Abstract
Introduction:
Understanding the pandemic-related influences on postpartum depression (PPD) is crucial to informing public health strategies and interventions that support maternal mental health during and after periods of crisis.
Objectives:
This study analyzed patterns of PPD during the pre-pandemic and post-pandemic periods, and evaluated whether PPD levels in the post-pandemic period differed from those observed before the pandemic. The post-pandemic period was examined to determine whether pandemic-associated differences in PPD persisted following the end of the pandemic.
Methods:
This is a retrospective cohort study, where Edinburgh Postnatal Depression Scale (EPDS) scores of primiparous women who gave birth at a tertiary private hospital between March 2018 and May 2024 were analyzed.
Results:
At the end, the cohort study consisted of a total of 1128 participants, with 248 (22.0%) in the pre-COVID period, 539 (47.8%) in the early post-COVID period, and 341 (30.2%) in the post-pandemic period. When examining the mean EPDS scores, the early post-COVID group had the lowest scores among the three groups. While there was no statistically significant difference between the pre-COVID (6.49) and early post-COVID (5.81) scores, a significant difference was observed between the early post-COVID and post-pandemic (7.01) scores (p = 0.002). A moderate, positive correlation was identified between EPDS scores and the length of hospital stay (r = 0.70). Prolonged hospitalization appeared to be associated with higher depression scores.
Conclusion:
The results of our study indicate higher PPD scores in the late post-pandemic period, suggesting that the pandemic’s mental health effects have evolved over time. While initial assessments showed comparable PPD scores pre- and post-pandemic, our findings reveal a concerning rise starting in 2023, aligning with emerging evidence on the pandemic’s prolonged psychological impact. Understanding the delayed impact of such global events is key to developing resilient maternal health systems.
Introduction
Postpartum depression (PPD) is a complex and prevalent mental health condition affecting mothers in the months following childbirth, with symptoms ranging from sadness, anxiety, and irritability to more severe depressive episodes that can impair a mother’s ability to care for herself and her infant. Globally, PPD has long been recognized as a significant public health concern, with studies reporting prevalence rates ranging from 10% to 20% among new mothers.1,2 The onset of the COVID-19 pandemic in early 2020 introduced additional psychosocial stressors that substantially influenced the experience, prevalence, and management of PPD. 3
Pandemic-related factors—including prolonged social isolation, limited access to health care services, financial strain, and heightened anxiety regarding infection risk—have profoundly affected postpartum women. Among them, first-time mothers emerged as a particularly vulnerable group due to the fear of exposure to the virus during hospital visits and stays, the loss of social and familial support, and prolonged emotional isolation. Several studies have demonstrated that the incidence and severity of PPD were significantly higher during the pandemic compared with pre-pandemic periods,3,4 consistent with established evidence linking major stressful life events in the perinatal period to poorer maternal mental health outcomes. 5
With many traditional support systems disrupted by lockdowns and health protocols, protective factors such as in-person family support, peer interaction, and community-based maternal care were diminished. Although telemedicine played a critical role in maintaining continuity of care, its limitations in addressing complex emotional needs have been widely recognized. Recent literature further suggests that the pandemic not only increased the incidence of PPD but also altered its clinical presentation, associated risk factors, and response to intervention.
This study aimed to examine differences in postpartum depression patterns across pre-pandemic, pandemic, and post-pandemic periods. We assessed whether maternal mental health indicators observed in the post-pandemic period differed from pre-pandemic levels. We specifically sought to determine whether the psychosocial consequences of the pandemic persisted following the official end of the global health emergency. We hypothesized that mean Edinburgh Postnatal Depression Scale (EPDS) scores would differ significantly across pandemic-related timeframes, with a potential rebound in depressive symptoms during the late post-pandemic period.
Understanding these pandemic-related influences on postpartum depression is essential for developing targeted public-health strategies that strengthen maternal mental health resilience during and after large-scale crises.
Patients and Methods
Study design and participants
This is a retrospective cohort study. Data analysis was performed using patient records extracted from the hospital’s electronic database. EPDS scores of primiparous women who gave birth at a tertiary private hospital between March 2018 and May 2024 were analyzed. In May 2023, the World Health Organization declared the end of the global health emergency caused by the COVID-19 pandemic.
6
Based on pandemic-related timeframes, records of primiparous women were categorized into three distinct groups:
Group 1: Pre-COVID—From January 2018 to January 2019 Group 2: Early post-COVID—From December 2021 to January 2023 (representing the early post-acute COVID-19 period) Group 3: Post-pandemic—From May 2023 to May 2024
In the pre-COVID cohort, the systematic assessment of postpartum depression scores had only recently been implemented in our institution. Consequently, due to loss to follow-up among some patients, the number of eligible cases involving primiparous women with singleton pregnancies during this period was relatively limited.
To obtain a homogeneous study sample, only primiparous women with singleton pregnancies who gave birth in the same tertiary-level hospital were included. Individuals who had COVID-19 at the time of delivery or during the administration of the test, as well as women who received treatment for psychological disorders during pregnancy or who delivered before 36 weeks and 6 days of gestation, were excluded from the study.
This study was approved by the Institutional Review Board of Koc University (Approval No: 2022.487.IRB1.196). Informed consent was waived due to the retrospective nature of the research.
In our hospital, in addition to the EPDS assessment, a standardized questionnaire is routinely administered to determine the demographic and socioeconomic characteristics of all women who give birth. The variables used in this study including demographic, obstetric, and mental health variables were derived from this existing dataset, which is systematically collected as part of routine clinical practice.
The EPDS, a standardized and widely used instrument for assessing postpartum depression, was administered between the 2nd and 6th weeks postpartum. The Turkish version of the scale, validated for use in the local population, was utilized. 7 A cut-off score of 12 was adopted in line with national guidelines, and participants scoring 12 or above were referred to psychiatric services.
In addition to the EPDS assessment, the following variables, which are considered to potentially influence postpartum depression, were included in the analysis:
Maternal age Paternal age Maternal educational status Paternal educational status Mode of delivery Presence of neonatal or maternal complications in the postpartum period Length of hospital stay Whether the pregnancy was spontaneous or achieved through assisted reproductive treatment Presence of professional postpartum support (defined as the use of hired professional assistance such as a nurse, doula, or maternity caregiver during the postpartum period)
Statistical analyses
Descriptive statistics were presented as means and percentages. Normality of the distribution for numerical variables was assessed using skewness and kurtosis values. All numerical variables except hospital length of stay were normally distributed.
Comparisons involving hospital stay were analyzed using the non-parametric Kruskal–Wallis test, and significant differences between groups were further evaluated using Bonferroni-adjusted Mann–Whitney U tests.
Categorical variables were analyzed using the Chi-square test where appropriate. The association between maternal education level and psychiatric referral was evaluated using the Pearson Chi-square test, whereas the relationship between paternal education level and psychiatric referral was assessed using Fisher’s Exact test due to the small sample size in some categories.
The relationship between maternal age, hospital stay, and EPDS scores was assessed via both Pearson and Spearman correlation analyses to account for the non-normal distribution of some variables.
Group comparisons for normally distributed numerical variables were conducted using One-Way ANOVA, and significant findings were further explored using post hoc tests.
Results
Initially, data from 1,196 primiparous women out of 1783 deliveries were included in the analysis. However, 65 participants were excluded for the following reasons: 19 women (17 from Group 2 and 2 from Group 3) had COVID-19 infection either at the time of delivery or during the administration of the EPDS; 3 women (one from each group) had received psychological treatment during pregnancy; and 43 women delivered before 36 weeks and 6 days of gestation (9 from Group 1, 22 from Group 2, and 12 from Group 3).
Approximately 65% of the women who delivered during the study period were primiparous. Annual numbers of births in Groups 1, 2, and 3 were 496, 752, and 535, respectively.
At the end, the cohort study consisted of a total of 1128 participants, with 248 (22.0%) in the pre-COVID period, 539 (47.8%) in the early post-COVID period, and 341 (30.2%) in the post-pandemic period.
The mean maternal and paternal ages were similar across all three groups (Table 1). The majority of the participants were highly educated, with 1031 women (91.4%) holding undergraduate or postgraduate degrees. The proportions of participants with primary and high school education were 7.3% (n = 82) and 1.3% (n = 15), respectively. Fathers’ education levels demonstrated a similar distribution: 0.3% had primary education, 6.9% had completed high school, and 92.8% held a university or postgraduate degree.
Demographic Characteristics of the Cases by Delivery Period
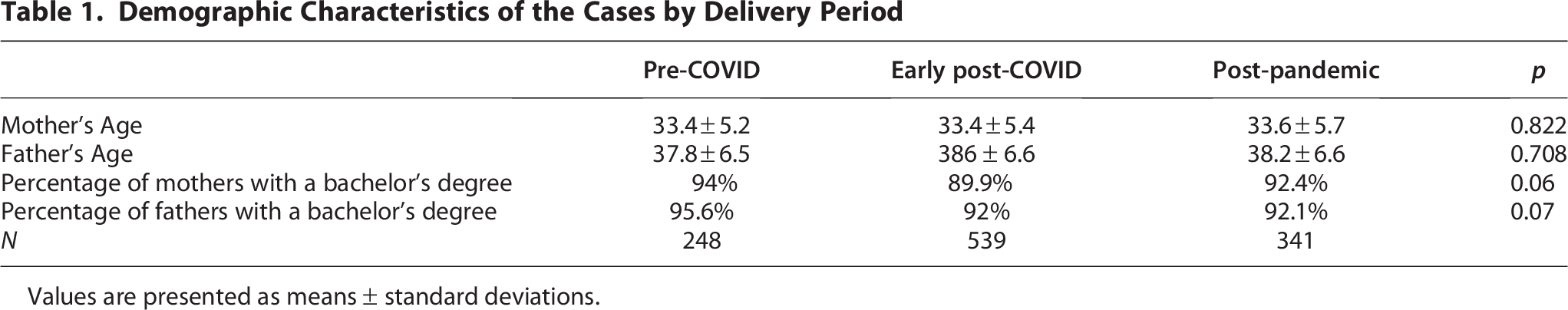
Values are presented as means ± standard deviations.
Chi-square tests showed no statistically significant differences among the three groups in terms of referral to psychiatry when analyzed by maternal and paternal education levels, mode of delivery, postpartum complications, neonatal complications, spontaneous vs. assisted conception, or the presence of domestic or professional support (Table 2).
The Percentage of Miscarriage, Infertility Treatment, Newborn, and Maternal Complication Rates Among All Patients with High Edinburgh Scores

When examining the mean EPDS scores, the early post-COVID group had the lowest scores among the three groups. While there was no statistically significant difference between the pre-COVID (6.49) and early post-COVID (5.81) scores, the post-pandemic (7.01) scores were significantly higher than the early post-COVID scores (p = 0.002). No significant difference was found between the pre-COVID and post-pandemic groups (p = 0.442).
A moderate, positive correlation was identified between EPDS scores and the length of hospital stay (r = 0.70, p < 0.001) indicating that longer hospitalizations were associated with higher depression scores. Although the referral rate to psychiatry was higher in the late post-COVID group (17.3%), this difference was not statistically significant (p = 0.131; Table 3).
Edinburgh Postnatal Depression Scores, Length of Hospital Stay, and Referral Rates to Psychiatric Services by Group

Edinburgh Postnatal Depression Scale scores were observed to be significantly higher in the post-pandemic group compared with the early post-COVID group (p = 0.001).
No significant association was found between postpartum psychiatric referral rates and variables such as previous abortion, history of dilation and curettage, neonatal complications during delivery, spontaneous or assisted conception, type of family (extended or nuclear), mode of delivery, or parental education levels.
The average length of hospital stay was significantly longer in the late post-COVID period (3.31 days) compared with both the pre-COVID (2.74 days) and early post-COVID (2.88 days) periods (p < 0.001; Table 2). However, no significant difference was found between the pre-COVID and early post-COVID groups (p = 0.327).
A striking finding of this study was the significant reduction in the utilization of professional postpartum support. The proportion of participants employing professional assistance was significantly lower in the late post-COVID period (3.8%) compared with the pre-COVID (32.7%) and early post-COVID (14.7%) periods (p < 0.001).
Discussion
In our study, we observed that PPD scores remained similar before and immediately after the COVID-19 pandemic. However, in 2023, during the late post-pandemic period, the PPD scores were notably higher. This pattern suggests that while the immediate psychological impact of the pandemic on postpartum mental health may have been limited, its long-term effects have become more evident over time.
Recent literature supports the notion that the cumulative psychosocial stressors associated with the pandemic—such as prolonged social isolation, economic instability, changes in health care access, and uncertainty surrounding recovery—may have contributed to delayed exacerbations in maternal mental health. 8 Studies indicate that chronic stress and disrupted support systems can have persistent effects on postpartum well-being, even after the resolution of acute crises. 9 Therefore, our findings emphasize the necessity of continued screening and mental health support for postpartum women well beyond the end of major global crises.
At this point, the pandemic-driven expansion of telemedicine appears to have reshaped approaches to maternal mental health care, with effects that extend beyond the acute pandemic period. Even as in-person services resumed, telehealth remained a valuable tool for extending access to psychological support and counseling. This integration of virtual and traditional care modalities may have improved postpartum care continuity and accessibility for women with logistical or emotional barriers to in-person visits.
Nevertheless, incorporating a risk stratification model beyond routine screening could facilitate more targeted interventions. The study by Clapp et al. demonstrates the feasibility of stratifying the risk of PPD using electronic health record data routinely collected before discharge after an individual’s delivery. Implementing such models to identify individuals at higher risk may enable more targeted screening and reduce unnecessary assessments. 10
Consistent with our findings, Khoury et al. reported that the long-term psychological consequences of COVID-19 on postpartum women became more apparent as the pandemic’s acute phase subsided, emphasizing lingering vulnerabilities. 11 Similarly, Steward et al. demonstrated that elevated rates of postpartum depression and anxiety persisted beyond the initial pandemic period, suggesting that psychological recovery lagged behind physical recovery. 12 These findings collectively underscore that postpartum mental health requires long-term monitoring and integrative care strategies, particularly following prolonged global disruptions.
The COVID-19 pandemic introduced unprecedented challenges that significantly affected maternal mental health, with elevated PPD rates reported due to fear of infection, isolation, restricted health care access, and financial strain. 13 While these environmental stressors intensified depressive symptoms during the pandemic, evidence suggests that as restrictions eased and access to health care improved, PPD rates began to decline toward pre-pandemic levels.
Our study did not include data from the active pandemic phase. Previous comparative studies reported significantly higher EPDS scores during that time. 14 In contrast, our early post-pandemic results demonstrated EPDS scores comparable to the pre-pandemic period, suggesting a transient recovery phase in postpartum well-being. This improvement may be attributed to the restoration of social contact, resumption of health care services, and reduction of infection-related anxiety. The re-establishment of family and community support systems likely played a central role in restoring psychological resilience among postpartum women.
While PPD rates in the post-pandemic period were comparable to pre-pandemic levels, it is important to recognize that this observation should not be interpreted as evidence of a reduction in baseline risk. Rather, it suggests a return to a state in which pre-existing psychosocial stressors—such as economic hardship and limited childcare support—again dominate maternal mental health outcomes.
Besides, our study identified a marked decline in the use of professional postpartum support (such as hired maternity caregivers or nurses) in the late post-pandemic period. This observed reduction may reflect a combination of financial constraints and changing family dynamics following the pandemic.
We also found a significant correlation between longer hospital stays and higher EPDS scores (r = 0.70, p < 0.001), suggesting that extended hospitalization could indicate increased maternal anxiety and sensitivity in the post-pandemic context. Yet, prolonged hospital stay may result from medical reasons related to the mother (e.g., fever, abdominal distension, bleeding) or the newborn (e.g., respiratory or feeding difficulties, hyperbilirubinemia), as well as from social factors. Due to the retrospective design of the study, we were unfortunately unable to further elaborate on these reasons.
The higher EPDS observed in our study during the late post-pandemic period may be primarily associated with worsening economic conditions both globally and within Turkey. The financial crisis that surfaced during this period may have compounded stress for families, thereby reducing mothers’ coping capacity and resilience. Davenport et al. previously warned that early deterioration in maternal mental health during the pandemic could have long-term consequences—a prediction that is consistent with our findings. 15 Nevertheless, alternative explanations should be considered. Higher EPDS in the late post-pandemic period may partly reflect more screening coverage and heightened awareness of postpartum depression, as the EPDS was completed by a larger proportion of patients during later periods. Additionally, unmeasured confounding factors may have contributed to the observed associations.
A major strength of this study lies in its relatively large and homogeneous sample, composed exclusively of primiparous women with higher educational and socioeconomic status, all of whom had private insurance and delivered at a tertiary-level private hospital. The exclusion of participants with active COVID-19 infection during delivery or EPDS administration further isolated the psychological impact of the pandemic environment itself. This methodological design minimized confounding effects and allowed a clearer interpretation of the pandemic’s indirect effects on postpartum depression.
Limitations
The primary limitation of this study is its retrospective design, which inherently restricts causal inference. As data were collected from existing medical records, the accuracy and completeness of certain variables may have been constrained by documentation quality. At the beginning of the study period, the EPDS assessments had only recently been implemented, and, therefore, it is highly likely that they were not yet administered to all eligible cases. In the later periods, as the assessment became fully integrated into clinical routine, data collection became more consistent and reliable.
Although the study’s homogeneous sample—comprising primiparous women with high educational and socioeconomic status who delivered in a tertiary-level private hospital—can be considered a methodological strength in terms of internal validity, it simultaneously constitutes a limitation in terms of external validity. This specific demographic profile limits the generalizability of the findings to the broader population, particularly to women from lower socioeconomic backgrounds or those delivering in public health care settings. Therefore, the results should be interpreted with caution, as they primarily reflect the experiences and outcomes of a well-resourced subgroup rather than the general obstetric population.
Additionally, the inability to evaluate a wider range of psychosocial, hormonal, and environmental variables that could influence postpartum depression—such as relationship quality, perceived stress, or social network size—constitutes another notable limitation. Furthermore, the absence of longitudinal follow-up precludes evaluation of changes in depressive symptoms beyond the 6-week postpartum period.
Future studies employing prospective, multicenter designs with more diverse participant groups and longer follow-up durations could provide a more comprehensive understanding of the long-term trajectories of postpartum depression after large-scale societal stressors.
Conclusions
Although early assessments revealed comparable PPD scores before and shortly after the pandemic, our findings indicate higher PPD scores in the late post-pandemic period beginning in 2023. This trend in PPD scores supports the hypothesis that the pandemic’s psychological burden persisted and re-emerged during the post-pandemic recovery phase.
These results highlight the importance of sustained mental health surveillance and early intervention strategies for postpartum women, even after the apparent resolution of global crises. Recognizing the prolonged and cumulative nature of psychosocial stressors can help clinicians and policymakers design more resilient maternal mental health frameworks.
In summary, understanding the delayed impact of large-scale global events such as the COVID-19 pandemic is essential for strengthening postpartum care systems, improving preventive mental health strategies, and ensuring the long-term well-being of mothers and their infants.
Authors’ Contributions
E.A.: Conceptualization, methodology, investigation, formal analysis, writing—original draft. T.A.: Writing—reviewing and editing.
Footnotes
Author Disclosure Statement
No conflict of interest was declared by the authors.
Funding Information
The authors declared that this study has received no financial support.
Ethical Approval
The ethics committee approval of the study has been obtained from the Institutional Review Board of Koc University. (Approval no: 2022.487.IRB1.196).
