Abstract
Background:
Sickle cell disease (SCD), the most common monogenetic childhood disorder, imposes a significant psychosocial and financial burden on caregivers of affected children. Despite the availability of community-based support programs, few are tailored to the specific identified needs of caregivers managing SCD. This study presents a comprehensive program evaluation of a community-partnered caregiver retreat hosted by the St. Louis Sickle Cell Association (SCA).
Methods:
Researchers collaborated with the SCA to evaluate their annual weekend-long retreat. Year 1 employed a cross-sectional design using the General Self-Efficacy Scale. Year 2 implemented a pre-post design using the Family Empowerment Scale. In Year 3, a mixed-methods design included the Social Support Survey Instrument, 2 focus groups, and 6 interviews. Data were analyzed using descriptive and inferential statistics and thematic analysis.
Results:
Findings revealed no significant group-level empowerment changes in Year 2, though individual improvements were noted. In Year 3, caregivers reported strong emotional and social support but low tangible support. Thematic analysis identified 5 themes: SCD awareness gaps, caregiving burden, psychological toll, support variability, and caregiver-identified solutions. Caregivers emphasized a need for peer connection, mental health support, practical advocacy training, and expanded access to retreat programming.
Discussion:
This program evaluation demonstrates the meaningful support provided by community-based caregiver retreats while highlighting areas for enhancement. The findings underscore the value of systematic evaluation in identifying program strengths and opportunities for improvement to better serve caregiver needs.
Conclusion:
Community-based partnerships can enhance support for caregivers of children with SCD. This evaluation identifies essential program components and demonstrates how systematic assessment can inform program development to better address unmet caregiver needs and advance health equity.
Keywords
Introduction
Sickle cell disease (SCD) is the most prevalent monogenetic childhood disorder, affecting about 1 in every 365 African American births in the United States (U.S.) 1 and 7 million people worldwide. 2 SCD causes red blood cells to become sickle-shaped, leading to poor oxygen delivery, vaso-occlusion, and hemolytic anemia. 3 Typically diagnosed via newborn screening in the U.S., 4 SCD is characterized by symptoms beginning in early childhood, including fatigue, severe pain episodes, infection, splenic sequestration, acute chest syndrome, stroke, and developmental delay.5,6
Caregivers of children with SCD play a critical role in managing frequent appointments, unpredictable hospital admissions, and missed school days. 7 The complex care required to manage SCD contributes to annual total medical costs exceeding $1.1 billion in the U.S. 8 Caregiving demands impact relationships, job performance, daily activities, mood, cognitive functioning, sleep, and overall quality of life.9 -11 The emotional and financial toll on caregivers is substantial, 12 with 1 study reporting annual losses due to unpaid work productivity estimated at nearly $3 million for their 187 study participants alone. 13 Caregiving demands limit employment capacity, exacerbating healthcare-related financial burden. 14
Caregivers report higher levels of emotional, traumatic, and situational life stress compared to the general U.S. population.15,16 They face systemic barriers including limited social services, employment constraints, educational disruption, and social stigma due to poor community awareness of SCD.17,18 Community support programs have demonstrated success in supporting caregivers of individuals with chronic diseases.19,20 However, programs for caregivers of children with SCD must be designed to address their unique challenges, including racial disparities in healthcare and stigma associated with the disease. 17 Systematic evaluation of caregiver support programs is essential to assess their alignment with caregiver needs, measure their effectiveness, and help secure funding to sustain and expand available support programs.
The St. Louis Sickle Cell Association (SCA) hosts an annual retreat for caregivers of children with SCD and initiated this research through an established partnership with therapists and scientists. The SCA independently designed and implemented the caregiver retreat and requested support in measuring the impact of the retreat to inform future programs. Our research team included SCA leadership, occupational therapists, a nurse practitioner, and implementation scientists. Over 3 years, we developed and refined our approach to understanding and supporting caregivers of children with SCD through the annual retreat. The process began with basic outcome measurement, evolved to include standardized assessment of caregiver empowerment, and culminated in qualitative study of caregiver-identified needs and preferences.
This study aims to conduct a comprehensive program evaluation of a community-based retreat for caregivers of children with SCD, with specific aims to:
Document the retreat’s impact on caregiver outcomes across 3 years using evolving measurement approaches.
Compare insights from quantitative and qualitative evaluation methods about the program effectiveness and caregiver experiences.
Identify essential components and areas for improvement in caregiver support programming based on caregiver-reported feedback and systematic assessment.
Methods
Program Evaluation Approach
This study emerged from a request by the SCA director to evaluate outcomes of their annual caregiver retreat. Our research team collaborated with the SCA over 3 years (2022-2024) to conduct a systematic program evaluation using evolving methodological approaches. Figure 1 summarizes the progression of design, participants, measures, and data analysis across 3 years. We adhered to the Consolidated Criteria for Reporting Qualitative Research Checklist (COREQ) 21 guidelines throughout our process. The study received Institutional Review Board approval from Washington University in St. Louis School of Medicine.
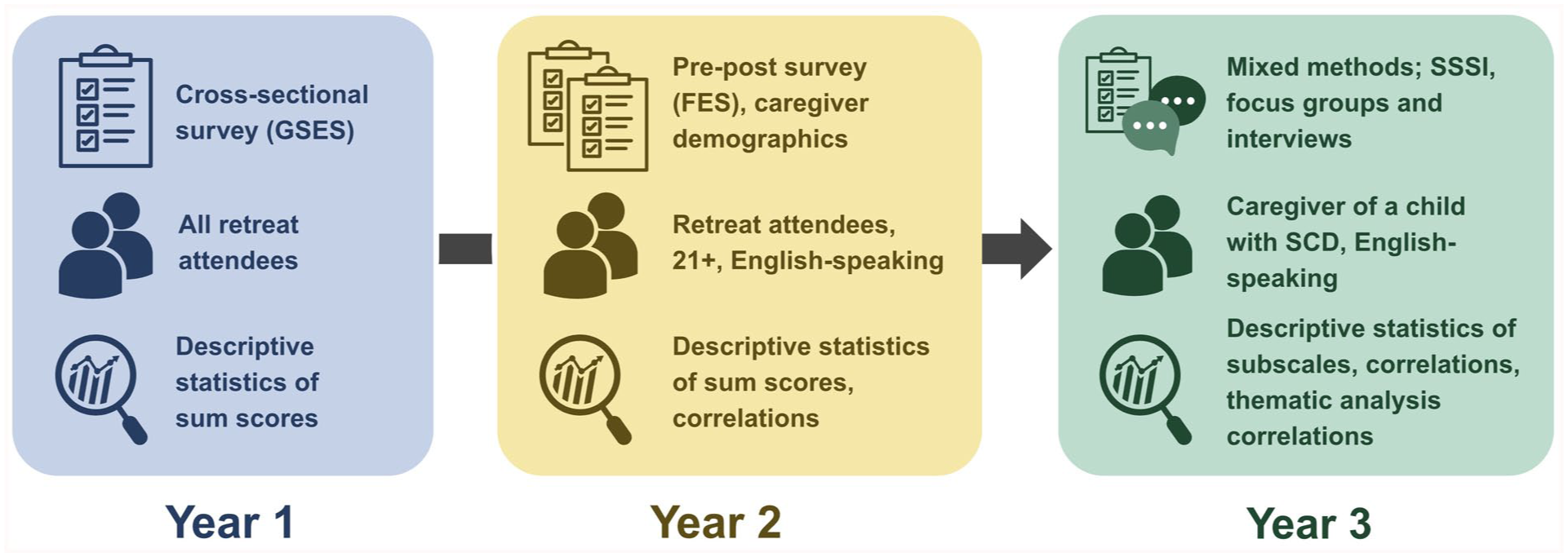
Iterative evolution of evaluative methodology.
Intervention
The SCA, a local not-for-profit organization, hosts an annual weekend-long retreat for SCD caregivers. The retreat provides educational and participatory sessions focused on self-care, stress reduction, guilt management, advocacy, role fulfillment, and goal development. The retreat also incorporates spa activities, meditation sessions, and information about community resources.
Study Design Evolution
Our evaluation methodology evolved across 3 iterations based on preliminary findings and the need to capture different aspects of program impact. Year 1 (2022) utilized an exploratory cross-sectional design to assess initial outcomes. Year 2 (2023) enhanced the approach with a pre-post design with data collected at the beginning and end of the retreat to better measure intervention impact. Year 3 (2024) expanded to a comprehensive mixed-methods evaluation incorporating quantitative measures and qualitative exploration of caregiver experiences and program perceptions.
Recruitment
A unique group of caregivers participated each year. Across all 3 years, participants were primary caregivers for a child with SCD. Year 1 included all retreat attendees, Year 2 required participants to be at least 21 years old, and Year 3 included both retreat attendees and 6 caregivers unable to attend. Focus groups included 7 participants each, following best practice guidelines. 22 Non-English-speakers were excluded in Years 2 and 3, though none were excluded for this reason. IRB approval was obtained each year, with informed consent obtained in Years 2 and 3.
Measure Selection and Implementation
Evolution of Measures
Our measurement approach evolved responsively over 3 years. In Year 1, we collaboratively selected the General Self-Efficacy Scale (GSES) 23 for its brevity to assess caregivers’ perceived ability to respond to obstacles on a 1 (not true at all) to 4 (exactly true) Likert scale. However, the GSES proved inadequate for capturing caregiving-specific outcomes, and the single-point measurement limited our ability to attribute changes to retreat participation.
In Year 2, we shifted focus to caregiving-specific outcomes and collaboratively selected the Family Empowerment Scale (FES), 24 which measures empowerment across Family (12 items), Service System (12 items), and Community/Political (10 items) domains. The Family subscale addresses everyday care management at home. The Service System subscale represents interactions with healthcare professionals and institutions. The Community/Political subscale indicates collaboration with community members, organizations, and policymakers. Higher mean scores indicate stronger empowerment. Internal consistency reliabilities of .98 to .88 and test-retest reliabilities of .77 to .85 have been reported. 24 This pre-post design better captured specific retreat outcomes but still did not fully explore caregivers’ lived experiences.
During Year 3, we expanded to a mixed-methods approach. We selected the Social Support Survey Instrument (SSSI), 25 which measures perceived support across Emotional/Informational Support (8 items), Tangible Support (5 items), Affectionate Support (3 items), and Positive Social Interaction (3 items). Emotional/Informational support represents availability of someone to confide in; Tangible Support refers to assistance with daily tasks; Affectionate Support represents available love and affection; and Positive Social Interaction refers to having someone for enjoyable activities. Items are rated on a 1 to 5 Likert scale with higher scores indicating more perceived support, with an internal reliability of 0.97. 26
To explore caregivers’ experiences and needs, we developed a semi-structured interview guide with 7 questions and additional probes, designed for 30- to 60-minute sessions. Developed by a graduate student and reviewed by an occupational therapist with SCD expertise, a qualitative researcher, the director of the SCA, and a research coordinator, questions focused on caregiving burden, available supports, perceptions of retreat impact, and future support needs. The interview guide aligned with the Health Equity Framework (HEF; Figure 2; Supplemental Material).

Select interview question alignment with the Health Equity Framework (HEF).
Focus groups were conducted in person at the end of the Year 3 retreat, led by occupational therapists with qualitative training and 15 years of collaboration with the SCA. Individual interviews were conducted via Zoom over 2 months following the retreat based on caregiver availability. 27 A research coordinator trained in qualitative methods with 1.5 years of experience working in the sickle cell community conducted the interviews.
Demographics Questionnaire
Demographic information collected in Years 2 and 3 included caregiver age, gender, education, employment, household income, and household size. Year 2 (Supplemental Materials) additionally collected the caregiver’s relationship to the child with SCD and the child’s age, gender, insurance status, and SCD genotype. Year 3 (Supplemental Materials) also gathered caregivers’ race/ethnicity, employment type, and the child’s SCD care location. Year 2 annual income ranges were categorized as very low (under $20 000), low ($20 000-$40 000), medium ($40 000-$60 000), and high ($60 000-$80 000). Year 3 income ranges were categorized as very low, (under $25 000), low ($25 000-$50 000), medium ($50 000-$75 000), high ($75 000-$100 000), and very high ($100 000-$150 000). Income ranges differed between years due to variability in team member involvement.
Theoretical Framework
In Year 3, we incorporated the HEF 28 to contextualize caregivers’ experiences within broader systems. The HEF conceptualizes health outcomes resulting from interactions between individuals and their environment across 4 domains: Systems of Power (policies, processes, and practices), Relationships and Networks (connections with family, friends, community, schools, and workplaces), Individual Factors (response to social, economic, and environmental conditions), and Physiological Pathways (physical, cognitive, and psychological functions). The domains represent the connections, responses, systems, and physiological factors that either promote or intensify health equity. Interview questions were deliberately aligned with these domains to capture multi-level factors impacting caregiver experiences.
Data Analysis
Quantitative Analysis
Descriptive statistics summarized participant demographics and scale scores across all years. Year 2 analysis included dependent samples t-tests to assess pre-post changes in empowerment and correlation analyses between demographic factors and outcomes. Year 3 analysis explored relationships between demographic characteristics and social support domains using Spearman’s correlation coefficients, with statistical significance set at P < .05. Analyses were completed with IBM SPSS Statistics, Version 29.0.2.0. 29
Qualitative Analysis
Qualitative interviews were audio-recorded, transcribed verbatim using IRB-approved transcription software MS Word Version 16.93, 30 de-identified, and reviewed for accuracy. Using thematic analysis, 31 2 team members (SL and HM) generated a preliminary codebook before uploading the transcripts to NVivo Version 14 32 for coding. The coding team (SL and HM) tested the preliminary codebook by independently coding 2 individual interviews and 2 focus groups to ensure the codebook captured content across both data types. After independently coding each subset, they reviewed discrepancies, discussed code application, and expanded the codebook to better reflect caregivers’ experiences. After revisions, SL and HM independently recoded 4 transcripts with the updated codebook to confirm accuracy, then separately coded remaining transcripts. They met to resolve discrepancies and refine definitions through consensus, systematically applying all refinements to previously coded transcripts. Patterns were grouped into themes and adjusted until achieving comprehensive understanding of caregivers’ experiences.
Results
Participant Characteristics
Twenty-two caregivers attended the retreat in Year 1, 18 in Year 2, and 14 in Year 3, with 6 additional non-attendees completing interviews in Year 3. Table 1 summarizes participant demographics from Years 2 and 3. Demographic information was not collected in Year 1.
Participant Demographics.

In Year 2, participants (n = 18) had a mean age of 43.78 years. Gender distribution was relatively balanced. Educational attainment varied across categories, with over one-third holding bachelor’s degrees or higher. Half were employed, and household size averaged between 4 and 5 people. Most caregivers used government-sponsored insurance such as Medicaid.
Year 3 participants (n = 20) had a mean age of 39.12 years and were predominantly female. Educational levels were distributed across categories, with a third of caregivers holding bachelor’s degrees or higher. Most were employed, with about half reporting income in the $25 000 to $50 000 range. Consistent with Year 2 data, average household size was 4 to 5 people, and insurance coverage was primarily government sponsored.
Years 1 and 2
Year 1 assessed caregivers’ perceptions of self-efficacy with the GSES. Scores (n = 22) ranged from 20 to 40 with an average score of 33.05 (SD = 5.33), indicating moderate self-efficacy. Data was collected at caregivers’ convenience during the retreat weekend, and collected data was incomplete. Due to these challenges, meaningful conclusions were limited.
In Year 2, we assessed the retreat’s impact on caregivers’ empowerment using the FES. Of the 18 retreat attendees, 17 completed both the pre- and post- surveys. Overall group FES scores showed no significant pre-post changes. However, 8 participants demonstrated significant differences on at least 1 subscale (Family, Services, or Community), suggesting variable intervention impact. Education level positively correlated with Services (ρ = .422, P = .040) and Community subscales (ρ = .751, P < .001), while income positively correlated with the Community subscale (ρ = .468, P = .025). Most participants whose responses indicated significant pre-post changes had low annual incomes (under $20 000), suggesting lower-income individuals may benefit more from the retreat.
While Year 2 findings provided additional insights, our measurement approach did not fully capture the impact of the retreat or caregivers’ lived experiences. In Year 3, we refined our methodology to prioritize capturing caregivers’ perceived social support, lived experiences, and needs.
Year 3
We assessed caregivers’ perceived social support in Year 3. Scores on the SSSI revealed varying levels of perceived social support. The highest mean score was for Positive Social Interaction (M = 4.13, SD = 1.11), followed by Affectionate Support (M = 4.08, SD = 1.26) and Emotional/Informational Support (M = 3.94, SD = 1.07). Tangible Support received the lowest rating (M = 3.85, SD = 1.27). The lowest-rated items were “How often do you have someone to share your most private worries and fears with?” (M = 3.55) and “How often do you have someone who understands your problems?” (M = 3.60), both from the Emotional/Informational Support domain. Household size negatively correlated with both Tangible Support (Spearman’s r = −.468, P = .038) and Total SSSI score (Spearman’s r = −.482, P = .031), indicating that larger households reported lower support levels.
Interview and Focus Group Analysis
Caregiver interviews (n = 6) and focus groups (n = 14) revealed 5 themes illustrating the complex experience of caring for a child with SCD. These themes highlight challenges from diagnosis through ongoing treatment, as well as caregivers’ resilience and recommendations for improved support systems. Figure 3 illustrates relationships between themes, subthemes, and HEF domains.

Themes in relation to Health Equity Framework domains.
Theme 1. Awareness Gaps: Limited SCD Knowledge and Caregiver Burden
Many caregivers reported limited exposure to SCD prior to their child’s diagnosis and therefore limited prior knowledge about the disease. Upon diagnosis, families face the disproportionate burden of seeking and digesting information on how to care for a child with SCD, adding to the stress of navigating complex health systems. Theme 1 aligns with the Systems of Power domain of the HEF, illustrating how SCD, predominantly affecting Black communities, is underprioritized in health education, research, and policy.
Theme 1a. Caregivers’ Initial Knowledge Gap Following Diagnosis
Caregivers consistently reported feeling underprepared for their child’s diagnosis, having limited prior knowledge about SCD:
When I first found out that she had sickle cell, I do not think that I was educated enough, nor do I think that it was really explained to me. – Caregiver 103 (individual interview)
For many caregivers, navigating new parenthood alongside processing a child’s chronic disease diagnosis contributed to significant stress. Even those with previous family exposure to SCD reported feeling unprepared for the specific challenges of caring for a child with SCD. Many described a learning curve as they struggled to understand the disease:
When she was first born, I was like, ‘Are you just crying, or are you in pain? Is it the start of pain?’ You really have to get to know them, and the unknowing can really be nerve-racking. – Caregiver 115 (focus group)
Despite awareness of common SCD symptoms, many new caregivers expressed significant anxiety about identifying true medical emergencies. Distinguishing between pain crises and normal childhood discomfort presents an inherently difficult challenge.
Theme 1b. Public and Institutional Lack of SCD Awareness
Caregivers encountered limited understanding of SCD in both public and institutional settings. School systems were frequently highlighted as environments where knowledge deficits prompted additional challenges:
A lot of schools don’t have information on [SCD]. Like to know how to handle a pain crisis. – Caregiver 105 (individual interview)
Concerns about schools’ lack of preparedness manifested in constant advocacy for basic accommodations to prevent disease complications, such as ensuring proper hydration and avoiding temperature extremes:
When my child started school, her teacher really knew nothing about [SCD], so I did try to give her a lot of information on it . . . So it’s been a huge learning experience. – Caregiver 103 (individual interview)
The burden of education often fell entirely on caregivers, requiring them to initiate new conversations with school personnel each academic year.
Theme 1c. Healthcare System Deficiencies in SCD Understanding
Most concerning were knowledge gaps within healthcare environments. Multiple caregivers reported experiences with medical professionals unfamiliar with SCD:
I would say like the lack of knowledge from others . . . even medical professionals. The first time we were at the hospital, they put us on a not-hematology floor, and we had the worst experience. It was horrible. – Caregiver 113 (focus group)
Caregivers consistently described a contrast between knowledgeable hematology teams and other healthcare providers, particularly in emergency settings. Hematologists were generally characterized as accommodating and knowledgeable, while other providers were often perceived as judgmental (especially regarding pain management) and displaying alarming knowledge gaps about SCD. The perception that some healthcare providers were not only uninformed but uninterested in learning about SCD was particularly distressing for some:
They don’t understand it . . . the hospitals don’t know either. And some of them don’t necessarily care to know. – Caregiver 105 (focus group)
Theme 2. Competing Priorities: Balancing SCD Management with Life Responsibilities
Caregivers described the ongoing struggle to balance intensive SCD management demands with other essential life roles and responsibilities. This theme reflects the Individual Factors domain, where factors like employment type, family structure, and access to resources affect caregivers’ experiences. These factors are not simply personal choices but are shaped by historical and structural inequities that influence employment opportunities, available family support, and economic stability.
Theme 2a. Time-Intensive Nature of SCD Management
Participants described the unpredictable, yet demanding time commitment required for SCD management as a central challenge, with hospital stays disrupting normal routines:
They make us wait the whole week. You might as well bring a bag, it always two to five days they make you wait. – Caregiver 110 (focus group)
Prolonged hospital stays created significant disruption to caregivers’ lives, often requiring them to relocate their daily lives to the hospital for unknown periods. The unpredictability made planning nearly impossible, as caregivers needed to be prepared for potential crises. Beyond overnight hospital stays, caregivers emphasized the time dedicated to routine management:
We always in the hospital, I must say, since he started getting his blood transfusions every three weeks. – Caregiver 101 (focus group)
Even during periods of stability, caregivers reported significant time devoted to routine care—regular appointments, specialist visits, medication management, and monitoring for complications—creating competing demands:
I have another child at home, so we’re trying to manage the time, and I still have to work. I still have to make sure the house is running. And then he may be hospitalized from five or six days, and now what do I do?– Caregiver 102 (individual interview)
Theme 2b. Challenges Finding and Maintaining Employment
The unpredictable nature of SCD crises directly impacted caregivers’ ability to maintain stable employment. Many described the impossible choice between being present during medical emergencies and maintaining job security:
Not being able to keep stable employment because when she’s sick or having a pain crisis, it’s three to four days. . . you can’t call off work twice a month for four days. – Caregiver 105 (individual interview)
Many caregivers reported exhausting all available sick and vacation time early in the year, leaving them vulnerable to job loss when subsequent crises occurred. Some caregivers ultimately found traditional employment untenable given their unpredictable caregiving responsibilities:
I want to work, but I can't work because of her health (Caregiver 105). This participant described needing a job in which she “won’t be terminated because [she’s] in a hospital with [her child] while the pain crisis is going on.” – Caregiver 105 (individual interview)
Theme 2c. Balancing Care of Multiple Children
For caregivers of multiple children, hospitalizations prompted particularly difficult decisions about dividing their attention and resources:
Whenever we get admitted, we have to find care. Either we find outside care or one of us has to stay at home with the other children to make sure they get fed, they get to school – Caregiver 104 (individual interview)
Many described feelings of guilt about prioritizing their child with SCD’s needs and highlighted the logistical complications of maintaining routines for other children while managing a pain crisis. Single parents reported especially challenging circumstances:
When she do have her crisis, I have to choose between my kids . . . One of my biggest challenges having to balance both of my kids’ lives as a single parent – Caregiver 101 (individual interview)
For single parents without reliable co-parents or extended family support, these situations often required creating complex networks of temporary caregivers for emergencies. Some single parents described making the difficult decision to bring other children to the hospital during extended stays, which added further logistical considerations.
Theme 3. Psychological Impact: The Emotional Toll of SCD Caregiving
Practical challenges of SCD management were often accompanied by negative psychological impacts on caregivers. This theme connects to Physiological Pathways, illustrating how the chronic stress of caregiving for a child with SCD manifests in caregivers’ physical and psychological health. Many caregivers expressed feelings of helplessness during times of disease complications:
The crisis. The hospitalizations. The emotions behind it, just looking at my son when he gets sick, you know, and I can’t really do nothing. – Caregiver 110 (focus group)
Many caregivers described feeling powerless despite closely following medical recommendations. Often, caregivers described putting their own emotional needs aside for the sake of their children during crises. Several caregivers described intense emotional responses to seeing their children hospitalized, highlighting the traumatic impact of witnessing their child in acute medical distress:
I can’t come to the hospital and see my son like that. Like when I seen him like that, I am scared. When I am in the room I broke down. And when I told her I'm like, I can't see my son hooked up to all this, my whole body shut down. – Caregiver 102 (focus group)
Some caregivers described physical manifestations of emotional distress, such as losing sleep, or as this caregiver expressed, experiencing a full “body shut down.” The ongoing vigilance caused increased worry in caregivers, sometimes leading to social isolation in attempts to avoid a crisis. When asked why they chose to attend the SCA retreat, 1 caregiver replied:
It’s just a peace of mind, because we have to constantly be there. Besides school, we haven’t been outside the house since we been here last year. – Caregiver 111 (focus group)
Theme 4. Support Variability: Navigating Available Resources
Caregivers shared their various forms of support. However, their experiences reveal significant inconsistencies in the availability, accessibility, and effectiveness of these support systems. Theme 4 aligns with Relationships and Networks, highlighting how both personal and institutional supports shape caregivers’ capacity to manage SCD.
Theme 4a. Caregiver-Identified Supports
Some caregivers reported positive experiences with healthcare professionals who provided comprehensive information and support beyond standard medical services:
When we went to our first hematology appointment, they laid out everything. Like when they go to school, they need a IEP, a 504 . . . They start talking about if they miss school, if I ever need family medical leave, they’d tell me how to get it in place. (Caregiver 114, focus group), and “My child have a card where all her medications are . . . What they’re supposed to give her when she goes to the emergency room.” – Caregiver 103 (focus group)
Outside of healthcare interactions, extended family support was critical for many caregivers, enabling them to fulfill employment responsibilities and maintain a better life balance:
We have a lot of people in our family who help us take care of her, so we are all informed about what to look for . . . It allows for us to be able to work and do more than I’d be able to do if I had to do it all by myself. – Caregiver 115 (focus group)
Several caregivers reported having no support from family, friends, or their physical communities. However, online communities offered unique targeted support, connecting caregivers with other parents or caregivers:
I also am in groups on Facebook, where they talk about sickle cell where it’s families are or even carriers themselves . . . about different things they do to help . . . Show me a lot as far as hope as well. – Caregiver 103 (individual interview)
Multiple caregivers noted that meeting adults or older adults with SCD in the community gave them hope for their own child with SCD’s future. Community support through the SCA provided valuable resources and connection for some:
The Sickle Cell Association will always provide support. Have the monthly support groups and caregiver retreats, the Christmas parties, and the walk . . . I know that they are a staple in the community and some place I can go to make sure I have the support I need. – Caregiver 104 (individual interview)
Theme 4b. Gaps in Existing Support Systems
Although some caregivers benefitted from available support systems, many described feeling isolated or lacking consistent support:
I don’t have no groups. I don’t have no support. It’s just me and [child], facing these challenges . . . we’re just in the hospital alone. – Caregiver 105 (individual interview)
Some caregivers reported that information delivery by the medical team could be more distressing than helpful, emphasizing the impact of communication on caregivers’ ability to process information and respond effectively:
They gave me this big packet about how she could possibly pass away from this . . . I was 22, and they telling me she’s going to pass away. I don’t think anyone sat down and said this [packet] was gonna go to a person who is dealing with this; they just sat down and was like, ‘This is the information you need. Here it is.’ – Caregiver 115 (focus group)
Others described exasperation with local organizations that offered various supports but were difficult to access:
They [SCA] say they can help you with all these different resources, but when you reach out to them, you don’t really get that type of help . . . No one will pick up. – Caregiver 101 (individual interview)
The inconsistent availability of both personal and institutional support networks demonstrates how social connection disparities contribute significantly to broader health inequities among SCD caregivers.
Theme 5. Caregiver Solutions: Pathways to Enhanced Support
Building on their experiences with existing supports and challenges, caregivers articulated specific recommendations for improving the support ecosystem for families managing SCD. Both retreat attendees and non-attendees shared many overlapping needs, with some key differences in their suggestions for future retreat implementation. Theme 5 reflects Relationships and Networks—caregivers’ themselves identified relationship-building and formal support services as critical to managing a child’s SCD .
Theme 5a. Requested Caregiver Resources
Both retreat attendees and non-attendees aligned well in their identified needs, with many caregivers identifying emotional support through counseling as their most critical unmet need:
Somebody like a 24-hour advocate . . . Listening to the parent or the caregiver . . . Counseling is not cheap. With reputable counselors, with people who are going to be readily available. – Caregiver 105 (individual interview)
This caregiver also emphasized the around-the-clock nature of caregiving, specifying that caregivers would benefit from someone on-call for advocacy and mental health challenges that arise.
Theme 5b. Increased Connection Within SCD Community
The most frequently identified need among both retreat attendees and non-attendees was establishing meaningful connections with other families affected by SCD. The desire for community was not merely for casual interaction but for structured, regular engagement that could provide emotional validation and practical knowledge exchange:
The number one thing that would have been the most help would have been being able to connect with other people who were going through the same thing, like some type of group setting that met regularly. – Caregiver 102 (individual interview)
Caregivers emphasized how witnessing successful SCD management in other families served as both educational and inspirational, particularly for those newly navigating an SCD diagnosis. Beyond connecting with other families, participants strongly advocated for community-based support that extends to children with SCD:
I would like more support groups. In different communities . . . Not only just for the parents, but for the kids as well. – Caregiver 106 (individual interview)
Theme 5c. Caregiver Suggestions for Future SCA Retreats
Both retreat attendees and non-attendees suggested that increasing the frequency of retreats would enhance accessibility, with multiple retreats per year making it easier for caregivers to attend. Additionally, both groups identified education about rights and effective advocacy techniques as crucial for improving healthcare experiences:
Medical advocacy, like how to be an advocate for your kid, what is appropriate, what is not appropriate. What is your rights as a parent, what is your child’s rights as a patient? – Caregiver 114 (focus group)
However, there were notable differences in other suggestions between the 2 groups. Retreat attendees expressed interest in extending the duration of the annual retreat, allowing for more comprehensive programming and deeper community building. They also requested content focused on practical strategies rather than general wellness topics:
Information on how to navigate the emergency room . . . What are the dos, the don’ts. What are the language you need to know to conduct well? What if you don’t have an advocate? – Caregiver 107 (focus group)
Retreat attendees sought specific communication strategies to help them secure appropriate care during critical moments. Many caregivers also requested sessions focused on concrete resources related to employment accommodations and financial support:
I probably do the sessions more geared towards what is the resources for us? These [current sessions] are nice to have the discussions, but what’s out there for—(Caregiver 114 (focus group) “—For disability, or medical leave, and how you do it.” – Caregiver 113 (focus group)
In contrast, non-attendees’ suggestions primarily focused on addressing participation barriers. The availability of childcare at the retreat was identified as their main recommendation, as many lacked reliable caregivers for their children during potential retreat attendance. Additionally, non-attendees reported information gaps about the retreat itself, with some expressing confusion about eligibility criteria or scheduling, and some entirely unaware that such a retreat existed.
Discussion
This program evaluation’s key contribution lies in demonstrating how systematic assessment can evolve to capture increasingly meaningful insights about community-based interventions. Through our methodological progression from basic outcome measurement to comprehensive mixed-methods evaluation, we identified 5 themes: gaps in SCD awareness, competing caregiver priorities, psychological impact of SCD care, variability in support systems, and caregiver-identified solutions.
Our quantitative findings revealed no significant group-level changes in empowerment following the retreat, though individual improvements were noted. This aligns with the complex nature of empowerment as a construct that likely requires sustained intervention and longer follow-up periods to manifest measurable change. The challenges caregivers face are deeply rooted and extend beyond what a weekend retreat can address. However, the individual improvements observed suggest that some caregivers do experience immediate benefits, and the qualitative findings reveal that caregivers value the retreat for reasons that may not be captured by traditional empowerment measures, such as temporary respite, peer connection, and practical resource sharing.
Caregivers strongly desired increased community connection with other SCD-affected families, valuing these relationships for both emotional support and practical strategy exchange. The widespread lack of SCD knowledge among providers and the general public contributed to isolation. This finding aligns with research showing that peer support groups can improve psychological well-being and coping. 23
A novel finding from our iterative approach was caregivers’ prioritization of specific, practical resources over general wellness support. While traditional interventions emphasize psychological support and education, our participants emphasized needs for guidance on employment accommodations, emergency room advocacy, and legal rights. These needs emerged clearly in Year 3, demonstrating how our responsive approach surfaced priorities that may have otherwise remained unexplored.
Our findings align with and extend existing literature. Blakey et al 33 identified gaps in SCD awareness, noting that families and clinicians were affected by limited provider knowledge. Caregivers in our study described alarming encounters with unprepared medical personnel, particularly in emergency settings. Patients with SCD benefit significantly from hematology-specific care, but many providers lack specialized SCD training, which negatively impacts both patients and caregivers.
The pattern of caregivers’ competing priorities aligns with Hoyt et al 18 showing children with SCD manage multiple responsibilities alongside disease demands. Our participants described helplessness and psychosomatic responses like sleep disruption during crisis. These experiences support findings from Bruzzese et al 5 of heightened distress and poorer mental health in caregivers of youth with SCD. The financial strain described by caregivers aligns with our participants’ reports of employment disruptions, particularly affecting single-parent and lower-income households.
Limitations
Several limitations are noted. Year 1 provided limited insights due to incomplete demographic data collection and minimal research team involvement. In Year 2, while research team involvement increased, the selected measures yielded insights misaligned with retreat objectives and caregiver priorities. Variation in demographic collection tools between Years 2 and 3 further constrained comparative analysis. The methodological changes between years, while responsive to evaluation needs, limited our ability to make longitudinal comparisons.
Additionally, 1 focus group included 2 caregivers affiliated with the local SCA, which may have introduced bias. Future studies should establish clearer participation guidelines and ensure balanced contributions.
However, these methodological adjustments represent a strength of responsive program evaluation, allowing us to progressively refine our approach and generate increasingly relevant findings. The evaluation from basic outcome measurement to a comprehensive mixed methods assessment ultimately produced insights more directly applicable to program improvement and caregiver experiences.
Implications
Our findings have implications for healthcare practice, system design, and policy. Identifying caregivers’ most pressing knowledge, support, and resource needs offers a foundation for more responsive, equity-driven interventions. Future efforts should prioritize caregiver-identified needs, including access to peer support networks, practical advocacy training, and structural supports addressing the unique financial and employment challenges of caring for a child with SCD.
Conclusion
This program evaluation reveals the complex experiences of caregivers of children with SCD and demonstrates both the value and limitations of community-based retreat interventions. Our findings indicate that while the retreat provides meaningful support, particularly through peer connection and temporary respite, caregivers continue to navigate significant systemic challenges in employment, healthcare navigation, and accessing resources.
Through systematic assessment, we identified essential program components that directly reflect caregiver priorities: opportunities for peer connection, practical advocacy training, mental health support, and concrete resources for employment and healthcare navigation. A key finding was that caregivers consistently prioritized actionable. Practical resources over general wellness programming—insights that emerged by centering caregiver voices in our evaluation process.
This 3-year evaluation demonstrates that meaningful program assessment must be grounded in authentic engagement with the communities being served. Our methodological evolution—from basic outcome measurement to comprehensive mixed-methods assessment—was driven by the recognition that traditional evaluation approaches often miss what matters most to participants. The most valuable insights emerged when we directly asked caregivers about their experiences, needs, and recommendations rather than assuming what outcomes would be most relevant.
Moving forward, community-based organizations must prioritize evaluation approaches that elevate participant voices in identifying program strengths, gaps, and priorities. Only by centering the lived experiences and expressed needs of caregivers can interventions be designed and refined to truly address the realities families face while advancing health equity for the SCD community.
Supplemental Material
sj-pdf-1-rpo-10.1177_27536351251387234 – Supplemental material for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation
Supplemental material, sj-pdf-1-rpo-10.1177_27536351251387234 for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation by Sophia C. Larson, Hunter G. Moore, Rosemary Britts, Alison S. Towerman, Ashley J. Housten, Madison Griffith, Kaylin A. Antonoff, Kelly M. Harris, Allison A. King and Catherine R. Hoyt in Advances in Rehabilitation Science and Practice
Supplemental Material
sj-pdf-2-rpo-10.1177_27536351251387234 – Supplemental material for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation
Supplemental material, sj-pdf-2-rpo-10.1177_27536351251387234 for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation by Sophia C. Larson, Hunter G. Moore, Rosemary Britts, Alison S. Towerman, Ashley J. Housten, Madison Griffith, Kaylin A. Antonoff, Kelly M. Harris, Allison A. King and Catherine R. Hoyt in Advances in Rehabilitation Science and Practice
Supplemental Material
sj-pdf-3-rpo-10.1177_27536351251387234 – Supplemental material for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation
Supplemental material, sj-pdf-3-rpo-10.1177_27536351251387234 for Community Support for Caregivers of Children With Sickle Cell Disease: A 3-Year Process Evaluation by Sophia C. Larson, Hunter G. Moore, Rosemary Britts, Alison S. Towerman, Ashley J. Housten, Madison Griffith, Kaylin A. Antonoff, Kelly M. Harris, Allison A. King and Catherine R. Hoyt in Advances in Rehabilitation Science and Practice
Footnotes
Acknowledgements
We’d like to acknowledge the St. Louis Sickle Cell Association, Megen Devine, and study participants for their contributions.
ORCID iDs
Ethical Considerations
The study received Institutional Review Board approval from Washington University in St. Louis School of Medicine.
Consent to Participate
All participants provided written informed consent to participate in the study.
Consent for Publication
All participants provided written informed consent to have their data published.
Author Contributions
SL conducted data analysis for Years 1 through 3, assisted with focus groups, coded and analyzed qualitative data, and drafted the manuscript. CH served as Principal Investigator and supervised the work. HM assisted with Year 3 focus groups, conducted all interviews, and coded and analyzed qualitative data. AT led data collection in Year 2. AH served as qualitative expert, facilitated focus groups, and provided feedback on codebook iterations and manuscript. MG created the interview guide for the qualitative component in Year 3. KA assisted with focus group facilitation. RM designed and led caregiver retreats as director of the St. Louis Sickle Cell Association. AK provided guidance and feedback throughout the study. All authors provided manuscript feedback.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the Partnership Development & Sustainability Support (UL1TR002345), Missouri Foundation for Health, Mentored Patient-Oriented Research Career Development Award (K23HL161328), the Center for the Study of Race, Ethnicity, & Equity (CRE2), and Vertex, which helped fund the caregiver retreats.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
De-identified data will be made available upon request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
