Abstract
Improper disposal of medications poses risks to environmental and public health, yet participation in pharmaceutical take-back programmes remains low. This study examines barriers and motivations for return behaviour through the lens of care theory, using Tronto’s four phases – attentiveness, responsibility, competence, and responsiveness. We used a mixed-methods approach: a survey, contextual interviews, and two workshops with end users, pharmacy workers, and designers. Findings informed the Caring Factors Return Inspiration Toolkit, which organises behavioural influences by care phase to guide ideation. Results show that low awareness and convenience gaps constrain attentiveness and responsibility; competence depends on clear instructions and privacy safeguards; and responsiveness is strengthened by feedback and proportionate incentives. The toolkit supports designers in creating care-informed product–service systems that embed cues, feedback, and social norms to foster responsible return behaviour. By translating ethical insights into actionable design levers, this study advances design for care and circular pharmaceutical practices.
Keywords
Introduction
With the global rise in pharmaceutical consumption, the accumulation and improper disposal of unused and expired medications (UEM) in households has become a growing environmental and public health concern. A systematic review across 25 countries found unused medicines in households in 63.8% of observations on average (Wang et al., 2025). Most were discarded via trash or wastewater routes (66.9%), while only 12.9% were returned through take-back programmes. In the United States, disposal remains similarly problematic; in a pharmacy-customer survey, throwing medications in the trash was the most commonly reported method (27.5%), followed by flushing (15.8%) (Ehrhart et al., 2020). Unused medications often result from expiration, overprescription, or changing medical needs, yet they are improperly discarded or stored indefinitely at home (Makki et al., 2019; World Health Organization et al., 1999). These practices increase risks of accidental poisoning, misuse, and abuse (Vollmer, 2010) and contribute to environmental contamination, as pharmaceuticals enter waterways and ecosystems with long-term effects on human and ecological health (Kristina and Wulandari, 2020; Kusturica et al., 2020; Makki et al., 2019). Improper handling of UEM also imposes significant economic burdens, including the cost of medicine waste, secure disposal, and the mitigation of associated health and environmental impacts.
Take-back programmes – where end-of-life pharmaceuticals are returned to pharmacies, kiosks, or other designated collection points – are widely recognised as a Circular Economy (CE) strategy that reduces pharmaceutical waste and mitigates diversion and misuse (Kümmerer, 2010; Kusturica et al., 2016; Wang et al., 2024; Yanovitzky, 2016). Community-based medication take-back initiatives, such as the National Prescription Drug Take-Back Day (Drug Enforcement Administration, 2012; Thach et al., 2013), along with regulatory measures like the Secure and Responsible Drug Disposal Act of 2010 (S. 3397, 2010), have been introduced to expand access to collection infrastructure and legitimize safe return pathways (Drug Enforcement Administration, 2014; Fleming et al., 2016). However, participation remains low, with only a fraction of unused or expired medications (UEM) successfully returned in the United States. (Drug Enforcement Administration, 2012; Thach et al., 2013; S. 3397, 2010; Drug Enforcement Administration, 2014; Fleming et al., 2016).
Prior studies have documented barriers such as a lack of awareness, inconvenient infrastructure, and inadequate guidance. Greater emphasis is now being placed on the rational use of medicine, ensuring that patients receive the right medications at the right time and use them appropriately (Gad et al., 2020; Holloway et al., 2018). Much of the take-back literature frames return primarily as a policy and infrastructure problem, offering limited insights into the behavioural drivers of participation and the relational ethics that shape user engagement. While system-level infrastructures provide a foundation for sustainable disposal, household decision-making remains a key determinant of when and how medications are returned. Accordingly, strategies that cultivate care and responsibility among consumers are essential to improving return behaviour. We therefore adopt an ethics-of-care lens because pharmaceutical return is not only a matter of access and convenience but also a value-laden practice in which individuals negotiate obligations to family members, communities, and ecosystems. Returning UEM often requires effort beyond routine disposal, and decisions are shaped by how they weigh competing responsibilities (e.g. saving medications ‘just in case’ vs removing household risk) and whether they feel supported by institutions and infrastructures.
Care-oriented design scholarship frames care not merely as an individual disposition, but as something produced through designed relations, infrastructures, and everyday practices (Imrie and Kullman, 2016). Building on this view, care ethics is well suited to UEM return as it links moral motivation to the socio-material conditions that enable action, offering a structured way to examine where the return process breaks down and what kinds of supports may sustain it over time (Tronto, 1993). Drawing on Tronto’s four phases – attentiveness, responsibility, competence, and responsiveness – we examine how caring factors influence return decisions and identify barriers that limit participation. We address the following two Research Questions (RQs): • RQ1: What barriers and motivations shape users’ decisions to return of UEM? • RQ2: How can the caring motivational factors be translated and inform the idea generation process that supports responsible return behaviour?
Using evidence from surveys, contextual interviews, and participatory workshops, we developed the Caring Factors Return Inspiration Toolkit, which translates user motivations into actionable design levers. The toolkit provides designers with practical methods for embedding care into product–service systems, thereby supporting CE practices. More broadly, this work extends design for sustainable behaviour by adding a care-informed perspective that emphasises empathy, responsibility, and reciprocity, offering pathways for systemic change.
Background
Barriers to return
Studies have identified persistent barriers that can be grouped into three categories. First, awareness and knowledge gaps: many users are unfamiliar with safe-disposal practices, local drop-off sites, or the risks associated with improper storage and disposal (Kristina and Wulandari, 2020; Kusturica et al., 2016; Rani et al., 2019). Second, infrastructure and convenience barriers: uneven distribution of collection sites, limited hours, transportation challenges, and inconsistent preparation requirements (e.g. separating packaging and uncertainty about eligibility) reduce willingness to act. The absence of clear step-by-step instructions at drop-off points further undermines confidence and follow-through. Third household and behavioural patterns level, saving medicines ‘just in case’ as patients often discontinued medication once symptoms subsided, storing leftover drugs without recognising the environmental or public health risks (Ehrhart et al., 2020). Additional factors such as over-purchasing, failure to monitor expiration dates, and privacy concerns often lead to indefinite storage and eventual disposal. These barriers illustrate how systemic and behavioural factors intersect to prevent effective participation.
Behavioural factors and leverage in system change
Within systems thinking, behaviour is not viewed in isolation, but as the result of interdependent structures, feedback loops, and values embedded within the system itself (Arnold and Wade, 2017; Senge, 1990). As Meadows (1999) argued, systems can be transformed by identifying and acting on ‘leverage points’ – strategic places within a complex system where a small intervention can lead to significant, lasting change. Human behaviour is one such leverage point; rather than seeing users as passive recipients of designed systems, this perspective recognises them as active agents whose decisions – when properly supported – can ripple through and alter system dynamics. In CE contexts, behavioural barriers such as weak information flows, misaligned incentives, and limited opportunities for engagement often reflect deeper system shortcomings that constrain participation. Design can identify these behavioural leverage points and target them as sites for intervention (Lockton et al., 2013). Related work in behavioural economics has influenced design practice through nudge and choice architecture, which emphasise how default pathways, prompts, and the framing of options shape decisions (Thaler and Sunstein, 2009). While such approaches have informed sustainability interventions, they may under-specify the relational and ethical dimensions of responsibility that are central to sustained participation (Lilley et al., 2017). Meadows (1999) further emphasised that the highest leverage points involve shifts in mindsets, values, and system goals. In pharmaceutical return systems, this suggests the importance of approaches that foreground care, responsibility, relational engagement, and sustainable behaviour. Accordingly, this study draws on Tronto’s phases of care as a systemic lens to interpret return breakdowns and to translate caring motivations into actionable leverage points for circular product–service systems.
Care practice in design
Mapping concepts to the phase of care proposed by Laurin and Martin (2022) based on Fisher and Tronto’s care theory (1993).
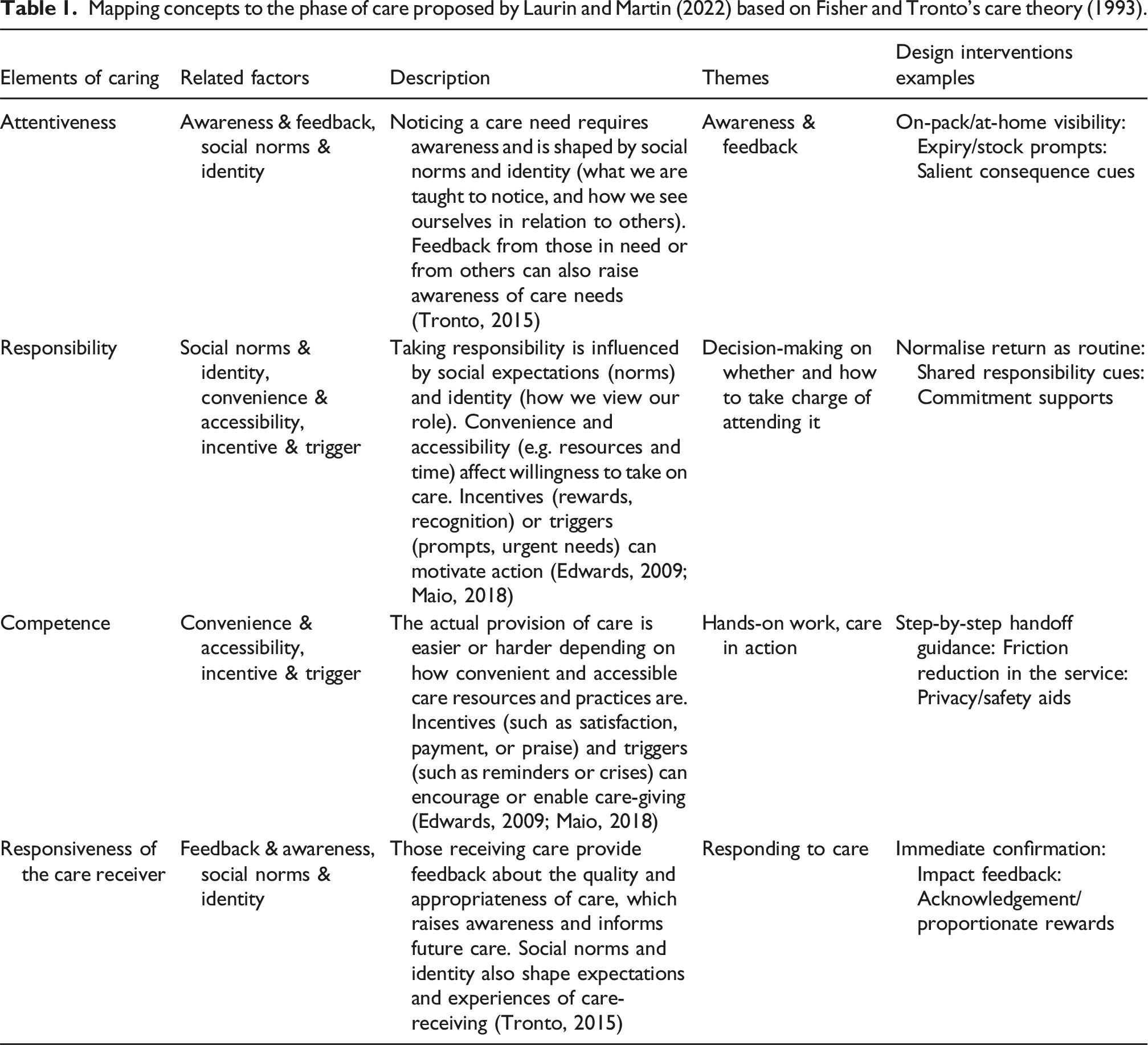
Attentiveness (caring about)
The first phase of care, attentiveness, involves the capacity to detect and acknowledge the needs of others. Care begins with recognising that a need exists and making the moral assessment that the need is worth responding to – laying the foundation for a compassionate and ethical response (Tronto, 2015). This ability to notice care needs is shaped by social norms and personal identity – what individuals are taught to observe, prioritise, and value in others (Edwards, 2009). Feedback from care recipients or peers can also heighten awareness by drawing attention to previously unnoticed needs. Promoting attentiveness requires strategies that foster both individual and collective awareness. Education and dialogue are particularly effective tools for this purpose. Engaging communities, organisations, and individuals in open conversations about the importance of recognising care needs can help shift cultural norms and enhance sensitivity to everyday acts of care (Niederdeppe et al., 2025). This can be achieved through workshops, exhibitions, seminars, and public forums that showcase real-life examples of unmet needs and the consequences of neglect or inattention (Fuad-Luke, 2013). Sharing personal narratives and case studies is another powerful approach. Stories that connect on both emotional and intellectual levels can foster empathy and reflection (Niederdeppe et al., 2025). In addition, visual media – such as images, video, and infographics – can make abstract care concepts more concrete and memorable, encouraging people to recognise and reflect on care needs in their everyday environments.
Responsibility (Taking Care of)
The second phase of care, responsibility, involves fostering a willingness to respond to identified needs. This phase is characterised by a receptive stance towards others and a recognition of one’s moral obligation to act when care is required (Webteam, 2009). Responsibility is shaped by social norms and cultural expectations, which influence who is expected to provide care – whether individuals, families, professionals, or institutions (Rogers and Weller, 2012). Identity also plays a central role; individuals who see themselves as caregivers or responsible actors are more likely to engage in caring behaviours. Practical considerations such as convenience, accessibility, time, and availability of resources further affect the willingness to act. Making behaviours visible – through social comparison, feedback, or traceable actions – can reinforce social norms and shared accountability (Dolan et al., 2012). Encouraging responsibility can be supported through community engagement strategies that promote collective ownership of care. This may include the formation of care-focussed groups or support networks, as well as advocacy for policies that institutionalise care responsibilities across sectors (Bradley, 2021). Design plays a critical role in shaping a user’s sense of responsibility. Thoughtfully designed product-service systems (PSS) can help users understand the consequences of their actions and how those actions contribute to broader sustainability goals.
Competence (care-giving)
The third phase of care – competence – concerns the knowledge, skills, and capacities required to deliver effective care, moving beyond recognition (attentiveness) and commitment (responsibility) to practical, hands-on action, and refined through feedback (responsiveness). Crucially, competence ensures that care is not only acknowledged but also delivered in a way that meets the needs of the recipient. Competence is interdependent with the other phases of care: attentiveness specifies what needs to be addressed, responsibility supplies the commitment and priority to act, and responsiveness provides feedback that calibrates and improves performance – together determining the likelihood and quality of competent action (Tronto, 1993). The quality and consistency of care are strongly influenced by convenience and accessibility – for example, the availability of instructions, facilities, and reminders (Ley, 2023). When care is easy to perform and supported by appropriate infrastructure, follow-through increases.
Responsiveness (care-receiving)
The final phase of care, responsiveness, focuses on how care recipients react and provide feedback about the quality and appropriateness of care, thereby informing adjustments to future practice (Edwards, 2009; Tronto, 1993). Responsiveness ensures that care is not a one-way action but part of a reciprocal relationship in which feedback is used to improve quality, relevance, and outcomes. Encouraging responsiveness involves creating systems and opportunities for care recipients to express their experiences, needs, and concerns. This may include feedback mechanisms such as surveys, interviews, digital prompts, or community forums that allow users to share how well their needs have been met. These insights help caregivers and systems reflect on their practices to continuously improve care delivery. Expectations around gratitude, silence, or emotional expression can influence whether and how recipients offer feedback (Edwards, 2009). Responsiveness can be activated by prompting users to reflect on the environmental and social impacts of their actions and by showing tangible outcomes. Feedback loops – such as real-time confirmations, visible community return rates, or summaries of environmental benefits – build care awareness and motivate sustained engagement. Complementary interventions, including deposit schemes or recognition/reward features, can reinforce timely return behaviour when paired with transparent feedback about impact. Integrating these mechanisms closes the care loop and feeds forward into attentiveness, responsibility, and competence in subsequent cycles.
In summary, scholarship on UEM take-back has documented barriers but rarely examines the behavioural drivers of participation through the lens of care theory. This presents an opportunity for design-led interventions that cultivate responsibility, commitment, and ethical engagement in disposal practices. While research in chemistry, medicine, and pharmacy has clarified risks and operational hurdles, a care-informed product–service system (PSS) perspective remains underdeveloped. This study addresses that gap by generating empirically grounded insights to guide designers in improving pharmaceutical return systems. Accordingly, this study aims to identify the barriers and motivations shaping participation in UEM take-back and explore how caring motivational factors can inform the design process that supports responsible return behaviour to advance the CE.
Method
This research employed an exploratory mixed-method approach conducted in three stages: (1) Contextual Inquiry, (2) Survey, and (3) Workshop. Figure 1 presents an overview of the study design and analytic flow. The first two stages – contextual inquiry and survey – were to understand the barriers and the motivation to pharmaceutical return behaviour in U.S. households. Data from both methods were analysed using thematic analysis to identify recurring patterns and insights. These insights were then organised according to Tronto’s (1993) four phases of care. Influential behavioural factors were then identified and categorised under each care phase. This process informed the development of the Caring Factors Return Toolkit, which builds upon and refines the previously developed Caring Factors Inspirational Toolkit (Choi, 2023). In the third stage, this toolkit was further refined through an ideation workshop involving end users and designers, which explored how caring motivations could be translated into the design of product-service systems that promote responsible pharmaceutical disposal. A diagram presenting the research process.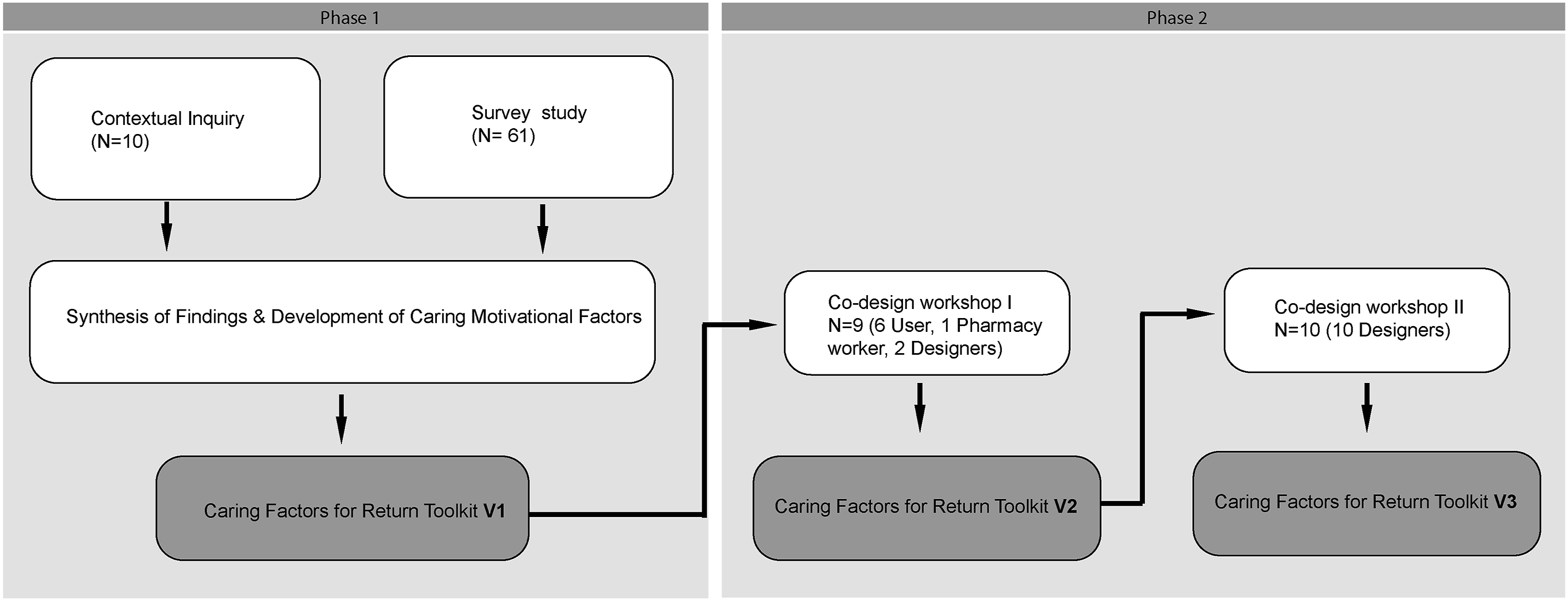
Participants
We recruited individuals via flyers, email listservs, and social media posts. None had previously participated in pharmaceutical take-back programmes, regardless of prior awareness. A total of 66 residents from Blacksburg completed the survey; due to its anonymous design, detailed demographics were not collected. Ten individuals (seven women and three men), aged 20–35 years (M = 25.2, SD = 5.17), took part in contextual inquiry interviews. Nineteen individuals then participated in ideation workshops. The first workshop convened a mixed group – everyday users, a pharmacy worker, and designers – most of whom (all but three) were unfamiliar with pharmaceutical take-back systems, enabling a bottom-up process centred on users’ needs, mutual responsibility, and relational ethics. The second workshop included designers only and was used to further develop the factor set, validate the collection, and examine its application within the design process.
Survey
Before beginning the survey, potential participants were presented with a screening section to determine their eligibility based on predetermined inclusion criteria, that is, at least 18 years old. The survey includes questions on environmental awareness and responsible behaviours, keeping and disposal behaviours, motivations, barriers, and current return system perception, and proposed design strategies to improve the current take-back systems. Participants were expected to spend approximately 20 minutes completing the survey.
Contextual inquiry
Each one-hour contextual inquiry included an introduction and consent, a contextual interview, and a debrief. Participants first described how they store pharmaceuticals at home and then discussed pharmaceutical waste and usual handling procedures. Interview prompts covered types of unused/expired medications (UEM) present, awareness of take-back programmes, motivations and challenges to participation, relevant social/system contexts and perceptions, and proposed design strategies to improve take-back systems. Sessions were audio-recorded. The debrief allowed us to address unanswered items and ask follow-up questions.
Workshop
To further explore motivations and barriers to pharmaceutical return, we conducted two co-design workshops (total n = 19) with individuals unfamiliar with take-back programmes. We selected co-design because it aligns with a care-informed approach by treating participants as knowledgeable partners and foregrounding shared responsibility in shaping return pathways that must fit everyday practices and local constraints. To avoid bias, no one from prior study phases participated. Each three-hour workshop comprised four segments: introduction, barrier/motivation exploration, ideation, and group presentations. Sessions began with an overview of objectives and procedures, followed by informed consent (20 min). We then introduced Tronto’s Five Phases of Care as the conceptual frame. Participants formed small groups (2–3 people) and, using a structured worksheet, identified practical, emotional, and systemic barriers to participation in take-back programmes (30 min). Next, each group created a care map to envision an ethical, user-supportive return system for unused/expired medications, considering how each care phase could motivate return behaviour and meet user needs (40 min). Participants were subsequently introduced to the Caring Factors Return Inspiration Toolkit, organised around four behavioural themes aligned with the care phases – Feedback & Awareness (Phase 1), Social Norms & Commitment (Phase 2), Convenience & Accessibility (Phase 3), and Incentives & Rewards (Phase 4) – and used it to generate system and service concepts addressing identified barriers. Finally, groups selected one promising concept to refine, specifying which barriers it could overcome, the relevant care phase(s), and how the design would be both feasible and engaging (30 min), before presenting outcomes to the whole group.
Data analysis
We used a mixed-methods approach across three phases. Interview and workshop recordings were transcribed and analysed using reflexive thematic analysis (Robson, 2024) informed by Tronto’s care framework. Survey data were analysed using descriptive statistics (mean, standard deviation, frequency, and percentage) to identify user awareness, perceived responsibility, and disposal practices. Two researchers coded utterances line by line and then collated codes into candidate themes related to motivations and barriers, refining the codebook iteratively as new patterns emerged. Likert-scale items were aggregated to indicate levels of agreement and behavioural intention. Survey findings were used to triangulate qualitative results and inform workshop design. Visual materials (e.g. ideation sketches and care maps) were also coded to identify recurring expressions of care, responsibility, and system-level reflections.
Findings
Barriers in the care system
Aligned with Tronto’s phases, reported barriers clustered and were interdependent: without action in Attentiveness (Caring about), progression to Responsibility (Taking care of) stalls; gaps in Responsibility hinder Competence (Care-giving); and weak Competence limits Responsiveness (Care-receiving) and the feedback that would strengthen earlier phases. In Attentiveness, unfamiliarity with safe-disposal practices and drop-off locations, low awareness of what UEMs are at home or whether they are expired, and early privacy worries (e.g. names on labels) constrained recognition that a response was needed. In Responsibility, willingness to act was undermined by poor visibility of clear, actionable instructions and by practical burdens in the infrastructure: limited site availability/hours, the need for a special trip, time–distance costs, and packaging/system requirements (e.g. required separation and unclear eligibility), alongside concerns about diversion/misuse and ongoing privacy risks. In Competence, barriers centred on know-how rather than motivation or access: uncertainty about correct preparation and handover (e.g. whether to remove labels, how to handle liquids/inhalers, and what sites will accept), and a lack of step-by-step guidance at collection points reduced confidence in action. In Responsiveness, the absence of incentives or acknowledgement and limited feedback about who benefits and what environmental/safety outcomes are achieved lowered perceived value and future engagement. Across methods, barriers were most pronounced in Attentiveness – ‘not knowing’ (what to do, what is eligible, what is at home) and inconvenience (time, distance, access) dominated – because Attentiveness functions as the gateway to the care cycle: when a need is not noticed or understood, people neither feel obliged to plan a response (Responsibility), nor acquire or apply the skills to act (Competence), nor receive feedback that would reinforce the behaviour (Responsiveness). In practical terms, if Phase 1 is not activated, movement to subsequent phases is unlikely.
Care motivational factors for returning pharmaceutical products
Attentiveness: Caring about
In this phase, attentional triggers clustered into three themes – Education, Visual Nudges, and Digital Support – that make the need to return unused/expired medications (UEM) visible, credible, and personally salient.
Education
Participants emphasised that proactive promotion by workplaces and academic programmes helps people notice and value take-back practices. Organisational modelling – education, campaigns, clear information, and on-site collection – was a strong cue to act (P3). Visibility at points of everyday activity also mattered; several participants said they would be more likely to act if information were embedded in classes (P5: ‘[It] would affect my knowledge and my actions if there was like some type of information in class’). Messaging that highlights why returns matter – environmental and health benefits – was seen as especially effective: as P1 noted, ‘[…] people [should be] aware that take-back programmes exist and the benefits of taking back medications instead of throwing them away’. Another participant elaborated, ‘It helps educate them on the proper disposal methods and the potential environmental and health risks of improper medication disposal’. Participants also wanted impact feedback (e.g. community totals and environmental savings) to sustain attention.
Visual nudges
Point-of-use guidance reduces cognitive effort. Participants also discussed the importance of having visual feedback on the medication packaging. Putting disposal instructions next to usage directions and adding clear warnings on packs (P2: ‘[…] placing that take-back programme information right beside the directions [would] be a good option’; P8: ‘Have easily visible warning instructions […] to properly dispose [of] meds on packaging’). To surface what needs attention at home, they proposed expiry prompts such as colour-changing labels. At collection points, design and wayfinding should signal ‘this is the place’: P3 remarked, ‘I feel like an eco-friendlier colour, like green or blue, will encourage me to approach the drop box’, while others suggested matching packaging and bin colours and adding feedback displays that show cumulative environmental gains (P4).
Marketing and digital support
Participants viewed take-back efforts as marketing-disadvantaged compared to major brands and suggested pharmacies close the gap with direct emails, flyers, or take-home cards; messages from known senders (e.g. CVS) were seen as credible triggers (P10: ‘[…] if the e-mail came directly from CVS because the emails I get from CVS are like coupons’; P5: ‘Well, I will definitely advertise when you buy the products or maybe put it on the mailbox […] you can bring this in’; P3: ‘I’m more prone to use email now […] TV or social media would be a good option’). Visual nudges were also proposed: clearer, more inviting drop-box design (P3: ‘I feel like an eco-friendlier colour, like green or blue, will encourage me to approach the drop box’), simple wayfinding (e.g. matching packaging and bin colours), and feedback displays that show cumulative environmental gains to reinforce participation (P4). Digital supports that ‘meet people where they manage medications’ were viewed as practical attentional prompts as well, especially when integrated into existing pharmacy or retailer apps (P4: ‘I mean, we’re digitising everything […] if I’m already keeping track of when I take it and [using an app] to remind me to take it’; ‘If you constantly use the CVS app […] or the Walmart app […] they can introduce [a take-back] section’).
Responsibility: Taking Care of
In this phase, willingness to respond to a recognised need was shaped by both convenience and social factors. Across the survey, interviews, and workshops, two convenience themes emerged – Easy, Convenient Process and Space Organization – alongside two social themes – Preventing Misuse and Protecting Others and Social Influence.
Easy, convenient process
Participants identified an easy, convenient process as their primary motivator for return behaviour. Proximity and flexible hours mattered (e.g. P3 described a 24/7 drop-off next to their home as a key motivator), and prior experiences with other take-back/collection schemes highlighted the power of convenience. As P6 explained, ‘[…] donate to the charity shop because they came to my school to collect the donation, so it was easy for me to participate. The easy accessibility will boost the user experience of the pharmacy take-back programme’.
Space Organisation (decluttering)
Clearing space at home was a practical, immediate payoff that nudged action. This desire to ‘get rid of clutter’ and ‘avoid accumulation’ reflects a broader need for household organisation and medication management. P10 noted, ‘It was just good to drop off things and free up space’. Seeing family members participate reinforced the organisational benefit and sense of contribution: P2 reflected that returning UEM ‘definitely open[s] up space and keep[s] track of medicine. I would also feel content in helping the community through this’. However, decluttering alone is not a sufficient driver – without additional cues or supports, medicines may be discarded unsafely rather than returned through the take-back systems.
Preventing Misuse and Protecting Others
Many respondents framed returns as a way to reduce risks to children, visitors, or community members. P4 recounted, ‘A couple of years ago, one of my daughters had wisdom teeth removed, and was [prescribed] an opioid for post-op pain. She did not need it, and we returned it to the pharmacy. We did not want any opioids in the house. While none of us would take them, we do entertain, as did our children, and we feared they might be found by a visitor and taken’. Others echoed the motivation to remove temptation or hazards: P7 emphasised, ‘Getting the medication out of my possession and ensuring they don’t fall into the wrong hands’. Another participant added, ‘Safety concerns if there is anyone who abuses or has had a history of substance abuse. Toddlers or older adults who need up-to-date medicines… Expired ones would create a lot of serious consequences’. As P6 summarised, ‘It helps prevent medication from being mistreated by getting in the wrong hands’.
Social Influence
Participants frequently referred to how the attitudes and behaviours of those around them, such as family members, peers, or even broader community norms, as well as by cues from healthcare providers and pharmacists, influenced their decisions. Community drives created salience and urgency; as P4 observed, ‘Food recycling and clothing collection service tend to get a lot more attention than any pharmacy take-back programmes […] often times Food recycling and clothing collection are organised by like a school or church or a social group’. Household role models mattered: P8 shared, ‘I always learn from my wife… I try to create less waste’. P5 suggested engaging parents as key decision makers: ‘[…] reach out to parents because they’re the ones that buy and dispose of everything’. Intergenerational learning also sustained habits; P2 reflected, ‘We would donate it to charity… I remember my mom doing [that]. Knowing this now, I’m going to pass down the same habit… it’s a habit I have maintained’. Participants also noted that specific guidance from healthcare providers or pharmacy staff – especially pointing out the collection box and explaining the process – would motivate returns.
Competence: Care-giving
This phase moves beyond recognition and willingness to the delivery of care through practical, hands-on action. In our data, competence depended on reducing the cognitive and physical effort of returning UEM and on providing the right tools at the right moment – echoing evidence that the availability of instructions, facilities, and time strongly shapes care quality (Ley, 2023; Meah and Jackson, 2017), two competence themes emerged.
Preparation aids and privacy safeguards
Competent return of unused/expired medications (UEM) depends on unambiguous, standardised instructions that travel with the user and the product. Step-by-step guidance on eligibility (‘what this site accepts’), preparation (e.g. how to handle liquids/inhalers and whether to remove labels), and packaging reduces hesitation and errors. As P4 stated, lightweight privacy aids (de-identification stickers/sleeves, tamper-evident pouches, category-coded bags) address label and sorting concerns, lowering cognitive load and increasing users’ confidence to proceed.
Frictionless hand-off and confirmation
At the point of action, easy-to-use interfaces and just-in-time help make competent performance the path of least resistance: clearly signed, height-accessible or drive-through drop points co-located with familiar waste streams; concise on-site prompts (icons + one-line steps), QR links to 60-s ‘how-to’ clips; and visible ‘ask-me’ cues for staff who can verify eligibility. Immediate feedback (e.g. a printed or in-app confirmation and brief tips for next time) closes the loop and equips users for subsequent returns. Together, these features translate intent into effective, repeatable action.
Responsiveness: Care receiving
In this final phase, participants evaluated the outcomes of returning unused/expired medications (UEM) and described how those outcomes reinforced (or failed to reinforce) future action. Five themes emerged – Feelings of self-reward, Environmental impact, Economic & social benefits, and Incentives – showing how experienced value and feedback close the care loop and feed forward into earlier phases.
Feelings of self-reward
Participants described their motivation to engage in pharmaceutical take-back programmes as deeply tied to personal values and feelings of self-reward. Many framed participation as an expression of personal ethics and civic duty that was satisfying in itself. P3 noted, ‘Incentives like that are nice as a bonus, but for me, it’s like [doing] the recycling or the vaccine’. P5 added, ‘I think [it] ties into [morals]… for the environment and things like that’. Others echoed intrinsic rewards: P9 and P10 mentioned a ‘feeling [of being] responsible and like a good citizen’, and a ‘sense of achievement… satisfaction… pride… in protecting the environment’.
Environmental impact
Protecting ecosystems was a powerful driver. Many expressed a desire to ‘do their part’ by disposing off medications responsibly to prevent harm to ecosystems and other living beings. P1 stated, ‘You are helping the world and environment. I can safely drop the medicines… without harming the environment’. P10 emphasised, ‘Doing my part to protect the environment and other living beings’. Participants also highlighted pollution prevention, as P8 remarked, ‘Get rid of junk in a proper way… [these] items can cause significant harm to environments and others’, and P9 added, ‘Help with preventing medications from polluting the environment’.
Economic and social benefits
Participants highlighted several economic and social considerations that shaped their willingness to engage in pharmaceutical take-back programmes. Some showed a concern for the financial value of medications, expressing reluctance to see money wasted and suggesting they might be more inclined to return unused items if doing so could help offset costs for others. The possibility that returned medications could support individuals unable to afford prescriptions, or be made available at cheaper rates, was viewed as a meaningful social benefit. P4 mentioned, ‘It could help people who are unable to afford medication to get medication at subsidized rates’. Others reflected on cost awareness shaping future behaviour; as P9 put it, ‘Self-awareness of how unused medicine can… harm nature will teach me… to buy less medicine’.
Incentives
Participants mentioned the potential for financial incentives to encourage their involvement in pharmaceutical take-back programmes. Many drew parallels to existing systems, such as bottle deposit refunds or electronics trade-in programmes, suggesting that small financial returns or coupons could be effective motivators. Some also proposed models similar to the take-back programme for milk bottles, where customers received a portion of upfront costs by returning UEM. P2 said, ‘Incentives such as gift cards or similar rewards [will motivate me]’. P8 and P10 compared to returns elsewhere – ‘give some incentive, such as the plastic bottles in California’ and ‘Apple device trade-in programmes’. P1 proposed, ‘Perhaps a deposit similar to milk bottles, where you get some money back when returning the unused or expired product’.
Application of care motivational factors to the design process
The Caring Factors Return Inspiration Toolkit (Figure 2) translates thematic findings on motivations and barriers – from surveys, interviews, and workshops – into actionable design levers aligned with Tronto’s four phases of care for pharmaceutical return. The toolkit supports early-stage ideation by organising influential behavioural factors into four phase-aligned levers: feedback and awareness (Attentiveness), social norms and identity (Responsibility), convenience and accessibility (Competence), and incentives and triggers (Responsiveness). In this framing, each phase corresponds to a distinct relational dynamic that shapes how people become motivated and supported to act responsibly. We iteratively developed and refined the toolkit for participatory ideation, enabling designers and participants to connect observed barriers with targeted levers and generate product–service interventions that help individuals recognise value and act responsibly. We developed a toolkit, rather than a single intervention, because barriers to pharmaceutical return are context-dependent and unlikely to be addressed by one universally applicable solution. Instead, the toolkit translates our empirical and theoretical insights into reusable, phase-specific prompts that practitioners can adapt across settings and implementation constraints. The Caring Factors Return Inspiration Toolkit translates study themes into phase-aligned design levers for pharmaceutical return, organised by Tronto’s four phases of care: Attentiveness (Feedback/Awareness), Responsibility (Social Norms/Identity), Competence (Convenience/Access), and Responsiveness (Incentives/Triggers).
Across two participatory workshops, participants produced concepts mapped to Tronto’s care phases. The most frequently leveraged levers were incentives and triggers and convenience and accessibility, suggesting that these remain the most disrupted aspects of the current return experience. The following sections synthesise workshop ideas by phase in prose form while preserving participants’ wording.
Attentiveness (Caring about) focuses on making needs hard to miss. Participants proposed embedding UEM management into pharmacy and health platforms so prompts appear where people already manage medications, including ‘On the expiry date, add it to a list of unreturned meds to return’ and ‘Before a pickup, remind me to bring old medications’. They described coordinated outreach through text, email, and social media to explain why returns matter and how to do them, and they emphasised visible pride signals such as collectible pins or badges that users can wear and share to motivate others. Participants also called for vivid education – short in-store or in-app visuals, mini videos, and footprint displays – using ‘graphic depictions of what happens when meds aren’t put in the kiosk’, ‘ads and mini videos showcasing the impact’, and ‘footprint displays that show your contribution’.
Responsibility (Taking Care of) focuses on distributing obligation and normalising action. Participants emphasised social proof and public acknowledgement, suggesting features like ‘a display that counts how many items were returned this week and plays a “ding’ when users add theirs’, a kiosk that can ‘vocalize thanks’, and a progress graphic that shows ‘a bar that grows to illustrate how much waste we’ve kept out of the environment’. They underscored the role of trusted messengers, proposing that ‘doctors inform patients when handing over meds’, that ‘store staff give verbal feedback’, and that ‘a sermon at a place of worship mention the take-back programme’.
Competence (Care-giving) focuses on making the right action the easy action. Participants prioritised always-on access through 24/7 drive-through chutes, curbside bins co-located with trash and recycling, and high-traffic placement near grocery cashiers, pharmacy counters, and residential dumpsters. They highlighted integrated errands, including ‘bring old with new’ flows at pharmacies and drive-through lanes that combine pickup and UEM drop-off in a single stop, with a prompt to sort at home beforehand. They also imagined mobile or autonomous handoff – app-scheduled pickup robots or kiosks, USPS-style pickups, and conceptually drones – to bring collection closer to users, with attention to safety and compliance. Campus solutions featured secure card-access kiosks in residence halls with a camera scan to verify eligibility before acceptance and clear, step-by-step on-screen guidance.
Responsiveness (Care-receiving) focuses on closing the loop with feedback and proportionate rewards. Participants suggested creative, incentive-based designs that keep intrinsic motives intact while nudging timely action. They proposed ‘specified time slots where you get double or triple rewards’, loyalty structures where ‘regular returns give discounts on medication orders, but if you stop returning, you lose the discount until you bring items back’, and points that convert into ‘points towards a coupon or discount in rent’, ‘Google Play points’, ‘App Store credit’, or ‘gift cards’. To build social visibility, they recommended ‘stickers or pins to collect or wear to motivate others’, along with ‘automatically entering participants into a raffle for a chance to win a prize’ and delivering ‘app discounts and rewards for participating in the programme’. A minority suggested deterrents, including ‘a fee if the bottle isn’t returned, similar to overdue library books’, which would require careful consideration for equity and unintended effects.
Bringing all four phases together, participants described phase-spanning concepts that combine attentional cues, social reinforcement, low-friction handoffs, and meaningful feedback, as illustrated by examples in Figure 3. One recurring direction was a secure campus or residential network of card-access drop-boxes serviced by pharmacies, with a camera scan to verify items, on-screen instructions, and small rent or insurer discounts when UEM are returned. Another was an app-scheduled pickup robot that users can book ‘when they have UEM to return’, paired with reminders to bring old medications at the next pickup and pride-building collectibles that users can wear and share. These integrated ideas operationalise the toolkit’s levers by helping people notice the need to return, feel responsible within their communities, act competently with minimal effort, and experience outcomes that reinforce the next cycle of care. Participant-generated concept sketches created using the Caring Factors Return Inspiration Toolkit. Panels (A–F) illustrate example directions. Detailed image descriptions are provided in Appendix Table A.2.
Discussion
This study identifies key barriers to pharmaceutical products take-back programmes – low awareness, weak cues, infrastructure limitations, unclear instructions, and lack of feedback – as well as motivational factors such as convenience, safety concerns, and pride in protecting the environment (RQ1). These findings were organised through Tronto’s phases of care: attentiveness (noticing), responsibility (committing), competence (acting), and responsiveness (receiving feedback). In addressing RQ2, these insights were translated into the Caring Factors Return Inspiration Toolkit, which operationalises motivational factors into actionable design levers. This toolkit provides designers with a structured method for generating interventions that embed attentional cues, distribute responsibility, support competent action, and reinforce behaviour through meaningful feedback.
This study contributes a care-informed lens to the design of circular product–service systems (PSS) for pharmaceutical return. By translating user motivations and barriers into the Caring Factors Return Inspiration Toolkit, we explored how phase-specific levers – awareness and feedback (Attentiveness), social norms and identity (Responsibility), convenience and access (Competence), and incentives and triggers (Responsiveness) – can be orchestrated to guide users from noticing a need to acting on it, and then receiving reinforcing feedback for sustained participation.
Role of care in design for pharmaceutical return
Phase-aligned levers clarify where in the journey and what form interventions should take. Attentiveness levers (expiry cues, trusted outreach, on-pack guidance) create motivational readiness. Responsibility levers (social norms, modelling by providers, community visibility) convert readiness into intention. Competence levers (co-location return points, standardised instructions, privacy aids) transform intention into action. Responsiveness levers (confirmations, impact feedback, appropriate rewards) create learning loops that stabilise behaviour over time. This allows designers to move beyond one-off campaigns and instead embed care, reciprocity, and responsibility into everyday routines – advancing both CE goals and user experience. Importantly, responsiveness – whether through emotional feedback (pride, responsibility to others) or system feedback (dashboards, acknowledgements) – feeds back to strengthen earlier phases, sustaining participation across cycles.
Design implications for practice
For design practitioners, this research offers the Caring Factors Return Inspiration Toolkit as a practical resource for early-stage ideation in product–service system design. The toolkit helps designers link user motivations and barriers to concrete interventions: attentiveness levers to make disposal needs visible; responsibility levers to legitimise participation; competence levers to reduce effort and uncertainty; and responsiveness levers to reinforce behaviour over time. By sequencing interventions along Tronto’s phases of care, the toolkit helps to move from user insights to service journeys, touchpoint requirements, and interaction-level mechanisms aligned with each care phase.
Design for attentional readiness – Packaging, apps, and pharmacy interfaces should act as early cues that help users notice and value return opportunities. Designers can make disposal needs hard to miss.
Distribute responsibility through design – Product–service systems should normalise safe return by embedding it into everyday routines, co-locating return points with familiar flows, and highlighting social visibility (feedback displays, provider prompts). Designers can use interaction design to make responsibility shared and legitimate.
Close the feedback loop – Confirmations, eco-feedback dashboards, and proportionate incentives help users see the outcome of their actions and sustain care. Designers should emphasise closure and acknowledgement, making disposal feel rewarding and consequential.
These insights suggest that effective PSS for pharmaceutical return should not only lower barriers but also embed responsibility and reciprocity into everyday interactions.
Notably, many participant concepts leaned towards digitally mediated services (e.g. apps, reminders, tracking, and dashboards). This tendency was partly participant-driven and reflects familiar implementation pathways, but it may also indicate a common design default when information flows and feedback are foregrounded. While digital touchpoints can reduce cognitive load and enable timely prompts and impact feedback, designers should also anticipate equity, privacy, and access constraints (e.g. device access, data plans, and digital literacy). Similarly, incentive-oriented concepts can help overcome inertia but require careful design to avoid fairness concerns, including who benefits, who is excluded, and whether rewards unintentionally disadvantage those with limited access to return infrastructure.
Implications for design for sustainable behaviour
Design for Sustainable Behaviour (DfSB) frameworks such as eco-feedback and choice architecture (Bhamra et al., 2011; Lilley and Wilson, 2017) have demonstrated how subtle cues, prompts, and interface design can reduce cognitive load and steer users towards pro-environmental behaviour. These approaches often operate at the level of individual decision-making, making the ‘right’ choice more visible, easy, or attractive. Our findings suggest that while these strategies remain valuable, they are insufficient to sustain long-term participation in pharmaceutical returns. A care-informed approach extends DfSB in three ways:
Relational grounding – Care emphasises responsibility to others (e.g. family, community, and ecosystems), not only self-interest or convenience. This reframes return behaviour as a moral and relational act, not just a rational choice.
Phased motivation – Tronto’s phases clarify when and how interventions matter: attentiveness (noticing), responsibility (committing), competence (acting), and responsiveness (feedback). This sequencing avoids one-off nudges and provides a roadmap for embedding care across the user journey.
Ethical commitment – Whereas nudges and eco-feedback can risk being manipulative or superficial, care foregrounds empathy, reciprocity, and responsibility as design values. This adds ethical depth to PSS development and supports system goals aligned with the CE.
Thus, care complements rather than replaces DfSB: while nudges and eco-feedback reduce cognitive effort, care ensures that interventions are relational, ethically grounded, and more durable over time. Accordingly, this care-informed approach may also be relevant to other take-back schemes where participation is low and improper disposal produces collective harms (e.g. household battery return and other consumer return streams). In such contexts, phase-aligned levers – attentiveness, responsibility, competence, and responsiveness – can help designers locate where the return journey breaks down, from noticing options and accepting obligation to completing a frictionless handoff and receiving reinforcing feedback. Overall, the approach offers a reusable scaffold for circular return challenges, while still requiring adaptation to local infrastructures and constraints.
Implication for system change
Care ethics, combined with systems thinking (Meadows, Donella H., 1999; Tronto, 1993), highlights how caring motivations – pride, environmental concern, responsibility to others – gain traction when system conditions reduce friction and make outcomes visible. In system-thinking terms (Meadows, Donella H., 1999), several leverage points emerge:
Information flows can be re-designed through real-time reminders, expiry cues, and eco-feedback dashboards that translate individual acts into environmental and community outcomes (Bhamra et al., 2011; Lilley and Wilson, 2017). Rules and incentives can be tuned so the easy, default path is the responsible one while light, proportionate rewards acknowledge effort without crowding out intrinsic motives (Deci et al., 1999; Dolan et al., 2012). Self-organisation and roles can be strengthened via co-design – engaging pharmacies, insurers, campuses, and community groups to co-create local return infrastructures and governance (Manzini, 2015). System goals/paradigms can be reframed from waste end-of-pipe to care-oriented circulation consistent with the CE (Geissdoerfer et al., 2017; Tukker, 2015). These implications shift design practice from isolated interventions towards system-level orchestration, where return behaviour is embedded in everyday contexts and reinforced through feedback.
Future opportunities
Future work will test the Caring Factors Return Inspiration Toolkit in real settings, tracking not only return rates but also time-to-return, repeat participation, privacy and safety issues, and costs. In parallel, we will co-design practical roadmaps that spell out roles, data stewardship, funding, service flows, and chain-of-custody and assess how well these hold up over time. A systems view is essential: coordinated interventions across pharmacies, clinicians and EHR/apps, insurers, manufacturers, municipalities, and community groups should be mapped to clear leverage points (information flows, rules/incentives, self-organisation, goals). We will also examine how upstream system conditions – particularly medication affordability, insurance design, and access to timely care – shape UEM accumulation and ‘keep just in case’ logics, and how these determinants interact with downstream take-back service design and prescribing/refill practices. Finally, we will examine equity and access across contexts and cultures, refine phase-aligned measures of attentiveness, responsibility, competence, and responsiveness, and turn the toolkit into reusable patterns (cards, heuristics, UI components) tested in live projects.
Limitation
This work has geographic, cultural, and system-level constraints. Participants were recruited primarily in [Location]; transferability to other U.S. regions and international contexts is not assumed. Furthermore, return behaviour is shaped by healthcare and policy conditions (e.g. prescription/refill norms, insurance coverage, out-of-pocket costs, and access to providers/pharmacies) as well as cultural practices (e.g. saving ‘just in case’, sharing within households, and trust in institutions). These conditions can shift motivations across the care phases – for example, higher perceived medication value may strengthen ‘keeping’ rationales, while clearer national guidance and ubiquitous pharmacy return options may lower competence burdens. U.S. drug prices are substantially higher than in comparable countries, which may amplify sunk-cost and risk-management motivations to retain medications. At the same time, this U.S. focus offers an opportunity for knowledge transfer and design inspiration. Several countries operate more standardised pharmacy-based return arrangements (e.g. Australia’s national pharmacy return infrastructure), suggesting possible directions for the U.S. context, such as more consistent ‘return-to-pharmacy’ norms, clearer public-facing instructions, and stable stewardship funding mechanisms that reduce friction and improve feedback.
This study relied on self-report and workshop concepts rather than fielded prototypes; future work should test toolkit-derived interventions in situ, examine longitudinal adherence, and compare how care-phase levers perform across cultural and healthcare-system contexts.
Conclusion
This study reframes pharmaceutical return as a practice of care, showing how Tronto’s phases – attentiveness, responsibility, competence, and responsiveness – clarify where and how to intervene. By translating barriers and motivations into the Caring Factors Return Inspiration Toolkit, we provide a structured method for embedding care into circular product–service systems.
The study makes three contributions. First, it extends scholarship on pharmaceutical take-back by shifting the focus from structural barriers to the relational and motivational dynamics that shape participation. Second, it expands Design for Sustainable Behaviour by showing how care offers relational grounding, phased motivation, and ethical depth beyond nudges and eco-feedback. Third, it delivers a practical toolkit that designers can apply in early-stage ideation to embed attentional cues, distribute responsibility, support competent action, and close feedback loops. For design practice, the findings highlight the importance of sequencing interventions across the phases of care. Designers can support attentional readiness through expiry prompts and on-pack guidance, normalise responsibility through co-located return flows and social visibility, enhance competence with clear preparation aids and privacy safeguards, and strengthen responsiveness through feedback and proportionate incentives. Taken together, these strategies move beyond one-off campaigns to create circular product–service systems that are ethical, relational, and sustainable.
Footnotes
Acknowledgements
We thank all participants who completed the survey, welcomed us into their homes for contextual inquiries, and engaged in the workshops.
Ethical considerations
The study was approved by the Institutional Review Board of Virginia Tech (protocol code 24-986; date of approval: 8 October 2024).
Consent to participate
Informed consent was obtained from all subjects involved in the study. Written informed consent has been obtained from the participant to publish this paper.
Author contributions
Conceptualisation, Y.J. Choi; methodology, Y.J. Choi; software, J. Dong and J. Pyon; validation, Y.J. Choi and J. Dong; formal analysis, J. Dong and J. Pyon; investigation, J. Dong and J. Pyon; resources, Y.J. Choi, J. Dong, and J. Pyon; data curation, Y.J. Choi, J. Dong and J. Pyon; writing – original draft preparation, Y.J. Choi and J. Dong; writing – review and editing, Y.J. Choi; visualisation, Y.J. Choi; supervision, Y.J. Choi; project administration, Y.J. Choi; funding acquisition, Y.J. Choi. All authors have read and agreed to the published version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was made possible by funding provided by Virginia Tech, Funding no 180584.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data is unavailable due to privacy or ethical restrictions. De-identified materials may be available from the corresponding author upon reasonable request and, where required, Institutional Review Board approval.
Appendix
Detailed description of contextual inquiry participants. Note. UEM: unused and expired medications.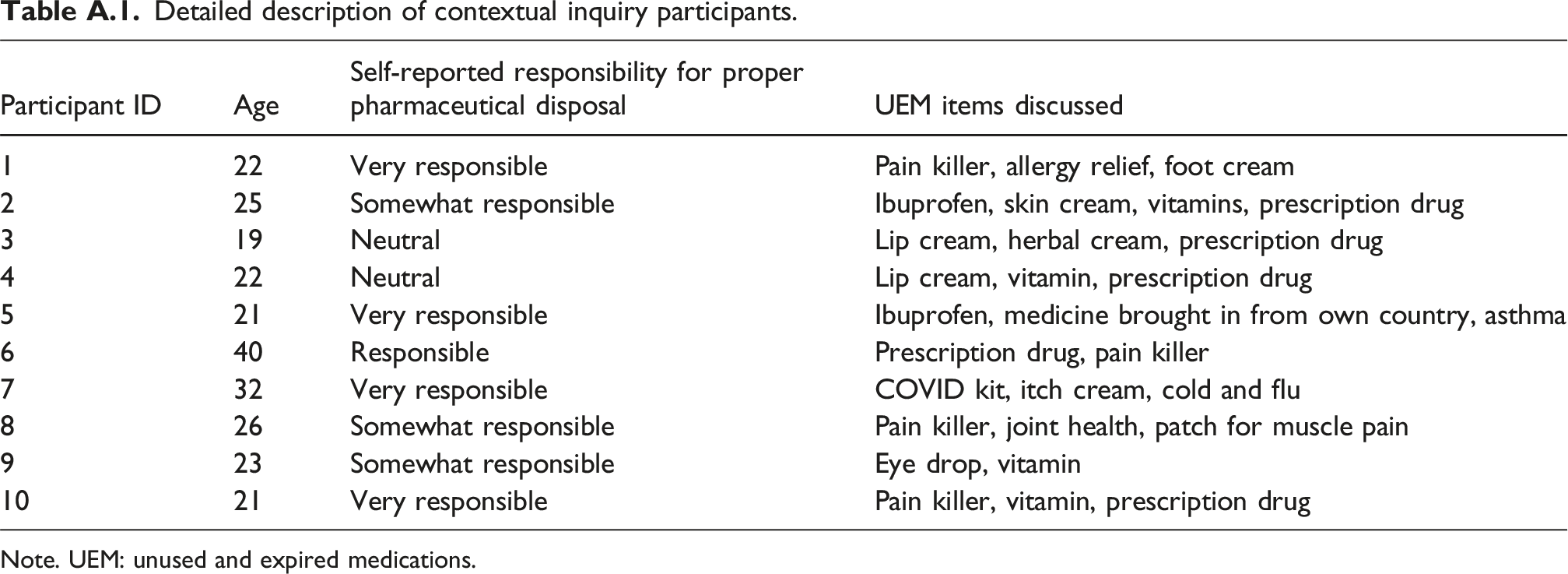
Participant ID
Age
Self-reported responsibility for proper pharmaceutical disposal
UEM items discussed
1
22
Very responsible
Pain killer, allergy relief, foot cream
2
25
Somewhat responsible
Ibuprofen, skin cream, vitamins, prescription drug
3
19
Neutral
Lip cream, herbal cream, prescription drug
4
22
Neutral
Lip cream, vitamin, prescription drug
5
21
Very responsible
Ibuprofen, medicine brought in from own country, asthma
6
40
Responsible
Prescription drug, pain killer
7
32
Very responsible
COVID kit, itch cream, cold and flu
8
26
Somewhat responsible
Pain killer, joint health, patch for muscle pain
9
23
Somewhat responsible
Eye drop, vitamin
10
21
Very responsible
Pain killer, vitamin, prescription drug
Detailed description of images shown in Figure 3.
Image
Description
Used themes
A
Collection box in a public, convenient space with a CCTV camera for security. A gamified app tracks behaviour and links to the insurance provider for discounts.
Awareness/Feedback
Convenience/access
Incentive/Trigger
B
App-scheduled pickup robot users can book when they have UEM to return, paired with reminders to bring old medications at the next pickup.
Awareness/Feedback
Convenience/access
Incentive/Trigger
C
App-scheduled pickup and delivery robot users can book when they have UEM to return, paired with reminders to bring old medications at the next pickup and a discount on the next delivery.
Awareness/Feedback
Convenience/access
Incentive/Trigger
Social norm/identity
D
Secure, 24/7 drive-through collection point located near an apartment, office, or school.
Convenience/access
E
Seasonal campaign from a local pharmacy reminding residents to sort through their UEM; offers pride-building collectible badges users can wear and share to spread the word.
Feedback/awareness
Social norm/identity
Incentive/trigger
F
UEM collection box next to an apartment building, secured by keypad and scan access; positive behaviour is recorded and eligible residents receive a rent discount.
Incentive/trigger
Awareness/Feedback
Convenience/access
Social norm
