Abstract
This case report describes the course of a patient diagnosed with Gorham-Stout Disease and reviews known complications and treatment options for this rare condition. An emphasis is placed on potential multi-systemic complications that may occur including surgical complications, obstructive sleep apnea, post-operative airway obstruction, respiratory failure and cardiac arrest.
Keywords
Introduction
Gorham-Stout Disease (GSD) is a rare medical condition that leads to progressive bone loss caused by infiltration of venous and lymphatic tissue in affected areas. Osteolysis and progressive bone resorption are characteristic findings of the disease, the exact cause of which is still unknown. Typically affected areas include the ribs, spine, pelvis, cranial vault, clavicle and mandible. Normally, involved bones have a propensity for osteopenia and fractures, as well as swelling and pain. Disfigurement and functional impairment are expected depending on the severity of the disease. Most cases are diagnosed before 40 years of age, and can vary from mild symptoms to life-threatening sequelae. This case report emphasizes the multi-systemic complications that may occur is a patient with GSD, and the surgical management of severe mandibular involvement with long span alloplastic temporomandibular implants.
Case Report
Written informed consent was obtained from the patient to publish the information and photographs below. S.W. presented to the Rheumatology Scleroderma Program of our institution as a 55-year-old female with a 6-month history of widening of the tufts of her fingers with whitening and curling of her fingernails. She also complained of left mandibular pain attributed to the use of an occlusal splint made by her dentist for the treatment of suspected bruxism. Her past medical history included hypertension, asthma, depression, and multinodular thyroid. Medications included hydrochlorothiazide, lorazepam, imipramine, and fluvoxamine. Electrocardiography revealed a right bundle branch block. Bilateral hand radiographs (Figure 1) revealed advanced acro-osteolysis with complete disappearance of the distal phalangeal bone with tapering and thinning distally. Subchondral cysts of the shafts of all long phalangeal bones, and osteoarthritic changes at the carpometacarpal joints were found. Erosive osteoarthritis (seagull appearance) was noted at the proximal interphalangeal joints. Systemic sclerosis was ruled out and review of systems did not reveal a prior history of arthritis. The patient was referred to the Oral and Maxillofacial Surgery clinic for further evaluation. Acro-osteolysis with resorption of distal phalangeal bones.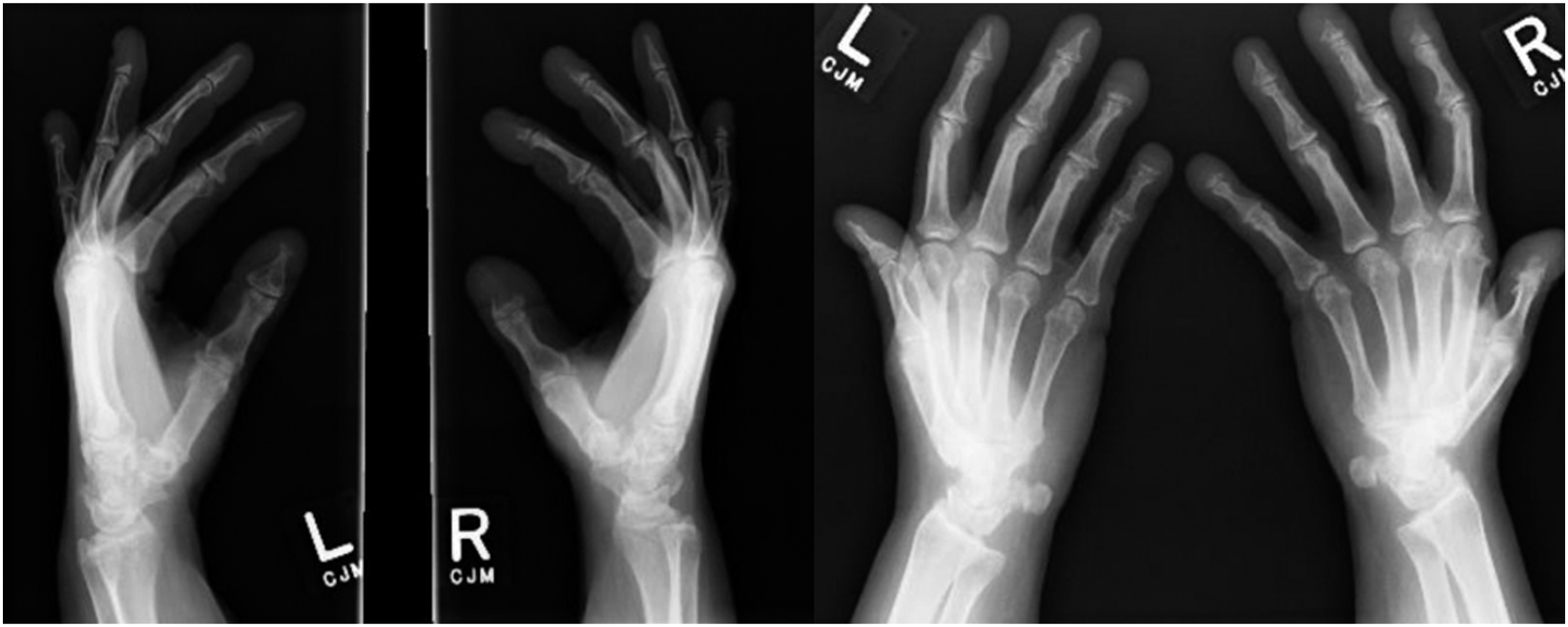
On maxillofacial exam, the mandible deviated to the left on opening, and the mandibular angles were not readily palpable. Computer tomography (CT) scan of the mandible was obtained demonstrating significant osseous resorption of the gonial angles, coronoids, and a fracture of the left ramus (Figure 2). A left mandibular biopsy was performed, along with simultaneous reconstruction of the left mandible with a left-sided iliac crest bone graft and a 2.3 mm reconstruction plate. Histopathology revealed skeletal muscle with degenerative changes, lamellar bone with resorptive changes and remodeling, and fibrous tissue with no significant abnormalities. There was no evidence of malignancy. Later that same year, the patient presented with left TMJ crepitus. 14 months after initial presentation, the patient suffered a ground level fall after slipping on ice, and presented with malocclusion and difficulty with chewing. A cone beam computer tomography (CBCT) scan showed progressive bilateral osseous resorption of the mandibular rami and the previously placed iliac crest bone graft. (Figure 3). CT Scan showing significant resorption of bilateral rami and coronoid processes. Also, a fracture on left mandibular ramus is present on the exam. Progressive osseous resorption involving bilateral mandibular rami, and of the previous iliac crest bone graft.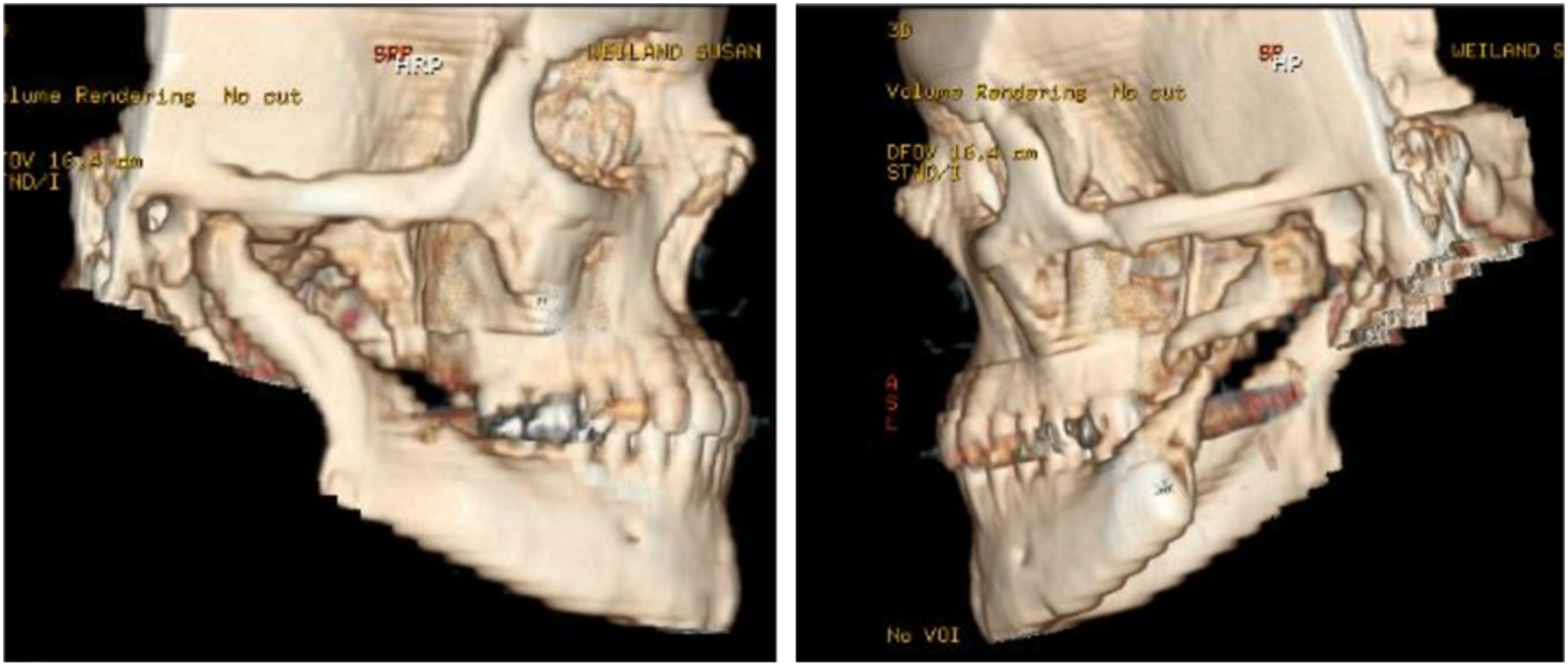
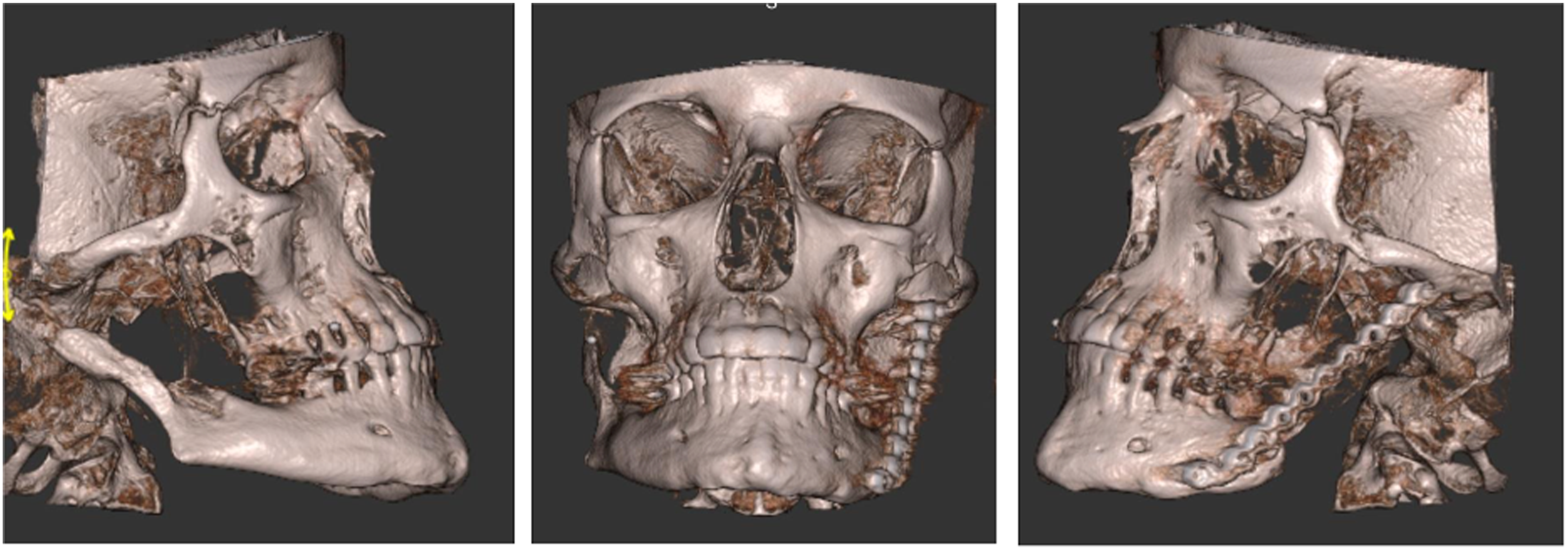
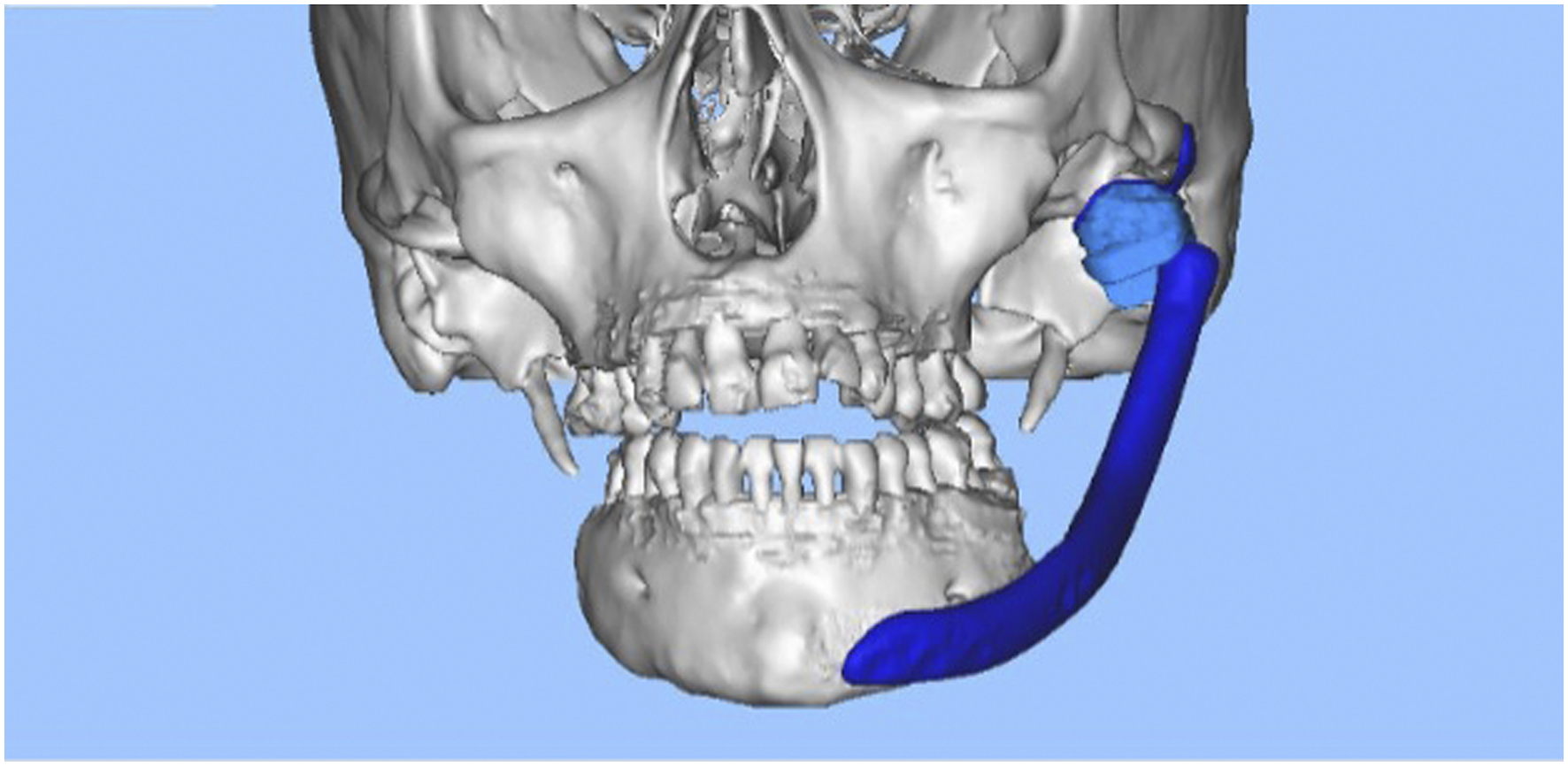
At that time, consideration was given to the use of systemic anti-resorptive medication to halt the bony resorption of the mandible. Ultimately, the patient was referred for a second opinion at another institution, for consideration of a long-span alloplastic temporomandibular joint replacement (ls-TJR). Shortly after her fall, the patient was referred to orthopedics for evaluation of a possible left hip fracture; in addition, nephrolithiasis, and multiple diffuse osteolytic lesions on the left femoral subtrochanteric region were noted. Genetic evaluation at that time was negative for Hadju-Cheney Syndrome, a condition that is also associated with acro-osteolysis of the hands and feet, osteoporosis, short stature, joint hypermobility, and craniofacial anomalies involving the mandible and skull. Due to significant ongoing mandibular dysfunction and pain, the patient was taken to the operating room 2 months after her fall, and a fracture of the right mandibular ramus was found. Due to lack of sufficient bone, no osteosynthesis were applied. The left mandibular reconstruction plate was removed at that time, and maxillo-mandibular fixation (MMF) was applied. 3 months later, the patient underwent bilateral ls-TJR at an outside institution (Figure 4). However, in the early post-operative period, the right prosthetic condyle dislocated, and had to be removed. The patient was kept in MMF for support. Eventually, the left ramus-condyle component dislocated laterally, leading to mandibular asymmetry, retrognathia, anterior open bite and posterior crossbite malocclusion (Figure 5). Meanwhile, because of a partial left temporal branch weakness and incomplete left eye closure, she was referred to the Ophthalmology service. Her facial nerve function recovered with time. 3D model of the patient’s facial skeleton, and design of long span custom TMJ implants for the case. 3D reconstruction demonstrating significant deviation of the mandible, lateral dislocation of the left prosthetic condyle, lateral tilt of the left fossa component, and the absence of right sided implants.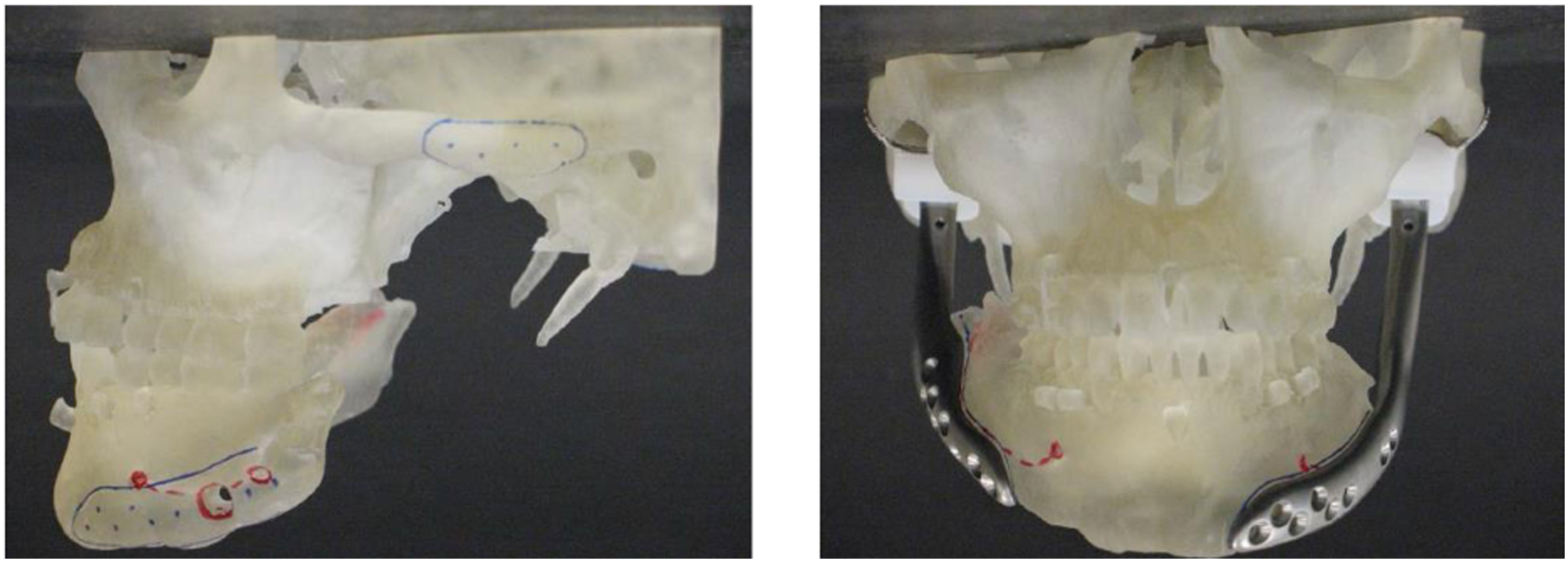
3.5 years after initial presentation, a diagnosis of Gorham-Stout Disease (GSD) was considered given the progressive osteolysis of the mandibular and multiple other bones including the cervical vertebrae. At that time, the patient underwent cervical spine fusion (C3-C5) with an autogenous bone graft from the spinous processes, and recombinant human bone morphogenetic protein-2. Postoperatively, while an inpatient, the patient developed upper airway obstruction, hypoxia and arrhythmia leading to a pulseless cardiac arrest, and required resuscitation and intubation. Two days later, persistent stridor was noted and there was concern for an impeding airway obstruction. An urgent percutaneous tracheostomy was performed by the Otolaryngology service. Subsequently, the patient reported witnessed apneas, snoring, progressively retrognathia, and concerns for obstructive sleep apnea (OSA). Attended polysomnography revealed an apnea-hypopnea index (AHI) of 114 events/hour, and a minimum oxygen saturation of 77%.
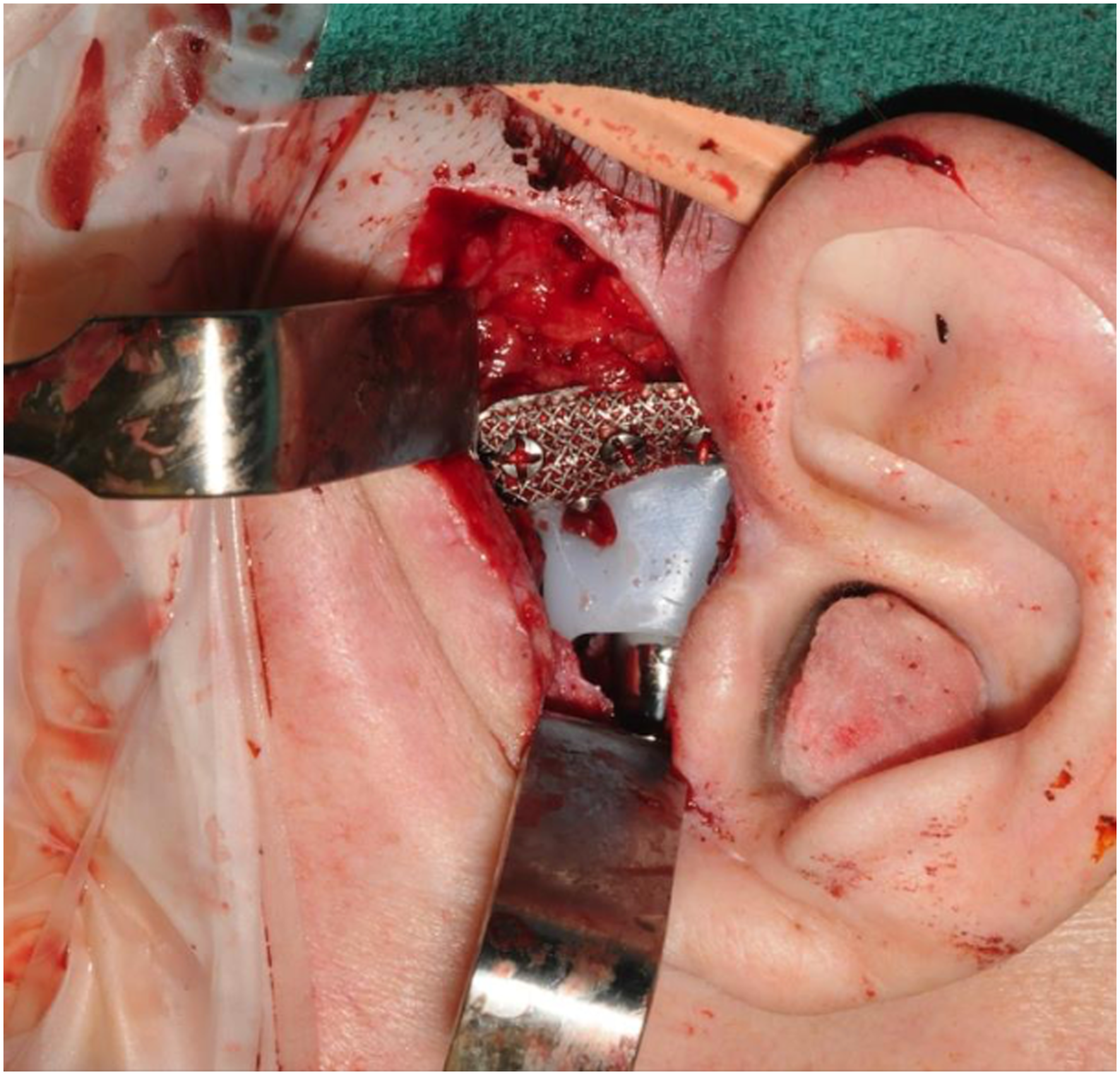
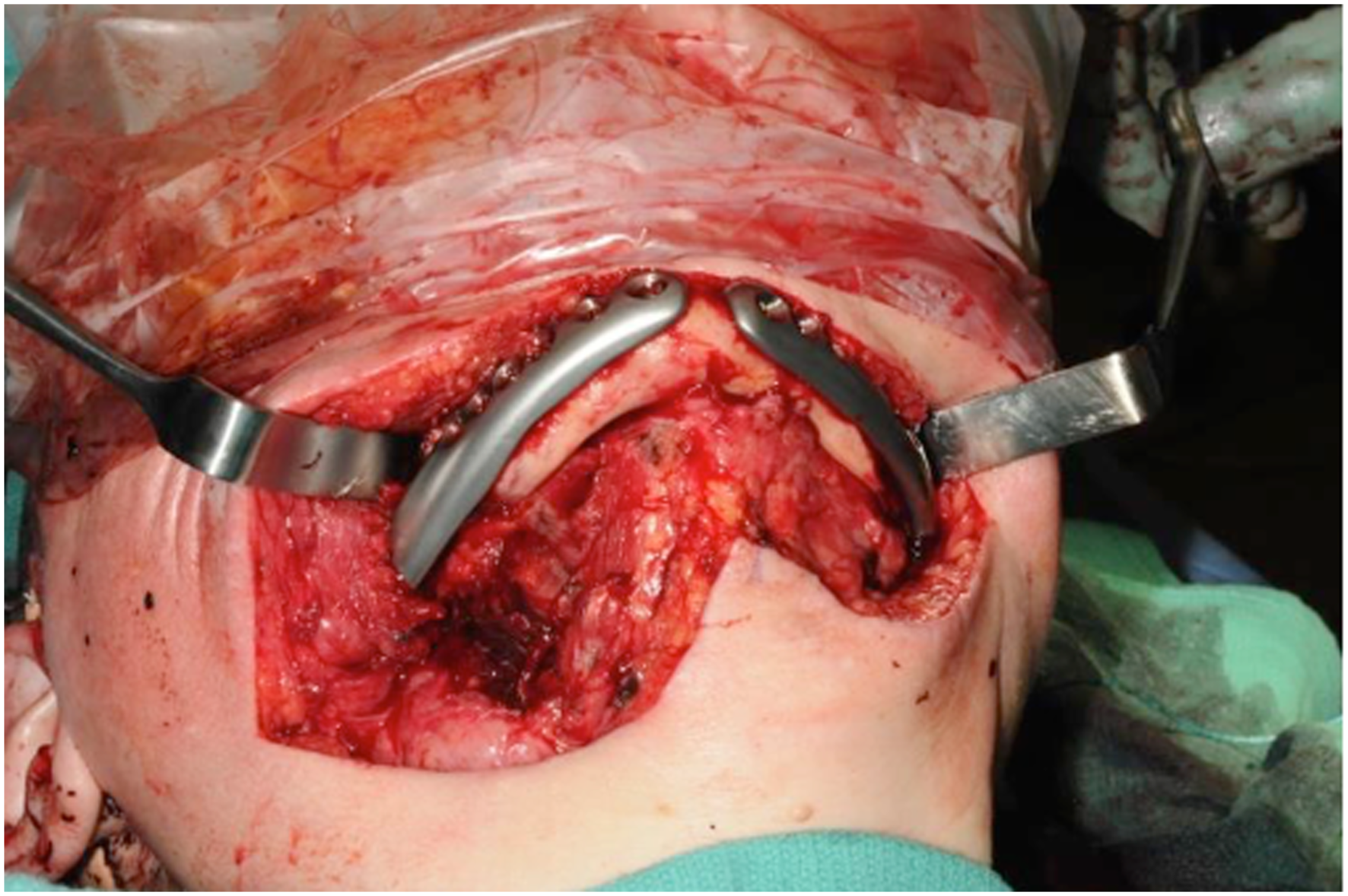
Following subsequent decannulation, formal elective tracheotomy was performed for management of her severe OSA which was inadequately treated even with the maximal CPAP setting currently available (30 cm H2O). Five and a half years after initial presentation, the patient was taken back to the OR for removal of retained and dislocated left TMJ implants, along with a redo mandibular reconstruction with bilateral ls-TJR (Figures 6–8). Intra-operative findings were consistent with progressive resorption of the right mandibular ramus and body as compared to her previous state. As the patient declined orthodontics, the mandible was advanced to an Angle class 1 relationship, but achieving intercuspation was not feasible. Left residual TMJ component after being removed. New left TMJ fossa and ramus-condyle implants after implantation. Inferior view of bilateral long-span alloplastic components extending to the symphysis.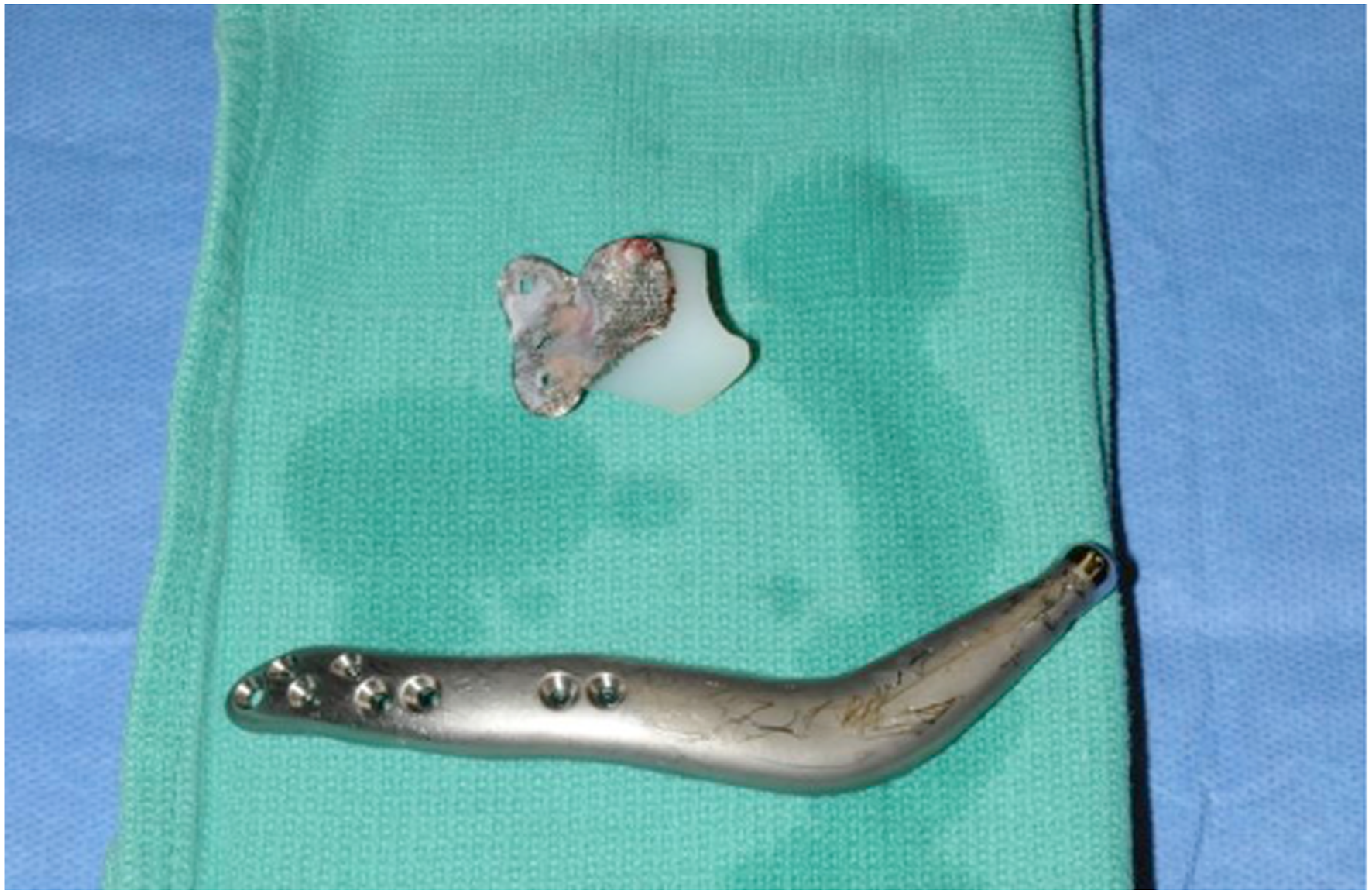
Her post-operative course was uneventful, with expected improvement in occlusion, mandibular projection, mastication and airway. There were no post-operative complications. A post-operative polysomnogram was obtained demonstrating an AHI of 63 events/hour and a minimum oxygen saturation of 86%. While this was a significant reduction in AHI, severe OSA persisted requiring further treatment with positive airway pressure. A CPAP and bilevel positive airway pressure (BiPAP) titration study tested various settings and recommended a setting of 22/18 cm of water with strict positional therapy namely, avoidance of supine position.
Six months post-operatively, the patient followed up and reported good mandibular function, a stable occlusion, and no further complications. Radiographic assessment demonstrates stable prosthesis components without concerning changes (Figure 9). The patient reported being satisfied with the reconstruction and reported a pain score of 1/10 on VAS, as well as a score of 4/200 on jaw functional limitation scale (JFLS). She was able to consume a regular diet, but reported avoiding hard foods. On exam, the maximal interincisal opening (MIO) was 40 mm without pain, and there was no pain to palpation or on loading the right and left dentition. Post-operative lateral and postero-anterior cephalograms, demonstrating stable alloplastic components and mandibular position.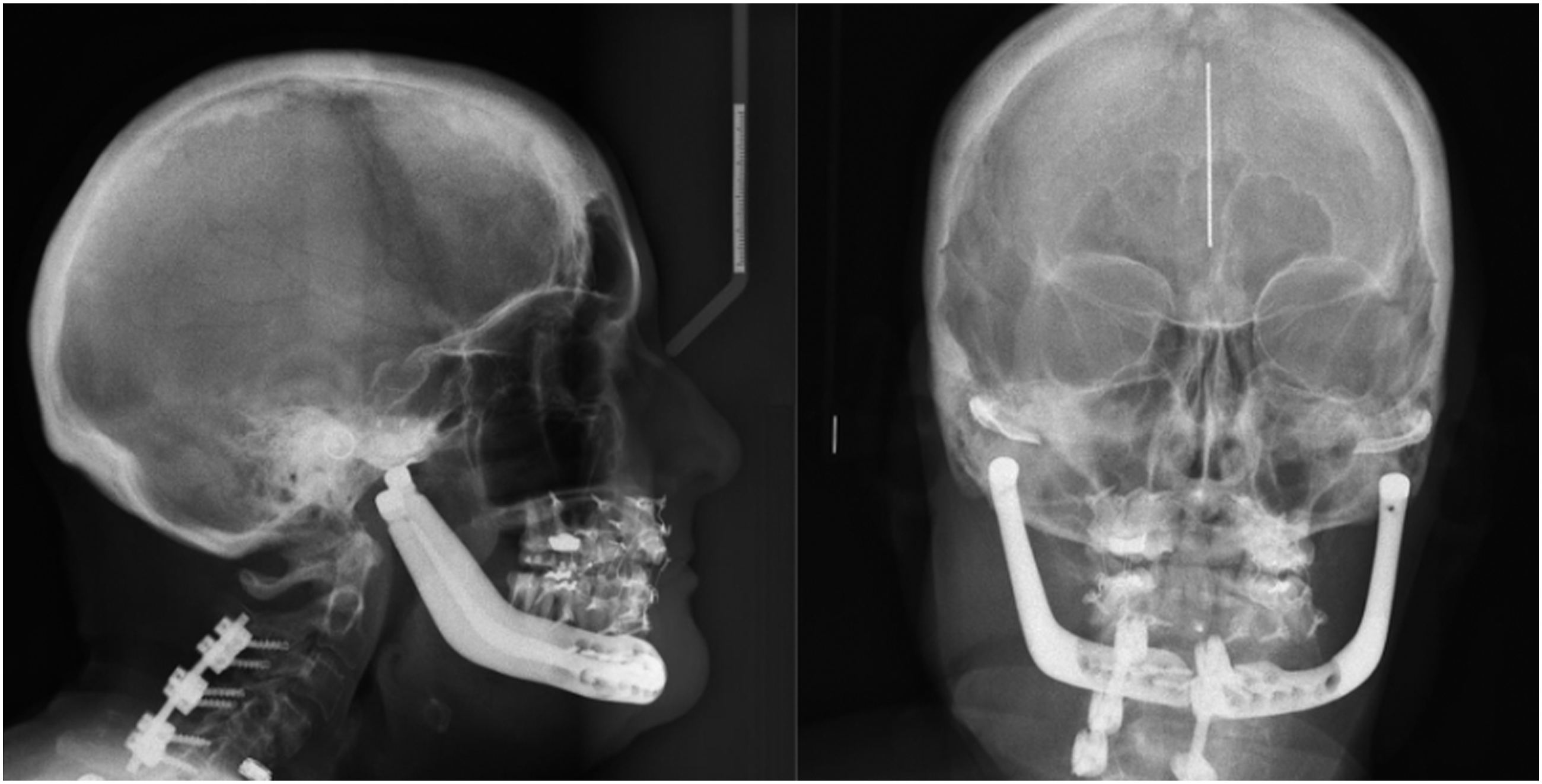
Eighteen months post-operatively, patient returned for follow up with no complains, maintaining her post-operative occlusion with no relapses. Six months later, patient presented with an infected tracheocutaneous fistula and acute airway obstruction that required surgical intervention for repair and hospitalization for intravenous antibiotics.
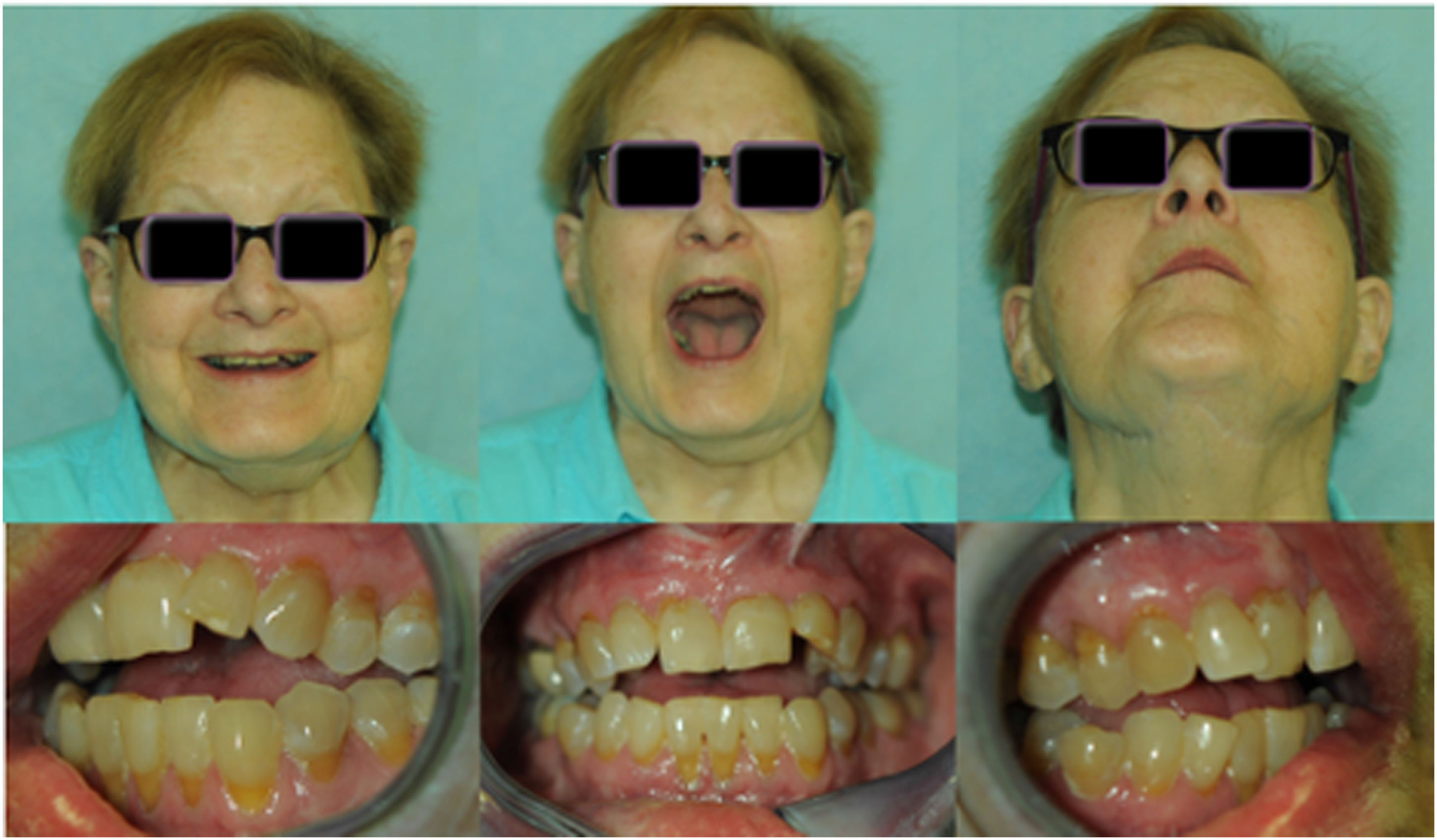
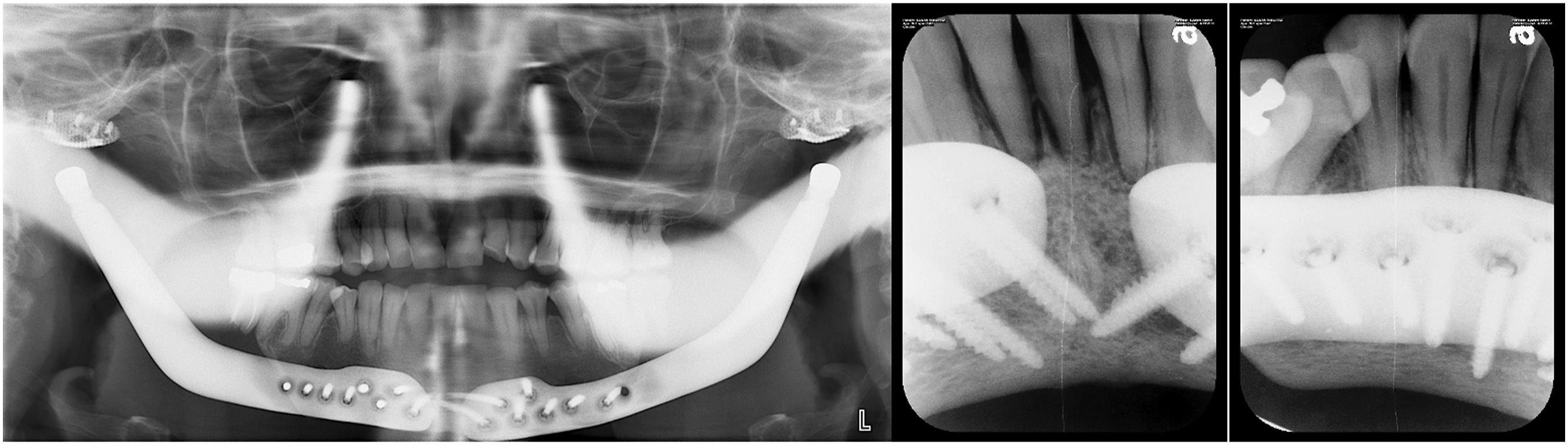
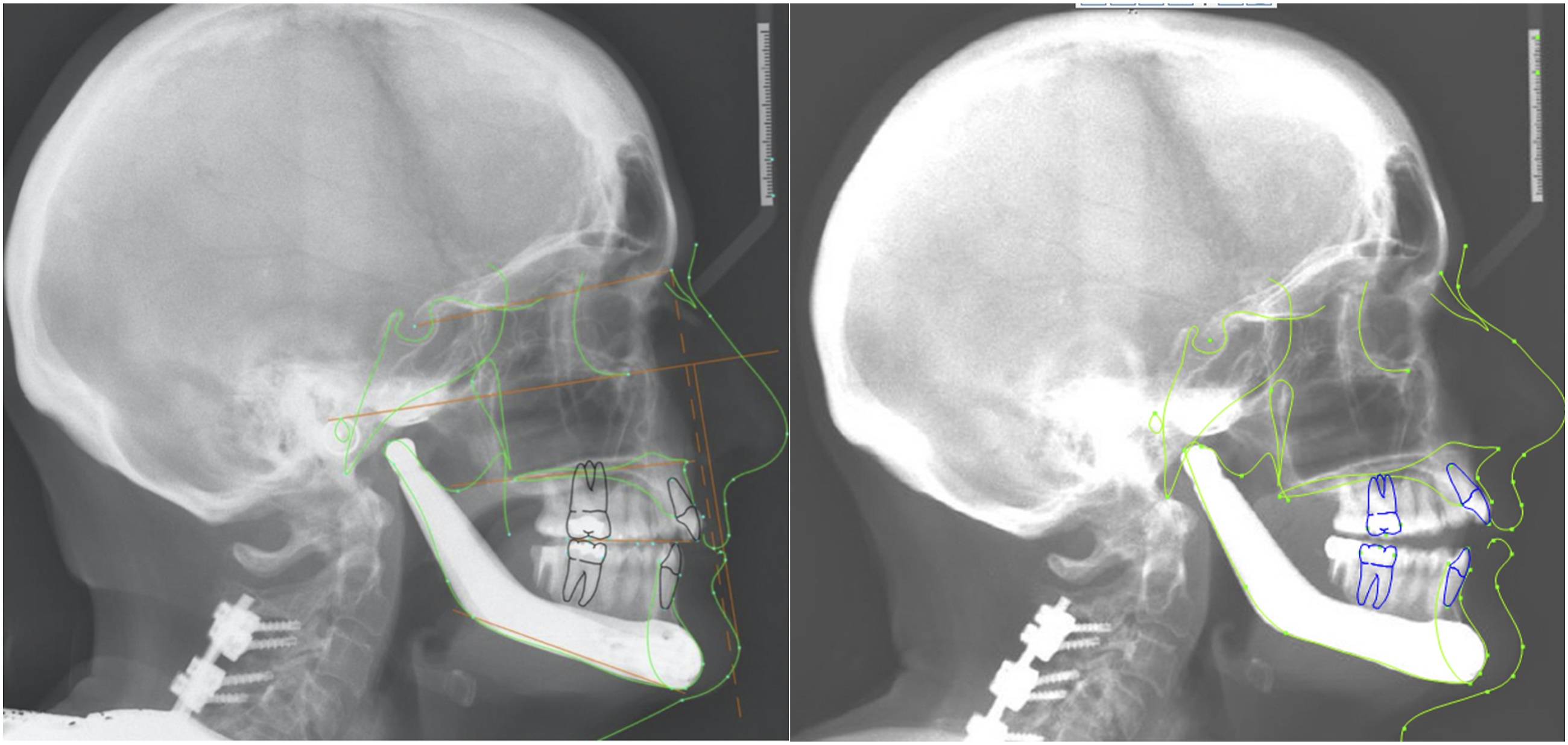
Fifty-four months post-operatively, a progressive malocclusion was noted with Angle class II molars, and a 3 mm anterior open bite (Figures 10–12). Serial cephalometric radiographs (Figure 13) were obtained to assess mandibular skeletal stability (Table 1). In addition, class III mobility of the mandibular incisors with pain was present. Episodic left symphysis pain, described as an electric sensation occurring 4 times per week and lasting for 1 second was reported. The JFLS score was 27. Periapical radiographs of the anterior mandibular dentition demonstrated horizontal bone loss involving teeth #23-26 and widening of the periodontal ligament. Clinically there was evidence of gingival recession and gingivitis in the area. A periodontal and endodontic consultation was ordered. There was no evidence of peri-prosthetic infection in the area, and adequate distance was noted between the prosthetic components and the affected mandibular incisors. (A). From left to right, lateral cephalograms taken in 2014, 2016, and 2019, demonstrating a progression towards an anterior open bite and the Class III molar relationship. There is preservation of forward mandibular projection over time. A. (B). From left to right, profile view from pre-operative state (far left), 2014, 2016, and 2019 (far right). Frontal and intraoral photos of the patient on 2019. Good mandibular range of motion and intact facial nerve is seen. There is an anterior open bite malocclusion, with gingivitis and recession of the mandibular incisors. Panoramic radiograph and periapical radiographs obtained in 2019. There is ongoing resorption of the mandibular body under the right second molar. There is horizontal bone loss involving the mandibular incisors, with widening of the periodontal ligament spaces. Cephalometric study performed on March 2016 and April 2019 follow up. Measurements from Lateral Cephalograms Obtained in 2014, 2016 and 2019.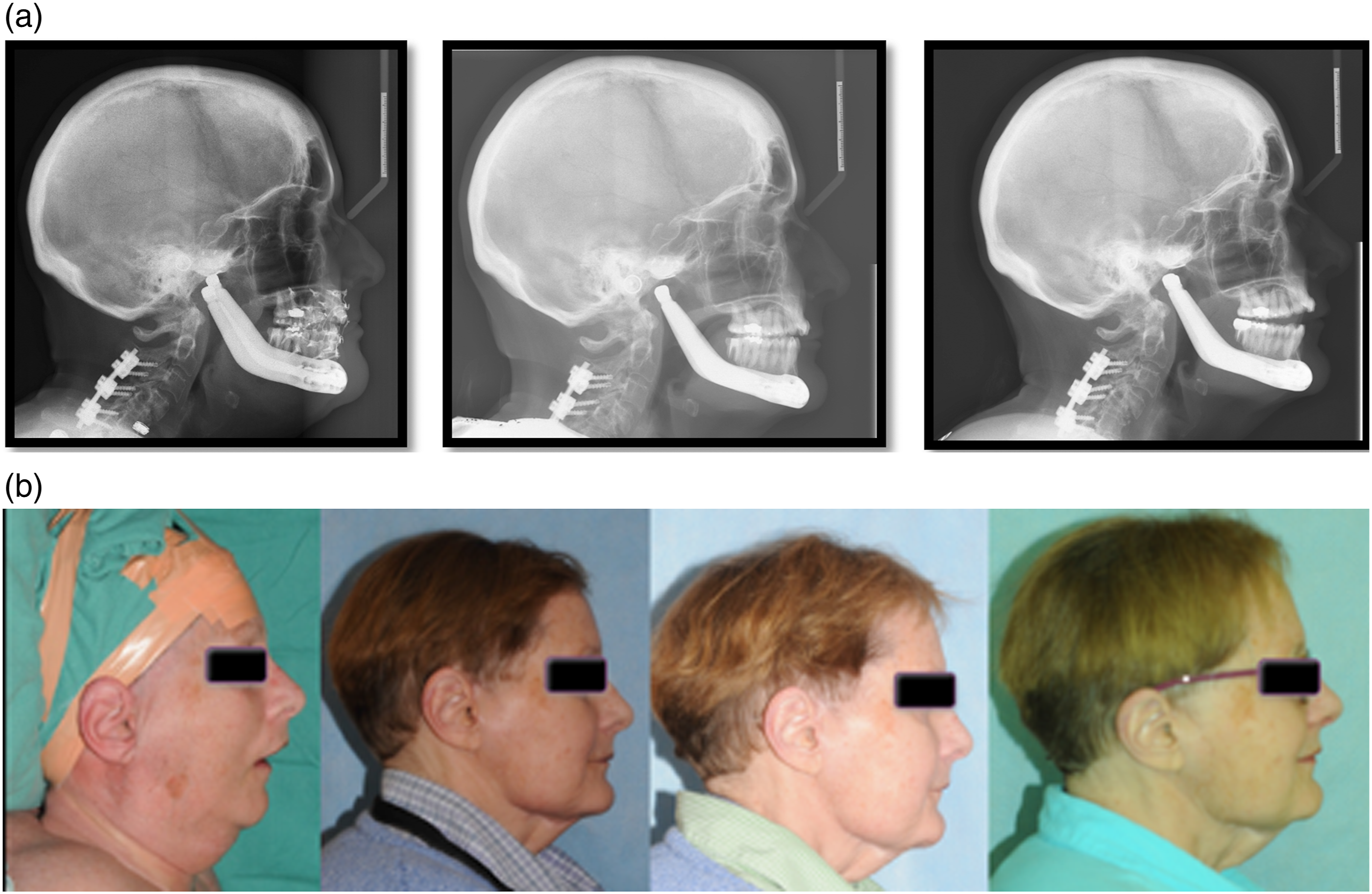
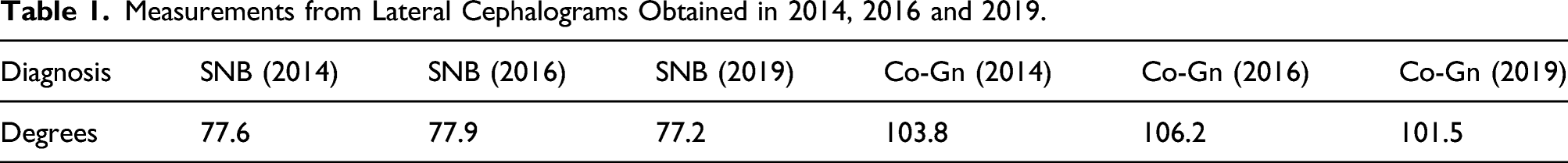
Discussion
Gorham-Stout Disease (GSD) or “Vanishing Bone Disease” is a known cause of extensive mandibular osteolysis. However, a multifocal presentation is not unusual, and requires a thorough clinical and radiographic skeletal survey, as well as laboratory studies and advanced imaging. Since GSD is a diagnosis of exclusion, histopathological examination of the involved tissue is indicated to rule out benign and malignant neoplasms.
In patients with GSD, common sites of involvement include the shoulder and pelvis, but this condition may affect any part of the skeleton including the skull, mandible, humerus, scapula, sternum, ribs and femur.1-4 Involvement of ribs, scapula or thoracic vertebrae may lead to a chylothorax as a result of lymphangiectasia infiltrating the pleural cavity, or via invasion of the thoracic duct, which can lead to protein loss, malnutrition and respiratory distress and failure. 1 The latter sequelae have significant implications on quality of life and prognosis.
At disease onset the radiographic analysis may be consistent with osteoporosis. However, the natural history of the disease is associated with progressive bone loss with the concentric shrinkage of long bones. In some cases, a complete resorption of the bone may occur. 2 Specific to the maxillofacial area, significant progressive resorption of the jaw has been reported.5-8 Initial clinical findings include tooth mobility, tooth loss, and swelling of the jaw, often preceding or presenting with resorption of the mandible.7,9 This process may compromise the upper airway leading to obstruction, and masticatory dysfunction.
Laboratory Tests
In a fatal case report of a 13-year-old boy, the serum alkaline phosphatase level was abnormally increased (728IU/L), and serum phosphorous level was slightly elevated (5.1 mg/dL). However, other hematologic studies were within the normal range (hemoglobin, red blood cell indices, white blood cell count, serum calcium, glucose, urea, creatinine, levels of growth hormone, thyroid-stimulating hormone, free thyroxin, parathyroid hormone, estradiol and insulin-like growth factor). 9 The standard laboratory blood tests are usually within normal limits and are not helpful to make a diagnosis of Gorham-Stout disease. 10 Obstructive sleep apnea has been noted secondary to posterior mandibular displacement and associated posterior displacement of the genioglossus muscle, the principal upper airway dilator. Polysomnography and upper airway imaging is thus recommended. Patients may require treatment with positive airway pressure, or other alternative surgical modalities. Enlargement of the upper airway should be considered when planning surgical reconstruction of the mandible 6
Radiological Findings
During the initial stages, radiolucent foci appear in intramedullary or subcortical spaces similar to those findings on an irregular osteoporosis. With the evolution of the disease, progressive slow atrophy occurs. Fractures, fragmentation and vanishing of a portion of the bone are also found. Bone scintigraphy may show increased vascularity in the affected area, and posteriorly, a decreased uptake related to the absent osseus tissue. On MRIs, an uniformly low signal intensity is observed on T1 weighted images, whereas an increased signal intensity is observed on T2 weighted images. 1 In the maxillofacial area, significative resorption of the mandible is found and additional head and neck bones can be involved such as the mastoid process of the temporal, and the hyoid bone.8,9
Differential Diagnosis
Acro-osteolysis has been reported in various conditions such as Hadju-Cheney syndrome, idiopathic multicentric osteolysis, multicentric osteolysis with nephropathy, hereditary multicentric osteolysis, neurogenic osteolysis, acro-osteolysis of Joseph, acro-osteolysis of Shinz, Farber’s disease, Winchester’s Syndrome and osteolysis with detritic synovitis. These are conditions that may resemble vanishing bone disease. The differential diagnosis should be considered based on history, physical examination, serologic testing, radiological studies and biopsies in order to exclude the aforementioned diseases. 1 The histopathologic analysis of GSD consists of a nonspecific fibrovascular tissue infiltrated with chronic inflammatory cells and vascular proliferation and numerous distended thin-walled capillaries.3,9,11 Neoplasia should be ruled out with tissue biopsy as well. This patient was initially felt to have Hadju-Cheney Syndrome which is a rare autosomal dominant mutation in the terminal exon of the NOTCH2 gene. The latter is a skeletal disorder characterized by short stature, coarse and dysmorphic facies, bowing of the long bones, and vertebral anomalies. Facial features include hypertelorism, bushy eyebrows, micrognathia, small mouth with dental anomalies, low-set ears, and short neck. There is progressive focal bone destruction, including acro-osteolysis and generalized osteoporosis. Additional and variable features include hearing loss, renal cysts, and cardiovascular anomalies.
Gorham-Stout Disease in the Craniofacial Region
Considering the rarity of the disease, there are 456 case reports describing varying presentations and complications of Gorham-Stout Disease in the literature. The vast majority of the published craniofacial cases reported show initial involvement of the mandible, and later progression to other bones of the maxillofacial region. Typically, the basal bone of the mandible is involved, with osteolysis extending to the mandibular ramus. Involvement of the periodontal ligament may lead to tooth mobility and loss of teeth. In a multifocal variant, the disease may affect frontal, zygomatic and temporal bones. The disease results in a dissolution of the cortical and cancellous bone through the substitution of bone for connective tissue containing dilated capillaries that culminates in fibrous bands that occupies the osseous tissues. 12
The airway deserves special attention in advanced cases of GSD. Posterior retro-positioning of the mandible, which developed as osteolysis of the rami progresses, may lead to obstructive sleep apnea. Ongoing and peri-operative management of OSA, as well as adequate post-operative monitoring, is essential to avoid severe airway complications. Reconstructive mandibular surgery should aim to restore the original A-P positioning of the mandible. 6
In this case, a C-spine fusion with recombinant human bone morphogenetic protein-2 in the setting of mandibular de-projection led to postoperative airway obstruction, and eventually pulseless cardiac arrest requiring resuscitation and emergent tracheotomy. This highlights the importance of screening for OSA prior to surgery in a patient with retrognathia or other symptoms of sleep disordered breathing, and assessment with a polysomnogram and treatment of underlying OSA as indicated to mitigate the risk of airway compromise.13,14
Treatments for GSD in Craniofacial Region
Given the rarity of this disease entity, there is no standard therapy available. Medical treatment for Gorham-Stout disease may include low-dose radiation therapy (up to 30-50 Gy) during the active phase of osteolysis, chemotherapeutic drugs, or a combination thereof. Surgical treatment may include biopsy, debulking, curettage, enucleation, as well as marginal or segmental resection of the affected areas. Surgical resection is usually followed by reconstructive efforts such as reconstruction plates, autogenous bone grafts, free tissue transfer, alloplastic grafts such as polymethylmethacrylate (PMMA), and total temporomandibular joint (TMJ) arthroplasty with extended alloplastic implants for reconstruction of the TMJ and mandible.1,2,8,15 Autogenous options for mandibular reconstruction, both vascularized and not, have been susceptive to resorption and may be less predictable than alloplastic material. Despite a paucity of data on outcomes of reconstructive options in cases of mandibular involvement, experience with custom long-span alloplastic temporomandibular joint implants suggests that this represents a predictable treatment option in the setting of ongoing bony osteolysis, and may be used with or without microvascular free tissue transfer to replace the entire mandible in severe cases.7,16 Use of Hegar dilators in this case, facilitated the creation of a soft tissue tunnel between the existing mandibular body and temporal fossa. In this case, mandibular projection has been maintained, however, the development of progressive apertognathia is indicative of ongoing disease activity affecting osseous and periodontal tissues.
Conclusion
This report describes a case of multifocal GSD with numerous systemic complications, including a pathologic mandible fracture, surgical complications after bone grafting and fracture stabilization, obstructive sleep apnea (OSA), as well as post-operative airway obstruction and cardiopulmonary arrest following C-spine fusion. In the management of patients with mandibular resorption of unknown cause, clinicians should perform a comprehensive work-up, consider ruling out malignancy (GSD is a diagnosis of exclusion), screen for OSA, and consider a multi-disciplinary approach to identify and manage all affected organs and portions of the skeleton. Custom long-span alloplastic temporomandibular joint implants represent a biomechanical option that may be used to replace large segments of the mandible without the risk of resorption. In anticipation of progressive bony osteolysis, consideration should be given to extend these alloplasts beyond the margin of active disease if clinically feasible.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
