Abstract
Study Design
Case Report.
Objective
Paranasal osteomas are rare, benign bony tumors of the craniofacial skeleton and most are treated endoscopically without the need for reconstruction. In rare cases, open traditional craniofacial approaches are required with a paucity of literature describing extirpative maneuvers in this setting. We present a unique case of a rapidly growing, paranasal bony tumor in a pediatric patient and describe our surgical technique for resection and reconstruction.
Methods
A 13-year old male presented with eight months of progressive, painless right periorbital swelling and proptosis. Trans-nasal biopsy confirmed an osteoma of the right ethmoid sinus and endoscopic resection was recommended. Due to interval tumor growth, there was worsening visual acuity that precluded a minimally invasive approach. Pre-operative and post-operative 3D computed tomography (CT) scans were completed, and a 3D printed skull model was produced to aid in surgical planning. A multi-disciplinary team of Otolaryngology, Neurosurgery, and Plastic Surgery was employed. The majority of the extirpation was performed with a highspeed carbide burr.
Results
Post-operative course was unremarkable and CT scan demonstrated a complete resection. Pathology confirmed the diagnosis of an osteoma. Six-month follow-up demonstrated normal ophthalmologic function and visual acuity with excellent aesthetic results.
Conclusions
This is a rare, complex presentation of a paranasal osteoma that was successfully managed with an open, multi-disciplinary approach. We highlight pearls gleaned from this extirpative and reconstructive technique. Due to the tumor density and location, a multidisciplinary team, Stealth navigation, an open, intra- and extra-cranial approach and use of a highspeed carbide burr were essential.
Introduction
A “giant” osteoma is defined as one that is larger than 3 cm in diameter. The majority of the literature describes management principles in the adult population.1,2 Osteomas are typically diagnosed between the third and fifth decade of life, though there have been pediatric cases involving the paranasal sinuses and orbital regions described.3,4 An increasing number of reports on pediatric paranasal and orbital osteomas suggest key differences in gender predilection, rate of growth, and need for surgical intervention; however, the current literature remains densely skewed to descriptions in the adult population. 5
As described in the current literature, osteomas are benign, slow-growing tumors most commonly occurring in bones formed by intramembranous ossification with an overall male predominance of 1.5:1.6,7 The prevalence is estimated to be 3% in the general population with most tumors varying in size from 2 to 30 mm. 1 The two most common regions in the craniofacial skeleton are the frontal and ethmoidal sinuses. 8 Many osteomas demonstrate a slow rate of growth, estimated to be about 1 mm/year, and if asymptomatic, tumors can be followed with close clinical and radiographic evaluation. 9
Depending on the size and location, osteomas of the skull can cause headaches, pain, contour deformities, visual disturbances and other ophthalmologic signs such as epiphora and orbital cellulitis 10 and even intracranial mucoceles. 11 When indicated, the majority of these tumors are resected via minimally invasive transnasal or transorbital approaches, though some tumors because of size or adjacent critical structures, may preclude this treatment paradigm.12,13 We present a unique case of a rapidly growing paranasal bony tumor with orbital extension in a pediatric patient and highlight pearls gleaned from this extirpative and reconstructive technique for a case that is typically managed in and described in the literature as an endoscopic fashion.
Case Report
History
A 13-year old male presented to a local facility in March 2021 with a two-month history of gradually worsening, painless right-sided periorbital swelling. He did not report any history of trauma, sick contacts, or recent travel. Visual acuity was reported to be normal, and two months prior, he had been prescribed anti-histamines and ophthalmologic tobramycin drops after complaints of discharge. He was seen by Ophthalmology two weeks later. There had been worsening proptosis, limited supraduction of the right eye (−1), and decreased sensation to light touch throughout the distribution of the ophthalmic division of the right trigeminal nerve. Magnetic resonance imaging was performed that showed a mass centered in the right orbital roof and ethmoid air cells that was hypointense on T2 and T1-weighted imaging. An endoscopic ethmoid biopsy was performed the week thereafter. One month after the biopsy, there was worsening proptosis, anterolateral displacement of the globe and worsened limitation of supraduction (−3).
Pathology was interpreted as an osteoma and plans were made for a combined endoscopic and trans-orbital approach for resection. However, at his next evaluation the mass had progressed to the point beyond the safe capabilities of endoscopic resection. He was referred to our center for further evaluation and management. The right medial canthus was displaced laterally and inferiorly but was intact with significant inferolateral displacement of the globe and proptosis. Due to the mass effect of the displaced globe, the zygoma and orbital floor were also displaced inferolaterally. Flexible nasopharyngoscopy revealed an irregular, mucosal covered mass occupying the middle meatus without purulence. Posterior to this mass, there was no other obvious mass or lesion inside the nasal cavity. After this initial consultation at our institution, ophthalmologic examination revealed disc edema and visual acuity of 20/200 on the right and 20/16 in the left eye. Tonometry was unremarkable at 11 and 10 mmHg, on the right and left, respectively. There was no evidence of ptosis.
The pathology slides were re-reviewed at our institution and the differential diagnosis included osteoma, osteoblastoma, low grade surface osteosarcoma, ossifying fibroma and fibrous dysplasia. The histology was not indicative of a sarcoma, and there was lack of positivity for CDK4 and MDM2. Given the predominance of woven bone and the location of the tumor, there was consensus on the diagnosis of an osteoma.
Pre-Operative Planning
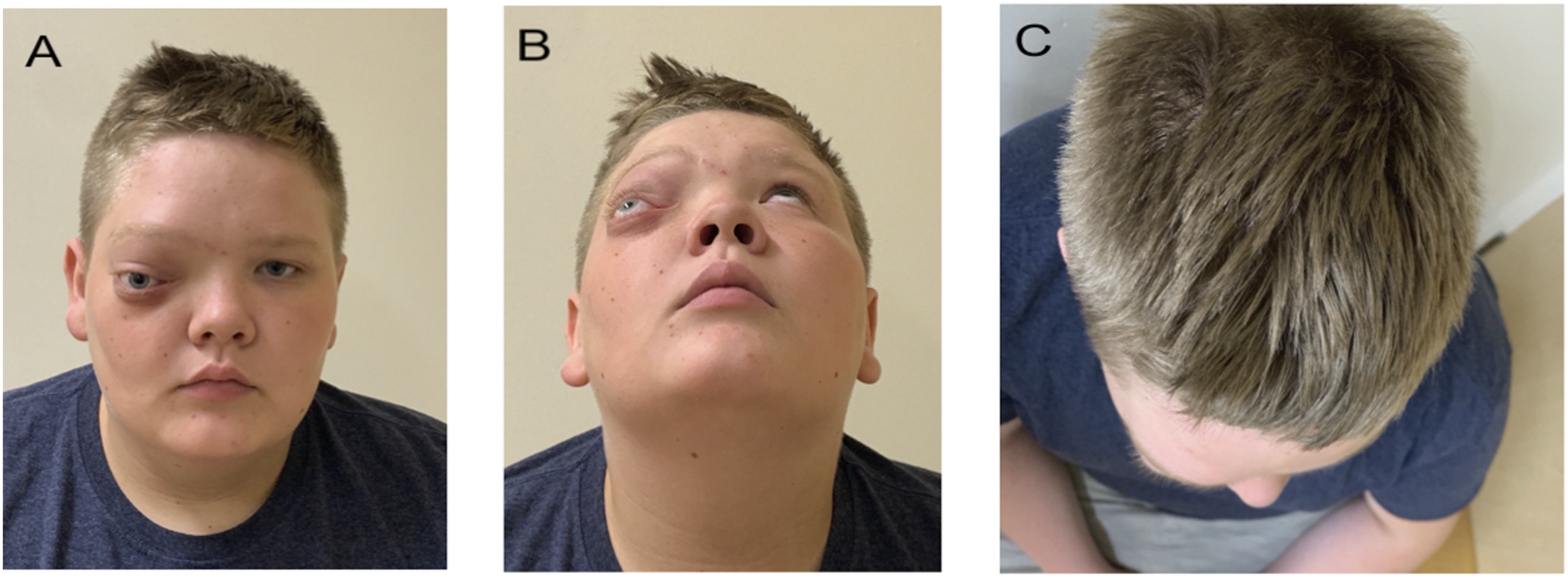
A pre-operative maxillofacial CT scan with multiplanar reformations (axial, sagittal, coronal, and 3-dimensional) (Figure 1) and a 3D printed skull model were performed to aid in pre-operative planning. A multidisciplinary team of Neurosurgery, Plastic Surgery, and Otolaryngology were convened to discuss the surgical approach. Pre-operative photos are presented in Figure 2. Written informed consent for patient information and images was obtained. A pre-operative CT scan was done and the axial (A), coronal (B), sagittal (C), 3-dimensional (D) views are shown. The lobulated mass lesion was centered within the right ethmoid air cells, with extension into the right frontal sinus and right orbit measuring 41 × 48 × 38 mm, TR x AP × CC. There was no evidence of periosteal reaction. Laterally, the lesion extended into the right orbit, resulting in marked proptosis, lateral displacement of the globe and stretching and lateral displacement of the right optic nerve. Abbreviations: TR, transverse; AP, anteroposterior; CC, craniocaudal. In coronal (B) image, the globe is highlighted in red and star denoting stretching and lateral displacement of nerve. The pre-operative photographs illustrate the severe asymmetry from the anteroposterior (A), basal (B) and bird’s eye (C) views.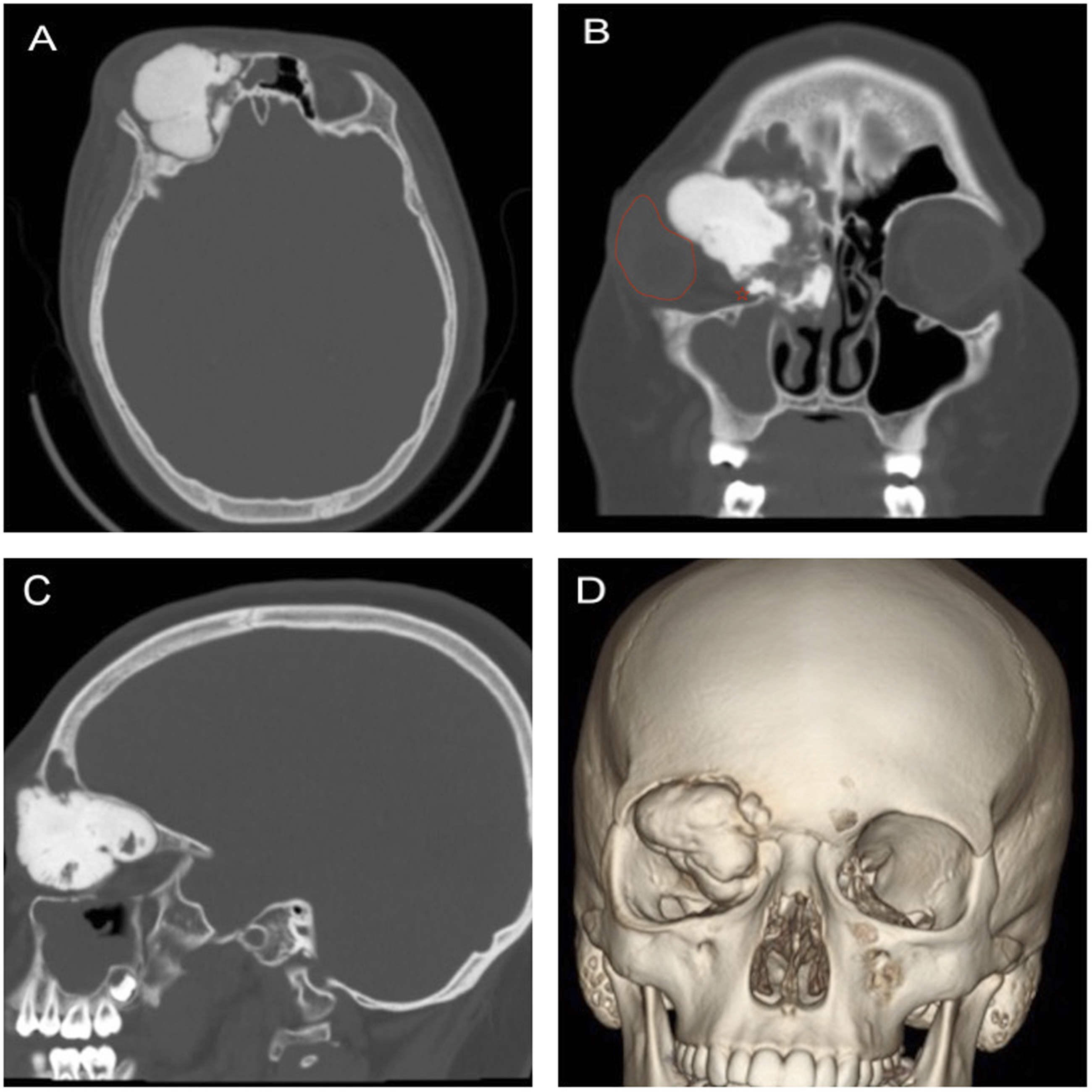
Surgical Procedure
The objectives of the surgery were as follows: 1. Total resection of the bony tumor 2. Preservation and restoration of visual acuity and extraocular movements 3. Reconstruction of the anterior table of the frontal bone, the superior and medial orbital walls, and the medial canthus. Through a coronal incision, dissection was carried out at the subgaleal level with creation of right temporal and left anteriorly-based pericranial flaps for cranialization and any possible dural violation. Subperiosteal dissection was performed to allow for exposure of the mass and to execute a bifrontal craniotomy by Neurosurgery. This exposure allowed for both intracranial and extracranial access to the mass. Similar to our pre-operative 3D printed model, we designed a D-shaped frontal craniotomy that was situated approximately 15 mm superior to the left orbital rim. The tumor had eroded through the right frontal sinus, and therefore, cranialization of the frontal sinus was performed by meticulously removing all mucosa and posterior table bone with highspeed carbide 4 mm burr and obliterating the nasofrontal ducts with particulate bone graft harvested from the endocortex of the frontal bone, pericranial grafts and fibrin sealant (TISSEEL, Baxter Healthcare Corp, Deerfield, IL). Further, removal of the posterior table allowed for better access to the superior margin of the tumor which had obliterated the orbital roof.
We used StealthStation Navigation System (Medtronic of Canada Ltd, Brampton, Ontario, Canada) to identify our proximity to critical structures like the orbital apex. A highspeed 9 mm carbide burr was used to drill away the center of the mass. The osteoma was an avascular, rigid tumor. We found that drilling the dense inner center away left a thin outer shell which was more pliable. There were distinct planes between the mass and the surrounding structures. As such, once the outer “shell” was thin enough, it could be easily separated from surrounding structures. This “inside out” approach creates the necessary room to mobilize the tumor in small working spaces. The StealthStation Navigation System was critical for gauging how much more of the tumor remained after intervals of drilling. We were able to release the medial extent of the mass emanating from the ethmoid sinus as one piece and endoscopically confirmed no residual tumor in the ethmoid sinus or nasal cavity.
The frontal bone and supraorbital bar were reconstructed with full-thickness parietal calvarium from the contralateral side, secured with titanium plates and screws. Particulate bone graft was harvested from the graft endocortex to fill the resulting donor defect. The orbital roof and medial orbital wall were reconstructed with titanium mesh. The right medial canthus was re-suspended to the contralateral lacrimal crest in the appropriate position, relative to the normal contralateral medial canthus via trans-nasal wiring and 3-0 polydioxanone suture. Estimated blood loss was 200 mL. Transfusion of blood products were not required. Intra-operative photos are demonstrated in Figure 3. Intra-operative Photos: Post-frontal craniotomy and exposure of the tumor’s core (A). The tumor was excised (B). The orbital roof and medial wall reconstruction (C) with the final reconstruction (D).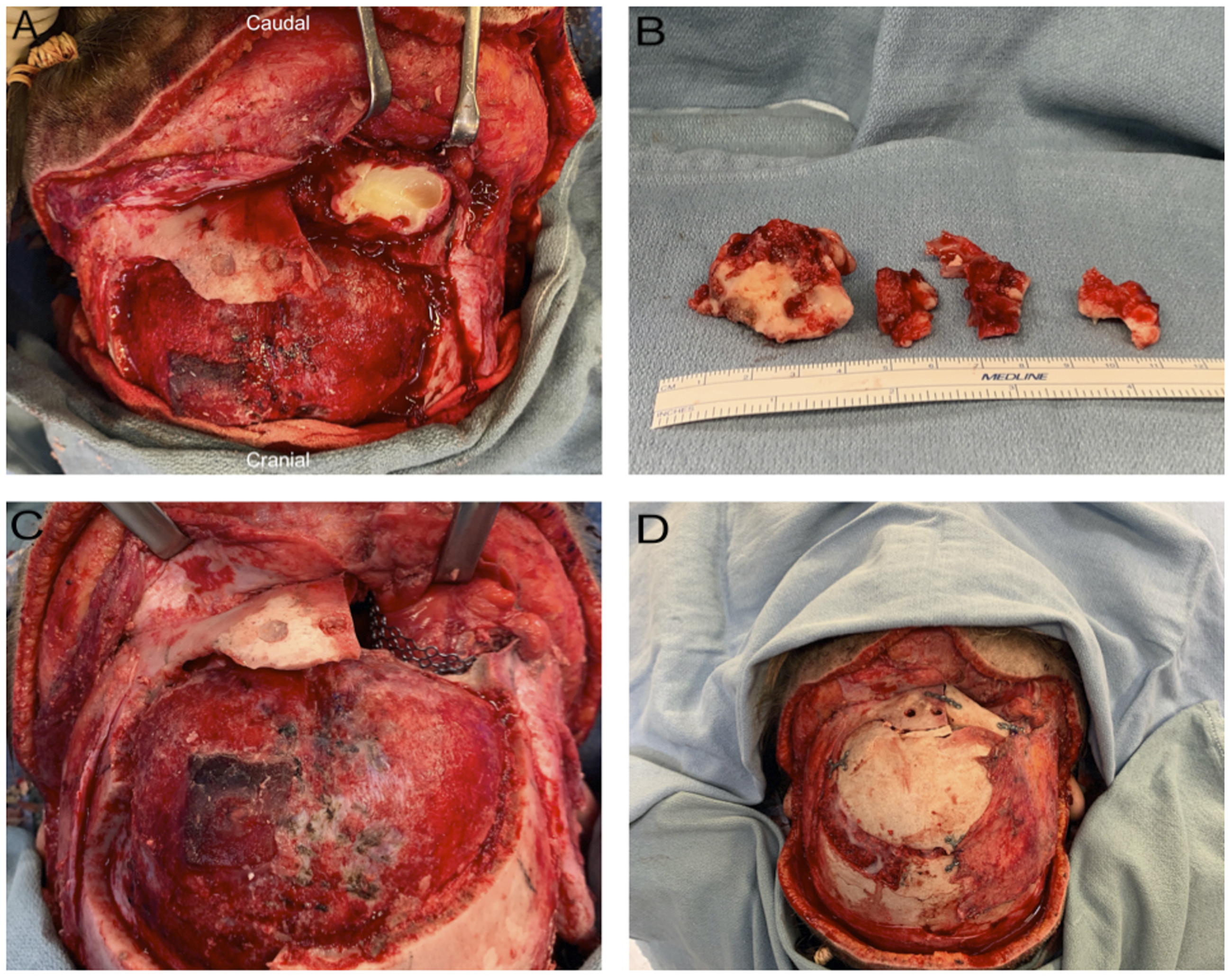
Post-Operative Recovery
Post-operatively, the patient was admitted to the intensive care unit overnight for vision checks and monitoring of neurovital signs. He was transferred to the surgical ward post-operative day (POD) #1. The post-operative CT scan showed complete resection of the bony tumor (Figure 4). The patient was maintained on prophylactic meningitic antibiotic coverage for five days and sinus precautions for six weeks. Visual acuity during his hospital stay was unchanged at 20/200 right eye with intact intra-ocular pressures (17 mmHg in both eyes), and mild (−1) restriction to upward gaze in the right eye. He was discharged home on POD#7. Histopathological assessment of the tumor was characterized predominantly by mature cortical-type bone and cancellous bone with moderately cellular and fibrous stroma filling the marrow space with foci of woven bone with osteoblastic and osteoclastic activity. Final pathologic diagnosis was confirmed as an osteoma. Post-operative CT scan is presented from the axial (A), coronal (B) and sagittal (C) views.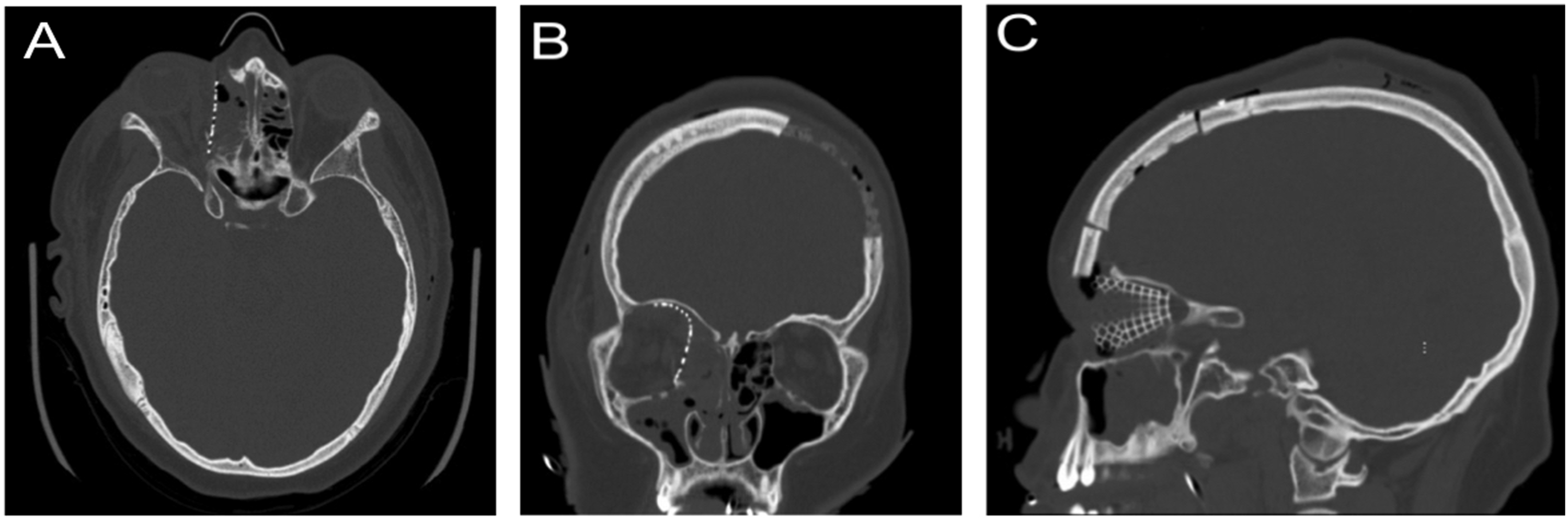
Six months post-operatively, the patient has not reported any crusting, nasal discharge, nor epistaxis. Flexible nasopharyngoscopy demonstrated healed nasal mucosa into the middle meatus and lateral nasal wall with no synechiae formation or crusting. Ophthalmologically, visual acuity had returned to baseline in both eyes (20/20), no globe ptosis and full extraocular movements including upgaze. Most importantly, his color vision returned to baseline indicating recovery of optic nerve function. Post-operative photos are presented in Figure 5. Post-operative photos show improved symmetry and decreased proptosis: AP (A), basal view (B) and bird’s eye view (C).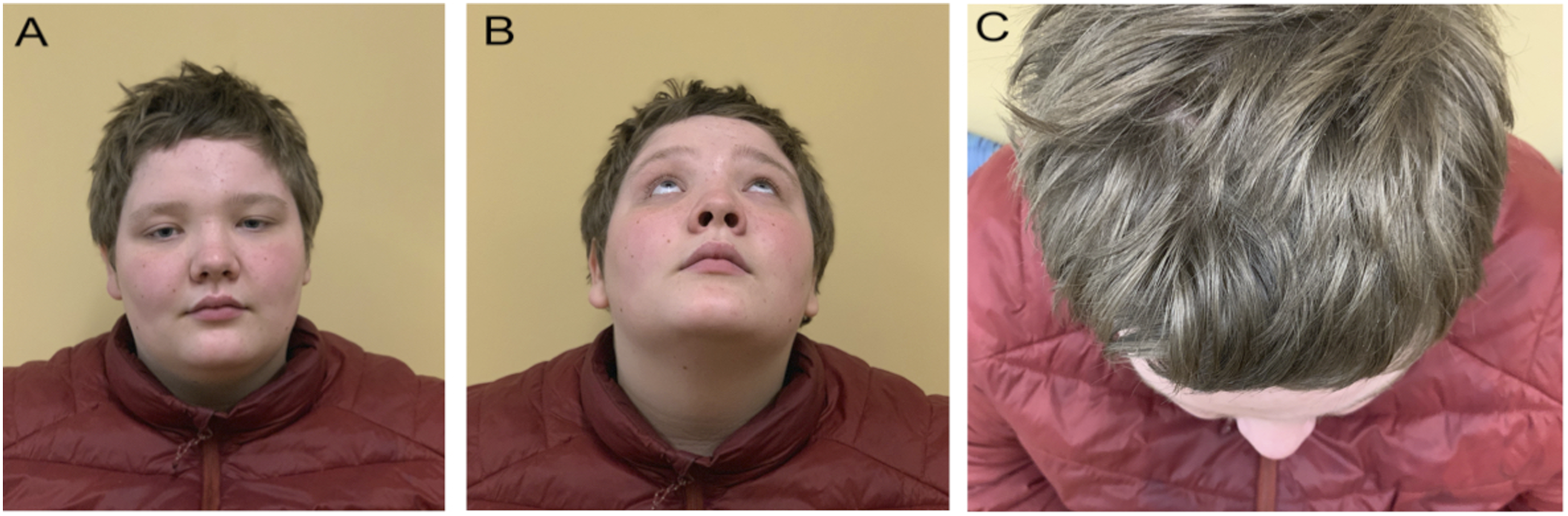
Discussion
We present a case of a rapidly growing, giant paranasal osteoma of the right ethmoid sinus invading the frontal sinus and orbit with compression of the optic nerve. Our patient developed rapidly worsening symptoms, highlighted by the disc edema and deterioration of visual acuity and limitations on upgaze all of which resolved within six months after extirpation and reconstruction. While most osteomas are slow-growing tumors, there have been more reports describing rapidly growing orbital osteomas in adolescents. A systematic review, comprising 59 patients in 46 articles, identified differences in demographics, symptoms, and need for surgical intervention when compared to adults. 5 In one publication, Earwaker reported only 6.5% of adults with osteomas required surgical intervention, 8 compared to 97% in a systematic review of pediatric patients published in 2021. 5 Our findings are consistent with those from prior reports and highlight the unique nature of paranasal osteomas in the pediatric population. Specifically, pediatric paranasal osteomas tend to be larger, with a significantly faster growth rate and more rapid onset of symptoms, than those reported in adults. In our case, the size of the patient’s tumor, approximately 41 × 48 × 38 mm, meets the threshold of a “giant” osteoma. The implications of these findings impact the decision-making regarding the management and follow-up of these tumors in the pediatric population. When indicated, most cases are amenable to endoscopic surgery. However, in a subset of cases, the tumor size and proximity to critical structures preclude a safe, minimally-invasive approach. In these cases, traditional open, craniofacial approaches to achieve a complete resection and reconstruction are indicated. 2 Importantly, a systematic review did not detect any differences in recurrence or rates of complications associated with surgical approach. 4 As previously reported by Chiu et al, surgical approach should be individualized to the patient and tumor. 2 In our particular case, given the tumor size, location, and proximity to the orbital roof, apex, and optic nerve, a surgical approach that included both extra- and intra-cranial exposures was optimal to successfully achieve a complete resection, restore visual acuity and full extraocular movements. While alloplastic materials such as porous polyethylene or polyetheretherketone implants have been used for similar bony reconstructions of the frontal bone and supraorbital bar, we preferred autologous tissue given the patient’s age and the need for cranialization.
In summary, a rapidly growing giant paranasal osteoma in a pediatric patient was successfully managed with a complete and safe resection using a multi-disciplinary approach, intra-operative navigation, and open, intra- and extra-cranial approaches for resection and reconstruction.
Footnotes
Acknowledgments
We would like to acknowledge Christine B. Novak, PT, PhD for her technical assistance with this manuscript. The authors acknowledge support from the AO CMF NA Fellowship (MAA, SZA).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Research Ethics
This case study was exempt from REB review as per the Hospital for Sick Children guidelines that state, “Case reports involving no more than two (2) separate cases, provided that the case reports are void of private identifiable information.”
