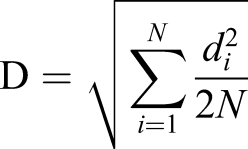Abstract
Introduction
We aimed to determine the ratios of the lower and upper lip landmarks in the sagittal and vertical direction for maxillary osteotomies and mandibular lengthening surgeries, in a prospective way.
Methods
This prospective cohort study is the second part of the OSRES (Orthognathic/orthofacial Surgery RESearch group); patients that underwent mandibular and/or Le Fort I surgery without genioplasty were included. Pearson correlation determined significant patient and surgical variables. The relationship between hard and soft tissue changes was determined by correlation analysis.
Results
An average ratio of 103% was found for sB:B for mandibular advancement surgery without genioplasty and 83% for sB:Pg with genioplasty. Lower jaw surgery yielded a ratio of 68% for Li:Ili in the horizontal direction and 69% with a genioplasty. Displacement of the upper jaw gave a ratio of 83% for Ls:Iui anteriorly for all surgery groups combined. Horizontal displacement of the upper jaw yielded a strong correlation with a ratio of 88% for sA:A.
Conclusions
The equations presented in this study for landmark sB, sA, labrale inferius, and labrale superius can aid preoperative planning of lip position. No accurate way was found to predict stomion inferius and stomion superius.
Highlights
We prospectively arranged for computerized measurements of sB:B, Li:Ili, Ls: Iui, Stoi:Ili, Stos: Iui, and sA:A ratios on lateral cephalograms using FaceWizz. The influences of direction and the type of surgery were studied. Moderate to strong correlations were found for horizontal ratios of sB:B, Li:Lli, Ls:Iui, and sA:A. Weak correlations were found for vertical movement of Stos:Iui and Stoi:Ili.
Introduction
Positioning osteotomies, including of the anterior dentition, affect the position and seal of the lips and may also affect their thickness and length. Numerous retrospective studies have defined the ratios between the changes in anterior jaw position and lip profile, only to conclude that great variation is present at the midline.1-4 We conducted a systematic review with regard to changes in the lip region after upper jaw and bimaxillary surgery.1,2 The identified studies with regard to midline lip changes used a variable study methodology and were retrospective; consequently, clear outcomes could not be deduced from these results. Parasagittal quantitative data are lacking, contemporary 3D models generated by soft tissue simulation software assign isotropic and linear elastic properties to the lips when displaced by underlying hard tissues, which may not be realistic.5,6 The upper lip is supported by the upper teeth and their supporting alveoli. The lower lip vermillion is supported by the upper and lower incisors; the caudal part of the lower lip is supported by the alveolar process of the mandible. By better understanding the soft tissue response from changes in the position of the alveolar process and anterior dentition, we can more accurately plan with the “face-first approach.” 7
The objective of this study was to perform a cephalometric analysis of the displacements of the lower and upper lip landmarks (Figure 1) [soft point A (sA), labrale superius (Ls), stomion superius (Stos), stomion inferius (Stoi), labrale inferius (Li), and soft point B (sB)], with dental [lower incisor (Ili) and upper incisor (Iui)] and osseous displacements [pogonion (Pg), point A (A), and point B (B)] resulting from lower or upper jaw osteotomies. Variables were specific osseous components and movement directions. To assess the changes, we quantified soft tissue changes of the upper and lower lip ratios (with multiple and linear regression analysis) after orthognathic surgery. Cephalometric landmarks in FacewizzExplanation of the landmarks: Or (orbitale), most inferior point of the right infraorbital rim; Po (porion), most superior point of each external acoustic meatus (averaged when a double contour); A, point of maximum concavity in the midline of the alveolar process of the maxilla; B, point of maximum concavity in the midline of the alveolar process of the mandible; sA, the most posterior midpoint of the philtrum; sB, most posterior point on the labiomental soft tissue contour on a horizontal plane parallel to Frankfort plane; Ili (lower incisor), most cranial point of the tip of the crown of each lower central incisor, Iui (upper incisor) most caudal point of the tip of the crown of each upper central incisor; Li (labiale inferius), the most anterior point of the vermillion line of the lower lip; Ls (labiale superius), the most anterior point of the vermillion line of the lower lip; Stoi (stomion inferior), highest point on the upper border of the lower lip; and Stos (stomion superior), lowest point on the lower border of the upper lip.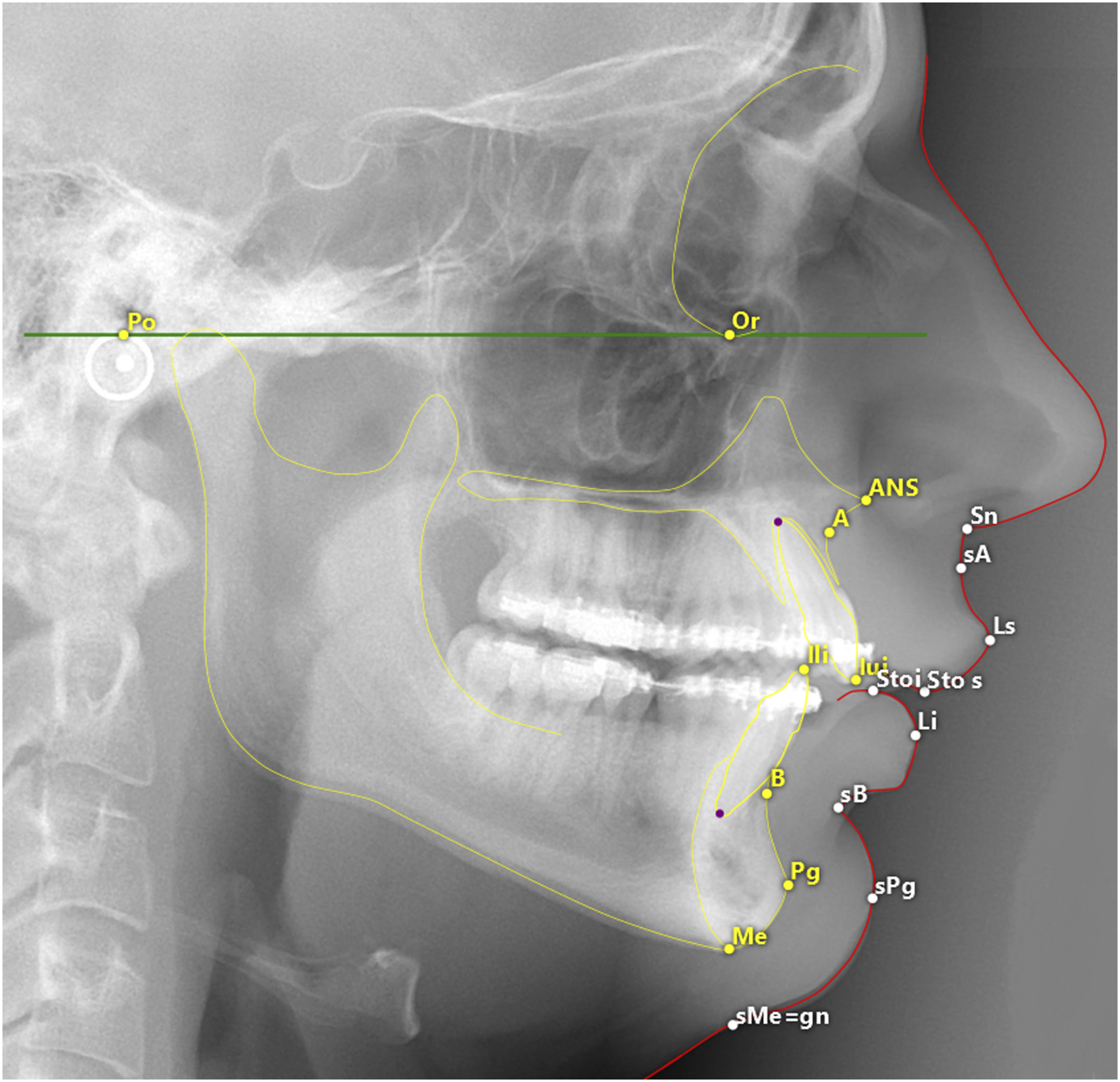
Material and Methods
Subjects and Inclusion/Exclusion Criteria
This study is the second of a series using the international Orthognathic/Orthofacial Surgery Research Study prospective registry. 8 The study was approved by the Ethics in Research Committee of the Universidad de La Frontera (protocol number 066/13). The study protocol was independently reviewed and approved by the internal ethical committees of the Universidad de la Frontera in Temuco (Chile), the European Face Centre at the Universitair Ziekenhuis Brussel (Belgium), the Hospital Sant’ Anna e San Sebastiano in Caserta (Italy), and the Amphia Ziekenhuis in Breda (the Netherlands). All participants provided written informed consent.
A total of 192 subjects from the database were eligible for inclusion in the study; however, 34 subjects were excluded due to incomplete data. Of these 34 subjects, 28 subjects were missed in follow-up and 6 subjects had brackets on their postoperative radiograph. The 158 included subjects (61 males and 97 females; mean age, 24 years 8 months; SD, 12.27) had mandibular advancement and maxillary or bimaxillary surgery with or without genioplasty between July 2016 and January 2020 at the 4 participating institutions. Subjects of any sex, age and ethnicity were eligible for inclusion; however, only Caucasian subjects were included. Subjects with a history of facial trauma, facial asymmetry with a chin midline deviation greater than 5 mm, or any malformation syndrome were excluded. Various surgeons operated on the included subjects using different surgical techniques and fixation methods. Mandibular positioning was performed using bilateral sagittal split osteotomies (BSSOs). Maxillary (Le Fort I-type) surgery was performed using the subspinal approach. Subjects who had undergone a classical Le Fort I-type osteotomy with detachment of the nasolabial muscles and subsequent cinch sutures and/or a conventional V-Y closure were excluded. 9 The sample population included all cases who had undergone the abovementioned surgeries and excluded all records that showed breaches of the standardization protocol. The number of mandibular setback surgeries (2) was too low for statistical analyses. To determine lower lip soft tissue ratios, subjects were categorized into the following subgroups: mandibular advancement surgery, mandibular advancement surgery with Le Fort I-type osteotomy, mandibular advancement surgery with Le Fort I-type osteotomy and chin osteotomy, and mandibular advancement surgery with chin osteotomy. To determine upper lip soft tissue ratios, the same subjects were categorized into the following subgroups: subspinal Le Fort I-type surgery with or without genioplasty and subspinal Le Fort I surgery and lower jaw advancement surgery with or without genioplasty.
Cephalometric Data
Lateral cephalograms were taken less than 1 month before surgery (preoperative baseline: T1) and after removal of the fixed orthodontic appliances (>6 months postoperatively: T2). Both cephalograms were taken at each institute using the same setup and craniostat for each subject, in centric dental occlusion and with the lips in repose. Because the ratios, not the distances, were analyzed, the (digitally corrected) focus-to-object (film) distances were not a problem, as long as they remained the same for each subject.
The T1 and T2 cephalograms were digitized using Facewizz software, version 1.2.4 (Orthoface R&D bvba, Sint-Martens-Latem, Belgium). The cephalograms were analyzed using a number of specified landmarks (Figure 1). A Cartesian coordinate system was used to register the position of the hard and soft tissue landmarks. The Frankfort horizontal plane was used as the x-axis and a line perpendicular through the porion was assigned as the y-axis. Facewizz was used to automatically designate the x- and y-axes after selection of the porion and orbitale landmarks as well as the x,y-coordinates after identification of the position of the landmarks.
The T2 cephalogram was superimposed on the T1 cephalogram using the manual best fit of cranial base structures. 10 Landmark displacements and ratios were calculated using the software.
Statistical Analyses
We performed statistical analyses using SPSS (version 25.0, SPSS, Chicago, IL). The Kolmogorov–Smirnov test was used for P values less than .05 to evaluate whether the continuous variables were normally distributed. Outliers were identified and confirmed to ascertain that no measurement error was present. Outliers with displacements of the dependent variable more than 1 mm were excluded. Independent t test analysis was used to determine the statistical association between predictor variables and the primary outcomes. The data were pooled depending on the results of the t-test.
The relationship between changes in the hard and soft tissues was tested using linear correlation analysis. The degrees of correlation were calculated as follows: weak correlation (r < .5), moderate correlation (.5 < r < .8), and strong correlation (r > .80). A multiple linear regression analysis was performed if multiple statistically significant correlations were found. Data was also tested using a simpler model to determine whether it could yield a better model. A two-tailed P value less than .05 was considered to be statistically significant.
Variations in image acquisition were not assessed as they could only be limited by requesting that the participating department use the same equipment for the pre- and postoperative radiographs.
To analyze measurements errors, 10 duplicated random data sets were digitized for pre- and postoperative cephalograms for the same investigator (AB) with a 2 weeks interval.
Measurement errors regarding the placement of the landmarks were calculated using the Dahlberg formula
Pearson’s correlation coefficient was calculated to determine the displacements of sB, sA, Li, and Ls in the horizontal direction and of B and Pg, A, Ili and Pg, and Iui, respectively. The Pearson correlations between Stoi in the vertical direction and the displacement of Ili and Pg were determined as was the correlation of Stos and Iui in the vertical direction. Multiple regression analyses were made with the specific landmarks, which showed a significant linear correlation with the displacement of a soft tissue landmark. For dependent variables sB, sA, Li, and Ls, analyses in the horizontal direction were performed; analyses for Stos and Stoi in the vertical direction were also conducted. The independent variables were the vertical and horizontal changes in B, Pg, A, Ili, and Iui.
Results
Error of the Method
The error inherent in the method differed between .15 mm and .63 mm for hard and soft tissue landmark placement on the y- or x-axis. The Dahlberg error was lower than 1 mm, which confirms the high reliability of the measurements. 12 The error variance, as a percentage of the total variance between the pre- and postoperative measurements, was 2.6%, 1.9%, 3.2%, 2.4%, 3.1%, 4.4%, 9.8%, and 6.1% for the x-coordinates of sB, B, sA, A, Ili, Iui, Li, and Ls, respectively, and 1.9%, 6.2%, 5.1%, and 18.7% for the y-coordinates of Ili, Iui, Stoi, and Stos, respectively.
Distribution and Correlation Between Hard and Soft Tissue Movements
All measured landmarks were normally distributed as were their pre- and postoperative changes (P < .05).
Independent t-tests for surgical groups and direction of displacement.
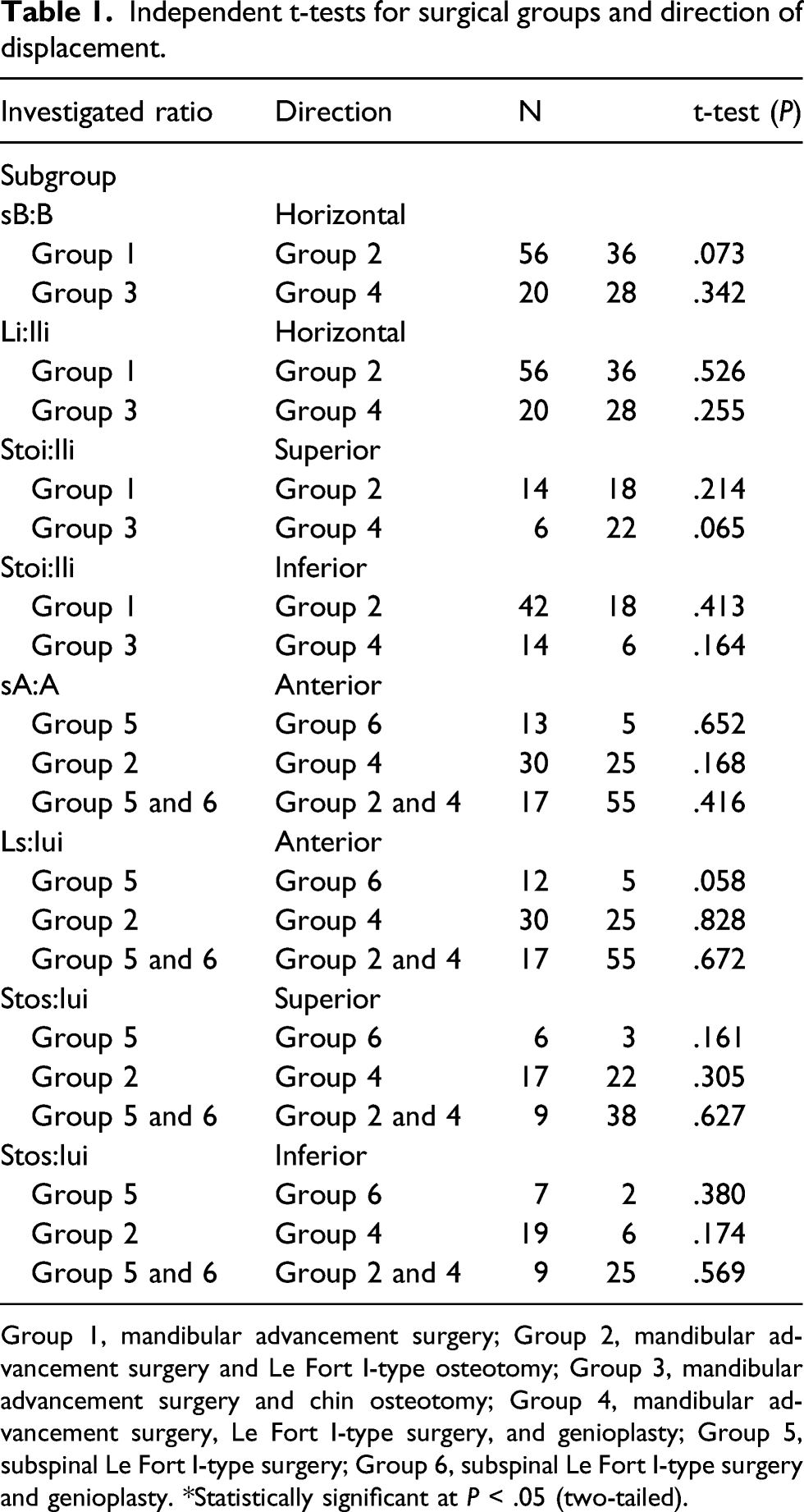
Group 1, mandibular advancement surgery; Group 2, mandibular advancement surgery and Le Fort I-type osteotomy; Group 3, mandibular advancement surgery and chin osteotomy; Group 4, mandibular advancement surgery, Le Fort I-type surgery, and genioplasty; Group 5, subspinal Le Fort I-type surgery; Group 6, subspinal Le Fort I-type surgery and genioplasty. *Statistically significant at P < .05 (two-tailed).
Horizontal Displacement of the Mentolabial Fold
We calculated the correlations for all BSSOs and/or bimaxillary surgeries separately from the groups that included genioplasty. There was no further subgrouping for the statistical analysis because no statistically significant differences were found between the ratios (Table 1).
Pearson test (correlation coefficient) for determining correlations between cephalometric landmarks.
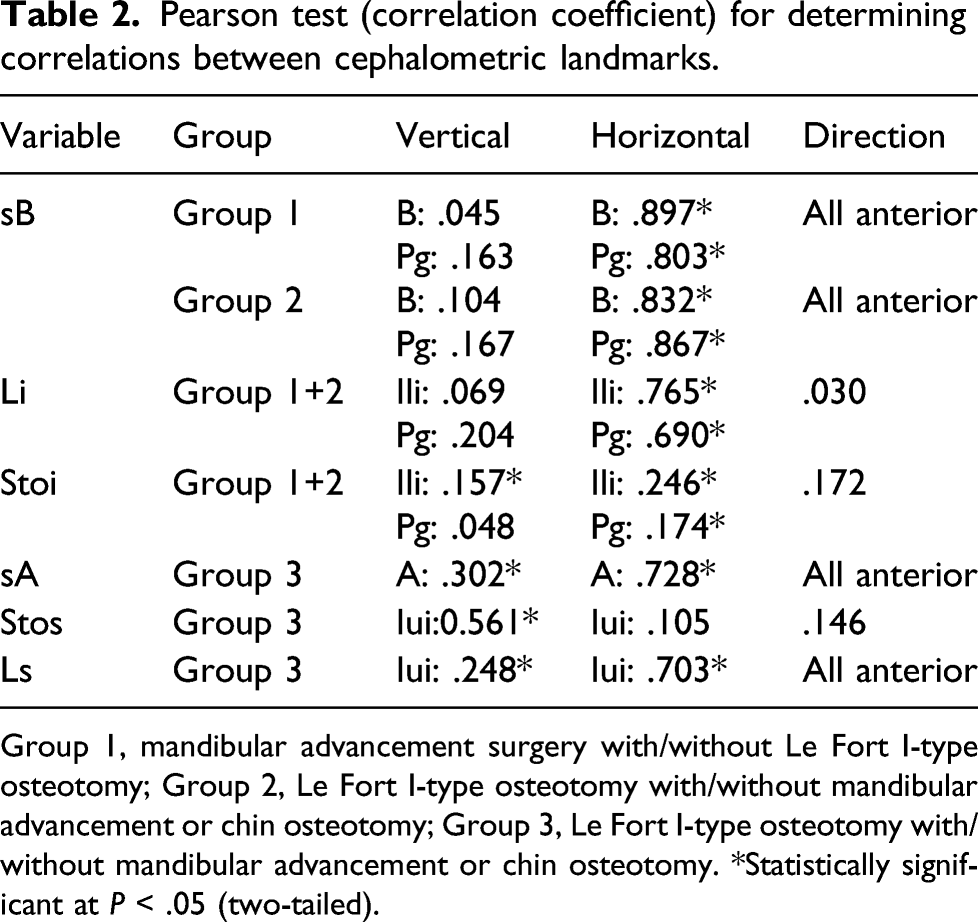
Group 1, mandibular advancement surgery with/without Le Fort I-type osteotomy; Group 2, Le Fort I-type osteotomy with/without mandibular advancement or chin osteotomy; Group 3, Le Fort I-type osteotomy with/without mandibular advancement or chin osteotomy. *Statistically significant at P < .05 (two-tailed).
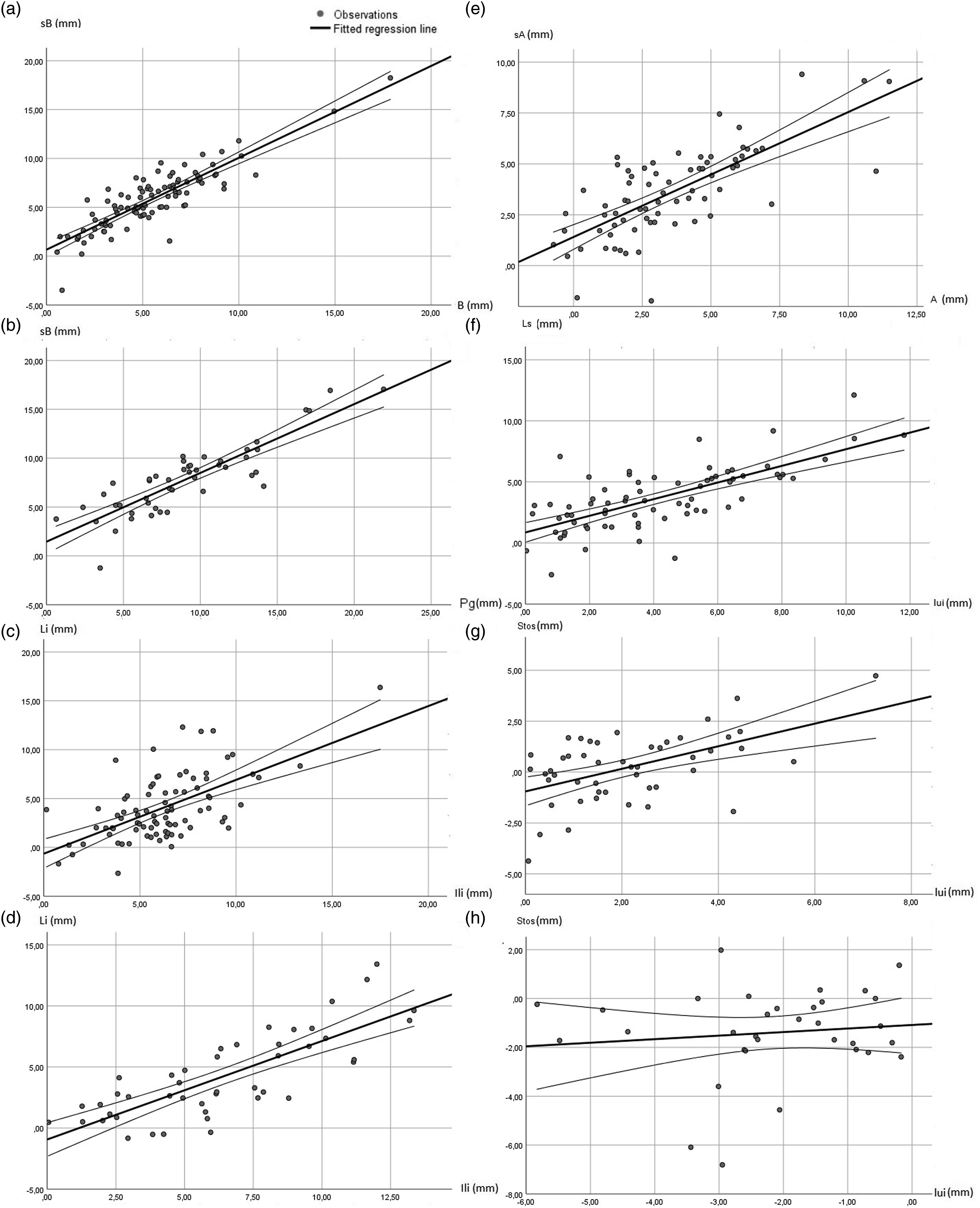
Linear correlation of the horizontal displacement of point B and the soft tissue point B for the mandibular advancement surgery group with or without Le Fort I-type osteotomy (A) and for soft tissue point B and pogonion for the mandibular advancement surgery group with or without Le Fort I-type osteotomy with genioplasty (B); anterior horizontal displacement of point Ili and Li for the mandibular advancement surgery group with or without Le Fort-type osteotomy (C) and for the mandibular advancement surgery group with or without Le Fort I-type osteotomy with genioplasty (D); anterior horizontal displacement of point A and point sA for the Le Fort I-type and (E) anterior horizontal displacement of Iui and Ls for the subspinal Le Fort I-type surgery group with or without additional lower jaw surgery (F); and the vertical displacement of the upper incisor and stomion superius for the subspinal Le Fort I-type surgery group with or without additional lower jaw surgery in the superior (G) and inferior (H) directions.
Linear regression equations and ratios for specified landmarks on x- and y-axes.
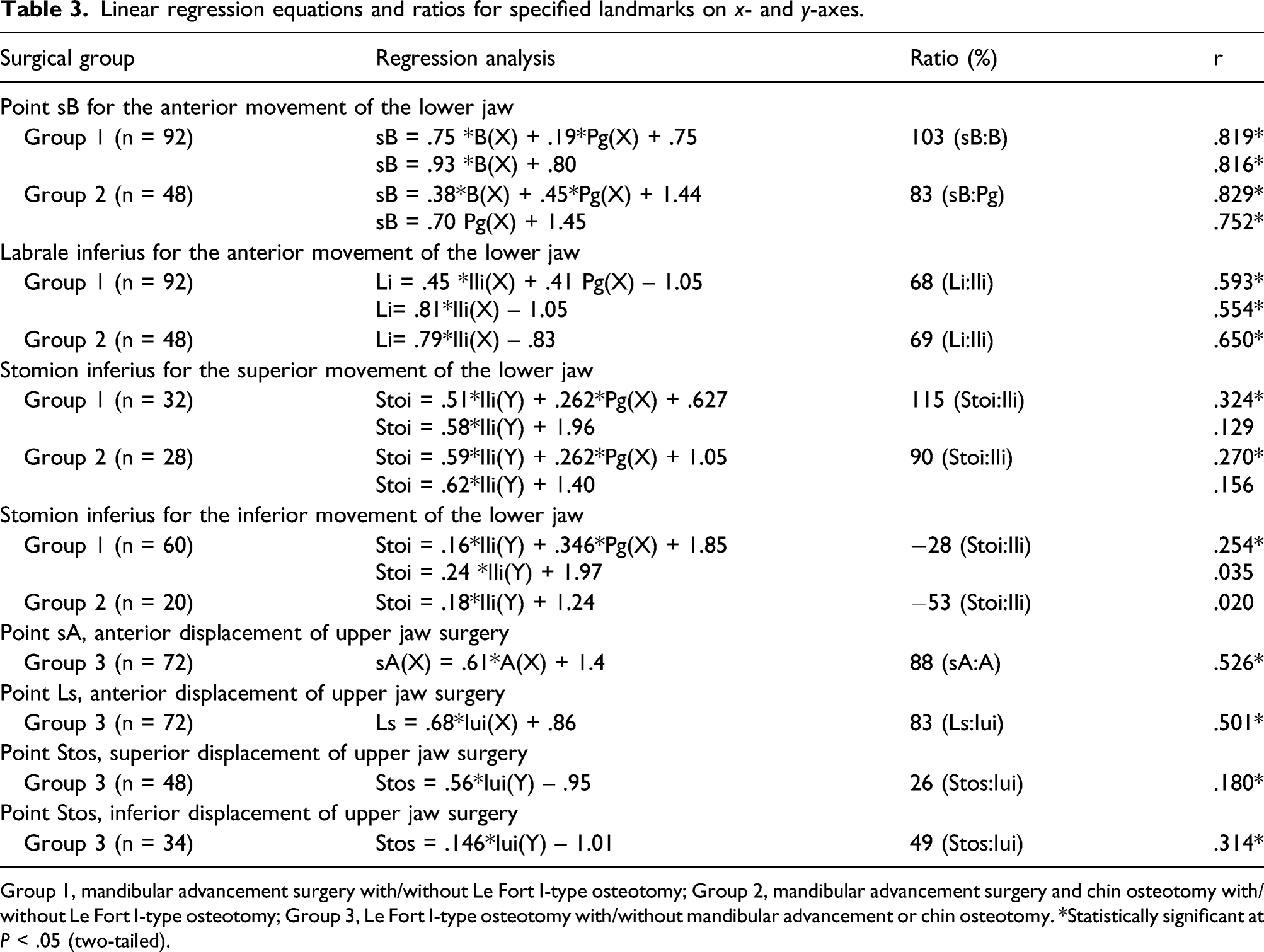
Group 1, mandibular advancement surgery with/without Le Fort I-type osteotomy; Group 2, mandibular advancement surgery and chin osteotomy with/without Le Fort I-type osteotomy; Group 3, Le Fort I-type osteotomy with/without mandibular advancement or chin osteotomy. *Statistically significant at P < .05 (two-tailed).
Displacement of the Lower Lip
The results of the t tests showed no differences between the subgroups for the Stoi:Ili and Li:Ili ratios. Hence, we combined these groups when determining the correlation equation (Table 2). No outliers were excluded for the measurements of the horizontal and vertical displacements.
There was a linear correlation between the horizontal changes in Li and the Ili and Pg landmarks. The best-fit line was Li = .45 *Ili(X) + .41 Pg(X) – 1.05 (R2 = .593) for the horizontal change of Li for the mandibular surgery group with or without upper jaw surgery. The linear equation (Li = .81*Ili – .83), which is dependent only on Ili, yielded a lower R2 value of .554 (Figure 2C and Table 3). For the mandibular surgery group with genioplasty and with or without upper jaw surgery, the equation Li = 0-79*Ili(X) – .83 with an R2 of .677 was used (Figure 2D and Table 3).
There was a weak correlation between the movements of Stoi and Ili [horizontal: r = .246; P < .05 and vertical (Y): r = .157, P < .05] and Pg [horizontal (X): r = .174; P < .05]. A multiple linear equation for the Stoi:Ili ratio in the cranial direction was used for the mandibular and bimaxillary surgery group without genioplasty: Stoi = .51*Ili(Y) + .262*Pg(X) + .627 (R2 = .324). An average ratio of 115% was found for Stoi:Ili for superior vertical movements (Table 3). For the superior movement of the mandibular surgery with genioplasty group, we used equation Stoi = .59*Ili(Y) + .262*Pg(X) + 1,05 (R2 = .270). No equation was used with only one independent variable for either group.
For the inferior movement of the lower jaw, a significant regression equation for the lower jaw and bimaxillary surgery group without genioplasty was used: Stoi = .16*Ili(Y) + .35*Pg(X) + 1.85 (r = .254). A constant .75-mm superior movement of Stoi was accompanied by the linear movement of Stoi equal to 16% of the change in Ili(Y). The anterior movement of Pg equals a respective superior movement of 35% for Stoi. No statistically significant equation was used for the lower jaw and bimaxillary surgery with genioplasty group (Table 3).
Displacement of the Upper Lip
Results of the t tests showed that for the Ls:Iui ratio in the anterior direction, there was no statistical difference (P = .672) with regard to the surgical subgroup. The ratio for the vertical movement of Stos:Iui showed no statistically significant difference with regard to differences in the t test results (P = .627). For the horizontal and vertical displacements, no outliers were excluded. For the sA:A ratio, no statistically significant differences were found with regard to the surgical subgroup (P = .416); therefore, these data were analyzed as a single group (Table 1). The data showed one outlier, which was excluded for statistical data analysis. There was an insufficient amount of data for the Ls:Iui and sA:A ratios with regard to the posterior displacement of the upper jaw. The horizontal displacement of Ls showed a low correlation with the displacement of Iui in the vertical direction (r = .248, P < .05) and a moderate correlation in the horizontal direction (r = .703, P < .05). A moderate correlation was found between the vertical movements of Stos and Iui (r = .561, P < .05). The horizontal displacement of sA showed a low correlation with the displacement of A in the vertical direction (r = .302, P < .05) and a moderate correlation in the horizontal direction (r = .728, P < .05).
The horizontal movement of sA yielded the following equation: sA(X) = .61*A(X) + 1.4 (R2 = .506) (Figure 2E and Table 3). There was an average ratio for sA:A of 88% for the horizontal movements.
For the anterior movement of Iui, the equation Ls = .68*Iui(X) + .86 (R2 = .501) was used with an average ratio of 83% (r = .813) (Figure 2F). The linear equation Stos = .56*Iui(Y) – .95 was used for superior movement (Figure 2G and Table 3). The constant, showing an inferior displacement of .95 mm, was accompanied by the linear movement of Stos equal to 56% of the superior movement of Iui(Y). A significant ratio was found for Stos:Iui, showing a vertical displacement of 26% for Stos in relation to the superior displacement of Iui. The inferior displacement of the upper jaw yielded the equation Stos = .15*Iui(Y) – 1.01 with a ratio of 49% (Figure 2H and Table 3), showing an inferior displacement of 1.01 mm and a linear displacement equal to 15% of the inferior movement of Iui(Y).
Discussion
This study was undertaken to explore the use of soft-to-hard tissue ratios in the midline lip area for mandibular, maxillary, and bimaxillary surgeries. A prospective registry design was chosen because randomization of surgical indications is impossible: Orthognathic surgery is typically performed to correct a specific malocclusion and improve facial aesthetics. The surgical indications were not influenced by inclusion of subjects in this registry, only by the surgeons’ preoperative planning in agreement with the subjects’ preferences.
The population of 158 subjects was relatively large but still heterogenous regarding affected jaws and direction and displacement of the jaw segments. Posterior maxillary displacements were not analyzed due to the small population size. Mandibular setback was only performed in 2 subjects in the prospective cohort. These subjects were not included in the analysis.
The Dahlberg 11 error analysis was chosen because of its simple interpretation and preservation of the original units (mm). The variance of error exceeded 10% of the total variance for the landmark Stos compared to the variances of the pre- and postoperative landmarks. The small average displacement of Stos after surgery is the cause of this high variance. While the Dahlberg analysis showed that the applied measurements were appropriate, the error intrinsic in the method compared to the displacements of pre- and postoperatively placed landmarks can be considered of major importance. 12 This is a confounding factor in the statistical analysis of this specific landmark.
A recent systematic review revealed that the average ratio for the anterior movement of the lower jaw was close to 100% when bimaxillary surgery was performed. 2 Results of another systematic review regarding the anterior advancement of the lower jaw after BSSO revealed the same ratio of 100%. 13 These data are consistent with our results. The strong correlation (r = .816) and narrow spread (Figure 2A) shows that point B is a good predictor of the displacement of sB. If genioplasty is included, the ratio of sB:Pg produced the best results. Point B was less effective because a chin osteotomy is inferior to point B, so the anterior displacement of the osseous chin is not represented by the displacement of this landmark. A systematic review by Olate et al. found ratios ranging from 55% to 99% for bimaxillary surgery, while a ratio of 50% was found for lower jaw advancement surgery.2,13 The literature reveals that with lower jaw surgery only, the lip will curl backwards to a greater extent than with bimaxillary surgery; this may be due to the displacement of the upper incisors. Our study did not find any influence by the type of surgery performed. A similar ratio of 69% was found if genioplasty was performed; a higher ratio might be expected due to the impact of genioplasty on the soft tissue of the chin. 13 A weak correlation was found for the placement of Stoi in the superior and inferior directions. A large part of the subject group had an open lip posture on the preoperative cephalogram, where the anteroposterior position of the lower jaw was partially responsible for this open lip posture. An ideal anteroposterior position improves lip closure and tone. 14 Anterior displacement toward an ideal jaw relation yields an average superior movement of Stoi in subjects with an open lip relationship. The factors responsible for the difficulty in predicting postoperative vertical lip position are the relaxation of the lip posture at the moment of radiographic exposure and postoperative changes in lip tonicity. In this study, the small vertical changes in Ili were weakly correlated with postoperative vertical lip position. The anterior displacement of the mandible toward an ideal esthetic profile improves lip seal; however, a predictable outcome of this cranial displacement of Stoi could not be determined.
A previous study showed ratios of Ls:Iui between .4:1 and .80:1 for Ls:Iui compared to our ratio of 83%; however, these osteotomies were performed using a conventional technique in which the nasolabial muscles are detached from the anterior nasal spine. 1 These data show that the adverse thinning of the lip is generally less for a subspinal osteotomy than for previously studied maxillary advancement osteotomies. If both VY cheiloplasty and cinch sutures are performed during a maxillary or bimaxillary surgery, this ratio is found to be comparable to the ratios found in our study. 1 However, lip lengthening is prone to relapse and unwanted extensions at the middle of the upper lip due to the nature of a VY cheiloplasty. 15 Studies concerning setback osteotomies found ratios between .53:1 and .75:1. 1 The number of subjects who underwent Le Fort I-type setback surgery was too small to calculate any ratios for upper lip changes after surgery.
A low correlation was found for the superior displacement of Iui with a ratio of 26% for Stos:Iui. A previous study showed similar results for bimaxillary surgery without VY closure with a ratio for 13% for upper jaw impaction. 2 During a maxillary impaction surgery, ratios between 32% and 42% were calculated for the ratio of Stos:Iui without VY closure. 1 A subspinal osteotomy shows similar results for the lengthening of the upper lip using jaw impaction compared to conventional Le Fort I-type surgical techniques without VY plasty. The aforementioned measurement bias and high spread of calculated ratios might be responsible for the low R2 value of .180, and lip tone might also contribute to the low value. For disimpaction surgery, we found a similarly weak correlation. The ratio we found was 49%, which is similar to the value of 57% found in the literature. 1 Equations for both impaction and extrusion used a constant of around 1 mm, which suggests that incision on its own is able to lengthen the upper lip approximately 1 mm.
For the horizontal sA:A ratio, we found a moderate correlation with a ratio of 88%, indicating that this is a good ratio to accurately predict postoperative changes. This ratio is higher than those found in previous studies for bimaxillary surgery, which ranged from 61% to 76%. 2 The ratio for advancement during monomaxillary surgery ranged from 39 to 66% in the literature, 1 suggesting that there is less thinning than was previously shown for Ls:Iui, which is important for the thickness of the vermillion. The difference between our study and previous studies might be due to subspinal osteotomies, which keep the paraspinal muscles intact. Loss of tension of the lateral midface musculature may be responsible for flattening and diminishing the anterior projection of the upper lip. 16 The thickness of the upper lip is an important indicator of youth and attractiveness, which can diminish after upper jaw advancement surgery.
The predictive value of equations using Stoi and Stos is more limited than for equations using sB:B and sA:A due to the important effects of the perioral musculature on lip posture. Changes in the resting lip position are mostly dependent on changes in the perioral musculature. 13 These changes together with the displacements of the lower and upper incisors yield equations that are unable to precisely predict horizontal and vertical lip positions. The ability of three-dimensional planning software to predict lip position is fully based on the elasticity of the tissues in response to the displacement of underlying hard tissues, which is probably less reliable. 17 Due to the high influence of the perioral musculature, it is highly unlikely that this approach can produce accurate results. Future inclusions in the prospective registry will allow us to more precisely analyze ratios and may yield a more precise equation with multiple variables to increase the accuracy of soft tissue landmark prediction. These ratios can be used in three-dimensional orthognathic planning software. Currently, the use of two-dimensional planning software that includes our findings will yield the most predictable soft tissue changes and will be more useful in a “face-first approach.” After all, most subjects require corrections in the anterior direction (mandibular lengthening to correct a dentoskeletal Class II malocclusion) and cranial direction (maxillary impaction osteotomy to create a proper lip seal and correct a long face). Minor corrections (not in the soft tissue profile) are necessary to correct midline deviations, prevent yaw asymmetries, and correct occlusal cants. These corrections can be currently accomplished using three-dimensional planning software after attempting an ideal facial profile using two-dimensional profile planning software.
The issue with using preoperative and post-orthodontic data is that the bracket system is an important factor on lip position. This study tried to minimize the importance of the orthodontic appliance with the removal before the postoperative cephalogram.
Another important factor is the relapse which is most important for lower jaw advancement surgery. This relapse is not constant and differs between surgical techniques and fixation methods. The skeletal relapse can be compensated during the postsurgical orthodontic treatment. 18 Orthodontic compensation performed in the upper dentition can influence the position of the upper lip. Relapse is therefore another factor that must be taken into account during surgical planning.
Conclusions
The changes in landmarks A, B, Pg, Ili, and Iui can aid preoperative planning of positioning osteotomies by providing a good approximation of horizontal lip movements. A linear equation with a narrow spread was found for soft tissue landmarks, indicating its accurate predictability. In this study, no accurate way was found to predict the vertical displacement of the upper and lower lips. Additional inclusions will lead to a better understanding of soft tissue behavior in and between the surgical subgroups and direction of displacement.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.