Abstract
Introduction:
Diabetes mellitus (DM) has been a global public health concern for decades contributing to increasing morbidity and mortality. The glucocentric approach of management has been effective yet inadequate in achieving glycemic control and preventing complications. This called for a continuous glucose monitoring (CGM) system where the approach is patient-centric and the study was thus undertaken to explore and understand the impact of CGMS in the management of DM.
Materials and methods:
A quasi-experimental study was conducted among patients diagnosed and under treatment for DM where their clinical profile and self-monitoring of blood glucose (SMBG) levels were recorded. Two CGMS sensors—Freestyle Libre Pro (FSLP) and Freestyle Libre (FSL) were used to record their glycemic profile for a duration of 15 days each. FSLP recorded their initial profile based on which diet and lifestyle modifications were advised by healthcare providers (HCP), followed by the use of FSL.
Results:
Forty patients were enrolled for the study where 53% belonged to the age group of 50-69 years and 65% were males. More than 50% patients had DM for more than 10 years and 77.5% patients had higher HbA1c levels (6.1%–10%). The CGMS sensors showed that their overall glycemic profile was improved including their average blood glucose and HbA1c which were 33.12 and 1.12 times lower in FSL recording than FSLP (before intervention), respectively.
Conclusion:
Given the dynamics associated with glucose in diabetes, and the inadequacy of SMBG to predict all the variations, upgrading to the CGMS approach has proven to be more clinically valuable in attaining the Time-in-Range (TIR) target and improving the patient’s quality of life.
Keywords
Introduction
Diabetes mellitus (DM) has been the most common clinical condition prevalent among millions of people in both developed and developing nations of the world for the past few decades. The disease has also been the causative behind increasing mortality and disability among all age and gender diversities. Type II Diabetes Mellitus (T2DM), classically viewed as a disorder of insulin deficiency and resistance is the most common type that results in significant metabolic conditions and severe complications. 1
The International Diabetes Federation (IDF) estimated that there were 451 million people with DM worldwide in 2017 and that number is estimated to increase to 693 million by 2045 with increasing industrialization, inappropriate work-life balance, poor food habits, and sedentary lifestyle. Moreover, it was estimated that almost half of all people living with DM were still undiagnosed and this poses a great challenge to many countries’ healthcare systems and resources. 2 The progression of DM is known to be associated with several complications, such as visual loss, amputation, neuropathy, end-stage renal disease, cardiovascular disease (CVD), infections, and cognitive impairment. Although DM management has been improving, it appears to be inadequate exposing a few significant gaps that need to be addressed. 3 It has been estimated that only one-third of people with DM were able to effectively manage their disease, while more than half of these people have been reporting significant distress related to their illness and its management. 4
Management of patients with both Type 1 (T1DM) and Type 2 diabetes mellitus (T2DM) demands a comprehensive approach that includes efficient blood glucose monitoring, diabetes education, an emphasis on lifestyle modification and screening for diabetes complications ensuring achievement of good glycemic control, minimization of cardiovascular risk, and avoidance of drugs that can aggravate glucose or lipid metabolism. 5 Among them, blood glucose monitoring becomes very important for individuals with diabetes due to its determining role in medication strength adjustment and observation of possible life-threatening hypoglycemia.
Self-monitoring of blood glucose (SMBG) has been a common practice over the years; however, the system now seems to fall short of the outcomes and impact expected out of it to create better diabetes management. The self-monitoring levels recorded are time-bound and the events that led to the observation and that follow the recorded value always seem to miss out of the picture leading to an incomplete understanding of the patient profile. Individualized diabetes management is essential in today’s medical world as traditional methods are proving to be quite ineffective in controlling and managing the glucose levels of patients and in the prevention of complications. Thus, modern medicine has come up with a technologically advanced solution in the form of a continuous glucose monitoring (CGM) system, wherein, the glycemic variability can be understood better and thus managed accordingly. This study was thus undertaken to explore and understand the impact of CGM in the management of blood glucose levels among patients with a history of DM.
Objective
To explore and understand the impact of CGM in the management of glucose levels among patients with uncontrolled DM erstwhile using SMBG.
Materials and Methods
A quasi-experimental study was conducted among patients with uncontrolled DM (both types) visiting healthcare professionals (HCPs) practicing in different parts of the country. Five profiles (Figure 1) were developed based on which patients were enrolled. Their clinical profile including socio-demographic data, history of diabetes, other laboratory investigations like urea, creatinine, and lipid profile, and treatment were recorded using a standardized questionnaire, and their SMBG levels were recorded before and after every meal for 10 days before commencement of the study.
Patient Profiles Developed for the Study.
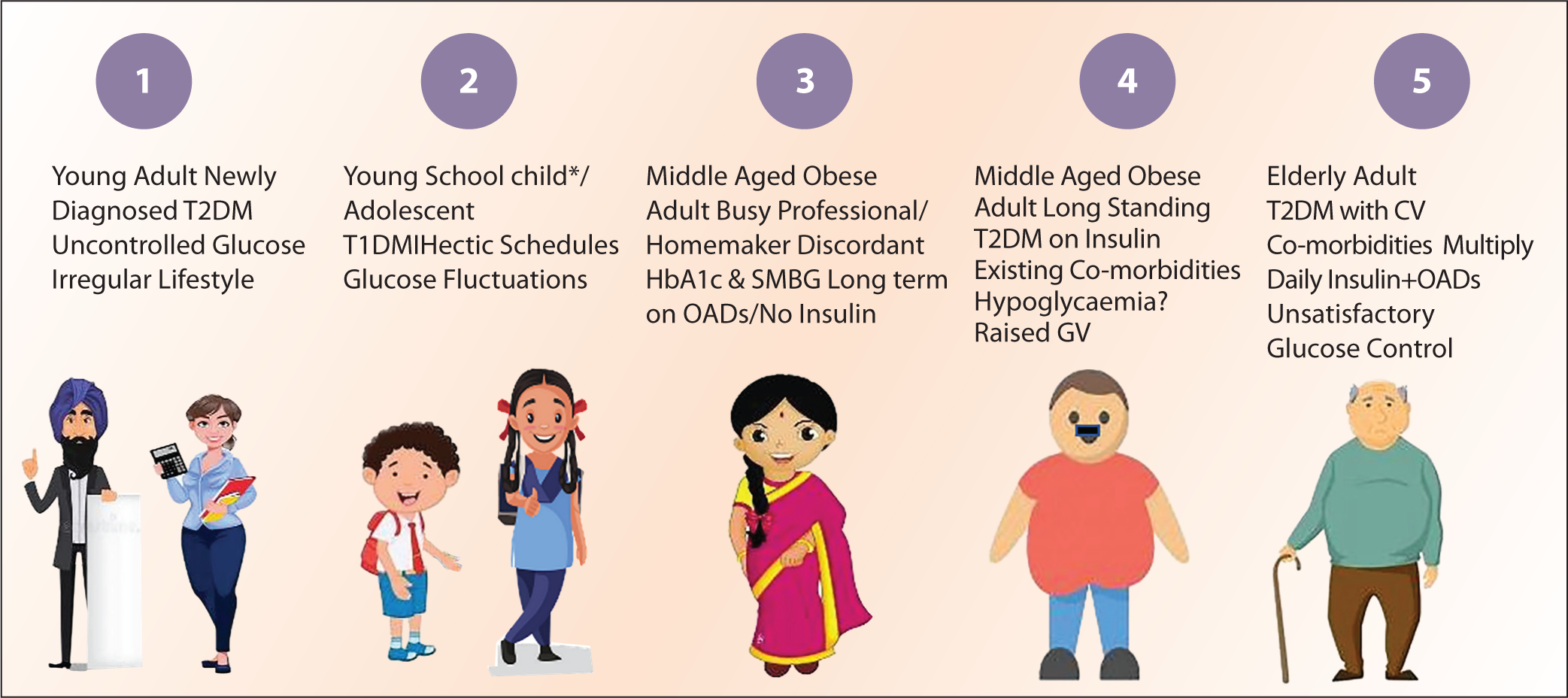
After recording and assessing the data of patients, HCPs briefed the details of the study and the role of CGM sensors—Freestyle Libre Pro (FSLP) and Freestyle Libre (FSL). Two follow-ups were planned for review—one after 14 days of FSLP and another after 14 days of FSL use.
After appropriate informed consent was given by patients, the FSLP device was fitted for 14 days, after which the data from FSLP was observed by HCP, and lifestyle changes including diet were curated and advised accordingly. The second sensor—FSL was then fitted to the patient for another 14 days. Upon review, the data derived from FSL was recorded to assess, compare, and understand the impact of lifestyle changes on diabetes management through CGM. After 3 months from the commencement of the study, their HbA1c levels were recorded for further analysis (Figure 2).
Patient Profiles Developed for the Study.
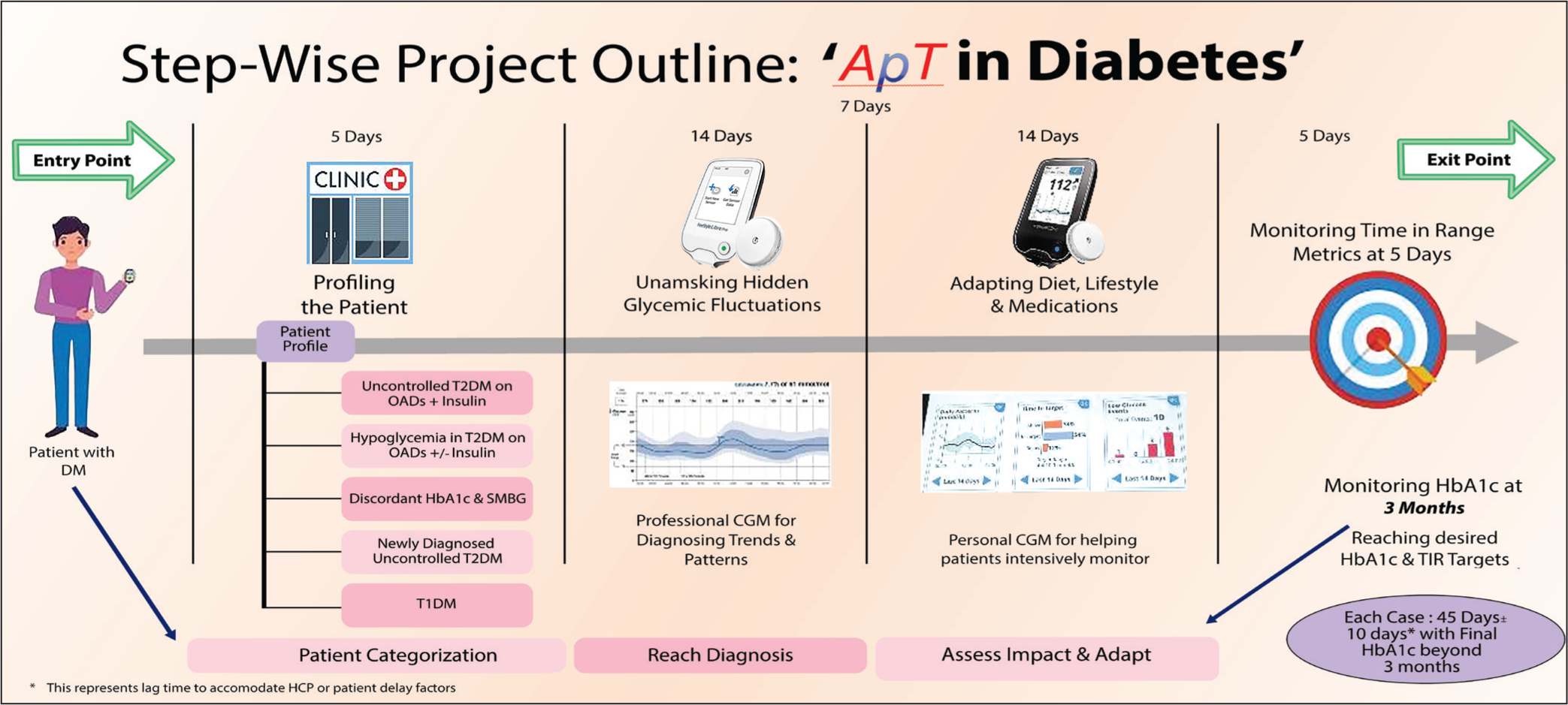
All patients were given an informed consent form and patient information sheet regarding the purpose and mode of study and only those who gave their consent were taken up for the study. This study was approved by the Local Institutional Ethics Committee of the Host Institution.
FSLP and FSL – About the Device
FSLP is a sensor-based CGM consisting of a handheld reader and a glucose sensor that is accurate, painless, and easy to use. It is a prick-free device that measures interstitial glucose of patients throughout the day. The sensor also gives glucose readings with a painless one-second scan, even through clothing, and can store up to 90 days of data on the reader.6,7
FSL is a similar device to FSLP with a three-in-one reader and replaceable sensors that include a continuous glucose monitor whereby the patient can monitor their levels at once. This device will help to understand their glucose patterns and the causative factors behind them, which may be in the form of diet, lifestyle and therapeutic interventions. 8
Both sensors help to develop an individualized Ambulatory Glucose Profile (AGP) for each patient as it identifies their areas of glycemic variations that are essential for appropriate and better management.
Data Analysis
Demographic data and clinical profile of patients including laboratory investigations were assessed and expressed in the form of frequency and percentage. The data obtained from FSLP and FSL sensors were recorded along with their HbA1c levels before and after the study. The resulting scores of all three sections were aggregated, analyzed based on average scores and expressed in the form of frequency and percentage. Cross tabulations, Chi-square tests, and Paired T-tests were used to analyze the correlation between variables that determined the clinical profile of DM.
Results
Demographic Distribution
Forty patients were included in the study where 37 (92.5%) were diagnosed with T2DM and three with T1DM and 47.5% of patients belonged to Profile 4 (Patients who were middle-aged and obese with a long-standing history of T2DM and Insulin dependent). 53% of patients belonged to the age group (Figure 3) of 50–69 years with a mean (SD) age of 53.8 (±17.02) and 65% were males. Concerning their Occupation, 30% of patients had desk jobs followed by 27.5% of homemakers and 85% of overall patients had a sedentary lifestyle.
Demographic Distribution of Patients (n = 40).
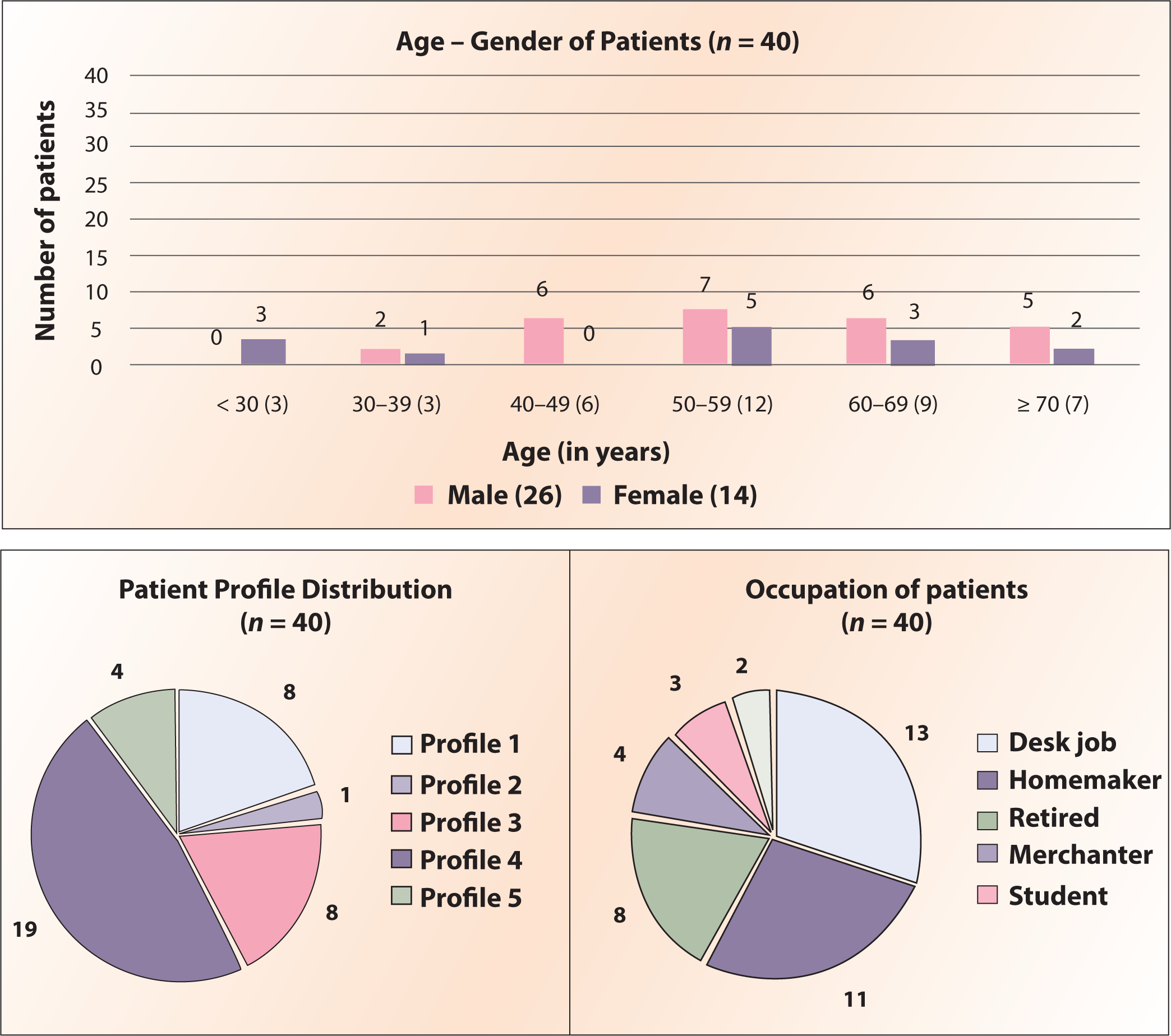
75% of patients had no history of any comorbidities and among those who had, 9 the commonest was Hypertension (40%).
Clinical Profile of Diabetes Mellitus
Concerning the duration of DM, 35% of patients had a long history of 11–20 years and among them, 36% belonged to the age group of 60–69 years and 35% were males, however, the results were not significant. 77.5% of patients had their HbA1c levels between 6.1% and 10% with a mean of 9.14 (±1.51) and among those who had HbA1c above 10%, mostly belonged to the age group of 40–59 (75%), and the values were significant.
Concerning their blood glucose levels, 47.5% of patients had their fasting glucose between 151 and 200 mg/dl with a mean (SD) of 167.8 (±75.8) and 65% of patients had their Post Prandial Blood Glucose (PPBG) between 151 and 300 mg/dl with a mean (SD) of 262.4 (±88.2). Out of 40, only 24 (60%) had their SMBG values recorded for all six times/day.
The other laboratory values recorded showed that 55% of patients had higher creatinine levels (>0.9 mg/d). 47.5% of patients had their cholesterol levels between 200 and 250 mg/dl and 42.5% of patients had borderline high triglycerides (150–199 mg/dl). However, approximately 68% of patients had normal HDL (between 40 and 60 mg/dl) and LDL levels (below 130 mg/dl). These values, however, when correlated with the duration of DM were insignificant (Table 1).
Other Laboratory Values Range Among Patient Profiles (n = 40).
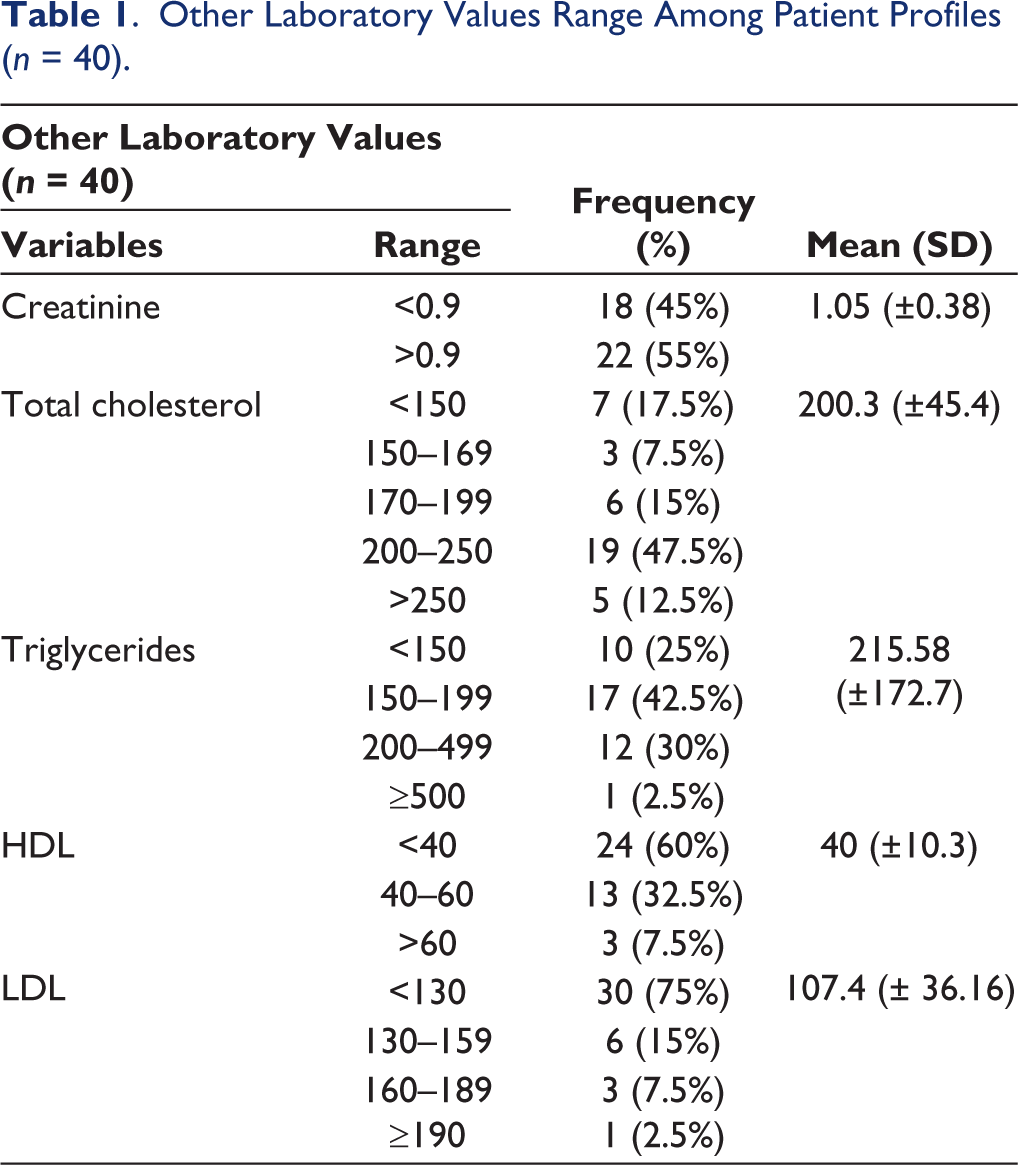
Patient Profiling – CGM Sensors
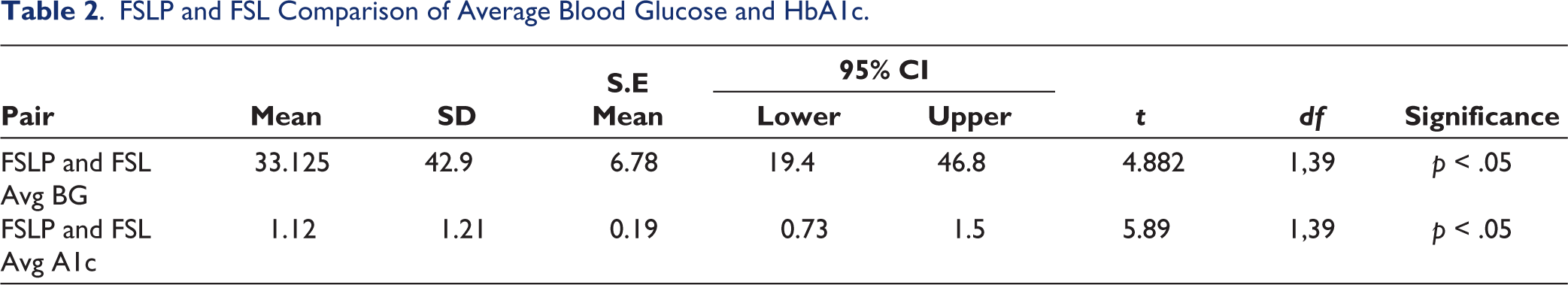
The FSLP and FSL sensors used for CGM recorded the average value of patients for 14 days which included their blood glucose, HbA1c, and their overall glucose levels in range (TIR), above (TAR), and below range (TBR) of normal. These data when compared showed that FSLP and FSL Average blood glucose (Table 2) were strongly correlated (r = 0.709; p < .05) where the latter was 33.12 times lower than the former. The FSLP and FSL Average HbA1c were also strongly and positively correlated (r = 0.835; p < .05) and FSL Average HbA1c was 1.12 times lower than that of FSLP.
FSLP and FSL Comparison of Average Blood Glucose and HbA1c.
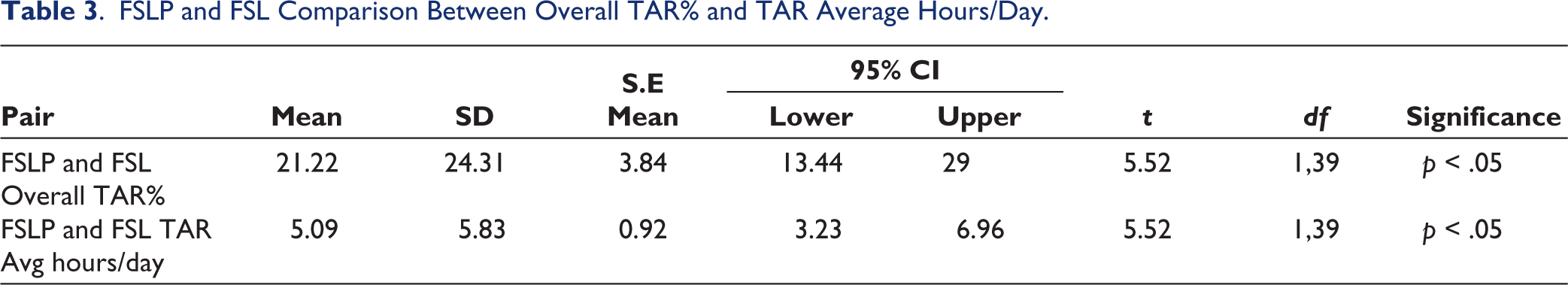
Their overall TAR% (Table 3) were moderately correlated (r = 0.406; p < .05) where FSL’s Overall TAR% was 21.22 times lower than FSLP’s Overall TAR%. Their TAR Avg hours/day were also moderately correlated (r = 0.0.406; p < .05) and FSL TAR Avg hours/day was 5.09 times lower than that of FSLP.
FSLP and FSL Comparison Between Overall TAR% and TAR Average Hours/Day.
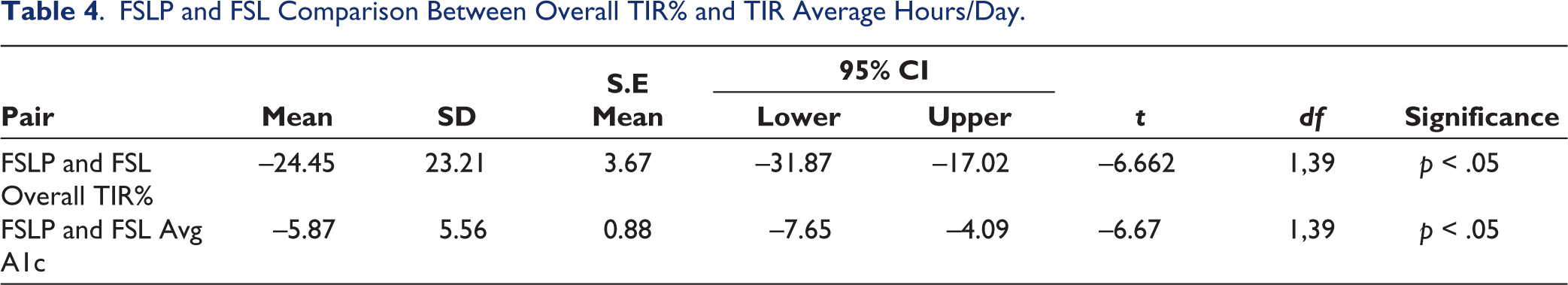
The FSLP and FSL Overall TIR% (Table 4) were moderately correlated (r = 0.374; p < .05) and FSL Overall TIR% was 24.45 times higher than FSLP overall TIR%. FSLP and FSL TIR average hours/day were also moderately correlated (r = 0.375; p < .05) where FSL TIR Avg hours/day was 5.87 times higher than that of FSLP.
FSLP and FSL Comparison Between Overall TIR% and TIR Average Hours/Day.
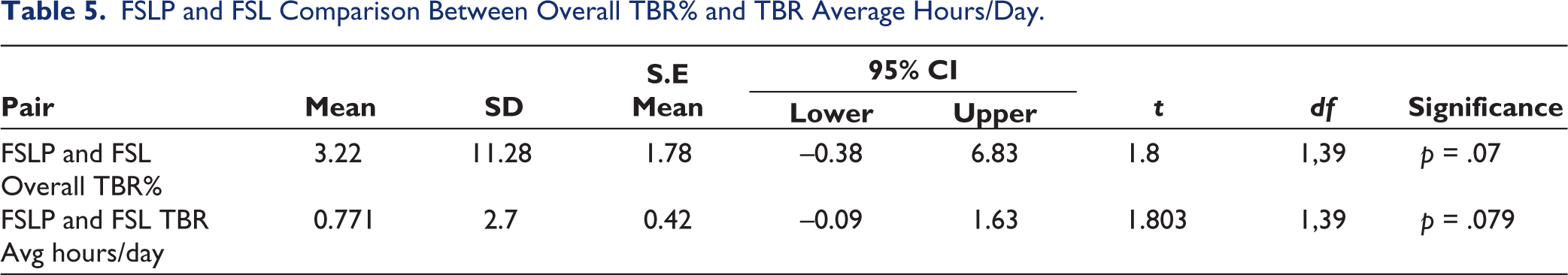
The FSLP and FSL Overall TBR% (Table 5) were weakly correlated (r = 0.259; p = .106) and FSL Overall TBR% was 3.22 times lower than FSLP Overall TBR%, yet non-significant. Their TBR average hours/day were positively correlated (r = 0.263; p = .101) where FSL TBR Average hours/day was 0.77 times lower than that of FSLP, yet non-significant.
FSLP and FSL Comparison Between Overall TBR% and TBR Average Hours/Day.
Discussion
DM has been a major public health concern for the past few decades and healthcare providers around the world have been keen on developing effective management for the disease that could help prevent complications and provide better prognosis. The current focus has been to look beyond glucose-centricity by attaining the TIR target and understand the individualistic picture of glycemic ups and downs caused by the diet and lifestyle of each patient.9,10
This study included 40 patients who were diagnosed and under treatment for DM among whom the major population was above 50 years of age (mean (SD): 53.8 (±17.02)) and 65% were males. This was similar to most studies indicating the focus point in the demographic diversity for intervention. 11 Few interventional and observational studies were conducted to review and evaluate the use of CGM and the results revealed that CGM promoted greater reductions in glycated hemoglobin, body weight, and caloric intake and this was similar to our study findings. The use of CGM has thus helped both patients and HCPs understand their glycemic profile better and implement the integration of diet, exercise, and glucose excursion education and counseling and yield better outcomes.10,11
Our study also showed better glycemic control among patients who were in SMBG-based therapeutic intervention, with the use of CGM when FSLP and FSL sensor results were compared. The FSLP sensors showed that more patients (70%) had poor glycemic control with their average glucose levels above 150 mg/dL and only 35% of patients had their average levels in TIR for more than 12 hours/day. However, after appropriate diet and lifestyle intervention based on the individualistic picture of each patient, the FSL sensor when applied showed that 60% got their average glucose levels below 150 mg/dl and 78% of patients had their average glucose levels in range (TIR) for more than 12 hours/day. These findings were similar to a pivotal study conducted by Bergenstal et al., 2016, where the TIR% improved from a median of 67.8%–73.4% to 76.4% for the overnight period. 12 Another multicentric similar study conducted by Tauschmann et al. 2018 also showed that the %TIR increased in eight of the nine cases from an average (SD) of 53.1% (13.7%) to 69.5% (6.8%) and the average change in %TIR was 12.9%–9.3% (SEM –3.1%) (p < .01). 13
Thus, the impact of real-time glycemic monitoring has been shown to benefit both patients and HCPs to monitor the effects of different types of food, timing of meals, their activity and stress levels and provide appropriate lifestyle and clinical management accordingly. This therapeutic intervention has been shown to improve the prognosis of DM and reduce the risk of complications.
Conclusion
Monitoring the glucose levels has been a standard practice for both patients and HCPs before and after intervention through SMBG, which has been effective yet inadequate. The CGM sensors were developed for patients with DM to cover glucose readings 24×7, which has now proven to be a valuable clinical application in reducing adverse hypoglycemic events, attaining TIR targets, and achieving better control. Providing visibility of the complete glucose profile of the patient in real-time, the personal CGM enables apt and timely decision-making for patients with DM. Thus, upgrading from SMBG to personal CGM is a promising approach for better diabetes management. However, an overview of CGM concerning specific attributes of effective interventions and its user-friendly relevance among HCPs remains unclear. Thus, further quantitative analysis on a large scale would be required to produce concrete evidence and detailed guidance among clinicians would ensure better implementation in the future.
Footnotes
Acknowledgements
We would also like to thank Arfect Business solutions for editorial and publication support.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
This research was approved by the Research Ethics Committee (REC) at Laddhad Hospital, Buldana.
Funding
We acknowledge Abbott Diabetes Care, India for offering unbiased financial support for this study and medical writing aspect.
