Abstract
Background:
Screening model-based risk stratification tools, such as American Diabetes Association (ADA) diabetes risk scoring are useful in increasing awareness toward one’s risk of developing Diabetes mellitus (DM) or prediabetes. The application of ADA risk score in the Asian population might have limitations.
Objective:
To evaluate (a) the scope of the existing ADA score in screening Indian population and (b) the incorporation of epidemiologically relevant factors in enhancing the sensitivity of the scoring system for a population-wide screen.
Methods:
A prospective observational study was conducted among adults with normoglycemia, a history of T2DM or prediabetes. Diabetes risk scores, with and without modifications of factors including age, BMI, and abdominal obesity based on Indian-specific criteria were calculated. The sensitivity was evaluated after incorporating each modification and with simultaneous incorporation of all modifications (Bharat Risk Score for Dysglycemia [BRS-D] scoring system).
Results:
Among 723 individuals screened, 101 participants had a history of DM, and 18 participants without a history of diabetes had a capillary glucose level ≥200 mg/dl. The sensitivity of the ADA scoring system with the standard ADA score (≥5) was 86.6%. With the inclusion of the modifications, the sensitivity of the scoring system increased: 91.6% (age), 90.8% (waist circumference) and 89.1% (BMI), 93.3% (all modifications).
Conclusion:
The application of population-specific criteria to the standard ADA scoring system could improve sensitivity. The proposed BRS-D scoring system can be a versatile tool that will enable large-scale screening to identify high-risk individuals for diabetes among, the Indian population.
Introduction
Screening model-based risk stratification tools are useful in increasing awareness toward an individual’s risk of developing Type 2 Diabetes mellitus (T2DM) or prediabetes. One such tool is the American Diabetes Association (ADA) risk screening model that calculates a score on a scale of 0 to 10 based on seven parameters: age, sex, height and weight, family history of T2DM, history of gestational DM, history of hypertension (HTN) and physical activity. The minimum cut-off score for identifying high-risk individuals is 5, and higher scores are associated with an increased chance of developing diabetes. 1 Validation of scoring has provided wide sensitivity ranges (36.8%–88.2%) among different ethnic populations.2–5 However, the application of ADA diabetes risk scoring in the Indian population might have limitations in terms of sensitivity due to the influence of population-specific risk factors associated with DM pathophysiology. While the ADA diabetes risk score considers an age cut-off >40 years as a risk for DM, a large country-wide study from India observed a sharp increase in T2DM incidence at an earlier age of 35 years. 6 The second major difference is in terms of the obesity parameters included in the risk screening system. Recently, the US Preventive Services Task Force recommended screening for prediabetes and T2DM among overweight or obese adults aged 35 or older. 7 The BMI classification for the South-Asian population varies from the criteria used for the Western population with a lower BMI cut-off defining the Indian overweight to obese population (11). 11 India has one of the highest prevalences of DM (39% vs. 11.9–21.1%), which is attributable to the partial lipodystrophy observed with abdominal obesity.9,10 Abdominal obesity is an independent risk factor for T2DM. 8 Focusing on women, young women with a history of polycystic ovary syndrome (PCOS) have been associated with a significantly higher risk of diabetes [HR: 5.13 (95% CI: 3.51–7.48)]. 12 Hence, there is a need for modification of the ADA risk scoring system by tailoring it to the risk factors associated with the pathophysiology of DM in specific populations. Accordingly, the study aims to evaluate: (a) the scope of the existing ADA scale in screening for the risk of diabetes in the Indian population and (b) the incorporation of epidemiologically relevant factors in enhancing the sensitivity of the scoring system for population-wide screening.
Methodology
A prospective observational study was conducted among a random group of individuals visiting a tertiary care facility in Bangalore and Kanpur. The study involved the analysis of data that were already collected as part of routine clinical care and not specifically for research purposes. As such, no additional burden or risk was placed on the patients. We strictly adhered to ethical principles and data protection standards. This included ensuring data security, maintaining confidentiality, and following ethical guidelines for conducting retrospective research.
The study population included adults (>18 years of age) with normoglycemia or a history of T2DM (<1-year duration) or a history of prediabetes and not under any treatment. Exclusion criteria included individuals with diabetes on Sodium-Glucose Transport Protein 2 Inhibitors (SGLT2i), Glucagon-like peptide-1 (GLP1) agonists, Sulphonyl urea (SU), Glitazones, with hypertension requiring more than three drugs, with endocrinological disorders which might interfere such as Cushing’s syndrome, acromegaly, uncontrolled hypothyroidism or thyrotoxicosis, or current diagnosis of malignancy, known chronic kidney disease, chronic liver disease, congestive heart failure, retroviral disease or pregnant women. The ADA risk score was adopted from Bang et al., 2009 (Table 1). 13 Demographic information (such as age, gender), BMI, history of gestational diabetes mellitus (GDM), hypertension, family history of DM, and daily physical activity (of at least 30 mins) were collected. An automated blood pressure monitor was employed and those with blood pressure of 140/90 (Systolic blood pressure [SBP]/Diastolic blood pressure [DBP]) mmHg or higher were considered hypertensive. The waist circumference was estimated by placing the measuring tape around the lateral aspect of each ilium at the mid-axillary line. A finger prick was conducted to obtain a capillary blood sample for glucose test from the participant and ISO-certified glucometers such as iSense, Accucheck performa, OneTouch were used to estimate the blood glucose level. 14 History of known diabetes, capillary glucose level 140–199 mg/dl (suggestive of prediabetes) or capillary glucose level ≥200 mg/dl (suggestive of diabetes) were used for study analytical purposes. 15
Comparison of ADA Diabetes Risk Score 13 and BRS-D Scoring System.
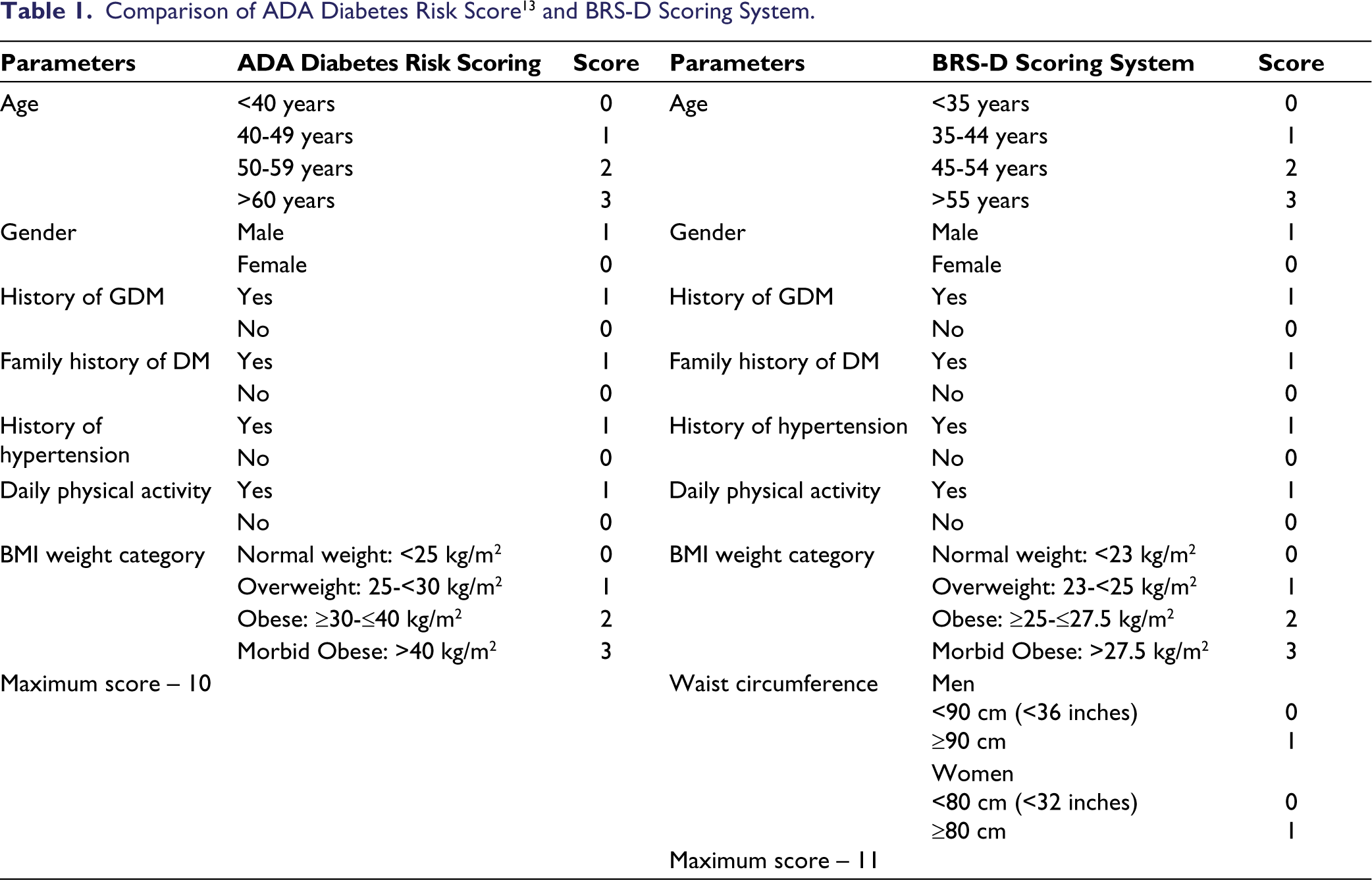
Modifying Factors Considered
The ADA diabetes risk scoring system was modified to account for recent recommendations and factors associated with the Indian diabetes phenotype (named Bharat Risk Score for Dysglycemia – BRS-D). The improvement in the sensitivity of the ADA risk score was determined by sequential refinement of the scoring system. Initially, the age limit for risk of Dysglycemia was reduced to 35 years from 40 years. This was followed by adjustments made to the BMI criteria to align with the Asian BMI categorization (Table 1). Next, for determining abdominal obesity, a criterion for waist circumference (Men ≥ 90 cm; Women ≥ 80 cm) was added to the scoring system (Table 1). The sensitivity of the scoring system was evaluated after each modification. Finally, all the modifications were incorporated and the sensitivity of the modified risk score BRS-D was estimated at a cut-off range between 4 and 7 (Standard ADA cut-off considered for screening is 5).
Data Analysis
The data was collected and deposited in an Excel spreadsheet. Individuals without a history of diabetes or RBS score were excluded from the analysis. Patient records missing information for even one of the factors for the risk score were not included for the analysis. For the sensitivity and specificity calculation, the study population was divided into diabetes (with a known history of diabetes or RBS score ≥200 mg/dl) and non-diabetes. The categorical variables were presented as n (%) and the continuous variables were expressed as mean ± SD. The sensitivity, specificity, positive predictive value, and negative predictive value were estimated after each modification was made to the standard ADA scoring system as well as with the inclusion of all modifications (BRS-D scoring system).
Sensitivity = True positive ÷ True positive + False negative
Specificity = True negative ÷ True negative + False positive
Positive predictive value = True positive ÷ True positive + False negative
Negative predictive value = True negative ÷ True negative + False negative
Results
The study population consisted of 723 participants with a mean age of 42.0 years with a male-to-female ratio of 1.18 (Table 2). The diabetes group consisted of 101 participants (14.0%) of the screened individuals who had a history of DM, 17 participants with no history of diabetes had an RBS score >200 mg/dl. Table 1 displays the demographic variables of the study participants. Half (50.8%) of the participants were obese (BMI > 25 kg/m2) and 10.1% had a history of hypertension (Table 2). Waist circumference indicative of abdominal obesity was observed in 68.0% of men and 93.2% of women (Table 2).
Demographics of the Study Population.
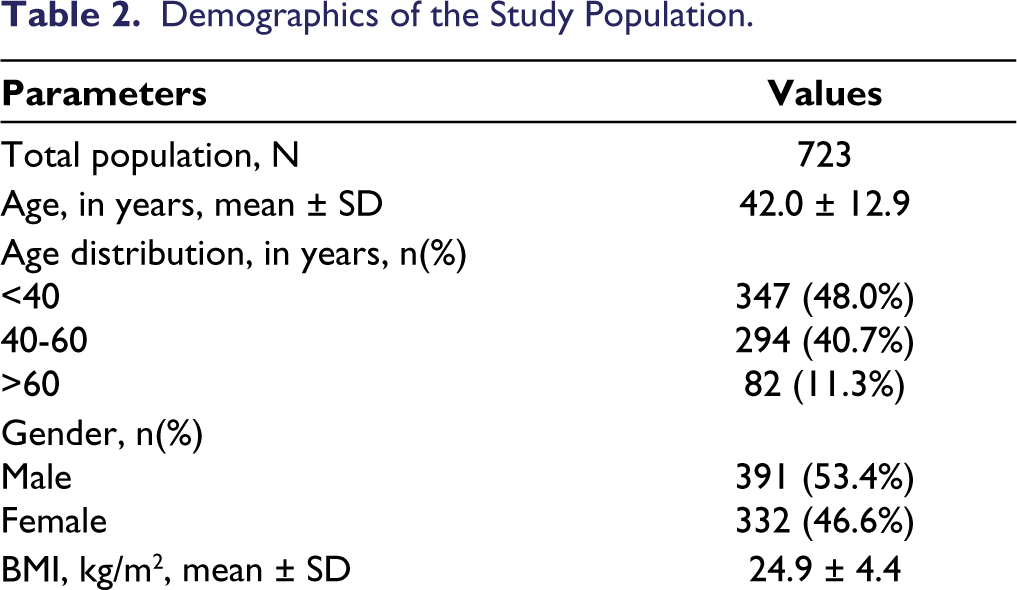
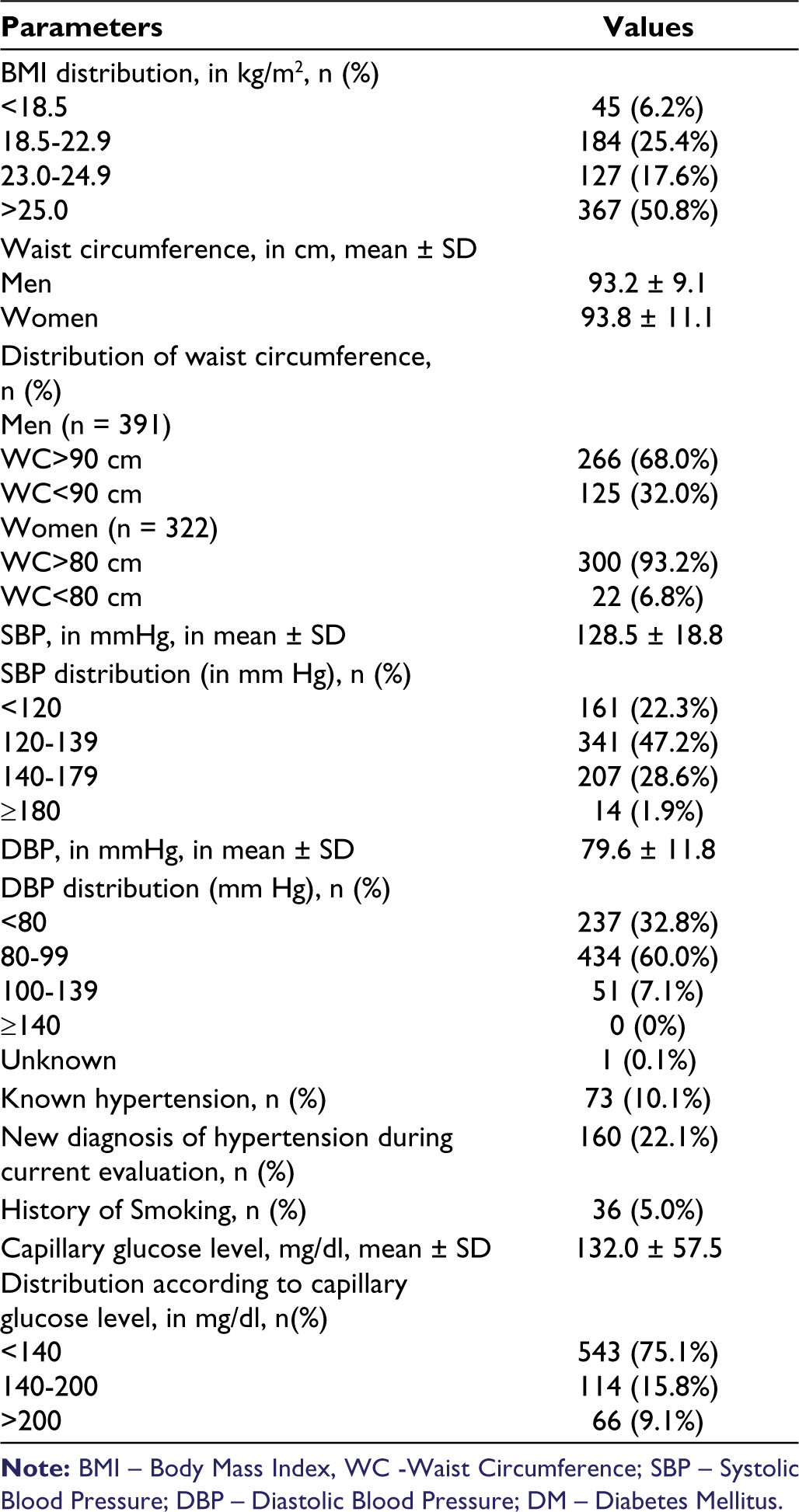
When applied to the Indian population, the ADA diabetes risk scoring system had a sensitivity of 57.1%, 76.5%, 86.6% and 96.6% at cut-offs of 7, 6, 5 and 4 respectively. The specificity of the ADA risk scoring at cut-offs of 4, 5, 6 and 7 were 29.8%, 43.0%, 60.6%, 77.8%, respectively. Modifying the criteria in variables including age, WC, and BMI, we observe an increase in sensitivity with respect to the ADA diabetes risk scoring. At cut-off of 5, sensitivity increased with age criteria modification (86.6%-91.6%), addition of WC (86.6%-90.8%) and BMI criteria modification (86.6%-89.1%) and age + BMI (86.6%-92.4%), age + WC (86.6%-93.3%), BMI + WC (86.6%-90.8%), and all modifications (86.6%-93.3%) (Table 2). The specificity, PPV and negative predictive value (NPV) of the scoring system with modifications are presented in Table 3.
Sensitivity, Specificity, Positive Predictive Value, and Negative Predictive Value of the Scoring Systems with Modifications.
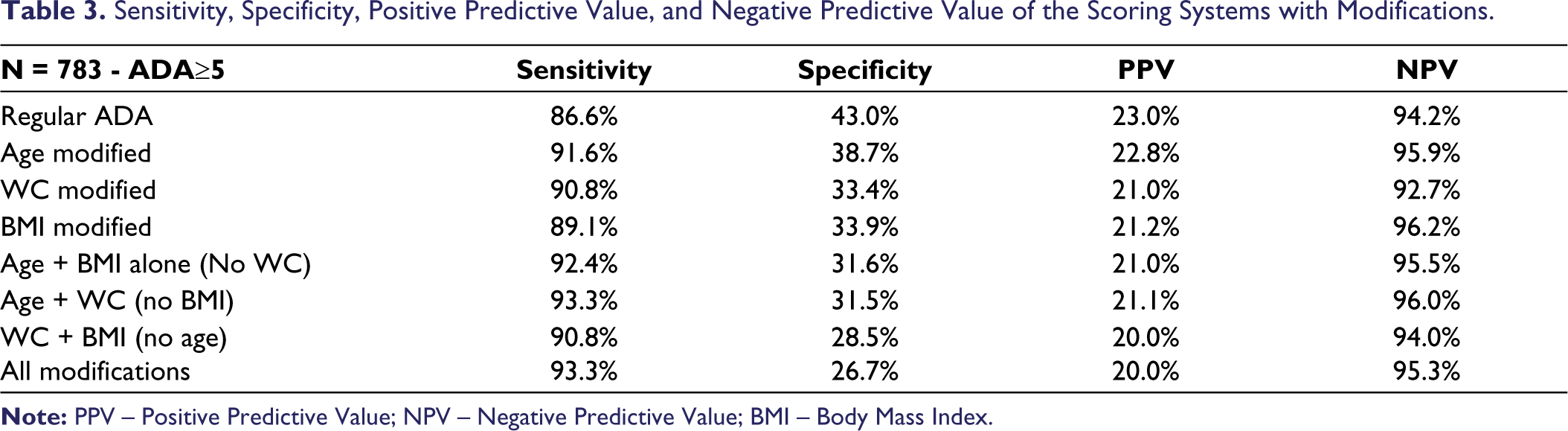
In the study population, 86 (11.9%) participants were indicative of prediabetes (capillary glucose of 140–200 mg/dl and no history of diabetes). The ADA score identified 75/86 (87.2%) and 68/86 (79.1%) individuals at high risk for prediabetes (cut-off ≥ 4), and diabetes (cut-off ≥ 5), respectively. The BRS-D system identified 82/86 (95.3%) and 77/86 (89.5%) individuals at high risk for prediabetes (cut-off ≥ 4) and diabetes (cut-off ≥ 5), respectively. Eighteen participants (2.3%) had capillary glucose ≥200 mg/dl. Fifteen participants (15/18–83.4%) were identified as having a high risk for diabetes according to standard ADA risk scoring. Seventeen individuals (94.4%) were at high risk of T2DM according to the BRS-D scoring system.
Discussion
The burden imposed by T2DM is largely attributable to its high prevalence. Furthermore, the commonness of latency of T2DM adds to the risk of microvascular and macrovascular complications of T2DM and therefore requires early risk stratification. The current study of 723 individuals evaluated the applicability of the standard ADA risk scoring in the Indian population. The sensitivity of the standard ADA scoring system (at cut-off ≥ 5) in the Indian population was 86.6%, with a specificity of 43.0%. Modifying the standard ADA scoring system to cater to the Indian population by adjusting the criteria for age, BMI, and adding WC measures improved the sensitivity of the scoring system (at cut-off ≥ 5) from 86.6% to 91.6%, 89.1%, and 90.8%, respectively. Inclusion of all the modifications (BRS-D scale), the sensitivity of the scoring system improved to 93.3% (from 86.6%).
Risk scores assessed using risk screening tools are dynamic as they rely on demographic parameters such as age, BMI and lifestyle habits that tend to change with time therefore, they have a contemporary value, especially in creating awareness and directing individuals to implement lifestyle measures in a timely manner in a diverse sociodemographic population with varying lifestyle habits and practices. Such scoring systems must take into account epidemiological variables for effective large-scale screening. Previous research in Egyptian, Hispanic and Indonesian populations has observed the sensitivity of the ADA scoring system (at a cut-off ≥ 5) to lie in the range of 66%-88.2%.2–4 In the present study, the standard ADA diabetes risk scoring system (at a cut-off ≥ 5) revealed sensitivity and specificity of 86.6% and 43.0%. One of the strategies employed to increase the sensitivity involved lowering the cut-off of the standard ADA risk score. In this study, reducing the cut-off to 4, maximized the sensitivity of the scoring system to 96.6%, while reducing the specificity to 29.8%. Similarly, increasing the cut-off to 6 and 7 improved the specificity to 60.6% and 77.8%, and reduced the sensitivity to 76.5% and 57.1%, respectively. Screening tests are not diagnostic in nature and are purposed to identify individuals who have a high likelihood of having or developing a disease. Therefore, these tests must prioritize high sensitivity to identify high-risk individuals while balancing specificity to reduce the proportion of false positives. The optimal cut-off was estimated to be 5 (Sensitivity– 86.6%; Specificity– 43.0%). A study employing the ADA diabetes risk score estimated a sensitivity of 36.8% in the Indian population. 5 This substantial difference in the sensitivity (86.6% vs. 36.8%) could stem from the differences in the methodology and the complex sociodemographic of the Indian population.
To enhance the applicability of the ADA risk scoring system in the Indian population, this study considered three major modifications including: (a) age criteria of 35 years; (b) the application of Asian BMI criteria and (c) the inclusion of waist circumference. Relative to the Western age cut-off of 40 years, the onset of DM among the Indian population has been as early as 35 years (6). With this age cut-off, the sensitivity increased to (86.6%-91.6%; Table 3). Since the Asian BMI criteria for overweight and obesity is lower than the Western criteria, the standard ADA score will tend to miss a substantial proportion of overweight, obese individuals during screening. This is reflected as an improvement in the sensitivity of the scores from 86.6% to 89.1% when modified for BMI (Table 3). Additionally, another independent association is the WC. The Thin-fat Indian T2DM phenotype is associated with increased abdominal obesity.8,9 Lipodystrophy in abdominal obesity has been observed to increase the risk of T2DM in the Indian population. 9 Therefore, the waist circumference parameter was added to the ADA diabetes risk scoring. The addition of WC to ADA diabetes risk scoring improved the sensitivity of the scoring system (86.6%–90.8%; Table 3). When all these modifications were applied (BRS-D scoring system), the sensitivity improved from 86.6% to 93.3% (Table 3). These risk factors, in addition to diabetes, may also play a crucial role in risk stratification of individuals for cardiovascular illnesses.
Among the screened individuals, 86 (11.9%) participants were indicative of prediabetes (capillary glucose of 140–199 mg/dl). The ADA score identified 75/86 (87.2%) and 68/86 (79.1%) individuals at high risk for prediabetes (cut-off ≥ 4), and diabetes (cut-off ≥ 5), respectively. The BRS-D system identified 82/86 (95.3%) and 77/86 (89.5%) individuals at high risk for prediabetes (cut-off ≥ 4) and diabetes (cut-off ≥ 5), respectively. Among individuals without a history of DM, 18 (2.3%) participants had a capillary glucose values ≥200 mg/dl. Among them, the BRS- D scoring identified 94.4% (17/18) to have a risk score ≥5, indicative of high risk for DM compared to 83.4% (15/18) by the standard ADA risk scoring. In India, more than 50% of individuals with diabetes are estimated to be undiagnosed or are unaware of their diabetes status. 16 The implementation of a quick self-assessing screening tool accounting for epidemiological factors, like the BRS-D scoring system, may prove to be effective in increasing awareness toward prediabetes and undiagnosed diabetes in the Indian population.
The ADA risk scoring system also takes into account gender-based risk factors. Specifically, it considers gestational diabetes in women. However, PCOS among younger women has also emerged to be a major risk factor associated with the metabolic syndrome cluster. Almost half the women with PCOS are expected to develop T2DM by the age of 40. 17 In a decade long follow—up study, the risk of T2DM was significantly higher among women with PCOS [HR: 5.13 (95% CI: 3.51–7.48)] than women without PCOS. 12 The risk was alarming high among women in the younger ages, with adjusted HR being 10.4, 5.28 and 4.06 in 18–24-, 25–29- and 29–34-year age groups respectively. 12 Despite the significant impact of PCOS in T2DM development, the current ADA diabetes risk scoring system does not include PCOS as a risk factor. Due to the limitation of the lack of available data, the BRS-D scoring could not take into account PCOS in women. This will be considered as an important factor in future studies. Although there are additional risk factors for T2DM, the self-assessment nature does not allow the inclusion of these factors in the scoring system.
In conclusion, the current study highlights the importance and need for adapting and validating risk-scoring systems to different ethnic populations. By accounting for population-specific factors, the current study enhanced the sensitivity of the ADA scoring system. Implementation of the BRS-D may assist in early and effective identification of individuals with prediabetes, T2DM and those at high risk for these conditions within the Indian population. Using BRS-D may be a cost-effective alternative approach for population-wide screening for risk of diabetes and prediabetes compared to conducting biochemical tests such as Oral Glucose Tolerance Test. The reduced specificity of the scoring system may be attributed to the self-reported status of diabetes and utilization of capillary glucose estimates for determining unknown diabetes in the study population. Random blood sugar value varies throughout the day and is highly influenced by factors including type and time of food and medication intake, physical activity, and stress, and hence may not reflect the actual status of T2DM in the study population. Large-scale studies with more robust diagnostic measures of T2DM status, that is, HbA1c may provide more insights into the applicability of the BRS-D in the Indian population. Nevertheless, as it is a self-administrable screening tool for risk assessment, it provides additional value for creating awareness among the public and provides an opportunity for public health intervention.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Statement of Ethical Approval and Informed Consent
The study was approved by the ACE Independent Ethics Committee (Ref no: TEM-01/ SOP-03-v05). All the study participants gave their informed oral consent to participate in the study.
