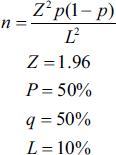Abstract
Background
It is essential to use orthodontic composites that possess favorable properties specifically; those that can be easily removed at the end of treatment but remain securely bonded during the course of treatment. Nanoparticles have gained attention for their antibacterial effects when incorporated into composite resins. However, the impact of nanoparticle incorporation in the adhesive and its relation with bracket failure rate has not been widely explored.
Aim
The aim of this study was to evaluate and compare clinical bracket failure rate of orthodontic adhesive modified with silver nanoparticles (AgNPs) with conventional orthodontic adhesive without AgNPs.
Materials and Methods
This in vivo study included patients aged between 15 and 35 years with mild-to-moderate crowding and healthy periodontium, requiring fixed orthodontic treatment with 0.022” × 0.028” slot metal brackets. Synthesis of colloidal AgNPs was performed using sodium tetrahydridoborate (NaBH4) as the reducing agent. 0.09% w/w of AgNP were manually mixed in one syringe of orthodontic adhesive (3M Unitek Transbond XT) using mortar and pestle. Twenty patients (10 each group) were selected who met the inclusion criteria and allocated to the control and experimental groups using the lottery method. A total of 195 teeth (96 control, 99 experimental) were bonded. Brackets in the experimental group used adhesive (3M Transbond XT) modified with AgNP, while the control group used conventional adhesive (3M Transbond XT). Bracket failure rate was recorded over 4.5 months. The wire sequence used was 0.012 Niti, 0.016 Niti, 0.018 SS, 17x25 Niti, 19x25 Niti, and lastly 19x25 SS. Descriptive statistics, Kaplan–Meier plots, and log-rank tests were used to compare failure rates.
Result
Bracket failure rates were assessed using the Kaplan–Meier plots which showed the survival (failure) rate of control and experimental group being 81.3% and 82%, respectively. There is no statistically significant difference in survival estimates of control and experimental group. Both survival curves start at 100% and show minimal decline across the 140-day period. The debonding occurred more on the initial aligning wires, that is, 0.016 Niti (control group) and 0.012 Niti (experimental group) between 24 and 75 days in average. Rate of bracket failure was higher in posterior teeth (15%) as compared to anterior teeth (3%).
Conclusion
The study found that orthodontic adhesive containing AgNP exhibited a 0.7% lower bracket failure rate compared to conventional adhesive. Bracket failures were more frequent in posterior teeth than anterior teeth. Further long-term studies with larger sample sizes are recommended to validate the effectiveness of AgNPs in orthodontic adhesives.
Introduction
Since the introduction of composite resin adhesives, they have remained the preferred choice for orthodontists when bonding brackets. However, one of the key challenges in clinical orthodontics is bracket failure, which not only prolongs treatment but also increases the risk of enamel damage due to repeated acid etching. 1 Several factors influence bracket failure rates, including bracket and bonding material, arch type (maxillary or mandibular), tooth position (anterior or posterior), and patient age.2, 3
Bracket failure has been reported in 0.6% to 28.3% of cases where light- or chemically-cured composite resins are used.4, 5 Common causes include improper force application, inadequate bonding technique, exposure to thermal fatigue and cyclic loading in the oral environment, and caries formation around bonded teeth. A bracket rebonded due to failure can increase the treatment duration from 0.3 to 0.6 months.6, 7 Bukhari et al. 8 reported that for every six months increase in treatment time, patient compliance to follow their appointments decreased by 23%. Thus, the cost of treatment is enormously increased both for orthodontic practice and for the patient.
Fixed orthodontic appliances complicate oral hygiene maintenance, leading to bacterial plaque accumulation around brackets and subsequent enamel decalcification, primarily at the adhesive-enamel interface.9, 10 Streptococcus mutans is the primary contributor to enamel demineralization and increased composite resin surface roughness. 11
To address this issue, researchers have explored incorporating antibacterial agents into orthodontic adhesives to control bacterial colonization and prevent white spot lesions. 12 Fluorides and chlorhexidine have been tested, but their biological effectiveness remains questionable, and they often compromise the mechanical properties of adhesives. 13 With advancements in nanotechnology, nanoparticles such as hydroxyapatite and nanosilver have been investigated for their antibacterial potential. Among these, silver nanoparticles (AgNPs) have demonstrated strong antibacterial activity against cariogenic bacteria. 14
Nafarrate-Valdez et al. 15 examined the antiadherence properties of AgNPs and found them effective in preventing S. mutans adhesion on orthodontic materials. Despite these promising antibacterial and antiadherence properties, some studies suggest that incorporating AgNPs into orthodontic adhesives may reduce the bond strength necessary to maintain bracket adhesion to enamel.
Resin composites containing silver ion-implanted fillers, which release silver ions, have exhibited antibacterial effects against oral streptococci. However, no studies have systematically evaluated the bracket failure rate of these modified adhesives. Therefore, this study aims to assess the impact of incorporating AgNPs into orthodontic adhesive systems on bracket failure rates, comparing them to conventional adhesives without nanoparticles.
The null hypothesis states that the addition of AgNPs to dental adhesives used for bonding orthodontic brackets will have no effect on shear bond strength.
Materials and Methods
This study took place at the Department of Orthodontics and Dentofacial Orthopedics. This study was approved by the Institutional Ethics Committee (IEC) on 26/12/2024. All participants provided written informed consent prior to enrollment in the study.
Inclusion Criteria
The sample included patients (15–35 years) with mild-to-moderate crowding and a healthy periodontium, who required fixed orthodontic treatment (0.022’’ × 0.028” slot metal brackets) at the Department of Orthodontics and Dentofacial Orthopedics.
Exclusion Criteria
The sample excluded patients with a compromised periodontium, clefts, syndromes, brackets debonded by the clinician, brackets bonded using a different adhesive or protocol, brackets from a different company, or patients who were allergic to silver and nickel.
Sample Size
Minimum 192 teeth (96 each group) were taken to estimate 50% bonding failure rate of AgNPs containing orthodontic adhesive at 95% confidence and 10% absolute precision.
Statistical Plan
Descriptive statistics like frequency, percentage
Kaplan Meier Plot
Log-rank test
Synthesis of Silver Nanoparticles
In this study, colloidal AgNPs were synthesized using sodium borohydride (NaBH4) as the reducing agent. A 10–³ M silver nitrate (AgNO3) solution was stirred at 70 °C, and 5 mL of 2 × 10–³ M NaBH4 was gradually added. The appearance of a grey precipitate indicated AgNP formation.
Mixing of Ag Nanoparticles to Adhesive
Four microliter of AgNP (0.09% w/w) was manually mixed in 4 gm of orthodontic adhesive (3M Unitek Transbond XT) using mortar and pestle.
Methodology
In this in vivo study, 20 patients (10 in each group) undergoing orthodontic treatment with a 0.022 × 0.028” slot MBT bracket system and meeting the inclusion criteria were selected.
These patients were allocated to the control and experimental groups using the lottery method, and all the maxillary teeth of control group patients were bonded using conventional adhesive and all maxillary teeth of experimental group patients were bonded using adhesive modified with AgNP. Therefore, a total of 195 teeth were bonded (96 in the control group and 99 in the experimental group).
All the teeth present in maxillary arch from 15 to 25 were cleaned and etched with 37% phosphoric acid, then bonding agent (OrthoSolo, Ormco) was applied and cured for 15 seconds. Further the brackets were bonded with modified adhesive (Transbond XT, 3M Unitek, Monrovia, CA, USA) containing AgNPs in experimental group, whereas brackets were bonded with conventional adhesive (Transbond XT, 3M Unitek, Monrovia, CA, USA) without AgNPs in control group.
The wire sequence used for all the patients was 0.012 Niti, 0.016 Niti, 0.018 SS, 0.019 x 0.025 Niti, and 0.019 x 0.025 SS.
All the patients were instructed to have same diet (vegetarian), avoid sticky foods and to brush twice a day using modified bass technique.
Patients were called when the bracket was debonded within the span of 4.5 months till they reached 0.019 × 0.025 SS wire and number of bracket failure rate was recorded.(T1) The following details were recorded for each patient:
Biographical details (name, age, and gender) Dominant hand Skeletal pattern (Class I and II) Time of bracket failure Tooth number Type of wire
Once the bracket had been debonded, no further assessment was done for that particular bracket and failure rates of both group were evaluated and compared.
Result
Table 1 shows association between bracket failure and different variables in control group. The results show that out of 96 teeth, debonding was observed in 22 teeth. The results also show that posterior teeth (14.5%) had more debonding rate than anterior teeth (5.2%). The debonding occurred more on initial aligning wires, that is, 0.016 Niti (31.25%).
Association Between Bracket Failure and Different Variables in Control Group.
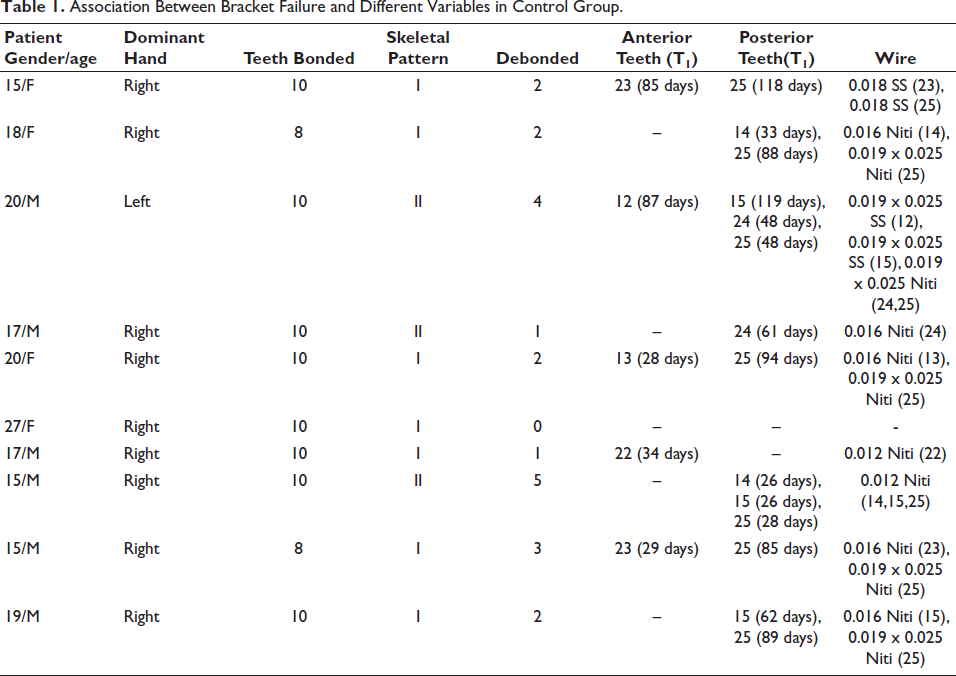
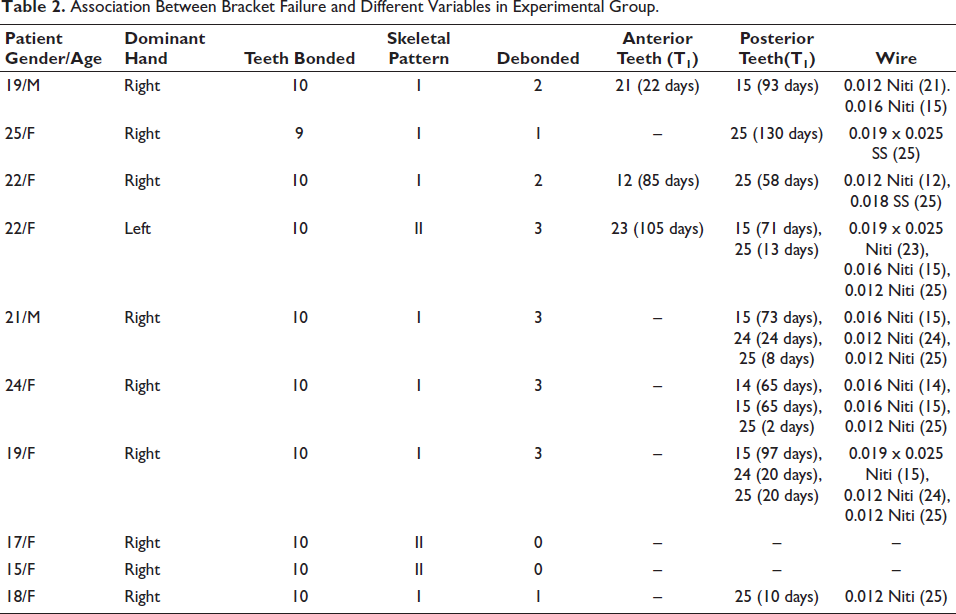
Table 2 shows association between bracket failure and different variables in experimental group. The results show that out of 99 teeth, debonding was observed in 18 teeth. The results show that posterior teeth (15%) had more debonding rate than anterior teeth (3%). The debonding occurred more on initial aligning wire, that is, 0.012 Niti (50%).
Association Between Bracket Failure and Different Variables in Experimental Group.
Data was analyzed using SPSS 26.0. In descriptive statistics, the overall frequencies as well as the frequencies for the censored group were reported along with the survival times for qualitative independent variables. Kaplan–Meier plots were used to assess the survival time graphically for bracket material and log-rank test was used to assess any significant difference in the survival times of the brackets within these groups.
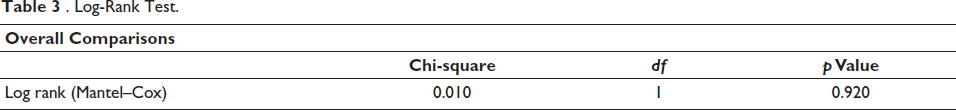
Table 3 shows that there is no significant difference in survival between the two groups being compared. The survival experience is statistically equivalent, based on the log-rank test (p = .920).
Log-Rank Test.

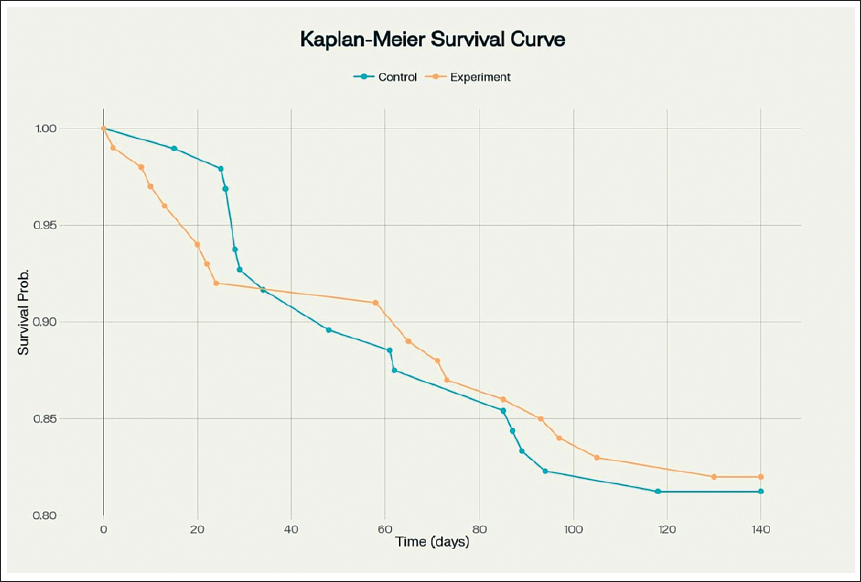
The Kaplan–Meier estimates were plotted for the categorical variables and log-rank test was used to assess any significant differences among the groups. The curves for control group and experimental group are closely aligned (Figure 1). The survival (failure) rate of control and experimental group is 81.3% and 82%, respectively. There is no statistically significant difference in survival estimates of control and experimental group. Both survival curves start at 100% and show minimal decline across the 140-day period.
Bracket Failure Rate Over Time.
Discussion
In orthodontics, bracket debonding is a major cause of repeated orthodontic emergencies. It can prolong overall treatment time, increase chairside workload and treatment costs, potentially compromise treatment outcomes, and even lead to enamel damage. Bracket failure is a multifactorial issue influenced by a combination of operator-, patient-, and material-related factors. Patient-related causes include malocclusion, poor oral hygiene, harmful oral habits, lack of compliance, age, masticatory forces, and prior dental procedures such as restorative treatments or bleaching. Operator-related factors include bonding technique, type of adhesive used, curing light effectiveness, and the properties of brackets and wires. Several studies have investigated the various contributors to bracket failure during orthodontic treatment, with most focusing on the effects of age, gender, tooth type, bracket type, and bonding materials.
This study measured the clinical bracket failure rate of a new orthodontic adhesive (Transbond XT) modified with AgNP and compared it with conventional adhesive (Transbond XT) without AgNP. AgNPs have been chosen as they have shown to inhibit biofilm viability and growth, especially Streptococcus mutans. 16 In addition to antibacterial properties, it is essential that the nanoparticles added to the composite maintain a reasonable shear bond strength or in a more favorable condition, to improve this property. In this study, the effect of adding concentrations of 0.09% AgNP in the adhesive has been evaluated.
The concentration of nanosilver particles chosen in the current study was 0.5 µg/mL as Magalhaes et al. 17 showed that this concentration had better antibacterial activity with silver incorporation than commercial adhesives.
Our study indicated that the bracket failure(survival) rate of control and experimental group was 81.3% and 82% indicating that the new adhesive containing AgNPs show 0.7% less bracket failure. The results suggest that risk of bracket failure is 5.2% in anterior teeth and 14.5% in posterior teeth in the control group indicating more bracket failures in posterior teeth. In the experimental group, similar risk of bracket failure rates is seen, i.e. 3% in anterior teeth and 15% in posterior teeth.
Bherwani et al. 3 studied 1,074 brackets in 63 subjects using the Kaplan–Meier test and reported a statistically significant (p <.05) increase in failure rates in the posterior region as compared to the anterior region, which is in accordance with our study results. This may be due to greater masticatory forces in posterior teeth. In a study conducted by Vijayakumar et al. 18 comparing the anterior and posterior brackets, the indirect method showed more bond survival rate than direct, in the anterior than posterior.
When we consider bracket failure on which wire is more likely, our study concluded that there were higher debonding rates in the initial wire stages, that is, 0.016 Niti for the control group and 0.012 Niti for the experimental group.
Xiao et al. 19 studied the bracket failure rates among adolescents and adults and reported a significantly (p <.05) increased bracket failure in the posterior region in adolescents as compared to adults. In our study, 58.3% of the bracket failure occurred in adolescent patients (<18 years).
In this study, the failure rates were evaluated for a period of 140 days with a greater variability of debonding occurring within 2–130 days in posterior teeth in experimental group. Most failures occurred between 24 and 75 days after bonding.
Considering hand dominance, both the control and experimental groups consisted of nine right-handed and one left-handed patient. Among these, 54.5% of brackets in the control group and 55.5% in the experimental group were debonded on the side opposite to the dominant hand. This suggests that there is a higher likelihood of debonding on the contralateral side of the dominant hand, as greater force is typically applied during brushing on that side.
From the results of this study, it can be said that the most important actions in order to prevent debonding are careful verbal and written instructions to each patient regarding appliance care. The motivation of the patient is one of the reasons for better cooperation and a lower rate of bracket failure. Lastly from the operator’s perspective, orthodontic adhesive modified with AgNPs can be used to prevent enamel demineralization further leading to white spot lesions without the patient compliance. Despite fewer failures overall, the experimental group showed earlier failures in some cases;, this may warrant further study on adhesive setting time or strength under early stress.
Limitations of this study include small sample size, patient’s dietary habits, and the polymerization time mode may affect the mechanical properties of composite materials. On the other hand, Koupis et al. 20 have reported a higher failure rate in the mandibular arch as compared to maxillary arch which gives future scope of more studies evaluating failure rates in mandibular arch with more crowding.
Conclusion
The key conclusions of the study are as follows :
The study concluded that the bracket failure rate of orthodontic adhesive (Transbond XT) containing AgNPs showed 0.7% low bracket failure rate compared to conventional adhesive within a span of 4.5 months.
Rate of bracket failure was higher in posterior teeth (15%) as compared to anterior teeth (3%).
Considering the age factor, almost 58.3% of the bracket failure occurred in adolescent patients (<18 years).
Further long-term studies are required to evaluate the properties of AgNPs for the same with larger sample size.
Footnotes
Authors’ Contribution
Urja Modi was involved in methodology.
Udita Thakkar conceptualized the study.
Harshit Naik helped in editing – reviewing.
Kalpesh Patel supervised the study.
Data Availability
Available at Manubhai Patel Dental College, Vadodara, Gujarat, India.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The research was approved by the Institutional Ethics Committee (IEC) for research on 26/12/2024 (Ref No. IEC/MPDC_301/ORTHO-62/24).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed consent was obtained from all participants prior to the commencement of the study.