Abstract
Introduction: Midlife women, aged 40–65 years, are an under-researched population with poor and inequitable access to Women’s Health and Wellbeing Services (WHWS). This study, which was supported by a Patient and Public Involvement group, explored the enablers and barriers to WHWS, with a focus on sexual health and wellbeing services, cervical and breast screening, menopause care, contraception, and incontinence services. Methods: Semi-structured focus groups and interviews were conducted with sixty self-identifying women and gender non-binary participants aged 40–65 years living in the South-East of England. Recruitment was focused in underserved geographic areas and in underserved groups. Framework Analysis, also using the Socioecological Model, through an intersectionality lens, was used to analyse the enablers and barriers to WHWS. A feminist pragmatist approach was employed to interlink the findings into suggestions to improve access. The study was reported according to the Consolidated Criteria for Reporting Qualitative Research (COREQ). Results: Three main themes emerged: the lack of prioritisation of midlife women; the widespread deficits in knowledge of the needs of midlife women; and the impact of stigma on access to care, particularly sexual health and genitourinary syndrome of menopause services. The intersectional disadvantage of belonging to underserved groups for example due to ethnicity, income, and disability, overlapped across the themes. Participants advocated for integrated, holistic, community-based, women-only services. Conclusion: Further research, education, and policy investment is required to address the complex, and often highly sensitive nature of many health and wellbeing issues that face midlife women. These challenges are compounded by belonging to an underserved group.
Introduction
There has been a halt, and in some cases, a reversal, of the progress in gender equality in many countries. This has largely been attributed to concurrent geopolitical emergencies and the worldwide economic and climate crises.1,2 Gender inequality remains a significant barrier to achieving equitable public health outcomes globally. 3 There are international calls for investment in feminist healthcare leadership, support for feminist civil society organisations, and improved technical (including data) capacity to advance sex and gender integration in healthcare policies and programmes. 4 There has been a welcome and necessary increase in public and policy interest in improving health care for women in England. However, granular data about how to address poor, and widening inequity5,6 in access to Women’s Health and Wellbeing Services (WHWS) in England is lacking.
Midlife, generally understood as beginning at 40 years and extending to 65 years, a range that includes the late reproductive to late menopausal stages, 7 is a unique time in women’s lives, when hormonal and physical changes 8 are often accompanied by social, psychological, and relationship evolution. This stage can be an opportunity to empower women to improve their health and wellbeing trajectory. Midlife women in England do not feel that they have good access to WHWS, 9 and those who live in under-resourced coastal communities are a particularly under-researched population with some of the worst health outcomes in England. 10 WHWS have been classified as those that encompass care for conditions that are unique to women, and conditions in which men and women experience differences in risk, presentation, and response to treatment. 11 The first Women’s Health Strategy for England 12 highlighted particular elements of WHWS relevant to midlife women which require improvement: sexual health services (the prevention and management of sexually transmitted infections (STIs), sexual violence prevention, sexual function, desire, and arousal, and fertility management 13 ); sexual wellbeing services (sexual safety and security, sexual respect, sexual self-esteem, resilience in relation to sexual experience, forgiveness of past sexual experiences, comfort with sexuality, and self-determination in one’s sexual life), 13 contraception; and gynaecology services including incontinence services and menopause care.
Existing quantitative data highlights the challenges that women face in accessing WHWS.6,14 There are a wide range of barriers which affect access to WHWS for midlife women in high income countries. These range from: poor knowledge8,14; psychological factors such as low self-esteem 15 ; competing time and energy priorities 16 ; and cultural norms and stigma, 17 to healthcare system barriers, 18 including poor knowledge, skills, and attitude of Health Care Professionals (HCPs). 19 Many of these barriers disproportionately affect women from underserved areas and who belong to underserved groups. 14 The intersectional disadvantages of gender, ethnicity, sexuality, income and disability often exert compounded influences on access to WHWS and health outcomes. 6 Under-resourced populations have higher rates of new STIs, including Human Immunodeficiency Virus (HIV). 20 Human Papilloma Virus (HPV) vaccination and testing rates are lowest in the most underserved areas of the United Kingdom (UK). 21 Gender based violence is more prevalent in underserved areas. 22 After adjusting for risk factors, the prescribing rate for Hormone Replacement Therapy (HRT) in underserved localities is 18% lower than in affluent areas. 23
In the UK, minority ethnic groups are overrepresented in the 20% most underserved areas. 24 Inequalities related to ethnicity are complex, reflected in different patterns of inequality within and across minority ethnic groups. Women from minority ethnic groups are more likely than women of White ethnicity to have a late diagnosis of the menopause. 25 Black, Asian, and minority ethnic heterosexual women are disproportionately affected by HIV in the UK. 26 Indeed, 18% of new HIV diagnoses in 2022 were in women of Black African heritage, who make up only 2.2% of the UK population. 27 Inequalities in relation to healthcare experiences and health outcomes persist among patients who identify as lesbian, gay, and bisexual. 28 Societal and organisational heteronormativity, the stress of identifying as belonging to a minority group, and discrimination and stigma, contribute to poor access to health services.29,30 Despite the increasing awareness and visibility of people who identify as transgender and gender non-binary (TGNB), the strictly binary conceptualisation of health and wellbeing services, particularly WHWS, results in specific barriers to health and wellbeing services.31,32 A small number of studies have proposed methods to enable access to WHWS for some groups of poorly served midlife women, for example tailored education for women who identify as neuro-diverse, 33 and interdisciplinary services designed to serve women with different cultural identities. 34
The aims of this study were to determine the enablers and barriers to WHWS for midlife women and to outline feasible suggestions to improve access within the context of East Sussex, a region in South-East England. Sussex can be described as a ‘microcosm’ of England, as it contains some of the most and least affluent areas in the country. Stark disparities in access to health care services across the region continue to widen, with 75% of deaths and disability influenced by health inequalities. 35 There are significant regional data gaps about access to WHWS for people living in underserved areas and who belong to underserved groups, including those who identify as lesbian, gay, bisexual, transgender, queer, intersex, asexual, and minority ethnic groups. 30 We aimed to over-represent recruitment from underserved areas and groups. In this study, we have used the term ‘woman’ to describe a person assigned a female sex at birth or a person who defines herself as a woman, to foster inclusivity in our research. 36
As health inequalities continue to widen in the United Kingdom (UK), 5 an intersectionality lens 37 was chosen to explore the multiple axes which may contribute to the contexts which affect access to WHWS. Intersectionality proposes that identities which are markers of difference, such as gender, race, and sexuality, intersect and reflect large social structures of oppression and privilege, such as sexism, racism, and heteronormativity. 38 The intersectionality lens provided a tool to understand how access to WHWS for midlife women varied depending on their identity and unequal power dynamics.39,40 Conceptualising these differences between midlife women enabled an understanding of the different structural disadvantages that were experienced by underserved groups of midlife women. A feminist pragmatist stance, 41 a method utilised for patient-orientated research to improve access to services,42,43 was employed to design the study, and to outline suggestions to improve access to WHWS. Feminist pragmatism focuses on articulating ‘real life’ problems from the perspective of the lived experience of women. 41 Core components of this stance are the rejection of the hierarchical knowledge of ‘experts and the elite’, and a focus on problem solving for the ‘common good’. 44 The experience of the researcher helps to form the knowledge. 45 Our aim in utilising this stance was to project the experiential knowledge of midlife women from the most underserved communities, in combination with the experience of the PPI group and the steering committee, to provide feasible suggestions to improve access to WHWS. The Socio-ecological model (SEM) 46 which conceptualizes health as affected by the interaction between the individual, the community, and the physical, social, and political environments, has been successfully employed in women’s healthcare research to highlight the interconnectedness of systemic processes with individual experiences.47,48 It was therefore chosen to categorise the data into the intrapersonal, interpersonal, organisational, and public policy, enablers, and barriers to WHWS.
Method
Study Design
An exploratory qualitative study design was chosen to capture the depth and nuances of the experiences of this underserved population. Qualitative studies which employ focus groups, interviews or a mixture of both methods are considered appropriate for eliciting views on sensitive topics such as WHWS and sexual health and wellbeing. 49 A combination of interviews and focus groups was utilised in recognition of the different impact of group dynamics, the number of participants, and the role of the researcher, 50 in deriving sensitive information from members of an under-represented population. Focus groups allowed participants to stimulate ideas that might not have been recognized or remembered, and individual interviews enabled more in-depth and private data collection from each participant. The use of qualitative pluralism therefore resulted in a wider variation of responses, improving the scope and depth of data. 51
The Socio-ecological model (SEM) 46 was utilised to categorise the data. The SEM considers complex connections across the four dimensions of existence: the material dimension, the biophysiological processes, the cultural dimension, and the social dimension. 52 It therefore emphasizes opportunities for comprehensive, multilevel interventions, which are interactive and reinforcing, and are more likely to be sustained for the benefit of individuals embedded in larger social systems. 53 A feminist pragmatist model 54 was used to design and analyse the study to enable the projection of the suggestions of ‘situated knowers’. 41 An intersectionality lens 38 was employed to review the data, enabling an appreciation of the importance of the social determinants of health, a core tenet of intersectionality, within discourse about women and health and wellbeing inequity. 55
A Patient and Public Involvement (PPI) group, which consisted of five midlife women from a range of social identities in the South-East of England, was created to ensure that intersectionality was incorporated throughout all phases of the study. They were asked to support the study design (development of the objectives, methodology, topic guide), and the dissemination of the findings. The study design included inviting members of the PPI group to co-facilitate the focus groups and support data analysis. One member of the PPI group (JH) elected to receive basic community researcher training and co-facilitated one focus group and supported data analysis (transcription verification, theme identification, coding, final review). This member of the PPI group (JH) joined the steering committee, which also consisted of five researchers (KS, CL, CI, SB, DH). The steering committee contributed to the study design and data analysis. The study was reported in line with the Consolidated criteria for Reporting Qualitative research checklist (COREQ) 56 (Supplemental file 1).
Setting and Participants
This study was conducted in East Sussex, a region in the Southeast of the UK with significant disparities in health care access and outcomes. WHWS are predominantly commissioned by local authorities, and provided by primary care and sexual health services, who can refer patients to secondary care services. 57 Women can also access private and charitable services. The inclusion criteria were people who self-identified as women (including cis-gendered women, women with a trans identity, non-binary people) and trans-masculine gendered people, aged 40–65 years who lived in East Sussex and could speak English.
Sampling
Convenience sampling 58 was employed due to economic and time limitations. 59 The aim of a sample size of 54–78 participants was based on the concept that recruitment would continue to reach both data saturation 60 and information power. 61
Procedure and Recruitment
Participants were recruited between March 2023 and June 2023. Posters and online information (via websites and email distribution lists) were displayed in the most under-resourced areas and to underserved groups. Providers in community health and wellbeing settings, focusing on those serving under-resourced areas and underserved groups, also provided information (verbal, pamphlets) to potential participants. Under-resourced areas were defined as geographic areas with English Indices of Multiple Deprivation in deciles one and two 62 in East Sussex. Underserved groups were identified by the Patient and Participant Involvement (PPI) group and included: groups for minoritised ethnic groups (excluding white minorities); groups for women living with HIV; groups for women living with disabilities; groups for people who identify as having transgender and gender non-binary identities (TGNB).
Participants were given the choice between interviews and focus groups. Participants who chose an interview were asked to choose between a face-to-face or virtual (via Microsoft Teams) interview. Participants who chose to participate in focus groups were asked to self-identify which group they would prefer (groups for people who identified as: TGNB; minoritised ethnic groups (excluding white minorities); living with a disability; mixed groups of midlife participants). Participants who chose a focus group were also asked whether they would prefer a face-to-face or virtual (via Microsoft Teams) focus group. The decision of whether the focus group was face-to-face or virtual (via Microsoft Teams) was determined by the preference of most participants and subsequently explained to them by email or telephone. There were seven focus groups, with a total of 33 participants. One group was for people who identified as TGNB (three participants), one group was for people who identified as belonging to minoritised ethnic groups (excluding white minorities) (three participants), one group was for people who identified as living with a disability (11 participants), four groups were mixed groups of participants. One of these groups had 10 participants, the other three were very small (two participants each). Focus groups lasted 65 to 90 minutes. There were 27 individual interviews. Interviews lasted between 50 and 90 minutes.
Participants provided written (or audio-recorded verbal) informed consent to KS, the study investigator prior to enrolment in the study. A sociodemographic form was completed prior to the focus group or interview. A topic guide, based on the findings of a systematic review, 14 and co-produced with the PPI group, was used. Focus groups and in-depth interviews were conducted by KS. A trained member of the PPI team (JH) co-facilitated one focus group (mixed group of midlife participants). Focus groups and in-depth-interviews were digitally audio-recorded. Participants received a £25 high street voucher to compensate for their time and travel or Internet costs.
Research Team and Reflexivity
KS works as a sexual health/ HIV physician and a PhD researcher. She conducted the interviews and facilitated the focus groups. One of the focus groups was co-facilitated by JH, a member of the PPI group. Both KS and JH identify as cis feminine. Reflexivity 63 was maintained by ongoing documentation in field notes, and regular discussions with the PPI group and the steering committee (KS, CL, CI, SB, DH).
Data Analyses
We used the Framework Analysis Approach 64 to analyse the data. The Framework Analysis Model is a matrix-based approach which consists of five stages: familiarisation, identifying themes, indexing, charting and summarising, interpretation and mapping. 64 The first author (KS) transcribed and analysed the interviews and focus groups verbatim, with the assistance of Microsoft Teams transcription. This enabled sampling until theoretical saturation for breadth of data and information power for depth of data. Three authors (KS, CL, CI), who employed Microsoft Excel to manage the data, independently triple hand-coded four sets (10%: one focus group and three interviews) of data. Consensus discussions, in which researcher reflexivity and active personal engagement enabled the consideration of disagreements for joint decisions to be reached, were employed to ensure intercoder reliability. 65 Emerging themes and subthemes were identified, guided by the SEM, using an intersectionality perspective. The feminist pragmatist lens 41 was employed to extract feasible suggestions from the data which may not previously have infiltrated policies and practices. 29 The three authors (KS, CL, CI) agreed upon two initial coding frameworks, one for the focus group and one for the interviews. As the two initial coding frameworks were almost identical, the three authors and the steering committee elected to combine these into one framework. The first author (KS) coded the remaining sets of data and created the final coding framework (Appendix 1), which was reviewed by KS and JH and discussed with the steering committee. The final analysis, in the form of enablers and barriers and suggestions for improvement, was then written by the first author (KS), reviewed by two members of the PPI group, and reviewed by the steering committee.
Data Validity
Validity was assessed in several ways. KS, JH, and DH independently cross-checked four transcripts for consensual validation. 66 The focus groups were initially analysed separately from the interviews, after which the results were compared for the purpose of structural corroboration. 67 The steering committee (KS, CL, CI, SB, DH) supported the comparison of the themes and subthemes and the initial and final coding frameworks and agreed on the final analysis. The final draft analysis was reviewed by two volunteer members of the PPI group to enhance interpretative validity. Peer debriefing, which entailed the data and research process being reviewed by a researcher (CL) with expertise in both the subject and qualitative research also occurred.
Ethics
Study protocols were approved by the PPI group, the University Hospitals Sussex NHS Foundation Trust and the HRA and Health and Care Research Wales (HCRW) Committee. (Ref no: 24/EE/0032)
Results
Description of Sample
Socio-Demographic Characteristics of 60 Participants.
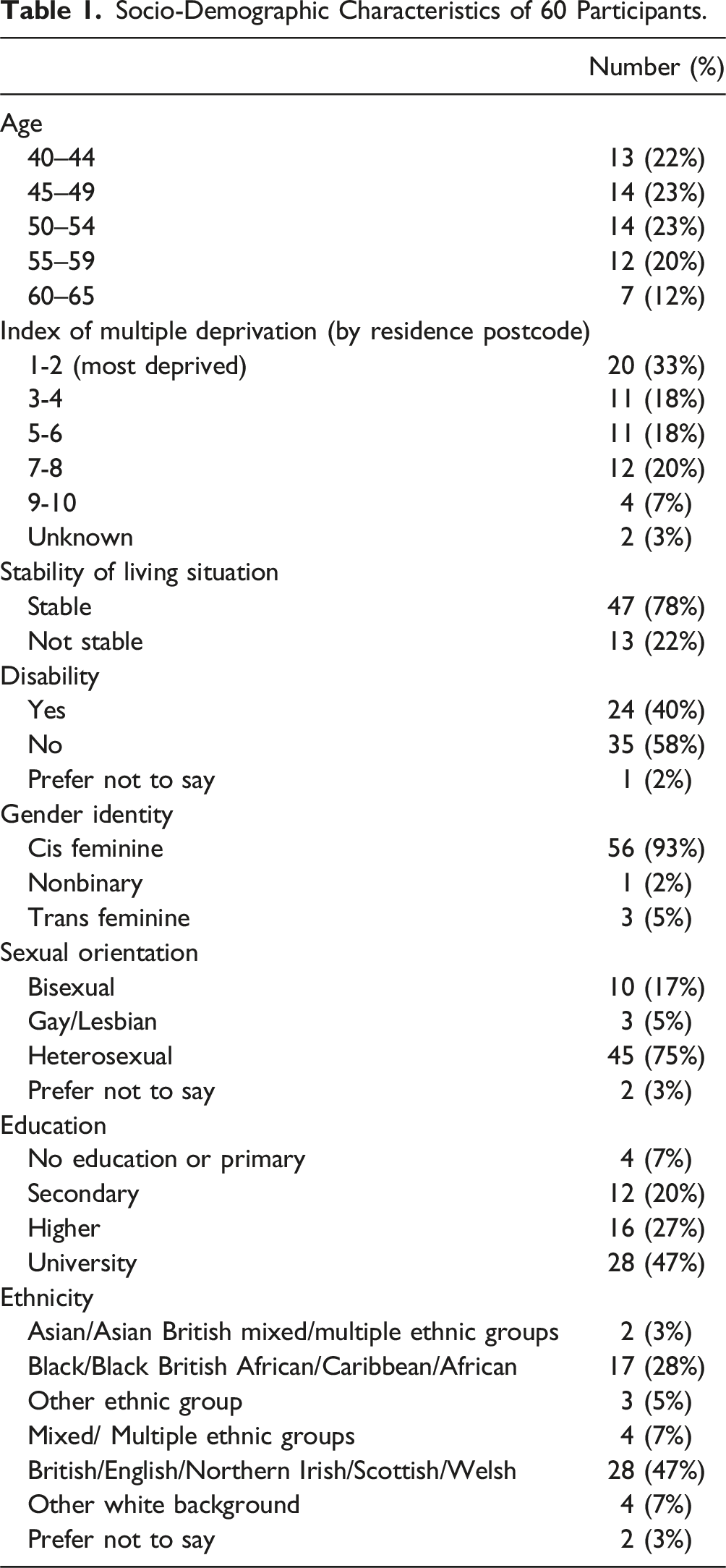
Overview of Findings
Data are presented in three interlinked themes: the lack of prioritisation of midlife women in society; the lack of general knowledge around midlife women’s health and wellbeing; and the stigma and cultural norms which prevented access to care. Each theme is introduced with a description of how the theme relates to the enablers, barriers, and feasible improvements to WHWS for midlife women. A table which summarises the enablers and barriers which have been identified within the theme accompanies each introduction. Within each theme the data are discussed in the context of interpersonal, intrapersonal, organisational and public health policy constructs of the Socio-ecological model (SEM).
46
Barriers and facilitators for each are discussed in parallel. Quotes are presented as supporting evidence, with the interview or focus group number, participant age, and the Index of Multiple Deprivation (IMD) which has been derived from the postcode of their area of residence cited. Common to the three themes was the intersecting disadvantage conferred by being a midlife woman and belonging to a marginalised group, due to income, education, sexuality, gender identity, ethnicity, disability, and comorbidities. The relationships between the themes and subthemes are represented by Figure 1. Methods to build on current strategies, such as utilising the Integrated Care System (ICS)
71
to fill gaps in poor service provision using self-testing services, as well as novel facilitators to access were also endorsed, such as modernised education which is targeted at midlife women. Visual representation of the relationships between themes and subthemes.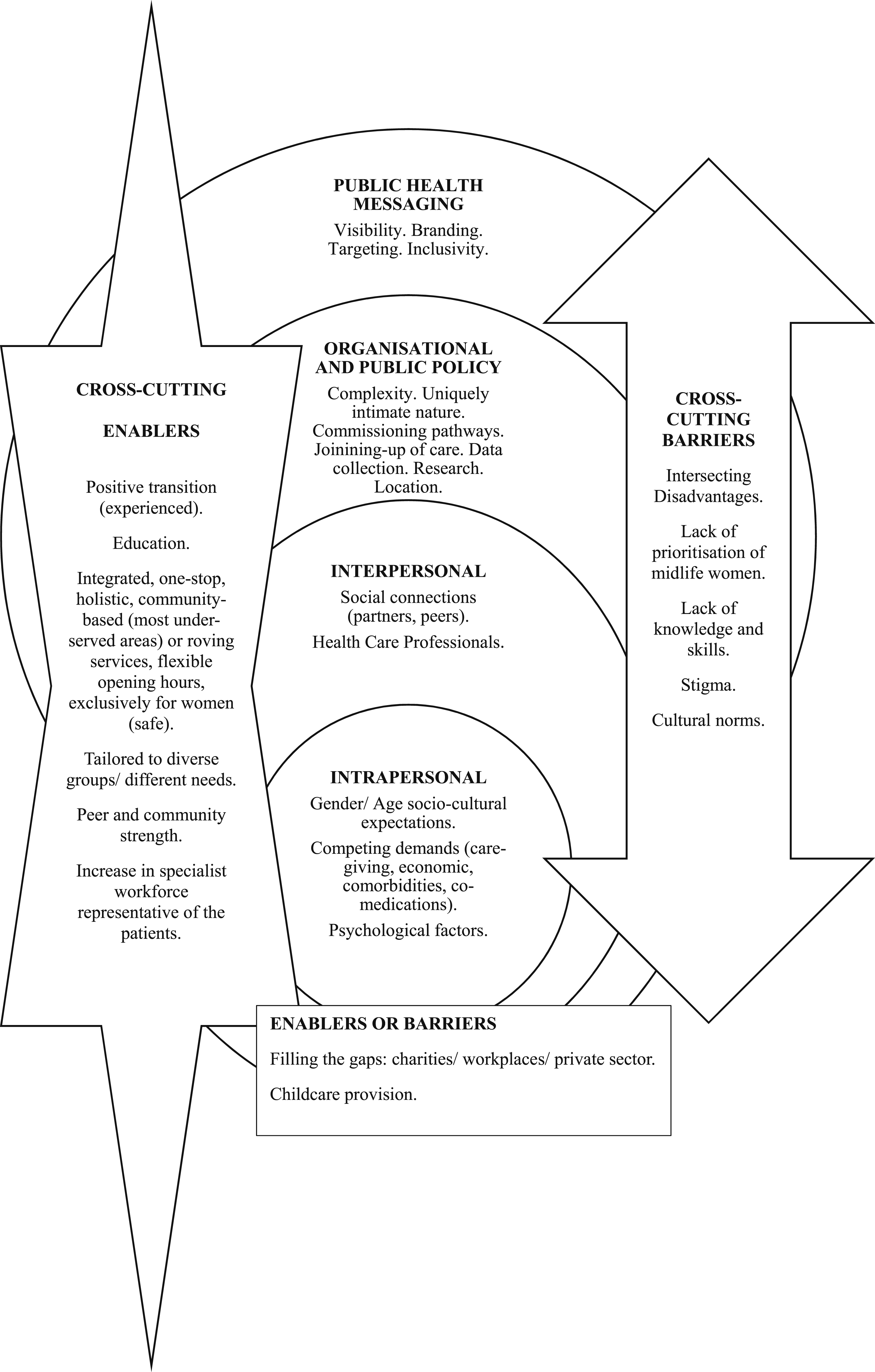
Cross-Construct Theme 1: The Prioritisation of Midlife Women
Cross-Construct Enablers and Barriers (Theme 1: The Prioritisation of Midlife Women).

Theme 1: Intra-Personal Constructs
Psychological Factors
Several participants viewed midlife as a time of positive transition. They described an increased sense of self-worth, self-trust, and an improved ability to self-advocate, having learned from past experiences. This empowered them to prioritise their own health and wellbeing and to access WHWS. When I decided to accept (cervical screening) again years later I felt a bit stronger. And (I) was able to say (to the nurse) “this was my last experience, and I really hope that this time around is different”. So, it was different. (Participant 29, age 53 years, IMD 1)
Gendered Socio-Cultural Expectations
However, participants also described, in the context of a national healthcare system that was facing unprecedented financial and workforce pressures,
72
how they altruistically self-rationed access to services. They attributed their endurance of pain without seeking help, and the tendency to put the needs of others first, to gendered socio-cultural expectations. In comparing the severity of their own symptoms with others, they had minimised their own health problems. Similarly, the prioritisation of the sexual requests of (male) partners had disconnected some participants from the needs of their own bodies. A few participants described how they had expected discomfort during sexual intimacy. It can be postulated that their anticipated tolerance of this may have inhibited them from seeking WHWS. (We have) just been taught that, you know, a certain amount of pain for women is normal. (Participant 27, age 54 years, IMD 6)
Competing Demands and Comorbidities
The stoicism that many participants successfully employed to cope with daily life sometimes prevented them from accessing services. This had often been bred from previous experiences of a healthcare system that had failed to meet their needs. Several participants described how they had prioritised learning to cope with debilitating symptoms, rather than repeatedly exhaust themselves trying to obtain (inadequate) help. So, when I do get a lot of pain, I feel it's not worth contacting anybody anymore. Last time I was in a lot of pain (endometriosis) and ended up in A&E (Accident and Emergency). But I was just given painkillers and told to wait for another referral. And then obviously you have to wait another year for that referral. (Participant 5, age 47 years, IMD 1)
Care-giving responsibilities (child and elder), combined with careers, resulted in a limited capacity to prioritise timely use of WHWS in a system that was arduous to navigate. From my own example I can see it because I’m always so busy and leave myself at the last place. It’s always probably my family, my mother, my husband, everyone else. And then suddenly with oh, I’m not really okay. (Focus group 3, mixed group, age range 42–59 years, IMD range 1–9)
Professional Carers were often unable to take time for their own healthcare appointments. Participants with multiple marginalised identities such as those on low incomes, participants with transgender and gender non-binary identities (TGNB), and migrants to the UK, were disproportionately affected by competing demands. This was due to less workplace flexibility in taking time out of work to try to book or attend appointments when they needed to earn enough money for food and housing.
Although a few participants had benefited from the support to access WHWS which had been provided by HCPs from other seemingly unrelated health services, the increased number of comorbidities that often occur with age had made it challenging for participants to ensure that they received the correct treatment. This was particularly true for participants who had also struggled with poverty. One participant described how a reduction in her state benefits had coincided with cost-saving measures that had left her with inadequate continence products. This had made it impossible for her to attend urogynaecology appointments. Participants living with mental health conditions outlined points of vulnerability in their mental health journeys when actively seeking support, which was hard to find, had been too challenging. This had resulted in some participants repeatedly missing cervical screening. Sometimes also like you’re in a place that you need help, and you can’t exactly reach out for help. (Participant 9, age 45 years, IMD 2)
Theme 1: Inter-Personal Constructs
(Male) Partner Support
Through lack of knowledge, and sometimes lack of interest, some participants described how intimate (male) partners had not supported them to seek help from WHWS. Several participants reported that new (male) partners had prioritised pleasure over taking joint responsibility for safe sex and had displayed outdated negative fears about STI testing. One participant described her surprise and appreciation when a new (male) partner had broached the subject of testing for STIs. I was very grateful that he took the initiative and was so open about things and said let’s just go (to the sexual health clinic). We did both go and get tested. I would just have taken the risk if he wouldn’t have brought it up. (Participant 1, age 55 years, IMD 2)
The lack of joint responsibility, compared with the instigation of care seeking by (male) partners for symptoms which affected shared sexual intimacy such as vaginal dryness and loss of libido, demonstrated a complex dynamic in the impact of (male) partners on how midlife women prioritised WHWS. Several participants described the benefits that they had derived from (male) partners being educated about women’s midlife changes.
Theme 1: Health Care System Factors
Insufficient, Inequitable Services
Many participants recognised the national funding challenges in healthcare. However, the lack of health system policies that benefited midlife women, perhaps due to the significance with which their needs were viewed in society, disappointed and frustrated them. It’s funny, the argument for paying for HRT (Hormone Replacement Therapy). If men needed this, they wouldn’t be paying for it. (Participant 21, age 49 years, IMD 4)
Participants had an almost universally negative perception of WHWS, and described them as, for example, “unavailable, invisible, complicated, fragmented, dangerous, stressful”. They reported long waiting lists for basic care (menopause, gynaecology, vulval dermatology, TGNB care, mental health). A few participants had resorted to using costly private providers. It’s very, very difficult to get through on the phone, it’s engaged, or they just don’t answer…And then when I have managed to get through which sometimes has been after like dozens of attempts, you’ve missed the boat for any appointments. (Participant 16, age 41 years, IMD 9)
Many participants felt that there was a lack of organisational understanding within the healthcare system of the uniquely personal and intimate elements of many health and wellbeing problems that are faced by midlife women. This had resulted in a lack of prioritisation of joined-up care within primary care networks, for example between practices who shared long-acting reversible contraception provision. You know, smear tests, Mirena coils, none of them are that pleasant. And they feel a bit invasive. Yeah. And if you’re going to a practise which is outside of yours, you really want that process to be as smooth as possible (it was not). (Participant 12, age 58 years, IMD 6)
Participants had also experienced a lack of coordinated care between primary care and gynaecology services. This had particularly impacted participants who had required complex care due to comorbidities in midlife, for example menopause while living with endometriosis. Participants advocated for mechanisms such as dedicated telephone lines for professionals to share expertise to improve care for women with multiple comorbidities. I just wish that was another option for the GPs (General Practitioners) so (that) they could speak to someone, but it seems like it’s just as hard for GPs (General Practitioners) to get in touch with consultants as it is for the patients. (Participant 5, age 47 years, IMD 1)
Several women reported suboptimal care due to GPs not having regularly updated, easily accessible resources about where they could refer women for complex menopause care, psychosexual services, vulval dermatology, and TGNB care. A regular mapping exercise with a real-time updated database which could detail local services was suggested.
An absence of streamlined commissioning of services (e.g., sexual health clinics not commissioned to provide progesterone-releasing intrauterine device as part of Hormone Replacement Therapy), and a dearth of commissioning or a ‘postcode lottery’, for services important for many midlife women (pelvic physiotherapy, incontinence services, psychosexual care (unless women fulfilled the heteronormative and multi-exclusionary criteria of suffering from painful penetrative sexual intercourse)) were repeatedly raised. I have a lot of pain in my vagina and my bladder, and I got told there was no sexual dysfunction clinic for women. So basically, they (providers) were like, we only have it for men, we don’t cater for women that have issues, you know. (Participant 22, age 52 years, IMD 6)
Participants suggested that these barriers were particularly challenging for women from more underserved groups, who had less knowledge, capacity, and time to advocate for themselves.
Re-branding and Public Health Messaging
When considering the current model of care, a re-branding of sexual health services to ensure that midlife women are aware that they do not solely cater for young people was proposed. Public awareness campaigns about: sexual wellbeing for midlife women, STI testing (including online methods), and information about incontinence and genital dermatological conditions (all of which they had never seen) were suggested. Like when you’re a teen or in your 20s, there’s always information about sexual health and getting tested. Obviously, it’s very different when you’re in your midlife. I don’t think there’s any information out there really. (Participant 10, age 44 years, IMD 7)
However, some women cautioned against an increase in public health messaging about midlife women’s issues, even if it did serve to improve access. They worried that in a society that they already viewed as structurally sexist, too much visibility, for example, about menopause symptoms, may perpetuate negative views about women.
Model: Integrated; Community-Based; Continuity of Care; Underserved Locations; Holistic
Although a minority of participants expressed doubts about the economic viability of moving from the current model of General Practice in the UK as the initial point of contact, many participants advocated for a new life-course model of women’s health which would be co-designed with midlife women. They described combined preventative and treatment services (primary care, cervical and breast screening, gynaecology, sexual health (including psychosexual services), incontinence services, pelvic physiotherapy, mental health, and easy access to specialist services such as for female genital mutilation survivors (FGM)). The preference was for community-based or roving services, which many participants specified should be in the most underserved locations, with a face-to-face option, and continuity of care of practitioners, with the advantage of saving time and tackling the often-interconnected conditions associated with midlife. If I’ve got an hour free with no children, you know, what would I do? I would cook and clean and shop. I wouldn’t look after myself, but if I knew that in an hour if I could, I could have my sexual health, get my repeat contraception, have my smear test done. That stops 5 separate appointments. (Participant 15, age 49 years, IMD 10)
Participants recognised the association between menopause and mental health, the culmination of life stressors in midlife, and the impact of these factors on the ability to access WHWS. Adequate treatment for mental health problems, and provision of mental health services, including counselling services, was viewed as an essential (but lacking) component of menopause care which would have encouraged them to access WHWS.
Several participants advocated for holistic care. They felt that the breadth of symptoms associated with menopause, and the range of challenges during midlife transitions, were best approached with a combination of medical and alternative health support, such as acupuncture and reflexology. Menopause group coaching, the availability of free exercise classes and low-cost vegetable stalls were all suggested as part of a holistic WHWS.
Practical Considerations and Progressive Practices
The breast screening process (a one-condition service) was used by several as an exemplar of how services should operate. It supplied clear information, easy parking, universally welcoming staff, flexible appointment times, and an efficient service which ran to time and provided punctual results. Although many participants felt that child-friendly services (ranging from the permission to bring children to appointments to onsite government funded child-care) would enable access, others opined that this may detract from the importance that women placed on prioritising their own health. It is more unhelpful if you can take your kids there… (it is better to have) something that says “no actually you’re important, this is for you”. (Participant 13, age 49 years, IMD 2)
Participants who identified as TGNB described the change in STI self-testing kits, from being based on gender to anatomy. This had improved their experiences and encouraged their use. Participants described how being able to conduct their own HPV screening, an option currently being trialled in some parts of the UK, would have encouraged them to access services. Already frequented by midlife women for different reasons, and viewed as safe spaces, participants felt that pharmacies could have been better utilised to reduce waiting times, for example, for the treatment of genitourinary syndrome of menopause (vulvovaginal and lower urinary tract symptoms related predominantly to low oestrogen levels), and provision of HIV Pre-exposure prophylaxis.
Cross-Construct Theme 2: Knowledge and Skills
Cross-Construct Enablers and Barriers (Theme 2: Knowledge and Skills).
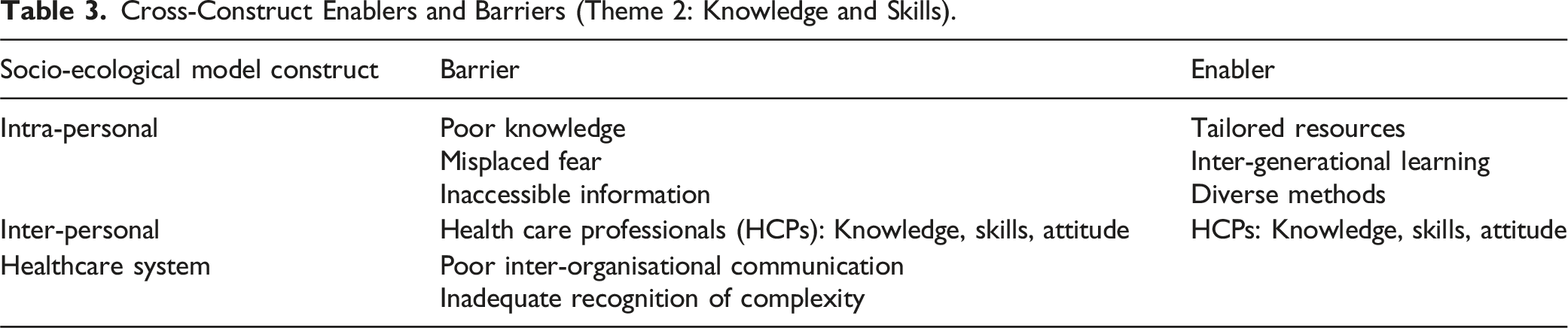
Theme 2: Intra-Personal Construct
Poor Knowledge
Lack of knowledge about the risk of contracting STIs, symptoms, management options, and available WHWS inhibited access to menopause services, sexual health services, primary care (including breast and cervical screening), dermatology, gynaecology, and urogynaecology. We (midlife women) are not really going to pick anything up (STIs). Like you probably would have got some immunity or picked it up earlier in life. (Participant 27, age 54 years, IMD 6)
For many participants information had been too late. Several participants described how they had only happened upon explanatory information about psychological and cognitive menopause symptoms many years after their symptoms had started. Years later you realise actually it wasn’t anything to do with the fact that you were so stressed out. It was actually this thing called brain fog, which I discovered online. (Focus group 3, mixed group, age range 42–59 years, IMD range 1–9)
Misconceptions among some participants about how to ‘diagnose’ the menopause had fostered distrust in providers and thereby may have affected their subsequent access to WHWS. They had surmised that tests had been withheld on financial grounds, rather than appreciating that the menopause is usually diagnosed without investigations. Most participants described a lack of knowledge about the breadth of menopause symptoms. They advocated for a long list of possible symptoms to be included when menopause awareness was raised in the public sphere, rather than what they viewed as the current inaccurate focus over hot flushes. So, there weren’t any obvious symptoms. It wasn’t like I was suddenly hot flushing all over the place and all that, which I’ve never really had. It was suddenly this kind of like doubting yourself in your normal work environment… and having to sort of like work this out with friends. (Small (2 participants) Focus group 2, ages 54 and 51 years, IMDs 2 and 8)
Two symptoms associated with the menopause that participants repeatedly mentioned as poorly recognised by midlife women were mental health changes and genitourinary syndrome of menopause (GSM). Most participants were unaware of management options for GSM. This had inhibited some from new sexual relationships, and they had viewed it as a normal part of ageing. I’m not sure where I would go (for treatment of GSM) if I’d suddenly decided I wanted to have a (sexual) partner. (Participant 7, age 63 years, IMD 4)
Misplaced Fear and Inaccessible Information
Despite attempts by scientists, and to some extent, the mainstream media to correct outdated public health misconceptions, several participants had been deterred from seeking treatment for menopausal symptoms by an inflated fear of the breast cancer risk associated with Hormone Replacement Therapy (HRT). I tried to manage without it (Hormone Replacement Therapy) until I got desperate. I had heard things, and I was worried about the breast cancer risk. I didn’t know where to get (the) right information. (Participant 1, age 55 years, IMD 2)
Participants felt that enablers to WHWS would have been translation of WHWS information, multi-lingual representation among HCPs, and culturally tailored and co-produced information (including outreach work) about midlife changes and available services. For example, the absence of the word ‘menopause’ in some languages, the non-medicalised views of the menopause in some communities, and differences in cultural empowerment in the ability to seek help among midlife women meant that to provide menopause care for migrant women, education that served specific communities was required. I was in my 30 something years. I’d never heard of that word (menopause). I didn’t know what it was (Focus group 1, disabilities and multiple ethnicities group, age range 43–65 years, IMD range 1–8) I can ask the right questions (about menopause care) when I know what is available (Focus group 1, disabilities and multiple ethnicities group, age range 43–65 years, IMD range 1–8)
Inaccessible prose, described by women as ‘dense leaflets’ and ‘heavy language’, was felt to be prevalent in women’s healthcare information. This had rendered some services inaccessible for women with a lower level of literacy or health literacy, or who spoke English as a foreign language.
Opportune Time for Acquisition (Knowledge and Skills) Using Diverse Methods
Participants displayed an appetite for acquiring the knowledge and skills to improve their health and wellbeing and use of WHWS. They suggested themes, methods and locations for education. Some participants proposed that midlife was an ideal time to obtain this knowledge. They related this to the strengthened ability to self-prioritise that they had developed with midlife (theme 1).
A range of methods to improve education about midlife changes and thereby widen access to WHWS for midlife women were suggested. Participants generally advocated for GPs to deliver this information, either opportunistically or using dedicated appointments. A ‘Bible’ with resources about midlife changes distributed by primary care was proposed. Others suggested that information about the midlife changes should be enclosed in cervical or breast screening invites. Text messages and e-mails with information from trusted sources, such as the National Health Service (NHS) were also recommended. However, one participant who identified as TGNB expressed suspicion of NHS messaging, having experienced that services were not as inclusive as they had purported to be. They preferred to rely on recommendations from community members. Indeed, peer support (‘Meno-wives’ (women supporting others through menopause), health coaches, support groups) was advocated by women from different nationalities as providing accessible, community-specific, education. It offered an intermediate link for support and the sharing of experiential knowledge that some women found uncomfortable to obtain from other sources. I went to this workshop, and they talked about vibrators. It was just so open and freeing to speak to a group of women who were having the same issues (sexual dysfunction). (Participant 8, age 55 years, IMD 5)
Conversely however, several participants had been dissuaded from accessing menopause services by friends as they had worried that they would be prescribed antidepressants (which although sometimes correctly used as treatment, they did not want).
A few participants felt fortunate to have received menopause education in their workplaces. Not only had this provided information for themselves, their colleagues, and their managers, but it had also validated their symptoms and had promoted better workplace support when they had required WHWS. Although some participants were aware that menopause guidance in the workplace was gradually being introduced in the UK, they felt that it had not reached the places where it would benefit the most under-resourced women. Participants recommended that information about midlife women’s issues and symptoms and the locally available WHWS should be distributed in a wide range of places. These included public billboards, libraries, buses, gyms, public toilet doors, nail bars, supermarkets, television, radio, magazines, podcasts, story lines in soap operas, and dedicated safe spaces such as women-only clinics that dispensed education as well as services, food banks, and children’s centres. There were mixed views about whether social media had enabled access to WHWS. Some participants had been distrustful of accuracy, whereas others cited celebrity ambassador ‘influencers’ as valuable sources of information. One participant had been inspired by a midlife acquaintance who had announced on social media that she had successfully persuaded an HCP to allow her to insert her own speculum.
Theme 2: Inter-Personal Construct
Health Care Professionals (HCPs): Knowledge, Skills, and Attitude
Participants described deficiencies in the knowledge of primary health care providers which tellingly mirrored the main areas of poor knowledge among midlife women. These regarded the diagnosis of menopause, mental health symptoms related to the menopause, and genitourinary syndrome of menopause. This had eroded trust and prevented several participants from accessing timely and correct care. One participant outlined how she had felt that the assumptions made by HCPs (of hypochondria and attention seeking) due to her mental health condition, had led to catastrophic failings in her care. These had resulted in ongoing incontinence, and had deterred her from seeking help again. The prevalence of assumptions about gender identity and heteronormative sexual identity that were made by a variety of HCPs was a barrier to accessing care for participants of different gender identities, different sexualities, and for participants with sexual problems that were not based on male-orientated pleasure. Sometimes the reaction they (HCPs) have towards you when you identify yourself as such (TGNB), it’s not very comfortable. If there are times I need to reach out for help, I tend to try to hide my identity, which I do not like. (Small (2 participants) Focus group 1, ages 45 and 48, IMDs 1 and 3)
A few participants described experiences in which they had been subjected to procedures, perhaps partly due to time pressure on HCPs, which had compromised their dignity and safety. This had affected their confidence in seeking further help. I am there, quite literally naked. Yeah, legs wide open. There are men walking here like a bus station. And then he’s sticking the needles inside my private. I'm in so much pain. He didn’t say “it is hurting?” …And then he said, “get yourself dressed”. So, I went to change in the other room when he was busy telling me my results. I wasn’t paying attention because if you wanted to talk to me, you would have sat me down and speak to me and explain everything. (Focus group 1, disabilities and multiple ethnicities group, age range 43–65 years, IMD range 1–8)
One participant, after several negative interactions which had resulted in her feeling that the HCPs may have racist and misogynist beliefs, had resorted to only attending WHWS appointments if she was accompanied by a friend or family member. For some people who identified as TGNB, separate services, preferably with HCPs who identified as TGNB and therefore had lived experience of some issues, felt safer and more comfortable. They had experienced that many HCPs did not know which care it would be advisable for people who identified as TGNB to receive, for example, mammograms, sexual health, and which services would provide these.
Theme 2: Health Care System
Complex System
When HCPs did have good knowledge and skills, they were often limited by the amount of time that they had available in a system that was not designed to deal with complexity. Participants described how this contributed to the feeling of futility when they had considered accessing WHWS. They viewed their conditions as best treated in a manner that acknowledged diagnostic and management uncertainty, and the inextricable links between mental, physical, and sexual conditions. They felt that increased consultation lengths for WHWS, supported by women leaving consultations with a clear plan to return, if necessary, were vital to HCPs being able to work effectively. This would avoid repeated presentations due to hasty diagnoses and ensure that both HCPs and women had the time and space to make well-informed decisions. I was just focusing on headaches, ‘cause they were the number one thing. But there’s so much more to this (the menopause) than just one thing. So, I just thought right, I’ve got 5 min. This is what I want to explain. Just get rid of these bloody headaches because I can’t work with them anymore. (Small (2 participants) Focus group 2, ages 54 and 51 years, IMDs 2 and 8)
Cross-Construct Theme 3: Stigma and Cultural Norms
Cross-Construct Enablers and Barriers (Theme 3: Stigma and Social Norms).

Theme 3: Intra-Personal Construct
Sexual Health Stigma
Participants described discomfort with the idea of being seen using a sexual health clinic. Some had been dissuaded in the past by the thought of encountering younger acquaintances. They had worried that others would assume that they had contracted a STI, and they felt that they were not places that midlife women were expected to visit. STIs are very stigmatised- you only go there (sexual health clinic) if you have lots of partners or are worried you may have an infection. But I wouldn’t go to the GP- I would worry about confidentiality and anonymity. I see them more as a family doctor, not treating sexual things. If there was a special service for women that was available that I knew about, then I would use it. (Participant 1, age 55 years, IMD 2)
Theme 3: Inter-Personal Construct
Cultural Expectations, Beliefs and Practices
Participants described their reticence in speaking to family, partners, and HCPs about the mental, physical and sexual changes that midlife had presented. They attributed this to many reasons which were often interlinked with stigma and engrained social norms, such as embarrassment and the insufficient societal normalisation of women’s sexual issues in midlife. I think it’s around having permission to talk and feeling confident. And not being alone because the conversations (sexual dysfunction in women) aren’t happening. And it can be really frustrating because you can’t turn on the TV without seeing something about Viagra (Participant 13, age 49 years, IMD 2)
Many participants were optimistic that there had been a gradual cultural shift, perhaps assisted by the online world. They felt that younger generations (their own children or people that they worked with) were more open to discussing previously stigmatised issues, and more accepting of people who may be different from them.
The highly prevalent worry about being judged by others for accessing sexual health services was compounded by specific cultural beliefs. Two participants described the taboo within their different Black African communities of midlife women. Women may not be assertive, about safety when it comes to sex with partners especially in our Black communities because men have always been dominant (Participant 12, age 58 years, IMD 6)
Theme 3: Health System and Public Policy Construct
Health Care Professionals (HCPs) to Broach Sexual Health and Wellbeing
Several participants had experienced a lack of professional curiosity from HCPs about sexual health and sexual wellbeing difficulties. I asked about testosterone, and it was just a “no, we can’t give those”. It wasn’t “why do you need testosterone, let’s book you in for a chat”. (Participant 15, age 49 years, IMD 10)
Many participants believed that the onus should be on the professional to broach these issues when appropriate. It can be postulated that societal stigma around intimate health and wellbeing issues, coupled with time restrictions, affected some HCPs. Some participants compared their negative experiences with GPs with the confidence with which sexual health clinicians had raised similar issues and wondered whether sexual health services should be the initial point of health and wellbeing care for midlife women. You know, at no point during any of the conversations that I've had around HRT (Hormone Replacement Therapy) has sexual well-being ever come into it. No one’s ever asked about the sex. No one’s asked about vaginal dryness. Those conversations just haven’t happened. (Participant 29, age 53 years, IMD 1)
‘Women-Only’ Services With Representative Health Care Professionals (HCPs)
Among the participants in this study, there was extensive advocacy for ‘women’-only services (most participants in this study expressed their understanding that this included people who identified as TGNB), and ‘women’-only waiting rooms, from safety, comfort, equity, and some religious and cultural perspectives. Participants had noticed that some regional sexual health services offered evening clinics for men but not women. As a woman, you already feel a bit vulnerable, but you might have to sit opposite some guy who’s staring at you. (Participant 27, age 54 years, IMD 6)
Similarly, for some participants, consulting a provider who identified as male was not acceptable, for cultural or religious reasons. Several participants narrated negative experiences with HCPs who they opined identified as men, regarding lack of empathy, dignity, and safety. And I do think personally for me, if I’ve got women’s problems, I feel really, uncomfortable and it’ll put me off going if men are in there. (Participant 25, age 44 years, IMD 2)
Recommendations Proposed by Participants, Categorised by Construct of the Socio-Ecological Model.

Discussion
A diverse group of midlife women described a multiple range of intersecting barriers which they felt contributed to the low uptake of important Women’s Health and Wellbeing Services (WHWS) and poor health outcomes, as well as the widening health inequalities between midlife women in a region of South-East England. This study bridged a wide range of findings from more focused studies in the fields of women’s health, sexual health, and public health, and provided a structured evidence base for the impact of the lack of prioritisation of midlife women within society, the inadequate knowledge about the health and wellbeing issues of midlife women, and the stigma and cultural norms of structurally embedded sexism and ageism on access to WHWS. By employing the Socio-ecological model (SEM), with an intersectionality lens and a feminist pragmatist stance to project the factors affecting access to WHWS from the perspective of midlife women with a focus on those from the most underserved groups, the study enabled a granular understanding of the complex, interlinked, and holistic nature of acceptable strategies to improve access to WHWS.
Comparison With Existing Literature
This study confirms findings from previous work that many women recognise the midlife transition as an opportunity for a fresh psychological perspective for self-prioritising health and wellbeing. 73 However, this is often muted, across different contexts, by the barriers of competing demands on time and energy, 74 psychological factors such as poor self-esteem, 14 and inadequate health literacy. 75 In particular, lack of knowledge among midlife women and wider society, around sexual health in midlife, 14 mental health, 75 and genitourinary syndrome of menopause 76 continues to inhibit access to WHWS for midlife women.
Associated with the lack of public knowledge around midlife changes, are pervasive gendered and ageist attitudes across society which continue to affect access to WHWS.17,77 They are evidenced in this study by the non-existent public health messaging around midlife sexual health changes, and fundamental healthcare system omissions. These include the absence of important pelvic physiotherapy and psychosexual services. Structural sexism, the unequal gendered distribution of power, status, resources, rights, roles, and opportunities that are manifested within society and health care systems, has a significant impact on access to WHWS. 54 A move from considering gender as something that can be added onto the existing health model, to a system which reflects a gender equitable society, and acknowledges that gender inequity continues to shape health systems and outcomes, is required. 78 By employing a feminist pragmatist perspective, this study has highlighted the frequently unrecognised impact that the intimate and vulnerable nature of many midlife challenges has on access to WHWS. This augments the existing evidence for a diverse, trauma-informed workforce79,80 who work in co-designed organisations which feel safe for women. Health care policies and programmes that acknowledge and address the unique health and wellbeing, including sexual health and sexual wellbeing, needs of midlife women, are overdue.81,82
Barriers to WHWS are particularly apparent for, and have the most ramifications for, midlife women from underserved groups. These have previously been demonstrated to be midlife women from migrant communities, 83 with a lower socioeconomic status, 84 and living with stigmatised conditions such as HIV. 85 The persistence of heteronormative assumptions when planning and delivering WHWS continues to reinforce outdated and discriminatory messages. 28 The inequities inherent to accessing WHWS, which are based on discriminatory hetero and gender normative models, for people who identify as lesbian, gay, bisexual, transgender, queer (or sometimes questioning), intersex, asexual, and other sexual identities, are likely to be further affected by global political threats. 86 The intersectionality lens employed in this study highlighted that those women from underserved groups due to income, education, sexuality, gender identity, ethnicity, disability, and comorbidities (especially mental health), have less power to demand adequate WHWS. A small number of adequately resourced participants indicated that private providers (paid for services) and charities filled some health care system and policy gaps, for example in menopause care. It can be postulated that this may have disguised the extent of insufficient provision and have resulted in commissioning decisions that further widened the gap in care for underserved groups.
Strengths and Limitations
To the best of our knowledge, this is the first study to contextually explore the enablers and barriers to WHWS and provide feasible solutions (prioritisation of the needs of midlife women, modernised and inclusive education, integrated, holistic, community-based, and safe services) for improving access and equity of access, for midlife women in England. Although the study was limited to an area in the South-East of England, it can be postulated that the barriers to services, many of which were the result of nation-wide challenges, were true in other regions within England. Three of the focus groups which had a mixture of midlife participants only had two participants. Although this limited generalisability, the format allowed an interactive, detailed discussion between the participants, which enabled the extension of the data beyond an individual interview. The wide age range of participants in this study provided a breadth of perspectives across time and evolving social norms. However, there is great variation in mental, physical, and social health between the ages of 40–65 years. 87 There are also significant differences between women of the same biological age due to genetic and environmental influences. 88 By aggregating data from women across this age range, it is possible that societal nuances that relate to specific ages may not have been captured. A small minority of participants (seven percent) in this study identified as TGNB, and most participants (75%) identified as heterosexual. Although the inequities inherent to the care of gender and sexual orientation minorities when accessing WHWS was raised by these participants, this has not been discussed in detail in the results. While valuing the opportunity to highlight this issue, the steering group recognises the significant and unmet need for focused community led research within this area. Although strategies to avoid cultural bias were employed, including researcher reflexivity, it is possible that important cultural differences between participants were not illuminated. The exclusion of non-English language speaking participants may have resulted in the lack of representation from important national and cultural perspectives. Women who do not speak English have unique needs, and further research is required to elucidate how to distinguish their challenges in accessing WHWS.
Implications for Research and Practice
Provision of modern, holistic education, at the appropriate time, about midlife changes, is imperative for destigmatising, and encouraging the utilisation of WHWS. Improvements in nursing and medical training curricular, and continuing professional development, particularly communication skills, and multidisciplinary clinics should be combined with co-produced changes to healthcare, social, and workplace policies, to recognise the neglect of midlife women in these spheres, and the erosive and outdated nature of hierarchical, paternalistic, medical care. A wider societal understanding of the importance of midlife issues that occur for all women, including problems in access to WHWS, may engender support from (male) partners and facilitate joint ownership of health and wellbeing issues. Employing a feminist pragmatist approach, which seeks to place the women’s voice at the centre of feasible suggestions, we propose the development of accessible (via public transport, extended hours, and self-bookable), safe (women-only, provided by women), holistic, integrated (cervical screening, primary care, menopause care, urogynaecology care (including pelvic physiotherapy and FGM care), sexual health and wellbeing care (including psychosexual services), social care), community-based (underserved areas), feedback-responsive WHWS, which make better utilisation of pharmacy and self-testing options.
Supplemental Material
Supplemental Material - The Enablers and Barriers to Accessing Women’s Health and Wellbeing Services for Women Aged 40–65 Years: A Qualitative Study
Supplemental Material for The Enablers and Barriers to Accessing Women’s Health and Wellbeing Services for Women Aged 40–65 Years: A Qualitative Study by Kiersten Simmons, Jenny Hyde, Damla Harmanci, Collins Iwuji, Stephen Bremner, and Carrie Llewellyn in Community Health Equity Research & Policy
Supplemental Material
Supplemental Material - The Enablers and Barriers to Accessing Women’s Health and Wellbeing Services for Women Aged 40–65 Years: A Qualitative Study
Supplemental Material for The Enablers and Barriers to Accessing Women’s Health and Wellbeing Services for Women Aged 40–65 Years: A Qualitative Study by Kiersten Simmons, Jenny Hyde, Damla Harmanci, Collins Iwuji, Stephen Bremner, and Carrie Llewellyn in Community Health Equity Research & Policy
Footnotes
Acknowledgments
We would like to express our gratitude to our Patient and Public Involvement Group and to the participants who gave their time and energy to participate in this project.
Author Contributions
Kiersten Simmons: Conceptualization, data curation, formal analysis, investigation, methodology, project administration, validation, visualisation, writing. Jenny Hyde: formal analysis, investigation, validation. Damla Harmanci: formal analysis, validation. Stephen Bremner: formal analysis, validation, supervision. Collins Iwuji: formal analysis, validation, supervision. Carrie Llewellyn: formal analysis, methodology, validation, visualisation, supervision, writing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) declare that financial support was received for the research, authorship, and/or publication of this article. This research was conducted with funding provided by Brighton and Sussex Medical School, Brighton, United Kingdom. They had no role in the development, execution, and dissemination of this work.
Ethical Statement
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
