Abstract
Background:
Concomitant cartilage injury is commonly associated with patellofemoral instability. While nonoperative treatment remains the gold standard for first time dislocators, there has been an increased trend toward addressing patellar instability when symptomatic cartilage disease is present.
Indications:
A healthy active 29-year-old woman >2 years of patellar instability and pain symptoms in the right knee. Imaging revealed tibial tubercle to trochlear groove (TT-TG) distance of 19.8 mm, and a Caton Deschamps Ratio of 1.54. Initial staging arthroscopy demonstrated a near full thickness cartilage defect of the lateral patellar facet measuring 2x2 cm.
Technique Description:
In the index procedure, a staging diagnostic arthroscopy is performed to evaluate the extent of the cartilage defect. Given the size of the lesion, a matrix-induced autologous chondrocyte implantation (MACI) biopsy is performed for later implantation. At the second stage procedure, a midline approach to the patella and tibial tubercle is performed. A 45° osteotomy is initiated with a cutting jig. The osteotomy is detached distally to allow for both anteromedialization and distalization to offload the cartilage defect and improve patellar articulation. The lateral patellar facet cartilage defect is prepared, and a combination of fibrin sealant and digital pressure is used to implant the pre-shaped MACI transplant. The osteotomy is then secured with 2 bicortical screws. A semitendinosus allograft is secured to the upper half of the medial border of the patellar and secured to its anatomometric point on the femur to reconstruct the medial patellofemoral ligament (MPFL).
Results:
Patient successfully returned to running and is currently working on return to other sports with no anterior knee pain or instability. Recent studies have demonstrated overall good clinical outcomes following MACI for patellofemoral lesions. Addressing underlying bony deformity and offloading patellofemoral cartilage lesions with tibial tubercle osteotomy in combination with MPFL reconstruction has improved patellar stability and good patient satisfaction.
Discussion/Conclusion:
Combined tibial tubercle osteotomy, MPFL reconstruction, and MACI in a comprehensive approach can successfully address symptomatic patellofemoral cartilage disease in the setting of patellar instability with underlying bony abnormalities.
This is a visual representation of the abstract.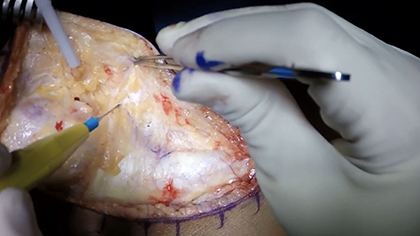
Keywords
Video Transcript
In this video, we are going to demonstrate a technique for combined anteromedialization tibial tubercle osteotomy with distalization, an medial patellofemoral ligament (MPFL) reconstruction, as well as a matrix-induced autologous chondrocyte implantation (MACI) for the patella for a large lateral facet lesion.
The author disclosures are listed here.
The following topics will be covered in this video.
The patient is a 29-year-old woman with a history of recurrent left patellar instability and pain. She had a total of 5 previous dislocations. She had progressive pain that prevented her from participating in physical activity and persisted despite adequate conservative treatment. Her examination is notable for positive patellar grind and patellar apprehension. Her hip range of motion is normal without suggestion of significant femoral anteversion. Her plain radiographs showed significant lateral tilt and patella alta with a Caton-Deschamps index (CDI) of 1.54. Her magnetic resonance imaging (MRI) demonstrates a 20 mm cartilage lesion of the lateral patellar facet, as well as increased tibial tuberosity-trochlear groove distance of nearly 20 mm.
Given the significant pain and cartilage defect seen on MRI, a diagnostic arthroscopy as a part of a planned first stage index procedure. Under anesthesia, it was noted that the patient had significant lateral patellar tracking and inability to evert the patella to neutral. A 2 x 2 centimeter squared nearly full thickness cartilage defect was noted on the lateral patellar facet. Given the size of the lesion, a cartilage biopsy was performed for future MACI implantation.
Based on the patient’s clinical symptoms, physical examination, and findings at the diagnostic arthroscopy, she was determined to have a symptomatic cartilage lesion in the presence of persistent patellar instability.
We aimed to address the cartilage lesion with the MACI transplant and addressing the patellar instability with a combined tibial tubercle osteotomy and MPFL reconstruction. A lateral lengthening was required due to the tight lateral retinacular structures and need to medialize the tubercle. We aimed to both medialize and anteriorize the patellar by approximately 10 mm using a 45° angled cut, as typically 1 cm of anteriorization is needed to offload the patellofemoral joint. 1 Distalization was also needed given the elevated CDI, which is typically considered when the CDI index is above 1.4. 2
The patient was positioned in the dorsal lithotomy position on a regular operating table. We used a nonsterile thigh tourniquet, as well as tranexamic acid, to reduce bleeding intraoperatively.
A central incision was made extending from the tibial tubercle to the superior pole of the patella. Medial and lateral soft tissue flaps are required for the lateral lengthening, as well as our medial approach.
The anterior compartment was dissected off the proximal tibia to expose the bone for the initial tibial tubercle osteotomy. This was done initially with bovie and then with elevator to elevate off the soft tissue off the posterior aspect of the tibia to place our retractor.
An alignment guide was attached. A 45° angled guide was secured with 3 breakaway pins. We start off distally and then work proximally with the pin, and then add the centrally threaded pin to fully seat the cutting guide. Here we are checking to make sure we have an adequate cut and that we are not too deep. You will see here with the saw we penetrate the cortex close to the outer cortex proximally. Distally we will go all the way through, but the key is that we are not coming out the posterior cortex to prevent any damage and reduce the fracture risk. We will now do our diamond cut with the saw. Given this is a distalization, we will completely remove the tubercle and then do shortening of the tubercle osteotomy. The proximal cut is again a diamond cut here: we extend down but do not go through the posterior cortex, and then we turn horizontally and make our way toward the previous cut where we had come out more distally. Here you can see the osteotomy is easily mobile and can be easily distalized and moved.
Given the severely tight lateral retinaculum, we opted to perform a lateral lengthening. The 2 layers of the lateral retinaculum are then carefully divided, and the deep layer is cut as far posteriorly as possible. After anteromedialization, the 2 layers will naturally glide to their appropriate length and can be secured with interrupted absorbable sutures.
Here we are working toward the MPFL. We are rongeuring the medial side of the patella. We are placing our first central anchor, which were 2.6 knotless all suture anchors. After confirming adequate placement, we placed a second one more superiorly.
Here we are preparing the lateral facet lesion for the MACI. These are preset cutting guides that make it easier to prepare the base of the lesion. The key is to go down to the calcified cartilage layer and no deeper, and we use a combination of multiple different curettes to remove any of the cartilage. In the patella, the cartilage is quite thick in certain areas, so it is important to take your time.
This patient had a small bone cyst, so we curetted it out and used autograft from the tubercle osteotomy site. We packed this in, and we cleaned out the area for the MACI transfer.
Following this, this is the MACI transfer preparation. You want to keep the corner portion in the bottom left-hand side with the cells up. Here the fluid is transferred to keep the graft moist and we are using the cutting guide. We also put a little fluid into a small specimen cup top. Here we are laying the cutting guide on there, malleting down, making sure not to damage any of the MACI implant. Following this we will place it and again the rough side is still up the entire time. We are placing fibrin sealant and we are impacting this to make sure there’s no bleeding as too much bleeding may prevent the implant from sticking to its recipient site.
The tourniquet is down at this time point. We then flip the MACI implant and now the rough side is facing down, and the shiny side is up. We gently lay it on there and place another round of fibrin sealant. And then we gently apply manual digital pressure for 3 minutes to secure the transplant.
Following this, we turn our attention back to the tubercle osteotomy for the distalization.
We measure and cut the small piece of bone, which will be used for bone graft at the osteotomy site when we distalize. We have also medialized and anteriorized this patient’s tubercle to address the lateral tracking and also offload the cartilage lesion. Once we are happy with our correction, we place a single out of plane pin, and then place 2 pins for our cannulated screws.
In this patient no washer was needed for the distal screw as we had excellent fixation. The more proximal screw we used a washer.
We are filling the osteotomy site with putty to prevent further bleeding in the area in addition to improving healing. We are measuring and checking after final tightening to make sure we brought the tubercle and patella down, as they had significant alta. We then range the knee and confirm good range of motion and good fixation, and you can see that the patella has appropriate tracking. We will then check our MACI implantation to make sure there is no further delamination; here it’s in a good position. We are taking a small portion of the tubercle osteotomy medially to prevent overhang; in some cases, we get a larger fleck that we can use as bone graft.
Finally, we return to the MPFL. Here we are locking these knotless anchors. There’s a small learning curve to this implant, but provides very fast and effective fixation for your MPFL reconstruction. You can see here how it nicely cinches down the semitendinosus allograft. Here you can see further cinching down of the knotless anchors. There is excellent fixation and we have had no issues with pullout. We dissect out and pass the free limbs of the graft between layers 2 and 3. We found our Schottle’s point under x-ray which is not shown here. We then tie off separate limbs of the semitendinosus allograft so we can confirm and sequentially tighten each one. We then pass this through our femoral tunnel, and we check isometry and make sure the graft does not tighten in flexion. We want less than 2 quadrants of mobility, but we also do not want to over constrain the knee. Here we are placing a PEEK screw at around 40° of flexion. You can see here we have less than 2 quadrants of mobility, and then we will close the lateral retinaculum as described previously.
Postoperatively, we restrict weight bearing for the first 6 weeks after surgery. Passive motion is initiated to 45° for the first 2 weeks postoperatively, and range of motion is increased to 90° by 6 weeks. We expected patients to return to sport by 6 to 9 months after surgery.
While outcomes following early generation ACI are more robust, outcomes for MACI transplants are limited, particularly in the patellofemoral compartment. Ebert et al evaluated 47 patients with patellofemoral cartilage defects who underwent MACI transplantation and found significant improvements in all patient reported outcome measures at 2 year follow up. Surveillance MRI scans demonstrated significant graft infill, and more than 85% of patients had satisfactory results.
Given the relative paucity of literature regarding appropriate rehabilitation following MACI implantation, a group of U.S. orthopedic surgeons came together to establish consensus guidelines regarding postoperative protocols. Greater than 75% consensus was established for time to weight bearing and range of motion. However, no specific guidelines established for return to activities of daily living, work, and sports.
Some notable complications associated with the procedures are listed here and include nonunion, fracture for the tubercle osteotomy, graft failure for MACI, and recurrent instability, arthrofibrosis, patella fracture for MPFL reconstruction.
Our references can be found here.
Thank you.
Footnotes
Submitted December 30, 2021; accepted February 24, 2022.
One or more of the authors has declared the following potential conflict of interest or source of funding: A.E.W. received education and hospitality support from Arthrex, Stryker, Smith & Nephew, Medtronic, Micromed, DePuy Synthes, Team Makena, and Wright Medical Tech. G.F.R.H.III. is a paid consultant for Arthrex; received non-consulting services, travel and lodging support from Arthrex; and received food and beverage support from Micromed and Smith & Nephew. F.A.P. received IP royalties support from Exactech, Inc; and is a paid presenter or speaker for Stryker. J.N.L. is a board or committee member for AANA and ASES. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
