Abstract
Paramedicine is increasingly complex in affective, behavioural, and cognitive domains of practice. The ability to navigate this complexity is essential for paramedics who are required to simultaneously practice assertively, dynamically, sensitively, and professionally. Although these may seem to be superficially incongruent ways of practising, through insightful and reflexive practice underpinned by appropriate ethical approaches, paramedics can navigate the complexity inherent in paramedic work whether care episodes are routine or extreme. In what follows, we discuss the potential of virtue ethics as a way of navigating complexity in paramedic practice and preparing clinicians for the varied work they manage as paramedics. We do this by first describing some of the issues faced by the modern paramedic, outlining ethical approaches to practice, then working through a vignette showing how a deeper understanding of ethics and utilising a virtue ethics approach may have helped the clinicians navigate a typical ethical dilemma found in practice.
Introduction
The paramedic is a clinician who finds themselves working autonomously from an incredibly early stage in their career, managing undifferentiated patients in dynamic environments through unscheduled care episodes. Paramedics with little autonomous practical experience, as well as paramedics with decades of clinical experience, are equally expected to make complex decisions with little oversight. Paramedics will use different ethical approaches, either knowingly or unknowingly to navigate this complexity in practice, but also in everyday situations.
Navigating complexity, including complex ethical dilemmas, is a common feature of the paramedic role and is integral to the development of paramedic professional identity and philosophy of practice. 1 Eaton notes that paramedic students may be particularly vulnerable to acquiring maladaptive moral behaviours in the process of becoming paramedics as they tend to ‘emulate their practice educators’ values’ uncritically rather than reflect on, and subsequently integrate, their practice experiences with their own ethical framework1,2(p46). Students construct their ethical approach to practice in an intersubjective manner, in that their ethics are negotiated through the contextualisation of education and practice experiences. As such, university educators are increasingly aware of the need to bring students and clinicians into a way of thinking which includes signposting to the established frameworks for ethical practice that already exist, and also providing alternative ways of conceptualising and navigating the ethical issues that they encounter in routine and extreme aspects of practice. Through the introduction of more sophisticated ethical tools, better suited to the nature of paramedic work, the above-mentioned experiences may serve as unique opportunities to shape the moral character of paramedics and paramedic students regardless of their level of seniority.
In this paper, we offer a discussion of ethical approaches to practice and decision-making, introduce virtue ethics (VE) as an approach to navigating practice, and provide a case study example and discussion of the potential benefits of VE. In doing so, we provide a platform for consideration of VE as an approach to paramedic education and practice, insight into the future development of VE as an underpinning ethical approach, and ask the question ‘is there a better way’?
Background and context
Ethics in practice
Ethical principles in practice
Paramedics encounter situations rich with potential ethical dilemmas daily – through obvious ethical issues (e.g. the refusal of treatment from the patient with fluctuating capacity), or more frequently through everyday ethics (e.g. communicating with a diverse range of people, or the extent to which we engage with, or how we feel about, crew-room dialogue). These everyday ethical situations that paramedics need to navigate may not be reflected in the ethics education for undergraduate paramedics. However, they are being navigated in some way, paramedics may use deontological approaches or something similar to a VE framework but without being cognisant that they are using these tools.
Globally, programmes of paramedic education and training are grounded in the documents that outline the standards of conduct, performance and ethics (UK), codes of conduct (Australia), and codes of ethics (Canada) that underpin paramedic practice and education.3–5 These documents provide frameworks for paramedic practice that are deontological, in that they clearly articulate a right way of practising. While the principles outlined in these documents are clear, a decalogue-style list of ethical commandments, although appropriate in certain situations, is insufficient to adequately capture the nuance and complexity of what paramedics do in the enactment of these values. 6 Nor do they discern the specific nature of the challenges faced by paramedics in their work 1 as these ethical standards are often shared with myriad professions from Chiropractors (Australia) to Speech and Language Therapists (United Kingdom). Furthermore, such commandment-style frameworks fail to provide a sufficiently reliable moral compass that serves paramedics at the point of care, and as such may not be sufficient to prevent breaches of professional expectations.
The context of increasing expectations placed on paramedics coupled with a disproportionate (and staggeringly high) referral rate to the UK professional regulator of paramedics, 7 the health and care professions council, for fitness to practise predominantly for issues of conduct, performance, and ethics rather than matters of competence, indicates there is a gap in the literature and an opportunity to provide paramedics with a philosophical approach to their practice which centres moral virtue.
Theory praxis gap
Contemporary paramedic praxis in terms of both clinical and educational domains remains geared towards ambulance work despite paramedic practice encompassing an increasingly diverse range of clinical environments. The moral and ethical principles that underpin paramedic practice transcend the setting in which paramedicine is practised. The word setting in this sense may refer to paramedics who practice in a wide variety of different healthcare settings but can also be seen to represent the heterogeneity of environmental, circumstantial, or psychosocial domains in which ambulance work is done.
Ethics for navigating practice – complexity and everyday ethics
Navigating complexity is an essential trait for paramedics who are required to practise in assertive, dynamic, sensitive, and professional ways simultaneously. Although these may seem to be superficially incongruent ways of practising, through insightful and reflexive practice underpinned by appropriate ethical approaches, paramedics can navigate the complexity inherent in their work whether care episodes are routine or extreme.
The paramedic profession has complexity at its very core in that the nature of practice/praxis and the challenges paramedics must navigate are diverse, connected, interdependent, and dynamic in which there is seldom a ‘right’ answer and often non-linear responses to intervention. Due to the nature of this complexity, deontological or consequentialist ethical theory, although helpful, do not suffice to truly guide the paramedic through the range of moral dilemmas they are likely to encounter. The navigational aids of everyday ethics may be considered to be incomplete without an approach which centres moral virtue.
As educators, our ability to convey the benefits of a set of physical, psychological, and philosophical equipment of everyday coping, of which ethics forms a significant part, is paramount to preparing students for the reality of practice.
Ethical approaches
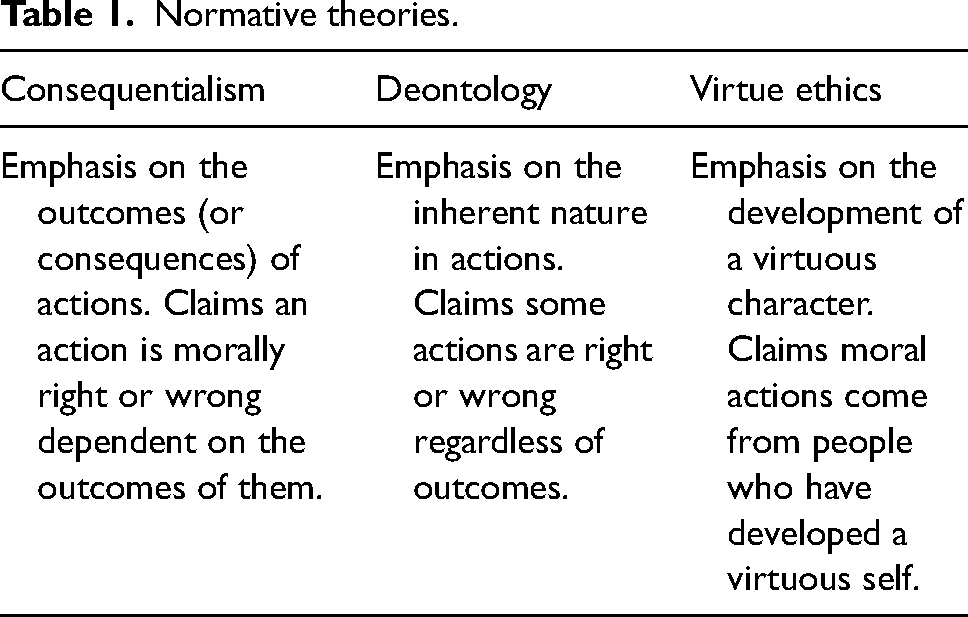
Table 1 shows a very brief overview of the three normative approaches towards ethics in philosophy and outlines their fundamental underpinning principles. 8 It is beyond the scope of this paper to delineate the principles of each of these approaches.
Normative theories.
In this paper, we present the way in which VE applies to paramedic practice. Of course, this case could be analysed through a number of different and potentially competing ethical frameworks. While we believe that the virtue ethical framing is superior in certain respects to its rivals when it comes to articulating the specific moral challenges presented in the case, our intention in this paper is simply to demonstrate the utility of a virtue ethical lens rather than to argue that it is the only way to approach scenarios such as this. This paper would risk either failing to do adequate justice to alternative ethical approaches, or become too long to be engaging for our audience where we to detail the following case through differing lenses.
Virtue ethics
VE is one of the three main theories in normative philosophy, and although it has been widely discussed in medicine and nursing, it is often overlooked, and rarely applied to understanding issues facing paramedics. The nature of austere, novel, and complex settings in which paramedics practise may benefit from an approach to decision-making that centres values rather than a mantra or rule book approach. 8 VE, as an approach to practice, may be relatively straightforward to understand but also may be equally difficult to deploy compared with conventional deontological or consequentialist approaches.
The essence of VE is understanding how one should strive to be, rather than identifying universal principles, rules, or consequences to be applied in any moral situation. It is therefore not a problem-solving tool, although arguably what is not needed for managing complexity in ethical issues is providing the right answer. In medical practice, algorithmic and yes/no decision-making, or utilisation of a checklist reduces clinical complexity. However, ethics, even everyday ethics, is unlikely to be reducible to a checklist. Rather, it is important that clinicians have a strong working knowledge of ethical theory they can apply (phronesis), in-depth practical wisdom of the clinical work they manage, and have developed moral character as such that they do right for their patients. This is VE in practice.
The strength of VE lies in navigating all matters of life and complexity. The following case (Table 2) and its discussion in the context of VE is intended to reflect a common situation in which paramedics need to exercise their capacity to navigate complex ethical situations.
Case study.

Discussion
Virtue ethics in the context of the case study
This is a difficult, but not uncommon case for paramedics to encounter. The glaring question here appears to be for the paramedics – is it right for them to non-convey a patient who lacks capacity, but has not pre-recorded their wishes, when by doing so that patient's life will likely be shortened?
A question no doubt on the mind of every clinician reading this will likely go something along the line of ‘what is our legal responsibility?’, and the related yet distinct ‘what will our employer/regulator think?’. In the interests of ensuring this paper can be read and understood wherever paramedics are encountering scenarios such as this, these points cannot be addressed in detail as the nuance of both the law, regulators, and employers differ across the world. However, it is worth noting the importance of working within local protocol/law, as Huxtable pragmatically suggests ‘Failure to heed the guidance (in-deed, edicts) of the law or the regulator would not be prudent, since this may lead to loss of liberty or livelihood. The same might be said of guidance that is issued by employers’. 9 (p3) That said, there is often a large amount of grey area in these cases and with local rules, and even where there is not, we have both a professional and moral duty to consider the ethics of our actions, and to perhaps advocate for change when we see our practice unrightfully constrained.
So, what is the correct thing to do in this case? An ardent follower of Beauchamp and Childress's four principles would likely tell you that primarily we must respect the patient's autonomy.10,11 But that is of questionable use when considering our patient who lacks the capacity to make decisions for herself and has not recorded these decisions when still maintaining capacity. It is generally held that in these cases by speaking to her loved-ones we gain insight into her as a person and what she would want and with this information we can make a decision that is respects her autonomy (as far as possible).8,10 However, these best interests decisions are not that straightforward, and there are a multitude of reasons why they can be questionably truly representative of the patient's wishes.8,12
These decisions and this process are truly fallible. There are multiple people involved between the clinicians (in this case the ambulance crew on scene and the family physician the case is discussed with) and the patient's loved-ones, and the information we are dealing with is second-hand. To understand why this makes these decisions fallible, it is useful to borrow from social sciences. As an example, individuals utilising a constructivist grounded theory approach recognise that research data derived through interviews is not objective, but rather coloured by the complex world in which we live, and our own perspectives and influence on those we are speaking to. 13 These shared best interest decisions fit that paradigm excellently. Humans have complex lives and experiences, and for many people one's family will only see a part of this. The family members perception of the patient's character and wishes is influenced by their own complex lives, moral biases, and the relationship they have with the patient. The clinicians themselves then also interpret this ‘data’ with their own experiences and (conscious or not) moral biases. Once this data is affected by so many influences it is at best a triangle shape being pushed through a square hole – they fit but are not a true representation. However, it is important to remember that although the act of making a best interests decision is, at its core, imperfect, that is not to say the decision made is the wrong one.
These best interests cases rely not just on an attempted understanding of the patient's true wishes, but also on an accurate prognostication of their condition. We know that in the out-of-hospital environment prognostication can be a very difficult task. 14 However, in this case it is rather straightforward in that treatment, if even offered by the hospital, will not improve the patient above their baseline. As the family have made it clear that this baseline was already intolerable for the patient then it could be fair to say that treatment will likely simply prolong the dying process rather than prolong her life.
Various theorists have proposed different virtues required for the healthcare professional.15–18 In this case, it is the moral virtues of courage and compassion that stand out as required for navigating the complexity these clinicians face. 19 It takes courage to make a best interests decision. The decision not to send this patient to hospital when not doing so might hasten her death, where her wishes are not formally recorded is not an easy one to make. However, with courage the clinicians can make this decision even though they are worried that there might be consequences for themselves, or that, due to the circumstances, they are making an imperfect decision. It is worth noting, that courage as a moral virtue is distinct from the concept of ‘clinical courage’, which is described in a number of texts in various healthcare disciplines.
Virtuous acts sit within a golden mean, 16 meaning that the virtuous act is the one that fits between two extremes both of which would be seen as vices. In this case, the clinicians must temper their courage with significant caution – they do so through shared decision-making with a family physician. To use an overabundance of courage would slip the clinician into that of rash decision-maker who breaks all protocol, perhaps becomes an unemployed ex-clinician, or perhaps not respecting the family wishes. On the flip side the cowardly clinician refuses to make any decision, pushing decision-making onto another team through taking the patient to hospital thereby causing both the patient and their family distress. By using courage backed up with their knowledge of ethics, law, and clinical skills, these clinicians are able to make a morally virtuous decision.
Compassion is the other virtue that underpins this interaction. It is a truly compassionate act to allow someone a good death for both the patient and their loved-ones. Ethical duty expands beyond the clinician–patient relationship and the effects of our actions on the family/loved-ones must also be considered. The family in this case are going through one of the hardest things that befalls a group – the sickness and dying of a loved-one. The compassionate clinician recognises the sensitivity of this issue and works together with the family to learn and understand what they can of the value system the patient and family hold. The compassionate clinician centres the patient and their family, considering the effect of their interactions on them, rather than being focussed on the potential effects of their decision on themselves (be that being late off work, or having a difficult conversation with their manager).
The concept of a good death is also of great importance to consider here. This is a broad concept, but what we know is many people want to die at home, this becomes even more common when in the advanced stage of illness.20,21 In fact, it has been suggested that allowing a good death is the ultimate goal of a life well lived and so healthcare workers owe a duty to help facilitate this and not aggressively treat dying. 22 It takes courage for clinicians to work in this grey zone and shows true compassion to allow this sort of good death take place.
Coming to the decision to leave a patient at home to die without valid medical or legal paperwork is made possible with strong clinical knowledge, a good understanding of ethical arguments, and courage and compassion. These are features that need to be developed and it is our duty as educators to develop them in our students.
Broader discussion on virtue ethics
The propensity for novice paramedics to err towards algorithmic methods of decision-making is perhaps a reflection of the isolated and remote nature of practice and reflects the tendency for some paramedics to follow guidelines-based approaches to practice, 23 as clinical decisions based on algorithmic thinking are more defensible than a decision based on values. For example, paramedics use the ABCDE assessment as a way of reducing complexity in clinical situations and may apply similar linear thinking to the complexity inherent in ethical decisions.
This may be in part due the recognition of paramedics that any clinical governance will be viewed from a perspective removed from the lived experience of the situation. For example, in ambulance paramedic practice – the individual and crewmate are the only clinicians immersed in the situation, everyone else is hermeneutically, and physically, removed from the patient presentation. The messy reality of ethical decision-making means that in addition to navigating the complexity inherent in situations paramedics also must be able to record, justify, and defend decisions undertaken in a complex and dynamic environment – which normally, in clinical practice, would be supported or validated by reference to some kind of clinical guideline.
This tendency towards algorithmic decision-making means for many of our colleagues, an understanding of ethics is rooted primarily in Beauchamp and Childress's four principles approach. 10 We posit that there is more that paramedics ought to consider. It is worth being clear that the principles are not in competition with VE, and we do a disservice to both VE and principlism by pretending that they are. 24 However, what we must ensure clinicians understand is that the principles are just a way of ordering thoughts when considering ethical issues in (para)medicine. 10 They are not a normative theory in themselves 10 and do not (arguably) cover all the issues and dilemmas encountered due to the complex nature of paramedic practice. This is why the development of strong moral character, and an understanding of moral reasoning is the duty of every healthcare worker, but particularly important for the paramedic whose work is defined by complexity.
Limitations to VE
VE with its focus on the development of moral character has an immense potential for preparing clinicians to manage the uncertainty and complexity inherent in paramedic practice. However, VE is not without its detractors. Historically, there has been a pushback against VE from clinicians as there is a feeling that VE does not adequately give answers to ethical dilemmas as they arise, leaving the clinician unsure how to act. 25 A checklist approach to morality where answers are given can be useful – especially in the developing clinician – but by its very nature it is limited. Rather, what we need to do is develop clinicians with in-depth ethical knowledge and the practical wisdom of how to apply it. This is why we do not argue against teaching and utilising other ethical approaches – but rather, we want to see virtue developed alongside as a part of creating the moral clinician. Another classic argument against VE is how you manage dispute – without a set of rules what if two ‘virtuous’ clinicians disagree? 26 The point of this argument highlights that a strictly VE approach does not deal with disagreement, or lend itself to a standardised application of moral principle. However, this argument is dependent on the assumption that other ethical theories will lead to agreement, or at least a standardised application of moral principle – such critique falls apart when considering the complex nature of paramedic practice. Even the strictest rule-based approach to ethics is unlikely to be evenly applied, and not lead to disagreement, in the changeable healthcare environment. VE with its focus on both moral development and practical wisdom is likely to help create clinicians who understand, and accept, nuance and disagreement in the process of reaching the correct decision.
A strong argument against traditional VE is that it is poor at managing complex considerations of power dynamics between individuals. 27 This is something we ought to be highly aware of in healthcare and therefore we propose that a modern understanding of VE should be used, 27 where one's understanding of morality comes alongside an understanding of social justice and power structures. Ill health and inequalities have a synergistic relationship. In the UK, it is well documented that people from lower socioeconomic groups and black or minority ethnic communities experience worse health and have worse health outcomes. 28 Paramedics therefore have a large amount of contact with these groups and ought to understand the complex power imbalances that exist within these clinical encounters.
The lack of simplicity in becoming a moral practitioner through a VE approach is both its strength and its weakness. There is likely to be pushback from students and clinicians alike with the common questions such as ‘how does this help me in the midst of a dilemma?’ This makes VE a harder initial sell, and the development of engaging and pedagogically sound learning materials a requirement. However, this lack of simplicity is, in fact, truly one of VE's great strengths. The quest to do better and become a moral individual is a lifelong journey, and encouraging this throughout the career of paramedics has the potential to fundamentally change practice.
Gap in current practice
We have discussed VE as currently lacking in paramedic education and practice. Arguably, as a field, we are rather immature when it comes to the subject of ethics more broadly, evidenced by the paucity of ethical literature published relating to paramedic practice. Current writing from our profession on paramedic ethics rarely mentions VE as an approach. Curriculum guidance for the UK does not suggest any specific requirement for VE in practice, rather suggesting that paramedic students must: ‘Demonstrate a critical and contextual understanding of the ethical frameworks surrounding paramedic practice’ and ‘Evaluate ethical issues associated with paramedic practice and apply ethical principles to practice’. 29 (p19) Though this guidance also gives equal weight to legal systems and healthcare law; frameworks for professional practice; philosophy in paramedic practice; and, healthcare ethics, we suggest this is not enough. Ethics should feature heavily in any curriculum, with approaches such as VE woven throughout a student's journey.
Other healthcare professions have recognised the utility of VE in both practice and education with multiple papers arguing for its utility.16,17,30–32 However, there is a paucity of empirical evidence to demonstrate the uptake of this approach, although the few studies which have attempted to do so have shown some promising results.33–36 This lack of evidence, however, should not be a reason to avoid pushing this approach forward. Empirical bioethics is a relatively new field of study and so clinicians would be hard pressed to find empirical evidence for whichever approach to ethical dilemmas they wished to use. VE has the potential to change the way we teach ethics in healthcare, working to develop staff as moral practitioners with in-depth knowledge is essential across all healthcare professions to allow us to stay attuned to the needs of our patients as society grows and changes.
Recommendations
Even without formal introduction of VE theory into curriculum or current practice, paramedic students are already having their moral character shaped by their placement mentors from whom they learn, or parrot, a significant part of their practice. 2 As any paramedic reading this will no doubt remember, newly qualified paramedics are also influenced by the people they work with and culture of their workplace. 37 Therefore, we would like to see more formal education of both students and their mentors in VE as this has the potential to increase reflexive practice from both mentors and students. As VE goes beyond this focus on the dramatic ethical dilemma, this will hopefully help prepare both our students and their mentors to navigate the challenges of everyday ethics.
There is a paucity of evidence relating to the adoption of a greater focus on VE into clinical education or practice. We therefore do not propose specific guidance on how this can be achieved, but rather see this as an area ripe for innovation for educators globally and strongly recommend the need for empirical study to understand the virtues and vices of adopting such an approach. Understanding VE and its potential applications within paramedic practice is an exciting and innovative possibility as, due to the nature of paramedic practice, it means learning the potential of VE in complex and dynamic environments, understanding which may contribute significantly to the wider discussion of ethics in multiple areas of healthcare practice.
Conclusion
There is a need for paramedics to have a reliable ethical framework due to the remote/unmoderated nature of practice which has limited clinical, managerial, or ethical/legal oversight. Operating in isolation in complex psychosocial and clinical situations is an added challenge to ambulance work necessitating robust systems of navigating ethically intricate situations; therefore, cultural competence and ethical practice should be interwoven into the fabric of education programmes. As we have shown through this paper, VE should be embraced by paramedics and paramedic educators as it has an important role to play preparing paramedics to achieve truly person-centred practice, maximising patient safety and workforce wellbeing, and in promoting civility between healthcare professionals. Due to the potential benefits for enabling paramedics, we advocate a deliberate exploration, application, and subsequent evaluation of a VE approach for all paramedics, paramedic educators, and paramedic students. Doing so may enable the philosophical development of our profession to keep pace with the diversifying clinical, educational, and research settings in which paramedics can be found practising.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
