Abstract
Background:
Achilles tendon ruptures occur most commonly in male individuals aged between 30 and 60 years.
Indications:
Surgical options for treatment of acute midsubstance Achilles tendon ruptures in the athletically active population include open, mini-open, and percutaneous techniques.
Surgical Technique:
The giftbox suture configuration has been popularized by multiple authors. Here, a modified giftbox technique for Achilles tendon repair is shown in detail and uses nonabsorbable suture loops, a novel method for primarily repairing complete Achilles tendon ruptures.
Results:
This mini-open technique has demonstrated, at a minimum of 1-year follow-up, outcomes that are comparable with previously reported Achilles tendon repair procedures with no re-ruptures and low overall complication rates in the first 60 patients who have undergone this procedure. The mean time to release to unrestricted activity following repair by this technique is 24.3 weeks, which is earlier than most standard techniques.
Conclusion:
Achilles tendon repair using the modified gift box technique with nonabsorbable suture loops is a safe and reliable technique for repair of midsubstance tendon ruptures in athletically active patients. The mean time to release to unrestricted activity following repair by this technique is earlier than most standard techniques.
This is a visual representation of the abstract.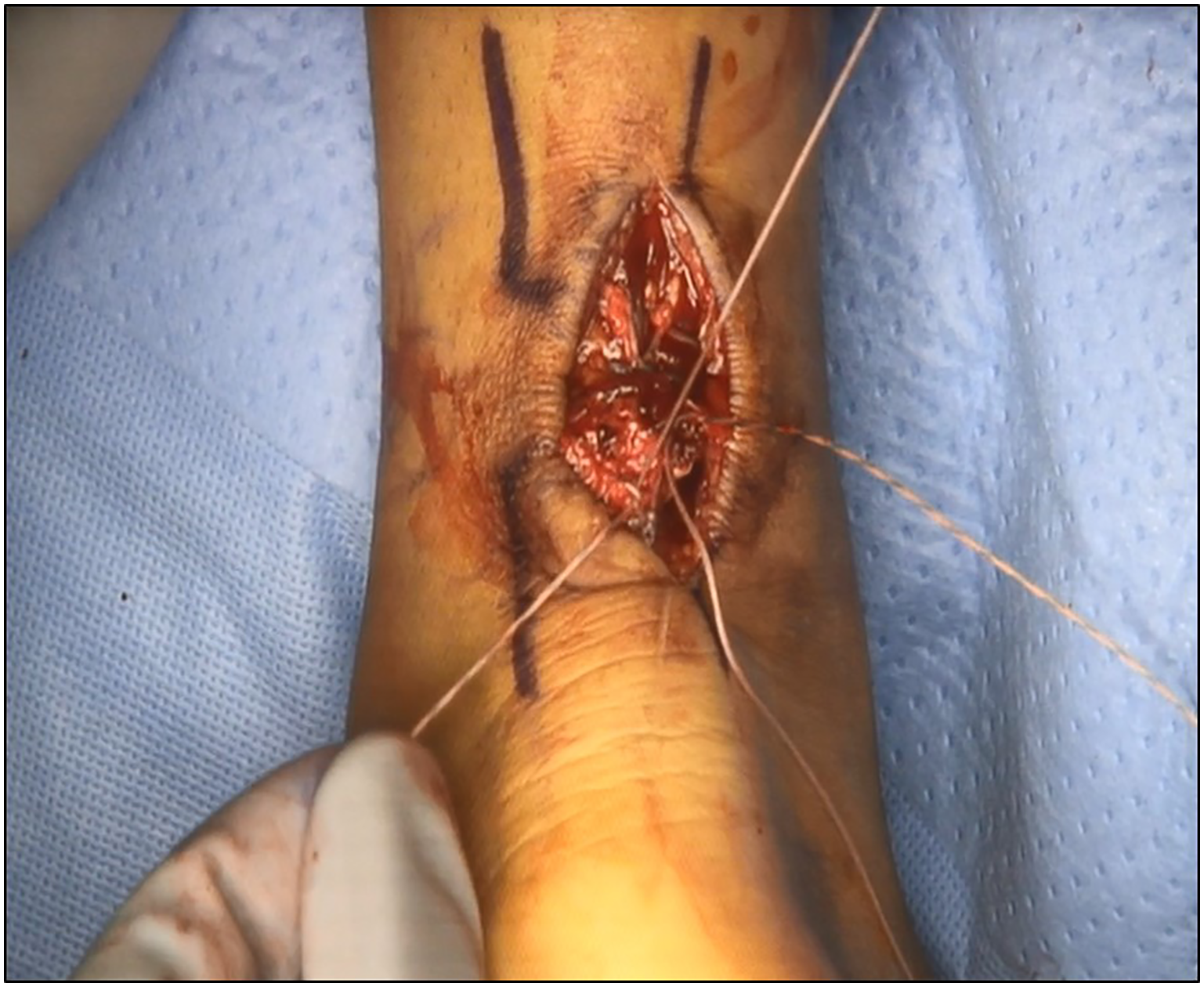
Video Transcript
Here, we present an Achilles tendon repair using the modified giftbox technique with nonabsorbable suture loops. It has been demonstrated to be a safe and reliable technique for repair of midsubstance tendon ruptures in athletically active patients. Among the first 60 patients who have undergone this technique, the mean time to release to unrestricted activity following repair was 24.3 weeks, which is earlier than most standard techniques.
The patient is a 35-year-old man who was running up a “warp wall” for American Ninja Warrior practice when he felt a pop in the posterior aspect of his ankle. He was unable to actively plantarflex his ankle and had difficulty with ambulation due to pain. His activity goals were to return to the same level of activity, including Ninja Warrior training.
End-to-end repair is the gold standard for acute midsubstance Achilles tendon ruptures. There are multiple techniques that have been described for repair, including Krackow, Bunnell, Kessler, triple bundle, percutaneous, and giftbox suture configurations. The indications for the use of this technique are all acute midsubstance ruptures in athletically active individuals. Contraindications include patients with poor healing potential, compromised overlying soft tissue, and distal avulsion tears from the calcaneus.
The technique you are about to see was described in Techniques in Orthopedics in 2015 and has been modified slightly to decrease the size of the incision and the type of the suture used. The modification of the gift box technique was developed by the senior author. The patient is placed under general anesthesia and placed prone with all bony prominences padded. A Thompson test is performed, and as can be seen, as the calf is squeezed there is minimal to no plantarflexion of the ankle. The injured side is then compared with the uninjured side where there is brisk plantarflexion with calf squeeze. This constitutes a positive Thompson test.
A longitudinal incision is made centered just proximal to the palpable gap in the tendon. Careful dissection is taken down through the soft tissues to expose the paratenon, which is then sharply incised to expose the underlying torn tendon. Here, you see the 2 tendon stumps being brought out through the incision site. We will now debride the 2 tendon stumps, removing approximately 1 to 1.5 cm of damaged tissue from each of the tendon stumps.
Keep in mind that the ideal position for the incision is slightly proximal to the palpable defect. We now sharply remove the most distal portion of the proximal stump to freshen it back to healthy tissue ideal for healing. The same debridement is performed on the distal stump in preparation for repair.
Once debridement is completed, we use the continuous loop of nonabsorbable suture to pass over the tendon stumps and then use a Keith needle to repeatedly pass the suture through the tendon. Starting with the proximal stump, we then weave the suture repeatedly through the tendon, removing the slack from the suture as we do this. Once 3 to 4 passes have been made through the tendon, the suture loop is then cut to create the free ends of the suture which are now locked and passed through the tendon end.
We then remove the clamps and test our fixation, showing very strong and very stable fixation within the tendon. We then repeat the same steps on the distal tendon stump, weaving a different colored suture through the tendon repeatedly and then locking it on the final pass and passing the tails out of the end of the tendon stump into the tear site. We have now created a medial and lateral suture tunnel down the longitudinal axis of each tendon stump.
The sutures have been passed and then exit into the tear site as seen; care is taken not to sever the sutures. We will then perform a giftbox repair by passing the tails of these same sutures across the opposite tendon stump through the suture tunnels that have been created using the suture loop (Figure 1). This can be done using either the straight Keith needle or a curved free needle as you are seeing here. The sutures are brought out proximal and distal to the suture construct. This minimizes the risk of severing the suture with the needle by passing it straight down the suture tunnel. We then repeat these same steps on the opposite tendon stump proximally.

The modified giftbox Achilles tendon repair is performed by passing suture from the distal tendon stump through the suture tunnels in the proximal tendon stump prior to tying the suture.
Once all sutures are passed, we place the ankle in maximal plantarflexion and tie secure knots to secure our initial fixation both proximally and distally. We now repeat the Thompson test, showing that there is clear appropriate tension and clear plantarflexion taking place as the calf is squeezed. We then reinforce the repair by taking the same sutures and passing them back across the tear site and tying them securely to create a total of 6 strands of nonabsorbable suture passing across the tear site with no knots within the tear site, which could reduce the surface area for healing. This also allows the knots to lie more flat, decreasing the irritation from the knots being applied from the repair.
Once all sutures are tied, we perform a final Thompson test confirming appropriate tension on the tendon. We then thoroughly irrigate the wound and close the paratenon in a water-tight fashion with absorbable suture. We then close the skin in a subcuticular fashion with Biosyn suture and apply a soft dressing with a posterior sugar-tong splint in approximately 30° of plantarflexion.
The patient is made non-weightbearing for 2 weeks in the splint. They begin weightbearing as tolerated in a Controlled Ankle Motion (CAM) boot with 3 heel lifts in it. One heel lift is removed each week beginning at 3 weeks. By 6 weeks, the CAM boot is discontinued by weaning out gradually. The ankle is not allowed passive dorsiflexion beyond neutral for a total of 3 months postoperatively. Athletes are allowed to return to running when their midcalf circumference is at least 80% of the uninjured side and when they can perform sustained single-leg heel raises for greater than 30 seconds. Athletes are cleared to return to sport when they are able to run for 10 minutes without a limp.
The indications for use of this techique are all acute midsubstance ruptures in athletically active individuals. Contraindications include patients with poor healing potential, compromised overlying soft tissue, and distal avulsion tears from the calcaneus.
Pearls for success with this technique:
Make the incision slightly medial to midline to avoid damage to the sural nerve.
Make the incision more proximal than you think is necessary to access the proximal tendon stump. The distal stump can always be brought into the surgical field with passive plantarflexion.
Create full-thickness soft tissue flaps through the paratenon to minimize the risk of wound healing complication.
Tension the repair in maximal plantarflexion as the tendon will elongate during the rehabilitation process.
Close the paratenon in a water-tight manner.
The results of this technique in the first 60 patients who underwent this procedure have shown no re-tears and overall high rates of return to sports within 6 to 9 months. Previous biomechanical studies of repairs using the giftbox technique have shown superior results compared with Krackow and Bunnell techniques regarding single load to failure and cyclic loading. Additional benefits of the modified giftbox technique is its ability to tubularize significantly frayed tendon tissue, create suture tunnels to decrease the risk of sutures being cut during passage, and apply 6 strands of nonabsorbable suture across the repair site with no knots within the tear site.
Thanks to the staff at the Ohio State University Wexner Medical Center and the Jameson Crane Sports Medicine Institute and Dr Eric Welder for their assistance in creating this video.
Footnotes
Submitted November 14, 2020; accepted January 14, 2021.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
