Abstract
Global learning is the practice of adopting and adapting global ideas to local challenges. To advance the field of global learning, we performed a case study of five communities that had implemented global health models to advance health equity in a U.S. setting. Surveys were developed using a Consolidated Framework for Implementation Research (CFIR) framework, and each site completed surveys to characterize their global learning experience with respect to community context, the learning and implementation process, implementation science considerations, and health equity. The immense diversity of sites and their experiences underscored the heterogenous nature of global learning. Nonetheless, all cases highlighted core themes of addressing social determinants of health through strong community engagement. Cross-sector participation and implementation science evaluation were strategies applied by many but not all sites. We advocate for continued global learning that advances health equity and fosters equitable partnerships with mutual benefits to origination and destination sites.
Introduction
The United States (U.S.) continues to lag behind comparable Organization for Economic Cooperation and Development countries in significant health indicators, due to enduring health and health care inequities. Societal, historical, and political oppression are all causal pathways to these inequities resulting in social stratification and systematic structural power differentials between the advantaged and disadvantaged.1–3 In the U.S., inequities in health and health care access disproportionately impact people of color and other marginalized groups, including in premature death and disability.4–10 In light of these widening health disparities, there is growing multi-sector interest in seeking pragmatic solutions from the wisdom and track-record of other nations in order to improve population health outcomes and advance health equity in the U.S.11–14
The practice of finding ways to resolve the widening health disparities in high income countries through lessons from low-income countries has shown promising results.15–17 However, the terms used to describe the practice and its components have been inconsistent. Some studies include ‘reverse innovation,’ ‘frugal innovation,’ reciprocal innovation,’ and more recently 'global learning' to describe the concept of bringing ideas from outside the border to the U.S. 23
Global learning, as used in this case study, is the practice of adopting and adapting global ideas to local challenges. A recent literature review defined global learning as “the practice of engaging with, exchanging, and adapting health equity-promoting ideas and interventions between countries that fosters implementation benefits that are reciprocal and beneficial to both communities.” 15 This definition emphasizes a holistic view of global learning that values equitable knowledge sharing across countries with a focus on community engagement to ensure that the practice is not extractive from an originator community, nor imposed on a destination community. By centering value and agency within implementing communities themselves, global learning seeks to redress patterns of colonization that have historically characterized many programs in international and global health.
While global learning is not a new praxis, its discipline for health equity has yet to establish a prevailing strategic framework with effective procedures and monitoring. Thus, the study aims to develop standardized framework for global learning that allows participants to apply and use common definitions, outcome measures and a methodical implementation plans in a practical realm. In an effort to expand opportunities for global learning in the U.S., the stakeholders of a university and foundation– convened a national panel of experts and established the Global Learning for Health Equity Network (GL4HE Network) with the goal of advancing the practice of global learning for health equity promoters. 18 The core of the network is a consortium of five of these experts who represent five “learning communities” in various stages of implementing global learning for health equity projects. These learning communities are in Baltimore, Maryland; Athens County, Ohio; Brooklyn, New York; Detroit, Michigan; and Navajo Nation in the Four Corners region of the Southwest. All five communities have successfully implemented global health models to advance health equity in a U.S. setting and represent diverse agencies, programs, and partnerships. The GL4HE Network initially conducted a literature review to understand the current landscape of global learning for health equity and a major gap identified in the review was the lack of reports related to implementation of global learning projects. Therefore, the team conducted a comparative case study analyses of health initiatives implemented in the learning communities to identify core principles and factors influencing the implementation of global learning toward health equity. This manuscript describes how analyses of common themes and characteristics informed the development of a global learning framework on how importing ideas outside the U.S. can be used to address local inequities.
Methods
A series of convenings were held in 2019 and the global learning literature review in 2022 identified three critical factors for expanding global learning toward health equity in the U.S.: (1) the value of global options as solutions for pressing health equity issues given the widening disparities in health and health care in the United States; (2) concerns of decision makers and other stakeholders to address the power dynamics at play in fueling inequities; and (3) factors that serve as barriers and catalysts to the dissemination and implementation of health equity research aimed at informing meaningful and scalable initiatives and policies toward health equity. 19
The funding foundation then put out a call inviting learning communities to be part of the GL4HE Network, and five communities were selected (as mentioned earlier). The network created a unifying Framework that mapped the process of global implementation to a local market while identifying and synthesizing the key elements of global learning (See Figure 1). This framework offers a practical tool to facilitate successful uptake of global learning among diverse practitioners across the U.S Global learning to advance health equity framework.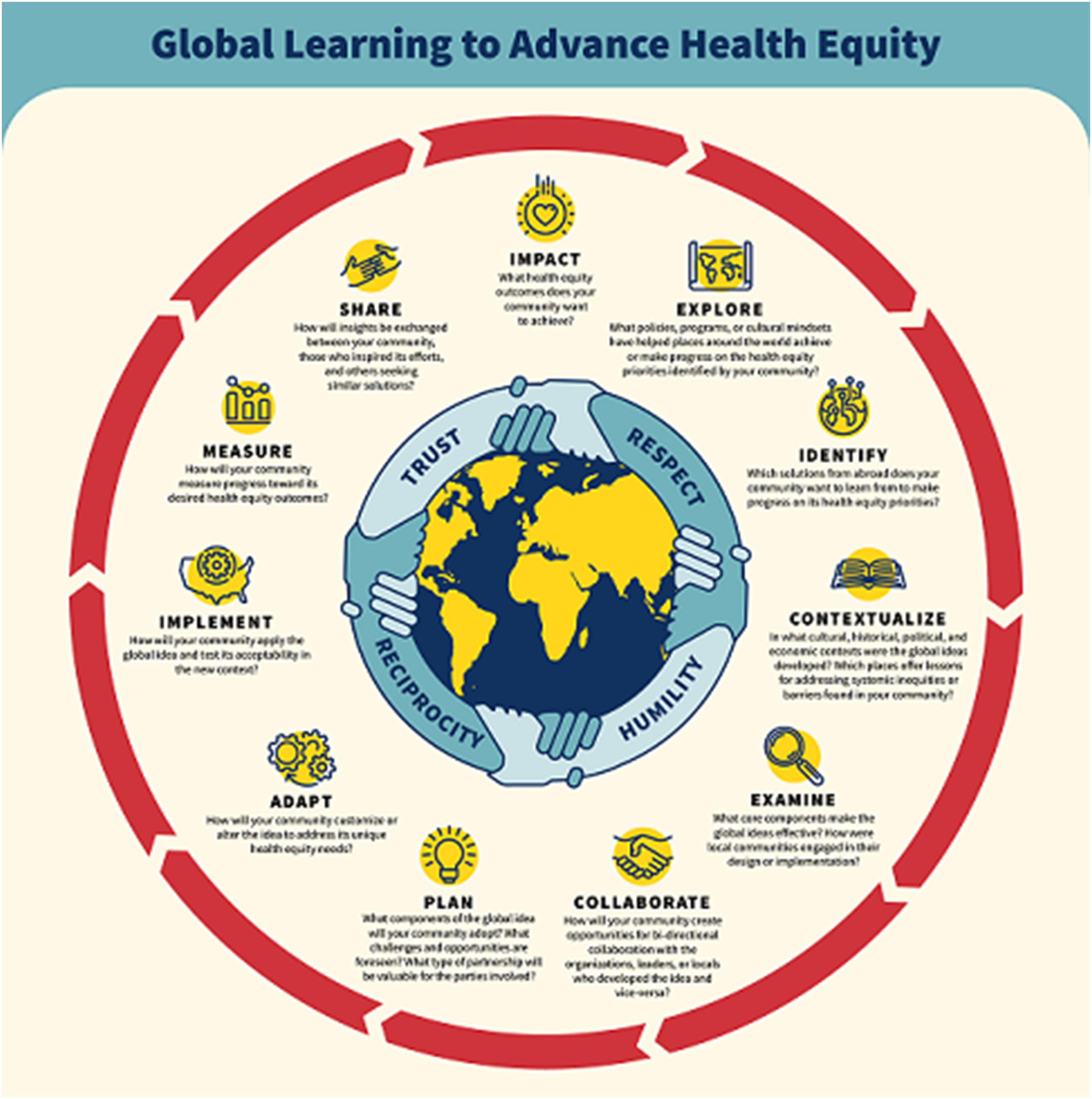
Sampling strategy
The five learning communities were purposively selected for this comparative case study based on their intentional application of global learning in U.S. domestic settings to advance health equity. The five cases represent diverse experiences, in terms of U.S. communities represented, convening institutions, global concepts applied, and the nature of interactions with global (originator) sites. As part of their global learning project, each U.S. based learning community engaged with an originator community outside of the U.S. and, based on this experience, was invited to take part in formative GL4HE Network discussions convened. Guiding principles for the GL4HE Network include cross-sector learning between and within diverse partnerships (ranging from academic, non-profit organizations, public health departments, and health care systems); collaborative leadership and inquiry allowing for broad learning and the contribution of insights from the communities' perspective; and shared activities, evaluation, knowledge building, and dissemination practices to advance the growing field of global learning. Institutional Review Board (IRB) approval was obtained from one institution and two other IRB of the institutions deemed the protocol exempt from human research.
Survey construction and validation
Two exploratory surveys were used to collect information from the U.S. based destination (implementation) sites and the global (originator) sites. The Consolidated Framework for Implementation Research (CFIR) model was used to develop the surveys (see Supplement for Survey questions). 20 Relevant CFIR domains and constructs were identified to formulate and organize survey questions. These questions were internally tested among the study team of global learning experts for clarity, face, and content validity. The survey items included demographic and context specific questions related to the sites and project leaders, socio-political context, community engagement strategies, evidence of bidirectional learning, implementation science, and health equity principles and measures. Both surveys were primarily comprised of 30-50 open-ended questions based on established CFIR domains, adapted using CFIR qualitative interview guides. The survey began with demographic and community socio-political contextual data which consisted of an exploration of the inner and outer settings of both originator and destination sites. Questions were asked to describe the characteristics of the lead implementer, influential stakeholders, and organizational structure and culture. It was also pertinent to understand community-specific assets and barriers experienced at each site. Additional questions asked how assets were used to advance the global learning project, how barriers were addressed, available resources on hand, and the networking capacity with other global learners. The remaining portions of the survey inquired about: implementation strategies utilized by the originator site in relation to the implementation process of the destination site, bidirectional learning that took place between originator and destination sites, and community engagement. The surveys were reviewed, pre-tested, and adapted accordingly.
Survey distribution and analytical strategy
Surveys were sent to 10 respondents, five site leaders of U.S. destination site teams, and five originator site leaders from the originator sites. All sites completed the surveys in Qualtrics (see survey supplement for further survey details). Survey raw data were extracted, proofread, checked for accuracy, categorized, and downloaded into an Excel file. Missing data were only encountered when respondents deemed the question to be “not applicable” and noted as such. Data were then coded by (JNK and YO) for themes of community context, demographics, program synopsis, health equity focus, community engagement, evaluation outcomes, and implementation science methods using an Excel spreadsheet. Data were then analyzed using the thematic approach, assigning teams of 2-3 individuals (VR, YO, KF, AP, RD, DP, AS, SS, ST) to review and synthesize one or two themes. Each group reviewed the coded data and raw data from each site to derive and summarize key findings. In the final step, thematic findings were then shared with the larger group to remove redundancies and lift out “cross-cutting” themes. The authors then met several times to arrive at consensus on the common themes expressed by the U.S. and originator site leaders, community members, and stakeholders and to derive a unifying construct of inter-related study findings.
Results: Case studies of learning communities
From Brazil to Baltimore: Multi-sector community engagement to support young families
How the project started
The University’s School of Nursing Office of Global Health actively searched for local and global programs with evidence of success in addressing social determinants of health and social isolation. Saude Crianca/Dara Institute in Brazil was identified as a potential program with 30 years of success and strong potential to be adapted to Baltimore. Dara was among the first organizations in the world to work with the social determinants of health (please refer to http://georgetown.app.box.com/s/8ehqo96ot9e643tbpd0p for the long-term impacts on vulnerable families with this approach). Over an 18-month period, teams embarked on the exploratory period by completing a pre-implementation assessment with teams from UMB visiting Brazil and the Brazilian team visiting Baltimore. These visits coupled with community outreach and local partnership development in Baltimore resulted in a joint submission of a proposal to the funding foundation for the Family Social Inclusion Study. Teams from both countries have continued to meet monthly over the past 4 years, first to culturally adapt and second to test the implementation of the global learning project in Baltimore.
Global concept implemented in the US
The Family Social Inclusion Study replicates the Brazilian model by implementing a one-year intervention with the purpose of promoting social inclusion and reducing social isolation and associated mental health outcomes. The intervention begins with a deep family assessment, development of a family action plan to address social determinants of health in five categories (health, housing, education, income, global citizenship), and a family navigator (community health worker) that works with families twice a month to achieve their self-defined goals in the five categories. The Family Action Plan methodology had its beginning in the pediatric department of the Hospital da Lagoa in Rio de Janeiro. There, staff understood that poverty and family life conditions were the root causes for the vicious circle of poverty, illness, hospitalization, rehospitalization and death of vulnerable children.
Health equity focus
The program addressed health equity by seeking to address underlying social determinants of health and social isolation and seeks to impact health outcomes for parents of young children in a marginalized community that has been negatively impacted by bias, discrimination, housing inequality, and racism.
Evaluation
The program evaluation includes both health and process outcomes. Process outcomes include community perspectives of social isolation, trust building, acceptability, and feasibility. Individual-level outcomes (social isolation, hope, anxiety, situational isolation, community sense of belonging, social determinants of health needs, stress, family interactions, social network analysis, progress on family action plan, barriers to completion of family action plan) were measured at baseline, six- and 12-month. The study also used an implementation science approach to measure adaptations. 21 Success stories were also collected to demonstrate impact.
Bi- and Cross-directionality
Dara Institute, the originator site, was deeply involved at all stages of the program, from conceptualization, proposal development, and implementation with constant feedback and audits for fidelity to original program throughout. The Baltimore team visited Brazil to see the program in action and the Brazilian team visited the U.S. to become familiar with the destination community. The originator site provided training and sample materials that could be adapted for implementation in the U.S. The proposal for funding the project was co-created and routine audit and feedback sessions were integrated into the implementation processes. During implementation, decisions related to modifications to the original program were discussed in meetings and implemented following consensus building. The Brazilian team was also consulted for implementation challenges, to better understand strategies that had been used in the past to overcome similar challenges in Brazil. An example included a consultation to better understand how the team coped with the mental health burden of assisting families in dire conditions. The Brazilian team shared strategies used to develop peer support groups to support the capacity of team members. The bidirectional learning between the originator and destination sites proved to be important and exemplified how one could adapt and learn from the lessons and best practices of bringing human connection to communities globally.
From Togo to New York: Community health worker aim matrix
How the project started
The bidirectional partnership between teams in Northern Togo and the Montefiore in the Bronx, New York is built on long-standing existing ties between a Montefiore provider and a community health worker (CHW) program in Northern Togo. Throughout Togo (originator site), there were efforts to optimize CHW program delivery with various partner organizations representing multiple contexts through a learning coalition called the Community Health Impact Coalition (CHIC, https://chwimpact.org/). When the opportunity presented to work with local Bronx-based organizations to improve current CHW programs locally, the team sought learning and best practices from guides established through CHIC.
Global concept implemented in the US
The Togo implementation team focused on utilizing a performance improvement tool, the CHW AIM Matrix, 22 as an implementing guide to optimize programs aimed at integrating CHWs into healthcare systems for primary care services through enhanced supervision, data systems, community engagement and quality improvement approaches.
Health equity focus
The program addressed health equity by providing a community solution (CHWs, i.e., communities experts) to partner with health systems to address social inequities that impact health outcomes. The direct engagement of community members in the Bronx and Northern Togo as part of the solution was an important part of an equitable process. There had been numerous previous examples in the Bronx and Northern Togo communities of both health systems and organizations that had not been successful at either engaging key stakeholders or identifying sustainment mechanisms to continue programming. The early contributions and engagement of community voice has been a key focus as a result.
Evaluation
Both teams used implementation science frameworks including RE-AIM & CFIR to assess fidelity, reach, effectiveness, and adoption. The Bronx team was interested specifically in measuring the percentage of patients identified with unmet social needs who were referred to a CHW.
Bi- and Cross-directionality
The Togo team was involved in providing early input into the program, and the Bronx team plans to provide feedback to the originator site about the program results in the future. There are research team members on both teams that work in both settings and the organizations/institutions involved are working on formalizing this partnership this year.
From Jersey UK to Detroit: CHW model (Knock and Check) for isolated elders
How the project started
In 2015, Henry Ford Health System based in Detroit, Michigan, was invited by the Institute for Healthcare Improvement (IHI) and the Commonwealth Fund to participate in a Learning and Action Network to promote global learning to transform U.S. health care systems. For this initiative, the sponsors developed a compendium of more than 100 global innovations in healthcare and matched each destination site to potential innovations based on their goals. 23 The Henry Food team (destination site in the U.S) identified goals of reducing social isolation, improving quality of life and reducing health utilization costs among Detroit seniors and was matched to four relevant programs. After conducting visits to originator sites, the Henry Ford team selected two originator site innovations, both of which focused on promoting better community health integration with clinical care delivery. Leading the team’s participation was Henry Ford’s Global Health Initiative, its international research, training, and capacity development arm.24,25
Global concept implemented in the US
The team adapted the “Call and Check” model that originated with the Jersey Post in the Channel Islands. There, letter carriers visit elderly residents who live along their routes for weekly chats to improve feelings of loneliness and social isolation. They work with regional medical and pharmacy authorities to fill prescriptions, make appointment reminders, and share urgent updates with care providers. While efforts to pilot the Call and Check model with the Detroit branch of the US Postal Service were unsuccessful, Henry Ford adapted the model leveraging its existing internal CHW program. These CHWs conducted weekly check-ins with elderly residents of a senior care apartment facility near their downtown flagship hospital. Screenings and referrals to community resources were made to address social determinant of health vulnerabilities including isolation and loneliness, while care management activities helped improve access to preventive care for elderly residents.
Health equity focus
A 2015 community health needs assessment identified significant burden of disease and disability from high rates of isolation and loneliness among seniors. By addressing these “whole-person” health needs, elderly adults living in low-income and resource-limited communities of Detroit, the “Knock and Check” program improved seniors’ access to social resources and strengthened perceptions of community connectedness among participating residents.
Evaluation
Evaluation assessed the extent to which “Knock & Check” reduced social isolation, improved well-being, and decreased unnecessary emergency room utilization. Validated instruments (WHO-524, PROMIS Scale25) were used to measure social isolation. The program enrolled approximately 40 individuals and while the sample size was too small to be statistically representative, comparing pre- and post-intervention data indicated some evidence of reduced social isolation. Participants reported a 75% reduction in social isolation measurements and 25% increase in preventative health screening participation. Process outcomes measured activity outputs, including weekly CHW visits, number of screenings completed, and number of community events held. Qualitative feedback from elderly residents on perceptions of collaboration with CHWs suggested an increased sense of trust among elderly residents and others living in the facility.
Bi- and Cross-directionality
The program’s success was attributed to the bidirectionality in the initial planning phases through quarterly meetings between the originator and destination sites. The program was funded with the intent of exploring how global learning can impact U.S. health systems and to disseminate experiences to other U.S. audiences. It was the first of several global learning initiatives toward health equity that have taken place at Henry Ford in successive years to address topics including maternal mortality, mental health, provider burnout, and social health integration. Knock and Check jumpstarted a culture of global learning innovation that remains strong across Henry Ford.
From Cuba to Navajo Nation: Sovereign, public systems to advance health equity
How the project started
A community-based non-profit organization in Navajo Nation was invited by Medical Education Cooperation with Cuba (MEDICC) to take part in a U.S. network of global learners. MEDICC is a non-profit that works to promote U.S.-Cuba health collaboration and highlight Cuba’s public health contributions to global health equity and universal health care. One of MEDICC’s initiatives – Community Partnerships for Health Equity (CPHE) – sends teams of community members from the U.S. (destination site) on a series of trips to Cuba (as the originator site) to learn from Cuban society, culture, and healthcare in order to apply concepts in their own U.S. communities. Teams invited by MEDICC to take part in CPHE all represent communities of color that have experienced health disparities due to systematic exclusion from social and economic opportunities.
Global concept implemented in the US
The Navajo Nation, along with all the other U.S. destination site teams participating in the MEDICC program drew from a broad array of strategies learned from Cuba, the originator site. These ranged from community-based healthcare delivery, programs addressing social determinants of health, as well as broader concepts of intergenerational teachings, appreciation of art, sovereignty and self-sufficiency over public food and health systems. Drawing loosely from their experiences in Cuba, the Navajo CPHE team set up a diverse group of youth-focused programs including “trash into art”, community gardening and local agriculture projects, and early child health promotion by celebrating local Champions and pride in Navajo culture.
Health equity focus
The program addressed health equity by emphasizing the importance of self-sufficiency and empowerment among participating community members and leaders. Navajo stakeholders identified strongly with an important Cuban concept: that equitable health systems are grounded in societal values of community engagement and inter-connectedness. In fact, the CPHE-inspired programs reflect the broader goals of embracing Navajo culture with pride and promoting change through a positive message of self-reliance as key steps toward achieving health equity. This approach reflects what the team witnessed in Cuba: that societies experiencing an oppressive history of colonization can often bear the present-day imprints of continued reliance on the external resources. The solution therefore lies in the “long game” of community-led efforts to re-center agency within communities themselves, promote self-reliance and local capacity, and nurture cultural connectedness. These inherent assets – which have endured despite the eroding effects of external policies and influences – are known to be positive influences on health outcomes.26,27
Evaluation
Community-based participatory methods were used throughout the program evaluation. Methods employed included a community needs assessment, focus groups, and the inclusion of a community advisory group. The Navajo team was interested in understanding feasibility and acceptability of programs with stakeholder feedback and disseminating successes back to collaborating stakeholders in the Navajo community. This early phase of the global learning adaption resulted in formative data that has informed future intervention research on promoting healthy diets and addressing water safety. Additional findings have focused on understanding health disparities within a socio-ecological framework, particularly highlighting positive social determinants of health present within the community and detrimental social determinants created by colonial policies and extractive industries.
Bi- and Cross-directionality
Bidirectionality was emphasized during the visits to Cuba, exchanging unique and honest perspectives between the originator and destination sites. However, between and after trips, Cuban community members and organizations were not involved in program adaptations in large part because travel from Cuba to the U.S. was very restricted. Instead of bidirectional collaboration on program implementation, the network worked to intentionally deepen collaboration across the eleven CPHE communities in the U.S., which all shared the experience of visiting Cuba. Because the originator site was restricted due to existing policies, the CPHE communities relied heavily on each other and continue to collaborate with a focus on youth leadership and environmental justice.
From Across the World to Ohio: Social Participation in Health
How the project started
The Athens City County Health Department (ACCHD) was invited to apply for an international exchange in social participation in health, facilitated by the Training and Research Support Centre (TARSC). The Training and Research Support Centre (TARSC) provides training and research support to state, national, and international organizations and with the public sector on participatory research methods, monitoring and evaluation, particularly in policy analysis, public health, and health systems. TARSC works closely with EQUINET, a professional network in East and Southern Africa to promote social justice in health. Five U.S. sites and 12 international sites were selected based on their interest and ability to apply various aspects of social participation in their own communities. Athens City was particularly interested because they were starting a CHW program to address chronic diseases and hoped to learn about how other countries recruited CHWs, how CHWs interfaced with the health care systems, and what types of training and funding platforms were used for CHWs. The initiative was supported by a Charities Aid Foundation of America from the RWJF Donor-advised Fund.
Global concept implemented in the US
The ACCHD and its local partners incorporated the broad concept of social participation in health. This framework includes adopting standards for community engagement; participatory budgeting; CHWs as advocates; laws and policy that require health systems to participate in shared decision making in health policy and service development; and creating social accountability processes.
Health equity focus
The ACCHD established a CHW workforce in Athens County to address social determinants leading to high-risk diabetes, such as health literacy, access to care gaps, isolation, and resources for daily living among Medicare and Medicaid populations. The program promotes social participation by empowering CHWs as advocates for their community and ensuring just and equitable distribution of power with (as opposed to power over) community partners. At the system level, these strategies to foster shared power in realms of policy, decision-making, finances, and service delivery advanced health equity.
Evaluation
The program evaluated health system- and patient-level outcomes. Outcomes measured access to care and analyzed health policies and practices with a health equity lens toward greater accessibility of services and shared decision-making. Patients' outcomes included health care utilization (e.g., hospital and emergency room visits), patient health (e.g., a 3.4% average reduction in A1c levels), and patient engagement (e.g., levels of trust and belief that community members are feeling heard). System-level changes were measured by new referral systems for social determinants of health and CHWs as part of the health care team; infrastructure/platform for exchange on health; and policy change/recommendations regarding access to health resources and inclusion. In addition, economic outcomes (e.g., return on investment) and operational metrics (e.g., CHW reach, sustainability, and program acceptability) were also examined.
Bi- and Cross-directionality
The program drew from a broad global concept of social participation in health, so a specific originator site was not involved. This concept is one that authentic engagement with communities through a CHW model have the potential to empower and lift communities toward health equity. In addition, among the different international sites, there is an emphasis on shared learning and collaboration including the development of implementers’ resources to evaluate community engagement.
Key Findings
Community context matters
The five global learning destination sites had diverse community contexts. Baltimore, the Bronx, and Detroit geographically represent urban environments with common legacies of racism and discriminatory health policies and practices, including racial segregation, redlining, and disinvestment. These experiences have culminated in generational communities of poverty and inequitable distribution of services and resources, which are drivers to exacerbated health disparities in health and health care, particularly for people of color in all three locales. Athens and Navajo Nation represent rural communities with limited resources and their own health equity challenges such as long distances for residents to access grocery stores and health facilities. Despite these contextual challenges, a commonality was the cognizance of each place’s socio-political context and how their structural determinants of health have been shaped by history and structural racism. In the U.S. one of the primary determinants of health is where you live. Just as important, another key finding was the emphasis on strengths and assets inherent in each community. In Baltimore, for example, survey respondents pointed to the great network of community organizations, outreach workers, advocates, and policy makers committed to health equity. In Athens, Ohio the geographic context was itself presented as a strength: “Because we live in a rural community, we have an advantage in that we don’t have competing resources. We need to work together [as community partners].”
Originator sites and their relationship with U.S. destination sites also varied widely. For instance, the ACCHD focused on the overall concept of community engagement being implemented by global partners rather than a specific program from specific country or site. In some cases, there were multiple originator sites in a country which reflects national dissemination of a particular innovation, e.g., CHWs in Togo. Community engagement – as a right for all members of a community to have a voice in decision making and to be consulted, informed, and empowered – is beginning to gain traction in U.S. health systems 6 and has been a common strategy in many global resource-limited settings.28–30 Navajo Nation drew from the experiential learning of multiple visits to Cuba without a pre-meditated program goal in mind. Other U.S. teams specifically reached out to global programs that aligned with their local needs and, in some cases, built bilateral corridors of learning with those international sites. Among the different sites, the Baltimore project provided an example of deep bidirectional learning, in which the Brazil team gained additional insight into the core components and adaptation process for its own intervention. What was common across these examples, however, was the perception that each U.S. site shared important similarities with their originator sites. In highlighting the shared context for global learning to take place, respondents revealed the importance of those contextual facilitators to their decision-making and evaluation efforts across all stages of their projects. 31
Community engagement strategies
Engaging communities was crucial for global learning interventions to appropriately address community needs and improve health equity. The equitable and meaningful involvement of community partners toward the transfer of decision-making power was also highlighted as a core component of the process, e.g., the importance of relationships and collaboration, trust building, shared decision making, and influencing changes in policies and practices. To this end, there are different examples of how this was accomplished.
Across the five destination sites, engagement strategies primarily relied on regular face-to-face, phone, and virtual meetings, as well as interviews, surveys, public events, stakeholder forums, patient advisory boards, presentations, flyers, word of mouth, providing literature, and outreach via email and social media.
Highlighting strengths-based approaches was another common community engagement strategy to achieve and evaluate outcomes at the systems level. For instance, all five programs emphasized shared decision making through CHW engagement and community capacity building. They also leveraged community assets, social networks, and trusted community relationships to improve health outcomes. UMB focused on specific psychosocial measures such as a sense of belonging, hope, social networks, and the ability to “activate” individual strengths to achieve key chronic health and wellbeing goals (such as diabetes and hypertension management). This proved important to ensuring inclusion, program sustainability and ownership, and health equity advancement.
While for ACCHD, “community engagement is an expectation for public health accreditation,” all five sites demonstrated commitment to authentic community engagement. It is important to recognize the policy implications of “community engagement as an expectation for public health accreditation” for the ACCHD. This accreditation requirement demonstrates how policies can ensure implementation and sustainability of community partnerships and engagement toward health equity.
Montefiore also leveraged the “shared lived experience of patients [and CHWs who] are experts in their community.” This is critical to building trust and ensuring that communities are willing to participate, feel a part of the process, and engage in programs or services offered, particularly by academic health care systems which, in many settings, have a history of distrust in the community.
The participating university “engaged the community pre-implementation and community members helped co-create content” for the intervention. UMB also hired community members as outreach workers and program managers to implement the intervention further demonstrating how to build on and catalyze community assets. Navajo Nation engaged trusted tribal leaders both at the local level as well as higher-level Navajo Nation delegates including the Vice President and Four Corners leaders over a period of six to 9 months to plan the launch of their Community Partnerships for Health Equity (CPHE) program. Athens City-County likewise identified and hired CHWs who were recommended by community leaders and/or were from the communities in which they lived and served. Engagement not only meant including community leaders and members but also shifting decision making and ownership of programmatic implementation to begin to address internalized oppression.
All programs highlighted the importance of partnering with communities that have systematically been excluded from resources and decision-making power. Each program describes different methods of outreach to engage with communities, such as employing CHWs, working with influential community leaders, leveraging existing networks and members of the community as “experts” in their own health and health care. A measure of shared power and decision making demonstrates a shift in transferring power traditionally given to the health care system and is essential to sustainable community development, empowerment, and well-being toward health equity.
For some sites, the community was initially reluctant to implement global learning. In Baltimore, overcoming this reluctance required holding additional in-person meetings with local stakeholders to share information. The project leaders found that both sharing evidence of the success of the originator program in Brazil, as well as making clear the commonalities between the Baltimore and Rio de Janeiro communities helped convince the community to participate. Both cities have severe social inequities, pockets of extreme poverty and consequent violations of human rights and dignity. A key community engagement strategy is for destination sites to facilitate their local community partners in seeing themselves reflected in the originator site. In Detroit, limited participation of the residents of the senior apartment building selected for the Knock & Check intervention necessitated hosting weekly “Coffee & Conversation” hours for the community health workers to share information and engage residents in a group setting. Global learning projects with detailed methodologies such as the Family Action Plan and Knock & Check that require a higher fidelity to adoption versus adaptation may require additional community buy-in.
By comparison, results from the surveys indicate that broader CHW models and principles deployed in Athens City-County, Ohio and the Bronx or the overall Cuban health paradigm adopted in Navajo Nation were more acceptable for destination communities to envision adapting to their local context, thus facilitating an easier uptake and acceptance.
Navajo Nation project leaders shared that MEDICC’s CPHE “community of practice” model enabled community participants to not only travel to Cuba to see the originator model first-hand, but it also connected these community members with 11 peer communities around the country who engaged in similar global learning. The global to local learning (Cuba to Navajo Nation) was reinforced by the local-to-local learning (for example, Bronx to Navajo Nation) occurring as the community partners participated in MEDICC’s U.S. network of global learners.
Both the Athens and Detroit sites shared that while the project staff were involved with respective originators from global sites, the global learning aspects of the interventions were not consistently communicated to participating community members. In Detroit, by the time the program was rolled out, it had been so extensively adapted that it was no longer recognizable as the original UK model. In Athens, the structure of the exchange was different from other participating sites in that global learning was focused on the concept of social participation in health rather than adapting a specific program.
Each project had an individual or organizational champion that enabled community buy-in and community support. When asked what facilitated program implementation, the project leader in Athens discussed the health department’s commitment to community partnership and identifying gaps in health and the advantages of a tight-knit rural community, but concluded by stating, “But, honestly, I just think my administrator trusts me.” In Detroit, having executive level sponsorship of the pilot program, along with buy-in from members of the U.S. Congress and the U.S. Postal Service innovation headquarters in Washington, DC, all helped to facilitate Knock & Check’s adaptation progress. The engagement process overall can thus unfold differently depending on the historical and current context, the relationships between the originator and destination sites, and the understanding of relevance of global health concepts, paradigms, health systems, or programs.
Implementation Science approach
Measuring adaptations and assessing barriers and facilitators using an implementation science approach was identified as a key component by the Global Learning for Health Equity Network of the draft global learning framework. The utility of using implementation science methods is applying rigorous assessment to real-world implementation with a focus on understanding not only whether an evidence-based intervention was effective in a distinct context, but the reasons “why” it was effective or not effective. It is this data, “the why”, that is likely critical to Global Learning activities, because implementation of evidence-based interventions (EBI) in new contexts are usually optimized when adapted to address contextual factors while maintaining the core components of the EBI31. Core components of an EBI are the characteristics or program elements that should not be modified when being replicated or adapted in a new context, to promote impact tantamount to those demonstrated in the original setting.
Each of the site implementers identified core elements that were empirically or theoretically associated with the desired outcome of the original program. In the Togo to Bronx program, core elements included ensuring CHWs were from the community where the intervention occurred, and that roles and methods were standardized across recruitment, training, accreditation, equipment, and supplies activities. In the Baltimore intervention, the implementation team identified several core components including use of the Family Action Plan (FAP) methodology with inclusion of all five components of the FAP (health, education, global citizenship, housing, and income generation). Maintaining intervention dose, touchpoints with families, and clear entry and exit criteria for program participants were also identified as key ingredients in the Baltimore and Brazil sites.
Adaptation involves modifying an intervention to the local environment and is essential to ensure that a program is tailored to distinct contexts. Review of the sites revealed that while ensuring that core elements were maintained, adaptations were made to some components of the intervention (e.g. specific health focus or target population) and important societal and political contexts. For example, adaptations for the Cuba to Navajo Nation exchange involved incorporating local traditions, honoring local leaders, centering heritage and nation in the implementation of the program. Another example is the CHW paradigm that informed interventions in several sites, in which the content/focus area of each CHW program was distinct and adapted to meet the community’s need. For example, the originator CHW program in Brazil focused multiple services, including maternal and child health, to vulnerable families in Rio de Janeiro while Baltimore’s adaptation focused on helping the community navigate social services.
External and internal factors that affect implementation of global learning innovations can become barriers and/or facilitators to the global learning process. Factors are considered as facilitators if their presence promotes effective implementation and barriers if they impede. Depending on the context, the same factor can be both a barrier and a facilitator. Barriers to implementation of global learning projects included challenges with funding and cultural differences. All sites reported funding challenges, one site noted “The program is grant funded and is research, the risk to sustainability is great due to reliance on funding for implementation.” Additionally, many sites utilized CHW models and noted limited reimbursement opportunities and challenges with funding the time needed to optimize the new staff members. Culturally, difficulties were noted with language barriers, cultural differences, and different political, healthcare structure, and social support referral systems.
The five implementation “facilitators” reported by learning community leaders in sites across originator and destination sites in our case study included: (1) having an evidence base for the approach, (2) similarities between the two communities, (3) alignment of values and community engagement approaches, (4) established working relationships and systems, and (5) a dedicated team. Having an evidence base for global interventions enabled facilitators to move forward with global learning. Survey respondents noted “there was completed health data that was evidence for our intervention planning,” and described how the established evidence base allowed for progress and a shift to focus on effective implementation. Establishing an understanding of the similarities between the global and local context also facilitated implementation. For example, one facilitator stated, “making the commonalities among the two communities clearer to partners, helped local partners see the benefits of the global idea/program.” Aligning values and community engagement was important across all sites with one global learning implementer noting, “Our organizational culture is based on values such as sharing, collaboration and partnership. We believe that it was possible to build a close partnership sharing values and principles, as well as information. It was essential for the project’s success.”
Health equity principles and measures
All sites stated that their programs focused on addressing social determinants of health to advance health equity. For instance, Athens used the CHW model to address challenges in transportation, housing and healthy foods and purposefully engaged communities to work together toward improved health. The Baltimore initiative measured how reducing social isolation led to reduced unnecessary hospitalization days and increased employment, home ownership and linkages to government social services. Both initiatives illustrate a direct response to health systems that adapted global practice of extending beyond traditional walls of the system to address the root causes of poor health.
Sites also describe the process of community development as a reflection of health equity. Meaningful and equitable involvement of community partners was viewed as one of the first steps towards transferring power to influence change in policies to ensure and support such collaboration and relationship building. For instance, shared decision making was important for all five global learning sites, yet the locus of agency varied across sites and over time. One factor that influenced the balance of power between champions and local community leaders was the type of institution leading the work and inherent legacy of institutional distrust for many underserved communities in the US. The three projects led by academic hospitals, the decision to pursue a global learning project was instigated by a community member PI (Baltimore) or by senior leadership (Bronx, Detroit). Once the decision was made, the academic project leader identified a global model and obtained community buy-in. Finding the right community partners and getting buy-in took time perhaps because not all stakeholders were initially vested. Knock-and-Check in Detroit could not engage the US Postal Service and instead opted for deploy CHWs and in Baltimore, local buy-in took time and resources to build trust, requiring in-person meetings to share information about Saude Crianza until community partners appreciated the relationships and commonalities of these two very different places. In these scenarios, building on existing networks and applying traditional academic models of communication and engagement proved to be effective.
In the other projects, a community-based organization (Navajo) and a public health department (Athens City) were invited to participate in global learning exchanges, and local community partners were consulted in the decision to participate through formal or informal community coalitions. For example, Athens City leveraged existing relationships with Health Committees as active members of the planning, execution, and evaluation of the program. The city initiative had already established trusted relationships, giving agency to local partners to make decisions, own the process, be invested in its outcomes, and foster sustainability. Regardless of the initial engagement process, all sites incorporated community input, including advisory groups, co-creation of programs and evaluation, and shared implementation roles. While all projects initially relied on a leader, almost all sites described how leadership was diffused to additional champions either within their lead institution (e.g., other medical providers) or in community partners (e.g., local champions, CHWs).
For instance, the Athens City team observed that international practices and policies of community engagement, social participation in health and overall civic involvement were often activated from, grounded in, and established from a fight for rights (“nothing about us, without us”). This historical need to fight for basic human rights – such as healthcare and formal social participation in local budgeting – has resulted in a vested interest by community stakeholders to acquire and maintain a place at the table. In contrast, U.S. political and healthcare structures are often structured in ways that exclude social participation and therefore require time to build trust and cultivate a vested interest in global learning projects among community partners. This is level of involvement and ownership is critical for the sustainability of the programs and long-term improvement in health.
In terms of assessing program impacts on health equity, there were varying degrees of formal evaluation of health equity outcomes. All sites identified process measures related to health equity. These included core principles of community engagement, community ownership, and trust building as critical process metrics to program implementation. For instance, the Bronx and Detroit programs emphasized the balance between health systems and community partners, with shared decision making through community report-backs and patient inclusion.
In addition to process measures, some sites also tracked implementation outcome measures associated with health equity. Health equity outcomes often reflected the core components that were adopted through global learning, such as measurements of social connectedness, engagement with and access to resources, and the development of policies to combat the structural root causes of ill health and inequities. None of the sites appeared to have a comparative effectiveness assessment, but several involved changes over time (both for individual and system-level outcomes) as well as implementation science measures, as described above.
Discussion
Five global learning projects were characterized using a CFIR implementation approach. This allowed the authors to explore differences and similarities of sites with respect to community context, the learning and implementation process, implementation science considerations, and health equity. The findings of this case study informed the development of a GL4HE framework (See Figure 1), a tool designed to guide and support the development and implementation of future global learning initiatives. The framework draws from these case studies, from a literature review 15 and stakeholder feedback from multiple seminars and conferences.32–34 As depicted in Figure 1, the global learning for health equity framework represents the “life cycle” of global learning collaboratives, core values of trust, respect, reciprocity, and humility, while providing specific guidance at each stage from exploration to implementation and measuring impact.
The case studies underscore the broad and heterogenous nature of global learning
Global learning is grounded in solidarity
All five U.S. sites linked health disparities experienced by their communities with broader economic and socio-contextual disparities, and thus found common ground with similar challenges faced by originator sites. Given the diverse community contexts of the five global learning destination sites, we conclude that global learning can be done anywhere by a group of community-engaged, health equity promoters. Despite the survey’s small sample size, the process of global learning across five core phases – exploration, pre-implementation, implementation, evaluation, and dissemination – does not appear to be dependent on specific community characteristics or areas of focus. Perhaps unsurprisingly, the “common ground” shared by all five sites is the acknowledgement of significant economic and socio-contextual disparities that have created persistent health equity challenges. Understanding the community’s socio-political context contributing to health disparities, along with its priorities, strengths, and assets is foundational to informing any global learning process.
Community engagement and ownership is core to the implementation process and goal of health equity
A wide variety of engagement strategies were used in these global learning projects. For instance, early communication of global learning elements with participating community members helped to gain buy-in, particularly sharing evidence associated with the originator program and the commonalities between originator and destination sites. Community involvement continued throughout the implementation process and was felt to contribute to outcomes at the individual (e.g., reduced social isolation) and community (stronger community partnerships with institutions such as academic centers and health departments) levels. All sites emphasized the importance of gaining community trust and respect, often facilitated by global learning project champions. The most successful projects were those that worked within the existing systems to change or dismantle the existing infrastructure of oppression and one-sided power dynamics. Unless these underlying causes of poor health and imbalance of authority, equity cannot be achieved.
We also recognize limitations of our study. For one, in that the key informants who completed the survey were project leaders, often affiliated with institutions of power. Though some respondents belonged to the communities served, the survey did not explicitly collect perspectives from community members with lived experience of the programs described.
We recommend that global learners interested in health equity incorporate community engagement at all stages of their projects (from design to evaluation) and continually assess how decision-making power can be placed in the hands of community partners and/or those most impacted by the inequity one is attempting to change. Our case study also highlights the need to understand power dynamics in origination and destination sites to avoid unintentionally perpetuating inequities.
It is notable that CHWs were central to programs in three of the five sites, including one site (Detroit) which adapted the original model to include CHWs rather than post office workers. Despite decades of robust evidence on CHW effectiveness and cost-effectiveness in the United States35,36 and national endorsements of CHW programs37,38, the U.S. lags behind other countries in mainstreaming CHWs into healthcare systems In part due to challenges in standardizing the CHW profession, integrating CHWs into healthcare teams and systems, and maintaining sustainable funding.39,40 These tensions however are not unique to the U.S. and highlight the importance of pursue bi-directional learning from global communities to influence and drive sustainable large-scale CHW programs to advance health equity41,42.
Implementation science methods are well-suited to explore the distinction and commonalities in global learning initiatives
Adaption was a key element that involved retaining core elements of the interventions, while making changes to respond to distinct contextual factors. Other key implementation science constructs included identifying key determinants to implementation, barriers and enabling factors. Despite differences in context and interventions, we found similarities across the learning teams in terms of key enabling factors and barriers that suggest there may be some generalizable guidance around effective global learning. We recommend that future research among global health learners consider applying an implementation science framework to deepen our understanding of how global concepts and practices are successfully applied in the U.S. to achieve health equity. Further validation of the Framework presented will continue to enable U.S. practitioners to adapt and adopt global solutions to local inequities.
Conclusion
Global learning can eliminate widening health disparities by addressing social determinants of health and other community level root causes of ill-health and community well-being. The learning communities in this case study highlight the importance of trust building for community engagement; consideration of community context, organizational culture, and infrastructure; and the identification of the essential facilitators for implementation. Solutions ranged from CHW models to broader strategies of participatory budgeting and requires broad cross-sector collaborations, including community-based organizations, academic partners, healthcare institutions and community advocates. This study advances the field of global learning by synthesizing factors essential to the implementation of global solutions and offers an important and novel GL4HE Framework from which U.S. communities and health equity promoters may scale and adapt lessons from abroad to improve health and advance health equity.
Supplemental Material
Supplemental Material - Global Learning for Health Equity: A Survey of Five Global Learning Sites in the United States
Supplemental Material for Global Learning for Health Equity: A Survey of Five Global Learning Sites in the United States by Sonya S. Shin, Ami Shah, Janette North-Kabore, Virginia Rowthorn, Kevin Fiori, Ruth Dudding, Rev Alexander Plum, Dana Parke, Carmen George, Stephen Thomas, Randal Pinkett, Keshia Pollack Porter, Adam Sirois, Vera Cordeiro and Yolanda Ogbolu in Community Health Equity Research & Policy.
Footnotes
Acknowledgements
We thank Krista Brooks for her administrative support.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is supported by Robert Wood Johnson Foundation (77717).
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
