Abstract
Background:
Outpatient substance use disorder (SUD) treatment is commonly delivered through integrated, colocated, or coordinated models. In integrated care, the primary care provider (PCP) manages both general health and SUD, while colocated and coordinated models involve a separate addiction specialist—either within the same clinic or at an external location, respectively. While coordinated care has historically been the norm, integrated models may reduce treatment barriers. However, little is known about patient preferences across these models. Understanding such preferences is essential to improving engagement and care delivery. This qualitative study explores patient preferences and the factors influencing their choices among the 3 models.
Methods:
Fifteen adults with diagnosed SUD were recruited from an integrated, primary care–based addiction medicine clinic in an urban, academic medical center in California. Participants completed 45 to 60 minute interviews in-person or by phone. Data were analyzed using the socioecological model of health as a conceptual framework.
Results:
At the time of the interview, 3 participants were receiving integrated care, 7 colocated, and 5 coordinated. Most (n = 10) preferred integrated care when given the option. Among those favoring the colocated and coordinated models, over half were willing to consider integrated care if their PCP had addiction training. Factors shaping preferences included SUD severity, quality of the patient-provider relationship, clinic convenience, and clinician competency. Across all models, participants preferred nonjudgmental, affirming providers knowledgeable in addiction.
Conclusions:
Most participants favored integrated care, highlighting its convenience and continuity with a trusted provider. However, concerns about PCP training in addiction care were common, suggesting the need for enhanced clinician preparation starting in medical school and residency. Regardless of model, participants emphasized the importance of wrap-around services, including peer recovery specialists, counseling, and care navigation, to support recovery and promote treatment engagement.
Keywords
Highlights
Patients value substance use care within primary care.
Integrated care supports convenience and continuity.
Clinician training shapes care preferences.
Introduction
Trends in Substance Use Disorder Treatment
Outpatient substance use disorder (SUD) treatment, defined as engagement with a provider for medication prescriptions or counseling without an overnight stay at a hospital, is designed to help individuals address substance use–related challenges. 1 However, SUD care remains significantly underutilized in the United States, with over 90% of adults with SUD not receiving treatment across all levels of care.2,3
Primary care serves as the initial touchpoint for many people with SUD, yet specialty addiction treatment and general medical care are commonly siloed. Integration of SUD treatment into primary care settings may bridge the gap between SUD prevalence, treatment access, and engagement in care.4-6 Notably, 82% of Americans with SUD expressed comfort seeking SUD treatment from their primary care provider (PCP), yet 61% of Americans remain unaware that primary care physicians can prescribe medications for opioid use disorder (OUD) treatment. 7
SUD Treatment Models
Currently, there are 3 dominant models of SUD treatment delivery: integrated, colocated, and coordinated ( Figure 1 ).8-10
Integrated model (primary care model): Patients receive primary care and SUD treatment at the same location with the same clinician.
Colocated model (partially integrated): Patients receive primary care and SUD treatment at the same location but from different clinicians.
Coordinated model (specialty care): Patients receive primary care and SUD treatment at separate locations from different clinicians.
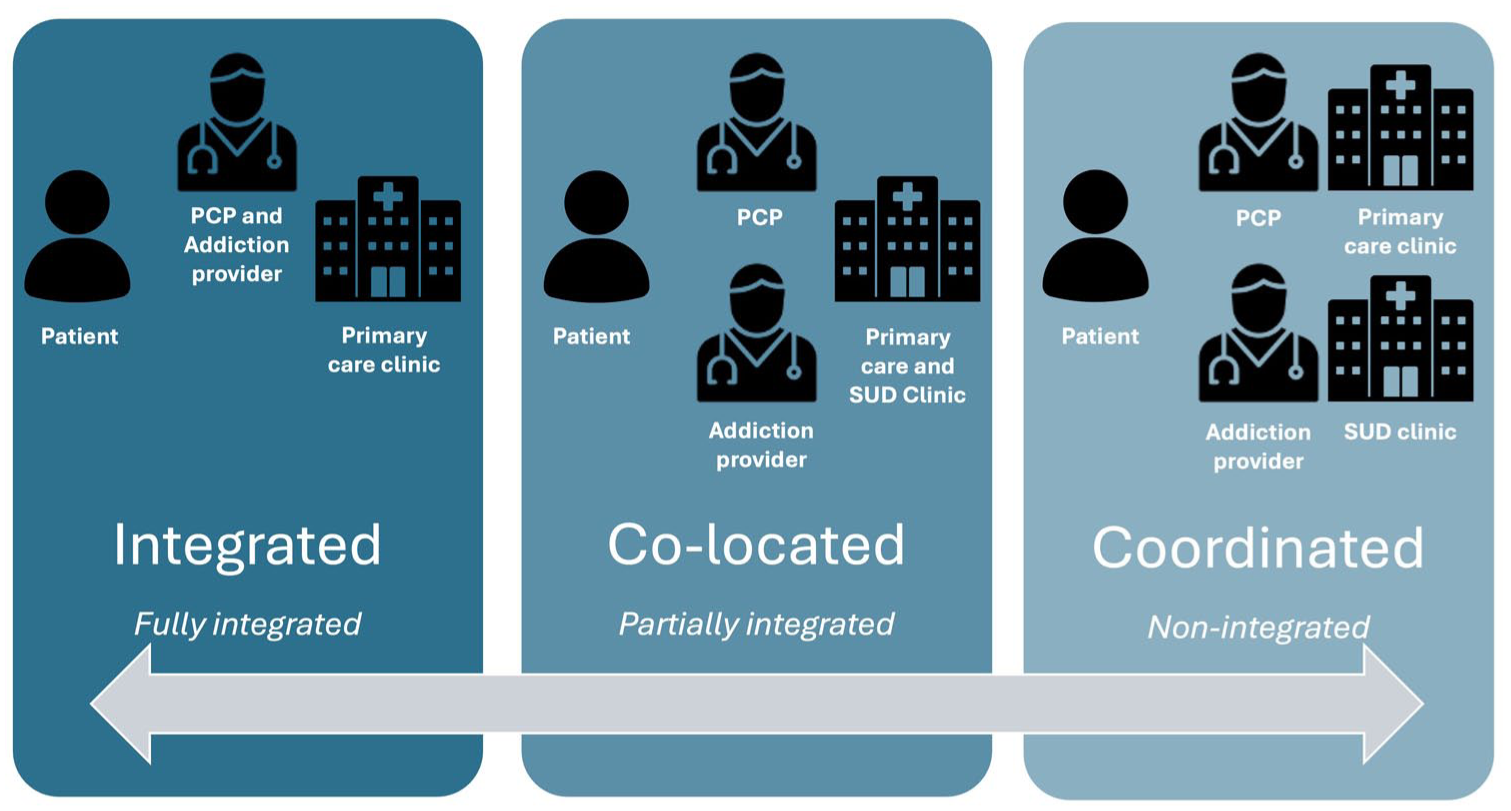
Models of SUD treatment: Integrated, colocated, and coordinated care. SUD, Substance use disorder.
Historically, SUD treatment was primarily delivered via the coordinated model in specialized treatment centers, such as hospitals, rehabilitation facilities, and mental health centers.11,12 However, new evidence-based integrated care models are being adopted in primary care settings to improve accessibility and outcomes.5,13,14 Integrating SUD treatment into primary care has demonstrated cost-effectiveness, increased treatment retention, and reduced utilization of inpatient and emergency services.15-19 Research also indicates that these models lead to reduced substance use and improved overall physical and behavioral health outcomes. 5
Patient Preferences for SUD Treatment Models
Research on individuals without SUD suggests that receiving mental health treatment in primary care settings can be more convenient and less stigmatizing than seeking care in specialized behavioral health centers. 20 One study on SUD treatment projected that individuals would be more willing to enter treatment within a primary care setting rather than a specialized drug treatment center. 21 Research on patient preferences for SUD treatment models, however, remains limited.
A qualitative study of individuals with OUD receiving treatment primarily from nonintegrated programs across diverse US regions found that most participants favored nonintegrated models. Key concerns included privacy and confidentiality, clinician competency, and stigma within the integrated model. 8 These differences may reflect variations in participants’ prior treatment experiences, regional availability of integrated care, and the study’s restriction to patients with OUD. Gaining deeper insight into patient perceptions of integrated care, particularly in settings where integrated care is offered and among individuals with broader SUD, may inform strategies to enhance care delivery and engagement.22-24
Aims and Objectives
This study aimed to assess patient preferences for 3 SUD treatment models: integrated, colocated, and coordinated. Through qualitative interviews, we seek to gain an in-depth understanding of the factors that shape preferences for models of care. By incorporating the perspectives of individuals living with SUD, this study identifies key barriers and facilitators to integration and can inform the future implementation and provision of SUD treatment on a national scale.
Methods
Study Design
A descriptive phenomenological qualitative design was selected to elucidate the lived experiences of individuals undergoing SUD treatment.25,26 We defined 3 treatment models: integrated, colocated, and coordinated ( Figure 1 ). These definitions were utilized in a previous study and purposefully adapted to meet the needs of this research. 8 Our study was approved by the appropriate institutional review board and adhered to the Consolidated Criteria for Reporting Qualitative Research guidelines to enhance credibility and reliability. 27
Setting and Study Population
Purposive sampling was used to recruit participants from a primary care–based addiction medicine clinic located in an urban, academic medical center in San Francisco, California. 28 The clinic is staffed by providers dual-boarded in internal medicine and addiction medicine. Not all patients at this clinic receive SUD treatment. Among those with SUD, some patients receive both primary care and addiction care at the clinic, following an integrated care model. Other patients are referred by their PCPs solely for SUD consultation, reflecting a colocated or coordinated model, depending on the PCP’s location relative to the addiction clinic. The coordinated model was specified as differences in location, not differences in health systems. All patients are covered by either commercial or public insurance. The clinic provides pharmacologic therapy, patient navigation, and referrals to counseling and social work. The patient population spans individuals new to treatment and those in long-term recovery.
Participants diagnosed with SUD were recruited to capture diverse treatment experiences across care models. Recruitment was iteratively reviewed to ensure the final sample represented the racial and social demographics of the broader clinic population. 29 Eligible participants had attended at least one visit between 2022 and 2023. Potential participants were cold-called by N.K.A. and provided information about the study. Voluntary participation and confidentiality were emphasized. Individuals under 18, without English fluency, or unreachable after 3 attempts were excluded. Qualitative interviews were conducted June to August 2023. Recruitment ended when thematic saturation was reached, and no new themes emerged from the interviews. 29
Data Collection
Interviews lasted 45 to 60 minutes, were audio-recorded, and transcribed verbatim. N.K.A., a medical student with 4 years of qualitative methodology experience, conducted all semi-structured interviews by phone or in-person at the clinic. N.K.A. was not known to the participants or involved in their clinical care. Self-identified demographic information, including age, race/ethnicity, gender identity, and substance use, was collected by survey (Supplemental Appendix A). Permission to access each participant’s electronic health record was obtained. A brief chart review was conducted to determine the participant’s current care model and to assess SUD severity based on DSM-5 criteria.
The interview guide was developed by a team of addiction clinicians (I.K., J.R., N.M.) and qualitative researchers (N.K.A., L.F.W.) following a comprehensive literature review of different SUD treatment models (Supplemental Appendix B).8,30,31 The interview guide was iteratively revised after conducting the first 3 interviews based on participants’ understanding of the prompts. Questions explored (1) participants’ substance use history, (2) experiences with SUD treatment, and (3) preferences among integrated, colocated, and coordinated models. To ensure a clear understanding, the interviewer read aloud the defining criteria for each model before eliciting participants’ perspectives. To assess model preference, participants were then asked, “If you could choose any of these models, which do you feel would best meet your needs, and why?” Open-ended follow-up questions were used to explore their reasoning further. Participants were provided $25 gift card compensation.
Data Analysis
Transcripts were imported into the Dedoose software, version D 9.0.85, and subjected to analysis employing both deductive and inductive coding methodologies, along with thematic analysis techniques.29,32 We applied the socioecological model of health as our framework to characterize patient-reported barriers and facilitators, given its utility in identifying factors shaping individual experiences and informing multilevel interventions.33-35 Production of deductive, first-pass codes was guided by the socioecological model and a literature review on barriers and facilitators to SUD treatment.30,31 Further inductive codes were generated during the interview process through the utilization of analytic memoing.29,36 Once all interviews were completed, N.K.A. and L.F.W. independently coded 2 interviews. The authors met to resolve coding conflicts and reach consensus. They repeated the process for 2 more interviews until consensus was reached and the codebook was finalized (Supplemental Appendix C). N.K.A. coded all remaining interviews. Initial subtheme analysis influenced the development of second-pass pattern codes, which were applied to all transcripts. The final thematic analysis was reviewed collaboratively, and consensus was achieved by the research team. This approach provided a nuanced account of the data and highlighted common threads across interviews.37-39 Additionally, one participant provided feedback on the findings, corroborating the results. 40
Results
Participant Characteristics
Fifteen individuals participated in this study and represented the demographics of the clinic at large. Participants’ average age was 56.9 years (standard deviation = 11.6). One third of participants (n = 5) were female, while two thirds (n = 10) were male. Most were white (n = 13) with 2 black or African American participants. Five identified as Hispanic/Latinx. Substances used included opioids (n = 9), alcohol (n = 9), stimulants (n = 5), and benzodiazepines (n = 3). Six reported polysubstance use. Seven participants were in a colocated care model, 3 in an integrated model where their PCP was dual-boarded in internal medicine and addiction medicine, and 5 in a coordinated model, where PCPs were located within the same county as the addiction clinic. Details on participant demographics and substance use are available in Table 1.
Self-Reported Demographics and Other Participant Characteristics (n = 15).

Abbreviations: DSM, Diagnostic and Statistical Manual of Mental Disorders; SUD, Substance use disorder.
Preferences for Treatment Models
When asked which model of care they would choose if given the option, 10 participants stated they would prefer an integrated model, 4 selected coordinated, and one chose colocated. Among the participants who preferred the coordinated and colocated models, over half expressed willingness to consider an integrated model if their PCP received addiction training. Specifically, all 4 participants with OUD-only preferred integrated care, whereas 3 of the 4 participants with alcohol use disorder (AUD)-only preferred colocated or coordinated care. Among participants with polysubstance use disorder (PSUD), preferences were mixed, with 4 preferring integrated care and 2 preferring coordinated care. The single participant with stimulant use disorder (StUD)-only preferred integrated care. The socioecological model was used to categorize data into 4 major themes that underpinned these treatment preferences (Figure 2; Table 2).
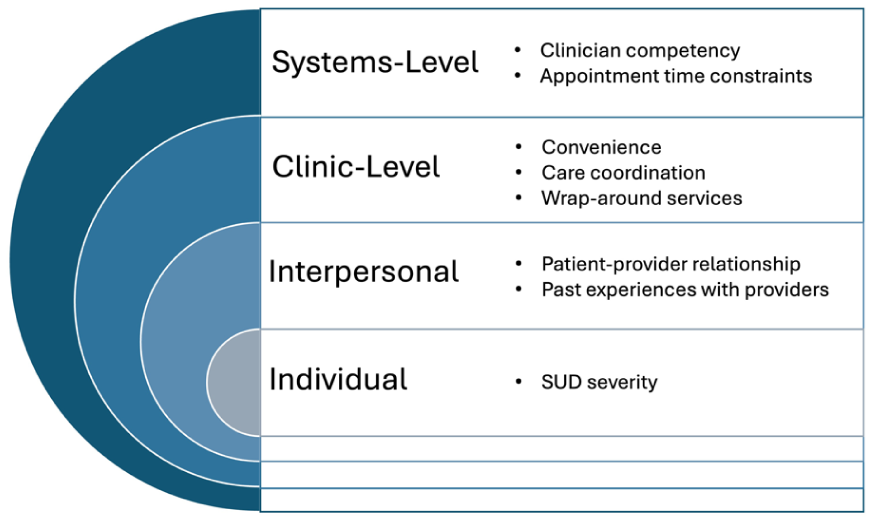
Socioecological model of health: Preferences for integrated versus colocated/coordinated care models.
Perceived Barriers and Facilitators of the Integrated Treatment Model: Emergent Themes and Quotes Organized Using the Socioecological Model of Health.

Abbreviations: SUD, Substance use disorder; PSUD, Polysubstance use disorder; PCP, Primary care provider; OUD, Opioid use disorder; AUD, Alcohol use disorder.
Individual—SUD Severity
Participants’ treatment model preferences were shaped by their assessment of their own SUD severity. Those who preferred the integrated model often described their condition as less severe, more stable, or manageable within primary care. Several participants in long-term recovery viewed specialist care as “overkill” (59, male, PSUD) or “unnecessary” (62, male, OUD): Comparing it to a healthy athlete going to a cardiologist on a regular basis if there’s no symptoms or signs. When I feel like it’s out of control, then I know that an addiction specialist is always there. (59, male, PSUD)
Some participants described their substance use as a short-term response to stressors rather than a chronic condition: It would make sense to speak to an addiction specialist for people that have less situational addiction problems than I do. . . I am going through a really rough patch in my life. It’s easier to focus on the appointments that seem more important. (40, male, PSUD)
Conversely, participants who preferred the coordinated model often described their SUD as more complex, refractory to treatment, or requiring a higher level of care:
The PCP only model might be good if you are still in the early stages—when your PCP can handle what’s on deck and it’s not too insane yet. But I think the point that I got was really severe and it did require the involvement of specialists. (48, female, AUD)
Therefore, while the integrated model was favored by those with an uncomplicated SUD diagnosis and treatment course, it was perceived as insufficient for patients with SUD of higher severity.
Interpersonal—Patient-Provider Relationship and Past Experiences with Providers
Preferences for treatment models were also shaped by the quality of participants’ relationships with their PCPs and their past experiences discussing substance use. Those who had established, trusting relationships with their PCPs often favored the integrated care model. They cited the benefit of having a provider who could address their health needs holistically and longitudinally: “Other doctors don’t know my whole story. Your PCP knows everything. They know your whole medical history. They know everything in your chart” (70, Male, OUD). These participants also expressed comfort with discussing substance use with their PCP, often referring to their provider as “a very empathic person” (57, male, PSUD) and “not judgmental” (47, female, StUD).
In contrast, participants who described negative experiences with PCPs often preferred to seek care from an addiction specialist. Some reported feeling stigmatized or dismissed when disclosing substance use in primary care settings. One participant recounted:
I was turning in dirty tests and the only thing they [PCP] would do was to threaten not to give me any pain medication versus giving me some help. That was the worst thing—I felt so low. (65, female, PSUD)
Another shared, “He treated me like I was some kind of criminal, like a scumbag addict” (70, male, PSUD).
These participants often viewed addiction specialists as more knowledgeable and more accepting. One participant noted that addiction specialists understood substance use as a “disease” rather than a “moral failing” (58, male, OUD). Ultimately, participants’ treatment model preferences were influenced by participants’ relationships with their provider, their previous experiences with disclosure of substance use, and where they perceived they were most likely to receive compassionate, nonjudgmental care.
Clinic-Level—Convenience, Care Coordination, and Wrap-Around Services
Participants who preferred the integrated model often described it as “convenient,” noting that receiving care for both general health and substance use in one setting reduced the need for multiple appointments and addressed transportation challenges. One participant stated, “I wouldn’t have to make additional appointments. I could address the problem readily” (70, male, OUD). Receiving SUD treatment within a primary care setting was also perceived by some as less stigmatizing than visiting specialty addiction clinics: “It’s embedded in a primary care clinic which is why I sort of feel okay. Not everyone who comes here is coming for addiction” (47, female, StUD).
In addition to convenience, several participants discussed care coordination as a valued feature of integrated clinics. They described the benefit of having a single provider manage both medical and substance use–related care. This provider was likened to a “quarterback” (40, male, PSUD) or “hotel manager” (39, female, OUD) who could guide patients through complex systems and promote continuity: “You have one person you can contact with questions and they tell you where you need to go and when” (62, male, OUD). Participants also noted addressing addiction alongside other medical issues felt appropriate and comprehensive. One participant explained: “A lot of preventive medicine and general medicine if you will—weight loss, low blood pressure, diabetes, etc.—go hand-in-glove with addiction treatment and recovery” (58, male, OUD).
Regardless of model preference, many participants expressed a desire for access to comprehensive, wrap-around services, including certified peer recovery specialists: “The professional—it’s more book-learning. I think that the peer—you’ve been there, done that” (75, female, PSUD). Others noted the importance of access to counseling, support groups, and 12-step programs:
For people who aren’t interested in medication as much as they are in like behavioral stuff, you need the therapists too. It’s rarely just addiction—it’s mental too. (40, Male, PSUD)
One participant described counseling services as essential to recovery, noting that while medication offered protection—“a seatbelt”—therapy helped them avoid the crash altogether: “Learning how to drive safely and not crash my car—seatbelt or not” (46, male, AUD).
Systems-Level—Clinician Competency and Appointment Time Constraints
Participants across all care models identified clinician competency as an important factor influencing treatment preferences. Many expressed concern that PCPs lacked the specialized knowledge needed to effectively treat SUD. As one participant put it, “Primary care doctors are not qualified” (70, male, PSUD), while another emphasized:
You want to be seen by the most competent and qualified person. There’s a lot to know and you can’t know everything. That’s why you specialize. (46, male, AUD)
This perception was particularly common among those who preferred the colocated and coordinated models, where the involvement of addiction specialists was viewed as essential: “There’s a big difference between diabetes and sorting out alcohol addiction. . . it’s much better to have a specialist to talk about that” (57, male, AUD).
Several participants who favored the integrated model also expressed concerns about PCPs’ ability to manage SUD: “I am afraid that the general practitioner just wouldn’t have that same nuance or same knowledge. . . that helps with recovery—or doesn’t hurt recovery too” (75, female, PSUD). However, participants with access to PCPs boarded in both internal medicine and addiction expressed high levels of satisfaction:
She is a medical doctor but also she is an addiction counselor too. We can speak the same language. We know the same recovery cliches. . . I feel like she gets me. (58, Male, OUD)
Participants across all models expressed greater openness to SUD treatment from PCPs with knowledge of addiction. Many who initially preferred colocated or coordinated models noted they would consider integrated care if they felt the PCP had sufficient expertise. Although the clinic providers in this study were dual-boarded in internal medicine and addiction medicine, participants were often unaware of their credentials. Instead of formal board certification, they described “adequate training” as a provider’s knowledge, recovery-oriented approach, and sensitivity to stigma. Still, the limited availability of addiction-trained PCPs was a commonly cited barrier: “We need more GPs trained in addiction” (57, male, PSUD).
Beyond competency, participants also raised concerns about structural time constraints in primary care. In integrated settings, limited visit durations were seen as insufficient to address both general health needs and SUD: “[My PCP] only has 30 minutes to talk to me. I don’t want to spend the whole time talking. . . about the booze” (57, male, AUD). In contrast, colocated and coordinated models were described as offering more dedicated time for complex or dual health needs.
Discussion
In this novel qualitative study, most participants (n = 10) favored the integrated care model, citing convenience and longitudinal patient-provider relationships as key advantages. Those favoring integrated care valued the ability to address substance use within routine primary care visits as part of a holistic approach to their health. Conversely, participants who preferred the colocated and coordinated models identified greater SUD severity, appointment time constraints in PCP visits, and perceptions of clinician competency as influencing their preference for specialty care. Across all models, participants emphasized the importance of a strong therapeutic alliance and access to wrap-around services, including behavioral health support and peer recovery specialists.
Notably, integrated care was preferred among participants with OUD-only, StUD-only, and for some with PSUD, whereas most participants with AUD-only preferred colocated or coordinated care. This may reflect varying levels of PCP training and comfort in managing AUD compared with OUD, as well as differences in the availability of evidence-based treatments.41-43 Limited familiarity with AUD medications, low confidence in their effectiveness, and insufficient time or resources for psychosocial interventions are key barriers to integrating AUD treatment in primary care.44,45 These findings highlight the need to tailor integrated care models to specific SUDs while continuing to address barriers such as provider training, limited appointment time, and access to comprehensive support services.
Prior studies support integrating SUD treatment into primary care, demonstrating benefits such as increased patient engagement and cost savings.16,48,46 Our findings suggest that people with SUD are not only comfortable receiving SUD treatment from their PCPs, but may even prefer it. Primary care is a convenient and accessible entry point for SUD intervention. It is especially beneficial for increasing access to SUD treatment in rural or underserved areas where there are shortages of addiction specialists and psychiatrists.47,48 The integrated model helps address these gaps by leveraging PCPs’ expertise in chronic disease management, continuity of care, and evidence-based approaches like motivational interviewing. Furthermore, a trusting patient-provider relationship plays a central role in recovery, with prior research linking therapeutic alliance to early reductions in substance use and increased self-efficacy.49,50
Despite the advantages of integrated care, barriers to implementation persist. Our findings raise concerns around provider training and confidence in managing complex SUD cases. While PCPs are equipped to handle complex chronic disease management, SUD treatment can require additional knowledge around medication initiation and tapering that is not widely emphasized in medical school and residency curricula.51,52 Additionally, time constraints during primary care visits reduce the ability of PCPs to comprehensively address both SUD and other pressing health concerns. 31 These challenges highlight opportunities to refine the integrated model by enhancing provider training and restructuring care delivery.
Participants in our study did not specify a need for board certification, which requires an additional year of fellowship. Addiction-specific training can instead be incorporated earlier in medical school and residency, without requiring fellowship. Addiction education holds promise for addressing patient concerns and facilitating the successful implementation of integrated care models. Existing evidence indicates that PCPs who prescribe buprenorphine deliver care of comparable or higher quality than specialists, as defined by treatment retention. 53 However, many PCPs report limited comfort managing SUD treatment. 54
The recent removal of the X-waiver, which eliminated a critical regulatory barrier for SUD treatment, now allows PCPs to prescribe buprenorphine with reduced training requirements. 55 While this policy expands access to treatment for OUD, it also raises concern regarding PCPs’ perceived readiness to manage SUD treatment, as removal of the X-waiver has not resulted in significant increases in the number of buprenorphine prescribers.56,57 Our study nuances these concerns. Participants with AUD-only, more so than those with OUD-only, reported PCPs as lacking the skills and knowledge necessary to provide addiction care. This suggests that gaps in addiction education may be especially pronounced for AUD care. Therefore, strengthening national addiction education at the medical school and residency levels, especially for AUD treatment, could enhance clinician competency and patient engagement in addiction care.
Systems-level advocacy for increasing SUD treatment funding and insurance coverage is also essential to effectively meet patient needs. Our study underscores time constraints in primary care settings as a significant barrier to integrated care. Participants expressed concern about the feasibility of addressing both general health and addiction-related issues within a short primary care visit. Implementing strategies to increase reimbursement rates for SUD treatment and extend PCP visit durations for patients with SUD could help primary care clinics mitigate some of these structural constraints.54,58
Finally, regardless of clinic model, participants valued having wrap-around services. Prior studies on integration emphasize the importance of having additional resources built into the clinic structure, such as patient navigators to assist with therapist or psychiatrist referrals, navigating insurance challenges, and connecting individuals to local recovery programs.59,60 Furthermore, participants valued access to peer recovery specialists, individuals with lived experience who offer support in the recovery journey.60,61 Multifaceted SUD treatment that extends beyond pharmacotherapy has the potential to address diverse patient needs and improve engagement and outcomes. In the implementation of high-quality, accessible SUD treatment, it is important to ensure providers are adequately trained, insurance coverage accommodates longer PCP visits, and primary care clinics provide wrap-around services.
Limitations
This study recruited a small, self-selected sample of predominantly white, insured, English-speaking patients from a single urban academic medical center. This setting allowed exploration of different treatment models, but underrepresented perspectives of those facing greater barriers to treatment, such as people who are uninsured, reside in rural communities, attend safety net clinics, or are not engaged in treatment.62-64 Additionally, recruiting from a primary care–based addiction clinic and conducting some interviews at the clinic may have biased responses toward integrated care. However, steps were taken to minimize bias by ensuring that the recruiter and interviewer were not involved in participants’ care. Finally, this study was conducted in an urban setting with interoperable electronic health records and may not generalize to more siloed systems with limited communication and data sharing.
Conclusions
We found that participants expressed a preference for receiving both SUD treatment and primary care from a single, longitudinal provider. This preference highlights the potential benefits of integrated care models in improving access to SUD treatment and enhancing patient engagement among patients who are already engaged in primary care. Adequate training for PCPs is a principal intervention in the future innovation and implementation of integrated care models. Medical directors establishing primary care–based addiction clinics should consider patient-perceived barriers and facilitators to tailor the clinic model to patient needs. This includes providing patients’ access to wrap-around services including patient navigation and peer support, facilitating clinician training on SUD treatment, and allotting additional visit time for patients diagnosed with SUD. Addressing challenges posed by persistent treatment barriers underscores the importance of ongoing efforts to integrate addiction care into primary care settings.
Supplemental Material
sj-docx-1-saj-10.1177_29767342261426173 – Supplemental material for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care
Supplemental material, sj-docx-1-saj-10.1177_29767342261426173 for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care by Nikki Kalani Apana, Noelle G. Martinez, Leah Fraimow-Wong, Jessica Ristau and Irina Kryzhanovskaya in Substance Use & Addiction Journal
Supplemental Material
sj-docx-2-saj-10.1177_29767342261426173 – Supplemental material for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care
Supplemental material, sj-docx-2-saj-10.1177_29767342261426173 for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care by Nikki Kalani Apana, Noelle G. Martinez, Leah Fraimow-Wong, Jessica Ristau and Irina Kryzhanovskaya in Substance Use & Addiction Journal
Supplemental Material
sj-docx-3-saj-10.1177_29767342261426173 – Supplemental material for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care
Supplemental material, sj-docx-3-saj-10.1177_29767342261426173 for “We Need More General Practitioners Trained in Addiction”: Patient Perspectives on Substance Use Disorder Treatment in Primary Care by Nikki Kalani Apana, Noelle G. Martinez, Leah Fraimow-Wong, Jessica Ristau and Irina Kryzhanovskaya in Substance Use & Addiction Journal
Footnotes
Ethical Considerations
The University of California, San Francisco Institutional review board approved this study.
Author Contributions
N.K.A.: Conceptualization, data curation, formal analysis, investigation, methodology, project administration, resources, validation, visualization, writing—original draft, and writing—review and editing.
NGM: Formal analysis, investigation, methodology, project administration, supervision, writing—original draft, and writing—review and editing.
L.F.W.: Formal analysis, investigation, methodology, and writing—review and editing.
J.R.: Conceptualization, investigation, project administration, supervision, and writing—review and editing.
I.K.: Conceptualization, formal analysis, investigation, methodology, project administration, supervision, writing—original draft, and writing—review and editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
