Abstract
Introduction:
Vaser liposuction has emerged as a safe and effective technique for body contouring. This study aims to present the results of body contouring procedures, both debulking and high-definition liposuction, using the Vaser system in a single surgeon’s practice.
Methods:
This is a retrospective review of 175 patients who underwent Vaser-assisted body contouring procedures between January 2022 and July 2024. The patient population included 102 females and 73 males. Various body regions were addressed, including the chin/jawline, arms, chest (gynaecomastia), abdomen, flanks, back, thighs and calves. Both debulking and high-definition liposuction techniques were utilised. Postoperative care involved the use of customised compression garments for three months.
Results:
Significant improvements in body contour were achieved in all treated areas, with high patient satisfaction. In the high-definition liposuction group, well-defined anatomical lines were created without the need for fat grafting. Gynaecomastia cases were successfully managed with Vaser liposuction alone, avoiding the need for open excision. Postoperative recovery was generally smooth, with minimal complications reported.
Conclusion:
Vaser-assisted liposuction is a versatile and reliable technique for body contouring in both male and female patients. The ability to precisely target and remove unwanted fat, while maintaining skin tightening and minimising complications, makes it a valuable tool in the plastic surgeon’s armamentarium. The presented results demonstrate the effectiveness of this approach in achieving desired aesthetic outcomes.
Introduction
Liposuction is a widely performed cosmetic surgical procedure aimed at removing excess fat from specific areas of the body. Vaser liposuction, also known as vibroliposuction or ultrasound-assisted liposuction (UAL), is a body contouring procedure that has gained widespread acceptance in recent years due to its ability to selectively target and emulsify fat cells while preserving surrounding tissues.1,2 The use of ultrasonic energy in Vaser liposuction allows for more precise fat removal and reduced trauma to surrounding tissues. 3
Developed in the late 1990s, Vaser liposuction has emerged as a safe and effective alternative to traditional liposuction methods. 4 The procedure works by using a specialised handpiece that emits ultrasonic waves, which are directed at the targeted fat deposits. This ultrasonic energy helps to break down and liquefy the fat cells, making them easier to suction out. 4
One of the key benefits of Vaser liposuction is its ability to precisely target and remove stubborn fat pockets while minimising damage to surrounding tissues. This results in a more predictable and consistent outcome, with a reduced risk of skin irregularities or contour deformities often associated with traditional liposuction. Additionally, the Vaser technique provides a more streamlined recovery process compared to other liposuction methods. Patients often experience less swelling, bruising and discomfort during the postoperative period, allowing for a quicker return to normal activities.
The versatility of Vaser liposuction allows it to be performed on a variety of body areas, including the chin/jawline, arms, chest (for the treatment of gynaecomastia), abdomen, flanks, back, thighs and calves. The procedure is particularly effective in addressing localised fat deposits that have proven resistant to diet and exercise.
This study aims to present the results of body contouring procedures, both debulking and high-definition liposuction, using the Vaser system in a single surgeon’s practice, encompassing a diverse patient population of both males and females.
Materials and Methods
A retrospective review was conducted of 175 patients who underwent Vaser-assisted body contouring procedures over a 2.5-year period at a single institution between January 2022 and July 2024. The patient population included 102 females and 73 males with a mean age of 42.5 years (range 21-64 years).
The targeted body regions included the chin/jawline, arms, chest (for the treatment of gynaecomastia), abdomen, flanks, back, thighs and calves. Both debulking and high-definition liposuction techniques were utilised, depending on the desired aesthetic outcomes.
In the debulking liposuction cases, the focus was on the selective removal of unwanted fat deposits to achieve a more streamlined and proportionate body shape. For the high-definition liposuction cases, the goal was to create well-defined anatomical lines and contours, without the need for additional fat grafting.
Technical Details
We performed all our liposuction procedures under general anaesthesia, and the patients were positioned according to the part to be operated upon. A tumescent solution is injected using a 2.5 or 3 mm multi-hole cannula with an Infiltrator machine. Our infiltration formula is 1 l of normal saline, 15 ml Loxicard, two ampoules of adrenaline and 5 ml of Soda Bicarb; injected both deep and superficially. Then, we start using the Vaser at 90% C (continuous) mode. We use ceramic ports while doing the Vaser and keep all our incisions open at the end of surgery for the fluid to leak out.
Conventionally, Vaser should be used for 10 minutes for a litre of tumescent fluid, but we use clinical endpoints like ‘free-flowing fatty fluid pouring out’ and ‘a smooth frictionless movement’ in any particular area to stop further Vaser treatment at that place. By doing so, Vaser is used for less than the prescribed time; hence, we have not had any complications like skin burns, etc.
We use a one ringed 3.7 mm probe for larger surface areas and the smaller 2.9 mm Vaser probe for smaller areas like double chin, etc. The Vaser machine used for our patients is manufactured by Bausch Health Company, USA (Solta Medical).
Following the Vaser, we performed aspirations using our Power Assisted Device to reach our goals. We generally use a 3 or 4-mm Double Basket Cannula for most of our liposuction cases. Smaller cannulas were used for more delicate areas like the double chin and superficial etching in high-definition cases.
Postoperative care involved regular dressing with open holes for the fluid to leak out and foam/gauze application in negative spaces for high-definition cases. We allow early ambulation on the same day of surgery, bathing the patient the next day morning and pressure garment application the next day morning. Massage by the nurse to milk out the fluid is optional, and the patient is discharged the next day on oral analgesics and antibiotics for five days.
Lymphatic massages were advised from day 10 at home (manually) and with a cavitation device at the hospital after two to three weeks (if required). We encourage patients to do plenty of ambulation, keep themselves well hydrated and use Arnica gel for bruising (if any).
We use customised compression garments, which the patients are instructed to wear for a period of three months. During the first six weeks, the garments are worn for 24 hours per day, and then for 12-16 hours per day for the subsequent six weeks. 5 The hospital stay for all our patients with major liposuction is one day, and discharge the next day.
Patients were followed up closely in the immediate postoperative period, with visits every two to three days for the first two weeks. Thereafter, a strict diet and exercise protocol was initiated, specialised massaging as per patient needs and patients were monitored at regular intervals to assess the progress of their results. We advise a diet comprised of a high protein diet with fewer carbohydrates and fats. Patients start brisk walking within a week to 10 days and do all their regular exercises after 14 days of surgery.
Results
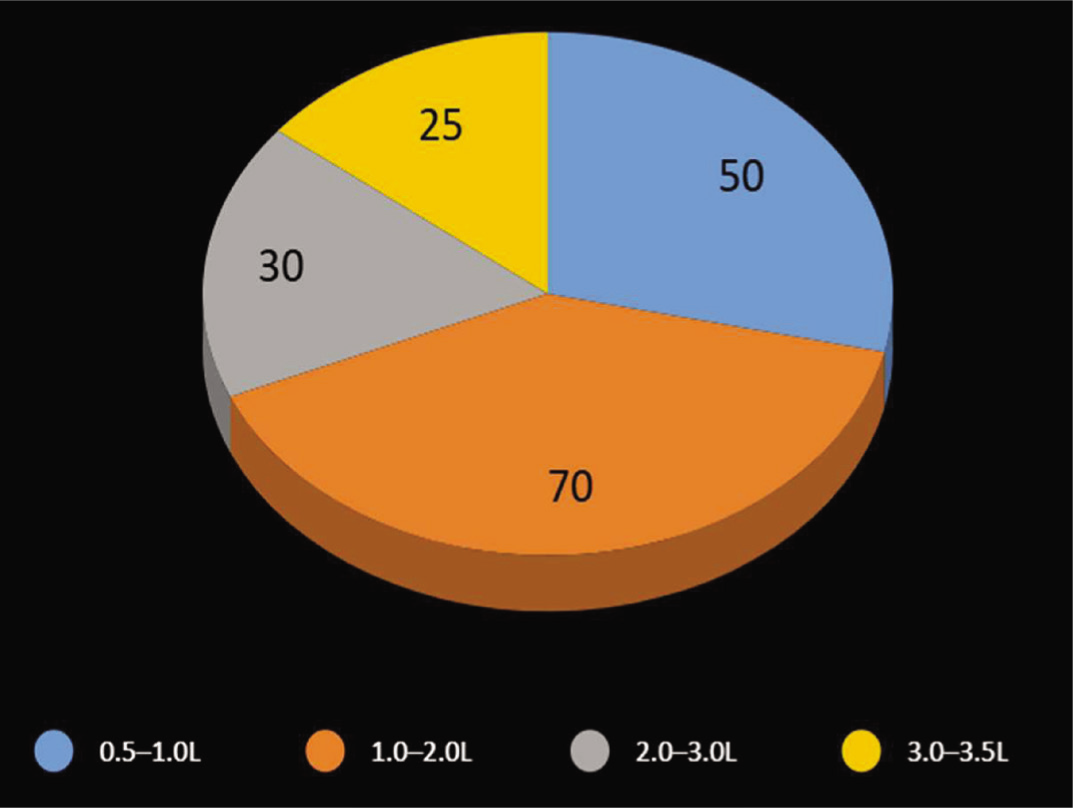
The mean operating time was 120 minutes (45-180 minutes). The most common areas treated were the abdomen, thighs and arms. The mean amount of fat removed was 2 l (range 0.5-3.5 l) (Figure 1).
Amount of Fat Aspirated (Number of Cases).
Postoperative recovery was generally smooth, with minimal complications reported. Patients experienced less swelling, bruising and discomfort compared to traditional liposuction methods, allowing for a quicker return to normal activities.
Postoperative complications were minimal, with four patients (2.3%) experiencing seroma, two patients (1.1%) experiencing infection and two patients (1.1%) experiencing skin irregularities. There were no major complications or fatalities. 6
The results were assessed by two independent medical personnel. Patient satisfaction rates were high, with 95% of patients reporting significant improvements in body contour and 90% reporting improved self-esteem (Table 1).
Details About our Liposuction Cases.

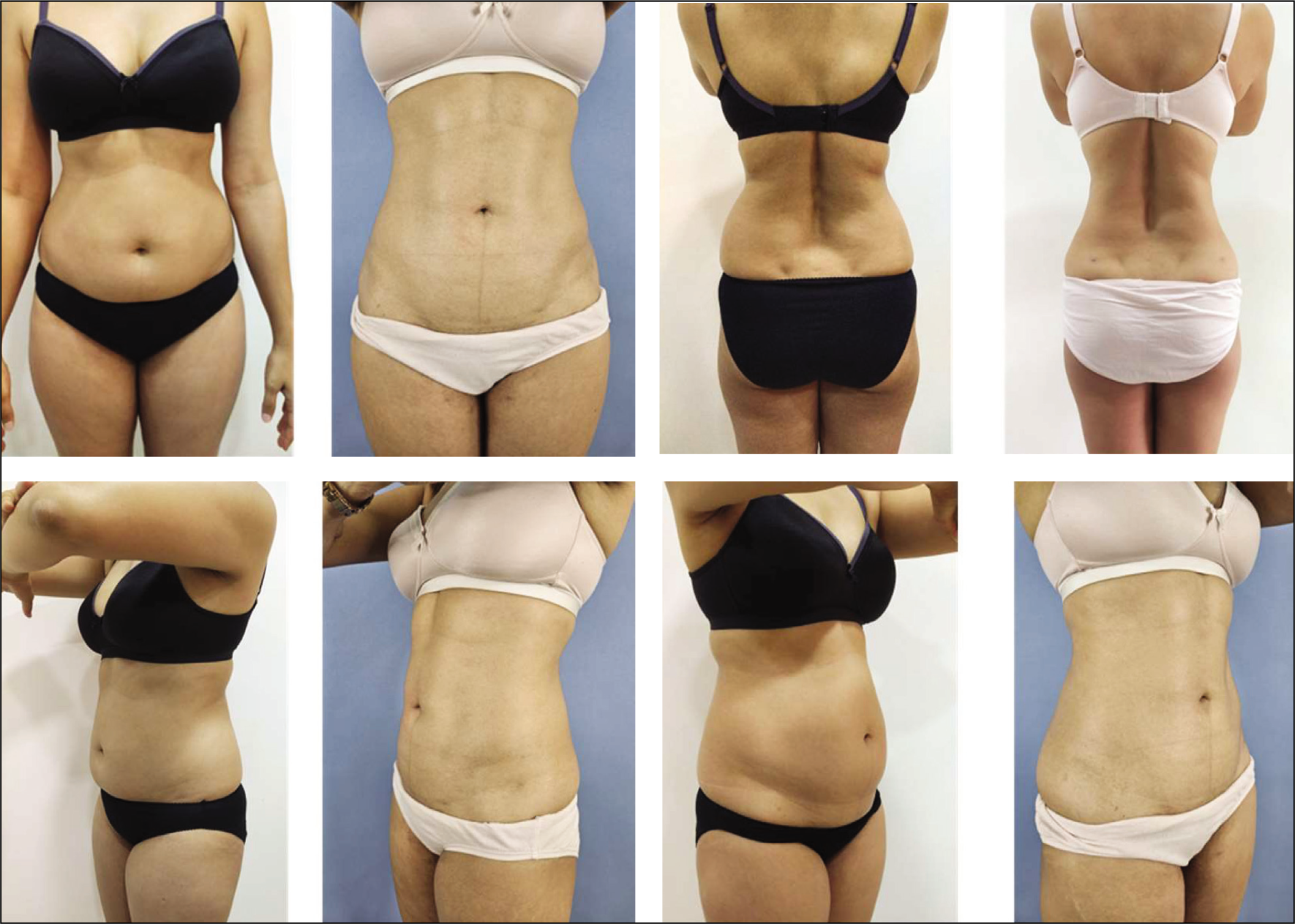
The Vaser-assisted body contouring procedures resulted in significant improvements in body contour for all treated areas, with high patient satisfaction. In the high-definition liposuction group, well-defined anatomical lines were created without the need for fat grafting, and the results appeared natural and aesthetically pleasing (Figures 2–6).
Showing High-definition Results of Abdominal Region Post Vaser Liposuction.
Showing High-definition Results of Abdominal Region Post Vaser Liposuction.
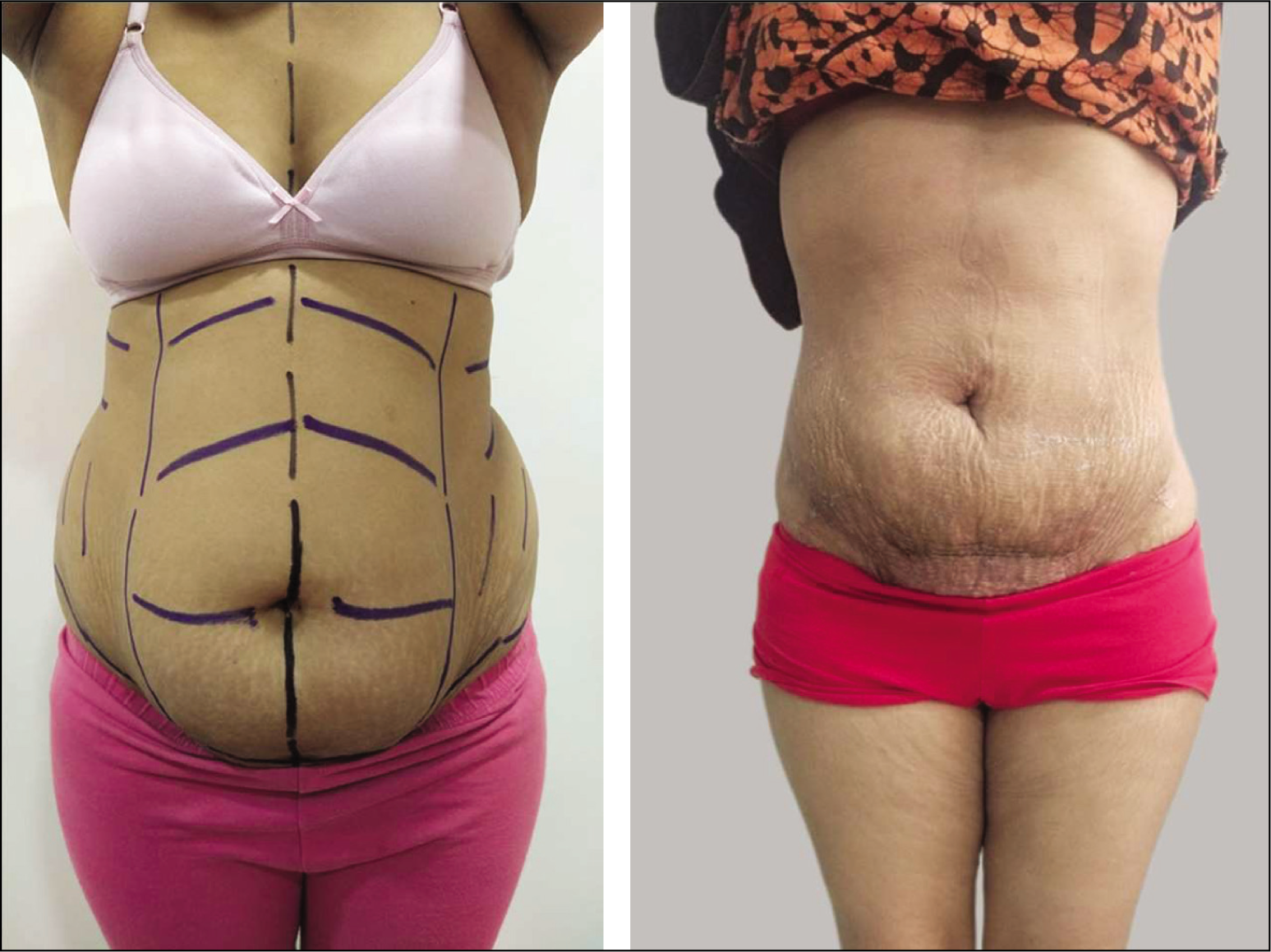
Results of Debulking Vaser Liposuction Tummy Region.
Results of Double Chin Vaser Liposuction.

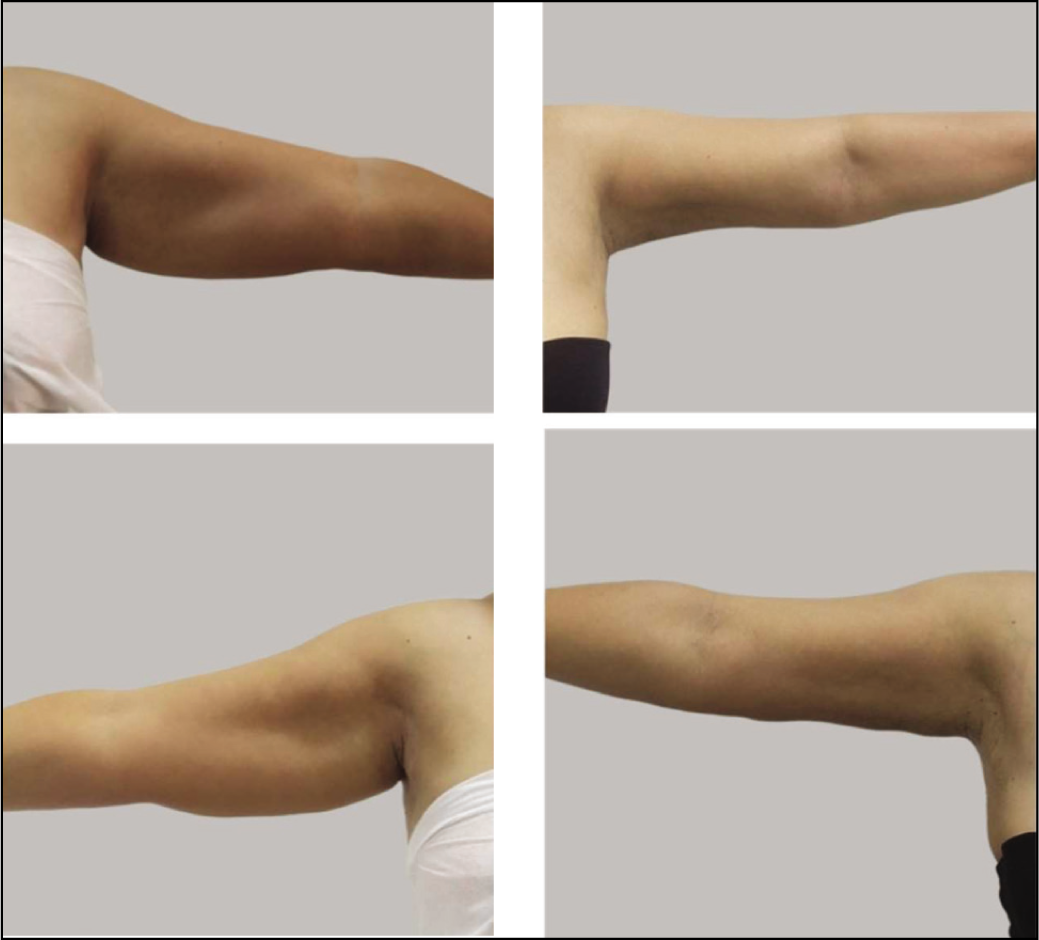
Results of Arm Vaser Liposuction.
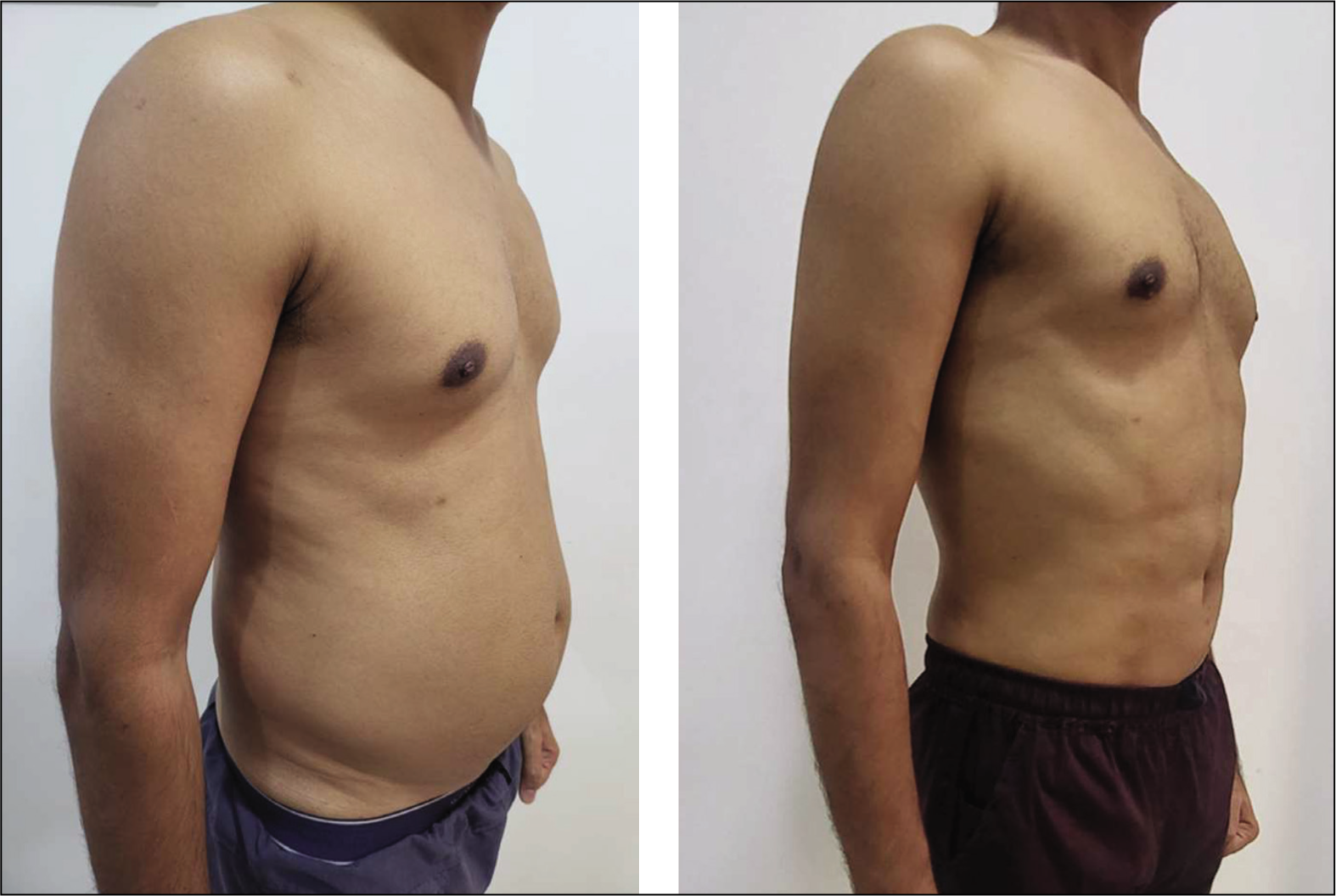
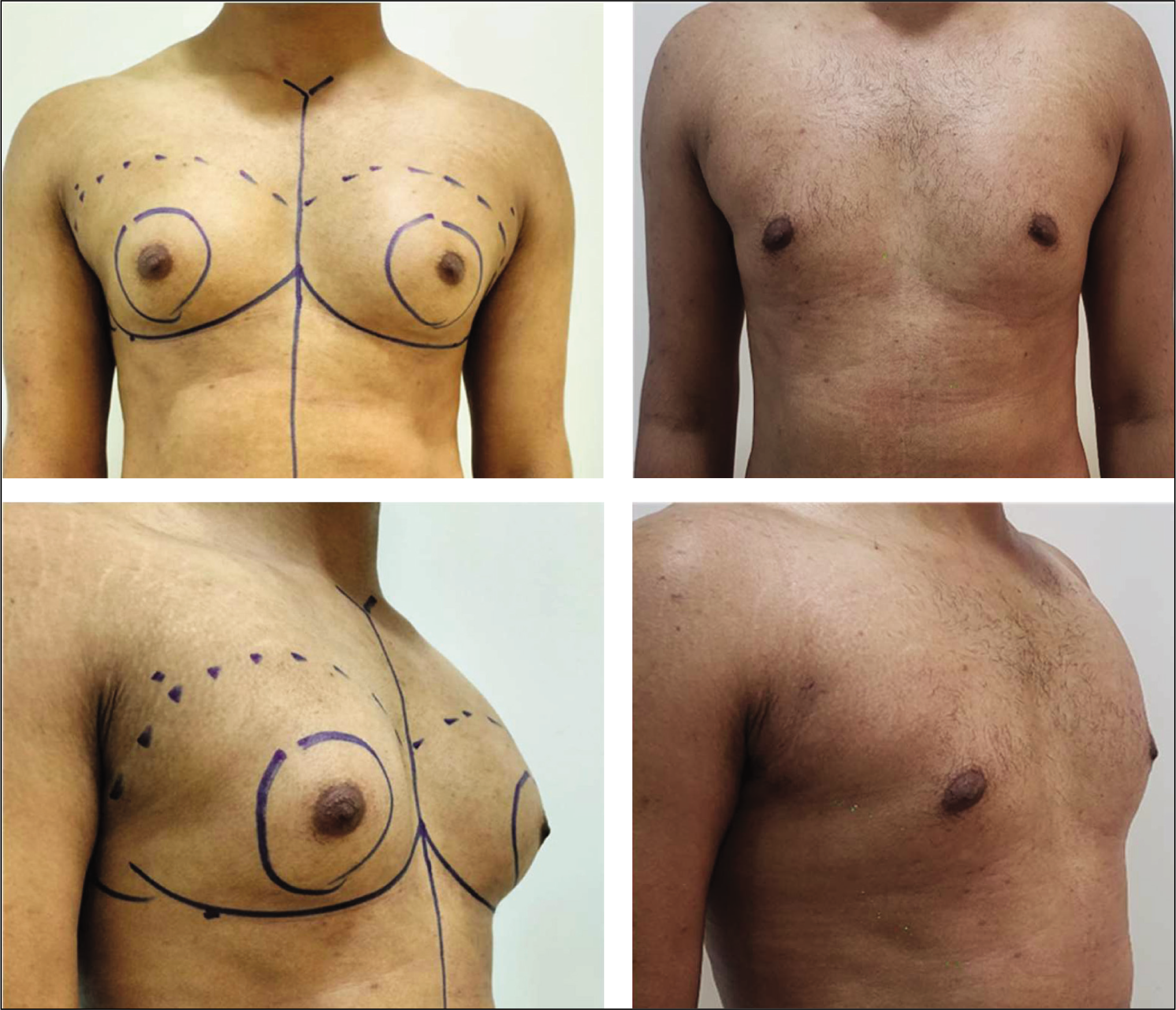
For the gynaecomastia cases, Vaser liposuction alone was successful, without the need for open excision of the glandular tissue. This approach resulted in a scarless outcome for the patients (Figure 7).
Results of Gynaecomastia Following Vaser Liposuction.
Discussion
Vaser liposuction, also known as ultrasonic-assisted liposuction, uses a specialised device that emits ultrasonic energy to break down fat cells. The procedure involves the insertion of a small probe under the skin, which emits ultrasonic waves that selectively target and emulsify fat cells. The emulsified fat is then removed through suction, leaving the surrounding tissues intact. 1
The results of this study demonstrate the effectiveness of the Vaser system in achieving desired aesthetic outcomes across a wide range of body regions, including the chin/jawline, arms, chest, abdomen, flanks, back, thighs and calves. The technique is particularly useful in addressing localised fat deposits that are resistant to diet and exercise.
Our findings align with the results published by Hoyos and Millard and Perez-Cano et al. highlighting the effectiveness of Vaser technology in achieving well-defined anatomical contours without additional fat grafting.7,8
Several studies have demonstrated the benefits of Vaser liposuction over traditional liposuction techniques. These benefits include:
Improved fat removal: Vaser liposuction has been shown to be more effective in removing fat, particularly in areas with fibrous tissue.
2
Reduced blood loss: The ultrasonic energy used in Vaser liposuction helps to coagulate blood vessels, reducing blood loss and the risk of hematoma.
3
Less trauma to surrounding tissues: The selective targeting of fat cells by ultrasonic energy reduces trauma to surrounding tissues, resulting in less swelling and bruising.
9
Shorter recovery time: Vaser liposuction has been shown to result in shorter recovery times compared to traditional liposuction techniques.
10
While Vaser liposuction is considered a safe and effective procedure, there are potential limitations and complications to be aware of. These include:
Skin irregularities: Vaser liposuction can result in skin irregularities, such as contour irregularities or skin laxity.
11
Seroma: The formation of seroma, a collection of fluid under the skin, is a potential complication of Vaser liposuction.
12
Infection: As with any surgical procedure, there is a risk of infection with Vaser liposuction.
13
Scarring: Vaser liposuction requires the insertion of a probe under the skin, which can result in scarring.
14
The results of this study demonstrate the effectiveness of the Vaser system in achieving desired aesthetic outcomes across a wide range of body regions, including the chin/jawline, arms, chest, abdomen, flanks, back, thighs and calves. The technique is particularly useful in addressing localised fat deposits that are resistant to diet and exercise.
Our findings align with the results published by Hoyos and Millard and Perez-Cano et al. highlighting the effectiveness of Vaser technology in achieving well-defined anatomical contours without additional fat grafting.7,8
Our study demonstrates the safety and efficacy of Vaser liposuction in a large cohort of patients. The low complication rate and high patient satisfaction rates support the use of Vaser liposuction as a reliable treatment for excess fat removal. 6
The selective targeting of fat cells by ultrasonic energy in Vaser liposuction allows for more precise fat removal and reduced trauma to surrounding tissues.9,10 This is reflected in our study, where we observed minimal complications and high patient satisfaction rates.
The use of Vaser liposuction has been shown to result in significant improvements in body contour and patient satisfaction.11,12 Our study supports these findings, with 95% of patients reporting significant improvements in body contour and 90% reporting improved self-esteem.
Conclusion
The presented experience highlights the benefits of Vaser liposuction, including the ability to create well-defined anatomical lines without the need for additional fat grafting, as well as the successful management of gynaecomastia cases without open excision. The streamlined postoperative recovery process further adds to the advantages of this approach. Overall, the findings of this study contribute to the growing body of evidence supporting the use of Vaser liposuction as a safe and effective technique for comprehensive body contouring in both male and female patients.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author received no financial support for the research, authorship and/or publication of this article.
