Abstract
Background
When a child is diagnosed with a life-threatening disease such as cancer, the best care comprises more than just the best possible medical treatment. Pediatric oncology nurses play an important role in supporting and guiding families, but the assiduous work of nurses is often hampered by nursing shortages and high workloads (Aiken et al., 2023). Nurses working with inadequate staffing and resources struggle to fulfill their vision of safe and high-quality care (Smeds Alenius et al., 2020). Feeling powerless to provide high-quality care has been recognized as one of the major occupational stressors among experienced pediatric nurses (De Almeida Vicente et al., 2016).
High-quality care has been defined as effective, safe, and patient-centered care (Stavropoulou et al., 2022; Wei et al., 2019; World Health Organization, 2022). Nurses describe it as holistic care that meets the comprehensive needs of their patients (Stavropoulou et al., 2022), and for the parents of sick children, it can also mean trusting relationships, positive patient experiences, and other elements that reflect their lifeworld (Wei et al., 2019). Missed care is an example of care quality deficiencies, and it often is related to discharge planning, emotional support, and education, but includes even fundamental, basic care, contributing to prolonged hospital stays and impaired patient safety (Chaboyer et al., 2021).
Nurses have associated missed care with frustration and moral distress (Molinaro et al., 2023). Moral distress occurs when nurses cannot take ethically right actions to meet their patients’ needs. It can evolve from external root causes, such as inadequate staffing, or from internal root causes, such as powerlessness (Hamric, 2012). Even clinical situations can prompt moral distress, for example, when a nurse feels pressured to provide futile care. Recurrent experiences of moral distress can make nurses less sensitive to the moral aspects of care, and lead to withdrawal from patients and even to resigning (Hamric, 2012). The subsequent nurse turnover drains the collective competence (Smeds Alenius et al., 2020) and jeopardizes the quality of care, because the delivery of quality care requires high levels of knowledge and practical skills (Stavropoulou et al., 2022), and many competencies on advanced level can only be achieved through professional experience (Lee et al., 2017).
Children with cancer undergo treatments that can cause severe complications, leading to long periods of hospitalization. While highly rewarding, caring for severely ill children comes with its own set of challenges. A deeper understanding of the demands and challenges that pediatric oncology nurses deal with can be helpful in developing strategies to support them to practice nursing to the best of their abilities. This, in turn, can attract them to remain in pediatric oncology nursing, and ultimately, improve the quality of care. Thus, the purpose of this study was to explore nurses’ experiences, their main concern, and how they deal with it, when unable to provide the best possible care to children with cancer.
Method
Design
To gain an understanding of pediatric oncology nurses’ experiences of not being able to provide the nursing care they believed should be provided, a classic grounded theory approach (Glaser & Strauss, 1967) was employed in this qualitative study. This approach was suitable for this study, because it aims to explore the main concern of participants and how they deal with it (Glaser, 1978). Furthermore, it aims for the conceptualization and generation of a theory or an integrated set of concepts.
Sampling and Data Collection
Initially, a purposive sampling was performed and nurses working in pediatric oncology care were identified as key informants. Registered nurses at two pediatric oncology centers were informed about the study by group emails that were sent to their work email addresses. Those nurses who consented to participate, scheduled an onsite interview, and were individually interviewed, face-to-face by the first author in a meeting room at the hospital. An interview guide with open-ended questions was developed to encourage nurses to describe their experiences. The initial question, “Please tell me about a situation when you felt that you were not able to provide care that you thought you should have provided,” was followed by probing questions such as “Please tell me what happened.”
Consistent with a classic grounded theory approach (Glaser & Strauss, 1967), a theoretical sampling was applied to include pediatric nurses who work in units other than pediatric oncology in order to explore and compare their experiences. One of the units provided care for children with cancer after stem cell transplantation and the other unit after brain surgeries, but they were also specialized in other diseases and injuries besides pediatric oncology. Nurses were invited to join focus group interviews, that were conducted to seek clarifications to the already collected data and to search for more detailed information, as suggested by Powell and Single (as cited in Stalmeijer et al., 2014). Prompting questions were used to shed more light on the experiences of settling for less and pulling together. The first author moderated focus group interviews, and the second and the last authors took turns to operate as observers and making field notes. Recruitment continued until interviews no longer contributed to new properties in the concurrent coding; data saturation was reached.
No other persons besides the participants and researchers were present during the interviews. All individual and focus group interviews were audio recorded after the participants had given their permission except for one individual interview when the batteries to the digital voice recorder had been discharged and only written notes were taken. All interviews were conducted in Swedish.
Data Analysis
Data analysis was performed iteratively and simultaneously with data collection, guided by the work of Holton (2010). All interviews were transcribed and analyzed manually by the first author. Coding was conducted in three steps—open, selective, and theoretical coding—according to the classic grounded theory (Glaser, 1978; Holton, 2010). As suggested by Holton (2010), the process began with open coding, which was performed manually line-by-line while working through the transcripts. To ensure that all codes were well grounded in data, the initial, line-by-line coding was performed in Swedish, the same language as the interviews. As the analysis proceeded, the fragments of data were summarized and named, and shifted into gerunds to emphasize actions. The identified codes were labeled in English by the first author, and subsequently reviewed by other authors, all fluent in English and Swedish. For example, expressions mirroring high workloads with many different tasks could be labeled in terms such as multitasking. This kind of conceptualization is central to classic grounded theory (Glaser, 1978; Holton, 2010).
By using the constant comparative method (Holton, 2010), data were compared within and between interviews, resulting in conceptual codes that in turn were compared to each other. The coding aimed to establish a central idea, a core category, by identifying repetitive patterns that reflect nurses’ main concern and the ways they dealt with it. It soon appeared that nurses often were pulled in different directions, which challenged their endeavors to do their best for sick children. Once the inductive analysis (Glaser & Strauss, 1967) had generated a core category, juggling compassion and competing demands, the coding proceeded selectively by focusing on its properties in order to explain the central idea. Informal analytic notes (memos) were written by the first author throughout the analysis process, detailing her contemplations and provisional analysis. According to Holton (2010), sorting and integrating memos are essential during conceptualization and improve the level of abstraction. Theoretical coding illuminated relationships between the substantive codes, that is, the codes generated directly from data (Holton, 2010), and organized the theory by weaving back the fractured data (Glaser, 1978). For example, memos about prioritizing, shifting up a gear, settling for good enough, acquiescing, and pulling together were all sorted in the same pile, theoretically coded as strategies.
Ethical Considerations
According to the Swedish Ethical Review Authority, no ethical approval was needed for this kind of inquiry, that did not include any interventions on research persons or sensitive personal data as specified in the Swedish Act (2003:460) concerning the ethical review of research involving humans. However, the agency provided an advisory opinion (2021-02255), and an external contact person was recruited in case any of the participants should express a need for psychological support. In order to minimize the risk of perceived coercion during recruitment, those pediatric oncology nurses who were colleagues with the first author were never approached in person about the study, but only received information about the study via work email. Prior to each interview, all participants were once again reminded about the voluntary nature of the study, and about their rights to withdraw at any moment. Each participant signed a written consent form. In order to protect participants’ confidentiality, the interviews were anonymized when transcribed, and thereafter, all audio files were deleted.
Rigor
Methodological triangulation (Polit & Beck, 2012) was employed during data collection by conducting both individual and focus group interviews, and triangulation of sources by recruiting participants from three different units. Analyst triangulation was used throughout the study: the first, second, and last authors were all involved in the data analysis, discussing codes and emerging categories. According to the grounded theory approach (Glaser & Strauss, 1967), the process of constant comparison ensures that categories are consistent with the data. The authors’ extensive experience in pediatric oncology care has contributed to a contextual understanding. However, in order to mitigate the risk of assumed understanding, all authors have tried to remain self-reflective by carefully examining their own thoughts throughout the entire research process. Some data extracts were reviewed and analyzed during a journal club meeting for academic nurses, each with a long experience in pediatric nursing and a good knowledge of qualitative methods as well as classic grounded theory.
Findings
Participants
Thirteen individual interviews and three focus group interviews (three to six nurses in each group) were conducted between September 2021 and May 2023. While most of the interviews lasted approximately 1 hr, the shortest one lasted only 15 min and the longest one for 90 min. On average, the participants (n = 25) had worked as registered nurses for 14 years (Mdn = 13; range = 1–34). In accordance with the gender distribution among nurses in the units, almost all participants were women. Thirteen of them worked at one of the pediatric oncology centers while 12 nurses worked in other inpatient pediatric care units.
Nurses’ main concern was to uphold children's best interests, which was more than taking a child's perspective and advocating for children's rights. It also included aspects of quality care that would benefit the child, such as patient safety, and timely medication. The core category, juggling compassion and competing demands explains how nurses handle challenging situations by prioritizing, shifting up a gear, settling for good enough, acquiescing, and pulling together (Figure 1). If one strategy turns out to be unsuccessful, nurses try another or combine them.
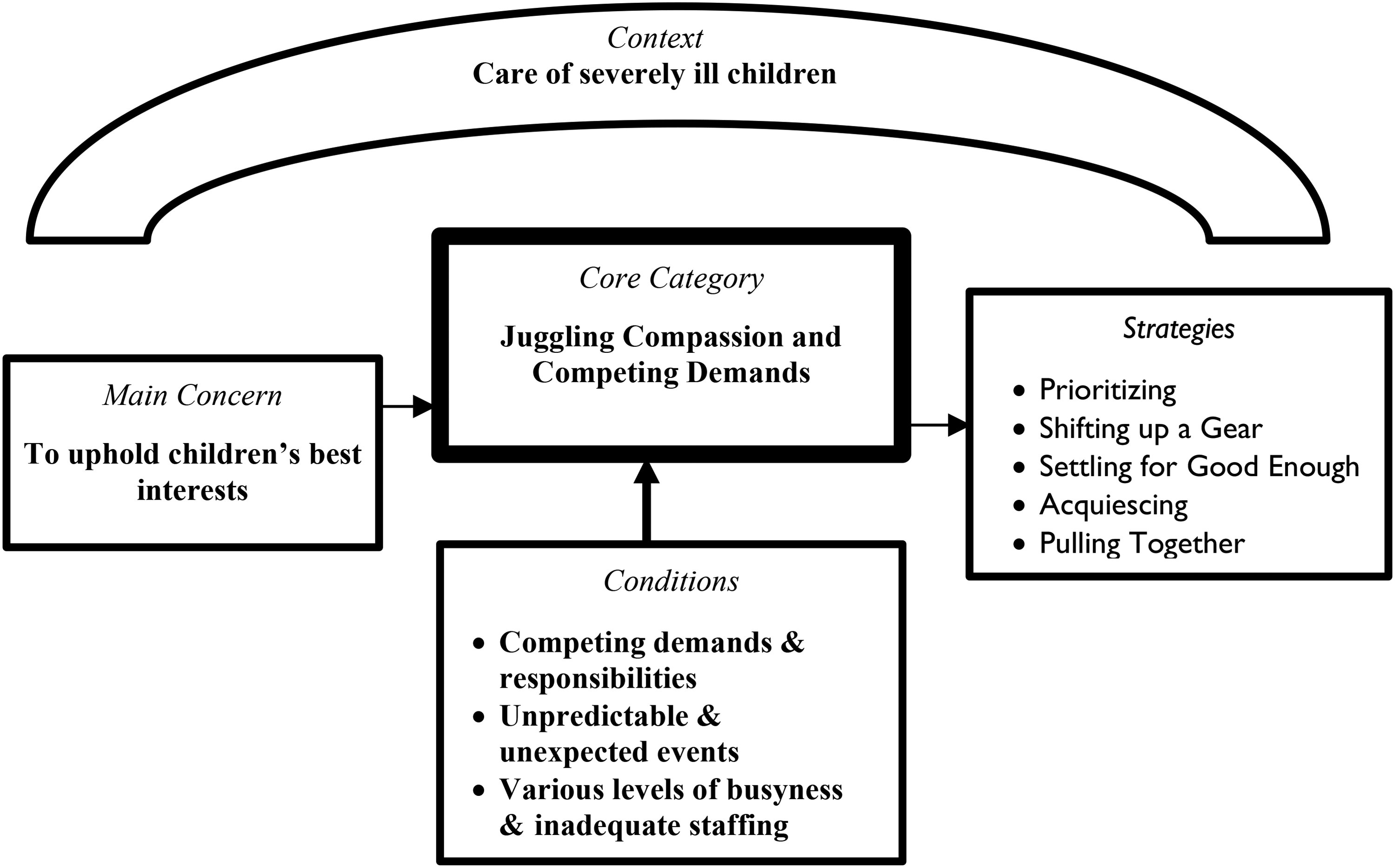
Overview of the Results in a Figure Inspired by the Six C's (Glaser, 1978).
Juggling Compassion and Competing Demands
Nurses juggled compassion and competing demands when multiple, and often simultaneous, responsibilities challenged their endeavors to provide children with the best possible care. Nurses talked compassionately about their young patients and regarded patient advocacy as one of their many responsibilities. They were keen to protect children from unnecessary suffering and to keep them safe, and they strove to practice holistic care that would meet the comprehensive care needs of sick children and their families: children's medical, physical, psychological, and cognitive needs, as well as other family members’ needs for information and emotional support. Pediatric nursing was perceived as a challenging specialty that required plenty of creativity: “I need to find a way to get around and to reach the same goal” (Participant 20), but overall, caring for children was a great joy, and the rewards of watching children returning to health motivated nurses to continue with nursing. In the reverse circumstances, when a cure was no longer possible, helping a child to achieve a good death was also an accomplishment that highly mattered.
Despite the nurses’ earnest endeavors to provide the best possible care, things did not always turn out as planned. Incompatible concerns between different actors involved in children's care caused disagreements about children's best interests. Work shifts were unpredictable and unexpected events occurred almost on a daily basis. Most often nurses cared for several patients, and there was a range of tasks that needed to be done, sometimes at the same time point. Some of the tasks could not wait or be rescheduled, for example, planned surgeries, or a worsening of a child’s clinical condition that required a nurse’s attendance. When nurses were juggling compassion and competing demands, they used various strategies, as described in the following.
Prioritizing
This is about giving one's attention to one task or an event with the highest priority. A precondition for successful prioritizing is to know what is most important at the moment—the most urgent is not always what is most important. When juggling compassion and competing demands, prioritizing involved continuous assessment of the acuity and the importance of patients’ needs. Usually, nurses strove to give timely care, and prioritizing was task-oriented: administering medications, collecting blood samples, and executing other similar tasks on time. Consequently, nurses had to omit nonurgent tasks such as emotional support: “you see a sad parent, and you would like to sit down and talk … but you can’t, because the chemo (infusion pump) is already beeping and none of your colleagues can help” (Participant 1).
When caring for several patients, nurses juggled a wide range of care activities, and not even the most experienced nurse could be in two places at once. Responding to a deterioration of a patient's condition could require the nurse's full attention, and in the meanwhile “the other patients got nothing” (Participant 22). While deciding what to prioritize was obvious in emergency situations, it was more difficult in situations when everything seemed equally important. Nurses were aware that wrong choices could jeopardize patient safety, and so they tried to delegate simultaneous tasks to others: “if there is someone to ask help from, you do that, otherwise you just work fast, and faster, and you prioritize, and you hope that you prioritize the right thing” (Participant 17). Even when concerned about the consequences of prioritizing, compassion urged nurses to prioritize end-of-life care when caring for dying children. This arose feelings of being torn between two patients: So while I cared for this dying child, the other child developed a high fever and I just didn’t have time to go to (the other child) … I know this (neutropenic fever) can be potentially very dangerous, but on the other hand, I have this palliative child here. (Participant 8)
When mere prioritizing was not enough, and with no help at hand, the nurse shifted up a gear.
Shifting Up a Gear
This is about putting in extra effort. Most often it equals increasing the work pace in order to get the job done. It can involve multitasking, or, on the contrary, require reducing distractions and focusing. The downside is that it can get exhausting in the long run. When juggling compassion and competing demands, nurses often put others’ needs ahead of their own and skip meal breaks, work faster, and multitask. Many nurses regarded shifting up a gear as crucial to nursing practice, as “work shifts are about administering as many medications as possible in the shortest possible time” (Participant 4). Nurses tried not to waste time, and sometimes they even avoided entering into discussions with families by “hoping that they (parents) won’t ask anything because I don’t have time to stay and answer” (Participant 10), even though neglecting families’ needs of information caused guilt and frustration. Shifting up a gear could also lead to positive outcomes: in unforeseen situations, nurses took the reins and gained control over the situation.
When unable to do their best despite the extra effort, nurses switched to settling for good enough.
Settling for Good Enough
This is about giving up the high ideals and accepting the mediocre. It occurs, for example, when one is overwhelmed by competing demands, or when one has no other options to act upon. Individuals respond differently to settling for good enough. Sometimes, but far from always, it results in frustration and dissatisfaction. When juggling compassion and competing demands, settling for good enough enabled nurses to modify their goals of care: if unable to provide the best possible care, nurses did their utmost to provide care that was at least good enough. Plenty of time was spent on “putting out small fires” (Participant 12), leaving little room for other nursing interventions. Several nurses felt that they did not even have a chance to do a decent job: You do what’s necessary, you access the port, you collect the blood samples, you administer the medications, but it’s about what you don’t do, you don’t sit at the bedside and check how the family and the patient are really doing, because you don’t have time for that and so you leave … and then when you’re writing notes you wonder, how was the patient doing, really, I don’t know, because I didn’t have time to check … you haven’t done anything wrong, so it’s not a bad job, but it’s not a good one either. (Participant 2)
Settling for good enough was not always frustrating, and a few nurses rather regarded it as inevitable and nothing to get too stressed about: “I think it was more of a bad luck for them to become ill that week” (Participant 7). Some relationships required settling for good enough, as nurses did not always succeed in building trustful relations with families. It troubled nurses especially when in conflict with the parents or when it was obvious that the family needed extra support: It was a kind of three-way conversation, so your child has a brain tumor, this is chemotherapy, and she (mother) is sitting at home (having COVID-19 and not allowed to visit the hospital), the interpreter is on the phone, and the father is just heartbroken and the mother hears over the phone how sad the father is and the boy, he is just terrified of us … whenever we opened the door he would just scream … we did not get any contact at all (with the boy), it felt awful. (Participant 5)
Poor communication and lack of skills could lead to situations when nurses had to settle for good enough. Due to a limited number of hospital beds, children with other health issues than the unit's specialty were quite often admitted to the units. Because their physicians came around only a few minutes a day, nurses found it difficult to convey information and to discuss patient care matters with them. Nurses worried about their lack of knowledge when caring for these patients: “this child is going to be sick the rest of its life, so it must be a good start … but to end up in a unit where they don’t have the competence … it's like … you’re guessing … you have no clue” (Participant 21). Nurses tried to seek information from colleagues, guidelines, and internet, but not possessing the expertise added stress and impaired the quality of care.
When settling for good enough involved different opinions about children's best interests, the strategy shifted to acquiescing.
Acquiescing
Acquiescing is preceded by different viewpoints. It takes place when one reluctantly adjusts to others’ decisions that one does not agree with, or when one is unable to prevent actions that transgress one's values. In the context of pediatric oncology nursing, acquiescing was often preceded by concerns for children's best interests. Nurses did not always agree with physicians and/or parents about the best actions. Differing opinions about children’s best interests caused feelings of powerlessness, when nurses felt unable to influence the decisions. This happened, for example, when nurses wanted an unstable child to be moved to an intensive care unit rather than keeping it in a unit without continuous monitoring, or when they wished to transfer a dying child from a busy unit to hospice care. Another typical situation was when nurses perceived prolonged treatment as futile, all the while they were the ones to carry it out. Many nurses called for a better dialog with physicians to discuss difficult patient care matters, because understanding the reasons behind medical decisions expanded their perspectives and often prevented acquiescing. Good communication and trustful relationships also made it easier to advocate for one's patients, and reduced the need of acquiescing. In general, nurses with longer work experience were more confident in questioning the orders they disagreed with, such as repeated testing that required capillary punctures, or inserting a nasogastric tube when the child had a good appetite. Acquiescing caused moral distress if it led to unnecessary suffering to a child, or if the nurse questioned the necessity of a procedure: They (physicians) are not the ones who perform these procedures … and I felt like, this is against all my principles, and it's a horrible feeling to have … I know this (procedure) is not necessary, I know it is all wrong … but you still do it. (Participant 9)
Sometimes distressed parents tended to complicate things, for example, by passing their own anxiety to their children during procedures. In general, nurses acquiesced, being too sensitive to show disapproval: “well, we cannot say (to a parent) that it (procedure) is easier when your partner is here (instead of you)” (Participant 8). Many nurses considered that parents' viewpoints often overshadowed children's voices: I can see that the boy is about to say something else, that he wants something else, but he does not get the chance and I don’t have time to tell him that let’s try again, let’s sit down and talk about how it really is with your nausea. (Participant 4)
Regardless of the work experience and the confidence level, nurses acquiesced and went along with parents’ requests of not telling the truth about a severe diagnosis or a poor prognosis. “The elephant in the room” (Participant 12) hindered nurses from finding out children's preferences and made it difficult to discuss palliative care options. Nurses questioned the limited truth-telling because they perceived it violated children's rights to know, but on the other hand, they understood that it often was rooted in parents’ needs to protect their children. However eager to stand up for the right values, nurses did not want to risk consequences that might negatively affect the child or its family. Some nurses, however, discussed the benefits of truth-telling with the parents. Acquiescing was easier when nurses were pulling together.
Pulling Together
This is about helping and supporting one another. It is about standing up for one another and working together as a team to achieve a common goal. Practical help can be needed when one is temporarily overstretched, for example, when prioritizing and unable to perform other simultaneous tasks. Support is also needed when one is uncertain about the right action, or wants to reflect on distressing situations. When juggling compassion and competing demands, nurses turned to their colleagues for practical assistance, guidance, and emotional support. It was not always necessary to actively seek support, because nurses showed solidarity and often helped one another even without being asked, and sometimes even stayed after their work shifts to assist other nurses. Nurses reflected on distressing situations they had gone through, often together with a colleague who had been involved in the same situation: “we talked about it a lot, I was quite upset about that (the way things had turned out), that nothing went the way we had hoped for” (Participant 3). Although nurses found other nurses as their best support, they truly appreciated collaboration with other healthcare professionals: “we are a great team and we stand up for one another, we enjoy working together, we do the best we can” (Participant 18).
Pulling together was not always feasible, for example, when everyone was busy: “healthcare nowadays is so slimmed down, there's never a pair of extra hands” (Participant 15). Not getting support and failing to turn around a distressing situation that jeopardized a child's best interests was highly distressing: It was so frustrating and I was so sad because the boy had told me he was in pain, and I had promised I would give him analgesics, but the mother wouldn’t let me do that, so he suffered … I got no support, I wanted the physician to go in and talk to the parents, but the physician would not do it. (Participant 6)
As described above, nurses in this study used a range of strategies when juggling compassion and competing demands. These strategies will be further discussed in the following.
Discussion
This classic grounded theory study explored pediatric nurses’ experiences of not being able to provide the best care for their patients. The findings showed that nurses’ main concern was to uphold children's best interests: taking a child's perspective and to provide holistic, safe care. When caring for multiple patients and facing constraints, nurses often found themselves juggling compassion and competing demands. To manage juggling, they used such strategies as prioritizing, shifting up a gear, settling for less, acquiescing, and pulling together. Despite the efforts, juggling often was intertwined with missed care, reduced care quality, and compromises on moral values.
The present findings align with Hamric's (2012) description of root causes of moral distress, and with prior research (Ventovaara et al., 2023) that have shown that external root causes, such as inadequate staffing, often are the most prominent root causes of moral distress. Many struggles described in the present study reflected external constraints of busyness and inadequate staffing. Nurses managed these situations by prioritizing, shifting up a gear, and by settling for good enough, while pulling together was not always an option during busy work shifts. Nurses also described struggles that stemmed from internal factors, such as lack of knowledge. They tried to manage internal constraints by settling for good enough and by pulling together, for example, when caring for children with illnesses that one was unfamiliar with. Acquiescing was used to cope with morally distressing situations that emerged from clinical situations, such as limited truth-telling and unnecessary procedures that caused suffering to a child.
Prioritizing nursing tasks is inevitable when caring for several patients. However, balancing patients’ needs against each other poses an ethical dilemma of how to prioritize when everything seems important. The ethical aspects of prioritizing have been explored by Suhonen et al. (2018) in a scoping review that linked prioritizing with moral distress and decreased job satisfaction among nurses. In the present study, compassion guided nurses to prioritize end-of-life care, and they strove to do their utmost to maintain high standards while caring for the dying children and their families. Studies by Pearson (2013) and Taylor and Aldridge (2017) suggest that nurses are anxious to do their very best because there may never be another chance to “get it right.” Unfortunately, by prioritizing dying patients and their families, nurses sometimes fail to give proper attention to their other patients’ needs, also described by Vinckx et al. (2018). Time is a prerequisite for end-of-life care and enables nurses to care for dying children in a holistic manner without risking other patients’ safety or their own well-being. Furingsten et al. (2015) suggest that having time to focus on dying children's needs could also reduce the emotional labor of nurses, that often accompanies end-of-life care.
It is already well established that lack of time is a prominent barrier to providing good care (Vinckx et al., 2018). Shifting up a gear was indeed helpful in getting things done, but it was experienced as exhausting in the long run. This aligns with Govasli and Solvoll (2020), who imply that while busyness can improve work efficiency, it becomes harmful when persistent or when important tasks remain undone. Nurses’ experiences of an overwhelming range of responsibilities have also been described by De Almeida Vicente et al. (2016). Nurses in this present study were quite used to juggling multiple demands to a degree that they regarded busyness rather as an integral part of nursing. Many nurses seemed to be less troubled by the busyness per se, and more concerned about its consequences, compromised and missed care, and failing to uphold children's best interests. This signals value conflicts between nurses’ professional environment and the unfulfilled professional expectations described by Molinari and Vander Linden (2019).
Sometimes when juggling compassion and competing demands, nurses had no other choice but to settle for good enough care and/or to acquiesce in others’ decisions. Having no power to influence circumstances and others’ decisions can be morally distressing (Hamric, 2012). Disagreements on children's best interests should initiate ethical discussions with the involved stakeholders, including bed-side nurses. While it is important to bear in mind that children's and their parents’ best interests often are intertwined, healthcare professionals should make decisions that first and foremost benefit the child (Bester, 2019).
The strategy of pulling together accords with a number of other studies that have identified collegial support, good interprofessional relations, and collaboration as successful coping strategies (Aburn et al., 2021; Ahlstedt et al., 2019; Taylor & Aldridge, 2017). These studies underline the importance of creating opportunities for discussions, social talks, and informal debriefings during work hours. Ahlstedt et al. (2019) suggest that trusting relationships and close collaboration between nurses and physicians influence nurses’ work motivation, and according to Aburn et al. (2021), guidance and support from leaders are especially important for the younger and newer staff members. This aligns with the present results implying that unexperienced nurses were less likely to question care decisions they disagreed with.
Even when nurses met the physical needs of sick children, they were distressed about all the other needs that contribute to children's well-being but now remained unmet, such as comforting a sad parent. It is important to support nurses to practice nursing to the best of their abilities, as over time, repetitive compromises on care quality and on one's own values can cause feelings of powerlessness and distress (Bragg & Bonner, 2014). Resilient staffing levels and ensuring practical support during busy shifts could prevent many demanding situations that nurses struggle with. Novice nurses may also need guidance in making conscious choices and explicit prioritizations, based on reflection and nursing ethics. The present findings confirmed the importance of collegiality, interdisciplinary communication, and teamwork; they are not only needed in busy situations with high workloads, but also when children's best interests are at stake.
Strengths and Limitations
Focus group interviews greatly benefited the present study, as they led to rich discussions between participants, providing clarifications and new insights into the core category. However, the group composition and interaction between participants are important aspects to consider when analyzing focus group interviews (Stalmeijer et al., 2014). Two of the groups, that were homogeneous (in terms of nurses’ professional position), were characterized by open communication, which encouraged nurses to share their experiences of disturbing situations. In the meanwhile, some power imbalances could be sensed in one of the groups that was more heterogeneous, which seemed to inhibit some participants from talking about their experiences in detail.
Recommendations for Further Research
While the present study explored experiences when nurses had not been able to provide the best care, there was an excess of allusions to excellent care, collaborative relationships with coworkers, and the joys and rewards of pediatric nursing. A critical review of those experiences could provide important insight into the positive side of nursing, which could be ever so useful in the progress toward the best nursing care of sick children.
Conclusions
Time obstacles and disagreements on children's best interests can hinder pediatric oncology nurses from working to the best of their abilities, contributing to compromises on moral values, reduced care quality and missed care. Juggling compassion and competing demands can be exhausting and morally distressing, but ensuring adequate staffing, collegial support and good interprofessional communication may help nurses to better endure the challenges of pediatric oncology nursing.
Footnotes
Acknowledgments
This study could not have been done without the nurses who willingly shared their experiences. We thank them all for their support.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
According to the Swedish Ethical Review Authority, no ethical approval was needed for this kind of inquiry, that did not include any interventions on research persons or sensitive personal data as specified in the Swedish Act (2003:460) concerning the ethical review of research involving humans.
Informed Consent
Each participant signed a written consent form.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request. The data are not publicly available due to the privacy of research participants.
Funding
The authors disclose the following financial support: Doctoral School in Health Care Sciences at Karolinska Institutet (Grant HK2018), Swedish Childhood Cancer Fund (Grants PR2017-0123; TJ2017-0011), and Mary Béve’s Foundation for Childhood Cancer Research (Grant A7241A).
