Abstract
Paramedic preceptors play a critical role in supporting a learner's transition to practice. However, many paramedics have received limited training or education on how to be a preceptor. Providing access to a targeted preceptor education programme may further enhance paramedics’ capacity in this role. To help inform preceptor education, this research answers the question ‘What capabilities are required for the paramedic preceptor role?’ Capabilities are a combination of knowledge, skills and attributes used to work effectively and take appropriate action in various and novel settings. MEDLINE, CINAHL, ERIC, Web of Science and Scopus databases were searched using the Joanna Briggs Institute (JBI) methodology. Manual searches of Google Scholar, Trove and relevant paramedic-specific journals were also undertaken. Eligible for inclusion were peer-reviewed publications and grey literature from 2004 onwards written in English which discuss paramedic preceptor capabilities. Thirty-six articles were included in the review utilising this search strategy. Four overarching capabilities were identified for the paramedic preceptor role. First, the learning and teaching capability included having knowledge of feedback, assessment, adult learning theory and how to guide critical thinking and be a coach. Second, the interpersonal capability included having the skills to build positive relationships, act as a counsellor, provide psychological safety, communicate effectively and support socialisation. Third, the professional capability comprised of preceptors being clinically competent and critical thinkers. Finally, the personal capability included having the attributes of a role model and possessing an intrinsic desire to be a preceptor. Paramedics require opportunities to develop the knowledge, skills and attributes identified in this review to be capable preceptors. These findings can also inform the design of a paramedic preceptor education programme.
Introduction
Preceptors provide educational and developmental support to learners as they transition to a new role. Preceptorship is a formal arrangement between a health professional (the preceptor) and a learner (the preceptee) which involves the training and assessment of the learner within a clinical setting. 1 In paramedicine, preceptorship can occur with various learner groups, including but not limited to; student paramedics undertaking a bachelor's degree, graduate/interns beginning their employment, return-to-work and intensive care paramedics. 1 The multi-faceted role of the preceptor involves assessing, coaching, role modelling, socialising, protecting and teaching.1,2
Paramedicine uses the term preceptor in parts of Australia, the United States of America (USA) and Canada3–5 and is recommended as the most appropriate descriptor in the paramedic context. 1 However, clinical ‘mentor’, ‘supervisor’ and ‘instructor’ are other titles used to describe the role.1,6 Edwards 1 described the ‘mentor-mentee’ relationship between two paramedics as informal, non-time bound, not involving assessment, and the mentor is chosen by the mentee. 1 A ‘supervisor’ is more of a managerial title and less associated with education and an ‘instructor’ is a more formal, top-down authoritarian position for teaching specific skills as opposed to an individual who guides and supports learning. 1 For the purpose of this scoping review, the term ‘preceptor’ is used to describe the paramedic who works with a learner in clinical practice.
The important role preceptors play in ensuring learners are safe and competent in their clinical practice cannot be understated. Effective preceptorship not only benefits the learner but also the preceptor and the employer. First, the preceptor can experience a concept described as ‘rebound learning’7,8 where their knowledge base is solidified through interactions with the learner and acts as a motivator to continue developing their knowledge. 9 Preceptors also experience a sense of pride, satisfaction and status from undertaking the preceptor role.7,8 For learners, effective preceptorship experiences lead to improved socialisation and opportunities to apply their knowledge and skills in a ‘real-world’ setting.10,11 Finally, employers can protect themselves against high attrition by ensuring preceptorship is optimal within their organisation. 12
Developing educational opportunities for preceptors may help to ensure they can effectively perform the role. Preceptor education programmes are well-established in nursing, 13 pharmacy, 14 physiotherapy 15 and medicine. 16 Education programmes have resulted in significant benefits to the preceptor, which include increased self-efficacy, role preparedness, opportunities for reflective practice and collegiality with peers.13,15,17,18 Many health disciplines have a strong evidence base that underpins the development of their preceptor education programmes through research that explores the key skills and knowledge for their role.19–21 A similar approach in Paramedicine may yield the same benefits.
The paramedic role is unique to other health professions which warrants the need for a paramedic-specific preceptor education programme. Paramedics have distinctive characteristics including a broad scope of practice and the requirement to work autonomously in diverse, unpredictable and complex environments. 22 A paramedic's individuality is also seen through nonclinical tasks such as emergency driving, complex patient extrication, scene management and radio communications.8,23 Moreover, paramedics often work in pairs which is different from other health professionals who regularly have the support of larger, more qualified interprofessional teams.
Despite the complexities of the paramedic role, there is a gap in paramedic preceptor education. This gap has existed for some time even though it has been recommended an education programme be developed.1,5,8 ‘Preceptor preparedness’ was also recently highlighted as a paramedicine research priority area and provides further evidence of the gap in preceptor education. 24 Further research is needed to inform the development of a paramedic preceptor education programme to ensure paramedics’ specialty skills and unique environments are considered.
This review's objective was to identify the capabilities of paramedic preceptors. Capabilities must be described in the paramedic preceptor context given the unique role, environment and relationship in which preceptors work with their learners. The capabilities can also form a basis for preceptor education, help set expectations for the position and assist in identifying and selecting appropriate paramedics to become preceptors.
Method
This scoping review was conducted following the Joanna Briggs Institute (JBI) methodology and was reported using the Preferred Reporting Items for Systematic Reviews and Meta-Analysis Scoping Reviews extension (PRISMA-ScR).25,26 The JBI methodology evolved from the original works of Arksey and O’Malley 27 and was later refined by Lavac et al. 28 The methodology incorporates nine steps, and to date, ensures the most rigorous and advanced approach to undertaking scoping reviews. 29 This review followed additional guidance for paramedicine researchers to enhance rigour in the review 30 and was also conducted per a priori protocol (https://osf.io/yz2tg). A scoping review was chosen as the methodology explores research gaps by mapping the existing literature, 31 which enabled the review to identify key components of the paramedic preceptor role. Scoping reviews also allow for the incorporation of grey literature in the findings of the systematic search. 29 Searches of MEDLINE, PROSPERO, the Cochrane Database of Systematic Reviews and JBI Evidence Synthesis were initially conducted. No current or underway systematic or scoping reviews were found on this topic.
Review question
‘What capabilities are required for the paramedic preceptor role?’
Inclusion criteria
Population
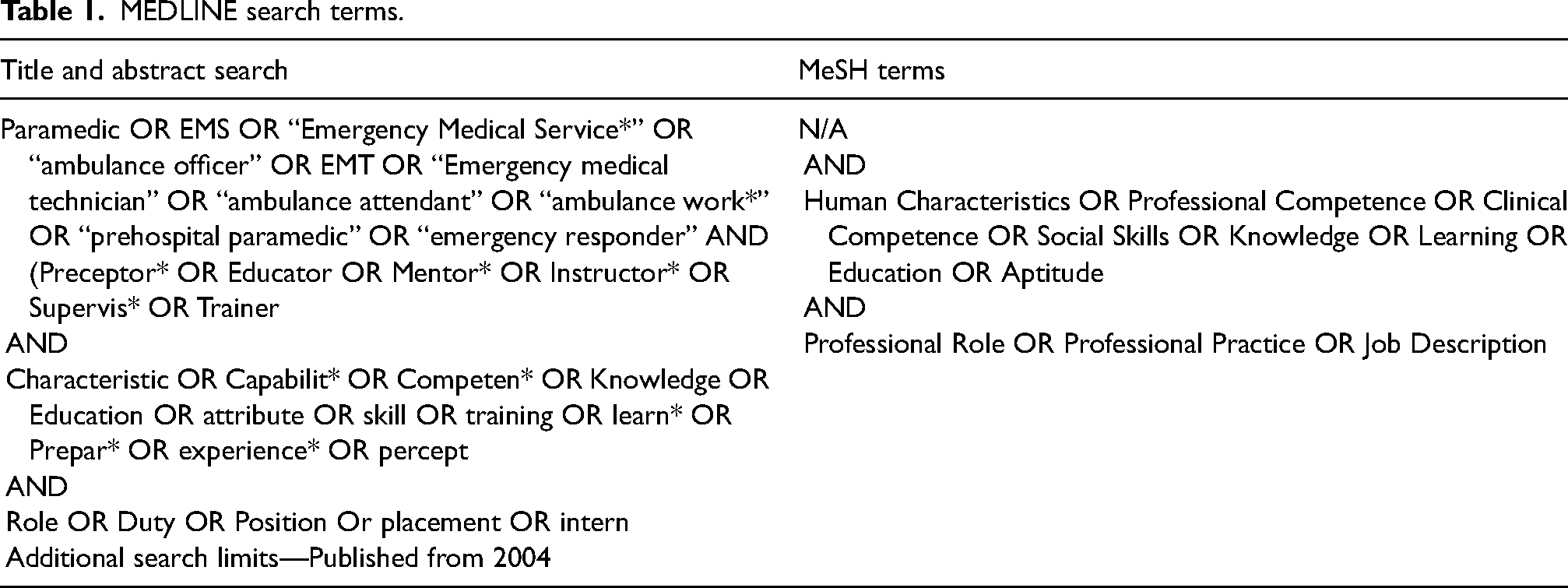
Paramedic preceptors to all learner groups were the population in this review. The various other terms used in literature to describe paramedics (e.g., Emergency Medical Services) and preceptors (e.g., mentors) and were incorporated into the search (Table 1).
MEDLINE search terms.
Concept
Capability was the concept explored in this review. Capabilities are the knowledge, skills and attributes required to work effectively with others, problem solve and take the correct action in known, unknown and evolving situations.32,33 Descriptors commonly used in the definition of capabilities and similar terms such as competency are examples of additional search terms used.
Context
The role of the paramedic preceptor over the past 20 years was the context for the scoping review. The preceptor role is most associated with student paramedics on clinical placements or graduate paramedics in their internship period. These are examples of other search terms used to help capture the literature.
Types of sources
This review considered literature originating from Australia, New Zealand, the United Kingdom (UK), Canada, the Republic of Ireland, the USA, South Africa and most of the Middle East. These countries formed the eligibility criteria due to the likelihood of having more well-established prehospital care pathways where paramedics have the largest scope of practice.34,35 All types of study designs were considered. Manuscripts written in English were part of the inclusion criteria to ensure accuracy and ease of interpretation. All forms of peer-reviewed literature were considered. Grey literature, such as published and publicly available handbooks, training courses, opinion papers and unpublished articles were also considered.
Eligibility criteria
Literature from the past 20 years was eligible for this review. In 2004, the Council of Ambulance Authorities (CAA) undertook the first external accreditation of undergraduate paramedicine degrees in Australia, changing the educational landscape of paramedicine. 36 This also meant preceptor expectations, skills and knowledge have evolved. Therefore, studies older than 20 years and from other health disciplines were excluded from this review. Table 1 outlines the MEDLINE search terms used.
Search strategy
A three-stage process was initiated to locate the literature described above. 29 Initial searches were undertaken on MEDLINE and CINAHL. Titles and abstracts that contained the text words and the associated MeSH terms and Subject Headings were used to inform the full search strategy. Then, ERIC, Web of Science and Scopus and manual searches of Google Scholar, Trove and relevant paramedic-specific journals were undertaken. Due to the limited advanced search functions on some platforms, a targeted search strategy was utilised. The intention was to screen the first 100 results of each journal. Grey literature was identified through Google Scholar and Trove. These searches were conducted in July 2023 and are outlined in the Appendix. The search strategy was developed in collaboration with a librarian to improve its quality. The collaborative process involved the development of an initial search strategy which was then modified based on the librarian's peer review. The librarian then assisted with undertaking the search in one-on-one consultations. The final stage involved reviewing the reference lists of all the studies initially included in this review to see if any other publications met the inclusion criteria. The MEDLINE search terms are provided in Table 1.
Study selection
All identified citations were uploaded to Endnote V.21 (Clarivate Analytics, USA) where duplicates were removed. The remaining citations were then uploaded to Covidence systematic review software (Veritas Health Innovation, Melbourne, Australia) and any further duplicates were removed. Three authors independently screened titles and abstracts to identify literature that met the inclusion criteria. AV screened all articles whilst EJ and SD screened half each. Any disputes were resolved from a third screening. Full texts of the eligible literature were then uploaded to Covidence and assessed in detail against the inclusion criteria independently by two reviewers with disagreements resolved through discussion or by a third reviewer. The PRISMA flow diagram (Figure 1) describes why some articles were excluded at this stage.
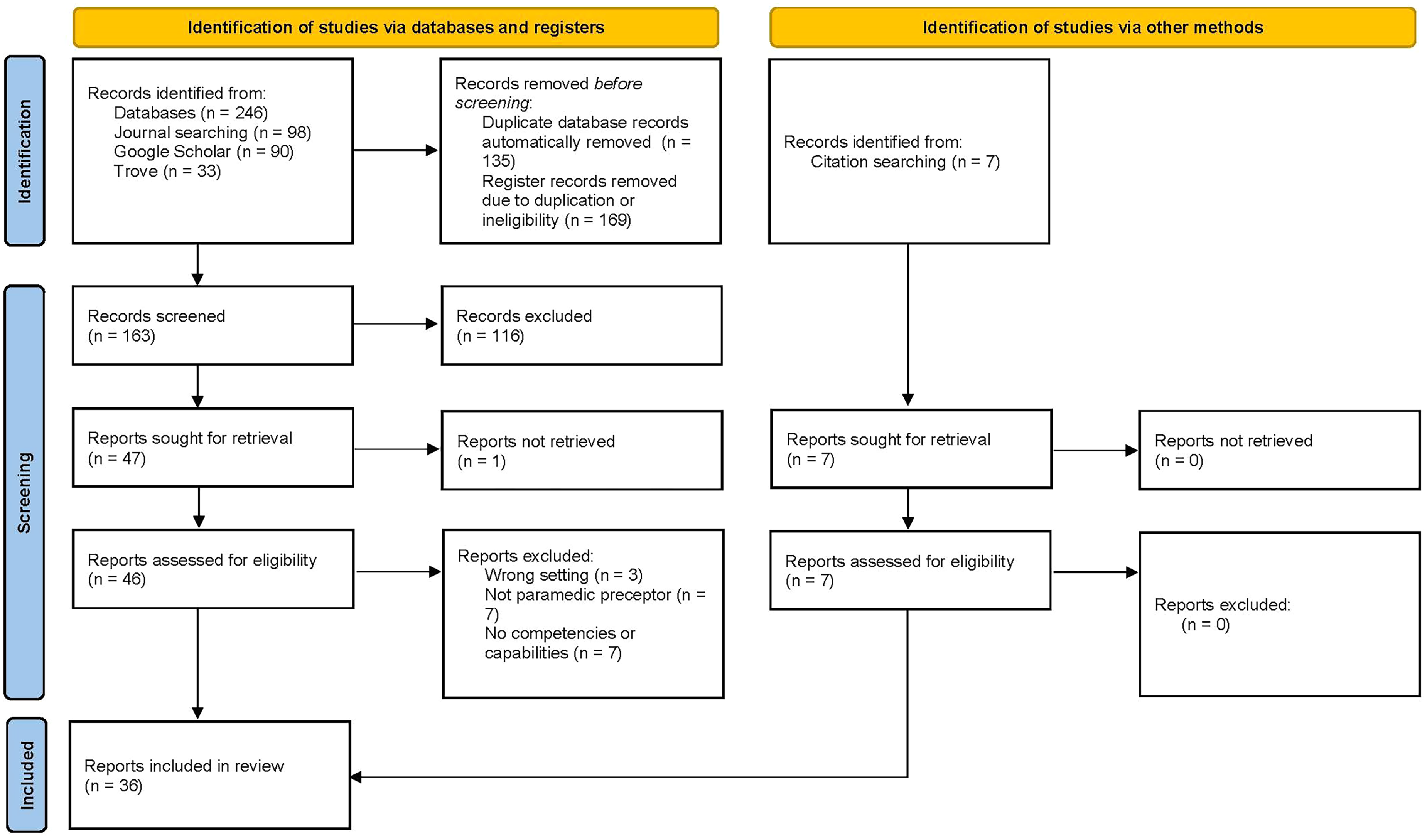
PRISMA flow diagram.
Deviation from the protocol
The final manuscript deviated from the priori protocol by:
Simplifying the manuscript's title to align with a new research question. Changes to the manuscript's keywords to align better with the research topic. ‘Competency’ as a focus was removed to improve clarity. Capabilities is a broader term and is more appropriate given they encompass individual competencies.
Data extraction
The data extraction tool was developed based on the example provided by Pollock et al. 29 The extraction tool was piloted with an article that has previously explored paramedic preceptorship before formal data collection. 2 Data from the included articles were independently extracted by three reviewers using Covidence. AV extracted data for each article whilst EJ and SD extracted data from half each. Any disagreements that arose between reviewers were resolved through discussion.
Data analysis and presentation
A content analysis method developed by Jacob et al. 37 was used to analyse the data. The method involved various paramedic preceptor skills, knowledge and attributes being uploaded to an Excel spreadsheet by AV. They were then mapped and descriptors with the same or similar meaning then grouped. For example, preceptors described as motivated, enthusiastic and dedicated were grouped into the concept of ‘intrinsic desire’. Authors EJ and SD independently cross-checked the spreadsheet to ensure accuracy and rigour. A meeting was held between all authors to discuss any disagreements. Frequency counting then identified the most discussed concepts to provide clear examples of the capabilities.
Results
Study inclusion
A total of 467 articles were identified through the initial search. Following the removal of duplicates, 167 citations were added to Covidence for title and abstract screening. Following full text screening 29 articles were included. Reference searching of the included articles identified another 7 articles, leading to 36 in this review. Figure 1 represents the PRISMA flow diagram.
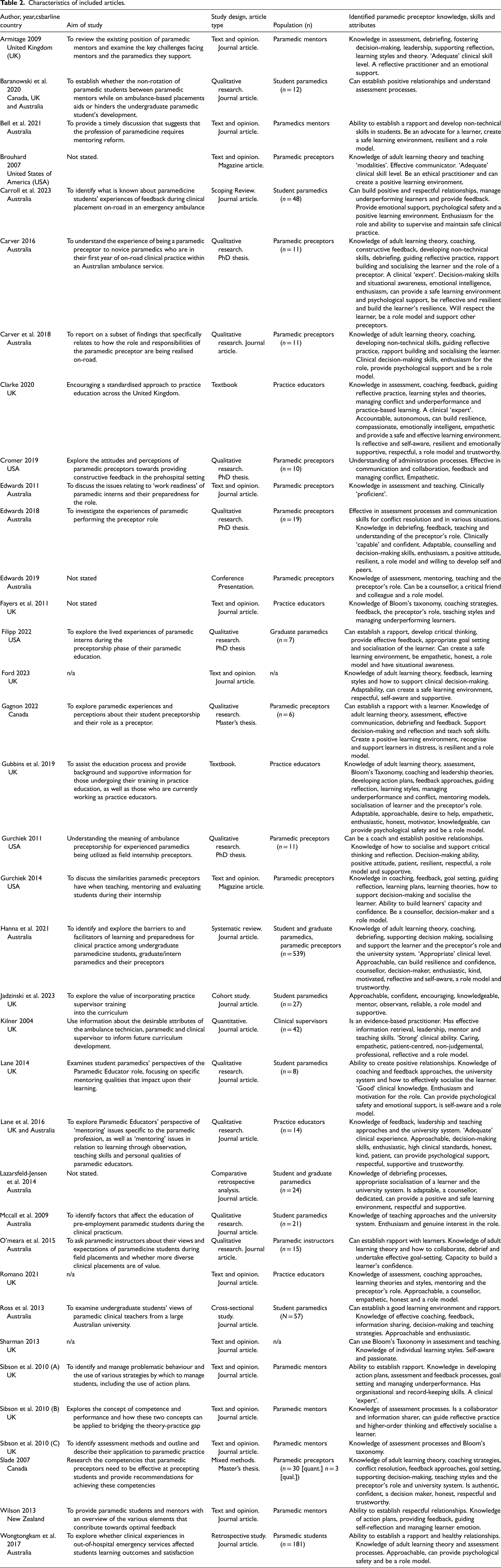
Most articles were written in Australia (n = 13) or the UK (n = 13). Opinion pieces (n = 13) and qualitative studies (n = 12) were the most common article type. The characteristics of all articles, including the identified paramedic preceptor knowledge, skills and attributes, are displayed in Table 2.
Characteristics of included articles.
Paramedic preceptor capabilities
Capabilities are the skills, knowledge and attributes used in combination to effectively work with others and take appropriate action in known, unknown and evolving situations.32,33 Four capabilities required for the paramedic preceptor role were identified in the review (Table 3).
Paramedic preceptor capabilities.
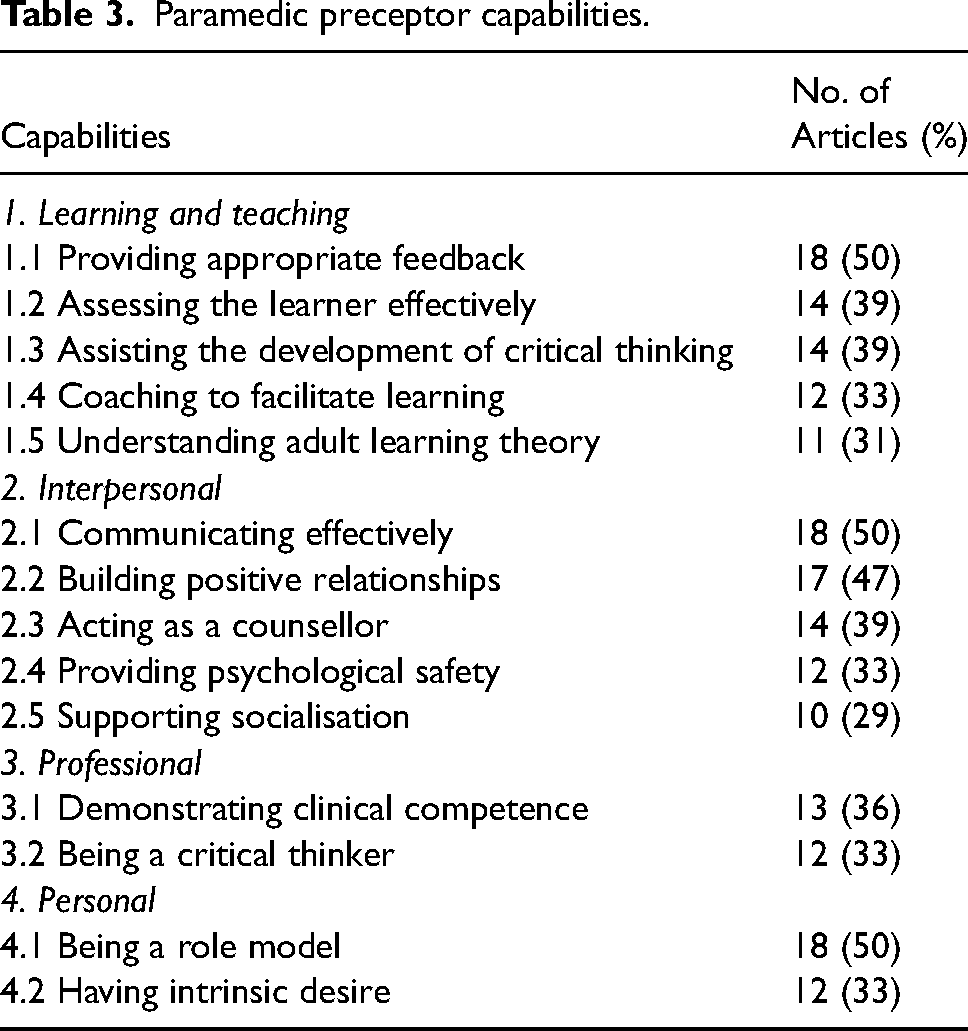

The four overarching capabilities of the paramedic preceptor role were: (1) learning and teaching, (2) interpersonal, (3) professional and (4) personal. A descriptive analysis of the paramedic preceptor capabilities is provided below.
Learning and teaching
This capability comprised the theories, processes and strategies used to facilitate learning. Knowledge of learning and teaching practices included five components: providing appropriate feedback, assessing the learner effectively, assisting the development of critical thinking, coaching to facilitate learning and understanding adult learning theory.
Providing appropriate feedback
The need for preceptors to provide feedback was outlined in 50% of the articles (n = 18).1,3,4,8,10,38–50 Feedback refers to the processes involved in informing the student about their performance. Feedback is essential as it facilitates the growth and development of the learner. 39 Constructive and effective feedback were the types of feedback most described.38,41,44,46 Additionally, being open, honest and objective were discussed as key elements of feedback.10,42,47,49 Preceptors need an understanding of feedback processes10,44,45 and to be mindful of a learner's emotional response after receiving feedback. 44
Assessing the learner effectively
The importance of a preceptor's ability to assess a learner was discussed in 14 articles.1,3,5,38,40,50–58 Effective assessment encompasses a fair and robust evaluation of a learner's competency. A preceptor must be able to assess the level of competence and identify underperformance.38,40 Preceptors should be proficient in assessing learners’ competence in scene safety, patient assessment, skill application and clinical handover. 58 Furthermore, understanding assessment processes and using a framework such as Bloom's Taxonomy to design appropriate assessments was seen as important.50,55,57 Three articles commented on the specific types of assessments that can be undertaken.40,52,55
Assisting the development of critical thinking
The concept of preceptors assisting in developing critical thinking was discussed in 14 (n = 14) articles.2–4,7,8,39,40,43,45,49–51,55,59 Critical thinking is a higher-order cognitive process allowing learners to analyse and improve their clinical ability. Developing critical thinking was suggested to be the most important role of a preceptor. 55 Preceptors can also support and guide reflective practice which can lead to the learners’ cognitive growth and improved performance.8,39,43
Coaching to facilitate learning
Coaching (n = 12) was the most described approach to facilitate learning.2,7,8,10,40,43,45,47,48,50,56,59 Coaching differs from a typical top-down teaching method and is an approach whereby improved performance comes from a preceptor appropriately guiding and navigating an individual through their learning journey. Coaching models, theories and approaches were seen as the most appropriate teaching method in preceptorship as a coach is more of a facilitator who provides support and advice to the learner.2,8,47,59 Coaching has other advantages for learners who are transition to practice such as; coaching is easily tailored to individual learning needs, 8 can be used in challenging clinical cases, and most effectively develops critical thinking.7,8,10,43
Understanding adult learning theory
Knowledge of adult learning theory is essential for preceptors. Elements of adult learning theory were discussed in 11 articles.2,3,8,43,45,49,50,58–61 Adult learning theory specifically aims to improve the learning experience for adults. Preceptors must have an understanding or familiarity with adult learning principles,3,45 respect the range of knowledge and experience adults bring into the role8,49 and understand what motivates adults to learn. 58
Interpersonal
This capability captures the interpersonal skills necessary to support a learner's well-being, development and transition into practice. Interpersonal skills that emerged from this capability were: communicating effectively, building positive relationships, acting as a counsellor, providing a psychological safe learning environment and supporting socialisation.
Communicating effectively
Communication is an essential skill for preceptors and was discussed in half the articles (n = 18).1–3,8,12,38,40,41,44,45,47,48,50,51,55,59–61 Communication skills are needed in various situations including having difficult conversations, handling conflict and managing underperforming learners.1,38,41,44,45,50 Preceptors also require communication skills to share information, provide feedback3,47,60 and work effectively in high-stress environments and hierarchical relationships. 1 Communication skills are also needed to debrief critical incidents.3,12,61
Building positive relationships
Building positive relationships was outlined in 17 articles (n = 17) and describes the importance of establishing a rapport and a connection with the learner.1–4,7,8,10,38,39,41–43,47,50,54,58,59,61 Positive relationships influence the learning experience and allow preceptees to make the most of their educational opportunities.10,39,42
Acting as a counsellor
Preceptors need the skills to be able to act as a counsellor. This includes having empathy and the emotional intelligence to provide psychological and emotional support to a learner and build their resilience. This was discussed in 39% (n = 14) of articles.1–3,8,12,39–41,43,46,53,55,56,59 Six (n = 6) articles specifically highlighted that preceptors must have the capability to recognise a learner showing signs of psychological distress, provide appropriate support and understand when to escalate care.2,3,8,40,46,59
Providing psychological safety
One-third of articles (n = 12) discussed that preceptors must be able to provide a psychologically safe learning environment.3,4,8,10,12,40–42,49,50,58,60 Psychological safety is a safe and supportive learning environment, free from any power imbalance or intimidation. Wongtonkam and Brewster 58 suggest psychological safety is required for effective learning to occur. Elements of psychological safety included learners feeling comfortable to ask questions or make mistakes without being heavily criticised.4,10,49 Additionally, a preceptor must advocate for their learner42,60 and can create a safe learning environment by being approachable and supporting the learner to discuss and reflect on the challenges they face in the workplace.
Supporting socialisation
Preceptors must have the skills and knowledge to support the socialisation of a learner in the workplace. This was discussed in 10 articles.2,4,7,8,10,12,43,50,51,59 Supporting socialisation refers to the preceptors assisting a learner's transition to their role. Socialisation elements included introducing them to workplace culture, colleagues and operational and non-operational idiosyncrasies of the workplace.
Professional
Professional capabilities are the clinical and cognitive skills required to maximise the learning opportunities for the preceptee. The preceptor demonstrating clinical competence and being a critical thinker are the key components of this capability.
Demonstrating clinical competence
Clinical competence was an identified professional skill for the preceptor role. Thirteen (n = 13) articles discussed the importance of a high level of clinical skill and knowledge required by the preceptor.1,5,8,38,40,45,46,50,55,59,60,62,63 It was outlined that a paramedic needs to be ‘confident’, 59 ‘capable’, 1 ‘expert’, 38 ‘adequate’, 46 ‘proficient’ 5 and ‘strong’ 50 in their clinical ability to be a preceptor.
Being a critical thinker
Preceptors must also be critical thinkers as outlined by 33% (n = 12) articles.1,2,4,7,8,40,43,45,46,55,59,63 Preceptors being critical thinkers refers to their ability to evaluate and analyse situations to maintain effective operations, learner development and the safety of their learner and patient. This includes understanding when to ‘step back’ to allow an educational opportunity or ‘step in’ and protect the patient.7,46 The safety of the learner can be enhanced through scene management and situational awareness, both of which require critical thinking skills. 8 Five articles (n = 5) also discussed the need for preceptors to be reflective and learn from their own experiences.8,40,55,59,63 Finally, preceptors with strong decision-making skills provide greater learning opportunities. 1
Personal
The personal capabilities are the attributes preceptors need to motivate a preceptee to succeed in their learning and professional development. This included being a role model and having intrinsic desire for the role.
Being a role model
The preceptor as a role model was described in 50% of articles (n = 18).1–4,7,8,10,40,42,43,50,53,55,56,58,59,62,63 Role modelling occurs when preceptors demonstrate interpersonal interactions,2,8 patient empathy, 8 ethical practice, 60 undertaking professional development opportunities, 55 and appropriate emotional responses. 59 Seven articles (n = 7) specifically outlined that preceptors should also role model professional behaviour, clinical skills and attitudes.2–4,8,10,40,59
Having intrinsic desire
Having the intrinsic desire to undertake the preceptor role was identified in 12 articles (n = 12).1,2,8,10,12,41,46,47,50,57,59,64 Intrinsic desire means a genuine interest in working with a learner and being invested in their development. Preceptors with intrinsic desire actively look for and initiate learning opportunities. 8 Enthusiasm was most frequently described as demonstrating intrinsic desire.10,46,47,57,64 Other terms were motivated 1 and dedicated. 12
Discussion
This scoping review identified the capabilities for the role of paramedic preceptor. Embedded within the capabilities are the knowledge, skills and attributes required for a preceptor to perform their role effectively.
Knowledge of learning and teaching appeared to be a crucial element the paramedic preceptor role. Providing feedback, assessing effectively, supporting critical thinking, using coaching strategies and applying adult learning theory were the specific areas of knowledge required for paramedic preceptors. Learning and teaching activities have been described as competencies for other health discipline preceptors. Ryan et al. 65 outlined the same knowledge of learning and teaching as competencies for nursing preceptors. Similarly providing feedback, undertaking assessment and facilitating critical thinking were competencies for preceptors in other health disciplines.66,67 Therefore, this finding is unsurprising in the paramedic context given the educative role preceptors play.
Possessing interpersonal skills to form positive relationships, effectively communicate and support preceptee socialisation are also key components of the paramedic preceptor role. These interpersonal skills are relevant in the context of learning and needed as paramedic workplace socialisation is a challenging experience for many. 23 A preceptee's socialisation in the workplace is heavily influenced by their preceptor given they help the preceptee to ‘fit in’ and develop their skills. 23 However, power imbalances also exist within the preceptor–preceptee relationship potentially impacting the learning experience and causing stress and anxiety for the preceptee. 68 Therefore, preceptors establishing a positive relationship with their preceptees is critical to their socialisation and will create an effective and safe learning environment.10,39 Communication is also a critical element of preceptorship. Preceptors must be effective communicators to debrief, provide feedback, have difficult conversations, and manage conflict and underperforming.8,40,59 Preceptors being honest and respectful during communication with their preceptee may help promote a positive relationship.7,46
This review highlighted the emotional and psychological well-being of learners must be a significant consideration for preceptors. Preceptors can support their learner's well-being by providing a psychologically safe learning environment and acting as counsellors. 69 Psychological safety allows the learner to feel comfortable, protected and supported 7 and is needed to encourage the reporting of clinical errors and promote a culture of patient safety. Creating a psychologically safe environment is the responsibility of all paramedics, however, as a role model to their learner, preceptors can be ‘champions’ in this area and drive a cultural change where mistakes are learnt from and not heavily criticised. Unfortunately, some learners in paramedicine do not have this experience, with research outlining occurrences of hazing, stigmatisation and bullying in paramedic practice,12,23 potentially indicating a poor underlying culture and motivation towards preceptorship.
‘Acting as a counsellor’ is a finding unique to paramedic preceptors and not mentioned in preceptor literature from other health disciplines.65–67 Exposure to many critical and traumatic events provides the rationale for this finding. As preceptorship in paramedicine is a one-on-one relationship, the preceptor must be able to support a learner in emotional or psychological distress.
Findings from this review indicate that the more clinically competent the preceptor, the greater the learning opportunities. This is due to the preceptor having more knowledge and clinical experience to share and greater confidence to ‘step back’ and allow the learner to provide patient care. 7 Clinical competence in preceptors is also highlighted in nursing and pharmacy literature.21,67 What ‘clinical competence’ in paramedicine looks like is challenging to quantify, but clearly, a level of clinical experience is beneficial. Benner's 70 Novice to expert theory states clinical competence typically develops after 2–3 years of clinical experience. This would suggest that paramedics should have at least 1–2 years of clinical experience as a fully qualified paramedic as a minimum requirement.
Linked with clinical competence is being a critical thinker. Having a preceptor with robust critical thinking, including advanced skill in clinical decision-making, reflection and situational awareness, may allow their preceptee to have increased learning opportunities.4,59 Learners require exposure to a range of clinical patient presentations to help close the theory-practice gap, so a preceptor being a critical thinker is highly beneficial to learning. 40
The need for paramedic preceptors to be role models was the first personal capability identified. The experience, knowledge and position preceptors hold leads to many being revered and highly respected by learners. 3 Preceptors play a significant role in a learner's development and therefore need to understand how broad their influence is and the lasting impact their actions can have. 2 The importance of being a role model is not unique to paramedicine, with many studies from other health disciplines showing the importance of preceptors acting as role models.65–67
Posessing the intrinsic desire to be a preceptor is a key attribute for paramedics to have. Individuals have intrinsic motivation toward an activity when they experience enjoyment and satisfaction. 71 This review uncovered that enthusiastic and dedicated preceptors are most effective in the role.3,10 Interestingly, the development of intrinsic desire may come from providing a preceptor education program. This appearred to be the case for nurses who experienced improved commitment, attitude and satisfaction toward the preceptor role after completing an education programme. 17
The capabilities of paramedic preceptors identified in this review are complex combinations of knowledge, skills and personal attributes. Many of the discussed preceptor skills and knowledge are not taught through undergraduate programmes which primarily focusing on anatomy, physiology and medical procedures. 72 Therefore, findings from this review support Edwards 1 who outlined that being a clinical paramedic and a preceptor are separate roles with two sets of capabilities. Given the different capabilities, it is questionable for preceptor education to sit within undergraduate programmes. Whilst accreditation standards may require undergraduate programmes to include preceptorship in their curriculum, 73 it is unknown how thoroughly preceptorship topics are taught or engaged with by students.
This review confirms a gap in paramedic preceptor education and highlights that many paramedics do not inherently possess the knowledge or skills required to be a preceptor. Education programmes are being developed for nursing and pharmacy preceptors based on their essential skills.19,20 This review takes the initial steps in paramedicine by identifying paramedic preceptor capabilities.
Limitations
This review has limitations. While other articles or grey literature may exist discussing preceptor capabilities, these were not found in our robust search strategy and thus were not included in this review. As an example, non-English language literature may discuss preceptor capabilities but were not included. Another limitation was the use of frequency counting. Frequency counting identified the knowledge, skills and attributes most common in the literature to give a concrete example of the capabilities. Frequency counting was used with the view that the most common concepts appearing in the literature were the most important to the preceptor role, however, this may not necessarily be the case. Other individual knowledge, skills and attributes contribute to the preceptor capabilities but were not discussed as frequently in the literature.
Conclusion
This scoping review identified the capabilities required for the paramedic preceptor role. The findings can inform the development of an education programme tailored to paramedic preceptors’ educational needs. Moreover, the findings can help to assess a preceptor's ability to perform the role and select and identify appropriate preceptors. This review also recommends clinically competent preceptors. This could be achieved by mandating a minimum timeframe of clinical experience before undertaking the preceptor role. Finally, further research needs to identify which capabilities are the most important to learn for each type of paramedic learner group (i.e., student and graduate paramedics). Further research is also required into the culture and motivations of paramedics toward preceptorship and preceptor training.
Supplemental Material
sj-docx-1-pam-10.1177_27536386241305157 - Supplemental material for Capabilities for the paramedic preceptor role: A scoping review
Supplemental material, sj-docx-1-pam-10.1177_27536386241305157 for Capabilities for the paramedic preceptor role: A scoping review by Andrew Van Noordenburg, Elisabeth Jacob and Scott Devenish in Paramedicine
Footnotes
Acknowledgments
We would like to acknowledge Meena Gupta, Librarian at Australian Catholic University, for their support and help with developing the search strategy and database searching.
Author contributions
All authors contributed to the design, acquisition, analysis and interpretation of data for the work. AV drafted the work and EJ and SD provided critical review. All authors approve the final version to be published and agree to be accountable for all aspects of the work.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: SD is an associate editor of Paramedicine but played no role in the editorial process which was conducted as per the journal’s double-blind peer review policy.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
Appendix: Search Strategy
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
