Abstract
The complexity of competencies required for leaders and other members of emergency medical services (EMS) crews has not yet been sufficiently investigated. However, understanding what it means to be a competent leader and a competent other team member, and how each should behave, remains crucial for minimising errors. This study, therefore, explores the competencies and corresponding behaviours associated with both leadership and membership roles in EMS crews. A sample of 17 paramedics was interviewed using the Critical Incident Technique and the Repertory Grid Technique. Thematic analysis of the interview data revealed four overarching competency domains: (1) interpersonal, (2) cognitive, (3) task, and (4) personal. Within these domains, several key competencies, sub-competencies, and behaviours emerged – some shared across both roles, and others specific to either leadership or membership. Notably, leaders were expected to demonstrate coordination, planning, prioritising and critical thinking, whereas other team members were typically responsible for driving an ambulance, actively engaging in emergencies and following the leader's instructions. Clarifying these role-specific competencies and associated behaviours is an essential step towards integrating them into training curricula and educational initiatives aimed at enhancing the quality and safety of EMS work.
Introduction
Competencies – defined as knowledge, skills, abilities and other characteristics, 1 or as a cluster of two or more of these attributes 2 – are critical for working in healthcare, with significant implications for patient safety and outcomes.3,4 Previous research has primarily concentrated on competencies for resuscitation teams, 5 surgeons 6 or anaesthetists. 7 These studies are grounded in the framework of non-technical competencies, which are defined as social, cognitive and personal skills that contribute to safe and effective task performance. 8 They complement medical and technical competencies, which encompass specific aspects of medical diagnosis, treatment and related physical procedures. 9 The non-technical framework offers a structured identification of competencies by proposing that broad competency domains (e.g. social) can be divided into competencies (e.g. communication), further broken down into sub-competencies (e.g. sending information), and then into corresponding behaviours through which competencies manifest. 8 This hierarchical structure is highly beneficial for understanding the requirements of a specific work environment. It provides clear definitions of competencies in action and identifies observable behavioural markers that support the development of competency-based assessment and training tools to enhance safety and quality of performance. This framework has already been successfully applied in hospital-based professions, with identified competencies and behaviours integrated into competency-based practical tools.5–7 However, because different professions and work environments demand context-specific behaviours – even when certain competencies, such as communication or decision-making, overlap – it is crucial not to directly adapt tools from one field to another.10,11
Emergency medical services (EMS) face challenges that necessitate a tailored approach, due to the unique characteristics of the pre-hospital environment – marked by urgency, unpredictability and high stakes. 12 Consequently, EMS professionals require competencies that are specific to this field and distinct from those needed in other healthcare fields. 12 Despite this, there is a lack of comprehensive studies that systematically identify the full spectrum of competencies for EMS professionals. Although previous studies11,13–17 have outlined general competencies for EMS personnel, only a limited number of studies18–20 have further elaborated on these by identifying sub-competencies and their corresponding behaviours, as well as by developing competency-based assessment tools aimed at improving performance and patient care in pre-hospital settings. This gap underscores the need for research that provides a more holistic and detailed perspective on the competencies essential for effective EMS practice.
Within EMS crews, certain competencies may be shared between leaders and other crew members, as indicated by empirical and review studies.11,13–17 Importantly, leaders and other members fulfil distinct roles and duties, and are not expected to behave identically. 21 This means that each role requires its own set of competencies and associated behaviours, which must complement one another through mutual interaction to ensure crew effectiveness. 21 In other words, leaders should engage in leadership-specific practices, while other crew members should carry out membership-specific practices. However, the literature typically addresses EMS professionals’ practices in general terms or focusses solely on leaders, who are traditionally seen as those bearing the greatest responsibility for managing emergency situations.13–15,18,19,22,23 In this study, “leadership” refers to clinical leadership – the ability to guide and influence others in clinical decision-making, particularly during emergencies. 24 Clinical leadership is critical in EMS, where leaders must make swift decisions, coordinate team actions and deliver effective patient care under high-pressure, time-sensitive conditions. 25 Although some research has identified leadership 26 and membership 27 styles among EMS professionals, as well as desirable characteristics of leaders (e.g. confidence, maturity, trustworthiness, communication, planning, task assignment and decision-making) and other members (e.g. anticipation, plan adherence, instruction confirmation, task completion and communication),21,28 role-specific competencies and associated behaviours remain underexplored. Therefore, further investigation is needed to identify the competencies and corresponding behaviours required for both leadership and membership roles in EMS crews, and to understand how these roles interact to support overall team effectiveness.
The context of EMS systems – shaped by educational frameworks and cultural influences – leads to considerable variability in the competencies and expected behaviours of EMS professionals. These competencies often differ across countries, highlighting the need for region-specific research. In Slovakia, existing studies have primarily focussed on cognitive and emotional competencies22,29–31; however, no comprehensive study has yet addressed role-specific competencies within EMS crews. Moreover, the current curricula and regulations for EMS offer only vague descriptions of professional competencies and fail to clearly delineate the specific requirements associated with different crew roles.
Drawing on the framework of non-technical competencies, 8 this study aimed to examine leadership and membership competencies required for EMS work from the paramedics’ perspective. Particularly, it sought to identify the relevant competencies and corresponding behaviours – essential for advancing the understanding of role-specific competencies and for establishing a foundation for a behavioural taxonomy and rating system tailored exclusively for EMS professionals. Such a competency-based framework has the potential to enhance safety, performance quality and patient outcomes. When integrated into EMS training programmes, it can help ensure that paramedics acquire the necessary skills for effective functioning in both leadership and membership roles.
Methods
Research design and paradigm
A qualitative, descriptive design incorporating thematic analysis was employed to gain an in-depth understanding of paramedics’ personal experiences related to leadership and membership competencies. This approach enabled the exploration and identification of the characteristic features of EMS crew leaders and other members, as perceived by paramedics, ultimately informing the conceptualisation of role-specific competencies and behaviours within EMS crews. Accordingly, the present study is underpinned by an interpretivist epistemology to capture participants’ subjective realities and interpretations. Furthermore, the study followed the Standards for Reporting Qualitative Research (SRQR) guidelines. 32
Researcher characteristics and reflexivity
As researchers examining the competencies of EMS professionals, we acknowledge that our backgrounds, experiences and perspectives have shaped our approach to this study. Although we do not have direct field experience in EMS, our understanding has been enriched through our participation in an international exercise and competition for EMS crews. Through observing these crews perform simulated tasks, we gained valuable insights into the nature of their work, the breadth of competencies required and the complex challenges they encounter in real-world emergency situations.
Both authors hold university degrees in psychology, bringing distinct academic backgrounds and areas of expertise to this study. The first author has foundational knowledge of qualitative research and a broad understanding of the various competencies of EMS personnel. The second author possesses advanced knowledge of qualitative research, with a particular focus on the cognitive competencies of EMS professionals. This deliberate combination allowed us to integrate complementary perspectives. To mitigate potential bias arising from any single viewpoint, we engaged in regular reflective discussions and actively worked to reconcile differing interpretations throughout the research process.
Although the first author served as the principal researcher, each phase of the study was discussed regularly, thoroughly and thoughtfully with the second author to enhance methodological rigour, minimise subjectivity and strengthen the overall quality of the analysis. This study was also conducted as part of a broader research project involving other qualified researchers with university degrees in psychology, who were also investigating psychological phenomena within EMS crews. While discussions with these colleagues occurred sporadically, their contributions further enriched the reflexive nature of our approach.
Our training in psychology provided a unique lens for examining the competencies of EMS professionals. However, we recognise that this disciplinary perspective may carry certain limitations. To address this, we undertook an extensive review of relevant EMS literature to ensure that our interpretations were well-grounded in the realities of EMS practice.
Setting
The Slovak EMS system works in the Franco-German style and distinguishes between two basic types of ground ambulance crews. A physician-led EMS crew consists of three members: the leader (a physician) and two other members (a paramedic and a driver/paramedic). A paramedic-led EMS crew consists of two members: the leader (a paramedic) and the other member (a driver/paramedic). Physician-led crews are typically dispatched to more severe and acute cases.
In Slovakia, the professional role of a paramedic requires formal qualification and registration. Three educational pathways are recognised: (a) a bachelor's degree in Emergency Medical Care; (b) a higher professional diploma; or (c) a complete secondary vocational education in the paramedic field. Graduates of these programmes are registered healthcare professionals under the Ministry of Health of the Slovak Republic and the Slovak Chamber of Paramedics, which formally recognises their scope of practice. Nurses specialised in Emergency Medical Care or Anaesthesiology and Intensive Care Nursing, or those with at least three years of relevant practice, can also work in the role of paramedics.
In the role of EMS physicians, doctors must hold a university degree in General Medicine and be specialised in Emergency Medicine or Anaesthesiology and Intensive Care. Those who have not yet completed specialisation in these fields, who hold other specialisations, and who have at least six months of relevant practice can also serve, if they are prepared to consult their decisions with a specialist in these fields.
Ambulance staffing also includes drivers with healthcare training and a valid driving licence. While the drivers in physician-led crews must at least undergo annual training in providing basic emergency medical care in order to assist physicians and paramedics, drivers in paramedic-led crews must have healthcare education at a level equivalent to that required for working in the role of a paramedic.
Participants and recruitment
The study sample (Table 1) comprised 17 paramedics (11 men and 6 women) working in both rural and urban areas in Slovakia. Participants were purposively selected based on predefined criteria aligned with the research aim. Given the focus on professional perspectives, eligibility required a minimum of three years of EMS professional experience – considered sufficient for developing a critical understanding of the competencies relevant to EMS crew roles. 33 Individuals with less experience were therefore excluded. Since our focus was on leadership and membership competencies, only paramedics – who may serve as either leaders or other crew members – were included. EMS physicians, who consistently occupy leadership positions, were excluded from the study.
Description of the sample.

Mdn: median; IQR: interquartile range; Max: maximum; Min: minimum.
Participants were recruited via emails distributed to all companies providing EMS in Slovakia. These emails contained general information about the research, including its aim to explore the competencies of EMS professionals, and invited interested individuals to participate. To encourage participation, a €30 gift voucher was offered as an incentive for completing the interview. Those interested were asked to complete a short registration form and provide their personal email address for further contact. Subsequent communication was conducted individually via email. Only individuals who met the inclusion criteria and confirmed their willingness to participate were invited to schedule the interview.
Data collection
All interview sessions were conducted by the first author between June and December 2019, continuing until data saturation was reached – that is, when no new themes emerged. This point of saturation was confirmed through discussion with the second author. Participants chose their preferred interview location; the majority of interviews were held at the paramedic's workplace, while three took place in participants’ homes. Each session lasted between one and just under three hours. The interview process, illustrated in Figure 1, was based on the Critical Incident Technique 34 (CIT) and the Repertory Grid Technique 35 (RGT). Both techniques are well-established methods for identifying the underlying characteristics of competent performance,36,37 making them well suited to the aim of this study. Furthermore, using both techniques enabled methodological triangulation and facilitated a more comprehensive understanding of competencies.
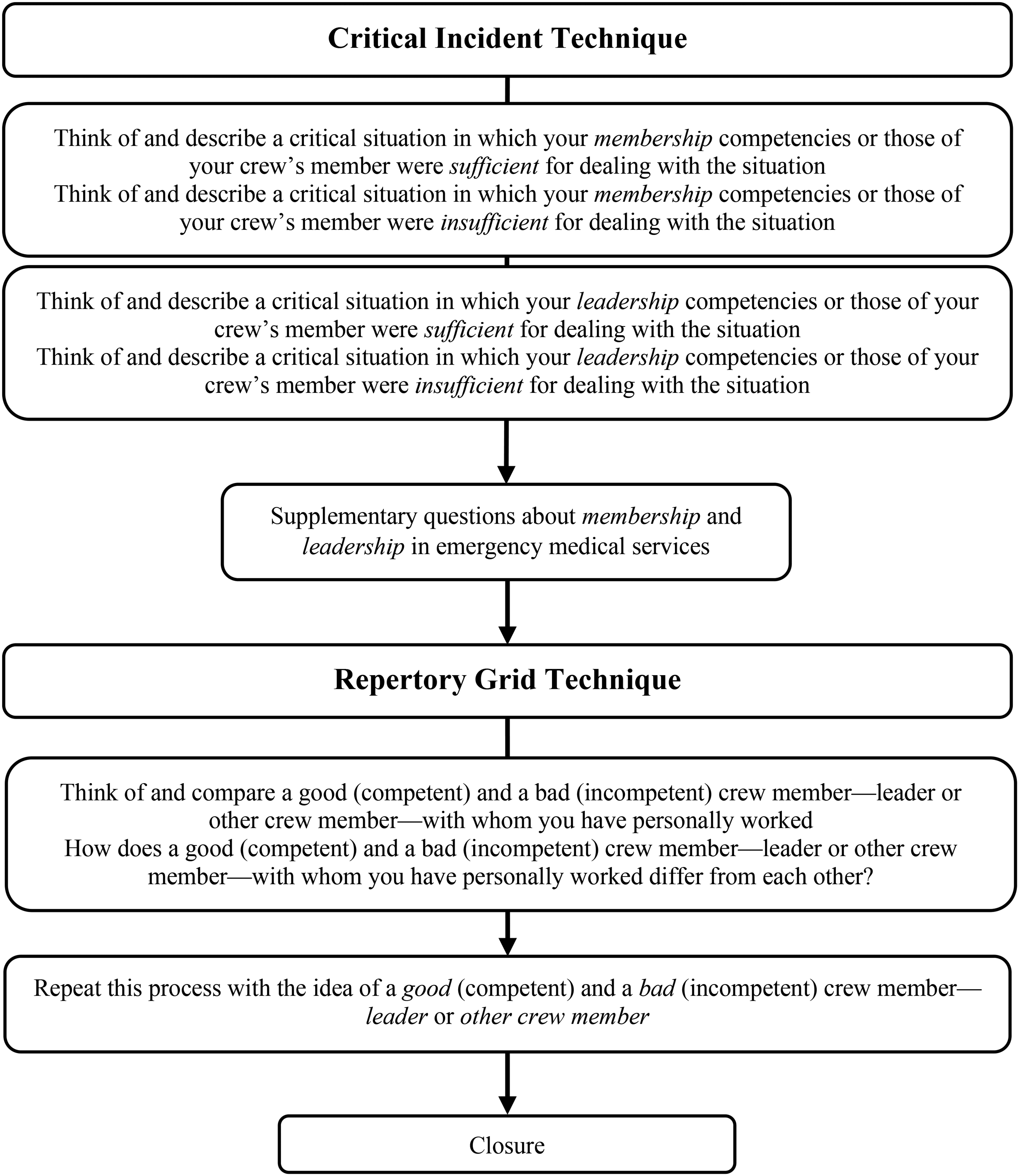
Interview process.
The CIT 34 is a semi-structured interview method designed to explore critical incidents – situations that participants identify as particularly significant in their professional experience. The focus is on events and contextual factors that impact performance in the given situation. It is widely recognised that critical situations elicit more detailed and insightful information about key aspects of professional performance – such as the knowledge and skills guiding actions – than routine ones. In the CIT-based phase of our interviews, participants were initially asked open-ended questions to think of and describe four critical situations: one in which membership competencies were sufficient, one in which they were insufficient, one in which leadership competencies were sufficient and one in which they were insufficient. Participants were instructed to reflect on their own competencies or those of their crew members in real-life situations they had personally encountered during EMS work. When initial descriptions of the situations lacked detail, follow-up probing questions were used to elicit more information. Some participants described more than the requested four critical situations, resulting in particularly rich and nuanced accounts of EMS practice.
The RGT 35 is a structured interview method designed to elicit how individuals understand and make sense of the world and the people in it. In occupational settings, it facilitates the exploration of how individuals perceive, categorise and evaluate key aspects of their work – such as competencies – thereby providing valuable insights into professional practice. In this study, participants were first asked to think of and compare a good and a bad crew member (either a leader or other crew member) with whom they had personally worked in EMS. They were then prompted to articulate the differences between these two members. These contrasting elements served to represent what participants considered a competent and an incompetent crew member, thus focussing reflection on leadership and membership competencies. Subsequently, this comparison process was repeated with participants selecting their own personal ideas of a good and a bad crew member, which functioned as metaphors stimulating deeper reflection and richer insights into the competencies required within EMS crews. 38
Although each technique has its own specific procedural guidelines, the entire interview session – including the transition from CIT to RGT – was conducted in a natural and casual manner, as both methods aimed to elicit membership and leadership competencies within EMS crews. At the beginning of each session, participants were informed about the research, signed the consent forms agreeing to participate and received a concise overview of the session structure. The first phase of the session, guided by CIT, then began with the interviewer instructing participants to recall in detail four critical situations involving both sufficient and insufficient membership and leadership competencies. Upon completion, supplementary questions were posed to expand on the CIT responses and further explore the research topic. Following this, participants were offered a brief intermission before transitioning to the second phase of the session, based on RGT. The interviewer then introduced the purpose and procedures of this phase, drawing attention to the comparison between competent and incompetent leaders or other EMS crew members. The session concluded with the interviewer expressing gratitude and providing each interviewee with a gift voucher.
Data analysis
The digitally recorded interviews were transcribed verbatim and anonymised using Microsoft Word. The transcripts were analysed using Microsoft Excel, following Braun and Clarke's six-step approach to thematic analysis, 39 which guided the entire analytic process. The first author systematically followed each step throughout the process. In total, 79 critical incidents were identified through CIT, categorised as either a well-managed experience (36 critical incidents) or a poorly managed experience (43 critical incidents). These two sets of paramedics’ experiences were analysed separately and classified under membership or leadership competencies. Initial codes were generated by the first author and subsequently organised into sub-themes and overarching themes. These codes formed the basis of an initial codebook, which included competency domains, competencies and sub-competencies. This codebook was subsequently applied to the analysis of data collected through RGT. When the RGT analysis revealed new codes not previously observed in the CIT data, these were incorporated into the evolving codebook. Where possible, behaviours were extracted directly from participants’ statements and linked to the corresponding competencies. To enhance reliability and rigour, the second author independently applied the codebook to the data. The inter-coder agreement was reviewed, and any discrepancies were resolved through multiple reflective discussions until a full consensus regarding the final codebook was achieved.
Notably, our four-tiered general-to-specific structure used in this study – comprising domains, competencies, sub-competencies and behaviours – aligns closely with the competency framework proposed by Flin et al. 8 This hierarchical framework emphasises the importance of categorising competencies into domains, which represent key areas of performance and are consistent with other healthcare competency frameworks. 40 Such categorisation helps organise the diverse skills required in high-risk fields like EMS, promoting clarity and specificity in both assessment and training. Within each domain, competencies represent specific, observable and measurable clusters of knowledge, skills and abilities that are essential for effective performance. They define the “what” of effective practice and form the foundation for safe, high-quality outcomes in healthcare settings. 8 Sub-competencies offer a more granular delineation of these competencies, providing detailed insight into the constituent skills or knowledge components. 41 Finally, behaviours are observable and measurable actions and communications that reflect the demonstration of a competency or sub-competency. They illustrate the “how” of effective practice and provide reliable indicators of an individual's real-world capabilities.
Ethics approval
This study is part of the Grant No. VEGA 2/0070/18 (Cognitive and Social Skills Supporting Decision Making and the Quality of Performance of Emergency Medical Services Crew Members) that has been reviewed and approved by the Ethics Committee of the Slovak Academy of Sciences, Bratislava, Slovakia. All participants signed a consent form to participate in the study.
Results
Four common competency domains for both membership and leadership emerged: (1) interpersonal domain, referring to interpersonal interactions between crew members; (2) cognitive domain, encompassing crew members’ cognitive processes; (3) task domain, focussing on crew members’ performance of tasks; and (4) personal domain, relating to crew members’ attitudes and qualities. Within the domains, competencies and sub-competencies accompanied by associated behaviours were identified. The full list is presented in Table 2. Regarding competencies, critical thinking was identified exclusively as a leadership requirement, while all other competencies applied to both leadership and membership roles. In terms of sub-competencies, involving crew members, prioritising and planning, and generating creative solutions were specific to leadership, whereas ambulance driving was unique for membership. The remaining sub-competencies were shared across both roles. Notably, no behaviours were linked to the competencies of critical thinking and performing procedures, nor to any competencies within the personal domain.
Competencies and behaviours required for membership and leadership of EMS crews.
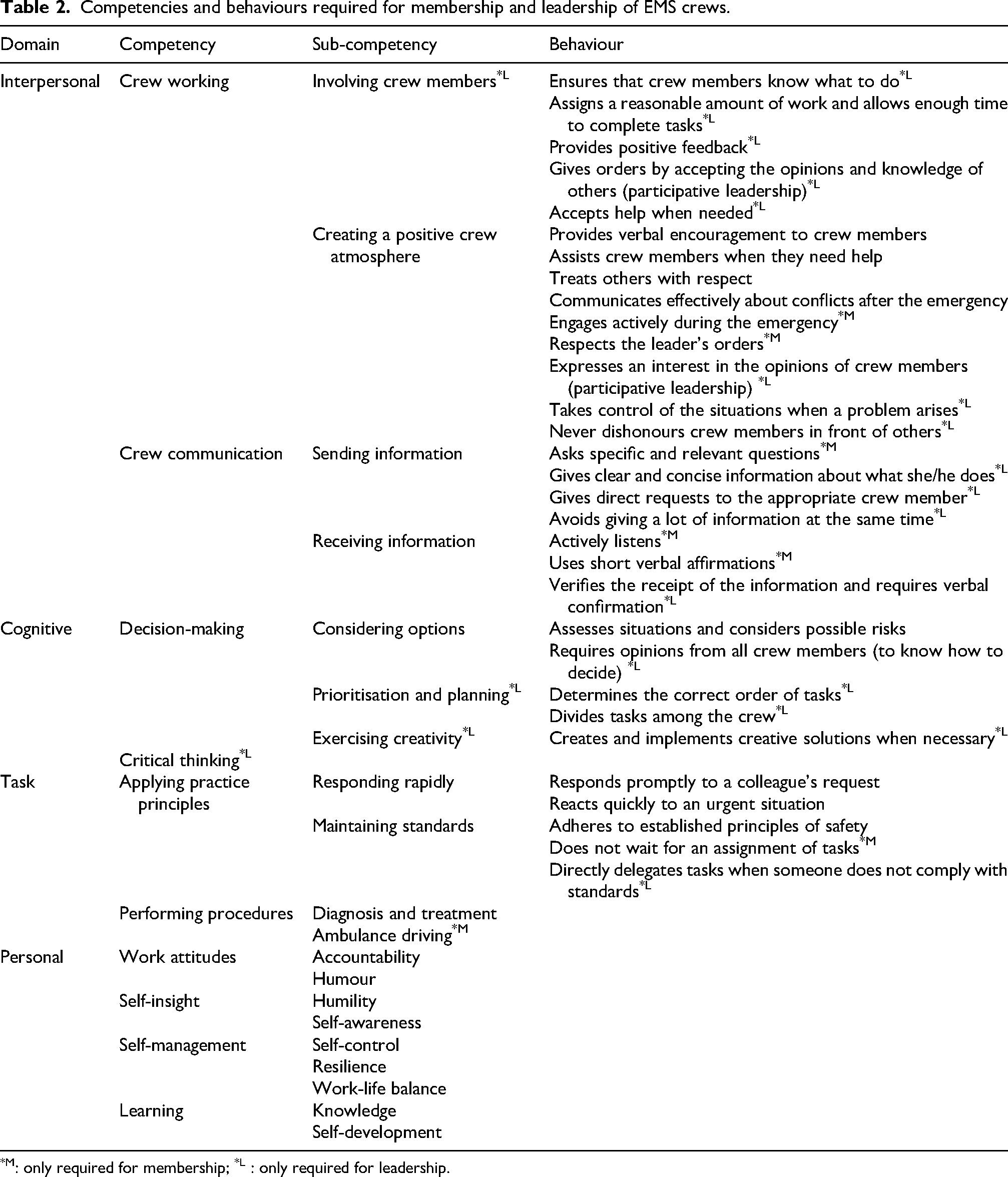

: only required for membership; *L : only required for leadership.
Interpersonal domain: crew working
Involving crew members. It was described as a key sub-competency specific to leadership and characterised by acknowledging individual members’ capabilities (e.g. accepting others’ opinions and knowledge, or accepting help when needed). According to paramedics, involving crew members enhanced crew effectiveness and fostered an atmosphere that encouraged greater initiative. In contrast, they noted that situations where crew members acted on their assumptions without accepting others’ input could result in diagnostic errors, patient harm or conflicts. A physician [the leader] prescribed the wrong treatment, but I wasn’t satisfied with the drug – magnesium – which is for cerebral blood flow. I didn’t give the patient the drug, but I said nothing. The patient could have bled even more into his brain. It was obvious that he was bleeding, but the physician didn’t listen to us. (P9) The leader didn't let me help, even though I wanted to try. He was nervous, the patient suffered, and the family saw it all. (P11)
Paramedics especially appreciated leaders who allowed them to learn and were willing to share their knowledge and skills – this is a specific example of involving crew members. When learning opportunities and collaboration were encouraged, paramedics were better able to identify areas for further improvement. I was working with a medical director, and he knew I had studied at university. So, he told me I could try to solve the situations as a leader. At that moment, I tried being the crew leader, but he helped me understand the situation. (P1)
Creating a positive crew atmosphere. This sub-competency concerns efforts to foster an atmosphere of collaboration, support, trust and respect within a crew during emergencies. When crew members accepted each other and demonstrated mutual respect and tolerance, interactions were perceived as more open, trustworthy and collaborative. I asked her [the leader] why she hadn’t given the patient the drug, and she told me she was scared and had no experience with the drug. I told her she didn’t have to worry because we were in it together. (P2) A good leader treats the crew as equals. They say, ‘we did it,’ not ‘I did it’ or ‘I saved them,’ but ‘we…' (P17)
The crew atmosphere also depended on three identified approaches to resolving disputes. The most common was a passive approach in which paramedics did not confront crew members when something bothered them. They described giving feedback as “a waste of time” (P4) or said, “I don’t think it is worth talking to a colleague” (P12). The second approach led to an open conflict in which crew members criticised each other in front of patients or colleagues but did not try to resolve it further. They believed they “would not find a solution anyway” (P6). This approach was associated with shame, guilt, embarrassment and reduced confidence. The third approach identified was attempting to resolve the dispute after an emergency, such as at the station. As indicated by our participants, this provided the best chance of successfully defusing the situation and restoring a positive crew atmosphere. The leader apologized for reacting poorly, and I apologized too. We agreed to resolve conflicts at the station, not in front of patients and their families. (P12)
Interpersonal domain: crew communication
Sending information. Paramedics described that leaders should give clear and concise information about their needs, and crew members should ask specific and relevant questions. When a message was conveyed by a third crew member or members who gave out a lot of information simultaneously, essential information and time were lost. I told her [the leader] the pressure readings, and instead of asking me, she repeatedly asked the driver, literally saying his name: ‘J. What was the pressure?’ So, I repeated it, and she continued to ignore me. I couldn’t understand why she wouldn’t talk to me, but we ran out of time. (P14) A good leader clearly states what they want. For instance, they'll say, ‘we're resuscitating, I need 2g of magnesium,’ giving precise instructions. (P11)
Receiving information. Although using two-way communication helped to avoid mistakes and paramedics recognised the importance of this type of communication, most of them did not use it. Moreover, according to paramedics, when crew members shared common experiences, communication was minimal because each member automatically knew what to do. They also stated that communication exchange with novices was not so fast, and providing them with more detailed information was essential. Well, when I work with a novice, I have to explain in more detail what I need and make sure they understand. Although my colleague studied everything about communication, it's not as spontaneous as when I’ve been working with someone for a long time. And with some colleagues, we communicate so well that I would say that it is not an optimal procedure, just one-word instructions, but we don’t need to communicate more. (P3) It helps when we communicate verbally with colleagues in critical situations. For example, when a physician asks us to prepare saline, we do it and then respond to confirm. This way, everyone knows what's happening. (P14)
Cognitive domain: decision-making
Considering options. Most of all, paramedics thought that considering options was an important sub-competency, especially for leaders, because they are legally responsible for emergencies and must weigh a series of serious issues before making a final decision (e.g. the consequences and the risks of treatments). Considering options was also identified as an important sub-competency for membership. As noted by paramedics, although other crew members do not make medical decisions, they do make key decisions in pre-hospital settings (e.g. they consider the distance between the pre-hospital scene and the hospital or other available treatment options). When facing a serious condition, the leader should know how to approach it, understand the available options, and decide what to do. (P2)
Planning and prioritising. The analysis uncovered that planning usually took place in the ambulance before the crews arrived on the scene and helped leaders to facilitate coordinated action during the emergency. Prioritisation, which was sometimes part of the planning process, was based on various criteria, such as the patient's condition. In this context, paramedics emphasised that the leaders’ ability to prioritise the assigned responsibilities in order of importance helped the crew to respond more quickly in critical situations. When we attend a critical situation such as a resuscitation or pulmonary oedema, we plan what each crew member will do. (P5) One must be able to make quick decisions, or correctly sequence them. The tasks themselves are usually clear (5–10 of them), but the challenge is deciding which to do first and which last, and then accurately delegating tasks to colleagues or doing them oneself. (P8)
Exercising creativity. As emerged from the analysis, crew leaders usually opted for creative solutions when there was no other obvious alternative and tried to keep patients safe in the face of failings or when confronted with a novel situation. However, creative solutions were useless in routine situations. The pressure did not stop the bleeding, and the dressing was soaked with blood. I [the leader] was working with an older colleague, and he taught me a trick: placing a coin on the bandage is a good way to stop the bleeding. It stopped the bleeding within a short time. I didn’t know that, and he just wrapped a coin in the bandage, and in a few seconds, the wound stopped bleeding. (P7) Some doctors withhold practical insights, but others share invaluable tips and real-world ‘know-how’ that can make a big difference during actual emergencies. (P7)
Cognitive domain: critical thinking
The ability to process, analyse and integrate information in a complex environment was identified as an essential competency for effective leadership during emergencies. It emerged that leaders must navigate high uncertainty, process the information quickly and incorporate additional factors into their professional analysis, including information from patients, family members and the social or legal context. Paramedics also highlighted a lack of experience and exposure to learning ‘outside the box.’ When a leader wants to achieve positive outcomes, he needs to connect things logically, to connect the knowledge, what he has learnt and what is required in that specific situation. (P17) The leader must have a complete overview of everything happening in the ambulance, including in the back, ensuring everything is as it should be. (P9)
Task domain: applying practice principles
Responding rapidly. Reacting quickly was described as one of the essential sub-competencies, particularly in urgent situations. According to many paramedics, waiting for instructions in such situations could delay the assistance provided or even lead to the patient's death. This was often the case when working with a novice or an inactive colleague. We worked very well, very quickly, and promptly. I knew automatically what I should do and didn’t wait for instructions from the leader. But I have new colleagues, and they don’t react so promptly. They wait for instructions, and the patients die unnecessarily. (P16) With a good doctor, they'll quickly direct: ‘We're doing this, I'm doing this, you're handling that.’ We arrive, and if the doctor is good, within 4 minutes, the patient is secured, intubated, and we're performing CPR. (P4)
Maintaining standards. Paramedics mainly mentioned the need to adhere to existing guidelines and standards for task completion. Moreover, in their opinion, since leaders must ensure compliance with standards, directive leadership was considered necessary and effective in cases where a crew member fails to maintain those standards. I [the leader] told him [another crew member] that he couldn’t do it this way. We need to have the correct documentation. I didn’t care if he wanted to or not, but we have guidelines, and we need to follow them. He was angry, but I had to take responsibility as the leader and gave him no choice but to accept it. (P3) It's crucial that no important step is missed and nothing is forgotten. (P7)
Task domain: performing procedures
Diagnosis and treatment. Performing typical medical diagnostic and treatment procedures was identified as a key leadership sub-competency for paramedic and physician crew leaders; however, it also pertains to membership. A physician's main role is to treat, cure, and master the diagnosis. (P4)
Ambulance driving. Driving an ambulance was naturally mentioned as a membership sub-competency, essential solely for other members, that is, drivers. The driving is rough—harsh acceleration and braking make it uncomfortable in the back. If I feel sick, I can only imagine how the patient must feel. (P4)
Personal domain: work attitudes
Accountability. The analysis revealed accountability as one of the personal sub-competencies, referring to a personal concept of responsibility and the ethical aspects of health care in performing functions associated with specific roles. Each crew member has to be responsible. That means that leaders should behave like physicians or paramedics, and they should want to help the patients. That is why we do our job. Plus, colleagues who are drivers should know what that job means. (P7) Some EMTs take the salary but lack knowledge or willingness. They aren't interested in the job. Some drivers won't even get out of the ambulance unless I explicitly call them for help, implying their job ends once they park. (P5)
Humour. Although humour was not considered an inevitable personal attribute for EMS work, from the perspective of paramedics, it was essential for building relationships, added a human dimension to the support provided to crew members, and helped counteract the effects of managing stressful situations. We don’t talk about serious cases or situations. More often, we tell morbid jokes. In our job, it's better to joke than be serious. We should stay calm and not get stressed. (P16)
Personal domain: self-insight
Humility. Behaving respectfully towards all crew members and understanding others’ limits was valued by paramedics and regarded as a core component of good crew relationships. In contrast, the exaggerated self-confidence created a hostile work environment and hindered members’ ability to work together. The physicians [the leaders] always think they are superior or better than the paramedics [other members]. Of course, they know more than we do, but I don’t think it's just in professional life, but in personal life as well. They think they are more than us. (P15) If you have a good leader who isn't arrogant, they won't be left alone; their team will support them. (P11)
Self-awareness. Another personal sub-competency identified was self-awareness, defined as the ability to recognise inadequate responses. According to participants’ statements, it manifested as a willingness to apologise to colleagues and an awareness of the factors that may contribute to the situation, such as being in a bad mood or having attended a highly stressful incident. Blaming colleagues and the inability to admit mistakes led to disputes, which negatively affected the participants. They [the leaders] can tell superiors how dissatisfied they are with you and how you did not follow their instructions, and then you can be penalised by management. They can revoke your licence and move you to another station with more emergencies. (P6) Most importantly, one must be able to accept feedback from colleagues or the team; it shouldn't be immediately rejected. (P8)
Personal domain: self-management
Self-control. The interview analysis showed that crew members also have to cope with negative emotional states and inappropriate reactions from colleagues, such as verbal aggression. They often did not know how to respond properly when faced with such unacceptable responses. The physician [the leader] didn’t like that I hadn’t written down when the first physiological function was measured. And he started yelling at me in front of the patient and family: ‘You are not fulfilling your duties! You are not paying attention to the things you should!’ Well, I shouted that the patient's treatment was important and that if he had a personal problem with me, I was sorry. I know I didn’t handle it well. (P9) When under pressure, they sometimes lash out and say, ‘What do you want?’ rather than staying composed. (P8)
Resilience. Paramedics appreciated that resilience in various situations helped them focus their attention on the quality of the service and on working together as a coordinated crew. A crew member's inability to withstand a stressful situation made it difficult for colleagues because they needed extra time to do all the work independently, especially when the crew comprised two members. Moreover, less experienced paramedics described feeling more fearful and unable to react promptly in critical situations. The child had fallen out of the window and couldn’t be saved. It was a severe trauma and there was nothing we could do. The crew leader couldn’t function, so I put him in the ambulance. And I was racking my brains and didn’t know what to do. Should I tell the father that we have a physician who is so shaken up he can’t even write the report? (P8) It's about not getting overwhelmed by panic and maintaining a cool head when chaos surrounds you, because otherwise, rational action becomes impossible. (P16)
Work-life balance. Paramedics highlighted the importance of balancing work and personal responsibilities. In doing so, some paramedics viewed misfortune as a natural part of life, while others struggled to cope. They experienced difficulty in sleeping and ruminated on the situation for several months. I couldn’t sleep and couldn’t stop thinking about the patient. So, I went to work at midnight because I had to find out what had happened to the patient. (P2) It's essential to have a way to vent stress, a hobby where you can release tension. For example, I exercise, which helps me clear my head. (P5)
Personal domain: learning
Knowledge. Paramedics, in particular, emphasised that colleagues’ knowledge helped them during emergencies, as they could rely on them. However, some felt the leaders and other members lacked prior experience working in highly stressful environments or dealing with critically ill patients. And he [the leader] did things that didn’t benefit the patient. For example, he wanted venous access. But it's not the most important thing for that kind of patient. What was needed was securing the airways and ensuring the patient was adequately ventilated. So the key was to check his pulse to see if he had a pulse at all. (P6) Regarding transport, the crew member should know how to prepare equipment, use a vacuum mattress, and help load a splint—it's part of their core competencies. (P2)
Self-development. Lifelong learning and the retention of practical skills were regarded by our participants as an integral part of EMS work, closely linked to the voluntary and self-motivated pursuit of knowledge. The difference lies in trying to learn. Even if a person hasn’t been to university, they can study, gain experience, and learn what to do from colleagues. But not everybody is like that. Some colleagues didn’t attend the training courses in our company, which unfortunately are voluntary, not compulsory. So, we have a colleague who didn’t know how to perform chest compressions. (P17) Some believe that once they graduate and have the diploma, further development isn’t necessary—they assume the title of ‘doctor’ says it all. (P14)
Discussion
The aim of this qualitative study was to identify perceived membership and leadership competencies required within EMS crews. Through thematic clustering in the analysis, four overarching competency domains emerged: (1) interpersonal, (2) cognitive, (3) task and (4) personal. These domains were consistent across both leadership and membership roles, and overlapped with those identified in previous studies involving healthcare professionals,6,7,42 reinforcing the interconnected nature of competencies.
Within each domain, relevant competencies, sub-competencies, and where possible associated behaviours were identified. In the interpersonal domain, two competencies emerged: crew working (with sub-competencies of involving crew members and creating a positive crew atmosphere) and crew communication (with sub-competencies of sending and receiving information). The cognitive domain comprised two competencies: decision-making (with sub-competencies of considering options, prioritizing and planning, and exercising creativity) and critical thinking, for which no discrete sub-competencies were delineated. The task domain included two competencies: applying practice principles (with sub-competencies of responding rapidly and maintaining standards) and performing procedures (with sub-competencies of diagnosis and treatment, and ambulance driving). In the personal domain, four competencies were identified: work attitudes (with sub-competencies of accountability and humour), self-insight (with sub-competencies of humility and self-awareness), self-management (with sub-competencies of self-control, resilience and work-life balance) and learning (with sub-competencies of knowledge and self-development).
The vast majority of these competencies and sub-competencies can be classified as non-technical. 8 Only diagnosis and treatment fall under the medical and technical category. 9 Additionally, ambulance driving can be considered a separate competency category. Importantly, at this granular level, clear differences in competencies, sub-competencies and behaviours emerged between leaders and other crew members. As these role-specific differences have not been sufficiently explored in previous EMS research,21,28 we discuss them along with other key findings in more detail below.
The most notable distinction between leaders and other crew members lies in cognitive competencies. The results showed that leaders, who are accountable for major decisions, must demonstrate the ability to facilitate coordinated action, prioritise based on various criteria, think critically and adopt creative solutions in complex and dynamic situations. Involving other crew members in decision-making was also emphasised by participants as a means of fostering collaboration and signalling trust in team members’ capabilities. This participative approach, corresponding to transformational leadership, 43 was found to be generally effective8,44 and underscores that participative leadership is vital for promoting team engagement in high-risk contexts. However, findings also indicated that a more directive, transactional leadership style 43 may be necessary in situations requiring strict adherence to standards or during high-stress emergencies.42,45 This dual necessity reflects the concept of leadership adaptability, according to which effective leaders shift between transformational and transactional behaviours in response to situational demands. 46
Another main distinction between leaders and other crew members emerged in the interpersonal domain. According to our findings, leaders are expected to ensure communication clarity, request assistance when needed and guide the delegation and coordination of tasks among crew members. They must also avoid overwhelming the team with excessive information, a practice that helps reduce both the communication burden and the short-term memory load required during high-pressure situations. 47 In contrast, other crew members are expected to execute tasks in alignment with the plan and adhere to instructions provided by the leader. These interactions contribute to the development of shared mental models – common understandings of tasks, roles and procedures – which are essential for enabling rapid and effective responses in emergency situations. 48
Interpersonal conflicts may occasionally arise between leaders and other crew members. Our analysis revealed three distinct approaches to conflict resolution: (1) a passive approach characterised by not going to the confrontation; (2) a public resolution occurring during the emergency, which often escalates into aggression and emotional distress; and (3) a post-emergency resolution, typically leading to effective conflict mitigation. Among these, the post-emergency approach emerged as the most constructive, underscoring the critical importance of timing in conflict resolution. These findings suggest that a collaborative conflict management style is particularly well suited to the EMS context.49,50 However, given that conflict dynamics within EMS remain relatively underexplored,50,51 future research should further investigate this area to inform evidence-based conflict management strategies.
Beyond the competencies previously discussed, possessing an extensive knowledge base was found to facilitate effective performance in all crew members, particularly in novel or high-stakes situations. Mutual support – manifested through continuous monitoring 52 and timely intervention when necessary 53 – was also emphasised as a critical component of both leadership and membership roles. Furthermore, personal competencies such as accountability, humility, self-awareness and maintaining a healthy work-life balance were deemed essential for sustaining long-term performance and well-being. These findings align with and contribute to the growing body of literature on burnout prevention and resilience in high-stress healthcare environments. 54
Our study further underscores the need to move beyond the traditional top-down model of EMS leadership towards a more collaborative and shared approach. 55 Such a shift more accurately reflects the dynamic and complex nature of EMS work, where high-pressure situations demand collective responsibility and joint decision-making. This perspective aligns with Zaccaro et al. 56 who conceptualise leadership as a dynamic process of team interaction rather than the sole responsibility of a single individual. In this context, effective collaboration among all crew members not only strengthens decision-making but also fosters mutual trust, ultimately enhancing the leader's capacity to guide teams through emergency situations.
Finally, our study emphasises the importance of self-development and lifelong learning for both EMS leaders and other crew members. While participants expressed a strong motivation for ongoing professional growth, they also reported limited access to structured training programmes that explicitly integrate leadership and membership competencies. This gap calls for the development of a comprehensive curriculum encompassing critical thinking, decision-making, conflict resolution and leadership training. 57 Existing literature on healthcare education58,59 reinforces this need, highlighting the effectiveness of scenario-based learning in enhancing preparedness among EMS professionals. In particular, well-designed fictional cases focussing on conflict management and decision-making under high stress, as suggested by Sinskey et al., 60 may serve to reduce the negative impact of blame and error,3,4 thereby promoting safer and high-quality EMS performance.61,62
Limitations
The study has five potential limitations that should be considered when interpreting the results. First, since our data are both introspective and retrospective, there is an inherent risk of recall bias or intentional distortion. However, critical incidents elicited through CIT are often unique and well-remembered. 63 The accuracy of retrospective data typically depends on the richness and specificity of participants’ accounts, which CIT tends to facilitate. 34 To further ensure data reliability, we also employed RGT, though it presents its own challenges. Notably, completing grids can be cognitively demanding, potentially leading to participant fatigue and compromised data quality. Moreover, the constructs elicited are inherently subjective and require careful interpretation. 37
Second, our analysis focussed exclusively on paramedics' perspective. As such, future research should explore the viewpoints of EMS physicians, who may offer different insights into leadership and membership competencies. Third, our interview protocol explicitly targeted membership and leadership, which may have led participants to emphasise the interpersonal competency domain, as this domain was the most extensive and contained the largest number of identified behaviours. Consequently, other domains contained fewer or no identified behaviours, suggesting that our competency and behaviour list may not be exhaustive or definitive.
This third limitation is particularly relevant for some cognitive and personal competencies, for which no explicit behavioural markers were identified. Rather than reflecting an oversight in the methodology, this highlights the nature of these psychological constructs, which are difficult to capture through interview data alone. Previous competency frameworks8,61 likewise recognise that while many skills can be defined behaviourally, other essential competencies (e.g. values, self-awareness) represent underlying capacities that inform but are not reducible to observable behaviours. The absence of markers has implications for future implementation, as these competencies may require alternative approaches to assessment and training. Identifying these domains in the present study is therefore valuable in itself, while future research may employ complementary methods – such as direct observation, simulation or longitudinal assessment – to capture how cognitive and personal competencies manifest in practice.
Fourth, although the inclusion criterion of a minimum of three years’ EMS experience was designed to ensure a baseline of professional insight, experience alone does not necessarily equate to expertise. Therefore, interpretations should take this limitation into account. Finally, a potential limitation of this study is its focus on the Slovak EMS system, which may limit the generalizability of the findings to other settings. Nevertheless, we propose that the core competency domains and crew roles identified may hold broader relevance. While adapting these findings requires consideration of key system differences – such as variations in crew composition, educational standards, equipment and protocols, and cultural norms – the competencies and behaviours described here can serve as a valuable reference point for strengthening EMS practice and training across diverse settings.
Recommendations
Given these limitations, we recommend further research to validate and extend the present findings. Future investigations would benefit from incorporating additional methodological approaches, such as the Delphi technique to achieve expert consensus, or observational and ethnographic studies conducted in either simulated or real-world EMS environments. Such methods are particularly well-suited for capturing competencies, such as critical thinking and those within the personal domain, which are not always reducible to a series of discrete, observable behaviours. These methods could yield richer insights into actual behaviours, contextual dynamics and situational factors that may not be fully captured through interview-based data alone.
Subsequent research should aim to refine and expand the identified competencies and associated behaviours, placing particular emphasis on delineating the distinct requirements of leadership and membership roles within EMS crews. Our findings indicate that these roles entail substantially different expectations, especially within the cognitive and interpersonal domains. Greater differentiation between the two could significantly enhance the specificity and effectiveness of training and assessment frameworks.
Moreover, since our study identified competencies that manifest both during and outside emergency situations, as well as over the long term, integrating situational and temporal perspectives into competency research would provide valuable insight. A more nuanced understanding of when, how and under what conditions different competencies are enacted would offer deeper insights into the dynamic nature of EMS work. Such an approach would provide a stronger foundation for designing educational activities and training interventions that are better aligned with the complex, evolving demands of EMS practice.
Implementations
Our proposed framework offers a foundational structure for developing educational activities by informing competency-based curricula, assessment tools and training programmes tailored to EMS professionals. By integrating the key competencies and associated behaviours identified in this study, educators and trainers can improve the quality and safety of EMS practice, ultimately contributing to improved patient outcomes. Additionally, the framework may support recruitment, selection, and staffing decisions by clearly outlining the competencies required for effective role-specific performance within EMS crews.
Conclusion
This study contributes to the growing body of research on healthcare professional competencies by identifying the predominantly non-technical competencies specifically required for both leadership and membership roles within EMS crews. In summary, we found that while EMS crew leaders and other members share overarching competency domains, they differ in competencies, sub-competencies and associated behaviours. Leaders are primarily responsible for facilitating coordination, planning, prioritisation and critical thinking, whereas other crew members usually drive an ambulance, engage actively during emergency situations, and follow the leaders’ instructions. Across both roles, effective conflict resolution, teamwork, clear communication, shared goals, mutual trust and collaborative interdependence are essential. All crew members must also manage high stress, possess relevant knowledge and skills and perform their duties reliably. These findings offer a valuable foundation for more detailed follow-up studies and can inform the development of competency-based curricula, training programmes and assessment tools tailored to EMS practice.
Footnotes
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Scientific Grant Agency of the Ministry of Education, Science, Research and Sport of the Slovak Republic and the Slovak Academy of Sciences (Grant No. VEGA 2/0070/18 – Cognitive and Social Skills Supporting Decision Making and the Quality of Performance of Emergency Medical Services Crew Members).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of data and material
The full interview transcripts analysed in this study are not publicly available, as this would violate the consent form signed by the participants, which includes a statement that only members of the research project have access to the raw data and that the results will be presented in anonymised form.
