Abstract
Adolescents with attention deficit hyperactivity disorder (ADHD) represent a significantly heterogenous group in terms of cognitive and social ability. Given the high co-occurrence of ADHD and autism, it is unclear whether the social difficulties seen in ADHD may be attributed to the same underlying factors which contribute to social difficulties in autism, or are a unique feature of ADHD. This study explores differences in cognition in adolescents with clinically elevated ADHD symptoms with and without social difficulties, and adolescents with ADHD symptoms and autism. Thirty-nine adolescents completed objective measures of cognition (attention, working memory, inhibition) and social cognition (affect recognition, theory of mind [ToM]). Adolescents with ADHD symptoms and social difficulties had poorer proactive inhibition than both those without social difficulties, and those with autism. Lower cognitive performance was only significantly related to social functioning for adolescents with ADHD who experienced social difficulties. ToM was weakest in those with autism. Social difficulties in adolescents with clinically elevated ADHD symptoms are associated with poor proactive inhibition, working memory and affect recognition. This highlights the potential benefit of cognitive strategies for remediating social difficulties in ADHD, and the need for ADHD specific interventions.
Lay abstract
Around half of teenagers with attention deficit hyperactivity disorder (ADHD) experience significant difficulties forming and maintaining friendships. This in turn often has negative effects on schooling and mental health. There is a large body of research that suggests the social difficulties commonly seen in ADHD may be due to weaknesses in skills such as impulse control, working memory, recognising emotions, and perspective taking. Given teenagers with autism often present with similar weaknesses and social difficulties, it is not known whether the social difficulties experienced by teenagers with ADHD have the same underlying causes. If so, this may suggest that social difficulties in ADHD represent undiagnosed autism, or low-level autism traits. This study compared these key skills in teenagers with clinical ADHD symptoms who experience social difficulties, with those who don’t experience social difficulties, and those with co-occurring autism. The results showed that social difficulties in ADHD and autism appear to have different underlying causes, suggesting that the social difficulties seen in teenagers with ADHD are unique to this disorder, and are not due to underlying autism, or autism traits. This highlights the need for social skills interventions, particularly those that target impulse control, emotion recognition and working memory, that are specifically tailored to the needs and weaknesses of teenagers with ADHD, rather than using existing interventions designed for teenagers with autism.
Keywords
Social connection and acceptance have long been acknowledged as basic human needs, with adolescence representing a period of increased social salience (Tomova et al., 2021), however, the last 2 years of the global COVID pandemic have demonstrated just how critical social relationships are to our mental health and wellbeing (Loades et al., 2020). For some adolescents, such as many of those with attention deficit hyperactivity disorder (ADHD), social isolation and loneliness are not new experiences, but rather something they have lived with since childhood (Grygiel et al., 2018). Whilst ADHD is largely characterised by difficulties in attention and impulsivity, social difficulties, social rejection and loneliness are often reported as the most significant concerns for those with ADHD, and their parents (Bora & Pantelis, 2016). The nature of these social difficulties has been well characterised in the literature (McKay et al., 2023; Morris et al., 2021), however the underlying causes of social difficulties in ADHD remain unclear. There is preliminary evidence to suggest that cognitive performance may be key to understanding why social difficulties in ADHD are so pervasive, and why some adolescents with ADHD are affected while others are not (Tseng & Gau, 2013).
ADHD is known to be a highly heterogenous disorder, with significant differences in presentation, cognitive ability and functional capacity (such as academic functioning and emotion regulation) between individuals (Faraone et al., 2021). The social experiences of adolescents with ADHD are equally varied. Research suggests that between 50% and 70% of adolescents with ADHD will experience social difficulties (Antshel et al., 2009), whereas others present with social skills and social relationships comparable to their typically developing peers (Maya Beristain & Wiener, 2020a). It is not uncommon for studies of social functioning in ADHD to produce seemingly contradictory findings as a result of the significant variability within the population. For those adolescents with ADHD who do experience social difficulties, social interactions are characterised by repeated rejection from peers, conflictual relationships, loneliness and feelings of social isolation (Houghton et al., 2020; Maya Beristain & Wiener, 2020b). Given the importance of social belonging to mental health and wellbeing (Tomova et al., 2021), it is imperative to understand why some adolescents with ADHD experience social difficulties when others do not.
Differences in cognitive functioning have long been recognised as a defining feature of ADHD. Both males and females with ADHD often present with difficulties across multiple domains of executive functioning including inhibitory control, working memory, cognitive flexibility and attention (Loyer Carbonneau et al., 2021). Of these, differences in working memory (i.e. the ability to temporarily hold information) and inhibitory control (i.e. the ability to suppress behaviours and responses) are the most prevalent (Areces et al., 2018; Kofler et al., 2019; van Hulst et al., 2018), and appear to be comparable across genders (Loyer Carbonneau et al., 2021), and are consistently present irrespective of intelligence quotient (IQ; Cadenas et al., 2020).
When it comes to cognitive difficulties in ADHD, inhibitory control has been one of the most widely researched cognitive domains (Francesco et al., 2016). Research into inhibitory control in ADHD has suggested that these difficulties are confined to reactive inhibition, whilst proactive inhibition is unaffected (van Hulst et al., 2018). At face value, it holds reason that difficulties in inhibitory control would be associated with greater hyperactive and impulsive symptoms such as risk taking and mood dysregulation, and behaviours such as interrupting and talking over others, all of which can negatively impact social relationships. Despite this, a relationship between response inhibition and social difficulties has not been consistently demonstrated with some studies providing evidence for (Bunford et al., 2018; Neely et al., 2016), and others against (Kofler et al., 2019). Studies examining the relationship between other executive functions such as working memory have produced similarly contradictory results (Bunford et al., 2018; Kofler, Harmon et al., 2018; Kofler, Irwin et al., 2019; Zendarski et al., 2021). The reason for the discrepancies in findings may be methodological, as not all studies have adopted an approach which takes into consideration the significant heterogeneity of adolescents with ADHD with regards to social functioning. One key feature and limitation of the majority of studies which examine cognition and social cognition in ADHD is the comparison to children and adolescents with ADHD (as a singular group) to their typically developing (TD) peers only (Bunford et al., 2018; Kofler et al., 2018). The concern here is that treating adolescents with ADHD as a singular group neglects the significant heterogeneity of this cohort, potentially obscuring findings in the process.
Research into social cognition in ADHD has also proven similarly inconclusive. Social cognition encompasses a range of skills necessary for perceiving, interpreting and responding to social stimuli, such as recognising emotions and perspective taking. These skills are considered to be related to, but independent from cognitive functions such as attention, inhibition and working memory (Beauchamp & Anderson, 2010). There is evidence to suggest that children and adolescents with ADHD present with similar difficulties in social cognition to those seen in Autism Spectrum Disorder (autism), though generally to a lesser severity (Bora & Pantelis, 2016; Demopoulos et al., 2012). These include difficulties in the domains of affect recognition and theory of mind (Bora & Pantelis, 2016; Sjöwall et al., 2013; Staff et al., 2021). This therefore raises the question of whether social cognition difficulties in ADHD may be attributed to undiagnosed co-occurring autism, or whether they represent a distinct feature of ADHD.
Differentiating between ADHD and autism in childhood can be challenging due to the considerable overlap in symptoms and high co-occurrence of these diagnoses (Mouti et al., 2019; Rommelse et al., 2018). Children with both diagnoses often do not receive these at the same time, as symptoms of one often mask the other (Mouti et al., 2019). Difficulties in differentiating adolescents with ADHD from those with ADHD and undiagnosed autism therefore presents a barrier to reaching a consensus on whether social cognitive difficulties are a core feature of ADHD or merely reflect undiagnosed autism in ADHD samples.
Children with autism typically present with restricted interests, repetitive behaviours and differences in social cognition and social communication (such as reduced reciprocity and use of non-verbal communication) when compared to their peers (American Psychiatric Association, 2013). It is widely accepted that children and adolescents with ADHD frequently present with elevated autism symptoms when compared with typically developing peers (Grzadzinski et al., 2016; Kochhar et al., 2011; Mulligan et al., 2009). Despite these two groups appearing similar with regards to their symptoms and behaviours at face value, the function and causes of these behaviours often differ significantly (Andrade et al., 2009; Barkley, 2014). For example, it is theorised that elevations on autism subscales relating to restricted interests and repetitive behaviours may reflect the adaptive coping strategies utilised by adolescents with ADHD, such as a preference for orderliness and routine, rather than representing the construct which the subscales are designed to measure (Neely et al., 2016). Similarly, low social motivation in ADHD samples may be attributed to repeated social rejection and elevated levels of social anxiety (Bishop et al., 2019; Vanhalst et al., 2017), rather than a lack of motivation to engage in typical social interactions such as that commonly seen in autism (Neuhaus et al., 2021). Given limitations in the specificity of autism screening measures to differentiate between autism and ADHD (Grzadzinski et al., 2016), the use of such measures to exclude participants who may have undiagnosed autism from ADHD studies therefore comes at a cost to the representativeness of the sample and generalisability of the findings by reducing ADHD samples to only those without autism symptoms.
Despite a wealth of research demonstrating the pervasiveness of social difficulties in ADHD and the negative consequences of social difficulties to mental health (Saeri et al., 2018), behavioural, academic and vocational outcomes (Mikami & Hinshaw, 2006; Mrug et al., 2012), the myriad of interventions and programmmes designed to remediate social difficulties in ADHD have been largely ineffective, particularly in adolescents (Storebø et al., 2019; Willis et al., 2019). These interventions have typically involved cognitive-behaviour therapy and psychoeducation approaches, with progress assessed on a range of parent, teacher and self-report measures of social functioning (Storebø et al., 2019; Willis et al., 2019). The ineffectiveness of current social skills programmes may be due in part to the fact that social difficulties in ADHD are associated with inconsistent performance of social skills, rather than a lack of social knowledge of social rules and norms (Aduen et al., 2018). Whilst some social skills programmes for adolescents with ADHD have been shown to improve social knowledge, this has not been found to translate to improvements in social skills (Mikami et al., 2017; Morris et al., 2020; Storebø et al., 2019), and improvements in social skills that have been seen tended to be inconsistent across reporters, and not maintained long term (Willis et al., 2019). Arguably this is because although adolescents with ADHD already possess the requisite social knowledge they may not have the ability to consistently apply it due to difficulties at a cognitive level; for example, a tendency to interrupt others in conversation may be due to difficulties inhibiting this response, despite knowing that interrupting is not socially acceptable. Providing a clearer understanding of the factors which contribute to social difficulties in ADHD will help guide strategies and recommendations for addressing these difficulties, which do not rely on unnecessary social skills training.
Aims and hypotheses
The challenges that arise in determining underlying causes of functional difficulties (due to co-occurring diagnoses and heterogeneity) has prompted an increase in studies which aim to better characterise these samples and identify subgroups within and across disorders (Knott et al., 2021). A similar approach to understanding cognitive and social difficulties in ADHD would be beneficial. To date, there are no known studies which compare cognitive profiles of adolescents with ADHD with and without social difficulties (including those with autism). Specifically, it is unknown whether adolescents with ADHD who experience social difficulties present with cognitive difficulties more similar to those of other adolescents with ADHD, or those with ADHD and autism. This study therefore aimed to determine: (1) whether there are group differences in cognition, social cognition and social difficulties; (2) whether there is a relationship between cognitive and social cognitive functioning, and social difficulties within groups and (3) whether the relationship between cognitive functioning and social cognitive functioning, and social difficulties differs between groups.
Based on past research it is hypothesised that subgroups of adolescents with ADHD will be identified, with these subgroups each characterised by differing profiles of social and cognitive functioning. It is hypothesised that social difficulties will be associated with difficulties in multiple cognitive domains (including social cognition) (Tseng & Gau, 2013). Finally, it is hypothesised that the relationship between cognition and social functioning will differ between groups, with social cognition difficulties most pronounced in those with co-occurring autism (Bora & Pantelis, 2016).
Method
Participants
The sample comprised 39 adolescents (male = 27; female, = 11; gender diverse = 1) aged 13 to 18 years with clinically elevated ADHD traits, who were recruited through schools across metropolitan blinded, and via ADHD and parenting related groups in the community, and via social media. Participants were excluded from the study if they had (a) a neurodevelopmental disorder (other than ADHD or autism); (b) a history of neurological impairment (e.g. Stroke, epilepsy and acquired brain injury) or (c) any physical or mental impairment which would prevent them from completing assessment tasks such as vision impairment or psychosis. Participants represented a diverse range of ancestries including non-indigenous Australian/New Zealander (79%), Aboriginal and/or Torres Strait Islander (3%), Asian (5%), African (3%), Middle Eastern (8%) and European (38%).
Participants were screened using the Conners-3 parent report form (Conners, 2008). Previous clinical ADHD diagnosis was reported by parents for 36 participants (92%), and all participants had clinically elevated ADHD symptoms confirmed by T-scores >60 on either the inattention or hyperactivity/impulsivity subscales on the Conners 3 parent report scale. Participants reported an average age of diagnosis of 9.31 years for males and 10.30 years for females (average age of diagnosis has only been reported for groups with more than one participant to maintain anonymity). Eight participants had a clinical diagnosis of autism reported by parents and confirmed using the Social Responsiveness Scale 2nd edition (SRS-2). Participants were grouped as ADHD (clinically elevated ADHD symptoms and no social difficulties), ADHD + SD (clinically elevated ADHD symptoms and social difficulties) and AuDHD (clinically elevated ADHD symptoms and co-occurring autism). Social difficulties were determined by T-scores >60 on the Conners-3 Peer Relations subscale (see Table 1 for participant characteristics and demographics).
Participant characteristics and demographics.
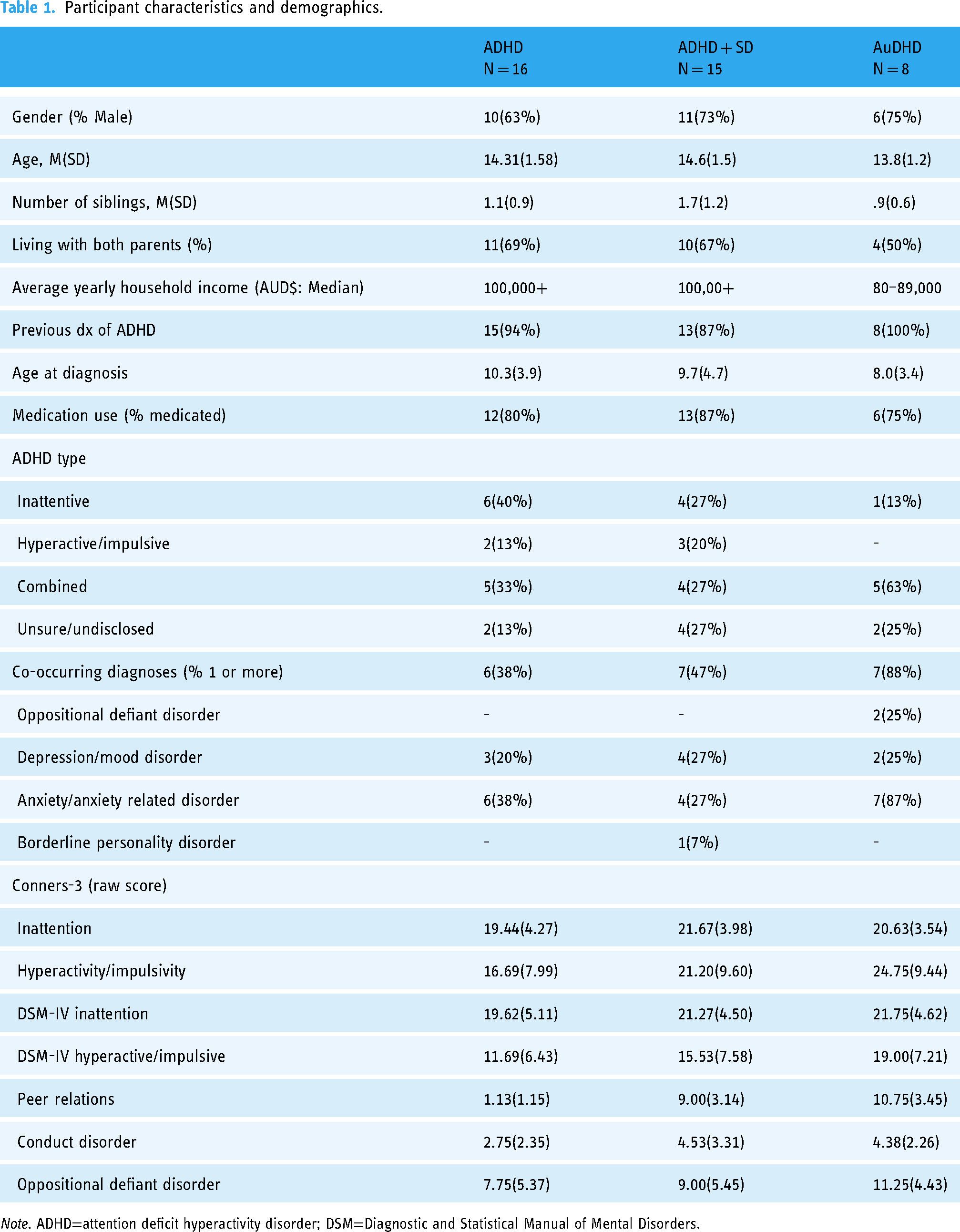
Note. ADHD=attention deficit hyperactivity disorder; DSM=Diagnostic and Statistical Manual of Mental Disorders.
Measures
ADHD symptoms and social difficulties
The Conners-3 parent report form (Conners, 2008) was used to measure ADHD symptoms and social functioning. The Conners-3 is a 99-item questionnaire designed to measure ADHD symptoms and related difficulties in children aged 6 to 18 years. The Conners-3 comprises subscales relating to ADHD symptoms and common co-occurring problems including four ADHD-related subscales: Inattention, Hyperactivity/Impulsivity, DSM-IV ADHD Inattentive and DSM-IV ADHD Hyperactive/Impulsive. Participants were determined to have clinically elevated ADHD traits if they obtained a T-score of 60 or above on any of the four ADHD-related subscales. The Peer Relations scale of the Conners-3 provides a measure of social difficulties, with clinically elevated scores (T-scores of 60 or greater) indicative of difficulties with forming and maintaining friendships, social connection, and peer acceptance. Parent report of social difficulties was used as adolescents with ADHD have been found to underestimate functional difficulties on self-report measures (Emeh et al., 2018).
Autism symptoms
The Social Responsiveness Scale 2nd edition (SRS-2; Constantino & Gruber, 2012) was used to confirm autism status. The SRS-2 is a 65 item, parent-report questionnaire designed for use in children and adolescents aged 4 to 18 years. Items are based on criteria for autism spectrum disorder from the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5). The SRS-2 comprises five subscales (Social Awareness, Social Motivation, Social Cognition, Social Communication and Restricted Interests and Repetitive Behaviours [RRB]), the sum of which gives a total score. Severity ratings are based on total scores, with T-scores of 66 and above indicative of clinically significant difficulties in reciprocal social behaviour, typical of autism of moderate severity or higher. Parents/caregivers are asked to rate how true they feel each statement is of their child on a four-point Likert Scale (ranging from not true to almost always true). The SRS-2 has strong internal consistency (.94 to .96) and concurrent validity with moderate to strong correlations with other comparable measures (Bruni, 2014).
Attention
Selective attention, sustained attention and attentional control were measured using the standard version of the Attention Network Test (ANT; Fan et al., 2002). The ANT is a computerised task suitable for use with adolescents and adults. Target stimuli comprise an arrow flanked by either congruent or incongruent arrows. Spatial cues are used to indicate the timing and placement of the stimulus appearance, double cues and central cues indicate only the timing of the stimulus appearance. The task comprised a practice block of 24 trials with feedback on speed and accuracy followed by three blocks of 96 trials without feedback. Default parameters were used with a cue presentation of 100 ms, fixation duration post cue of 400 ms and a maximum target/flanker presentation of 1000 ms with each trial lasting 4000 ms in total. Selective attention was measured using the orienting network score, calculated by subtracting the mean reaction time (RT) in the spatial cue condition from the mean RT in the central cue condition. Sustained attention was measured using the alerting network score, calculated by subtracting the mean RT in the double cue condition from the mean RT in the no cue condition. Attentional control was measured using the executive control score, calculated by subtracting the mean RT in the congruent flanker condition from the mean RT in the incongruent flanker condition. The ANT has good test–retest and split-half reliability, and construct validity (Macleod et al., 2010).
Inhibitory control
Inhibitory control was measured with the Open Source Anticipated Response Inhibition Task (OSARI; He et al., 2021). OSARI is a computerised task which measures the ability to inhibit prepotent motor responses. The task comprises 200 trials across five blocks with each block comprising 25% Stop trials and 75% Go trials. The tracking method is used to adjust the Stop Signal Delay (SSD), adjusting with a step size of 25 ms with bounds of 50 and 775 ms, initialised at 500 ms. Participants are instructed to fixate on yellow target markers before holding down the space bar, and then releasing the space bar when the indicator bar reaches the target markers. In Stop trials the bar stops before reaching the target markers, requiring participants to inhibit the initiated response to release the space bar. Reactive response inhibition is assessed by determining the Stop Signal Response Time (SSRT), with decreased SSRT indicative of greater inhibitory control. Proactive response inhibition is assessed by comparing the Mean Go response time on a block containing only Go trials, and blocks containing both Stop and Go trials.
Working memory
A backward digit span was used to measure working memory. In line with recommendations by Wells et al. (2018) on increasing digit span validity in participants with ADHD all trials were administered, rather than using a discontinue rule to account for fluctuations in attention. Two trials were administered for each digit span comprising a total of 14 trials (maximum digit span of 8), at a rate of one digit per second.
Social cognition
Social cognition was measured using the Social Perception Domain subtests of the NEPSY, 2nd edition (NEPSY-II). The NEPSY-II is a standardised neuropsychological test designed for children aged 5 to 16 years. The Social Perception Domain comprises Affect Recognition and Theory of Mind. These subtests measure how children and adolescents process social information. In the Affect Recognition subtest participants are presented with images of children's faces with different expressions of emotion (happiness, sadness, anger, disgust and neural). Participants are asked to identify which children are exhibiting the same emotion in a variety of conditions (e.g. Timed presentation of target stimulus), testing their ability to differentiate between different emotions of differing intensity. Low total scores are indicative of poor affect recognition. The Theory of Mind subtest measures the ability to understand experiences and perceptions from another perspective, and the ability to understand intent, deception, imagination and beliefs. Participants are asked questions based on different scenarios presented either verbally or visually. Lower scores on the Theory of Mind subtest are indicative of poorer ability to engage in perspective taking and difficulty comprehending the beliefs and experiences of others.
Procedure
Parents/Caregivers were emailed a link to an online questionnaire through REDCap (Research Electronic Data Capture), an electronic data capture tool hosted and managed by Helix (blinded) comprising the study consent form, demographic and screening questionnaires (Conners-3, SRS-2). Informed consent was provided by parents/caregivers, and participants provided signed assent. Participants were invited to attend an assessment session either at their school, or at the blinded facility. All assessments took place in a quiet room, to minimise visual and auditory distractions. The assessment tasks were administered by two researchers with the order of task administration counterbalanced across assessment sessions to reduce order effects. The ANT was administered via Inquisit Labs 5, with all computerised measures completed on an Alienware Area 51 m laptop with 17-inch display. Assessments took between 90 and 120 min to complete, with participants offered regular breaks between tasks. Participants were not required to cease medication prior to the assessment session. The study was approved by the blinded Human Research Ethics Committee.
Data analysis
Power analysis completed in G*Power v3.1 indicated a recommended sample size of 34 for a one-tailed Pearson correlation, based on an α of .05, estimated large effect size (.5) and power of .95; and a sample size of 102 for a one-way analysis of variance (ANOVA), based on an α of .05, estimated large effect size (.4) and power of .95. Due to the small sample size, bootstrapping was used for between group comparisons, using 2000 bootstrapped samples with a bias-corrected and accelerated, 95% confidence interval (CI). Bootstrapping is appropriate for small samples sizes and reduces type II error (Efron & Tibshirani, 1993; Shrout & Bolger, 2002).
Data were cleaned and analysed using SPSS v.26. Mean imputation was used to compute missing SSQ scores (N = 1; Hair et al., 2014). Case-wise deletion was used for cases with non-random missing data for the ANT (N = 3; < 10%) to avoid artificial increases in relationships with independent variables (Hair et al., 2014). Univariate outliers (+3.29SD; N = 1) were replaced with values one unit more extreme than the next most extreme score (Tabachnick & Fidell, 2007). All assumptions of linearity, homogeneity of variance and normality were met.
To assess differences in cognitive functioning between groups an ANOVA with Bonferroni Holm correction was used. This approach was chosen over multiple analysis of variance due to the lack of correlation between variables which is often associated with a lack of power (Tabachnick & Fidell, 2007). Pearson correlations were then used to determine whether there was a significant relationship between cognitive and social cognitive functioning, and parent reported social difficulties within each group, and whether this differed between groups.
Results
Participant characteristics
T-tests were used to determine whether there were significant differences between groups across demographic variables (see Table 1 for group means and standard deviations). Significant group differences were present for social difficulties; specifically the ADHD group had fewer social difficulties than both the ADHD + SD (t(29) = −9.40, p < .001) and the AuDHD group(t(22) = −10.26, p < .001). There was no significant difference between the ADHD + SD and AuDHD in social difficulties. There were no significant differences between groups on any other variables with the exception of the Hyperactivity/Impulsivity scales of the Conners-3, which showed significant differences between the ADHD and the AuDHD groups (Hyperactivity/Impulsivity, t(22) = −2.20, p = .039; DSM-IV Hyperactive/Impulsive, t(22) = −2.53, p = .019).
Group differences in cognitive function and social cognition
One-way ANOVA were used to determine group differences in cognitive function and social cognition. Group means, standard deviations and bootstrapped, bias-corrected, 95% CI are found in Table 2. There was a significant difference in proactive inhibitory control, F(2,33) = 4.63, p = .017, with η2 = .22 indicating a large effect size. This remained significant after Bonferoni Holm method for multiple comparison was applied. Tukey HSD post hoc comparisons revealed that there was a significant difference only between the ADHD and ADHD + SD groups, MDiff = 12.51, p = .022, Bootstrapped 95% CI [3.51, 22.56], with the ADHD + SD exhibiting significantly poorer proactive inhibitory control.
Group means, standard deviations and p values for between groups ANOVAs.
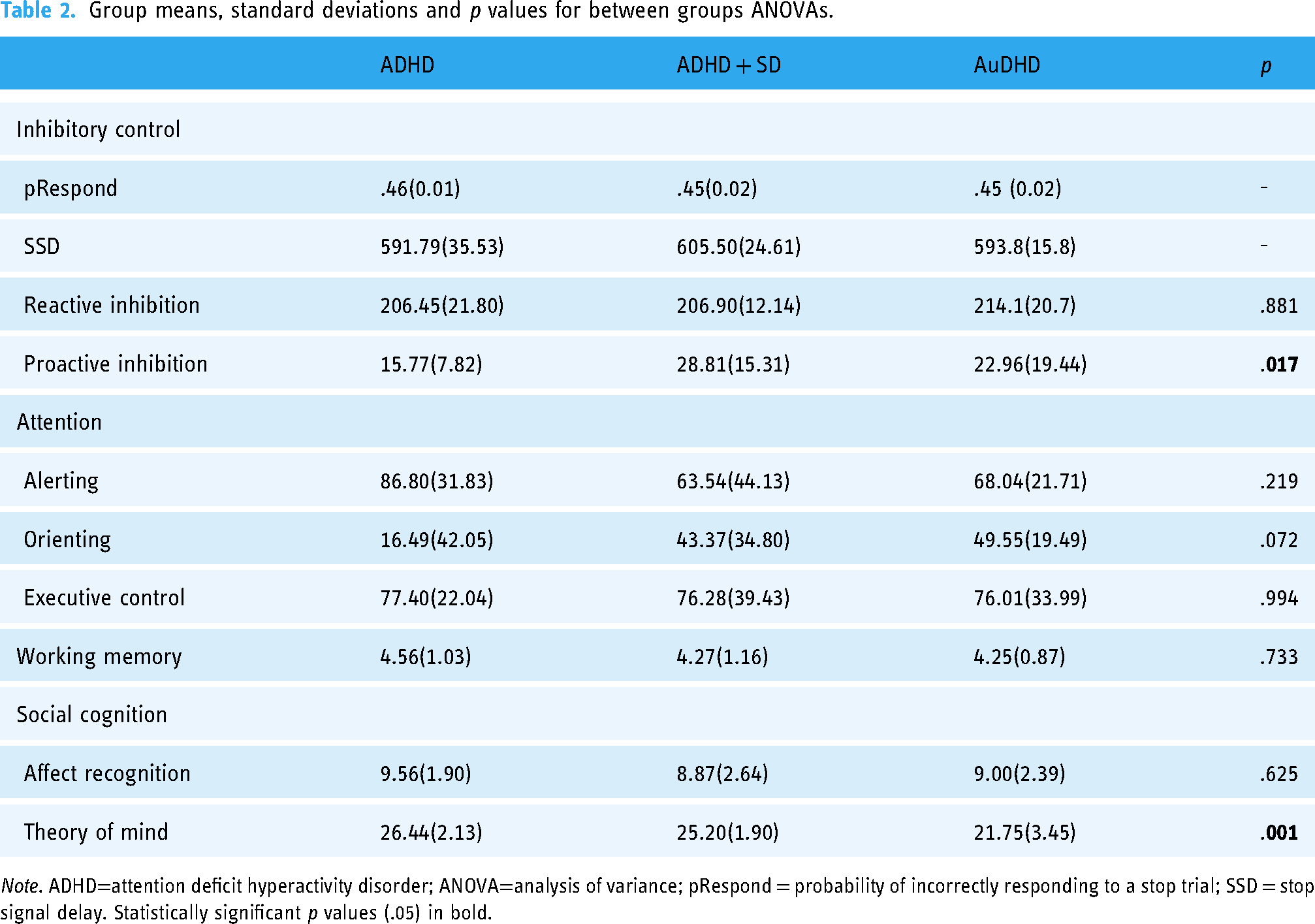
Note. ADHD=attention deficit hyperactivity disorder; ANOVA=analysis of variance; pRespond = probability of incorrectly responding to a stop trial; SSD = stop signal delay. Statistically significant p values (.05) in bold.
There was a significant difference in ToM between groups, F(2,33) = 9.40, p = .001, η2 = .36, with a large effect size. Tukey HSD post hoc comparisons revealed that there were significant differences between the ADHD and AuDHD groups, MDiff = 4.68, p = <.001, Bootstrapped 95% CI [2.05, 7.24]; and the ADHD + SD and AuDHD groups, MDiff = 3.45, p = .006, Bootstrapped 95% CI [0.84, 6.00], indicating that the AuDHD group had significantly poorer ToM than the other groups. There was no significant difference in ToM between the ADHD and ADHD + SD groups. No significant differences were found between groups on working memory, attention or affect recognition.
Relationships between cognitive and social cognitive functioning, and social difficulties
Pearson correlations between parent report social difficulties and outcome variables showed a significant, moderate to strong positive correlation between Alerting and peer relations in the ADHD group, r(14) = −.56, p = .040. This indicated that increased social difficulties were associated with better sustained attention in this group. The ADHD + SD group showed a moderate to strong negative correlation between peer relations and longest span backward, r(13) = −.57, p = .027; and peer relations and affect recognition r(13) = −.60, p = .017. This indicated that poorer working memory and affect recognition were associated with increased social difficulties. A significant, strong positive correlation was found between peer relations and executive control in the AuDHD group, r(6) = −.77, p = .042, indicating that better attentional control was associated with increased social difficulties. There were no other significant correlations between peer relations and executive functions and social cognition within groups (refer to Table 3 for correlation coefficients).
Correlations coefficients between parent report social difficulties (peer relations), executive function and social cognition.
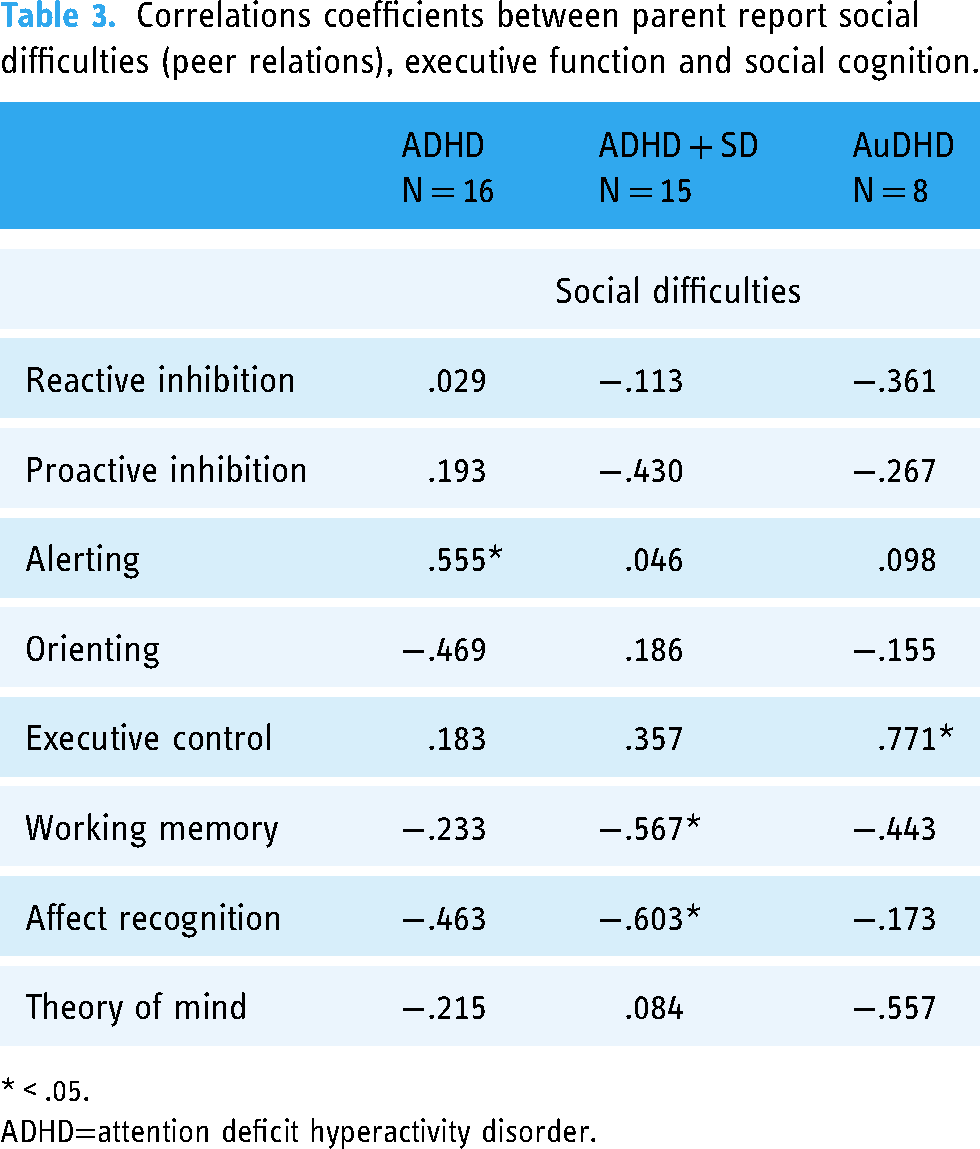
* < .05.
ADHD=attention deficit hyperactivity disorder.
Discussion
This study aimed to explore whether adolescents with clinically elevated ADHD symptoms differed in cognitive and social cognitive functioning based on their level of social difficulties, adding to previous literature by also examining how this compared to adolescents with ADHD symptoms and autism. The study also aimed to determine whether social difficulties were uniquely associated with cognitive difficulties within groups. As predicted, and consistent with previous literature (Tseng & Gau, 2013), adolescents with social difficulties performed poorer on all measures of executive functioning and social cognition than those who did not experience social difficulties with the exception of sustained attention, though these differences were only significant for proactive inhibitory control. Furthermore, adolescents with ADHD + SD were the only group whereby difficulties in social cognition and cognitive function were significantly associated with social difficulties. Correlations for the AuDHD group should be interpreted with caution given the small sample size for this group, however in both the ADHD and the AuDHD groups, social difficulties were associated with better sustained attention and attentional control respectively, rather than poorer cognitive function as would be expected.
The results provide preliminary evidence that adolescents with clinically elevated ADHD symptoms who experience social difficulties may represent a distinct sub-group, with a differing profile of difficulties than those with autism, and those with ADHD who do not experience social difficulties. In autism, difficulties in ToM are believed to be a key contributor to social difficulties (Mazza et al., 2017), and represent one of the defining differences between ADHD and autism (Rosello et al., 2020). The significant difference in ToM between adolescents with and without autism in the present study supports previous findings highlighting weaknesses in ToM in autism (Happe, 2015; Mazza et al., 2017). The significant differences in ToM between the ADHD + SD and AuDHD groups, taken together with the lack of relationship between ToM and social difficulties in these subgroups suggest that the social difficulties seen in adolescents with ADHD are not attributable to undiagnosed autism, but rather stem from a different, independent cause. This theory is supported by the differing nature of social difficulties across groups; with adolescents with co-occurring ADHD and autism often presenting with low social motivation and difficulties with shared interest (Chevallier et al., 2012; McVey et al., 2018; Vivanti et al., 2018), whereas adolescents with ADHD alone present with higher exuberance, poor turn taking and a tendency to interrupt peers (Nijmeijer et al., 2008; Thorell et al., 2017).
Whilst differences in ToM are what differentiates the ADHD + SD group from the AuDHD group, it is proactive inhibitory control that differentiates between the ADHD and ADHD + SD groups in the current study. These studies however do not consider the heterogeneity of ADHD. By treating adolescents with ADHD who experience social difficulties, and adolescents with ADHD who don’t experience social difficulties as a singular group, cognitive differences such as difficulties with proactive inhibition in one subgroup may be missed. The lack of proactive inhibition difficulties in broader ADHD cohorts does not therefore preclude the presence of difficulties in this domain in subgroups of ADHD, such as those with social difficulties.
Whereas reactive inhibition refers to the ability to inhibit an already initiated response, proactive inhibition requires inhibiting a not yet initiated response; for example the difference between stopping after you have already begun interrupting someone (reactive), or stopping before you interrupt someone (proactive). This fits with the theory that adolescents with ADHD who experience social difficulties do so because of performance deficits, rather than knowledge deficits (Aduen et al., 2018); they may have the social knowledge to understand that they should not interrupt people, but lack the proactive inhibition ability to effectively implement this knowledge. These differences in proactive inhibition may therefore explain some of the variance in social functioning between adolescents with ADHD. Furthermore, it supports the proposal that social skills training needs to focus on improving skills, rather than knowledge.
Previous research on the relationship between social difficulties and impairments in cognition and social cognition has implicated working memory and affect recognition (Bora & Pantelis, 2016; Bunford et al., 2018). Although the present study found that lower working memory, and poorer affect recognition were seen in the groups with poorer social functioning, these differences were not significant. The lack of significance may be due to a lack of power, particularly as both poorer working memory and affect recognition were significantly correlated with increased social difficulties in the ADHD + SD group. Though the observed differences in scores, particularly with regards to working memory, would not appear to be clinically meaningful, adolescents with ADHD + SD may also experience difficulties in other domains of working memory (e.g. Visuospatial) which taken together may contribute to meaningful, real world differences in working memory between groups.
This study represents the first known study to compare these two distinct subgroups (adolescents with and without social difficulties) with adolescents with autism and ADHD, and designed with lived experience input. Whilst the current study provides valuable insights into the differences in cognition and social cognition between adolescents with clinically elevated ADHD symptoms who experience social difficulties and those who do not, there are several limitations that warrant consideration. Firstly, the sample size, particularly with regards to the AuDHD group limits the representativity of the groups. Given the small sample size within groups, minimum recommended samples sizes for correlations as identified through a priori power analysis were not met, therefore results should be interpreted with caution and considered as preliminary evidence. Replication of this study in larger cohorts is needed, to establish the validity of these findings. Due to the face to face nature of data collection, and the study location (blinded) data collection was severely impacted by the COVID-19 pandemic. It should also be noted that it is difficult to determine if and how the significant restrictions on social interaction (including school closures) due to the ongoing COVID-19 pandemic may have impacted parent report of social difficulties. Whereas these external factors may have highlighted social difficulties due to changes in the way children and adolescents were able to interact with each other (online and sporadic vs. regular and face to face) and parents increased insight into the children's lives due to increased time spent together, it is also possible that fewer social interactions reduced the visibility of social difficulties. This highlights the need for further research examining changes in social difficulties, and how they are assessed, during periods of significant change or disruption. Further studies which include an autism-only groups would also be beneficial. Finally, research suggests that adolescents with ADHD typically present with low task-related motivation when compared with peers (Morsink et al., 2021). Results on objective measures of attention and inhibition may be confounded by motivation levels. It would be beneficial for future studies to include a measure of intrinsic motivation to control for the impact of varying motivation on task performance.
Overall these findings support the theory that ADHD + SD may represent a distinct subgroup of ADHD, which has both theoretical and clinical implications. Theoretically this supports emerging research which aims to use Research Domain Criteria (RDoC) to identify subgroups of ADHD and autism based on unique genetic factors and multidimensional measurement, by proposing subgroups of ADHD based on cognitive and functional (social) differences; whether these sub-groups present with differing genetic profiles is yet unknown. The findings also have implications for research aimed at better understanding social skills difficulties in ADHD. It is recommended that such studies would benefit from differentiating between adolescents with and without social difficulties, to avoid confounding results. Finally, from a clinical perspective, the differences in cognitive functioning and how this relates to social difficulties between those with and without autism suggests that social skills programmes designed for autism may not be appropriate for addressing difficulties in ADHD. Although a number of studies have trialled such social skills programmes in adolescents with ADHD, they have not proven effective (Storebø et al., 2019). Social difficulties in ADHD therefore warrant a different approach, potentially targeting cognitive difficulties in proactive inhibition, rather than social knowledge or theory of mind.
Whilst at face level the social difficulties seen across ADHD and autism may appear similar, the nature of these difficulties in reality has subtle differences, underpinned by the fact that they appear to stem from different underlying causes. The conceptualisation of adolescents with ADHD who experience social difficulties as a potential subgroup of ADHD, distinct from adolescents with co-occurring ADHD and autism may explain why social skills interventions designed for autism have not translated effectively to ADHD cohorts, and highlights the need for the development of ADHD specific social skills interventions, targeting the unique cognitive differences of this group.
Footnotes
Acknowledgements
This research is supported by the 5Point Foundation, and an Australian Government Research Training Program (RTP) scholarship awarded to Erin McKay. The authors would like to acknowledge Cassandra Li, Rachael Martin, and Brooke Dobson for their contribution to recruitment and data collection.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Australian Government, 5Point Foundation,
