Abstract
The addition of a Policy and Strategy pathway to the Career Framework for Paramedics in Canada represents a pivotal advancement for the profession, attempting to address our longstanding absence in senior health policy roles. In this commentary we explore the concept of paramedics in policymaking, emphasising the unique perspectives paramedics bring to strategic decision-making, creating novel career pathways, and enhancing professionalisation. Positioned at the intersection of healthcare, public safety, and social services, paramedics can offer invaluable insights into systemic barriers and patient needs. Their inclusion in policymaking fora aligns with global health trends, such as interprofessional collaboration, an increasing focus on sustainability, and acknowledging the need for harm reduction approaches, particularly in drug policy. By enabling paramedics to engage in high-level strategy and policy direction setting, the profession can help to address key systemic challenges including patient safety, quality of care, and equitable healthcare governance. This pathway can not only strengthen paramedicine's influence but also enhances the resilience and inclusivity of healthcare systems, contributing to better outcomes for patients and communities.
Introduction
The paramedic profession has, and continues to transform, marked by the recognition of its potential to influence not only individual patient outcomes but also broader health systems. Historically rooted in emergency response, paramedicine has evolved into a dynamic and multifaceted profession that extends far beyond the confines of the ambulance. 1 In a groundbreaking step, the recently published Career Framework for Paramedics in Canada 2 outlined ‘Policy and Strategy’ as a formal career pathway within the profession. The career framework is aimed at providing paramedics, employers, professionals and regulatory bodies with guidance and clarity on the roles and abilities of paramedics in Canada now, and in the future. 2 This addition compared to contemporary pathways internationally reflects a pivotal shift and a call from the profession in how paramedics are viewed within the healthcare system – not solely as frontline responders but as strategic influencers capable of shaping health policy and driving systemic change.3,4
The inclusion of ‘Policy and Strategy’ in the career framework acknowledges the unique insights paramedics bring to the table. Their proximity to communities,5–7 firsthand experience with gaps in the healthcare system8,9 and ability to navigate complex patient needs10,11 positions them as invaluable contributors to inform policy discussions. Paramedics routinely encounter the human consequences of policy decisions, from the lack of access to harm reduction services to systemic inequities that disproportionately affect structurally marginalised populations as just two examples.12–14 This perspective equips paramedics to contribute to identifying systemic barriers and proposing pragmatic, evidence-informed solutions alongside other health and policy professionals, supporting efforts to enhance equity, accessibility and efficiency across the continuum of care.
Understanding the role of paramedics in policymaking requires distinguishing between direct and advocacy-driven approaches, as well as the difference between advancing programmes and driving broader policy change. Policy operates at multiple levels, ranging from internal organisational policies within paramedic services to municipal, provincial and federal health policies that shape the broader system. 15 In Canada, meaningful health system change is most often driven by provincial health policy, with some areas influenced by municipal or federal directives. 16 Gaining influence at these levels requires more than expertise in policy analysis and advocacy; it also depends on social, cultural and political capital – the ability to build relationships, and navigate institutional power structures – to be recognised as a legitimate and trusted voice.
For paramedics to have a sustained impact on governmental policy, their integration into advisory roles and leadership positions must be intentional, supported by education, mentorship and institutional recognition. For the purposes of this discussion, policy refers to the frameworks, regulations and strategic decisions that shape healthcare systems, spanning legislative, organisational and funding-related directives. 17 Paramedics can engage in policy work through various mechanisms such as direct advising with government agencies or advocacy through professional associations.
Direct policymaking involves working within government or health organisations to draft, implement and evaluate policies that shape healthcare delivery. 18 In contrast, advocacy-driven policymaking focuses on influencing decision-makers through research, professional coalitions and public engagement. 19 Similarly, there is a key distinction between programme advancement – where paramedics develop and expand service models that may influence policy (e.g. community paramedicine) – and policy advancement, which involves structural changes such as funding reforms and legislative shifts. While both play a role in improving healthcare, achieving systemic change often requires sustained advocacy, cross-sector collaboration and the ability to translate the lived experiences of paramedics into compelling, evidence-informed recommendations for policymakers (Figure 1).
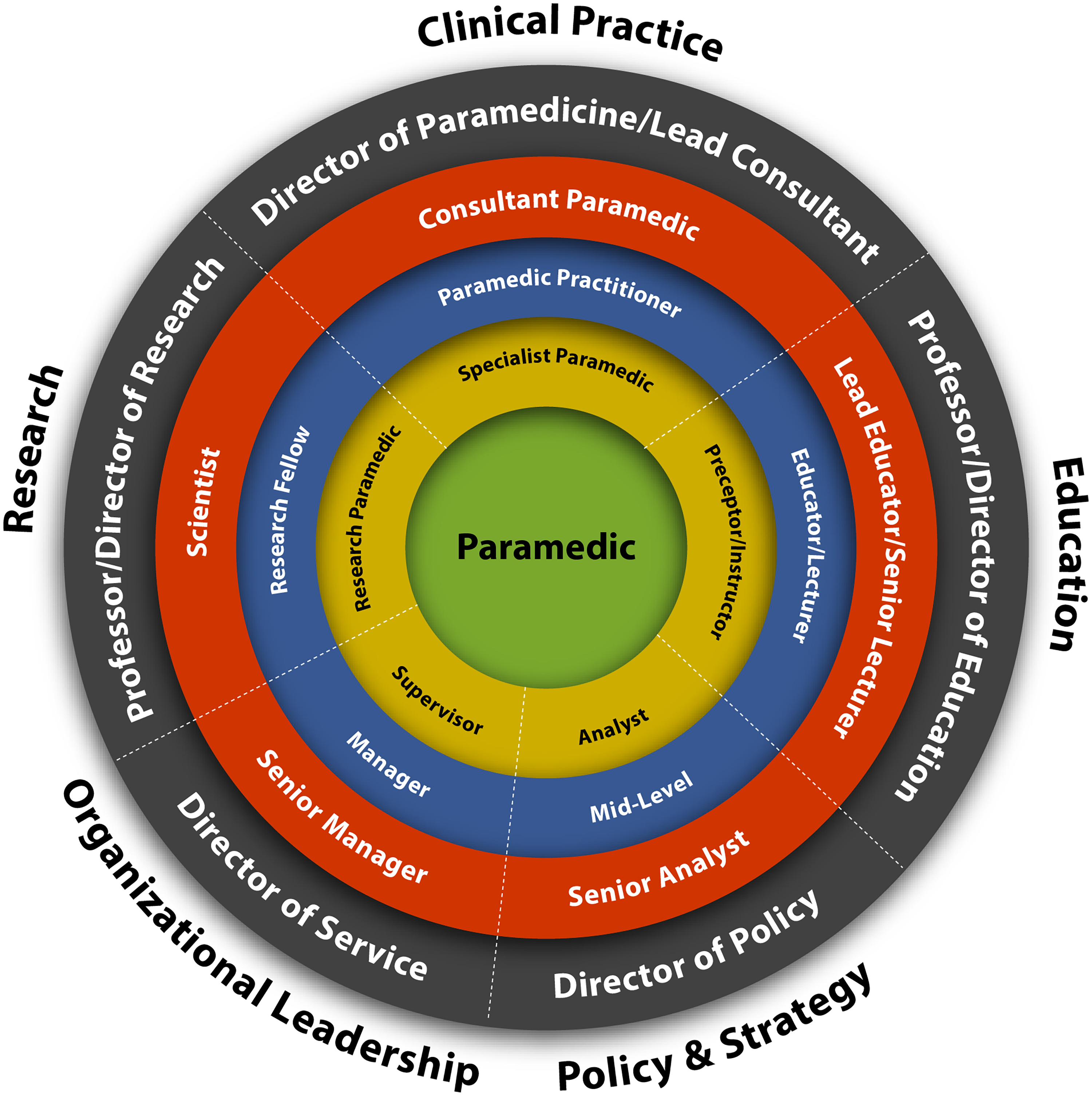
The career framework for paramedics in Canada. Reproduced under a creative commons attribution-non-commercial 4.0 International License. Original source: Cameron and Batt. Career Framework for Paramedics—1st Edition. 2024. Ottawa: Paramedic Association of Canada.
This career evolution aligns with broader trends in healthcare, where interprofessional collaboration and the integration of diverse perspectives are increasingly prioritised.20,21 Policymaking has traditionally been dominated by administrative, medical and academic voices, but the inclusion of nurses, paramedics and other allied health professionals as advisors signals a shift toward a more inclusive and representative approach. By incorporating the lived experiences of paramedics into the policy development process, health systems can gain valuable insights into healthcare provision challenges, contributing to more informed and responsive strategies that address the complex realities faced by patients and providers. For example, community paramedic programmes have emerged as a successful model of interprofessional collaboration, where paramedics work alongside other healthcare professionals to deliver primary care, outreach, care in the home, virtual care and long-term care among other models. 22 These programmes not only improve health outcomes by addressing gaps in primary care but also provide paramedics with a platform to indirectly contribute to health system strategic planning and policy development. The data and insights gathered directly from experiences in community paramedicine (e.g. patient utilisation patterns, unmet health and social needs, etc.) have been used to inform broader health policies and resource allocation decisions.23,24 In some jurisdictions, paramedics involved in these programmes have directly contributed to provincial and regional healthcare strategy discussions, influencing decisions on service expansion, funding models and integration with other community-based services.9,25 Additionally, their leadership in programme design and implementation has positioned them as important stakeholders in policy discussions related to mobile integrated healthcare, chronic disease care, and alternative care pathways. This growing influence demonstrates how paramedics, through community paramedicine and similar initiatives, are gaining a seat at the policymaking table and shaping health system evolution from the ground up.
The addition of a policy and strategy career pathway also underscores the growing recognition of the paramedic profession as a valuable player in system design and health governance. As healthcare systems grapple with unprecedented challenges – ranging from aging populations26,27 to the increasingly complex health and social needs of patients28,29 – paramedics are well-equipped to contribute to innovative policy solutions. Their ability to traverse the boundaries between acute care, community services, primary care and public health positions them as unique, but natural connectors who can bridge silos and promote cohesive, person-centered care models. Examples include mobile integrated health configurations like paramedic-staffed Mental Health Emergency Response Units,30,31 and playing a key role in providing alternative care pathways, such as mental health and substance use referral networks and nontraditional conveyance options. For instance, paramedics in British Columbia now have the option to refer patients to outreach teams following a drug poisoning, or convey patients to peer-run safe consumption sites, expanding opportunities to safeguard care in innovative person-centred ways. 32
However, such a shift is not without challenges. Embracing a policy or strategy advisor role requires paramedics to acquire new skills in policy analysis, advocacy and strategic planning. 2 It also demands a cultural shift within the profession, as paramedics expand their focus from individual patient care to systemic change. Paramedics seeking to transition into policy and strategy roles must take responsibility for developing expertise in health governance, public policy, and broader governmental processes. While institutions can support this through education and mentorship opportunities, paramedics must proactively engage with cross-sector policy and strategy programmes to build the necessary skills to navigate political dynamics.33,34
In this commentary, we explore the implications of integrating ‘Policy and Strategy’ into the paramedic career framework in Canada. We examine the opportunities this role presents for the profession, the health system and the communities served by paramedics, while also highlighting some of the challenges and considerations necessary for successful implementation. By leveraging the unique strengths of paramedics, this new career pathway has the potential to enhance health system resilience, improve patient outcomes and solidify the paramedic profession as a cornerstone of modern healthcare policy.
A brief history of health professionals in policy roles
Health professionals have historically played pivotal roles in shaping health policy, with physician voices often holding significant influence in policy leadership.35,36 This is exemplified by the roles of Chief Medical Officers (CMOs) in many governments and agencies. These positions, typically occupied by senior physician leaders, are integral to public health governance, providing expert guidance on health crises, policy development and resource allocation.37,38 However, it is important to distinguish between the formal policymaking responsibilities of physicians in government-appointed roles, such as CMOs, and the advocacy efforts of professional associations. While CMOs contribute directly to policy creation and implementation, professional associations primarily engage in policy influence by advising governments, lobbying for legislative changes and advocating for specific funding priorities. 38 This distinction is critical, as the authority and direct impact of policy development differ between these roles.39,40 Whereas CMOs work within governmental structures to shape policy from within, professional associations function externally, seeking to shape the policy agenda through advocacy and strategic engagement. 36
Chief Nursing Officers (CNOs) have also emerged as influential policy leaders, representing the nursing profession's perspective in health systems. 41 Nurses, with their holistic approach to care, have advocated for patient-centred policies and community health initiatives, broadening the scope of policymaking beyond traditional medical models.42–44 This expansion has been supported by initiatives like the Chief Nursing Officer Academy which has been developed to prepare aspiring and new CNOs. 45
Despite these contributions, the dominance of physician-led associations has sometimes resulted in an unequal distribution of health resources, with public health and preventative care receiving less funding compared to acute and specialised care.46,47 This legacy underscores the need for a more inclusive approach to health policy, incorporating diverse professional voices.
Paramedics and health policy in Canada: The current landscape
Canada's health policy landscape is shaped by a complex interplay of federal, provincial, territorial and municipal governance. 48 While the federal government sets broad health priorities, provides funding and regulates key areas such as pharmaceuticals and public health, provinces and territories are primarily responsible for healthcare delivery and system planning. 49 Policy decisions are influenced by a range of parties including government agencies, professional associations and regulatory bodies that oversee professional standards and practice.
Despite their experience and growing role in integrated care models, paramedics have historically been underrepresented in formal health policymaking structures. While some provinces have established Chief Paramedic roles at a service level (e.g. British Columbia), most policy decisions affecting paramedics are still shaped by administrators, physicians and policymakers without direct paramedic input.
Paramedics have already influenced policy in critical areas such as community paramedicine, mental health crisis response and harm reduction initiatives. For example, paramedic-led advocacy through research and more active participation contributed to policy changes in British Columbia's drug poisoning response. A study conducted in Vancouver's Downtown Eastside explored paramedics’ perspectives on drug poisoning events, emphasising their roles as both clinicians and patient advocates. 50 This research contributes to a deeper understanding of the drug poisoning crisis and informs evidence-based policy decisions aimed at improving models of paramedic-supported care for PWUD. As an example of more active advocacy, the lead author of this commentary advocated for the myriad ways paramedics can influence the patient journey for PWUD at a 2023 Select Standing Committee on Health led by the provincial government in British Columbia. 51 These examples highlight how paramedics can shape health policy through both direct involvement and advocacy-driven influence.
As paramedics increasingly engage in policy development, research and strategic planning, embedding them within Canada's health governance structures will be crucial. Strengthening these connections will not only enhance health system responsiveness and equity but also reinforce the profession's legitimacy as a critical stakeholder in shaping Canada's healthcare future.
The case for paramedics in policy roles
The inclusion of a Policy and Strategy pathway in the Career Framework for Paramedics in Canada represents a transformative step toward addressing the profession's absence in high-level health policy and strategy roles. This recognition elevates paramedicine's potential to influence organisational, regulatory and governmental policies while addressing critical gaps in decision-making and strategic planning. 2 Paramedics are trained extensively to think critically, make complex care decisions and apply the conditions of natural justice in their practice.52,53 These capabilities exhibit the natural traits required of strategic roles 54 highlighting that both their education and workplace experiences provide key foundational traits for success in such roles.
Informing policymaking
Paramedics bring a distinctive perspective to policy development, informed by the diversity of their experiences navigating health, social services and public safety systems (despite sometimes being ‘outsiders’ to the health and social care systems).9,55 This expertise allows paramedics operating at the entry-to-practice level to identify systemic barriers, propose practical solutions and advocate for underrepresented populations, including Indigenous communities and structurally marginalised patient groups.11,56 Because of the circumstances by which people tend to call for emergency health services, paramedics are well positioned to offer valuable insights into patient circumstances not otherwise observed by other health and social care professions. Because paramedics are often exposed to patients’ living conditions and social circumstances, over time, they may identify trends in public health matters otherwise invisible to the rest of the system. One such example is in Canada, where a highly contaminated supply of illicit street drugs has contributed to an ongoing public health crisis. Due to the frequency with which paramedics encounter people experiencing a toxic drug event, they may be well positioned to report anecdotal drug contamination information. Over time, this kind of reporting can contribute to the schema of drug checking and reporting, which may inform further advocacy efforts for safer drug supply policies. Developing roles where paramedics are in positions that proactively seek such information to inform policy improvements (e.g. as Directors of Policy) may allow all paramedics to have a more meaningful input into building policy.
Global trends in health policy and drug policy
Globally, health policy is increasingly focused on systemic sustainability, equity and harm prevention, particularly in drug policy. Paramedics’ involvement in these areas aligns with international movements toward integrated, person-centred care and evidence-based policymaking. For example, paramedics in the United Kingdom have embraced advanced clinical roles, including independent prescribing of medications.57,58 This regulatory change supports the health system's goals of reducing demand on primary care services and emergency departments while contributing to improved patient outcomes and satisfaction through timely, appropriate and accessible care.6,59,60 Similarly, the introduction of paramedic prescribing rights allows paramedics to autonomously manage patient care pathways, particularly for chronic conditions and urgent needs, enhancing system efficiency and patient satisfaction.
In some jurisdictions, paramedics have been integrated into opioid agonist therapy pathways, allowing them to administer buprenorphine for withdrawal management. 61 This development required changes to prescribing regulations, paramedic clinical practice guidelines and interprofessional collaboration agreements. While paramedics are now implementing harm reduction policy, their role in shaping these policies remains underexplored. For example, whilst paramedics may sit on policy advisory and development groups, their influence is not well reported in the existing literature. For paramedics to move beyond implementation and contribute to policy creation, structural changes such as formal inclusion in policy advisory committees, and dedicated policy education pathways would be necessary.62,63
Virtual care policies increasingly include paramedics, recognising their ability to facilitate telehealth consultations, remote monitoring and consistent communication.64,65 In Canada, for instance, paramedics have been integrated into virtual emergency care models to extend the reach of healthcare services to rural and underserved populations. 66 This innovation reduces barriers to care and supports the continuity of treatment for complex health and social needs.
Paramedics are also positioned to support sustainability and equity by reducing unnecessary hospital admissions through community paramedicine programmes and mobile integrated healthcare models. These initiatives align with the World Health Organisation's (WHO) call for universal health coverage by enhancing access to primary care and reducing disparities in healthcare delivery. 67 In sum, paramedics’ expanding scope of practice reflects their growing contribution to global health priorities, from harm reduction and substance use care to virtual and advanced clinical care, cementing their role as critical players in modern healthcare systems.
While paramedics have demonstrated success in implementing harm reduction, virtual care and integrated community care models, there is limited formal paramedic-led policy development. Unlike medicine and nursing, paramedicine lacks a widely recognised policy agenda or explicit policy priorities at national and provincial levels. For paramedics to transition from policy implementers to policy architects, the profession must clarify its collective priorities, strengthen its presence in policy advisory bodies, and establish formalised policy education pathways to equip paramedics with the necessary legislative and governance expertise. Achieving this shift requires moving beyond demonstrating programme success to actively engaging in the regulatory, legislative and funding structures that sustain healthcare initiatives. Paramedics must build expertise in policy analysis, governance and advocacy, while also securing formal representation in decision-making spaces such as government health committees and advisory bodies. Without these structural changes, paramedics risk remaining implementers rather than architects of systemic reform.
Professionalisation
Policy and strategy roles provide an avenue for paramedics to contribute meaningfully to health system improvements by working alongside other healthcare professionals. Key developments, such as the shift to degree-level education for paramedics, have supported their ability to participate in areas like primary care and advanced clinical practice. 68 The concept of professionalisation is complex, involving both the need to gain legitimacy within healthcare hierarchies and the ability to influence policy and governance. In this context, professionalisation is not simply about achieving status but about strategically positioning a profession within the broader healthcare and policy landscape. 69 This theory-driven approach to professionalisation recognises that while paramedics may need to develop the social and cultural capital required to engage in decision-making spaces, they also have an opportunity to shape these structures rather than simply conforming to them. By framing professionalisation around system integration, interdisciplinary collaboration and patient advocacy, paramedics can strengthen their influence in policy and governance while ensuring the profession's evolution remains centred on improving health system outcomes rather than reinforcing rigid professional boundaries.
Similarly, integrating paramedics into policymaking processes strengthens their capacity to advocate for systemic improvements, influence health priorities, and help address gaps in care delivery. These contributions enhance the profession's role within the broader healthcare system, reinforcing its ability to serve the public effectively as part of modern health governance. However, paramedicine's path to professionalisation must be informed by the lessons of medical dominance. 70 The historical marginalisation of nursing and other allied health professions in policymaking highlights the risks of rigid hierarchies and exclusionary professionalisation efforts.71,72 To avoid replicating these dynamics, paramedicine should prioritise interdisciplinary collaboration, inclusive governance structures, and policies that emphasise collective leadership rather than reinforcing silos within healthcare.
Enhanced career pathways
Finally, the development of policy-focused roles broadens career opportunities for paramedics, offering pathways that extend beyond traditional trajectories. 2 Expanding career pathways within the profession matters because paramedics report high levels of burnout and fatigue and many are leaving the profession to advance in other fields.73,74 Mason's recent research into paramedic flourishing (i.e. those who are happy and doing well in their career) identified that paramedics want goals, opportunities and support to develop, and to do meaningful work. 75 The five broad career pathways in the Career Framework for Paramedics empower paramedics to pursue a diversity of roles – even going so far as to encourage blended roles, or pursuing a portfolio of pathways in a career – thereby fostering professional growth and long-term career sustainability. Examples of policy/strategy career pathways could include policy analyst positions, executive leadership roles in the health sector (within or external to ambulance services), or even political roles such as potential Chief Paramedic Officer roles at provincial and federal government levels in the future.
Examples of paramedics advocating for systems change
Despite the current lack of formal strategy and policy roles within the profession, paramedics participate in policy advocacy efforts globally. Two such examples of paramedics advocating for systems change include our colleagues Alisha Macfarlane, 76 Dr Elizabeth Donnelly and Dr Justin Mausz 77 who have testified to parliamentary committees in Australia and Canada to inform policy and legislation advances related to gender equity and violence against health professionals (including paramedics), respectively. Another example is paramedic Jonathan Brooke, who authored an opinion piece in The Globe and Mail expressing concerns over the Ontario government's decision to close safe drug consumption sites 78 and highlighted how the replacement sites fail to provide the comprehensive and holistic care required to effectively address the ongoing drug crisis.
Challenges and considerations
The concept of paramedics in policy and strategy roles remains a critically understudied area and requires focused research attention to explore its potential. One limitation of this is the relatively small number of suitably qualified paramedic researchers (compared to other health professions), and current lack of a contemporary research agenda to guide research priorities in paramedicine in Canada. While the profession continues to evolve its identity to a more contemporary and holistic entity, 1 further exploration into what these roles look like in the job market is needed. Prioritising the exploration of paramedic roles that don’t directly engage in patient care will need to be balanced with the competing pressures of workforce shortages across the healthcare system. The argument, therefore, may need to emphasise the impact these upstream roles will have downstream (e.g. paramedic representation in policy decision making can influence funding streams that increase expanded paramedic roles in integrated care).
The continuous evolution of moving paramedicine further upstream will require a shift in mentality and a culture that supports this shift, in Canada this means starting with degree entry to practice requirements to align us with our allied health peers. 68 Degree entry to practice is not only about addressing knowledge gaps and professional alignment but also about reinforcing hierarchies that shape influence in health governance. Professions with standardised academic pathways and degree-based entry have historically been positioned as authoritative voices in policymaking and resource allocation, but this raises broader questions about how power is constructed and maintained in healthcare. The extent to which these hierarchies reflect expertise versus entrenched social and cultural capital remains largely unexamined. Understanding how these structures influence policy agendas, and whether they serve to advance equitable decision-making or reinforce exclusionary practices, requires further critical exploration.
This will serve as an essential foundation for future education to provide paramedics with the capabilities required to take on strategy and policy roles. Degree entry to practice requirements position paramedics to obtain post-graduate education including masters-level and doctoral degrees where they develop specialised skills to advance the profession. As an example, the lead author of this article (a paramedic by background) is a doctoral student studying paramedic models of care with an emphasis on drug policy reform. Systemic barriers also need to be considered, and may include resistance from other health professions, or organisational cultures that prioritise or maintain a status quo of physician leadership above paramedic leadership. 54
Lastly, practical, cultural and political barriers often limit the integration of evidence into health policy, including inconsistent access to timely and relevant research, conflicting stakeholder values, and the politicised nature of policymaking processes. Lancaster and Rhodes (2020) propose adopting systems-based approaches and ‘evidence-making’ interventions, which view evidence, context and interventions as interdependent and co-evolving. This perspective emphasises the relational and dynamic nature of evidence, particularly in local policy contexts. 33 Moreover, they advocate for rethinking policymaking to embrace complexity and uncertainty, fostering collaboration among diverse stakeholders. These arguments further underscore the value of including paramedics in policy discussions, as their experiences position them to contribute meaningful, context-sensitive insights.
Future directions
The addition of a Policy and Strategy pathway in the Career Framework for Paramedics in Canada creates opportunities for further advancements in paramedic leadership and influence within health policy. One key future direction is the establishment of Chief Paramedic Officer roles at provincial and federal levels, alongside CMOs and CNOs, akin to the structure of Safer Care Victoria. 79 These positions ensure paramedicine has a voice in high-level decision-making, enabling the profession to shape policies on healthcare quality, and system integration. The absence of a Chief Paramedic Officer means paramedicine remains underrepresented in strategic health governance, despite its expanding role in healthcare delivery. Establishing this role would provide dedicated leadership to advocate for paramedic-enabled models of care, and regulatory advancements, ensuring paramedics are integrated into broader system reforms rather than operating in the margins. While not all health professions necessarily require a similar role, the implications of excluding paramedicine from these leadership structures reinforce existing professional hierarchies and limit diverse perspectives in policymaking.
Policy enablement and involvement are critical to the continued growth and evolution of the paramedic profession. As our scope of practice expands and our roles increasingly intersect with complex health and social systems, a focused effort on policy development and advocacy is paramount. Nearly two decades ago, O’Meara (2006) emphasised the necessity of developing a sustainable academic workforce to support the profession's growth. 80 We now expand that call to action and urge the profession to meaningfully invest in developing a policy workforce from within.
Conclusion
The introduction of a Policy and Strategy career pathway in the Career Framework for Paramedics in Canada is not merely a milestone but a call to action for the profession to assert its role as a transformative force within healthcare systems. By equipping paramedics to engage in policymaking, we can not only address gaps in representation but also foster a culture of equity and sustainability in health governance. This pathway acknowledges the value of paramedic insights in addressing systemic challenges, from harm reduction to integrated care models, and positions the profession as an important system player in shaping the future of healthcare. However, for this vision to be fully realised, we must continue to advocate for research, mentorship and education that prepares paramedics to excel in these roles. By doing so, the paramedic profession can evolve its identity as architects of meaningful and lasting health system reform.
Footnotes
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Alan Batt (the second author) is the deputy editor with the Paramedicine journal.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
