Abstract
Background
Given limited yoga research in health disparities populations, we developed and evaluated a 12-week Spanish language yoga program for Latiné women with overweight or obesity affected by cancer. The program aimed to empower participants through culturally tailored yoga practice and opportunities for social connection and support.
Methods
Partnering with a community-based organization, the program was co-created by bilingual (English and Spanish-speaking) yoga instructors, Latiné cancer survivor support professionals, and integrative medicine researchers. The single arm intervention consisted of 12 separate, 60-minute Hatha yoga classes, including physical postures, breathing exercises, culturally relevant poetry, and post-practice socialization opportunities. Measures were administered at baseline, 12-week, and 24-week.
Results
Thirty-five eligible participants enrolled in the program, demonstrating high feasibility and relevance as well as high levels of engagement in home practice. Some participants faced barriers to regular home practice, including family responsibilities and concerns about proper pose execution. Preliminary outcome analyses indicated improvements in sleep disturbance, pain interference, depression, and blood pressure post-intervention, with sustained improvements in depression, anxiety, and blood pressure at 24-week. No significant changes were observed in fatigue, physical function, positive affect, satisfaction with social roles and activities, and weight. Structured post-practice social snack time with yoga instructors (compared with unstructured time with peers) was associated with self-reported improvements in satisfaction with social roles and activities and weight loss.
Conclusion
This yoga program successfully engaged female Latiné cancer survivors with overweight and obesity and serves as a foundational step in empowering this population to improve their health and well-being through culturally tailored yoga practice. Future research should utilize controlled study designs and engage participants from different geographical regions to study the efficacy and sustainability of findings.
Introduction
Despite growing public health efforts, health disparities continue to afflict different racial/ethnic groups in the United States, especially those facing language barriers. 1 Individuals with Latin American ancestry are 1.2 times more likely to be obese 2 and have the highest prevalence of physical inactivity comparted to other racial/ethnic groups.2,3 Latiné women are disproportionately affected by obesity compared to non-Latiné white women (79% vs 64%, respectively 2 ), often due to variations in socioeconomic status and inequities in healthcare (e.g., language barriers, lack of Latiné providers) and healthcare management. 4 Recent research has also shown that environmental factors, such as birth place and length of stay in the U.S., may play an influential role in increased obesity prevalence. 5 Consequently, obesity-related diseases are on the rise among members of the Latiné community, including heart disease, type 2 diabetes, and non-alcoholic fatty liver disease.4,6 Obesity is a key component of metabolic syndrome, the cluster of metabolic abnormalities (e.g., obesity, dysglycemia, high blood pressure) recognized as risk factors for type 2 diabetes, fatty liver disease, and atherosclerotic vascular disease, all of which are growing problems in US Latiné populations.7-9
Among members of the Latiné community, obesity and chronic stress have often gone hand in hand and have been associated with a host of economic, cultural, environmental, and lifestyle factors, such as financial insecurity, unemployment, poor access to healthcare, and social isolation. 5 For immigrants of Latiné descent, acculturative stress (stemming from language barriers, racism/discrimination, dietary changes, foreign customs, income inequality, separation from family, and fear of deportation) can also be a significant source of chronic stress and increased risk of obesity and being overweight.10,11 Furthermore, the combination of chronic stress and obesity increases risk for many types of cancer.12-14
One non-pharmacological mind-body practice that has demonstrated meaningful improvements in mental and physical health outcomes is yoga. Several recent meta-analyses have reported on the safety and physical and mental health benefits of yoga practice across a host of different medical conditions, including the reduction of: (1) pain intensity in low back pain suffers 15 ; (2) symptoms of depression, anxiety, and sleep problems in rheumatic disease 16 ; (3) depressive symptoms in individuals with major depressive disorder, 17 and (4) improvement in physical and psychological benefits in Parkinson’s disease. 18 Numerous recent meta-analyses have also focused on yoga’s beneficial role in improving cardiovascular risk factors in Type 2 diabetes,19,20 lipid profiles in metabolic disorders, 21 and weight-related outcomes in patients with obesity. 22 Lastly, recent meta-analyses have also confirmed the beneficial role of yoga practice during cancer survivorship on decreasing symptoms of depression and anxiety 23 and cancer-related fatigue. 24
An additional benefit of yoga practice reported by oncology patients includes feeling supported during treatment through fostering connections with other patients and having encouraging and knowledgeable instructors.25,26 Research on collaborative activities during yoga practice has highlighted yoga’s impact on social satisfaction through building positive relationships with peers, especially through shared conversation. 27 Yoga practice has helped improve social connection and decrease feelings of loneliness through the shared social environment. 28 For cancer survivors this can include shared experiences about bodily changes, enduring similar procedures, etc., all of which can positively influence participation rates. 29 However, yoga-based social support does not only stem from peer-to-peer interactions, but also from instructors who are supportive and help create a safe, inclusive and soothing environment. 29 Recommendations for future yoga interventions with cancer survivors have thus included “more than just physical movement;” by facilitating discussion and group meetings among participants where cancer patients can benefit from socializing with others, maintaining friendships, and providing support to one another. 29
While evidence supporting the mental, physical, and social health benefits of yoga is growing rapidly, few studies have focused on Latiné populations 3 and still fewer have addressed barriers to accessibility. Depending on different cultural, linguistic, and economic factors, many members of the Latiné community have faced barriers accessing healthcare services in general let alone integrative services such as yoga.30,31 Data has shown that roughly 52% of Latiné adults report annual household incomes of < $40,000 vs 29% of non- Latiné White adults and 78% of potentially undocumented immigrants report annual household incomes < $40,000 compared to 40% of U.S.-born Latiné adults. 32
Considering these economic disparities, the most prominent barriers to yoga practice in Latiné communities has been the perception of cost, followed by concerns about feeling like a stranger in class 3 or that yoga practice is associated with individuals of higher economic and educational status. 30 In addition to financial barriers, cultural-linguistic barriers present other challenges. Members of the Latiné community with limited English-language proficiency and acculturative stressors are often excluded from culturally appropriate psychosocial interventions in oncology care. 33 As Spanish is the most common language spoken after English, 2019 data revealed that 71.1% of Latiné individuals speak a non-English language at home and 28.4% are not fluent in English. 31 Offering yoga in Spanish at no cost, with additional supports for transportation, parking, family involvement, and community-building may not only encourage and increase yoga participation among minoritized communities but also establish feelings of safety and satisfaction.31,34
Given yoga’s potential for improving mental, physical, and social wellbeing, its growing popularity, and its unique contemplative, bodily, social, and spiritual components, yoga may serve as an effective mind-body health intervention for Latiné populations diagnosed with cancer, especially among those experiencing overweight and obesity. Research reports35,36 indicate that perceptions of the research community’s lack of understanding of cultural differences contributes to decreased rates of minoritized research participation, while cultural congruence promotes participation. Employing a community-engaged research approach to this work can help assure that community perspectives and considerations are built into the design, delivery, and implementation, ensuring that issues of participation, access, utilization, privilege, power, and cultural contexts of race and ethnicity are not left out, whether implicitly or explicitly.
The following study sought to develop and pilot test a culturally informed yoga program designed specifically for non-English speaking Latiné women diagnosed with breast cancer using a community-engaged research approach. This included an evaluation of the program’s feasibility and acceptability; perceived preferences, barriers, and facilitators, and early exploration of target outcomes (e.g., health-related quality of life, psychosocial wellbeing, weight loss and related cardiovascular disease risk factors), as well as the potential beneficial role of different types of peer and instructor-provided support.
Methods
This study was funded by a pilot grant from the Osher Center for Integrative Health at Northwestern Medicine and approved by the Institutional Review Board at Northwestern University (STU00102767). It was conceptualized, designed, and conducted in close partnership with ALAS -Wings (ALAS), a Chicago-based non-profit organization dedicated to empowering Latiné women about breast cancer awareness through comprehensive education and support, and resources for all women faced with a breast cancer diagnosis and survivorship. ALAS has established strong relationships with cancer centers, major hospitals, and community organizations throughout Chicagoland that provide support for uninsured and underserved Hispanic/Latina women and their families. ALAS distinguishes itself from other breast cancer organizations by offering personalized, vital services in every phase of the breast cancer journey, from diagnosis through survivorship.
Consistent with community-engaged research principles, 37 a memorandum of understanding (MOU) was created and signed by Northwestern University (NU) author DV and ALAS author JG, which emphasized a model of shared, bi-directional communications and decision making, trust, respect, co-education and capacity building, and conflict resolution strategies. This study included two distinct phases, each of which is described below.
Phase I: Partnership and Yoga Intervention Development
Phase I involved multiple meetings between ALAS and NU team members to discuss ways to acceptably modify the structure of the ALAS community yoga program into a more standardized, IRB-approved yoga research study that still retains its flexibility, accessibility, and community feel. It also included training in research ethics and human subjects protection by all team members; discussions about research design, intervention development, standardization, and fidelity; Latiné-specific conversations and trainings about important linguistic, cultural, and cancer-specific considerations to keep in mind; decisions about yoga program duration, intensity, length, flow, inclusion/exclusion criteria, instructor qualifications and characteristics, and culturally-informed ways to support adherence, participation, and encourage home practice.
We engaged in a series of meetings with a group of Spanish-language yoga instructors (most with specific training and experience in the delivery of yoga to cancer survivors) to create a program curriculum and identify core yoga poses that would be safe and achievable for cancer survivors across the adult age span, with a specific focus on women diagnosed with breast cancer given the population that ALAS serves. Meetings included basic education on breast cancer, common treatments and side effects, and physical areas to be aware of, including the arms, armpits, and chest, given potential sensitivities due to surgeries, lymphedema, and/or continued use of a chemotherapy port. As a group we addressed the following areas of yoga program development based on recommendations by Sherman. 38
Yoga Style
Hatha yoga was selected as the yoga style for its prioritization of stability, grounding, flexibility, balance, and strength, including its ability to be tailored to the physical needs of breast cancer patients and survivors. 39 Hatha yoga involves holding postures for a few breaths and emphasizing individual postures rather than the sequence or transitions between them, thus making it particularly suitable for beginners. The practice unfolds at a slower pace, allowing practitioners to dedicate ample time and attention to achieving proper alignment in each pose.
Dose and Delivery
Through an iterative, consensus generating approach, the team identified 40 breast cancer safe and relevant poses that would be available for instructors to use during the course. This allowed some level of standardization in poses yet offered instructors flexibility to tailor each class based on participants’ needs. Each class consisted of 60 minutes of yoga practice with a 30-minute healthy “social snack” period immediately following, occurring once each week for 12 consecutive weeks.
Intervention Components
Physical postures (asanas) were the primary components of each class, complemented by breathing exercises (pranayama) and select contemplative quotes and poetry that were translated into Spanish from authors such as Mother Teresa, Ghandi, and the Tao Tei-Ching. A 30-minute social snack period was also offered immediately following classes. The first two 12-week cohorts received informal, unstructured conversation opportunities among peers and instructors. When yoga instructors noticed that these post-yoga social exchange sessions might be good opportunities for more structured reflection, it was decided that the second two 12-week cohorts would receive more formal, structured conversations that were facilitated by instructors where they were asked reflective questions about what they were noticing and observing about their experiences in the course.
Course and Class Sequencing
Each weekly class centered on a different theme, including: 1) Breath of Life, 2) Listening to the Body, 3) Self-Compassion, 4) Emotion: Shifting Energy, 5) Beginners Mind, 6) Moving Toward Stillness, 7) Yoga Every day, 8) Sensing the Strength of Your Body, 9) Cultivating Joy, 10) Acceptance, 11) The Journey, and 12) Letting Go. Poetry corresponded with each class theme.
Selected Poses by Class Phase.

Using this information, yoga instructors were given an instructor manual for training and implementation purposes, a pose sequencing/tracking worksheet to document what was done in each class, and a semi-structured social snack time discussion guide for post-class interaction.
Yoga Instructors
All instructors were certified to teach yoga, and many had previous training and experience teaching yoga to cancer survivors. All were fluent in Spanish but not all were of Latiné decent. Even though the target population for this study was women given the mission of ALAS, since ALAS has already successfully worked with male yoga instructors in their breast cancer yoga classes, it was decided that both male and female yoga instructors would be invited to teach so long as they could speak Spanish.
Working With Modifications
Pose modifications (e.g., using a chair instead of the ground) in order to meet the physical needs of participants were expected and encouraged.
Home Practice Facilitation
Example Poses and Descriptions From Participant Workbook.

Intervention Fidelity
Several mechanisms were in place to monitor and increase intervention fidelity, including: (1) Development of an instructor’s manual of procedures, (2) Half-day training with yoga instructors to review the curriculum and ensure the protocol adequately addressed their needs, (3) 30-minute bi-weekly calls with yoga instructors to adjust the curriculum due to unforeseen challenges and ensure successful data collection, and (4) Use of a pose checklist where instructors were asked to mark which poses were included in each class.
Phase II: Yoga Intervention Implementation and Evaluation
Participant Enrollment and Eligibility
During Phase II, flyers, newsletters, and website announcements were used to enroll between 30-40 eligible breast cancer participants at ALAS locations into one of four different 12-week yoga programs. While our target population was breast cancer patients and survivors given the mission of ALAS, to be inclusive we allowed any eligible cancer survivor to enroll, as well as any identified caregivers/supporters (male or female) to also participate in classes. Given the scope of this current study we only present data from female cancer survivors in this report but provide basic descriptive information about any caregivers/supporters who attended. Eligible participants were required to be at least 18 years old and report speaking Spanish at home as their primary language. Cancer survivors were required to meet minimum criteria for overweight (BMI ≥25) and elevated blood pressure (systolic ≥121 and/or diastolic ≥80), self-report ability to perform basic activities of daily living, and ability to consent. While experiencing stress and fluctuating symptoms of depression and anxiety can be normal for cancer survivors, we asked that referring community partners (who generally knew eligible participants from previous programs) consider participants’ overall emotional wellbeing and whether they felt that their participation in an intensive, multiweek, group-based program like this may put them at increased risk of experiencing undue psychological distress given their knowledge of them. If so, the research team would meet to discuss on a case-by-case matter. Exclusion criteria included being bedridden or experiencing physical debilitation such that participation would not be feasible or cause undue hardship. Additionally, regular yoga practitioners (≥3 times/week in the past 2 weeks) were not eligible.
Yoga Intervention
The final yoga intervention consisted of 12 consecutive once-weekly classes, delivered at a convenient community location, such as a place of worship, community center, or within a medical facility. Each class included 60 minutes of yoga practice and 30 minutes afterward for a social snack period. Each class, instructed in Spanish, drew from a standardized pool of up to 40 different Hatha yoga-based poses, delivered across the class phases: Warm-up, Active, Deep Release, and Closing, which were selected to be appropriate for the different ranges of flexibility and strength among participants.
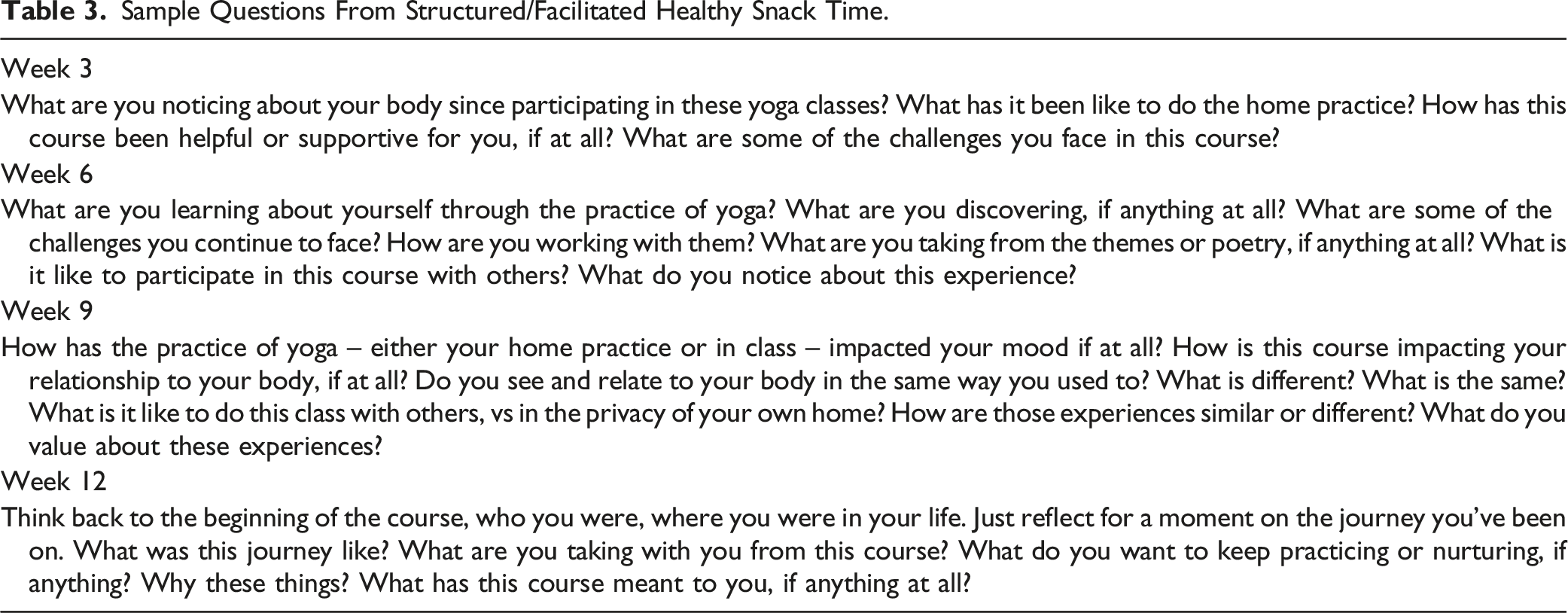
Sample Questions From Structured/Facilitated Healthy Snack Time.
Promotion of Adherence and Retention
To promote adherence and retention, participants were called the day before each class, and invitations were extended to any care provider wishing to participate in the classes (only data from female survivors was included in analyses). Transportation assistance (e.g. bus passes, taxi cash stipends, and carpooling) was also provided to participants who used public transportation. Participants who lived near one another were encouraged to carpool to class. Attendance was monitored, and absent participants were called in order to check in on them and welcome them back.
Study Design and Data collection
Consented participants were enrolled into a non-randomized single arm pilot study with repeated measurements over a 3-month period. All study measures (described below) were available in English or Spanish, consistent with participant preference. Baseline (T1) measures were administered following consent and immediately before the first session and included: basic sociodemographic (e.g. sex, race, ethnicity), clinical information (e.g. date of diagnosis, co-morbidities) and intervention expectancy/credibility. All responses were self-reported. No medical chart review was conducted. All other patient reported outcome (PRO) measures were administered at T1 as well as immediately following the 12-week intervention (T2), and at 3-month (T3). PRO measures were administered by a research coordinator in person or via telephone, in either English or Spanish, consistent with participant preference. Blood pressure (measured manually with a blood pressure cuff and stethoscope) and whole blood spots (collected with a finger prick lancet to examine levels of C-reactive protein and Interleukin-6) were also obtained by trained research coordinators at all time points, however these blood spot data are beyond the scope of this report and will be presented elsewhere. Weight and height (used to calculate BMI) were also recorded. Participants were weighed privately in a closed room by a trained, female Latiné study coordinator.
Measures
In addition to measuring blood pressure and weight, PROs included assessments of intervention acceptability, preferences and barriers, expectancy, and domains of physical, mental and social health.
Safety, Feasibility and Acceptability
Safety was monitored by any patient or instructor reports of any yoga practice-related injury. Feasibility was operationalized by the following metrics and milestones: (1) ≥ 70% class attendance on average, (2) ≤ 30% attrition, and (3) ≥ 70% of some engagement in home practice (logged throughout the 12-week course by participants) on average. Acceptability was operationalized by: (1) ≥ 70% of some reported home practice during the follow-up period (between weeks 12 and 24), (2) ≥ 70% of participants endorsing either “good”, “very good” or “excellent” on the T2 acceptability item, “Please rate your overall experience in the yoga program” using a 5-point Likert scale from poor to excellent.
Expectancy/Credibility
The Expectancy Credibility Scale 40 measures expectations of treatment efficacy and perceived credibility of the rationale for the intervention. This measure consists of 6 items on which respondents rate their beliefs (thoughts and feelings) about the ability of the yoga program to improve their health. Four items used 9-point Likert-type scales (1 = not at all, 9 = very), and two items used 10-point scales from 0% to 100%, incrementing in 10% intervals. This measure was evaluated as a possible covariate in outcome analyses.
Yoga Program Preferences, Motivators, and Barriers
Several items were administered at T2 that focused on participant preferences, motivators, and barriers to participation. Eight items rated participant course-related preference on 5-point Likert-type scales (0 = Not at all important, 4 = Extremely Important) which included statements such as, “If possible, I prefer that my yoga instructor can speak Spanish” or “If possible, I prefer that my yoga instructor is the same sex as me.” One item focused on participants’ primary motivation to continue coming to classes, while another asked about their perceived frequency of practice needed in order to experience benefit. Participants were asked to select their top 3 favorite yoga poses of sixteen images of course yoga poses (6 warm-up, 3 active, 4 deep release, and 3 closing). Relative importance of course components, home practice, social support, challenges to participation, and instructor satisfaction were also reported (11 items).
PROMIS
PROMIS 41 short forms for Anxiety (7 items), Depression (8 items), Fatigue (7 items), and Pain Interference (6 items) requests that respondents rate symptoms in the past seven days on 5-point Likert-type scales. For Sleep Disturbance (8 items) and Satisfaction with Social Roles and Activities (9 items) short forms, respondents rate frequency of experiences on 5-point Likert-type scales (1 = Not at all, 5 = Very much). The 10-item Physical Functioning short form rates current ability to complete activities on a 5-point Likert-type scale (5 = Without any difficulty, 1 = Unable to do). The Neuro-QOL Positive Affect and Well-Being short form 42 (within the PROMIS system) consists of 9 items rating frequency of experiences “lately” on a 5-point Likert-type scale (1 = Never, 5 = Always). These measures were examined for potential improvement over time.
Blood Pressure and Weight
At all assessment timepoints we measured systolic and diastolic blood pressure using a stethoscope and blood pressure cuff. Participants were assisted in sliding their left arm through the cuff, positioning it .5-inches above the elbow, and securing it with Velcro material. They placed their arm on a table so that the cuff was positioned at the same level as their heart. Weight was measured using a standard calibrated scale.
Data Analysis
SPSS 29 was used in all analyses. Descriptive statistics and frequencies were calculated for socio-demographic, clinical, feasibility, acceptability, and preferences/barriers data. These data include scaled responses to course experience items as well as quantified attendance and home practice both during and after the course. Covariates included expectancy and total number of sessions attended. Pearson correlation coefficients were used to examine the level of association between covariates with change scores in PROMIS measures, blood pressure, and weight.
PROMIS measures, blood pressure estimates, and weight values were analyzed using repeated measures analysis of covariance (ANCOVA) using the mixed-model approach to examine possible improvement over time. In a nonrandomized design, a General Linear Model was used to compare outcomes between courses that only had unstructured snack time (Unstructured) vs those that included instructor-led structured reflection healthy snack time (Structured). For all analyses, Cohen’s d effect sizes 43 were estimated to interpret the magnitude of change for statistically significant (P < .05) findings (small effects between .2-.4; medium effects between .5-.7, and large effects ≥.8), using the pooled standard deviation and adjusting for the intercorrelation of both groups per recommendations from Lakens (2013). 44
Results
All data were collected between the spring of 2015 through the spring of 2016. A total of 58 cancer survivors were approached, resulting in the enrollment of 36 women (62% enrollment response rate). One participant dropped out prior to the baseline assessment. Eleven male caregivers enrolled with an average age of 40.1 (SD = 9.8); the majority of whom reported being born in Mexico (64%) being married (64%), being employed (55%) and earning less than $35,000 in annual income (73%). Most caregivers completed the study (73%) and attended 7.7 sessions on average. All data in this current analysis reflect the 35 participants who provided T1 information. See Figure 1 below for study flow of cancer survivor participants. Non-randomized study flow of female cancer survivor participants.
Demographic Information (n = 35).

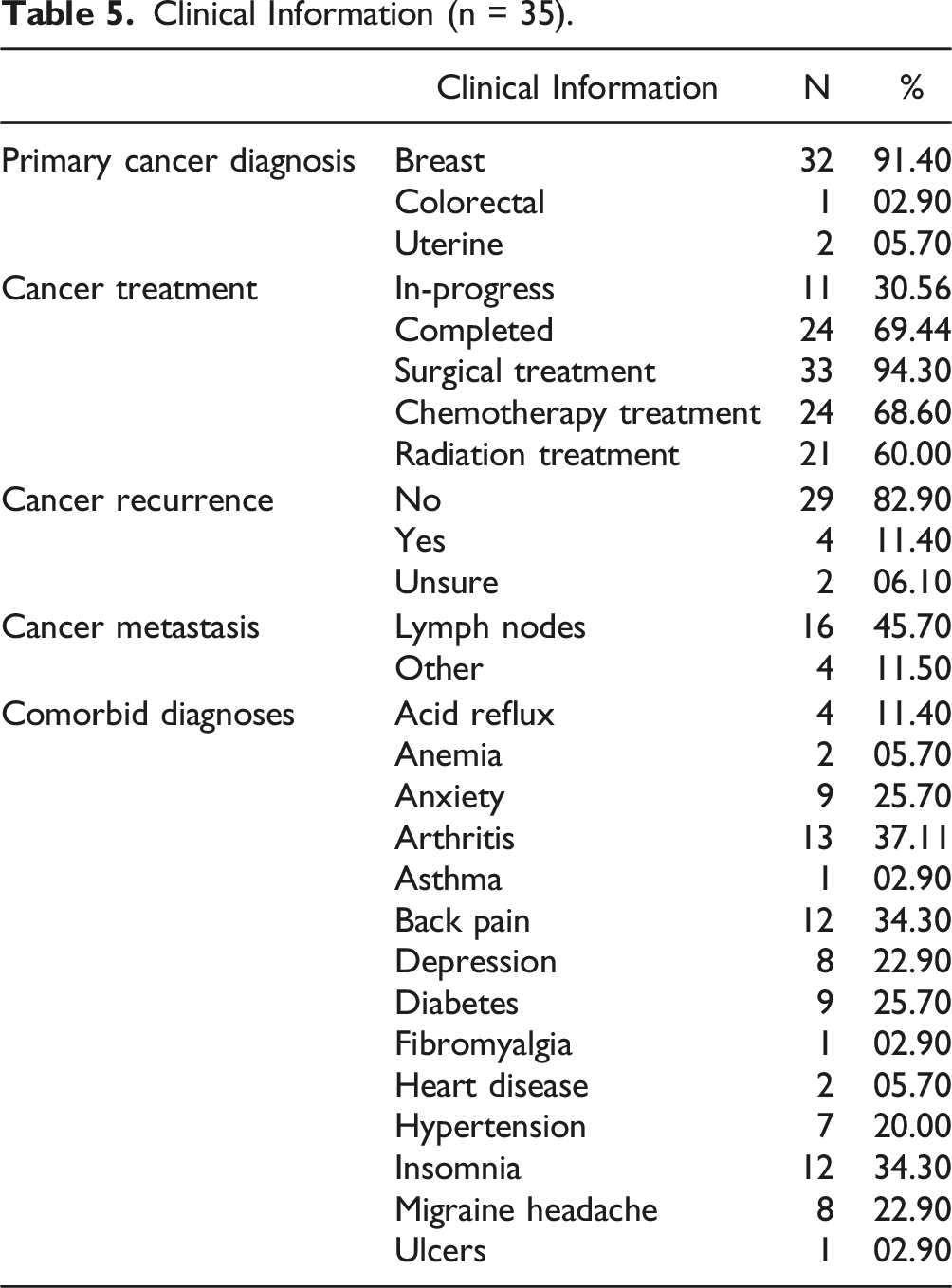
Clinical Information (n = 35).
Safety, Feasibility and Acceptability
During this study there were no reports by participants or instructors of any safety-related issues, injuries, or adverse events. One participant dropped out prior to starting her course, and five participants dropped out during their assigned 12-week course. Of those who began the course, there was 14% attrition during the 12-week period (feasibility benchmark was ≤30% attrition). Two more participants dropped out prior to T3, resulting in 20% attrition overall. There were no significant differences on demographic, clinical, or PRO information between those who dropped out and those who completed the T3 assessments.
The average number of sessions participants attended was 9.2 (SD: 3.2) out of 12 possible, which corresponded to an average attendance rate of 77% (Min: 66% - Max 86%). The attendance feasibility benchmark was ≥70% attendance. Ninety-seven percent (97%) of participants reported engaging in at least some home practice during the 12-week intervention period (acceptability benchmark was ≥70% of a least some reported home practice). On average, participants reported engaging in >20 minutes per day 31% of the time between classes during the 12-week intervention (Range: 0%-83%). Between weeks 12-24, 83% (77%-93%) of participants on average reported engaging in some amount of home practice, of which 43% reported practicing 4 or more days per week. The acceptability benchmark was ≥70% of some reported home practice during the follow-up period. Finally, at the T2 assessment, 4% rated their overall experience as being “good”, 32% reported it as “very good”, and 64% reported it as “excellent.” The acceptability benchmark was ≥70% endorsing either “good”, “very good” or “excellent.”
Preferences, Motivators, and Barriers
In total, 28 participants completed the 12-week survey focusing on preferences, motivators, and barriers to participation in the yoga course. Most respondents reported “very much” or “extremely” in their preference that their yoga instructor be able to speak Spanish (89%) and be of Latiné descent (54%). In contrast, the majority reported “not at all” in their preference that their instructor be of the same sex (64%), be of the opposite sex (71%), or be a cancer survivor (57%). Most reported “very much” or “extremely” in their preference to participate with other Spanish-speaking cancer survivors (64%) with a wide range of preferences to participating with a family member or friend. The majority recommended 3 yoga classes per week for future courses, either for 7-12 weeks (21%) or ≥25 weeks (43%). Most liked having more than one yoga instructor during their course (quite a bit (25%) or very much (58%)).
Physical health was the reason provided by 75% of respondents for their primary motivation for continuing to come back to the yoga class, followed by relaxation and stress relief (25%). Participants reported needing to practice yoga each week between a few times (39%) to every day (36%) to experience its health benefits. Most respondents ranked practicing yoga poses as the most valuable part of the course (54%), with 25% reporting snack time as the most valuable. The home practice packet was used between a few times (36%) to every week (39%) with the most valuable components being the images (46%) and variety of poses (39%). The majority reported their family and friends as being very supportive (29%) or extremely supportive (61%) of their participation in the course.
While most participants reported practicing at home to not be difficult at all (50%) or just a little difficult (25%), those who found it challenging reported a variety of barriers, including: being inflexible and unsure if the poses were being practiced correctly, feeling tired after work, being interrupted by children or the phone, not having the same privacy as the course, and being more stimulated and motivated to practice with others than by themselves at home. Also, while the majority reported no challenges getting to their yoga class (68%), those who had challenges reported difficulty finding transportation, and several reported needing to take multiple busses, trains, and needing to leave their home hours before the class began to arrive on time due to the distance.
Associations between Covariates and Outcomes
Expectancy was inversely correlated with changes in depression between baseline and 24 weeks (r = −.39, P = .03), and with weight between baseline and 12 weeks (r = −.45, P = .03). As depression scores and weight decreased, expectancy scores increased. The total number of yoga classes attended was inversely correlated with fatigue scores between baseline and 24 weeks (r = −.40, P = .03), and positively associated with positive affect scores between baseline and 12 weeks (r = .45, P = .01). As fatigue scores decreased and positive affect scores increased, the total number of sessions increased. Based on these significant associations, expectancy and total sessions attended were used as covariates in subsequent analyses with these specific outcomes.
Temporal Changes in PROs, Blood Pressure, and Weight
PROs, Blood Pressure, and Weight Measures Across Time Points.

Note: Comparisons are against baseline estimates; Bolded values are statistically significant ≤.05.
While weight did not significantly change over time amongst the total sample, at 12 weeks 52% of participants had lost weight, with 13% staying the same, and 35% gaining weight. At 24 weeks 60% continued to show weight loss since baseline, with 4% staying the same, and 36% showing weight gain. During the 24-week study period, after adjusting for weight gain between assessment time points, 71% of participants demonstrated a total mean weight loss of 4.9 lbs. (SD: 5.4). From this group, 45% lost up to 5 lbs., 20% lost between 6-10 lbs., and 30% lost between 11-20 lbs. In contrast, 29% of participants demonstrated a total mean weight gain of 2.6 lbs. (SD: 5.1) during the study period after adjusting for weight loss between assessment time points. From this group, 50% of participants gained up to 5 lbs., 25% gained between 6-10 lbs., and 25% gained between 11-20 lbs. There was a moderate, positive, statistically significant correlation (r = .51, P < .01) between baseline weight and total adjusted weight loss during the study, indicating that higher weight classification at baseline is associated with greater total weight loss. Those who lost weight attended ≥10 yoga classes each week with greater frequency (63%) vs those who gained weight (38%).
Unstructured vs Structured Healthy “Social Snack” Period
Statistically significant main effects (P < .05) were observed between baseline and 12 weeks in satisfaction with social roles and activities, as well as in total adjusted weight loss and weight gain during the 24-week study period, among participants who engaged in either unstructured (n = 16) or structured (n = 14) healthy snack time after their yoga classes. At baseline, there were no statistically significant differences in social role satisfaction scores between unstructured (Mean = 56.23) and structured (Mean = 52.45) snack sessions. However, at 12 weeks, members of the structured group reported statistically significant (P = .009) higher satisfaction (Mean = 56.66) compared to those in the unstructured group (Mean = 52.91), whose scores significantly decreased. The effect size for this difference was large (d = .756).
While no significant differences in weight were observed between groups at baseline (P = .57), participants in the unstructured group demonstrated significantly (P = .04) greater total adjusted weight gain during the 24-week study period (Mean = 3.9 lbs.) compared with those in the structured group (Mean = .03 lbs.). Conversely, participants in the structured group demonstrated significantly (P = .02) greater total adjusted weight loss during the 24-week study period (Mean = 7.7 lbs.) compared with those in the unstructured group (Mean = 2.7 lbs.). The effect sizes for these differences were large (d’s = .93 and .98, respectively).
Conclusion
This single arm pilot developed and implemented a community-engaged, culturally informed 12-week Spanish language yoga program for Latiné women with overweight or obesity and diagnosed with cancer, to examine feasibility, acceptability, preferences, motivators, barriers, and initial changes in outcomes, such as PROs, blood pressure and weight. Findings suggest this intervention met stated benchmarks for feasibility of enrollment, retention, participation, and engagement in course activities, as well as acceptability of course content and delivery. It also demonstrated preliminary patterns of improvement in certain PROs and weight-related outcomes.
The positive ratings of overall experience, along with high attendance, and engagement in some home practice, demonstrate that this community based, culturally informed Spanish language yoga program can effectively address barriers to yoga participation among minoritized communities. We learned that despite efforts to ease potential home practice barriers, other responsibilities with family members and concerns about proper execution of poses were barriers for some participants that directly impacted their home practice frequency. At both 12 and 24 weeks, the majority of participants reported having completed at least some home practice.
We learned that community-based yoga classes instructed in Spanish by relatable and qualified teachers helped bring participants back each week. This addressed known barriers to yoga participation among minoritized communities, including a lack of ethnic, linguistic, and socio-economic diversity and unrelatable yoga instructors. 45 Primary instruction in the Spanish language with Spanish-speaking peers and encouragement to engage in home practice facilitated by culturally tailored instructional packets that featured Latiné yoga practitioners of different genders and ages, as well as descriptions written in Spanish, likely contributed to an inclusive and supportive community. Furthermore, tailoring yoga poses to the needs and challenges of cancer survivors who experience limitations in range of motion, and obesity and cancer-related fatigue, contributed to its accessibility and inclusivity.46,47
Preliminary analyses of outcomes suggest promising patterns of improvement. Immediately post-intervention (at 12 weeks), participants reported significantly reduced sleep disturbance, pain interference, depression and blood pressure, which is consistent with findings from larger studies of yoga and quality of life. At the 24-week follow-up assessment, significant improvement was noted in scores of depression, anxiety, and blood pressure. These initial findings suggest that more physically based outcomes (e.g., fatigue, sleep, pain) may require ongoing intervention for gain maintenance, whereas changes in more emotionally-based and physiological outcomes (depression, anxiety, and blood pressure) may persist for a longer period of time without ongoing intervention. Similar long-term anxiety and mood-related benefits were found in a comparison of experienced yogis and matched controls, 48 supporting the hypothesis that dose, in this case longer duration of yoga practice, may be related to longstanding benefits.
No significant changes in weight were observed during the study period when examining the total sample as a whole, which is not unusual for a study of this nature. 49 Meta-analytic results of Lauche, et al (2016) suggest that, while more intensive yoga forms may contribute to weight loss, gentle, beginner-level yoga is likely insufficient for meaningful weight loss. 49 Qualitative data suggests that weight loss, mostly unintentional, has been experienced by yoga practitioners who were overweight before beginning regular practice, which is consistent with our findings that individuals of higher weight classification at baseline were more likely to lose weight during the study. 50 While increased muscle tone and related changes in metabolism play roles in the weight loss, shifts toward healthy eating, modeling of healthy behaviors within the yoga community and culture, and improvements in emotional and psychosocial wellbeing are cited as important factors, all of which this intervention addresses. 50 It is likely that longer duration of regular practice is necessary to experience weight loss-related benefits. Additionally, use of weight as an outcome may not fully address physiological benefits of a 12-week beginner-level yoga program. Incorporation of waist-to-hip ratio could be a more sensitive outcome measure for this type of intervention as previous meta-analyses and reviews of yoga aimed at weight loss demonstrate significant changes in this measure. 49
Non-randomized assignment to two different forms of post-practice support by way of unstructured and structured healthy snack time was used to explore the possible role of more deliberate reflection and processing among participants, vs simply offering an opportunity for informal social connection. While significant improvements in weight outcomes and satisfaction with social roles and activities were not seen in the whole group, significant improvements were observed among participants included in courses with structured social snack sessions. Closer examination of the specific items of the social role satisfaction measure highlights its focus on satisfaction with one’s ability to do things for one’s family, to do things for fun with others, to do things for one’s friends, to perform daily routines, to do things for fun outside of one’s home, to meet the needs of one’s friends and family, and to do work that is important. The structured and facilitated conversations during post-class healthy snack times may have contributed to improvements in some of these areas. This would be consistent with a trial aimed at improving satisfaction with social roles as part of a more holistic improvement in quality of life via group-based psychoeducation and skills training for Latiné breast cancer survivors. 51 While aspects of socialization in mind-body intervention studies can often leave one to ask “was it the mind-body practice that led to benefits, or was it the social support?” This question has also been asked time and again in group-based mindfulness intervention studies. The primary reason the post-yoga social snack time was included in the first place was due to strong recommendations from our Latiné study investigators and community partners, who felt that it was an important component for cultural tailoring that would be congruent with the cultural values familism, trust, communication, and respect.
As whole this intervention did not intentionally incorporate specific weight loss or weight maintenance counseling support or strategies (e.g., relapse prevention, cognitive reframing, motivational interviewing, expectation management) that might help explain the observed total adjusted weight gain in the unstructured group, and total adjusted weight loss in the structured group. However, it is possible that more opportunities for participant reflection and conversation occurred about their bodily observations, changes, and challenges in the structured group, which may have played a role. For example, questions from the facilitator guide (see Table 4) asked participants what they were noticing about their body since participating in the yoga classes, how the course may be impacting their relationship with their body and if it has changed, and what challenges they may be experiencing and how were they working with them. Specific components of the structured and unstructured groups should be examined more closely in future studies to better understand their potential role in why some people gained weight while others lost weight.
While our study achieved feasibility, acceptability, and early phase indicators of benefit, we acknowledge some limitations. The use of a single-arm pre-posttest design introduces potential direct and indirect confounding factors and limits causal inferences. To strengthen our findings, future research should incorporate time/attention-matched control groups and random assignment. Additionally, due to the early phase developmental nature of this study, the sample size was not intentionally powered to detect clinically meaningful score differences over time or between groups and therefore the small sample size may affect the generalizability of our results. Efforts to recruit a more diverse and larger cohort of Latiné cancer survivors (beyond breast cancer survivors of Mexican descent) will enhance the robustness of the intervention’s outcomes. A recent call to action 52 in the mindfulness field called for higher representation of the Latiné population in mindfulness‐based research, building a more representative workforce, and increasing the scientific rigor of research. Finally, even though unstructured, and structured groups were not significantly different at baseline on scores of social role satisfaction, since participants were not randomly assigned to one of these two groups, similar caution should be exercised when interpreting these findings. Continued exploration of programs like this one should continue both in research and as community delivered efforts. Offering such support can help traditionally under-resourced and historically marginalized groups, such as immigrant or first generation Latiné women affected by cancer to feel seen, regarded, and respected, imbuing trust and value.
Building on our successful 12-week intervention, future research should include randomized controlled trials with larger sample sizes and time/attention-matched controls to establish causal relationships and determine the long-term benefits of this yoga program. Additionally, exploring the involvement of caregivers and testing various delivery formats, such as online or hybrid options, can further expand the reach and impact of this intervention. By considering different formats and involving caregivers, we can also enhance the program’s scalability and potential for broader dissemination. Further, future studies would also benefit from exploring the potential role of endocrine/hormonal therapies given their known association with weight gain. Finally, future studies should continue to explore the relationship between the mental, corporal, and spiritual aspects of yoga, their relevance to psychosocial and clinical indicators, and their role in reducing health disparities.
Overall, this study offers a feasible and acceptable foundation for a 12-week culturally informed Spanish language yoga intervention that holds potential to improve the health and wellbeing of Latiné women with overweight or obesity affected by cancer.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by a pilot grant from the Osher Center for Integrative Health at Northwestern University.

