Abstract
Background:
The meniscal roots are essential for preserving the structural and biomechanical properties of the tibiofemoral joint. Posterior meniscal root avulsions can cause meniscal extrusion, joint space narrowing, and progressive knee arthritis. Iatrogenic avulsions after malpositioning of the transtibial tunnels during anterior cruciate ligament (ACL) reconstruction have previously been reported in the literature to account for poor long-term outcomes seen in some patients following ACL reconstruction. Therefore, correct transtibial tunnel placement during ACL reconstruction is essential to avoid iatrogenic meniscal damage.
Indication:
Patients are indicated for surgery when presenting with a verified, symptomatic, complete meniscal root tear seen on advanced imaging or diagnostic arthroscopy. Contraindications for a root repair include the development of advanced osteoarthritis in the ipsilateral compartment, older age, and malalignment in the affected compartment.
Technique Description:
The ACL graft was appreciated and noted to be vertical and posterior relative to its native anatomical position, violating the lateral posterior horn root attachment. A full lateral posterior meniscal root avulsion was then confirmed directly adjacent to the graft tunnel. A curette was used to prepare the footprint of the lateral meniscal root on the posterolateral tibia for the 2-tunnel transtibial pull-out tunnels, and a grasper was used to position the torn meniscal root back into its anatomical site. Two ultrabraided sutures were passed through the posterior horn of the lateral meniscus using a suture passer. These were then passed through the tunnels into the body of the meniscal root and reduced to its native anatomical position. The suture repair was then secured over an Endobutton Fixation Device at 90° of knee flexion through each tunnel into its native anatomical position while confirming its adequate tension by viewing arthroscopically.
Results:
Within 2 years postoperatively, patients are expected to have improved overall knee-specific quality of life, reduced pain, and a successful return to activities.
Discussion/Conclusion:
This injury underscores the importance of an accurate tibial tunnel placement during ACL reconstruction to avoid posterior meniscal root injuries and other associated complications. Physicians should consider such pathology in the differential diagnosis of patients presenting with persistent pain and instability following a primary ACL reconstruction.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.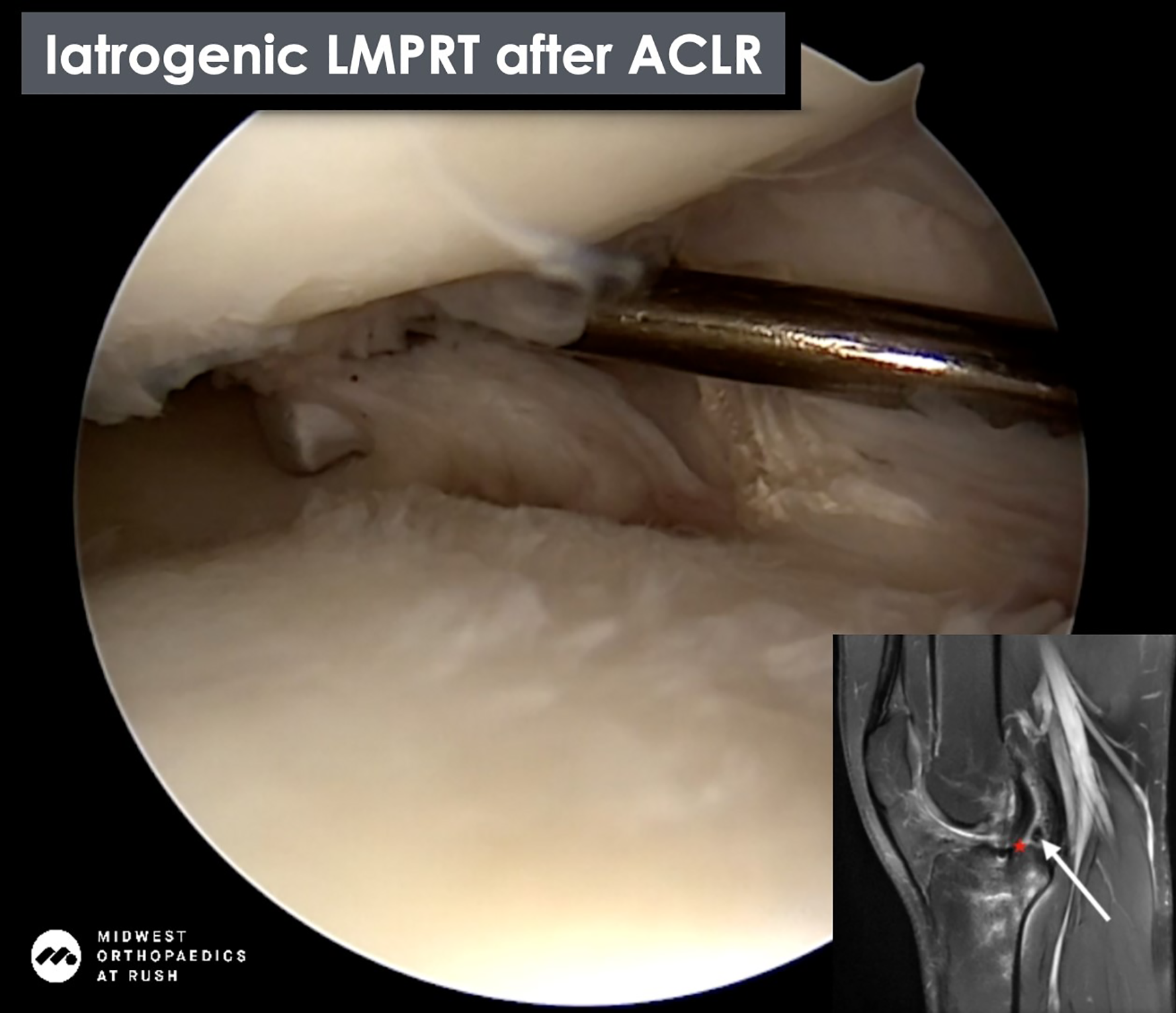
Keywords
Video Transcript
In this video, we present the unique case of the treatment of iatrogenic lateral meniscal root tear following anterior cruciate ligament (ACL) reconstruction.
Our conflicts of interest can be seen here.
The lateral posterior meniscal root is the primary restraint to meniscal extrusion under axial load. Injury to the meniscal root may cause meniscal extrusion, joint space narrowing, inadequate conversion of axial loads into hoop stresses within the joint, laxity, and eventual progression to advanced-staged osteoarthritis. 6 Lateral meniscal root tears are very common, with as high as 81% of tears reported to occur in the setting of an ACL injury. 7 Patients often present with pain, swelling, and instability in the affected knee, and may have heard an audible “pop” during the injury episode. Given the crucial role the meniscus plays in maintaining the function and health of the knee joint, it is essential to properly identify and treat these injuries.
Similarly, it is important to have a firm understanding of the meniscus anatomy and its relationship to the cruciate ligaments. Specifically, this anatomic image shows the relationship between the ACL footprint and the posterior root of the lateral meniscus. 1 One can see how if they are posterior with their ACL tunnel, it can potentially violate the posterior root of the lateral meniscus, as seen here. 4
Our patient was a 32-year-old male soccer player, who underwent ACL reconstruction with a hamstring autograph 15 months prior, as well as a partial medial meniscectomy on the same knee, approximately 7 months prior to this presentation. He re-presented to us with significant lateral-sided pain which never subsided following his ACL reconstruction.
Physical examination of this patient consisted of sharp, stabbing constant pain on the lateral aspect of the knee. The patient had motion from 1° to 110° with a mild effusion, as well as lateral joint line tenderness. He had a positive Lachman and lax anterior drawer on provocative testing.
Imaging was obtained to confirm the potential meniscal tear. There is no evidence of significant tunnel widening; however, with respect to the graft tunnels, the tibial tunnel appeared to be quite posterior in nature, with regard to its aperture within the joint on the tibial plateau.
Magnetic resonance imaging (MRI) evaluation demonstrates likely intact ACL, status post-ACL reconstruction with lateral meniscal root tear directly adjacent to the ACL graft. This is more clearly demonstrated in the still images shown here. The white arrows demonstrate the lateral root tear on coronal and sagittal imaging. Computed tomography (CT) scan shows a similar posterior position of the tibial tunnel with no significant tibial tunnel widening.
The surgical indications for meniscal root repair include acute traumatic tear of the meniscus with normal or near normal cartilage with minimal radiographic evidence of osteoarthritis, or a chronic symptomatic tear in a non-arthritic patient with the ability to comply with postoperative rehab protocol. Our patient fits into this second category.
Given the findings following evaluation of a detailed history, physical examination, and advanced imaging, the surgical plan for this patient was a lateral meniscus posterior root repair using the transtibial pull-out technique and a medial femoral chondroplasty. Intraoperatively, the integrity of the ACL graft will be evaluated to determine if repair or reconstruction is necessary.
Following diagnostic arthroscopy, the posterior root of the lateral meniscus was identified as torn. The probe identifies the proximity of the ACL graft to the lateral horn root attachment, and it was noted that the tibial tunnel likely violated the root, causing this iatrogenic tear at the time of the index surgical procedure.
ACL was noted to be stable, so the decision was made to leave the ligament in tact and avoid the risk of tunnel convergence.
A curette was then used to prepare the footprint for the meniscal root. An incision was made for the anterior medial tibia for bone tunnel entrance for transtibial pull-out tunnels. Using an aiming device, the first hole was placed into the meniscal footprint using a 2.4-mm drill. A second tunnel was then placed approximately 5-mm anterior to the first tunnel using an offset guide. The tunnels were visualized arthroscopically as seen here.
An arthroscopic canula was then placed in the medial portal. An arthroscopic suture passer was then used to place 2 sutures into the posterior lateral meniscal root. A Nitinol suture passer is then passed through the tibial drill tunnel and used to retrieve the sutures individually. A grasper is used to retrieve both the Nitinol suture wire and the suture passing through the meniscus, and the sutures are sequentially passed through the tibial bone tunnels.
When passing the suture, it is important to note that we pass the posterior-most suture through the posterior-most tunnel to avoid any tangling of the sutures during passing through the tibial tunnels.
The anterior-most suture is then passed through the anterior tunnel in a similar fashion.
As the sutures are pulled into their respective bone tunnels, the reduction of the meniscal root can be appreciated with care taken to not over-reduce the meniscal root.
The cannulas in the tibial bone are then malleted out as the suture is withdrawn from the tibia. Retractors are then placed through the open incision on the tibia, and the tibial cortex is visualized while the 2 sutures are tied over a button on the tibial cortex.
Final inspection within the joint reveals a well-reduced posterior horn lateral meniscus with 2 alternating-colored sutures dunking into their respective tibial tunnels. Postoperative imaging shows the position of the tibial button inserted on the tibial cortex.
Postoperatively, the patient should be kept non-weight bearing until 4 weeks postoperatively with the brace locked in extension and prescribed pain medications as needed. Rehabilitation should focus on increasing range of motion starting on postoperative day 1, with an estimated return to activities at 6 to 9 months.
Key pearls for this procedure can be seen here. Most notably, one should ensure to obtain parallel tunnel positioning to avoid tunnel convergence.
Risks and complications of an iatrogenic meniscal root repair include a repair failure, leading to a non-anatomical reduction of the meniscus, transtibial tunnel convergence with the posteriorly positioned ACL tunnel, and further iatrogenic damage caused by over-repair of the meniscus. In addition, long-term outcomes of repairs in a chronically unstable knee are suboptimal and may ultimately lead to the development of osteoarthritis and recurrent instability.
Outcomes of this technique have been previously described by LaPrade et al 5 in 45 patients undergoing the transtibial pull-out technique with minimum 2 years follow-up. The authors found significant improvement in Lysholm and WOMAC scores in patients aged both less than and greater than 50 with similar outcome scores in both groups, demonstrating the efficacy, effectiveness, and reproducibility of this surgical technique.
Although rare, iatrogenic damage to the meniscus caused by malposition cruciate ligament tunnels during reconstruction has been previously described in the literature for other types of meniscal root tears. Here, LaPrade et al 2 described a 2-patient case series of anterior horn, medial meniscal root avulsions due to malposition of the tibial tunnel as well as the subsequent successful treatment of this condition. These authors also described a similar presentation such as ours in which they treated a patient coming from an outside hospital who experienced a posterior lateral meniscal root tear following an ACL reconstruction due to a posteriorly placed tibial tunnel at the time of the index procedure. 3 However, this patient differed from ours in that they underwent a double-bundle reconstruction technique in addition to the meniscal repair to restore their previously placed ACL graft. During this technique, it is important to evaluate both the status of the cruciate ligament as well as the meniscus intraoperatively to determine the optimal course of treatment or surgical intervention without exacerbating the iatrogenic nature of the case.
We thank you for watching our technical description of the treatment of an iatrogenically caused lateral meniscal root tear from a previous ACL reconstruction using a transtibial pull-out technique.
Footnotes
Submitted August 16, 2022; accepted October 30, 2022.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical Approval
This study was exempt from ethical approval.
Informed Consent
Not applicable.
