Abstract
Due to the rapidly aging population, hospitals are increasingly caring for more older patient. Implementing volunteer programs focused on providing care to hospitalized older adults is a way for hospitals to better support them. Despite the growing presence of volunteer programs in hospital settings, there remains a limited understanding of how these programs are structured, their impact on patient care, and their integration within healthcare teams. Addressing this gap is essential for optimizing volunteer engagement and improving hospital-based support for older adults. The purpose of this scoping review is to assess the existing literature surrounding volunteer programs designed to support hospitalized older adults and identify gaps that are present for future research and inquiry. Employing Arskey and O’Malley’s scoping review methodology, 27 publications met our study’s inclusion criteria. Thematically analyzing our data surfaced three overall themes: (1) the Influence of Volunteer Training on Roles and Functions, (2) Volunteer Perspectives on their Roles, and (3) the Impact of Volunteers in Hospital Settings. We noted that volunteers have different motivations for participating in volunteer programs. Healthcare professionals generally have positive views of hospital volunteer programs for older adults, but also express reservations and tend to have limited interactions with volunteers. Moreover, as volunteer roles were seen mainly to supplement family caregiver roles, future volunteer programs are encouraged to also consider the unique roles and needs of families and develop solutions to ensure that quality care can be delivered to both older patients and their family caregivers. Future research should explore how volunteer programs can be better integrated within interdisciplinary teams, assess their long-term impact on patient outcomes, and identify strategies to strengthen collaboration between volunteers, healthcare professionals, and family caregivers to optimize care for hospitalized older adults.
Introduction
Healthcare systems worldwide are under increasing pressure to manage the high costs associated with caring for aging populations (McMullin & Needham, 2018). Older adults (≥65 years) often require and experience both the increased and prolonged use of healthcare services due to a higher prevalence of chronic conditions, multimorbidity, functional decline, and age-related physiological changes that increase their susceptibility to acute illnesses and hospitalizations (Hajek et al., 2018; Morse et al., 2019; National Academies of Sciences, Engineering & Medicine, 2020; Wiener & Tilly, 2002). As a result, older adults disproportionately represent emergency department (ED) visits, hospitalizations, and account for the majority of hospital bed days, making them the primary demographic accessing hospital-based care and contributing significantly to healthcare costs (Biber et al., 2013; Latham & Ackroyd-Stolarz, 2014). For instance, in Canada, adults aged 65 and older account for nearly 60% of all hospital bed days and approximately 40% of emergency department visits, despite comprising only about 18% of the population (Canadian Institute for Health Information, 2021). Similar trends are observed globally, with older adults representing a substantial portion of inpatient care utilization and associated healthcare expenditures.
One of the ways healthcare systems are achieving greater cost-effectiveness in their delivery of care is through the use of volunteers (Hshieh et al., 2018). Volunteering, defined as any activity where time is freely given to benefit an organization, cause or individual (Wilson, 2000), has historically been integrated into the care and support hospitals provides (Badger et al., 2022; Gonella et al., 2019). The roles and functions of volunteers vary between hospital settings. For example, volunteers may be utilized to socialize with patients, transport patients, give directions to families and visitors, perform administrative work, or staff hospital gift shops (Hashash et al., 2016; Pickell et al., 2020; Pritchard et al., 2021). Personal motivations to volunteer in hospital settings also vary, though they typically include altruism and self-development, socialization, and an interest in pursuing a career in healthcare (Hurst et al., 2019).
Existing reviews around volunteering in hospital settings from North America have tended to focus on supporting specific conditions or functions, such as cancer (e.g., Macvean et al., 2008) dementia/delirium (Pritchard et al., 2021), meal-time care for adult populations (i.e., not just older adults; e.g., Green et al., 2011), or improving the mobility of older adults following an acute care admission (e.g., Baczynska et al., 2016). At the same time, the broader literature on volunteers in care transitions is limited to their support across health settings (e.g., hospital to community) and does not examine their specific roles and functions within hospital-based programs (Nelson et al., 2021). Reviews to date have not yet comprehensively explored the various factors (e.g., the volunteers, the setting (Macvean et al., 2008)) that influence the success of hospital volunteer programs specifically designed to support or older adults. This scoping review aimed to examine and synthesize the recent literature describing volunteer-based programs specifically supporting older adults in hospital settings, to help address existing knowledge gaps and better inform the future development of more volunteer programs serving older patients,. Our scoping review included recent literature examining volunteer programs across hospital-based acute, rehabilitation and emergency care settings. We define recent literature as research published in the past 12 years (2012–2024) to ensure relevance to the current health context (e.g., policies, services).
This study aligns with global policy initiatives, such as the World Health Organization’s Decade of Healthy Ageing (2021–2030) and the United Nations Madrid International Plan of Action on Ageing (MIPAA), both of which emphasize the need for age-friendly health systems that enhance the well-being of older adults. Additionally, volunteer programs in hospital settings align with national and regional aging policies aimed at addressing healthcare workforce shortages, promoting social participation, and improving patient-centered care. By identifying gaps and opportunities in hospital-based volunteer programs, our study provides insights that can help shape future policy efforts to integrate volunteers as a sustainable resource in the care of older adults.
Methods
Study Design
We undertook a scoping review methodology informed by Arksey and O’Malley (2005) and the PRISMA-SCr (Preferred Reporting Items for Systematic Reviews and Meta-Analysis Extension for Scoping Reviews) statement guidelines for scoping reviews (Tricco et al., 2018; see Supplemental File A) to assess the breadth of existing literature on the topic and identify gaps that may exist for future research and inquiry. A protocol has been registered elsewhere (https://buff.ly/3Bl9crX) and is described below.
Stage 1: Identifying the Research Question
The study addressed the following broad research question: What is the scope of recent existing empirical literature exploring the role and impact of volunteers in hospital-based interventions supporting older patients in the following jurisdictions: North America, Europe and Australia? We also asked three sub-questions: (1) what are the characteristics (i.e., role and functions) of volunteers included in hospital-based interventions serving older adults? (2) what key elements makeup existing volunteer programs serving hospitalized older adults? (3) what are the reported impacts of these volunteer programs on patient, staff and system outcomes?
As the nature of hospital practices (e.g., operation and design) differs across geographical locations and associated healthcare system needs, we limited our study to the continents of Australia, Europe, and North America, where hospital-based care is generally organized and provided in similar ways (Gauld et al., 2014; Mounier-Jack et al., 2017).
Stage 2: Identifying Relevant Published Reports
A literature search was performed across five databases: EMBASE, CINHL, MEDLINE, PsycInfo, and AgeLine. We included English peer-reviewed full text publications published from 2012 to June 31, 2024. 2012 start date was selected because of the increasing global emphasis on volunteer programs in hospital settings over the past decade, alongside significant policy developments in aging and health that have shaped hospital-based volunteer initiatives. Additionally, preliminary searches indicated that the majority of relevant studies emerged after 2012, making this a meaningful timeframe for capturing contemporary evidence. This review’s search strategy was deliberately broad to capture the breadth of literature on hospital volunteer programs focusing on older adults. The final search strategy was developed by the first author (KMK) in consultation with the senior author (SS) and formatted in consultation with a medical information specialist (CDC; See Supplemental File B).
To enhance the scope of our peer-reviewed literature, we scanned the reference lists of included articles and conducted forward searching. To search for gray literature (i.e., non-indexed literature of relevance), we searched Australian, European or North American government reports, clinical practice guidelines and hospital organization publications using the first 200 pages of Google Scholar as recommended for reviews (Gyenes et al., 2021).
Stage 3: Study Selection
Three researchers (KMK, LJ, CBS) screened titles and abstracts (level-1 screening). Next, the full text of potentially eligible studies was reviewed by two reviewers (KMK, LJ, and CBS; level-2 screening). Disagreements or uncertainties between reviewers during screening were resolved by discussion with the senior principal investigator (SS). To be included, articles had to be published in English between 2012 and June 31, 2024; include a description of the nature and scope of services provided by an implemented volunteer-based hospital program serving older adults in Australia, Europe or North America; include empirical qualitative, quantitative or mixed-method data (e.g., no commentaries, hypothetical programs). Articles that did not explicitly examine volunteerism with older adults (e.g., volunteer programs for children), volunteering conducted in settings other than a hospital (e.g., nursing homes, home visits) and hospital programs run only by paid staff were all excluded from this analysis. For this study, we define older adults as individuals aged 65 years and older, in alignment widely used classifications in gerontological and healthcare research (Donnellan, 2024). Articles published before 2012, literature reviews or those conducted in jurisdictions other than Australia, Europe and North America were also excluded. We limited this review to articles published in English due to resource constraints. Before screening titles and abstracts, the eligibility criteria were pilot-tested on the first 10 articles by two research team members (KMK and LJ) until an inter-rater reliability of κ ≥ 0.75 was achieved. Covidence software helped to facilitate the screening process (Babineau, 2014).
Step 4: Charting the Data
To promote consistent results, the abstraction form was pilot-tested on the first five articles among two reviewers (KMK and LJ). Once the abstraction form was finalized, information about the study characteristics (e.g., year of publication, country of study), purpose of the survey, methodologies/methods, details on the participants (e.g., age, sex, medical-related inclusion/exclusion criteria) findings and limitations were extracted by three authors (KMK, LJ, CBS) using Excel from the included articles. Abstracted data also included outcome measures and indicator definitions (e.g., length of stay defined as the number of total days at a hospital without interruption). The study setting was categorized as follows: acute care (any acute care institution or department within an acute care hospital other than rehabilitation and palliative care), specialized outpatient services other than rehabilitation (e.g., hemodialysis, dentistry, podiatry, chemotherapy, endoscopy, and pain management clinics), ED, palliative care, and rehabilitation. The quality of the included studies was not assessed as the objective of a scoping review is to identify the current state of knowledge and gaps in the literature (Arksey & O’Malley, 2005).
Step 5: Collating, Summarizing, and Reporting the Results
All included studies were synthesized. Studies were first summarized through numerical counts that included their place of origin, characteristics of older adults included and characteristics of the interventions. The research team created a table of included studies, listing (when appropriate and available) the study type, aims, care settings, study outcomes (quantitative and qualitative), participants and details of the interventions. Next, a narrative synthesis of the included studies was conducted through discussions with the research team. Two reviewers (KMK and LJ) reviewed each article, and the coded data and a coding scheme were developed. One author (KMK) then applied this coding scheme to each paper using NVivo (Beekhuyzen, 2007). Through weekly team meetings, codes were then aggregated by key ideas centered on each research question. The entire research team discussed discrepancies in understanding the coded data to achieve consensus.
Step 6: Consultation
Consultation with knowledge users informed the study design and validated the results of preliminary findings. We consulted with two nurses who frequently work with volunteers and one volunteer coordinator of a hospital program about our initial results twice throughout the writing of this manuscript. Furthermore, we shared preliminary findings with health service providers within a geriatric medicine acute care unit outside the study team throughout the development of this manuscript to further validate results and support knowledge translation efforts. The consultative discussions identified gaps in the literature and areas for future systematic reviews.
Results
About 8,322 peer-reviewed titles and abstracts and 62 full-text studies were assessed for their eligibility. Subsequently, 32 studies fulfilled this study’s eligibility criteria and were included. In addition, two articles were added through a hand search for a total of 34 articles included in our analysis (see Figure 1). The gray literature search yielded no additional articles that met the inclusion criteria.

Volunteer-PRISMA numbers for today’s run.
Overview of Studies
An overview of the included articles can be found in Table 1. Most studies occurred in the United Kingdom (n = 12/34, 35%). Studies most often utilized a mixed-method (n = 13/34, 38%) (Ayton et al., 2020; Bird et al., 2016; Blair et al., 2019; Buys et al., 2013; Charalambous, 2024a; Huang et al., 2015; Howson et al., 2018; Huson et al., 2016; Lim et al., 2020; Louch et al., 2017; Roberts et al., 2014; Robison et al., 2015; Schulman-Green et al., 2023) or quantitative study design (n = 11/34, 32%) (Blair et al., 2018; Chabot et al., 2019; Gisch et al., 2022; Helfand et al., 2020; Piotrowicz et al., 2018; Roberts et al., 2017; Rubin et al., 2011; Sales et al., 2013; Sanon et al., 2014; Strijbos et al., 2013; Zaubler et al., 2013). Most studies occurred in acute inpatient wards (n = 27/34, 79%) (Ayton et al., 2020; Bird et al., 2016; Blair et al., 2018, 2019; Brighton et al., 2017; Buys et al., 2013; Chabot et al., 2019; Charalambous, 2024a, 2024b; Godfrey et al., 2013; Helfand et al., 2020; Howson et al., 2018; Huang et al., 2015; Hurst et al., 2020; Lim et al., 2020; Louch et al., 2017; Nelson & Yi, 2018; Piotrowicz et al., 2018; Roberts et al., 2014, 2017; Robison et al., 2015; Rubin et al., 2011; Sales et al., 2013; Schulman-Green et al., 2023; Strijbos et al., 2013; Zaubler et al., 2013).
Characteristics of Included Peer-Reviewed Studies.

Characteristics of the Older Adult Patients
Volunteers were often introduced to help older adults with dementia and/or delirium or those at risk of developing delirium (Ayton et al., 2020; Blair et al., 2018, 2019; Hurst et al., 2020; Piotrowicz et al., 2018; Rubin et al., 2011; Sanders et al., 2018; Strijbos et al., 2013; Zaubler et al., 2013). Several publications included studies specifically focused on supporting older adults aged ≥65 years (n = 7/34, 21%) (Ayton et al., 2020; Blair et al., 2018; Buys et al., 2013; Godfrey et al., 2013; Sanon et al., 2014) or ≥70 years (n = 10/34, 29%) (Ellis et al., 2020; Howson et al., 2017, 2018; Huson et al., 2016; Piotrowicz et al., 2018; Roberts et al., 2014, 2017; Robison et al., 2015; Rubin et al., 2011; Strijbos et al., 2013; Zaubler et al., 2013). One program (n = 1/34, 0.03%) lowered the age of inclusion to ≥45 years if patients were of Aboriginal or Torres Strait Islander backgrounds (Blair et al., 2018). The ethnicity of the older adults was seldom mentioned, although some programs described themselves as caring for ethically diverse older adults (Sanon et al., 2014). One study (n = 1/34, 0.03%) included almost exclusively white older adults (Zaubler et al., 2013). Nearly all studies that reported on sex included predominantly female older adults, with three studies having exclusively female samples (Roberts et al., 2014, 2017; Robison et al., 2015; Table 2).
Included Sample of Older Adults.

Characteristics of Volunteer Interventions
All programs described were offered in person and in a hospital. The goal of embedding volunteers in hospitals was often to supplement the care being provided by existing care providers and families (Blair et al., 2018, 2019; Ellis et al., 2020; Nelson & Yi, 2018). Thus, Blair et al. (2019) described the role of volunteers as being “similar to that of a family carer” (p. 1709). Volunteers delivering described interventions were often female (Brighton et al., 2017; Hurst et al., 2020; Robison et al., 2015) and ranged in age from 16 to 82 (Brighton et al., 2017; Chabot et al., 2019; Howson et al., 2018; Hurst et al., 2019, 2020; Huson et al., 2016; Lim et al., 2020; Roberts et al., 2014, 2017; Robison et al., 2015).
A thematic analysis further revealed three distinct themes: the influence of volunteer training, volunteer perspectives on their roles, and the impact of volunteers. Volunteer training is crucial in shaping their roles, with most programs focusing on person-centered support, enhancing retention and effectiveness in tasks such as mealtime assistance, supporting mobility, and reducing loneliness. Volunteers value interactive training and learning from their peers and experts, which further strengthens their level of commitment as a volunteer. However, some volunteers described facing challenges, including experiencing feelings of invisibility, unclear roles, and a lack of integration with staff, leading to high turnover in certain cases. Despite these challenges, volunteers generally report having positive experiences, driven by altruism and personal satisfaction. Their reported impact is also significant, with studies highlighting benefits such as achieving increased patient safety, reduced workloads for staff, and a positive effect on hospital outcomes like shortened stays, reduced readmissions, and delirium prevention. Volunteers were also found to aid in the physical and emotional well-being of older adults, improving mobility, preventing falls, and promoting post-discharge reintegration into the community, ultimately enhancing quality of life and reducing social isolation.
Theme 1: Influence of Volunteer Training on Role and Functions
Most of the described interventions involved 9 to 50 volunteers, although one trained 100 (Rubin et al., 2011). Volunteers were often trained to provide person-centered, one-to-one emotional and practical support (Ayton et al., 2020; Blair et al., 2018, 2019; Charalambous, 2024a). Thirty studies reportedly trained volunteers (n = 30/34, 88%) (Chabot et al., 2019; Godfrey et al., 2013; Roberts et al., 2014). When training was provided, the volunteers highly regarded it (Hurst et al., 2019; McDonnell et al., 2014). Brighton et al. (2017) noted that volunteers valued opportunities to learn from their peers and subject-matter experts, like end-of-life specialists, using real-case examples, and interactive teaching methods. Training volunteers was believed to retain volunteers in the long-term as well (Ayton et al., 2020; Brighton et al., 2017; Howson et al., 2018; McDonnell et al., 2014; Roberts et al., 2014; Robison et al., 2015). Some programs developed their own training curriculum, such as MyCare Ageing (Ayton et al., 2020), Boredom Busters and Fitness Friends (Charalambous, 2024a), and the Volunteer Dementia and Delirium Care Implementation and Training resource (Blair et al., 2019). However, even training for established volunteer programs such as the Hospital Elder Life Program (HELP; an intervention to lower delirium-related cognitive and functional decline among hospitalized older adults) varied across hospital settings where the program was implemented because modifications were required to meet the specific needs of each hospital (Rubin et al., 2011; Strijbos et al., 2013). For instance, HELP volunteers at the University of Pittsburgh Medical Center (UPMC) Presbyterian Shadyside were given enhanced training in feeding and mobilization protocols by speech and physical therapists (Rubin et al., 2011). The characteristics of volunteer training are reported in Table 3.
Intervention Delivery Characteristics.
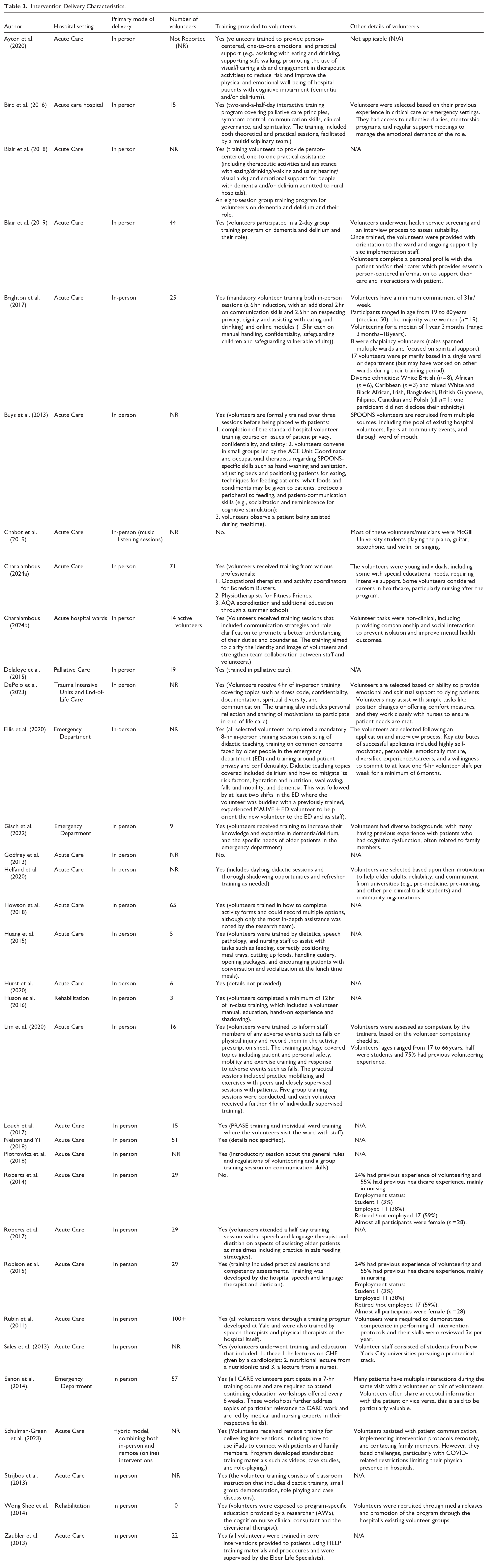
Roles of Volunteers
The described roles of volunteers often included providing mealtime assistance (e.g., providing verbal prompts to encourage eating; Blair et al., 2018; Brighton et al., 2017; Howson et al., 2017; Hurst et al., 2020; McHugh et al., 2016; Roberts et al., 2017; Robison et al., 2015); supporting mobility exercises (Helfand et al., 2020; Lim et al., 2020); supporting post-discharge transitional care (e.g., discharges from hospital to home) and community reintegration (Brighton et al., 2017; Nelson & Yi, 2018; Sales et al., 2013); obtaining patient feedback (i.e., through the Patient Measure of Safety [PMOS] and Patient Incident Reporting Tool [PIRT]; Louch et al., 2017); monitoring sleep, hydration and pain levels (Piotrowicz et al., 2018; Sanders et al., 2018); and, helping older patients to overcome loneliness, such as through acting as visitors and providing socialization (e.g., fostering interaction between hospitalized patients; Ayton et al., 2020; Brighton et al., 2017; Delaloye et al., 2015; Ellis et al., 2020; Helfand et al., 2020; Hurst et al., 2019, 2020; Nelson & Yi, 2018; Piotrowicz et al., 2018). Volunteers also served as hospital guides (e.g., signposting services) and chaplaincy volunteers (Brighton et al., 2017). Some volunteers provided patients with manicures and foot massages (Hurst et al., 2020). The roles and functions of volunteers sometimes depended on the specific older patient population being served and the type of hospital care setting (e.g., palliative care, surgical unit; Delaloye et al., 2015; Sanon et al., 2014).
Theme 2: Volunteer Perspectives on Their Roles
11 (n = 11/34, 32%) of the included studies investigated the perspectives of hospital volunteers in greater depth using qualitative methods such as focus groups, interviews, and participant observations (Delaloye et al., 2015; Hurst et al., 2019; Huson et al., 2016; McDonnell et al., 2014; Nelson & Yi, 2018; Shee et al., 2014). Volunteers described volunteering within hospital programs for older adults due to altruistic beliefs, self-interest (e.g., interest in pursuing a career in healthcare or learning new things) (Howson et al., 2018) and sharing their own hospital experiences with others (Hurst et al., 2019). Volunteers described personal satisfaction in their ability to help others through volunteering (Shee et al., 2014). Volunteers mentioned wanting to feel appreciated by patients and health care providers (Shee et al., 2014). Many studies included volunteer-described negative perceptions and experiences, including not feeling useful, which may be one key reason why volunteers quit participating in hospital volunteer programs (Shee et al., 2014). One study found that volunteers felt invisible to hospital staff due to the frequent staffing changes occurring in the units (Delaloye et al., 2015). Another study noted that volunteers felt that staff chose not to communicate with them due to their clinical care priorities and the limited scope of the volunteer roles that existed (Huson et al., 2016). Another study noted challenges managing young volunteers due to their lack of confidence and skills to work in complex hospital settings. These issues required extra preparation and ongoing support and reportedly contributed to a high turnover rate, leading to increased administrative work for staff (Charalambous, 2024a). One study also noted challenges with delivering remote volunteer interventions, highlighting the importance of in-person interactions especially for engaging cognitively impaired patients and ensuring clear communication (Schulman-Green et al., 2023). Healthcare providers may also lack clarity about the role of volunteers. For instance, one study reported that staff asked if volunteers could wash clothes and change the water in flower vases rather than perform some of their trained care duties (Shee et al., 2014).
Theme 3: Impact of Volunteers in Hospital Settings
Studies found that staff opinions about volunteers were overtly positive, as staff reported ample integration into the care team, and achieving increased patient safety and quality of care, and a reduced workload burden for staff (Blair et al., 2019; Robison et al., 2015). Studies also described the importance of volunteers in filling support gaps when family and care providers are unavailable (Huson et al., 2016) and reducing the burden on families and staff (Blair et al., 2019). For example, in an ED, a volunteer intervention was shown to reduce discomfort and prevent delirium by “training skilled volunteers to provide additional care to older adults and their families/carers in the ED” (Ellis et al., 2020, p. 518).
In some studies, hospital staff were found to be initially skeptical around the involvement of volunteers because they feared potential overcrowding in their care settings (Bird et al., 2016; Gisch et al., 2022; Robison et al., 2015), the inability to differentiate staff from volunteers easily, and the privacy logistics of volunteers accessing patient information (Shee et al., 2014). In most instances, these initial reservations were resolved. For example, in one study, the volunteer program implemented a rule against volunteers wearing the same-colored shirts as nurses so that they could be easily differentiated (Shee et al., 2014).
Staff in many studies reported that volunteers freed up their time (e.g., Bird et al., 2016; Blair et al., 2019; Charalambous, 2024a; DePolo et al., 2023; Huang, et al., 2015; Roberts et al., 2014, 2017; Robison et al., 2015). In a study by Robison et al. (2015) regarding implementing a mealtime assistance program in a hospital, staff said volunteers could assist many patients requiring straightforward support at mealtime, which allowed them to focus their attention on patients with severe swallowing issues. Howson et al. (2018) noted that reluctance to eat increases with age, so older adults and staff appreciate volunteers encouraging reluctant eaters. Interestingly, however, volunteer interventions during mealtimes were not found to significantly increase the total dietary intake of patients in the studies where this was analyzed (Huang et al., 2015; Roberts et al., 2017). Instead, mealtime volunteer assistance was found to release nursing staff to fulfill other care duties or tend to more complex patients (Huang et al., 2015; Roberts et al., 2014, 2017; Robison et al., 2015). Mealtime assistance by volunteers also reduced older adults’ confusion (Roberts et al., 2017), offered cost-saving benefits (Buys et al., 2013; Howson et al., 2018), and informed care decisions and referrals through a relay of person-centered information about patients to staff by volunteers (Blair et al., 2019; Roberts et al., 2014; Robison et al., 2015).
Addressing and mitigating the risks associated with delirium, such as prolonged hospital stays and readmission, were among the most commonly cited benefits of volunteer interventions targeting older patients. For example, the HELP initiative (Helfand et al., 2020; Huson et al., 2016; Rubin et al., 2011; Zaubler et al., 2013) successfully reduced 30-day readmissions (Rubin et al., 2011) and length of hospital stays (Zaubler et al., 2013). These findings are consistent with those of Blair et al. (2018), who reported that volunteer intervention in the hospital was linked to reductions in 28-day readmission rates for patients with delirium. Piotrowicz et al. (2018) explored similar volunteer-led non-pharmacological strategies and concluded that these interventions decreased the hospital lengths of stay and the need for antipsychotic medications.
Volunteers were also found to play a valuable role in promoting community reintegration. Sales et al. (2013) found that congestive heart failure patients (mean age = 73 years) who received dietary and pharmacological education from a trained volunteer before discharge experienced decreased 30-day readmissions and a 12% absolute risk reduction of readmission as a result. Nelson and Yi (2018) also advocate for the role of volunteers in bridging the transition between hospital and home/community, reporting that the provision of social and emotional support by volunteers to older adults in hospital predicts decreased ED admissions post-discharge, increased quality of life, and reduced social isolation.
Relating to impacting the mobility of older adults, volunteers were found to improve the physical mobility of older adults by providing mental stimulation and a new face to walk around with (Helfand et al., 2020). In addition, volunteer-led exercises have been shown to increase trends in daily step count (Lim et al., 2020) and prevent falls (Helfand et al., 2020). Finally, Chabot et al. (2019) concluded that exposure to musical performances by volunteer musicians was significantly correlated with a lower risk of falls among hospitalized older adults.
Discussion
This study aimed to synthesize the literature on volunteer programs specifically supporting hospitalized older adults in high-income countries. While numerous studies on hospital-based volunteerism exist, we intended to examine the specific roles and functions and consequent outcomes of engaging volunteers in the care for older hospitalized patients. Most of the studies we analyzed were from the United Kingdom and reported on volunteer programs within acute care and most specifically specialized inpatient geriatric care settings. The roles of volunteers working with older patients typically revolved around delirium prevention and management through socialization, mobility assistance, and mealtime assistance.
Overall, the studies included in this review suggest that one of the most significant impacts of volunteer-led interventions targeting older hospitalized adults, is the time it saves hospital staff. In particular, hospital volunteers were able to supplement the support provided by both hospital staff and family caregivers. However, most of the supporting data related to these findings were derived from staff perceptions; thus, assessing these interventions via rigorous randomized control trials or systematic reviews exploring clinical and resource outcomes would bolster this claim. Also, while staff and volunteer perceptions are valuable, an exploration of validated instruments to assess the effectiveness of volunteers may be warranted. Studies exploring the perspectives of patients as care recipients are also justified. For example, even though socialization was mentioned as being frequently performed by hospital volunteers, its effectiveness as an intervention has not been explored in detail. In future studies, using validated instruments to examine the effect of socialization on mood (e.g., depression, anxiety) among individuals hospitalized older patients may be worthwhile.
Moreover, the time-saving function of volunteers is juxtaposed and potentially in conflict with resource-intensive volunteer onboarding and training, which several studies described (Ayton et al., 2020; Brighton et al., 2017; Howson et al., 2018; McDonnell et al., 2014; Roberts et al., 2014; Robison et al., 2015). Combined, these two findings may speak to broader issues across the healthcare system related to both inadequate staffing and underfunding for volunteer programs (Bradley et al., 2005; Handy & Srinivasan, 2004; McKenzie et al., 2011; Rosenthal et al., 2021). As Brighton et al. (2017) tells us that in order to fully harness the commitment and benefits of hospital volunteers, the necessary resources and support for them require investment.
Volunteers play an integral role in supporting older adults in hospital settings. However, having volunteers to supplement the provision of family support may also impact the unique role of family caregivers. For example, older adults frequently depend on their families to help negotiate their care with health and social care providers, and as such, family-centered care has been identified as a critical element of quality hospital care delivery (Feinberg, 2014). Hospitals committed to a family-centered philosophy of care should continue to develop approaches for supporting families through the use of volunteers and work with both volunteers and families to facilitate the advancement of family-centered care. The volunteers delivering programs should be seen as an integral part of supporting family-centered care for older patients, such that volunteers are better able to also provide family caregiver support rather than solely focusing on directly supporting an older adult patient. Allowing opportunities for family-volunteer interactions may also improve patient and family caregiver outcomes. Finally, future studies could examine how volunteer training and policies have been implemented across various regions to determine opportunities to support family caregivers better. This research might serve as a mechanism for enhancing family-centered care through hospital volunteer programs.
It is important to note that variations in hospital organization and payment mechanisms (e.g., fee-for-service, third-party, or governmental support) across different regions may influence the implementation and utilization of volunteer programs. These factors can shape the roles volunteers play, the resources allocated to volunteer initiatives, and the overall effectiveness of these programs in supporting patient care. Future research could further explore how these organizational differences impact the integration and sustainability of volunteer programs in diverse healthcare systems.
We identified that individuals volunteer in hospital-based programs with older adults to both learn and contribute, among other reasons which vary from person to person. This study adds further dimensions to the literature on hospital volunteers by exploring their roles and functions, which may provoke further examination into who volunteers for specific roles and why in supporting older adults. While our study noted no conclusive findings related to gender-based differences around motivations for volunteering, we did note that most volunteers in the included studies were female. Future studies may wish to assess differences in preferred roles or functions amongst male, female and gender-diverse volunteers. Such information could help inform a better understanding of what volunteers interested in supporting the care of older patients are looking to do in a volunteer position and could be helpful for volunteer recruitment. Existing literature suggests that varied communication strategies impact male and female volunteers differently (Waters & Bortree, 2012). Volunteer managers should also be conscious of these preferences to help provide opportunities that align with them. Of equal significance is that the adult volunteer population noted across the studies and the older adults included in those studies are not necessarily representative of the population in the countries these programs operate in or the patient population the programs serve. Given the cost associated with a higher turnover rate of short-term volunteers, better retention strategies are required (Handy & Srinivasan, 2004). Studies included in this review note that training may retain volunteers (Ayton et al., 2020; Brighton et al., 2017; Howson et al., 2018; McDonnell et al., 2014; Roberts et al., 2014; Robison et al., 2015). Finally, as the interventions reported in this review occurred in acute hospital care settings only, it may be worthwhile to explore any inherent differences in volunteer characteristics (e.g., demographics, the types of interventions being performed, perceptions of role) across hospital settings as this can potentially inform the implementation and sustainability of volunteer programs.
At the global level, our findings have important implications for the achievement of health-related United Nations Sustainable Development Goals (SDGs), particularly SDG 3: Good Health and Well-being (Das et al., 2021) and SDG 10: Reduced Inequalities (Oestreich, 2018). Our study highlights the potential of volunteer programs to enhance hospital care for older adults, contributing to the goal of improving access to quality healthcare services for vulnerable populations. By addressing gaps in healthcare service delivery through the inclusion of volunteers, hospital programs can help reduce the disparities faced by older adults in accessing timely, patient-centered care. Additionally, these programs align with SDG 11: Sustainable Cities and Communities, by fostering social inclusion and community engagement, essential components of age-friendly environments (Küfeoğlu, 2022).
Strengths and Limitations
We acknowledge some limitations of this scoping review. This review was limited to only English language studies and specific jurisdictions; thus, we likely have a bias toward studies from English-speaking countries. Thirdly, we only included published research literature; as a result, we have likely missed reports on other available, relevant programs (e.g., volunteer programs without evaluation). Despite these limitations, this review highlights the breadth of existing data exploring the roles and functions of volunteers within hospital programs designed for older adults. An experienced information specialist performed the literature search, which was peer-reviewed. Our review is also strengthened by its rigorous methodology, which included completing screening by two reviewers independently and in duplicate and consultation with key knowledge users and stakeholders.
Conclusion
Many hospitals are increasingly relying on volunteers to enhance care quality and cost-effectiveness for growing numbers of older patients. Volunteer programs have positively impacted key outcomes such as nutrition, socialization, delirium management, mobility, length of stay, and readmissions. Volunteers are motivated by a sense of “usefulness” and “purpose,” while hospital staff generally view these programs favorably, though with some initial reservations and limited interactions. Future research should focus on overcoming hesitations to expand volunteer use, assessing their impact on patient, staff, and system outcomes (e.g., reduced staff workloads), evaluating specific interventions (e.g., hydration), and exploring differences across hospital settings. Such research could improve the accountability and effectiveness of volunteer programs in supporting family-centered care and ensuring quality care for older adults and their caregivers.
Supplemental Material
sj-docx-1-ggm-10.1177_30495334251337259 – Supplemental material for Volunteer Programs for Hospitalized Older Adults in North America, Europe, and Australia: A Scoping Review
Supplemental material, sj-docx-1-ggm-10.1177_30495334251337259 for Volunteer Programs for Hospitalized Older Adults in North America, Europe, and Australia: A Scoping Review by Kristina M. Kokorelias, Laura M. Jamieson, Marianne Saragosa, Hardeep Singh, Charles Brian Serapio, Salsabeel Jasiem and Samir Sinha in Sage Open Aging
Footnotes
Acknowledgements
We would like to thank and acknowledge the contributions of Charmaine De Castro, Information Specialist at the Mount Sinai Hospital – Sinai Health System, for providing guidance on the search strategy development, and conducting the literature searches.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Mount Sinai Hospital Healthy Ageing and Geriatrics Program Research Fund. HS holds the March of Dimes Paul J.J. Martin Early Career Professorship.
Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
