Abstract
Background:
Proximal patellar tendinopathy is common in athletes, with a reported incidence up to 45% in jumping athletes, and can often be treated nonoperatively. If surgery is required, open debridement is often performed, but arthroscopic debridement has several advantages—including higher rates and earlier return to sports.
Indications:
Patients with (1) symptoms of anterior knee pain or pain with patellar tendon loading activities, (2) who have not responded to nonoperative treatment, and (3) have proximal partial articular-sided fraying of the patellar tendon on magnetic resonance imaging (MRI).
Technique Description:
The patient is positioned supine, and standard arthroscopy equipment is used. The anterolateral portal is created more laterally than the standard portal, and the anteromedial portal is created under vision more medially than the standard. The ligamentum mucosum and Hoffa's fat pad are debrided until the proximal part of the patellar tendon is visualized. A spinal needle is placed through the tendinopathy part of the tendon based on preoperative MRI. The tendon is debrided with a shaver from the anteromedial and later anterolateral portal until healthy intact patellar tendon fibers are visualized. Bony resection of the inferior pole of the patella is performed to avoid impingement.
Results:
Arthroscopic partial patellar tendon debridement has been shown to lead to superior outcomes compared to open debridement, with a treatment success of 91%, a return to sports of 96%, a return to the previous level of 77%, and a mean time to return to sports of 3.9 months. Inferior pole resection has been shown to be superior compared to no resection.
Discussion/Conclusion:
Arthroscopic debridement of proximal patellar tendinopathy with partial tearing is a minimally invasive and successful procedure and should be considered for athletes after failure of nonoperative treatment.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
Level of Evidence:
Level 3.
This is a visual representation of the abstract.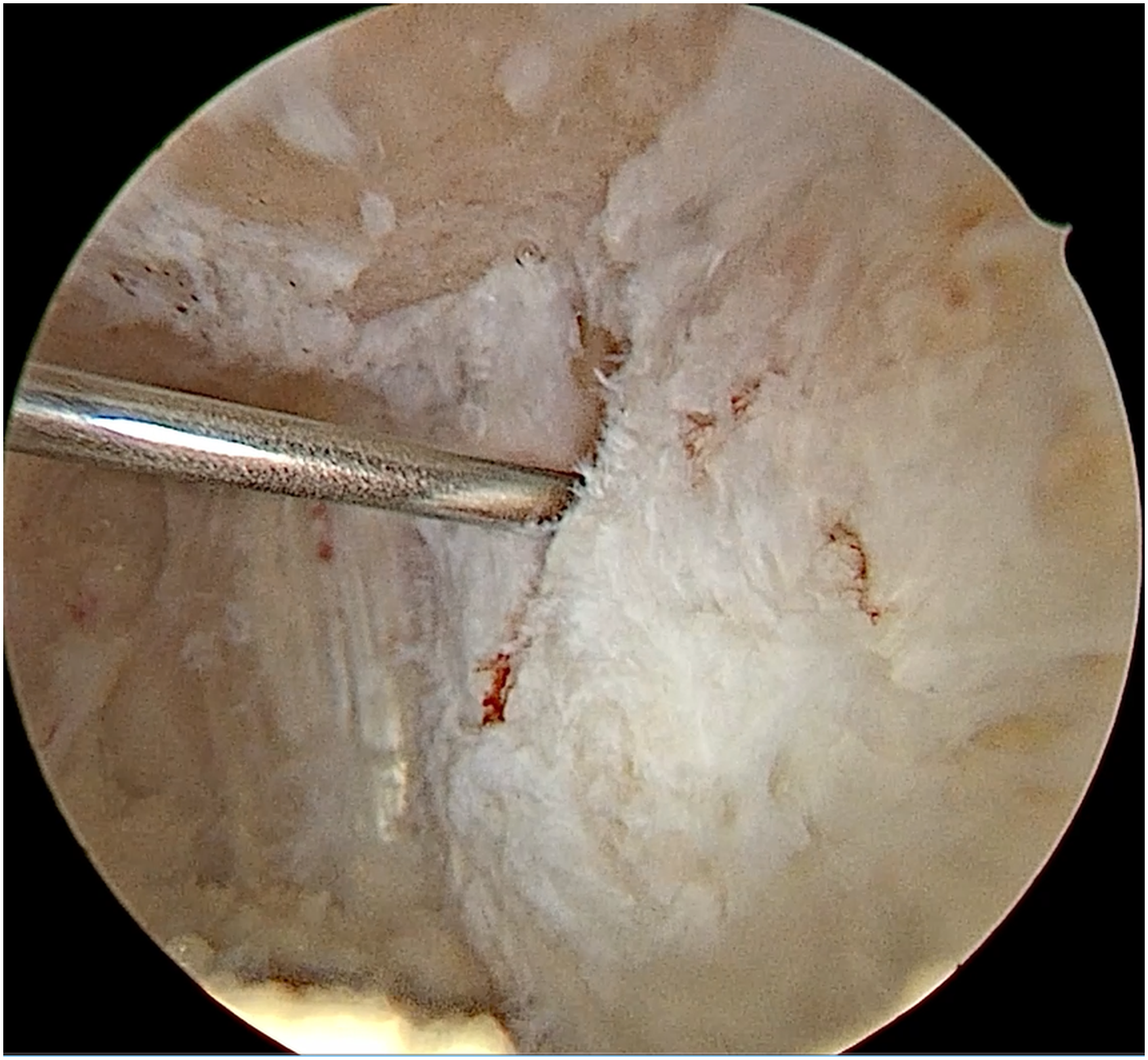
Keywords
Video Transcript
We present our study, Arthroscopic debridement of proximal patellar tendinopathy in athletes. These are our disclosures. One or more of the authors has declared a potential conflict of interest as specified in the VJSM Conflict of Interest statement.
In this video, we will review the background, preoperative planning, patient positioning, and procedure of arthroscopic debridement of proximal patellar tendinopathy, along with potential complications, rehabilitation and return to sports, and patient outcomes in the literature.
Background
We present the case of a 16-year-old basketball player who is having anterior knee pain for 5 months without single-event trauma.
Indications
His symptoms are aggravated by flexion, stairs, jumping, and playing sports. Treatment has consisted of 5 months of physical therapy without improvement. No injections have been performed. Radiographs reveal normal alignment and show no trochlear dysplasia or patellar alta. Physes are nearly closed. Magnetic resonance imaging (MRI) T2 images of sagittal, coronal, and axial slices show proximal patellar tendinopathy, with thickening up to 11 mm, bony impingement, and partial proximal tendon articular-sided tearing. The decision was made to perform an arthroscopic debridement of the proximal patellar tendinopathy. Arthroscopy is preferred over open surgery, as this keeps the paratenon and patellar tendon intact, and is associated with higher rates and earlier return to sports.1,2,4 The case will initially take around 30 minutes, but with a learning curve, this can be performed in 15 to 20 minutes.
For preoperative planning, it is important to set expectations with the patient on rehabilitation and the time frame for return to sports and patellar tendon loading. One should critically review the preoperative MRI with the location of tendinopathy, presence of impingement, and the thickness and amount of tendinopathy. Portal placement is different from standard knee arthroscopy, and surgeons should be aware of this with logistics and portal creation. Patient positioning is supine with either a post or leg holder. Standard knee arthroscopy equipment is used with an 18-gauge spinal needle and shaver.
Technique Description
One should identify the midportion of the proximal patellar tendon, the medial and lateral borders of the patellar tendon, the standard arthroscopy portals, and the modified, more lateral and medial portals that are used for this procedure. First, as preferred by the senior author, an inflow portal is created superolaterally, but this is not required for this procedure. Now, an anterolateral portal is created approximately 2 cm lateral from the lateral border of the patellar tendon, and this is more lateral than the standard anterolateral portal. Under vision, a spinal needle is first used to identify the ideal location of the anteromedial portal, which is not displayed here. Then, the anteromedial portal is made and opened with the blunt trocar. This portal is approximately 2 cm more medial than the standard anteromedial portal (Figure 1). A spinal needle is placed through the tendinopathy portion of the proximal patellar tendon, which was central in the patellar tendon in this case. This helps with identification during debridement.

An image of a left knee shows approximately 8 cm of the distance between the anteromedial and anterolateral portals, which is greater than that of standard arthroscopy portals.
With the arthroscope in the anterolateral portal and the shaver from the anteromedial portal, the fat pad is then debrided using the shaver. As can be seen during the video, the spinal needle is moved multiple times further into the joint for localization and then partially retracted in order to create space for the shaver. Ultimately, the distinction can be made between the more yellow fat pad and the white tendinopathic tendon tissue. This tissue will also be debrided until healthy intact tendon fibers are seen that have good tension, indicating that they are intact. The tendinopathic white tendon tissue is debrided. Then, the shaver is set at forward and the inferior pole of the patella is resected in order to avoid impingement and remove tendinopathic tissue. It is recommended to pass the camera to the assistant and control the bur with 2 hands in order to avoid iatrogenic tendon damage. At the end, healthy fibers of the patellar tendon can be seen on the lateral side that contain proper tension, indicating that these fibers are not torn. The arthroscope is then switched to the anteromedial portal, and the shaver is introduced via the anterolateral portal, and the same process is repeated. This often provides a good assessment of the amount of resection. Further resection on the anteromedial side can then be performed. As can be seen here, the angle and location of the portal are very important to reach the tendinopathic tissue. The final inspection is performed, and the spinal needle is introduced into the defect. Intact fibers of the patellar tendon are seen medial and lateral of the small central defect, and no tendinopathic tissue or partially torn fibers are seen anymore.
Several complications should be avoided during this procedure. The indication is important, as 70% to 85% of patients can be treated without surgery. Placing portals too centrally makes surgery difficult and should be avoided. Insufficient bony resection and tendon overresection should also be avoided. Finally, too early heavy patellar tendon loading should be avoided to decrease the risk of rupture or recurrence of symptoms.
Results
The first 6 weeks of rehabilitation consist of full weightbearing and range of motion as tolerated and closed-chain exercises. From 6 to 12 weeks, light patellar tendon loading will be started to allow the patellar tendon to adapt to increasing loads. After 12 weeks, progressive loading and functional activities are progressed. General return to sports is recommended after 3 months and explosive loading after 4 months, although the literature has shown this might be performed earlier.
Discussion/Conclusion
Proximal patellar tendinopathy is common, with an incidence of up to 45% in jumping sports.5,6 Nonoperative treatment should be attempted first, with a success rate of treatment in 70% to 85% of patients.3,5 Arthroscopic debridement is preferred over open debridement, as this prevents the need for paratenon and patellar tendon opening and closure.1,2,4 Furthermore, arthroscopic treatment has been shown to lead to higher rates of return to sports and earlier time to return to sports.1,2,4 In addition, the literature suggests that bony resection should be performed, both with open and arthroscopic treatments.1,4
Footnotes
Submitted March 10, 2025; accepted June 30, 2025.
Winner of the Silver Medal Prize at the 2025 VJSM Fellows Video Technique Challenge.
One or more of the authors has declared the following potential conflict of interest or source of funding: J.P.V. is on the Editorial Board of Arthroscopy and received Fellowship Education from Arthex and Smith & Nephew. C.C.K. is a paid consultant for Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
