Abstract
Background:
Meniscotibial ligament disruption and medial meniscal extrusion may represent early and predisposing events contributing to medial meniscal root tears. If left untreated, these extruded tears may result in loss of medial compartment cartilage. As a result, multiple approaches have been developed to centralize the extruded meniscus.
Indications:
In this case, we present a 45-year-old man who sustained a left medial meniscal root tear with extrusion while playing tennis. Indications for root repair with meniscal centralization include extrusion >3 mm seen on magnetic resonance imaging after an acute meniscal root tear or subjective meniscal extrusion seen intraoperatively.
Technique Description:
The medial meniscal root tear is first repaired arthroscopically per surgeon preference. Then a medial incision is made along the proximal tibia and a submeniscal arthrotomy performed. Two double-loaded 3.0-mm anchors are placed along the proximal medial tibial edge. Sutures are passed in a Mason-Allen configuration through the meniscal body and capsule. Tightening of the sutures results in meniscal centralization. The root repair sutures are then tensioned and fixed along the medial proximal tibia.
Results:
Recent data have shown meniscal root repair with centralization is associated with significant improvements in pain, function, and quality of life and no significant progression of osteoarthritis.
Discussion/Conclusion:
Medial meniscal centralization can be safely performed with an open approach. An open approach may allow for more accurate anchor placement and more near-anatomic replication of meniscotibial ligaments.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.
Video Transcript
In this case, we present our technique for open medial meniscus centralization in conjunction with a meniscus root repair. We have no significant disclosures.
Background and Indications
This is a case of a 45-year-old man who injured his left knee acutely while playing tennis. He had no prior knee pain before. He had significant pain, swelling, and an effusion associated with medial meniscus and medial-sided knee pain. He had done several weeks of conservative treatment with physical therapy and activity modifications. His examination demonstrated isolated pain over the medial joint line with normal motion and a normal ligamentous examination. He had no prior knee injuries and no significant medical history.
Standard weightbearing radiographic imaging demonstrated no significant degenerative changes in the medial or lateral compartments. Magnetic resonance imaging (MRI) of the left knee demonstrated a complete tear of the medial meniscus root attachment with an associated 3 mm of extrusion and otherwise well-preserved chondral surfaces.
The anterior and posterior root attachments of the medial meniscus play key roles in applying resistance to hoop stress on the articular cartilage as well as providing secondary stabilization to the knee. Laprade et al 5 have published on the biomechanical consequences of root tears and nonanatomic repair, finding that the peak contact forces across the cartilage are synonymous with a total meniscectomy and are only restored with anatomic repair.
Our current understanding of the etiology and the pathoanatomy of meniscal root tears continues to evolve. Krych et al 4 at Mayo have done fantastic work understanding the development of root tears with serial MRIs. On a case series of 27 patients with symptomatic knees, they found that most tears of the medial meniscus root proceeded with detachment of the meniscus at the tibial attachment, also referred to as meniscotibial ligaments. Significant biomechanical work has been done as well. We further appreciate the importance of addressing the extrusion that occurs with root tears. As we understand, when the meniscus is extruded, it is not providing the functional hoop stresses, which ultimately results in increased stress on the cartilage surfaces. 1 So as we move forward in understanding and appropriately treating medial meniscus root tears, it is now clear that some technical considerations to address the extrusion are likely and expected to improve our outcomes.
Surgeons should consider centralization as an adjunct to root repair and apply the same indications. Acute root tears by history with evidence of well-preserved chondral surfaces on MRI are likely to result in a better surgical outcome than chronic tears with evidence of chondral degeneration. 6 When identifying a root tear, it is important to look, measure, and quantify how much extrusion is happening. Good indications for considering a medial meniscus centralization are when extrusion is present more than 3 mm and detected on the MRI and should also be subjectively intraoperatively assessed during normal diagnostic arthroscopy. 3 It is our opinion to avoid delay in repair to prevent degeneration of the medial compartment articular cartilage. We know that relative contraindications would be full-thickness chondral defects. While this can still be considered, we expected outcomes in terms of restoring the anatomy to be less optimal when full-thickness cartilage defects are present. Chronic meniscal tears may not do as well, and patients with a body mass index over 40 may struggle with postoperative restrictions and weightbearing; this ultimately may still result in excessive stress on the medial compartment despite adequate repair.
Technique Description
For planning and positioning, we use standard arthroscopy set up for any type of knee arthroscopic procedure. Implants unique to this repair use suture anchors that can be inserted into the bone, and typically we use a double-loaded anchor. In this case, we used SutureTack anchors (Arthrex) and then physician preference on fixation of the medial meniscus root, depending on preference and variable anchors available. In this case, we used a drop limb position. A nonsterile tourniquet was applied, and typically we inflate this to 250 mm Hg, although you could also position supine on a flat-top table with a well-leg holder. By standard perioperative protocol, we administer 2 g Ancef within 20 minutes of incision.
This illustration depicts our desired construct. In Figure 1, you can see a normal medial meniscus. In Figure 2, you can see that the detachment of the medial meniscus root as well as the detachment of the meniscotibial ligaments will ultimately result in meniscal extrusion with weightbearing. We fix the medial meniscus root in a standard fashion, and this can be done by any surgeon preference in terms of fixation and drilling. The medial meniscus centralization is performed with an open incision over the medial meniscus similar to an inside-out approach with 2 anchors in the tibia and sutures passed in a Mason-Allen configuration horizontally through the meniscal body and vertically through the meniscal body and capsule (Figure 3).

Illustration of a coronal view of the medial compartment of the knee with an uninjured meniscus.
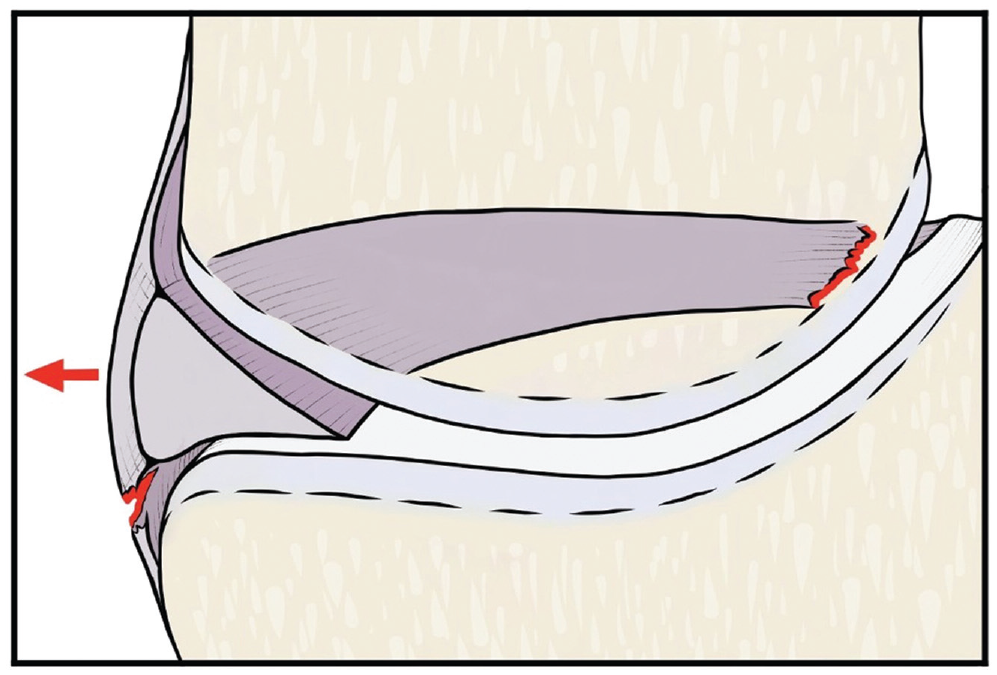
Illustration of a coronal view of the medial compartment of the knee with detachment of the medial meniscus root and meniscotibial ligament resulting in meniscal extrusion.

Illustration of a coronal view of the medial compartment of the knee with our desired construct. Two anchors are placed in the tibia and sutures passed in a Mason-Allen configuration horizontally through the meniscal body and vertically through the meniscal body and capsule.
The procedure begins with preparation of the medial meniscus root. It is safe to take down part of the tibial eminence to allow access to the root. Two sutures are passed and a drill guide is used to drill a pin at the insertion of the medial meniscus root. This is then overreamed with a 4-mm reamer, and a shuttling suture is passed. The shuttling suture is used to shuttle the meniscal root repair sutures down the tibial tunnel, and the root is then provisionally reduced but not fixed yet on the tibia.
We then begin the centralization portion. A medial incision is made along the proximal tibia and a standard inside-out meniscal repair technique. The sartorius fascia is split in line with its fibers. The medial head gastroc is mobilized off the capsule to allow for access to the medial tibia and meniscus. A spinal needle is then used to triangulate to plan a submeniscal arthrotomy. The submeniscal arthrotomy is made with a No. 15 blade.
The drill guide is then used to place two 3.0-mm anchors along the proximal medial tibial edge. We feel that an open approach allows for the most accurate placement of these anchors to fully reproduce the meniscotibial ligaments. A second anchor is then placed, and sutures are then passed. A suture from each anchor is passed in a horizontal mattress configuration, followed by a vertical mattress component. The superior leaflet of the vertical mattress passes through the medial meniscal body and capsule, and the distal pass will go through the deep medial collateral ligament (MCL) distally. This vertical mattress component will then close with a submeniscal arthrotomy. Here the sutures are seen nicely placed at the periphery of the medial meniscus and on the edge of the proximal medial tibia. The sutures are then tied, demonstrating nice centralization of the medial meniscus. Following final suture tying, the medial meniscus is now secured and centralized on the proximal medial tibia. We then secure the medial meniscal root sutures in a knotless anchor along the medial tibia after drilling and tapping accordingly. Alternatively, sutures can be secured by tying over a button or cortical screw per surgeon preference.
Postoperatively, a standardized protocol is used similar to a medial meniscus root repair protocol. Patients are made toe-touch weightbearing for 6 weeks, and motion is limited from 0° to 90° in hinged knee brace. Physical therapy starts within 2 weeks. Aspirin 81 mg twice a day is prescribed for deep vein thrombosis prevention for 4 weeks. Patients are discharged on a multimodal pain regimen. Typical return to sport occurs in 3 to 6 months, depending on progression of rehab.
Results and Discussion
At 6 weeks, the patient returned with well-healed incisions and motion from 0° to 100°. He already felt better than before surgery. By 6 months, he had a full return to sport with no knee pain and is extremely satisfied with his outcome.
Satisfactory outcomes can be achieved with medial meniscus repair in the setting of centralization. Krych et al 3 reported on 25 patients who had significantly improved subjective and objective knee outcome scores, as well as improvement in pain, and no progression of arthritis radiographically.
Potential complications of this procedure including arthrofibrosis as well as failure to prevent progression of arthritis. 3 Unique to open exposure is risk to the saphenous nerve when exposing the proximal medial tibia. 2 Sometimes gaining access to the medial compartment can be challenging. Pie crusting the MCL for visualization in the joint space can be a helpful tool to prevent iatrogenic chondral injury with instrumentation. Taking care to appropriately identify and split the sartorius fascia is also crucial to avoiding iatrogenic injury to the saphenous nerve. Lastly, use of an elevator can be helpful to assist with mobilization of the meniscus and subsequent reduction.
Centralization with an open approach may allow and facilitate more accurate placement of anchors and more near-anatomic replication of the meniscotibial ligaments. Further studies are still needed to determine truly how powerful centralization is in restoring medial tibial anatomy. However, it is safe and a reasonable approach to achieving more anatomic repair of the medial meniscus.
Footnotes
Winner of the Silver Medal Prize at the 2024 VJSM Fellows Video Technique Challenge. The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
