Abstract
Self-medication is a common phenomenon; the risks are greater in the older people. This study was conducted aimed to determine the relationship between self-medication and frequent hospitalization of the older people in Yazd. The samples size was 348. Sampling by stratified sampling was selected from the teaching hospitals of Yazd based on the attendance list of older people in these centers. The data of this research was collected by a researcher-made questionnaire. The prevalence of self-medication was 77.58%. Painkillers, pills, cold syrups, and herbal infusions were the most used drugs in self- medication. Colds, headaches and digestive problems were the problems that were treated with self-medication more than others. There was no significant relationship between frequent hospitalization and self-medication. Considering the high prevalence of self-medication among hospitalized older people, it is necessary to increase the awareness of the society about the dangers of self-medication, which is possible only through education.
What this paper adds
- The most important factors related to self- medication were determined, the belief that diseases are not important, the experiences of friends and acquaintances, the availability and belief in the safety of herbal medicines, and the expensiveness of visiting doctors.
- The most important sources of information for self- medication were friends and acquaintances (40%) and mass media (22%).
- The most frequent causes of hospitalization were cardiovascular diseases, endocrine and respiratory diseases, respectively.
Applications of study findings
- The arbitrary consumption of herbal medicines is very high due to the perception that they are safe, and it is necessary to provide sufficient information to increase awareness among people, especially the elderly.
- The results of this research can help experts in the field of health and health educators in designing educational programs to consider appropriate planning to improve the health status of older people in the society.
Introduction
The older people population is increasing in Iran as in other countries of the world, so it is predicted that the percentage of older people will increase from 7.8% to 28% respectively in 2050 (Fakhari et al., 2023). The concept of healthy aging has become important both in everyday life and in the academic world and policymaking of aging health. Healthy aging goes beyond the presence or absence of disease and is influenced by various factors (Edwards et al., 2021; Santini et al., 2020). During the aging period, some body organs such as cardio-reno vascular system are affected by the aging process, which play a significant role in the occurrence of changes in the bioavailability of drugs (Singam et al., 2020; Stielow et al., 2023). Various studies emphasize the fact that during the aging period, the costs of treatment and medication use increased, as well as chronic diseases, leading to pain and disability and loss of quality of life (Christopher et al., 2022; Dagnino & Campos, 2022; Uragami et al., 2021). Medication use is one of the most important methods of disease treatment, but irrational and arbitrary medication use or self-medication may cause drug side effects (Brandão et al., 2020; Christopher et al., 2022). Self-medication is a behavior in which a person tries to reduce his health problem without prescription of a doctor or specialist. Lack of awareness, economic, cultural and social issues have an effect on the prevalence of self-medication in societies (Chang et al., 2017).
In practice, self-medication, as the most common method of self-care, can be done by consuming an industrial or homemade medicine, obtaining medicines without a specialist prescription, dividing prescribed medicines for one person among family members and Friends, the use of additional medicines at home and the use of previously prescribed drugs were defined. The world health organization (WHO) definition of self-medication is “ the selection and use of medicines by individuals to treat self-recognized illnesses and symptoms” (Azócar et al., 2023). Self-medication is common in the world, 54.4% of people in Ghana and 58.6% of people in Chinese and 63.5% of people in Malaysia also self-medicate (Brandão et al., 2020; Mok et al., 2020; Morgan et al., 2023). Self-medication by drugs has been a problem of health importance, and causes factors such as increasing per-capita drug use, drug resistance, lack of optimal treatment effect, poisonings, and side effects. There was high prevalence of self-medication in countries with less socio-economic development (Karimy et al., 2019; Vahedi et al., 2021).
Scientific studies have revealed the various prevalence rates of self-medication, and that there are some factors leading to arbitrary use of drugs among Iranians older people. For example, rate of self-medication among Iranians estimated in different studies were 28.5%, 94.4%, and 55.5% (Ghorbani et al., 2019; Heshmatifar et al., 2021; Payvar et al., 2022). The other study showed the prevalence of self-medication in public population was 41% in Iran (Nakhaee & Vatankhah, 2019). Self-medication is very common in Iran due to the lack of proper monitoring of drug consumption and the possibility of buying different types of drugs without a prescription. Also, self-medication and taking drugs in some cases leads to frequent hospitalization which defined as hospitalization more than twice a year (Mortazavi et al., 2017; Yazdan Nasab et al., 2019). Older people consume more drugs than other age groups. On the other hand, because older people have multiple chronic diseases, they usually use chemical drugs along with traditional drugs. There are risks of dangerous drug reactions and drug interactions in older people are more than others. One of the results of self-medication is drug reactions and poisoning (Rafati et al., 2023). Increasing hospital admissions is a complex and important issue that increases health budgets. It is one of the problems faced by health services in the world. According to the conducted research, previous admission in the hospital is a predictor of readmission and frequent hospitalization (Longman et al., 2012).
Since social and cultural factors can influence the level of self-medication, and in different regions, the level of self-medication can have different values. Therefore, this study was conducted aimed to determine the relationship between self-medication and frequent hospitalization of the older people in Yazd.
Method and Material
Study Design
This cross-sectional descriptive-analytical study was carried out from December 2021 to December 2022 based on survey design. The inclusion criteria were patients who were hospitalized in Kerman University of Medical Sciences hospital, 60-year-old and more. The purpose of research was described to all the participants and informed consents were obtained.
Participants
The sample size in this research was 348 older people patients hospitalized in the government hospitals of Yazd city. Sampling by stratified sampling was selected from the teaching hospitals of Yazd based on the attendance list of older people in these centers. It should be noted that sampling was done on even days. After obtaining the code of ethics from Kerman University of Medical Sciences for dialysis centers in Kerman, the researcher extracted the information of the patients according to the admission criteria.
Sample Size
According to similar study related to self-treatment and frequent hospitalization (Jafari et al., 2015) and using the following sample size formula, the power of the test was 80%, the sample size was 200 people. Due to the possibility of non-cooperation of the elderly, 20% dropout was taken into account and the final sample size was 240 people, for more certainty, 348 people participated in the research.
n-sample size,
Instruments
A researcher-made questionnaire was used to collect information. The questionnaire consisted of several parts. A) Questionnaire related to demographic characteristics: This part of the questionnaire was related to background information. There were questions about age, level of education, marital status, employment status, and income, having or not having insurance. The questions related to this part were eight questions.
b) The area related to the type of drugs used: this part of the questionnaire included 9 questions that were asked separately from each drug and the degree of its use was also questioned.
c) The area related to hospitalization factors: In this part, the number of hospitalizations as well as underlying factors and diseases that led to hospitalization were asked, this part included 3 questions.
d) The area related to factors related to the disease: this part expressed the type of underlying diseases separately in the studied subjects. The importance of this part was in the type of people’s underlying diseases, which mostly led to self-medication. This part consisted of 4 questions.
e) The area related to drug information: this part of the questionnaire included the ways of familiarizing the subjects with drugs, followed by self-administration of drugs and finally frequent hospitalization. Among the factors that were questioned were acquaintance or self-medication through friends and acquaintances, previous experience of using medicine, mass media, internet, books and magazines, and medical centers. This part was asked in the form of 3 questions.
The rest of the questions were supplementary and emphatic questions in the above fields so that the authors can be sure of the correctness of the answers. To score the questions, the items never (0), very little (1), little (2), average (3), high (4), very high (5) were used. The lowest score that could be calculated in the questionnaire was zero and the highest score was 105.
Reliability and Validity of Measure
To measure the validity of the questionnaire, the content validity method was used, so that first the questionnaires were given to 10 experts in gerontology and health education from Medical Sciences of Kerman and Kerman University of Medical Sciences to determine the qualitative validity of the content. which were defective, were corrected and inappropriate questions were removed and replaced by other questions. Then, in order to determine the quantitative validity of the content, they were asked to first examine the questions of the questionnaire in terms of these issues: which questions are necessary to be in the questionnaire, which questions are useful but unnecessary, and which questions are unnecessary and better. is to be deleted.
Second, whether the set of questions of each structure reflects the corresponding structure, and finally, the simplicity, clarity and cultural appropriateness of each question were evaluated. Due to the fact that the number of experts was 10, the minimum value determined for the content validity ratio (CVR) according to the criterion in the Lawshe table, was considered to be 0.62. CVR was calculated for each of the items, which was higher than 0.62 and was acceptable. The calculation of CVI for the self-medication questionnaire indicated that all items had a CVI score higher than 0.79, so they were considered suitable. To measure the reliability of the questionnaire, Cronbach’s alpha was used to calculate the answers given by 20 people from the research samples. Finally, according to the reliability of 0.89 which was calculated in this study, the questionnaire had good reliability.
Data Collection
Researcher-made questionnaire was completed by self-reporting form, and for people who were not literate, the questionnaire was read to them by the questioner. included questions related to the practices, name of the medications used, an ill condition related to the practice, reasons for self-medication practices, source of medication and information and frequent hospitalization due to self-medication. Finally, completed questionnaires were collected.
Data Analysis
Data was checked for completeness and cleaned manually, and finally, it was coded and entered into SPSS version 20. In order to describe the variables of the research, frequency indicators (percentage), mean and standard deviation were used and for their analysis, chi square tests, t-test of two independent samples and Pearson’s correlation coefficient or Spearman’s correlation coefficient were used. In this study p ≤ .05 was considered as statistically significant.
Result
A total of 348 questionnaires were distributed to assess the self-medication practice in which 270 of patients had a history of self-medication in the last year who included to this study. In demographic findings, the mean and standard deviation of patients were 72.4 ± 4.6-year-old. Women (51.1%) consisted majority of patients in this study. The most of the self-medicated patients had middle school education. Majority of participated had further average level of income (10–15 million tomans) and the most of occupation of the patients were retired (44.1%). Most of the patients studied were covered by social insurance (36.3%). In this study, there was no relationship between frequent hospitalization and demographic factors (Table 1).
Distribution of Absolute and Relative Frequency of Patients According to Demographic Characteristics.

Findings of this study indicates that diabetes (56.6%) and heart problems (14.1%) were the most underlying diseases (Table 2).
Distribution of Absolute and Relative Frequency of Patients According to Underlying Disease.

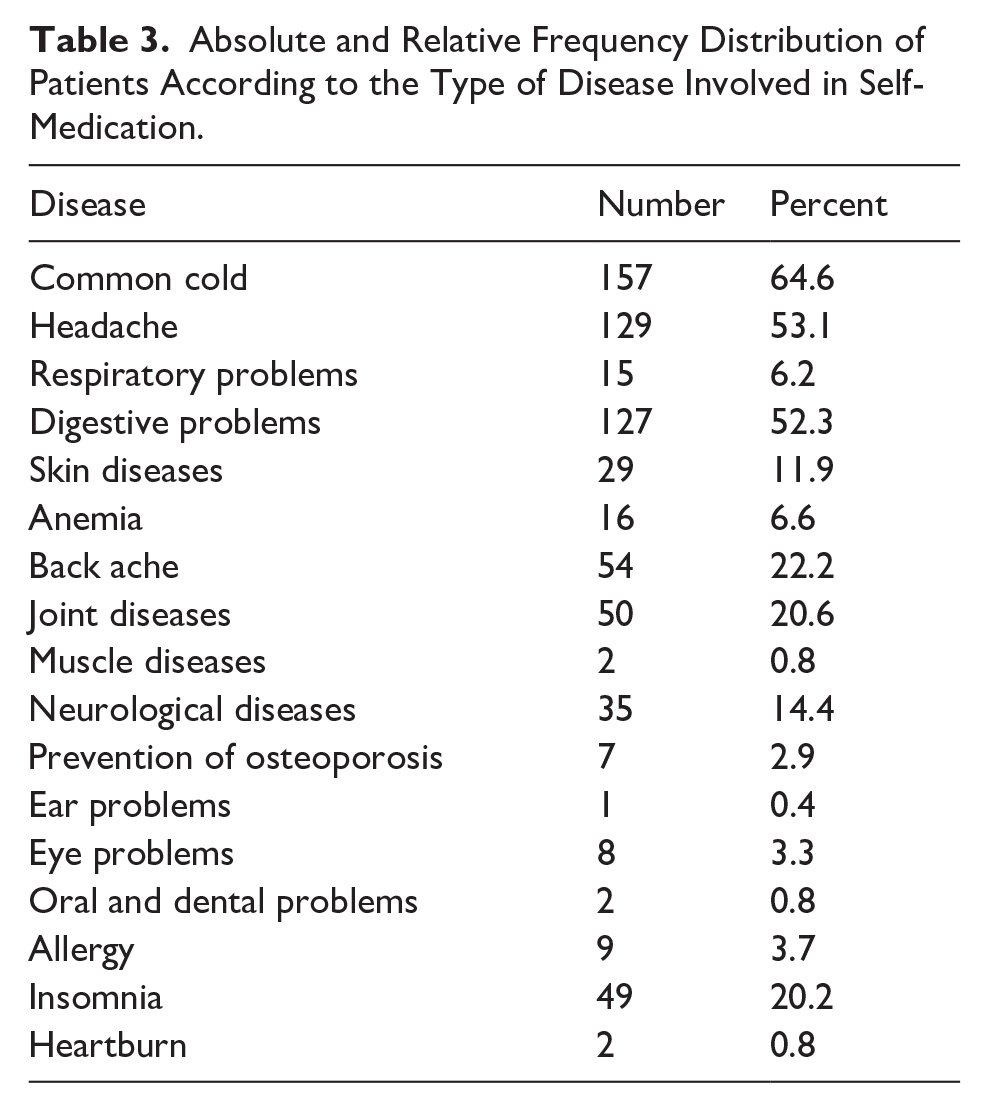
In this study Common colds (64.6%), headache (53.1%) and digestive problems (52.3%) were the most common diseases that were self-medicated and ear problems (0.4%), mouth and teeth problems (8.8%), heartburn and muscle diseases were less self-medicated than others. (Table 3) show distribution of this frequency.
Absolute and Relative Frequency Distribution of Patients According to the Type of Disease Involved in Self-Medication.
The most important sources of information for self-medication were friends and families (42%) and multimedia (22%). Through our study, we found that the most patients used self-medication because of their previous experience, recommendations of friends and disregarded to diseases. In this survey, 19 patients of 270 older people admitted patients to the hospital had a history of frequent hospitalization. This study indicated that painkillers (58.5%), cold tablets and syrups (48.8%) and herbal drinks (56.8%) are the most commonly drugs used in self-medication. Blood sugar control drugs (24%), anticonvulsants (0.8%) and eye drops (3.7%) were the least used drugs in self-medication (Table 4). This survey showed that the most frequent causes of hospitalization were cardiovascular diseases, glandular and respiratory diseases, respectively (Table 5).
Absolute and Relative Frequency Distribution of Patients According to the Type of Drug Used in Self-Medication.

The Rate of Frequent Hospitalization in the Hospitalized Older People With a History of Self-Medication.

Frequent hospitalization due to self-medication was showed only in one patient (7.6% of patients with frequent hospitalization) who hospitalized directly due to self-medication (herbal medicine). Oral medicines (99.6%) were the most used and the least used form of medicine in self-medication was suppository (0.4%).
Due to the non-normal distribution of demographic data, non-parametric Kruskal-Wallis and Chi-squared tests were used for the relationship between self-medication and demographic variables. This relationship is shown in (Table 6). This table shows that there was no significant relationship between any of the demographic factors (demographic factors) and self-medication.
Relationship Between Self-Medication and Demographic Variables.
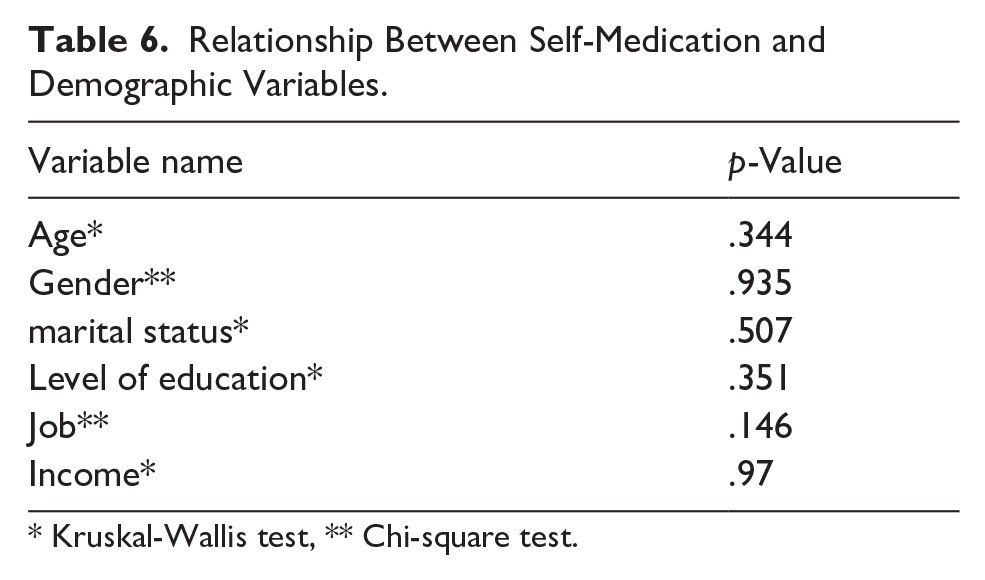
* Kruskal-Wallis test, ** Chi-square test.
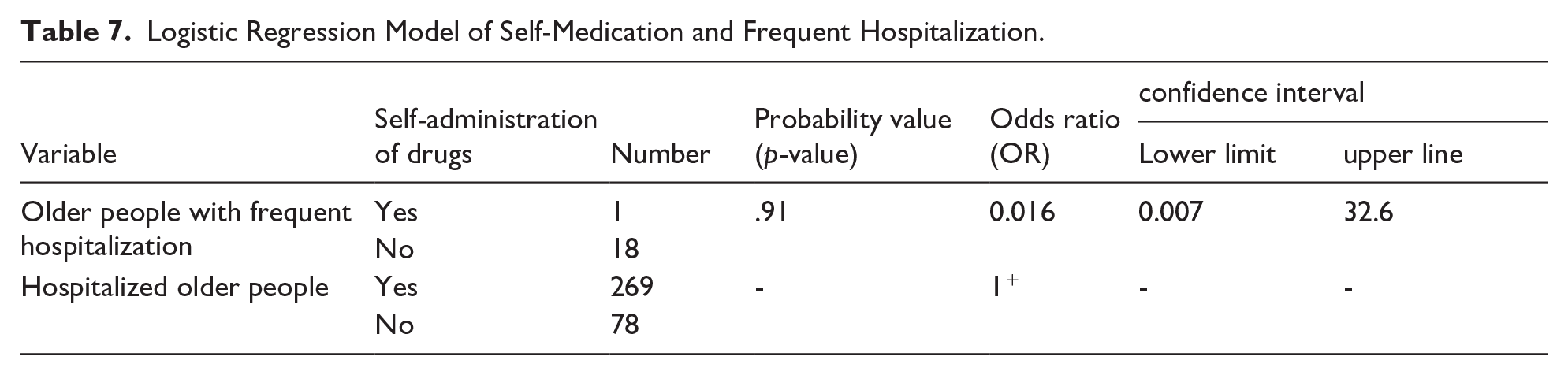
The results of logistic regression model processing showed self-medication and frequent hospitalization. The probability value is .91, which indicated that there was no significant relationship between frequent hospitalization and self-medication. The odds ratio, as shown, was 0.016, means that the probability of frequent hospitalization following self-medication was .016 in patients with frequent hospitalization, compared to hospitalized patients, and according to the upper and lower limits of the interval shown, it was confirmed that there was no significant relationship between frequent hospitalization and self-medication (Table 7).
Logistic Regression Model of Self-Medication and Frequent Hospitalization.
Discussion
The average age of the patients was 72.4 ± 4.6 years, and the majority of patients were women (51%). This shows that older people as well as women had more self-medication. Similar to this finding, in the most studies related to self-medication in the older people, the majority of subjects that had self-medication were women (Abdi et al., 2018; Dadashihaji et al., 2021; Farazmand & Toloei, 2002) 348 patients studied, 270 of them had self-medicated, which means that 77.44% of the older people hospitalized in Yazd hospital have self-medicated during the last year to treat their health problems. Comparing these findings of this study with other similar findings, the rate of self-medication in the older people in Brazil was more than 80.5% (Oliveira et al., 2018). Also, The mean self-medication prevalence was 26.3%, being the highest in Poland (49.4%) and the lowest in Spain (7.8%; Brandão et al., 2020). Also, all hospitalized patients with a history of self-medication, 19 patients were hospitalized more than twice a year (repeated hospitalization). In this study, the average hospitalization of self-medicated subjects was 1.09 ± 0.1. So far, no study similar to this study has been conducted on self-medication and frequent hospitalization of the older people, and for this reason, the author is not able to compare it with other similar studies. Of course, this comparison is one of the strengths of this study and it can open a new topic in the future research of older people health.
In the present study, the most drugs used in self-medication were painkillers, cold pills and syrup, herbal medicines and infusions, stomach syrup, and antibiotics.
In the study of Oliveira et al. most drugs used were non-steroidal anti-inflammatory central, acting muscle relaxants, analgesics and antipyretics and antirheumatic agents (Oliveira et al., 2018). In a study conducted in Syrian, as in the present study, the most commonly used drugs used in self-medication by the adults people were antipyretics, analgesics, and antibiotics (Abdelwahed et al., 2022). A common drug in self-medication is painkillers, which can be due to the desire for quick pain control. Also, the high prevalence of chronic pain in the older people can be the reason for self-medication use of painkillers. Although arbitrary use of painkillers in other communities was also reported high, so in the research of Shehnaz et al. (2013) . The results of another study also showed that self-medication is highly prevalent among the older adults, and the most commonly used medications were analgesics (Almadi et al., 2021).
In the present study, the highest rate of self-medication was due to cough and cold (64.6%), headaches (53.1%) and digestive problems (52.3%). In line with the present study, Shaiste et al. also stated in their research that the most common reasons for self-medication in the elderly are due to headache (38.9%) and cough and cold (48%; Shayeste et al., 2018). In a study conducted by Payvar et al. in Qochan, the most arbitrary use of medicine in the elderly was in cases of colds and headaches (Payvar et al., 2022). In George et al. research headache 54.68%, Fever 66.25%, cough and cold 38.43%, were the most common illness where self-medication being used (George et al., 2020). Also, the time of the study can have an effect on the type of diseases.
In the present study, the oral form (99.6%) of drugs was determined as the most used form of medicine in self-medication. In the study by Davati et al. (2007), the most commonly used medicinal forms included tablets and capsules, respectively, which can be attributed to the easier use of these medicinal forms (Davati et al., 2007). In other studies, the medicinal forms used in self-medication were not investigated (Almadi et al., 2021; Mortazavi et al., 2017).
In this research, the most important factors related to self-medication, the belief that diseases are not important, the belief that herbal medicines are safe, and the cost of visiting doctors were determined. In line with the present research, Ghorbani et al. also pointed out the economic and financial problems for self-medication in the elderly (Ghorbani et al., 2019). In the study of Ocan et al, having drug information, having previous experience, long waiting time, and distance to treatment centers were introduced as influencing factors on self-medication behavior (Ocan et al., 2014). In the research of Eslami et al, previous experience of illness (35.2%), easy obtaining of medicine from pharmacies (29.7%), lack of time to visit clinics and medical centers (27.2%) were the main causes of self-medication (Eslami et al., 2012). Drug therapy in the older people requires dose adjustment, which may only be within the ability of geriatrics specialists.
Other things such as the distance from medical centers, the time-consuming nature of visiting doctor can be related to the urban context, the concentration of doctors’ offices and medical centers in a certain part of the city, the number of doctors and medical centers in different cities under study. It seems that the high consumption of herbal medicines and the belief in the safety of herbal medicines in the present study can be related to the traditional way of thinking that governs the older people in Yazd and the popularity of herbal medicines among the older people.
Conclusion
In the current research, there was no significant relationship between self-medication and frequent hospitalization, because frequent hospitalization directly due to self-medication included only one patient. Among the most important factors of frequent hospitalization are heart diseases, glands diseases (such as diabetes) and respiratory diseases.
Considering the high cost of drug production and preparation as well as the unwanted side effects of self-medication, increasing awareness and knowledge, improving the attitude and performance of households, and monitoring the sale of drugs in pharmacies seems necessary. Self-medication alone is neither good nor bad. Policymakers at the lower level should make interventions to reduce the appropriate use of drugs and the consumption of harmful drugs. Studies on self-medication in the older people and its adverse health effects are clearly lacking. There is a need to perform prospective studies on this topic to gain a clear understanding of the extent of this problem and to enhance the awareness of health professionals to better inform seniors.
Footnotes
Acknowledgements
This study is part of the results of a MSc thesis on Aging and Health. We acknowledge all the officials of Kerman University of Medical Sciences, the hemodialysis centers and all the patients who participated in this study.
Ethical Considerations
Before starting the study, Ethics Committee of Faculty of Medical Sciences of Kerman provided the permission with ethics code of IR.KMU.REC.1402.390, related references were provided by Kerman University of Medical Sciences for dialysis centers in Kerman.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Kerman University of Medical Sciences. The funders of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.

