Abstract
Background:
Excessive gingival display, or “gummy smile,” occurs in up to 14% of adults and is associated with lip hyperactivity, dentoalveolar extrusion, or vertical maxillary excess. Botulinum toxin A (BTA) has emerged as a minimally invasive therapeutic option, but protocols vary widely and long-term data are limited.
Objectives:
To critically evaluate the current literature on BTA in gummy smile management, focusing on classification systems, injection techniques, efficacy, safety, and comparative outcomes against conventional surgical and orthodontic treatments.
Methods:
A narrative review was performed using PubMed, MEDLINE, and Scopus (2000-2023) with the terms “gummy smile,” “excessive gingival display,” and “botulinum toxin.” Clinical studies, case series, and reviews addressing BTA use were included. Data were synthesized into thematic categories.
Results:
BTA consistently reduced gingival exposure by 3 to 5 mm, with effects lasting 4 to 6 months. Three main injection strategies were identified: single-point (Yonsei), multi-point, and orbicularis oris (“lip flip”). Reported complications were rare and transient (mild asymmetry, lip weakness). Standardized protocols were lacking, with heterogeneity in dosing (2-5 units per site) and injection depth. Comparative studies suggested BTA is less durable than surgical approaches but offers superior patient acceptability and safety for mild to moderate cases.
Conclusion:
BTA provides reproducible, temporary improvement in gummy smiles with high safety and satisfaction rates. However, absence of consensus on optimal technique and limited long-term evidence highlight the need for standardized protocols and prospective multicenter studies.
Introduction
Gummy smiles, also termed excessive gingival display, afflict 14% of women and 7% of men 1 and can negatively impact patient self-esteem. 2 They can be defined as the appearance of excessive gingival tissue between the upper lip and the gingivodental margin during full smiling. 3 Although the notion of excess varies between authors, ranging from 1 4 to 4 mm, 5 a gingival display of 2 to 3 mm is generally considered to be esthetically unpleasing.3,6-9
Gummy smiles may originate from skeletal (eg, vertical maxillary excess), muscular (eg, hyperactive labial elevator muscles), gingival (eg, gingival hyperplasia), dental (eg, delayed passive dental eruption), and labial (eg, short lip length) etiologies. 5
Conventional treatment includes orthognathic (eg, Lefort osteotomy), orthodontic, muscular (eg, lip repositioning), and gingival (ie, crown lengthening, gingival recontouring) interventions. 10 Expectedly, the more invasive procedures often entail significant cost and time investment. 11 In recent years, botulinum toxin A (BTA) has been increasingly used to manage gummy smiles. 5 Recent preliminary evidence suggests that BTA may be more effective than its surgical counterpart (ie, lip repositioning surgery). 12 Interestingly, even when it is less successful than alternative options (eg, laser gingivectomy, orthognathic surgery), patients may still prefer BTA because of its lower cost and non-invasive nature. 13 Furthermore, BTA has been reported to be a simple but effective adjunct to surgery in complex and refractory cases.14-16 In light of its simplicity and versatility, BTA has become a cornerstone in managing gummy smiles for cosmetic physicians, surgeons, and dentists.9,17
In this narrative review article, we discuss the muscles involved in upper lip elevation, the classification of smiles and gummy smiles, and the different techniques and comparisons between techniques for BTA. Furthermore, we identify areas requiring future investigation.
Methods
A structured literature review was conducted in PubMed/MEDLINE and Scopus for articles published from January 1, 2000 to March 31, 2023 using combinations of the terms “gummy smile,” “excessive gingival display,” and “botulinum toxin.” The search strategy was adapted to each database and limited to human studies. Records were exported to a reference manager and duplicates removed.
Two reviewers independently screened titles/abstracts, followed by full-text review. Inclusion criteria were peer-reviewed clinical studies (randomized trials, prospective/retrospective cohort studies, case series) and review articles describing botulinum toxin A use for excessive gingival display, including injection targets and/or outcomes. Exclusion criteria were editorials, letters, conference abstracts without sufficient clinical detail, non-English articles, and studies not reporting gummy-smile outcomes. A total of 51 articles met inclusion criteria and were synthesized qualitatively.
Data extraction included gummy-smile classification and severity, toxin formulation and dose, injection sites/technique, follow-up duration, outcome measures (mm gingival display reduction and/or photographic analysis), complications, and patient satisfaction. Discrepancies were resolved by consensus.
Results
Fifty-one articles were included after full-text review. Across clinical studies, botulinum toxin A consistently reduced gingival display, with the most pronounced effect observed at approximately 2 weeks post-injection, followed by a gradual decline in effect thereafter.23,24,26-28,31 However, there was substantial heterogeneity in classification systems, injection landmarks, toxin formulation and dosing, outcome measurement methods, and follow-up duration, limiting direct comparison and preventing the establishment of a single standardized protocol.17,19,25
Anatomical Targets and Rationale
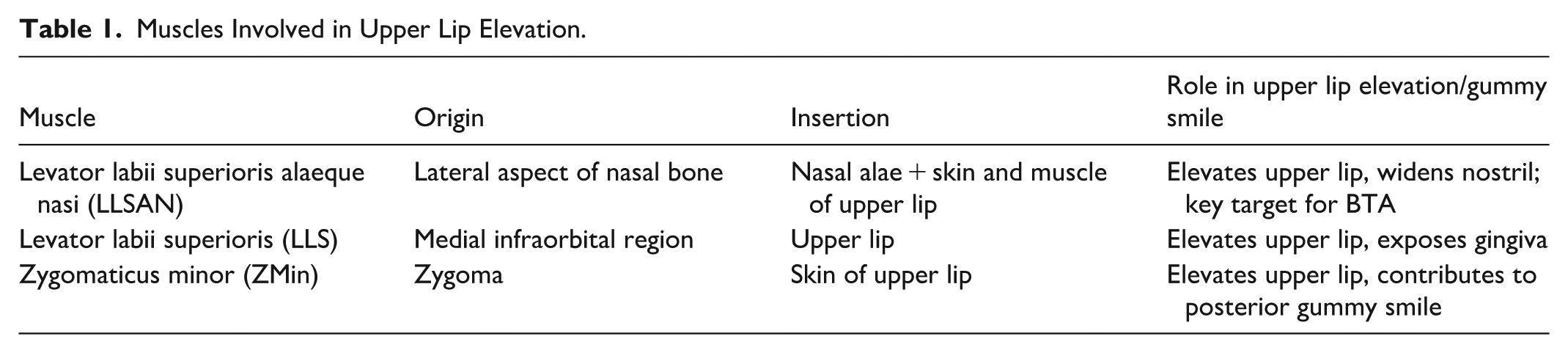
Among the facial muscles involved in upper lip elevation, 3 were consistently identified as primary targets for gummy-smile reduction: the levator labii superioris alaeque nasi (LLSAN), levator labii superioris (LLS), and zygomaticus minor (ZMin; Table 1).18,19 Most injection strategies aimed to weaken one or more of these muscles to reduce upper lip elevation during smiling, with target selection guided by the anatomic distribution of gingival exposure and facial symmetry.17,19
Muscles Involved in Upper Lip Elevation.
Classification Systems Used for Injection Planning
Multiple classification systems for gummy smile were described in the literature.1,3,17,20-22 Location-based classifications were most clinically useful for injection planning, as they correlate patterns of gingival exposure with likely muscular contributors. The classification proposed by Mazzuco and Hexsel was frequently referenced in adult patients and categorizes gummy smiles into 4 types: anterior (type 1), posterior (type 2), mixed (type 3), and asymmetric (type 4). Asymmetric presentations were noted to often require differential dosing between hemifaces (Figure 1 and Table 2). 17
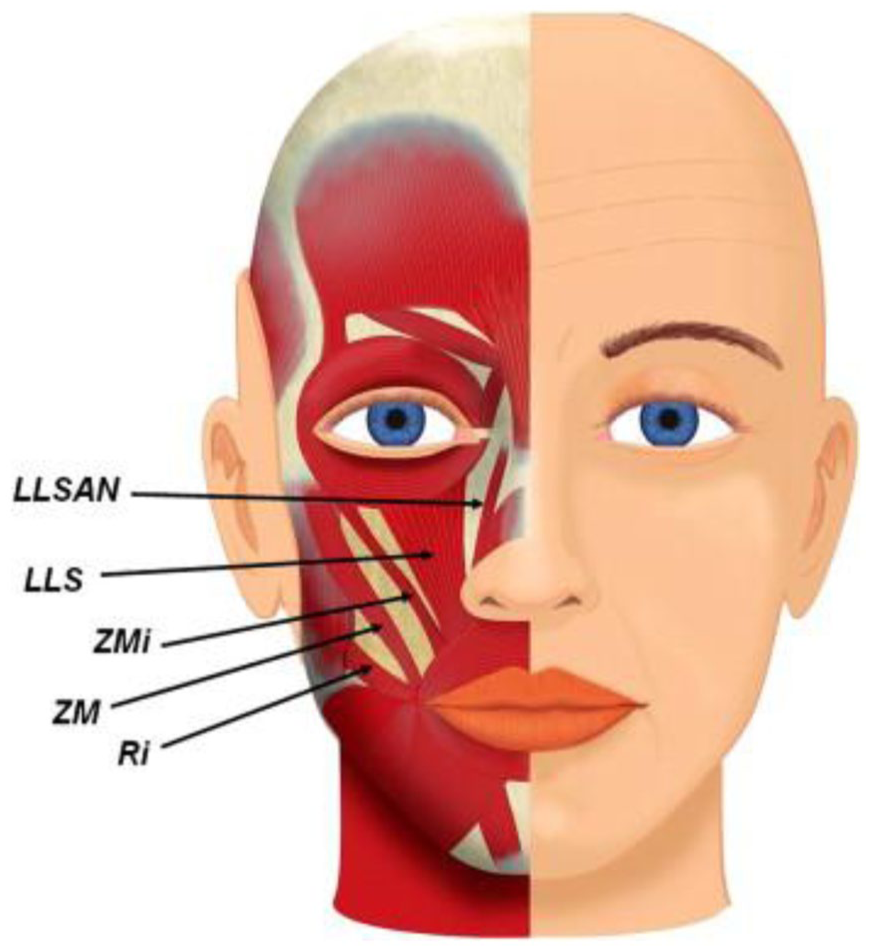
Main muscles involved in gingival exposure. 17
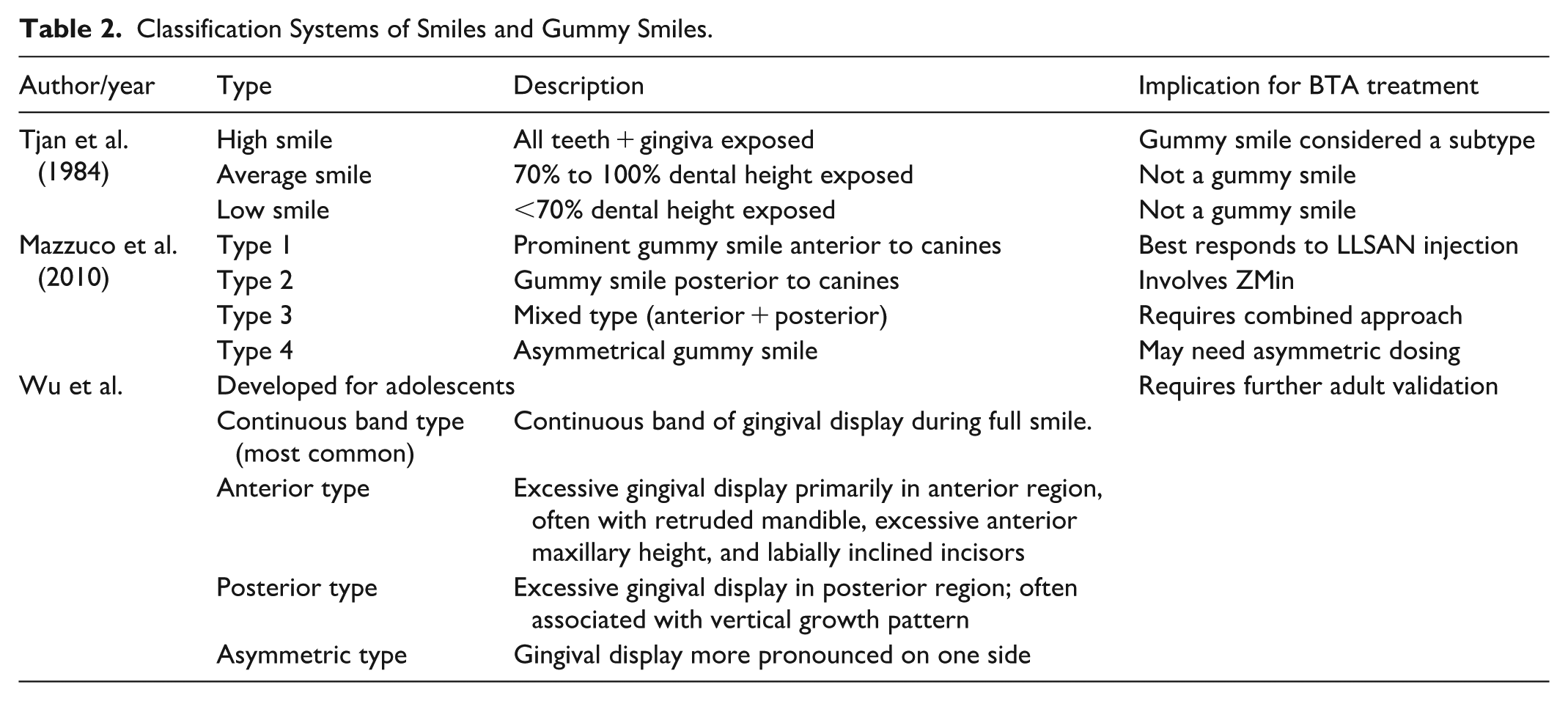
Classification Systems of Smiles and Gummy Smiles.
Injection Techniques
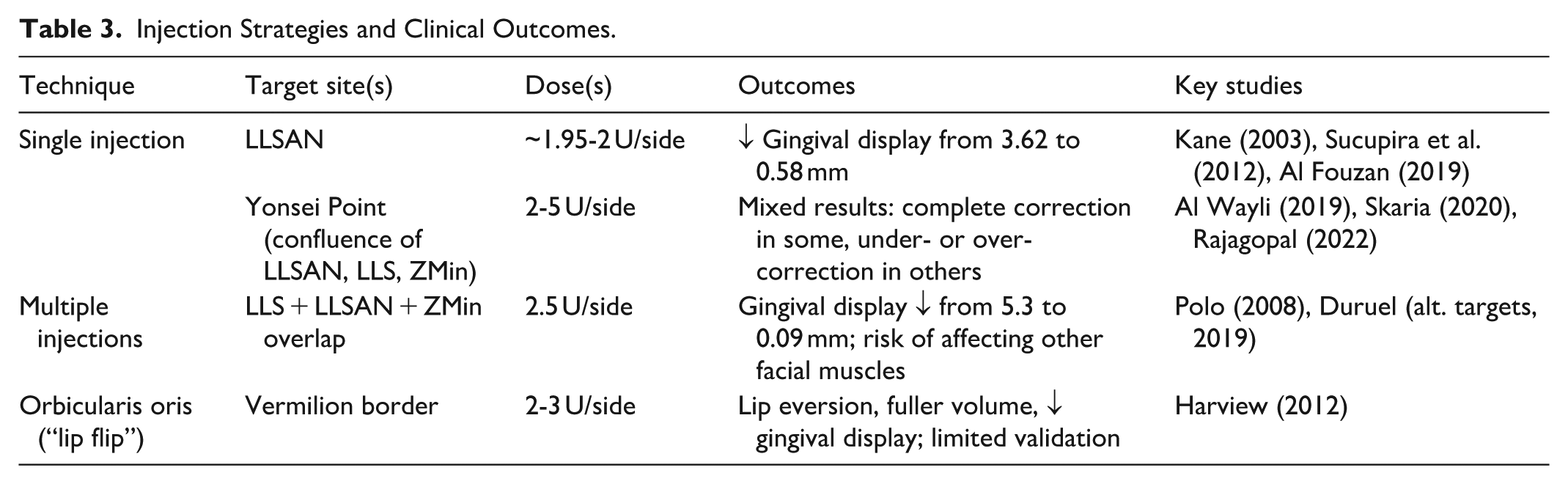
Three families of injection techniques were identified (Table 3).
Injection Strategies and Clinical Outcomes.
Single-point Techniques
Several studies targeted the LLSAN using low-unit dosing per side and reported meaningful early reductions in gingival display at approximately 2 weeks post-treatment.23,24 Another commonly described single-point approach involved injection at the Yonsei point, a surface landmark intended to affect the confluence of the LLSAN, LLS, and ZMin (Figure 2). 25 Outcomes with Yonsei point injection varied across studies. Al Wayli 26 reported complete coverage of the gingivodental margin using 2 to 3 U per hemiface, whereas Skaria et al 27 observed statistically significant but incomplete correction. Variability was attributed to anatomical differences in muscle convergence and injection depth, as demonstrated in cadaveric studies by Hwang et al. 25 More recent longitudinal data further illustrated dose-dependent differences in correction based on baseline severity. 9
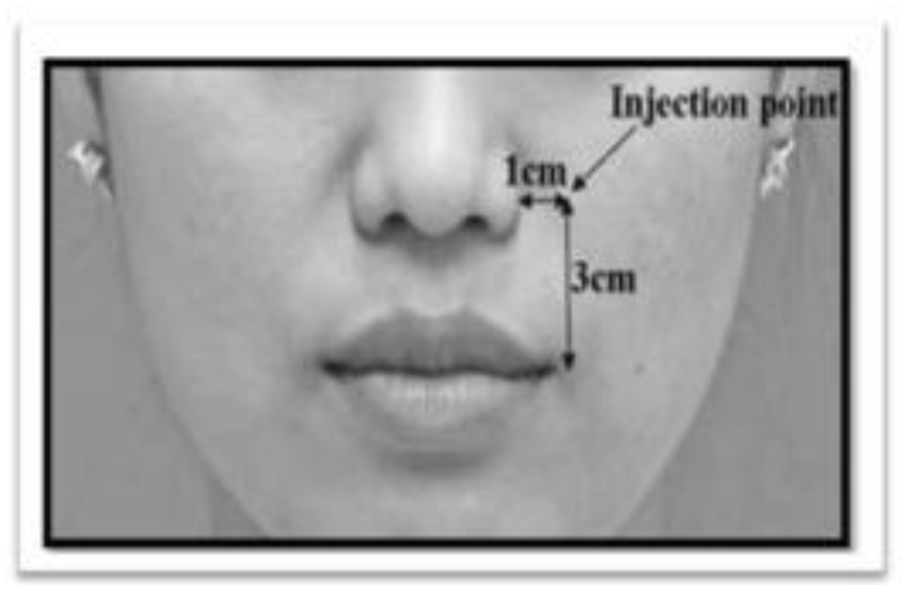
The location of Yonsei point. 9
Multi-point Techniques
Multi-point injection strategies, most notably those described by Polo, involved bilateral toxin deposition at overlap regions between the LLS and LLSAN and between the LLS and ZMin.19,28 These techniques produced substantial early reductions in gingival display, particularly in patients with more severe baseline exposure. 28 However, in patients with gingival display below 5 mm, overcorrection with descent of the upper lip below the gingivodental margin was reported, supporting the need for severity-based dose adjustment (Figure 3). 28 Alternative multi-point targets have been proposed more recently, though validation remains limited. 29
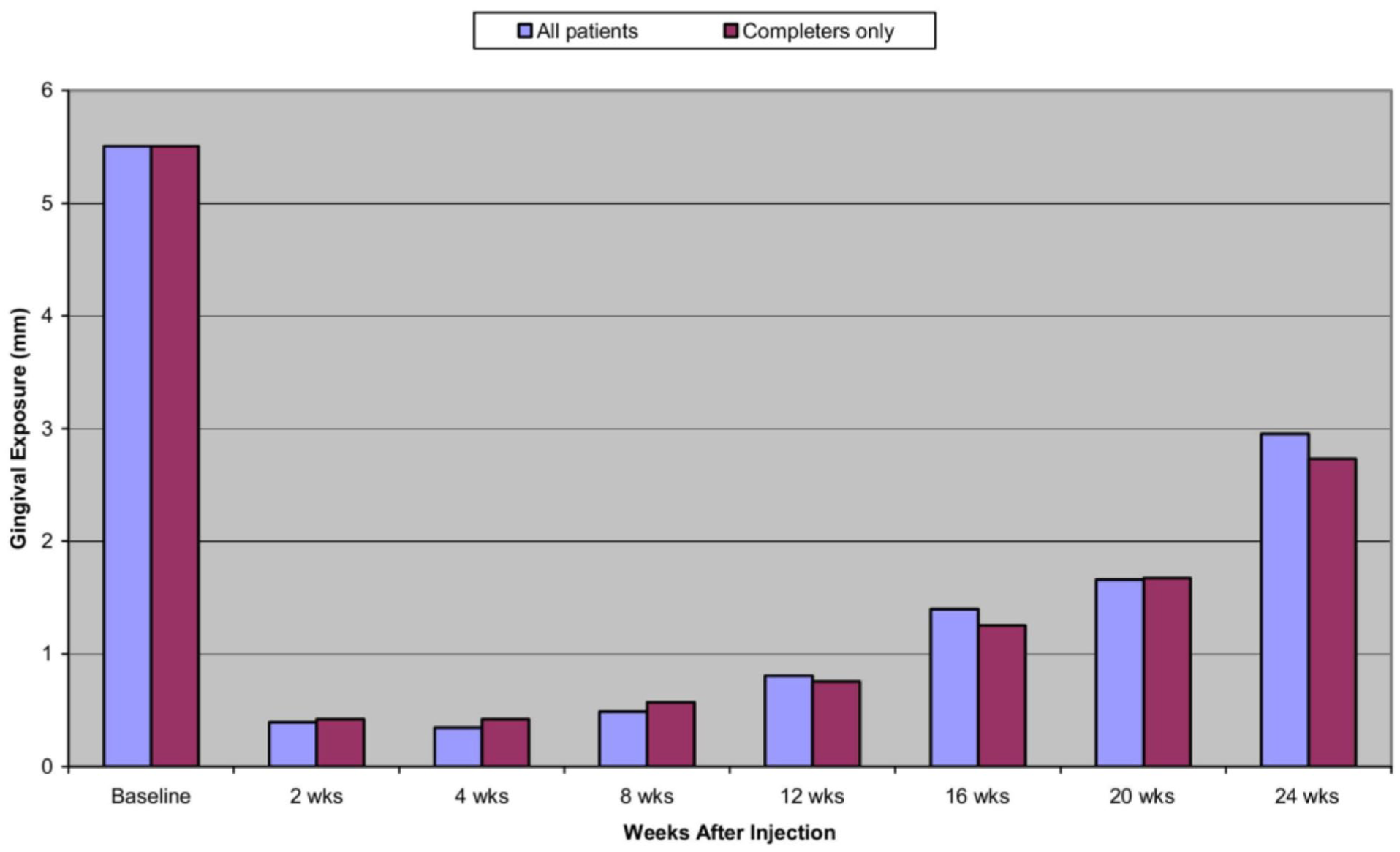
Gingival exposure before and after treatment with multiple injection technique BTX-A in all subjects. 28
Orbicularis Oris (“Lip Flip”)
Injection of small doses of botulinum toxin A (2-3 U per hemiface) into the marginal portion of the orbicularis oris muscle at the vermilion border was described as producing lip eversion, smoother perioral rhytides, and a secondary reduction in gingival display. 30 Evidence supporting this technique for gummy-smile correction remains limited, and outcomes were less consistently reported compared with approaches targeting the upper lip elevator muscles. 30
Magnitude and Durability of Effect
Across studies, maximal improvement in gingival display was generally observed around 2 weeks following injection.23,24,26-28 Clinically meaningful reduction was reported to persist for approximately 4 to 6 months, depending on technique, dose, and baseline severity. 31 Longitudinal analyses demonstrated gradual return toward baseline by 6 months, confirming the temporary nature of treatment. 31
Safety and Complications
Adverse effects were infrequently reported and were generally mild and transient, including temporary asymmetry, lip weakness, or altered facial expression.19,28,30 Considerable variability in dosing strategies, injection depth, and patient selection limited the ability to derive pooled complication rates across studies. 25
Long-Term Outcomes of BTA Treatment for Gummy Smiles
One significant study conducted by Zengiski et al, 31 which examined research findings provided insights on this topic. Their findings reveal that while BTA effectively reduces gum exposure, it is mostly temporary. 31 The greatest improvement is typically seen within the 2 weeks after treatment. These results gradually diminish and return to their original state after about 6 months. 31 Therefore, patients who wish to maintain the benefits of BTA treatment for gummy smiles may need to consider getting re-injections every 6 months. 31
Similarly, Fatani’s review supports this understanding. It emphasizes the speedy action of BTA 32 and mentions that the treatment’s impact lasts between 4 and 6 months. 32 Hence, individuals seeking long-term solutions should consider this time frame and the treatment requirements.
These insights are crucial in establishing expectations for patients and healthcare providers regarding how BTA effectively treats gummy smiles. Although BTA can be effective, its advantages are not long-lasting and need upkeep.
Across many clinical studies analyzing techniques to treat the gummy smile and achieve an ideal esthetic smile, the standard method is injecting botulinum toxin type A (botox) at the levator labii superioris alaeque nasi, a muscle of facial expression that widens the nostril and elevates the upper lip, and levator labii superioris, whose primary function is the elevation of the upper lip.18,19 These muscles contribute to excessive gingival display. In a clinical pilot study to examine the effectiveness of botulinum toxin A as a treatment for the gummy smile, 19 during Phase 1 of the treatment, 1.25 U per side was injected in both the right and left levator labii superioris and levator labii superioris alaeque nasi muscles. All 5 patients began to show improvement approximately 10 days after the injections. 19
Treatments of the gummy smile aim to reduce the number of injection sites and do not always follow the standard treatment. As mentioned before, clinical study to find an injection point for botulinum toxin-A utilized 3 lip elevator muscles. 25 A triangle was constructed by connecting the landmark’s Lateral point of the ala, the Midpoints of the nasolabial fold between the ala and commissure and the Maxillary point at a one-quarter distance between the ala and tragus on each side. 25 At the center of the triangle is the Yonsei point, and because of the overlap of the circles from each of the 3 landmarks, 1 single injection site of botulinum toxin type A should affect all 3 muscles.
There is controversy; it is not always required even to use botulinum toxin-A injections to treat gummy smiles. Instead of determining the use of diagnostic and therapeutic approaches, a case study determined that it was necessary to reduce maxillary protrusion through orthodontic treatments, such as temporary anchorage devices or crown lengthening procedures, with no injections involved. 40 Nonetheless, despite the treatment method, all studies showed some positive improvement in their patients.
Approach to Injections
The standard approach utilized to inject botulinum toxin was a 25 to 30 gage needle with an accompanying tip. A clinical report that presents the satisfying and unsatisfying treatment of excessive gingival display by targeting Yonsei Points and Zygomatic Major Muscles used a 50-unit insulin syringe with a 30-gage needle to inject onabotulinum toxin A. 23 Additionally, local anesthesia with ice was used to provide comfort during the procedure. Similarly, in a vivo clinical study 24 to evaluate the effect of botulinum toxin injections as a conservative treatment for a gummy smile, in addition to a 30-gage needle, extra precautions were taken to ensure the safety of the patient, including topical anesthesia gel and an alcohol swab saturated with 70% isopropyl alcohol used at the injection site to sterilize it. The mean percentage of improvement in the gingival display was 99.6% (a significant decrease in the amount of gingival display). 24
However, neither of these studies used advanced imaging technologies, as botulinum toxin injections are usually based solely on the surface anatomy of the face. A pictorial essay and narrative review by the authors in 18 used high-resolution ultrasound imaging using a hockey-stick transducer to facilitate needle insertions and make them more accurate. High-resolution ultrasound imaging can identify asymmetry of the face, so the botulinum toxin A treatments can be personalized, and risk can be further reduced. The study concluded that further gummy smile treatments should explore the benefits of ultrasound imaging.
Based on the reviews of these papers,18,23,24 high-resolution ultrasound imaging and anesthetics can improve the quality of the treatment of a simple gage needle. The importance of high-resolution imaging and anesthetics can be highlighted by examining the clinical study 28 that did not report using anesthetics or high-resolution imaging. As a result, while the BTX-A treatment was overall well tolerated, patients reported pain at injection sites, twitching, headaches, and dizziness.
Patient Demographics and Variability
The effectiveness and approach of BTA treatment for gummy smiles can be influenced by a variety of factors, including patient demographics, severity of gingival display, muscle dynamics, medical history, patient expectations, and responses to previous treatments (Table 4).8,33,34
Patient Factors Influencing Treatment.
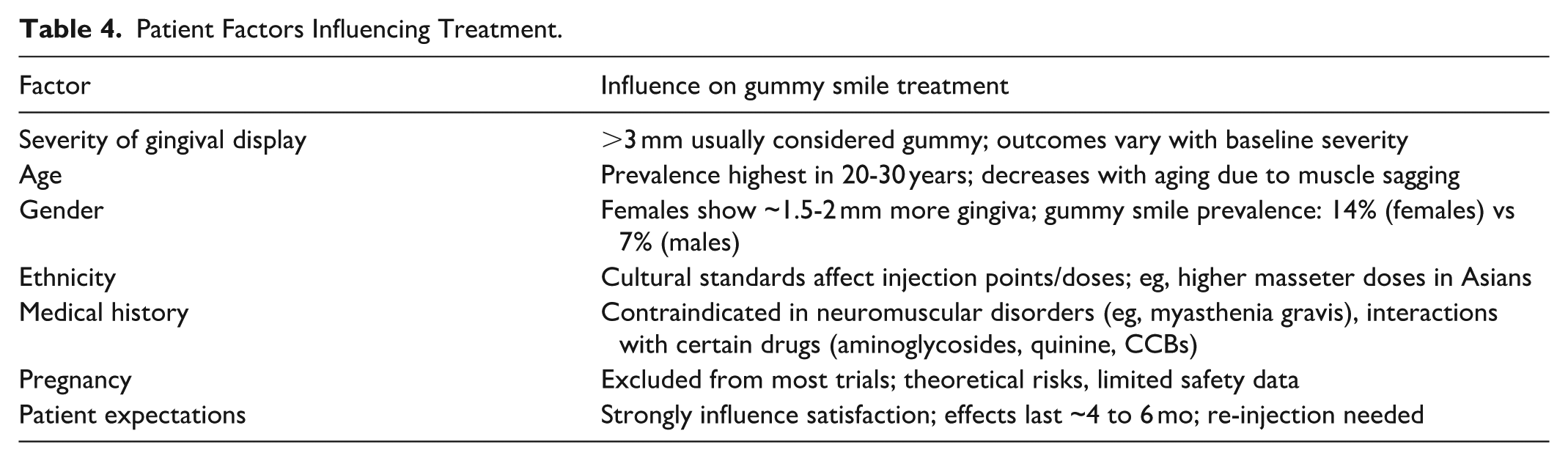

Certain types of patients are not allowed to receive botulinum toxin Type A injections and participate in the study, which ultimately changes the patient demographic and affects how effectively the treatments are rated. In a clinical study, women who were pregnant, planning a pregnancy, or capable of becoming pregnant but were not using nor willing to use birth control were excluded from the study. Furthermore, women of child-bearing age were required to submit a negative blood pregnancy test 1 to 4 hours before the first round of botulinum toxin Type A injections. Having not taken into account these types of women, the study resulted in a mean gingival exposure reduction of 5.2 mm. 28
The fear is that the botulinum toxin will not stay localized at the injection site, which could then cross the placenta or be absorbed into the breast milk, bringing harm upon the mother and the unborn child. Based on current data, case studies of expectant mothers with botulism poisoning during pregnancy where their babies do not suffer any adverse outcome or birth defects, it seems that botulinum toxin can be administered to these types of women. 35 However, until more data are available, benefits and potential risks to both the mother and the infant should be considered when considering botulinum toxin A, and thus should be excluded from participating.
Controversy, the effect of patient demographics on gummy smile treatments can also be considered negligible. A clinical study that reported that the treatment of excessive gingival display with onabotulinum toxin A is an effective and safe procedure. The study conducted a
Age and Gender
The prevalence of gummy smiles is reported to be 10% to 15% at the age of 20 to 30 years, but with age, due to sagging muscle tissue of the upper lip and its covering with gingival tissue along with part of the teeth of the upper jaw, the incidence decreases 36 Studies have found that the amount of gingiva exposed when smiling in females was 1.5 to 2 mm greater than males, at a rate of 7% in males and 14% in females. 36 However, the effect of average-dose BTX-A treatment for GS depended on GS severity and patient’s sex. 34
Age and gender both have an impact on gender disparities in dental esthetics. Studies indicate that an esthetically pleasing smile for women often involves the appearance of approximately 3 mm of gum when smiling naturally. On the other hand, men typically display only their anterior teeth without a contiguous gingival margin. 37 Research suggests that women often exhibit more gum tissue in their smile than men, and the prevalence of a smile that reveals excessive gum tissue decreases with age. 37 The decrease in muscle tone contributes to the reduced appearance of the upper teeth and increased visibility of the lower teeth as individuals age. Several researchers have discovered that the usual range for normal gum displays is between 1 and 4 mm. 37
Ethnic and Racial Backgrounds
While there is limited research on the influence of ethnic and racial backgrounds on the effectiveness of BTA treatment for gummy smiles, it is generally accepted that esthetic standards, including perceptions of the ideal smile, can vary across different cultures. However, according to a systematic review by Hong. 38 The injection points vary slightly between culture and ethnicity. Injection doses for the masseter muscle are higher in the Asian population, and this may be due to slightly different standards of beauty, with Asians preferring a slimmer jawline. 38
Medical History
While there is limited research on the influence of medical history on the effectiveness of BTA treatment for gummy smiles, it is generally accepted that any pre-existing conditions or medications that affect muscle function could potentially impact the effectiveness of the treatment or put the patient at risk, for example, facial paralysis. Certain drugs, such as aminoglycosides, penicillamine, quinine, and calcium channel blockers, can enhance the effects of Botox and should not be used together with it. Individuals diagnosed with neuromuscular disorders such as myasthenia gravis and Eaton-Lambert syndrome are not good candidates for Botox treatment.34,40
Patient Expectations
Patient expectations play a crucial role in the perceived effectiveness of BTA treatment. Satisfaction with treatment lasted 21 weeks in 1 group and 16 weeks in another in a study. 8 However, female participants with baseline anterior GE ≥ 6.0 mm or male participants were less likely to show complete improvement at 4 weeks. 34
Discussion
The available evidence supports botulinum toxin A (BTA) as a targeted, minimally invasive option for the management of gummy smile when excessive gingival display is primarily driven by hyperactivity of the upper lip elevator muscles. Across the reviewed literature, BTA consistently reduced gingival exposure by weakening some combination of the levator labii superioris alaeque nasi (LLSAN), levator labii superioris (LLS), and zygomaticus minor (ZMin), with maximal clinical effect typically observed within 2 weeks of injection.18,19,23,24 Although treatment durability is limited, with gradual return toward baseline by approximately 4 to 6 months, patient satisfaction rates were generally high, particularly among individuals seeking a reversible or non-surgical alternative to orthodontic or orthognathic interventions.23,24
Injection planning is most effectively guided by the anatomical distribution and severity of gingival display. Location-based classification systems, particularly that proposed by Mazzuco and Hexsel, 17 provide a practical framework for selecting injection targets. Anterior-predominant gummy smiles tend to respond best to approaches that emphasize LLSAN and LLS involvement, whereas posterior or mixed patterns may require greater engagement of the ZMin. Asymmetric presentations often necessitate differential dosing between hemifaces to restore balance. 17 These classification systems allow clinicians to tailor injection strategies to the underlying muscular drivers of gingival exposure rather than applying uniform treatment patterns. The recommended injection point for gummy smiles is illustrated in Figure 4.
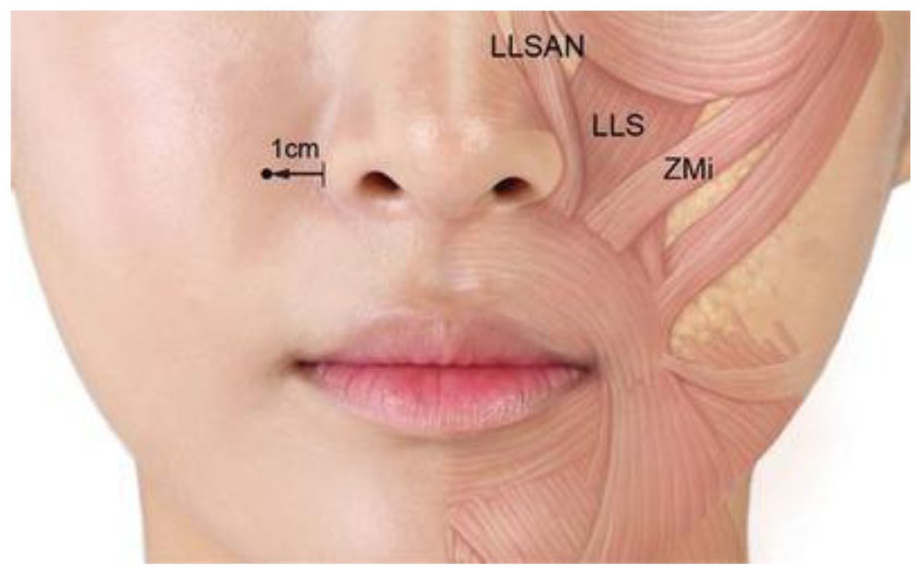
The recommended injection point for gummy smile treatment. 33
Single-injection techniques targeting the LLSAN or the so-called Yonsei point have been widely described and offer the advantage of procedural simplicity. Injection of the LLSAN alone has demonstrated meaningful reductions in gingival display using relatively low unit dosing per side, particularly in patients with mild to moderate severity.23,24 The Yonsei point, intended to affect the confluence of LLSAN, LLS, and ZMin, has produced more variable outcomes across studies.25-27 This variability likely reflects interindividual differences in muscle anatomy as well as differences in injection depth, as deeper placement may disproportionately affect the LLS and lead to overcorrection. 25 These findings underscore the importance of cautious dosing and meticulous attention to injection plane when using single-point strategies. 25
For patients with more severe gingival display, multi-point injection techniques have been associated with more robust reductions in gum exposure. By distributing toxin across overlapping regions of the upper lip elevator muscles, these approaches can more comprehensively limit lip elevation during smiling. 28 However, several studies reported that in patients with milder baseline gingival exposure, multi-point techniques may result in excessive lip descent below the gingivodental margin, negatively affecting patient satisfaction. 28 This observation highlights the necessity of severity-based dose titration and supports reserving multi-point approaches for patients with more pronounced gingival display unless lower doses are used. 28
Injection of the orbicularis oris muscle at the vermilion border, commonly referred to as the “lip flip,” represents an alternative technique that reduces gingival display indirectly through lip eversion rather than direct weakening of the elevator muscles. 30 While this method has been shown to enhance upper lip fullness and smooth perioral rhytides, its role in gummy smile correction remains less clearly defined. 30 The available evidence is limited, and outcomes are less consistently quantified compared to elevator muscle-targeted techniques. 30 As such, the lip flip may be best considered an adjunctive or secondary option rather than a primary treatment modality for excessive gingival display. 30
Across all techniques, reported dosing varied substantially, reflecting the absence of standardized protocols.23-28 Most studies employed low single-digit unit ranges per side or per site, with higher doses reserved for more severe cases.23,24,28 The literature consistently favors a conservative, titration-based approach, particularly in patients with mild to moderate gingival display, to minimize the risk of overcorrection and functional impairment. 28 Reassessment at peak effect, approximately 2 weeks post-injection, allows for refinement of treatment in subsequent sessions.23,24
The temporary nature of BTA treatment is a critical component of patient counseling. While BTA offers high safety, rapid onset, and minimal recovery time, its effects are not permanent, and maintenance injections are typically required every 4 to 6 months to sustain results.23,24,28 This characteristic distinguishes BTA from surgical and orthodontic approaches and positions it as either a standalone option for patients prioritizing non-invasiveness or as an adjunct in more complex or refractory cases. 28 Importantly, patients with gummy smiles driven predominantly by skeletal or dentoalveolar factors should be counseled that BTA may provide only partial cosmetic improvement and should not be presented as definitive management. 17
Limitations and Future Directions
Despite encouraging clinical outcomes, the current literature is limited by heterogeneity in classification systems, injection landmarks, dosing strategies, outcome measures, and follow-up duration. Many studies are small, non-randomized, and rely on photographic analysis without standardized measurement protocols. Future investigations should focus on prospective, comparative designs with standardized reporting of anatomical targets, injection depth, toxin formulation and dilution, and validated measures of gingival display. Such efforts are necessary to establish consensus-based protocols and to optimize both safety and esthetic outcomes in the cosmetic management of gummy smiles with botulinum toxin A.
Conclusion
In summary, using botulinum toxin A (BTA) for treating smiles in cosmetic procedures presents a promising option compared to traditional surgeries. BTAs effectiveness in reducing gum exposure, its minimally invasive nature and its cost-effectiveness make it an appealing choice for many patients. Different techniques like multiple injections and the “lip flip” have shown varying levels of success, underscoring the need to customize the approach based on each patient’s unique anatomy and the severity of their gummy smile. Although BTA delivers results necessitating re-injections every 6 months, it remains a valuable tool in cosmetic treatments. Future studies should aim to refine these methods and investigate long-term outcomes to boost patient satisfaction and treatment effectiveness.
Footnotes
Ethical Considerations
Not required.
Consent to Participate
The authors confirm to have participated in the development of the study and consent to its submission and publication.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Author Gaby Doumit is a member of the Editorial Board of FACE and did not take part in the peer review or decision making process for this submission.
