Abstract
Background
While the Liaison Committee on Medical Education emphasizes the teaching of cultural competence in medical education, the concept of cultural humility, focusing on self-reflection and lifelong learning, has been proposed as a more effective approach. Although there have been numerous discussions on both topics, understanding how faculty in clinical settings help students develop cultural humility skills remains limited.
Objective
Our multimethod study utilized a survey and semi-structured interviews to identify strategies that faculty at one institution use to help students develop cultural humility skills.
Methods
We administered a 10-question survey to assess faculty demographics, teaching characteristics, and familiarity with cultural humility. Participants most familiar with cultural humility were invited for semi-structured interviews. Survey data were analyzed with descriptive statistics, and interview data were thematically analyzed to identify key teaching strategies.
Results
In our study of 49 medical faculty members, the majority of participants were female (61%) and predominantly White (67%), covering a wide range of specialties and years of teaching. Of the participants, 74% expressed being at least somewhat familiar with cultural humility, and 10 consented to interviews. Strategies for cultural humility education included one-on-one instruction, feedback, and reflections. Thematic analysis underscored fostering learner curiosity about cultures, early patient exposure, and incorporating diverse learning perspectives as essential in developing students’ cultural humility skills.
Conclusion
Cultural humility is an important attribute for healthcare professionals that can enhance patient-centered care. Through focused interviews with faculty in our study and subsequent thematic analysis, our results suggest the need for longitudinal and multimodal educational strategies to cultivate cultural humility among medical students. By understanding current teaching methods, educators can design and assess more effective curricula to prepare future doctors for a culturally diverse patient population.
Keywords
Introduction
Since 2005, the Liaison Committee on Medical Education (LCME) has required medical schools to teach students “cultural competence,” which is defined as how different cultures view health, illness, and treatment, and to address gender and cultural biases in healthcare. 1 Cultural competence assumes a basic threshold one can reach to understand a culture fully. 2 On the other hand, cultural humility has been introduced as an alternative to cultural competency and focuses more keenly on self-reflection and lifelong learning when considering culture. 2 Incorporating cultural humility training over cultural competency training can bring about lasting individual and systemic changes in healthcare delivery. 3
Educating medical students on how to gain skills in their cultural humility will be critical to addressing the health needs of a growing ethnically diverse population in the United States. 4 However, accreditation bodies provide little guidance on how to accomplish this task. Medical education literature describes a mix of cultural competency and cultural humility curricula that vary in content, design, and implementation. These educational interventions range from didactic lectures to learning traditional dances with patients.5-8 Related articles that explore how healthcare professionals understand cultural humility include: the cultural awareness that medical students developed after providing medical care to refugees; student perspectives on their cultural humility training regarding Asian American patient inclusion; and nursing students’ perspectives on cultural competence.9-11 There is a gap in the literature regarding the development of cultural humility curricula, as educators often create these programs without understanding the existing methods faculty use to teach cultural humility skills to their students.
Our study addresses this gap in medical education by examining the specific strategies faculty at one urban tertiary care medical center use to develop medical students’ cultural humility skills. Cultural Care Theory (CCT) is the framework that aims to explain the interdependence of care and culture in providing more congruent support for the health and well-being of people. 12 Regarding curriculum development, Kern’s six-step approach involves problem identification and general needs assessment, targeted needs assessment, setting goals and objectives, developing educational strategies, implementation, and evaluation with feedback. 13 By applying CCT to Kern’s approach, we can gain much-needed insight into how faculty develop their students’ cultural humility skills and thus design educational strategies to help students provide more culturally appropriate care. We aim to highlight the faculty’s current practices in teaching students how to develop their cultural humility to inform future curriculum development, address the lack of detailed accreditation guidance, and support systemic changes in healthcare delivery through lifelong learning and self-reflection.
Methods
Survey Design
We developed a 10-question survey for our multimethod study to describe faculty demographics, teaching characteristics, and familiarity with cultural humility (Appendix A). The first six questions pertained to age, sex, gender, race, ethnicity, and medical specialty. The following four questions asked participants about how long they have been teaching medical students, contact hours with medical students in a given academic year, familiarity with the framework of cultural humility (definition provided), and strategies they use for helping medical students develop their cultural humility skills (e.g., lectures, simulations, small group discussions). These questions were inspired by Weissman et al. 2005’s Cross-Cultural Care Survey, which aimed to assess residents’ self-perceived skills and preparedness in delivering cross-cultural care. 14 However, we did not utilize all items in the Cross-Cultural Care Survey or other existing surveys. We were particularly interested in the faculty’s familiarity with the framework of cultural humility and their strategies to help medical students develop these skills. The 5-point Likert Scale was used to rank the answers.
Interview Guide Development
At the end of the survey, participants who answered “somewhat,” “quite a bit,” or “very much” in terms of familiarity with the cultural humility framework were invited to participate in the qualitative interviews. We developed the interview guide by reviewing current literature and incorporating insights from content experts on our team. The guide included follow-up and probing questions to gain deeper insights into the participants’ experiences. Specific topics addressed how faculty developed their own cultural humility skills and their strategies for helping medical students develop their skills. After a formal pilot test with the first three interviews, we iteratively refined the guide based on feedback from both interviewers and interviewees. The complete interview guide is provided in Appendix B.
Data Collection
The survey was created in Qualtrics, a secure online application, and responses were recorded anonymously. The survey’s Qualtrics link was initially emailed to each department’s Chair and Administrative Assistant at Boston Medical Center (BMC). Informed consent was obtained when participants received the screening email, read the purpose of the study and the eligibility criteria, and completed the questions. We employed purposeful sampling for the qualitative interviews to ensure that we only included participants with a baseline familiarity with the cultural humility framework, facilitating focused insights on developing these skills. For the participants who opted in for the qualitative interview, the interviewer set up a password-protected online meeting time using the email provided. Interviews were audio recorded and transcribed verbatim in a deidentified manner. Audio files were then destroyed following the study period. This research study was deemed exempt by the Boston Medical Center, Boston University Medical Campus Institutional Review Board, and the Harvard Longwood Campus Institutional Review Board.
Inclusion/Exclusion Criteria
Participants were required to read the study information at the beginning of the survey and consent to answering the questions. Faculty needed to meet the following inclusion criteria: (1) Licensed attending-level medical doctor practicing at BMC; and (2) English-language speaking.
Statistical Analysis
Data was collected between January 12th and March 23rd, 2024. Only completed surveys from participants who consented and met the inclusion/exclusion criteria were analyzed. Data from non-responders were not collected, given the nature of the survey, as it was sent out broadly to all eligible BMC faculty. Descriptive statistics were computed for demographic characteristics and participant responses to survey questions, and the number of responses per category was included with their percentages.
Inductive coding generated codes that emerged directly from the responses provided by the participants in the interviews. A reflexive approach to thematic analysis was conducted, and the researcher’s interpretation of the data was used to identify emerging themes. Reflexivity in qualitative research requires interviewers to explore their personal beliefs and be aware of potential judgments during data collection and analysis. Researchers must immerse themselves in the participant’s experience and examine the participant-researcher relationship to ensure a more personal and less hierarchical interaction. 15 In this reflexive method, the investigator analyzes the gathered data to discern themes, seen as patterns of shared meaning.16,17 Therefore, two researchers may not have the same analysis and outcomes. Dedoose was employed to analyze and group the gathered data into codes, categories, and themes. Data collection and analysis were finalized once saturation was achieved and no new themes emerged after conducting 10 interviews. 18 No compensation was provided to participants.
Results
Demographic Characteristics
Summary of Participant Demographic Characteristics and Responses Regarding Cultural Humility.

Teaching Characteristics
Of the 49 participants, 37% (n = 18) have been teaching medical students for more than 20 years, 14% (n = 7) for 15-20 years, 14% (n = 7) for 10-15 years, 22% (n = 11) for 5-10 years, and 12% (n = 6) for less than 5 years (Table 1). When asked about how many hours were spent each academic year teaching medical students, 18% (n = 9) responded more than 200 hours, 10% (n = 5) reported 150-200 hours, 4% (n = 2) replied 100-150 hours, 33% (n = 16) said 50-100 hours, 26% (n = 12) stated 20-50 hours, and 11% (n = 4) answered less than 20 hours (Table 1). Regarding familiarity with the framework of cultural humility, 16% (n = 8) responded that they were very much familiar, 29% (n = 14) were quite familiar, 29% (n = 14) were somewhat familiar, 16% (n = 8) were a little bit familiar, and 10% (n = 5) were not at all familiar (Table 1). When asked to provide all possible strategies that they have used to help their students develop cultural humility skills, 69% (n = 34) used one-on-one instruction, 45% (n = 22) used feedback, 39% (n = 19) used reflections, 33% (n = 16) used small-group discussions, 16% (n = 8) used lectures, 8% (n = 4) used simulations, 6% (n = 3) large-group discussions, 4% (n = 2) used online modules, and 4% (n = 2) used research (Table 1). Of the eight participants who were very much familiar with cultural humility, 88% (n = 7) employed reflections, one-on-one instruction, or feedback to help develop their students’ cultural humility, while 63% (n = 5) used small group discussions.
Thematic Analysis
Of the 36 faculty invited to be interviewed based on their responses indicating they were at least somewhat familiar with the framework of cultural humility, 27.8% (n = 10) responded. The data analysis identified 20 codes through inductive coding of the 10 interviews, which resulted in three themes regarding how faculty work with their students to develop cultural humility: (1) Encourage learners’ curiosity about culture; (2) Early direct exposure to patients, and (3) Bringing in diverse learning perspectives (Figure 1). Considerations for designing cultural humility curricula.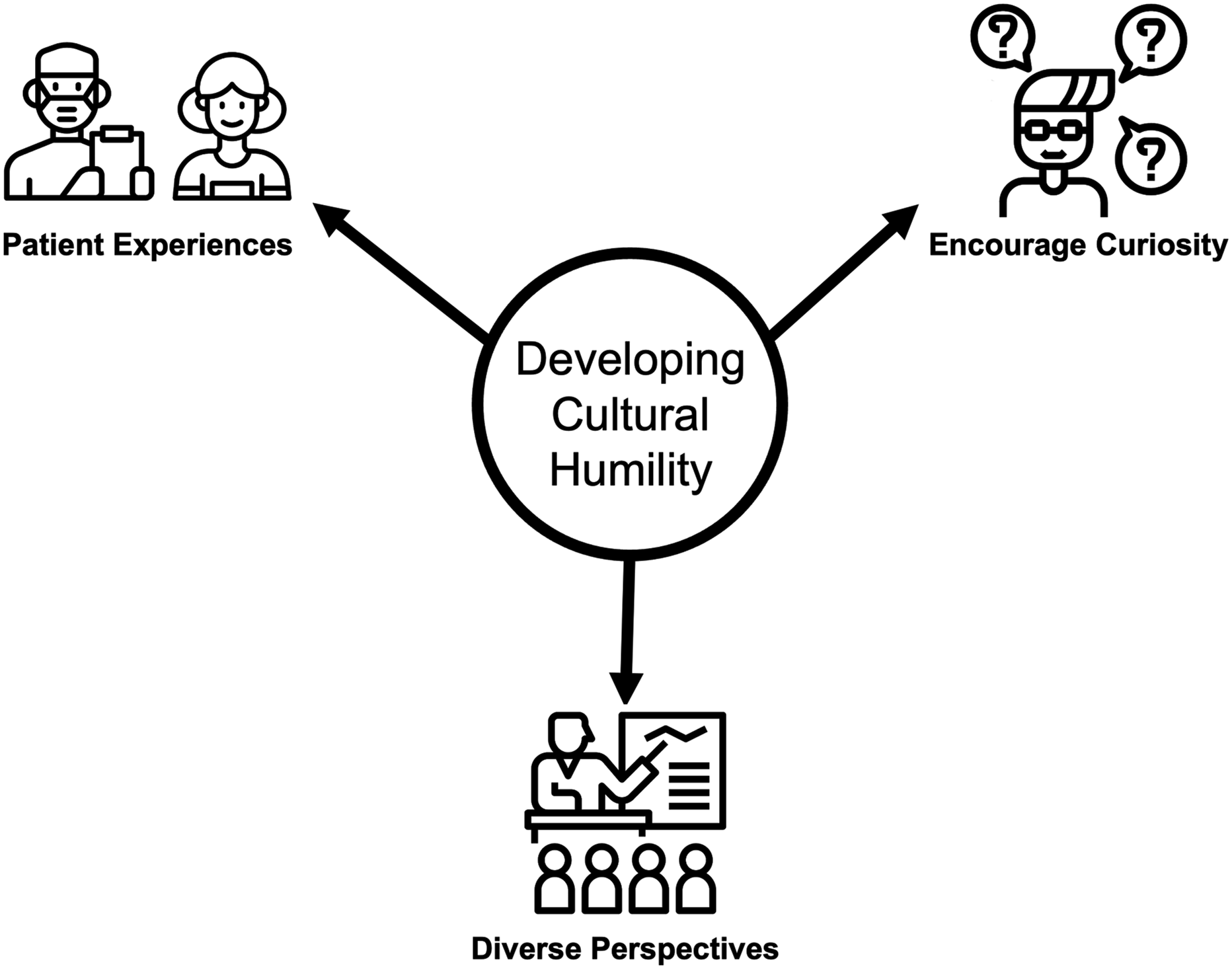
Theme 1: Encourage Learners’ Curiosity About Culture
Most participants mentioned how they developed their cultural humility skills through personal interest in improving the health outcomes of their minoritized patients. They suggest that students must be motivated to learn about other cultures before being taught specific strategies for providing culturally responsive care.
One participant described the utility of first motivating students to want to develop their cultural humility instead of focusing primarily on lectures or other content-specific tools. “I think, in most instances, it is not about the tools to educate people. It is about the motivation and the desire to develop cultural sensitivity. The incentives are very low and people don’t feel like investing time and energy into developing these skills…How can we motivate them rather than how can we expose them to educational material?”
Another participant similarly described how educational strategies to build cultural humility would only be effective depending on students’ receptiveness. “The didactics are only the beginning because they’re only as effective as the audience is willing to allow them to be effective.”
This same participant also commented on the resistance received when attempting to incorporate more cultural humility curricula for faculty and trainees. “There’s certainly resistance. I’ve met resistance to even accepting the concept that people’s unconscious biases alter the way they care for patients. Attendings come and tell me that they don’t see color and that they treat all patients the same. There is some eye-rolling sometimes when the grand rounds topic is on social disparities.”
Theme 2: Early Direct Exposure to Patients
Every participant stated that the main factor in developing their cultural humility came from directly caring for culturally diverse patients. They propose that students should be exposed early in their careers to caring for patients from different ethnic backgrounds.
One participant remarked how experience caring for culturally diverse patients is more valuable than lectures or readings. “Developing this type of skill [cultural humility] requires exposure. I don’t think it is something that can be just taught by reading a book or having conversations. Rather, it must be in an environment where you are exposed to patients of different backgrounds. And ideally, it should be an environment where you are the minority.”
Another participant similarly mentioned that making mistakes through experiences with different patients helps build cultural humility. “The most important thing of all that helps our students develop [cultural humility] is just practice. You need to be humbled a whole bunch of times where you walk in thinking you know what you’re doing, and then it turns out to be totally different. You can’t take shortcuts, because you’ll just fail constantly if you’re making assumptions.”
This same participant went on to note that these patient experiences should also be longitudinal so that students could observe the effect of culturally sensitive care on health outcomes. “If students have longitudinal experiences where they’re responsible for patients, you get to know a family, and you figure out what’s going on with them. It’s like an empathogenic experience because they become your people. You’re very much seeing their world and medical experiences from their perspective.”
Another participant stated that these health outcomes would be impactful in showing faculty and trainees the importance of cultural humility in improving patient care. “We have been able to measure how language and race and gender concordance improves health care outcomes. If you could create a measure of cultural humility, and then see if that measure of cultural humility improved healthcare outcomes, that would be your home run.”
Theme 3: Bringing in Diverse Learning Perspectives
Many participants spoke about the importance of recruiting more diverse residents and faculty to their programs. This diversity in learning perspectives will broaden students’ understanding of, and ability to empathize with, various cultures.
One participant mentioned how they would like to include more faculty of color in giving presentations on healthcare disparities and bias-related topics. “I think what needs to be incorporated in my curriculum is more diverse faculty because this coming from me is, it is not an intuitive sell. I think having a [Black resident] give his grand rounds on disparities or the experiences of Black patients in the healthcare system or a Muslim to talk about the experiences of a Muslim in the healthcare system. You really need that person to give that talk. I can’t give that talk. It just doesn’t work.”
Another participant who identified as White talked about how colleagues from different backgrounds have helped them better understand and empathize with their patients of color. She recalled learning more about vaccine hesitancy in the Black community from one of their Black colleagues. “The COVID vaccines and vaccine hesitation I logically understood. But I didn’t really feel it. I know people are distrusting of the system because of Tuskegee. I could answer it right on a test, but I didn’t really get it until I saw [a Black] highly esteemed physician that I regard as a role model speaking to students one time. The first words out of her mouth were, ‘When that vaccine was introduced, I wasn’t so sure about it.’ And I was shocked.”
Discussion
In our multimethod study, we fill a gap in the medical education literature by identifying the strategies faculty use to develop medical students’ cultural humility skills in the clinical setting. We found that most faculty are aware of and value the framework of cultural humility, recognizing its importance in providing care to diverse patient populations. Faculty emphasize the significance of motivating students to develop their cultural humility skills, early direct patient exposure, and the need for more diverse faculty and trainees in medicine. These practices contribute to clinical excellence and play a crucial role in reducing healthcare disparities and improving patient outcomes.
Encouraging Learners’ Curiosity About Culture
Educators can employ several strategies to instill cultural humility in medical students and motivate them to be curious about culture. For instance, participation should be encouraged in cultural immersion experiences, e.g., global health initiatives or community service, to develop empathy and cultural curiosity. 19 One participant recounted how their travels to West Africa during residency enabled them to collaborate with physicians in Liberia, gaining an appreciation for how medicine is practiced within different cultural contexts. Such experiences can foster empathy and interest in diverse cultures.
While immersion experiences can enhance students' cultural sensitivity, clinical skills, and exposure to global health challenges, these programs raise ethical concerns about their quality and sustainability. 20 Learners working beyond their expertise often experience moral distress, potentially compromising patient care, while one-sided partnerships and reliance on foreign volunteers can erode trust in local healthcare and discourage sustainable investment, deepening health inequities when volunteers depart. 21 Designing effective immersion programs requires training students to critically examine and address colonial influences on global health. 22 Programs should foster long-term, bidirectional partnerships that strengthen local healthcare systems and address root causes of inequities, avoiding short-term fixes and emphasizing sustainable, measurable community health gains. 23
Cultural humility courses and workshops should incorporate metacognitive reflection on personal biases. 24 Ogunyemi et al. (2024) reported that their 90-minute interactive reflective workshop offered both in-person and virtually increased participants’ understanding and awareness of cultural humility principles. 25 Of the eight participants in our study who were very much familiar with the framework of cultural humility, seven reported using reflections to guide the development of their students’ cultural humility skills. Everyone has subconscious preconceptions and stereotypes that can influence their interactions and understanding of different cultures. By bringing these biases to the forefront of consciousness, students can begin to address and mitigate their impact. 26
Additionally, patient cases involving cultural considerations can stimulate critical thinking and discussion. 27 Balzora et al. (2015) designed an Observed Structured Clinical Examination (OSCE) for gastroenterology fellows involving three cases to assess how learners handled culturally sensitive issues. 28 Their assessment revealed some significant gaps, including the fact that only 18% of students recognized the standardized patient’s low health literacy. In our study, one participant noted that familiarity with diverse cultures aids in making tailored recommendations, especially in dietary advice for conditions like iron deficiency anemia. Engaging patients in conversations about their typical foods and suggesting culturally relevant iron-rich options is more effective than providing generic food lists. Medical students should be encouraged to research and present on cultural aspects of healthcare relevant to the patients they see. Educators should make an effort to invite diverse patients to share their experiences with the healthcare system, making cultural issues tangible and relatable. 29
Early Direct Exposure to Patients
Cultural humility skills take time to nurture and grow. Longitudinal training must be implemented in the medical curriculum for continuous exposure to cultural humility concepts. 30 One participant described how longitudinal experiences enable their students to adopt the patient’s perspective and get to know their family and circumstances, creating a profoundly empathogenic experience. As noted by most of our study participants, hands-on experiences in diverse settings, like urban or rural clinics, should be provided to students for practical skills development. 31 Another participant emphasized that cultural humility cannot be taught solely through books or lectures. Instead, it must be learned in an environment that provides exposure to patients from diverse backgrounds, including immigrants, uninsured individuals, and those from various cultures.
Early clinical exposure programs, however, face challenges in balancing clinical experience for students with foundational education, ensuring patient safety and confidentiality with novice learners, and supporting student well-being, particularly for those who do not have much clinical exposure. 32 Additionally, limited patient diversity can hinder the development of cultural humility, while students’ concerns about knowledge gaps, fear of mistakes, and readiness may affect their confidence, commitment, and sense of vocation in medicine. 33
Group discussions and regular feedback should be encouraged to help identify opportunities for personal growth as students progress through medical school. 34 Seven of the eight participants in our study who were very much familiar with the framework of cultural humility described one-on-one instruction and feedback as essential strategies they used with their students to enhance their cultural humility skills. Five of these eight participants also incorporated small group discussions in their student education. Cultural humility curricula should include mechanisms for regular feedback, allowing participants to understand the effects of their biases and track their progress over time. This goal could be met through peer feedback, self-assessment, or facilitator evaluations. Mentors who exemplify cultural humility should be assigned to students to offer guidance and role modeling. 35 One participant remarked that observing students with patients or in role-play scenarios and providing immediate feedback effectively improves the students’ cultural humility skills. However, another participant noted that the lack of personnel makes it challenging to offer timely observation and feedback.
Furthermore, cultural humility assessments do not only provide valuable information about the effectiveness of the curriculum, but they can also be a motivational tool for students, encouraging a mindset of continuous self-improvement and learning. 36 Similar to the lack of assessment described in anti-racism curricula, one participant mentioned the challenge of evaluating the effectiveness of cultural humility training, noting the absence of outcome measures for the hidden curriculum. 37 They expressed uncertainty about its success due to the lack of supporting data, relying instead on subjective perceptions of interactions. Another participant suggested that creating a measure of cultural humility and linking it to curricula with improved healthcare outcomes would be ideal for student education.
While many cultural competency studies have reported positive changes in student awareness or knowledge, assessment methods were often vague, relied heavily on self-reporting, and frequently lacked a well-defined process for measuring changes in cultural competence. 38 Objective assessment approaches could provide more meaningful insights. For example, third-year medical students at SUNY Upstate Medical University participated in a one-hour cultural competence and humility intervention that used case examples and reflective exercises to emphasize self-evaluation, the culture of medicine, and power dynamics in clinical encounters. 39 This study distinctively emphasized behavior change in actual patient interactions rather than traditional post-intervention assessments of knowledge or attitudes. Supervising physicians observed that students who completed the course displayed enhanced competency in “relating to patients in a respectful, caring, empathetic manner” during clinical encounters.
Bringing in Diverse Learning Perspectives
Incorporating diverse instructors who can train students in cultural humility is vital for several reasons. Diverse faculty members serve as invaluable role models, offering students tangible examples of cultural humility in practice. 40 They bring a wealth of diverse viewpoints to the educational setting, enriching the learning experience and helping students grasp the complex nature of cultural interactions in healthcare. 41 For instance, lecturers with lived experiences, such as those with disabilities or from the LGBTQ + community, can enhance students’ cultural humility by providing authentic insights that deepen understanding and encourage engagement with diverse patient populations. 42 One participant in our study shared a personal experience of better understanding vaccine hesitancy after hearing a respected colleague express initial doubts about the COVID-19 vaccine. This revelation helped the participant empathize with the mistrust people from specific communities feel toward the healthcare system.
Faculty diversity also fosters an inclusive learning environment, where students feel represented and are more receptive to learning about different cultures. 43 This inclusivity is not just about comfort but also about creating a space where cultural humility can be effectively taught and internalized. Moreover, interactions with faculty from varied backgrounds can significantly improve students’ communication skills, especially in cross-cultural scenarios. One participant recalled how one of their patients was repeatedly resistant to a new surgical treatment. The participant explained the need for patience and understanding to their team, drawing from their culturally-influenced apprehensions when they needed surgery. Diverse teachers encourage students to engage in self-reflection and personal growth, challenging their preconceptions and biases.27,44
While bringing in faculty from different backgrounds is valuable, students are calling for more actionable approaches to address health inequities. 45 The Keck School of Medicine, for example, introduced a Health Justice and Systems of Care curriculum, which incorporates health systems science, structural competency, and service-learning across required courses in both pre-clerkship and clerkship phases, with an optional post-clerkship elective. 45 Although students generally provided positive feedback on discussions with guest speakers, they expressed a need for more concrete, practical examples of addressing health inequities in clinical settings.
The presence of diverse faculty has a profound long-term impact on healthcare delivery. Students trained in diverse, culturally sensitive environments will likely become culturally sensitive healthcare providers, leading to more equitable healthcare delivery and improved patient outcomes. 46 Furthermore, the diversity among faculty is beneficial and essential in shaping a healthcare workforce that practices humility, demonstrates empathy, and is well-equipped to address the diverse needs of patients.
Responsibility of Educators
The responsibility of diversity and inclusion work often falls upon minoritized faculty because their experiences from specific communities are perceived to make them more qualified to speak on these topics. However, any educator, regardless of background, can effectively teach cultural humility, if committed to continuous learning. By broadening the responsibility of teaching cultural humility to all educators, institutions can ensure that this critical aspect of medical education is embedded throughout the curriculum. This approach not only alleviates the burden on minoritized faculty but also enriches the learning environment for students, preparing them to provide culturally sensitive care in their future practice. As Acholonu et al. (2020) suggested for anti-racism teaching, faculty members who are eager and committed to engaging in anti-racism efforts should be trained, ensuring those most equipped and motivated are teaching these vital topics. 47 Ongoing faculty development is essential for fostering students’ cultural humility, with long-term, research-based training supporting alignment between the curriculum, faculty development, and the needs of patients and society. 48
Limitations and Future Research
This study has several limitations, including a small sample size from one institution, reliance on self-reported measures subject to social desirability bias, a cross-sectional design limiting causal inferences, and a focus on faculty perspectives without directly assessing student outcomes or patient care. Additionally, the 27.8 % response rate from participants may suggest a potential for nonresponse bias, as the responses may not fully represent the views or experiences of the entire target population. However, in qualitative research, the focus is on the depth and richness of the data rather than the size of the sample or response rate. 49 This approach was particularly important when we explored the framework of cultural humility, where capturing the intricacies of experiences and nuanced attitudes was prioritized over breadth and generalization. 50
Future research should address these limitations by using larger, diverse participant samples from different institutions and regions, conducting longitudinal studies to track the development of cultural humility over time, and creating objective assessments of cultural humility. Further studies are needed to explore the effectiveness of different curricular approaches to teaching cultural humility, such as experiential learning, metacognitive reflection, and interprofessional education. Content analysis of the most commonly used strategies, especially among those most familiar with cultural humility, will help inform curriculum building. These strategies should be assessed for their impact on students’ self-awareness, empathy, and ability to provide culturally sensitive care. Furthermore, examining the challenges and barriers to implementing cultural humility training in medical education and identifying strategies to overcome these obstacles is essential to cultivating cultural humility among medical students and improving healthcare delivery for diverse patient populations. Our study’s findings, while specific to a single institution’s faculty, offer preliminary insights. A more extensive investigation across multiple medical schools would help validate these observations and establish best practices.
Conclusion
Identifying the strategies faculty relevant to the study use to nurture medical students’ cultural humility skills in clinical settings is necessary to facilitate the development of more effective cultural humility curricula. Through focused semi-structured interviews and subsequent thematic analysis, we found that the faculty in our study emphasized the importance of early patient exposure, motivation for cultural humility, and diverse medical teams for helping medical students develop their skills. Strategies include cultural exposure, integrated curricula, case-based learning, guest speakers, longitudinal experiences, self-reflection, mentorship, and assessments. These practices embed cultural humility into medical education and professional identity, contributing to a more equitable and effective healthcare system that respects diverse patient populations.
Supplemental Material
Supplemental Material - Examining the Role of Medical School Faculty in Developing Students’ Cultural Humility Skills: Insights From a Single-Center Multimethod Study
Supplemental Material for Examining the Role of Medical School Faculty in Developing Students’ Cultural Humility Skills: Insights From a Single-Center Multimethod Study by Dhanesh D. Binda, Angelique C. Harris, Taralyn Tan, Krisztina Fischer, Rose L. Molina, and Darshan Mehta in Global Advances in Integrative Medicine and Health.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
