Abstract
Background:
Tenodesis is an effective surgical technique for the management of a pathologic long head of the biceps tendon. Tenodesis is performed with either an onlay (tendon opposed to cortical surface) or inlay (tendon docked into a reamed intra-cortical tunnel). Both techniques can be performed either from a subpectoral location, which is typically done through an open approach, or from a suprapectoral location, which is performed arthroscopically. The arthroscopic suprapectoral approach, when compared with its subpectoral counterpart, has been shown to report similar patient outcomes and complication rates.
Indications:
Arthroscopic suprapectoral biceps tenodesis is most commonly indicated in patients undergoing surgical treatment with anterior shoulder pain and biceps tendonitis, often associated with concomitant pathology. Less common indications include patients with superior labrum anterior and posterior tears as well as biceps tendon subluxation or dislocations. Patients with ruptured proximal biceps tendons are contraindicated, as the tendon is typically too distal for arthroscopic management.
Technique Description:
The biceps tendon is identified arthroscopically within the bicipital groove, just proximal to the pectoralis major tendon superior border. Suprapectoral tenodesis is then performed utilizing 2 knotless suture anchors for fixation.
Results:
Patient-reported outcomes following arthroscopic suprapectoral tenodesis in the literature have been found to be excellent with minimal complications. Despite current literature being inconclusive regarding the optimal site of fixation, the arthroscopic procedure minimizes the risk of infection, cosmetic deformity, and neurovascular injury that is seen in the open approach. In addition, the use of onlay fixation has traditionally avoided the risk of humeral fracture that is seen with inlay fixation.
Discussion/Conclusion:
This arthroscopic onlay suprapectoral tenodesis has the benefit of a time-efficient and easily reproducible technique that safely minimizes the risk of humeral fracture or neurovascular injuries. This technique historically has provided a strong fixation with excellent patient-reported outcomes.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.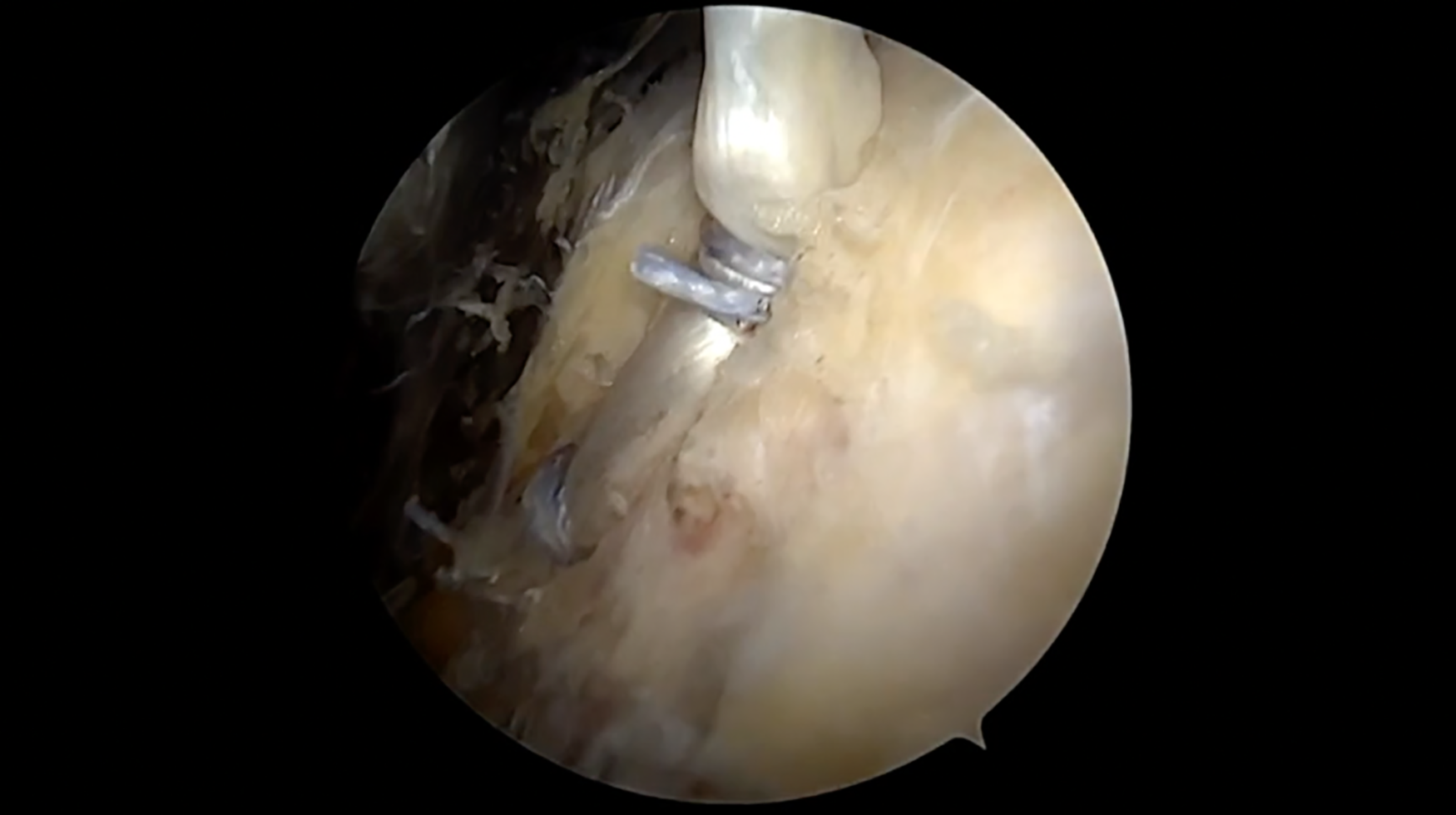
Video Transcript
The following video describes the surgical technique for an arthroscopic onlay biceps tenodesis utilizing 2 knotless all-suture anchors for the treatment of long head of the biceps tendon pathology.
These are our disclosures and the authors’ full disclosures are available online.
We will begin with a brief background, followed by a case presentation highlighting the surgical technique and then conclude with postoperative rehabilitation and a review of patient outcomes from the literature.
Long head of the biceps tendon pathology is a common source of anterior shoulder pain. 4 Biceps tenodesis is an effective surgical treatment for pathologic conditions of the biceps-superior labral complex. The procedure may be performed in numerous ways, including via an open, subpectoral approach or an arthroscopic, suprapectoral approach, as well as with fixation via an onlay or inlay technique. In this video, we describe an efficient, reproducible arthroscopic, suprapectoral biceps tenodesis with onlay fixation via 2 knotless, all-suture anchors.
Indications for biceps tenodesis include inflammation and instability of the biceps in the groove, rupture, and also superior labrum anterior and posterior lesions.
Our patient is a 54-year-old male police officer with 3 years of left anterior shoulder pain. Conservative treatments have failed to improve the patient’s symptoms and diagnostic injection with ultrasound guidance confirmed the biceps tendon as the source of pain.
On physical examination, forward flexion was 160°, which was slightly deficient compared with the contralateral side due to pain, with 90° of external rotation. There was tenderness to palpation over the biceps groove, with a positive Speed and Yergason test. There was otherwise 5/5 strength in forward elevation, abduction, and with external and internal rotation.
Imaging included radiographs and preoperative magnetic resonance imaging. Anterior and axillary radiographs reveal no abnormalities with well-maintained glenohumeral joint space.
Magnetic resonance imaging scan shows mild acromioclavicular (AC) joint arthropathy and significant fluid surrounding the biceps with a possible split tear in the biceps itself.
The procedure is performed with the patient in a seated beach chair position as pictured.
Standard portals are used with an additional accessory anterolateral portal approximately 3 cm distal to the anterolateral corner of the acromion, which is used for the tenodesis.
A diagnostic arthroscopy is performed from a standard posterolateral portal. A standard anterior working portal is also made, and the biceps tendon is evaluated with a probe, demonstrating considerable biceps tenosynovitis in this case with a positive “lipstick” sign and incarceration within the groove itself.
Next, an arthroscopic biter or scissor is used to perform the tenotomy, which is performed as close as possible to the biceps anchor, without compromising the integrity of the labrum.
At this point, any remaining intra-articular work is performed, and the scope is moved to the subacromial space. An additional lateral portal is made, which initially is used as a working portal, but then transitioned to the primary viewing portal. A thorough bursectomy is performed in the subacromial space, paying particular attention to the anterior portion of the gutter. Any AC joint pathology or rotator cuff management would be completed at this time.
When performing the tenodesis, the arm is positioned into a forward flexed position (about 45°) and externally rotated 10° which helps bring the more medial bicipital groove into view, as well as relaxing the soft tissues in the anterior space.
An accessory anterolateral portal is established approximately 3 cm distal to the anterolateral corner of the acromion, using spinal needle localization. The trajectory should be toward the superior border of the pec tendon. The biceps tendon is generally easier to identify distally, using the transverse fibers of the transverse humeral ligament as a guide. Any remaining bursa should be debrided for improved instrumentation and visualization. Vascularity is common in this area and controlled with a radiofrequency device.
Using either an 11-blade scalpel or radiofrequency ablation device from the accessory anterolateral portal, the tendon sheath is opened longitudinally to expose the underlying biceps tendon. The tendon is taken out of its sheath using a grasping device from the anterolateral portal, and held from an instrument through the posterior portal, freeing the anterolateral portal for anchor placement. An assistant manipulating the tendon from the posterior portal has been critical to simplifying the technique.
The bicipital groove is then debrided to facilitate anchor placement in a desirable position. The first anchor is placed via the accessory portal at the base of the groove at the transition zone between fibrocartilage and normal cortical bone. A 1.6-mm pilot hole is drilled and an all-suture knotless anchor implant is inserted, then deployed under the cortical surface.
A cinch is then created, using the working suture from the anchor. The blue working stitch is initially placed posterior and lateral to the tendon, then grabbed from the medial side of the tendon, creating a loop around the biceps. A grasper is placed through this created loop, and the working stitch is retrieved, creating a cinch construct. The role of the assistant cannot be understated, as manipulation of the tendon is key to facilitate suture management and ultimately tendon tension.
The assistant, holding the tendon from the posterior portal, then tensions the biceps by approximating its normal position in the proximal portion of the bicipital groove. When appropriate tension is applied, the cinch is tightened. The cinch can be translated distally as needed to create more room for a proximal cinch. The working suture and the passing suture are then retrieved through the anterior portal to avoid a soft tissue bridge.
The working suture is then placed through the loop of the passing suture. There is a mark that delineates the appropriate amount of working suture to be placed through the loop. The nonlooped end of the passing stitch is then pulled, which shuttles the working suture through the anchor, which both tensions and locks the construct. Here you can see the compression of the biceps, making sure to check that the length is appropriate before reducing the biceps into the groove itself. The tail of the working stitch is left in place for final tightening.
A second anchor is then placed approximately 1 cm proximal to the first in the same manner. The luggage tag suture technique allows for incorporation of the entire tendon width with the knotless suture construct. This is as opposed to directly piercing the tendon with the working suture, which would then only incorporate approximately half of the tendon width within the fixation construct. While data exist demonstrating superiority of the luggage tag configuration, there is a paucity of data comparing the strength of different numbers of anchors. 6 Given the lack of existing evidence, it is the authors’ preference to use 2 anchors to provide for 2 points of fixation.
Both cinches are finally tightened, demonstrating excellent apposition of tendon to bone within the groove portion creating a low-profile construct. Suture tails are then cut.
Finally, a shaver is used to remove the remaining proximal portion of the biceps leaving about a 1-cm stump to be sure that there is no slippage through the sutures. Instrumentation was then removed, and portal sites were closed with 3-0 Prolene.
The authors recommend 4 technical pearls to facilitate successful and efficient performance of this procedure.
Positioning of the operative arm in 30° to 45° of forward flexion and 10° to 15° of external rotation to improve visualization.
Identification of the long head of the biceps tendon distal to the groove after removal of the anterior bursa.
Use of coagulation throughout the procedure to minimize bleeding as the area is very vascular.
Manipulation of the tendon from the posterior portal with the help of an assistant using an arthroscopic grasper.
Postoperative rehabilitation includes passive and active range-of-motion as tolerated with the use of a sling for comfort for the first 4 weeks after surgery. Active elbow flexion is allowed; however, resisted elbow flexion must be avoided. From 4 to 8 weeks the sling is discontinued, active range of motion is progressed, but resistance training is still discouraged. At 8 to 12 weeks, progressive strengthening of the rotator cuff muscles is initiated.
Excellent clinical and functional results have been reported following biceps tenodesis. Suprapectoral and subpectoral surgical techniques have shown similar improvements in postoperative outcomes.2,3,7 Utilization of a 2-anchor fixation in arthroscopic biceps tenodesis has previously demonstrated a 5-fold decrease in Popeye deformity compared with a single-anchor technique. 5 Therefore, a 2-anchor construct is now the senior author’s preferred method of fixation in arthroscopic biceps tenodesis. Overall, the reported rate of postoperative complications following arthroscopic suprapectoral tenodesis is low. A recent systematic review of 471 patients reported a complication rate of 9.1% compared with a rate of 13.5% following open subpectoral tenodesis with the most common complications being persistent anterior shoulder pain and Popeye deformity. 1
Here are our references. We would like to thank you for your time and for watching this technique video on an arthroscopic onlay biceps tenodesis utilizing 2 knotless all-suture anchors.
Footnotes
Submitted November 20, 2022; accepted March 1, 2023.
One or more of the authors has declared the following potential conflict of interest or source of funding: N.N.V. is a paid consultant for Arthrex, Minivasive, Stryker, and Smith and Nephew; is a board or committee member for AOSSM, American Shoulder and Elbow Surgeons, Arthroscopy Association Learning Center Committee, and SLACK Incorporated; has stock or stock options in Cymedica, Minivasive, and Omeros; receives research support from Arthrex, Arthrosurface, DJ Orthopaedics, Ossur, Smith and Nephew, Athletico, ConMed Linvatec, Miomed, Mitek, Breg, and Wright Medical Technology; receives royalties from Arthroscopy, Smith and Nephew, Vindico Medical-Orthopedics Hyperguide; and receives financial or material support from Arthroscopy and Vindico Medical-Orthopedics Hyperguide. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
