to plan 42 and policies to address the workflow changes. 49
Adequate training is critical for a successful CPOE system because lack of dedicated training would result in an increase in MEs. 31 Because most medical schools do not train medical students on the use of electronic systems, a CPOE system might be too complex to use, increasing physician workload and stress. 11 It is suggested that medical schools engage in teaching students on electronic software and how to use it. Training of personnel should involve explanations of jargon and software commands to minimize frustration and motivate staff. 42 Continuous training is important to accommodate software changes and/or updates. Having super users who can train and teach their colleagues has been a successful way to achieve continuous training. 45 Nurses who had training or a background knowledge of computers felt higher comfort, and this is important because the more uncomfortable staff feel with the technology, the less likely they are to adopt it. 42
As users become dependent on the technology of a CPOE system, their manual skills may start deteriorating. Thus, a backup system should be set up to be available when there is system downtime.24,49
Limitations of the Review
The literature search was carried out using three databases, and the inclusion and exclusion criteria focused on articles published in English during the previous 10 years. This may have resulted in missing out on some important literature. Data extraction was conducted by one researcher, and this could have introduced an element of bias.
Conclusion
The literature showed that a CPOE system can have positive and negative impacts, and it is therefore recommended that prior to the introduction of such a system, a hospital should do a thorough evaluation based on the way in which the factors impact its specific situation. The literature showed various motivators and barriers for the introduction of a CPOE system, and what is a motivator for one entity can be a barrier for another depending on the availability of resources and on the perceptions of the staff involved. Mapping of motivators and barriers as applicable to the respective entity will help in increasing the readiness of the entity to adopt and implement a CPOE system. Communication with all the relevant stakeholders is key. It is suggested that a change-management model be developed for implementing a digitalized CPOE system.
Supplemental Material
sj-docx-1-pmt-10.1177_87551225241284919 – Supplemental material for Implementation of Computerized Prescriber Order Entry Systems: A Review of Impacts, Barriers, and Facilitators
Supplemental material, sj-docx-1-pmt-10.1177_87551225241284919 for Implementation of Computerized Prescriber Order Entry Systems: A Review of Impacts, Barriers, and Facilitators by Ian Farrugia and Patricia Vella Bonanno in Journal of Pharmacy Technology
Footnotes
Declaration of Conflicting Interests
The author(s) declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
