Abstract
Background:
Traumatic anterior glenohumeral instability is a commonly encountered shoulder pathology among young active patients. Nonoperative management and arthroscopic techniques are associated with high rates of reoccurrence, particularly in patient populations with known major risk factors.
Indications:
The coracoid process transfer (Latarjet procedure) is typically reserved for cases of anterior glenohumeral instability where glenoid deficiency exceeds 20% to 25% or when soft tissue stabilization techniques have failed.
Technique Description:
We use a standard open deltopectoral approach. The coracoid process is exposed and released from the pectoralis minor and coracoacromial ligament. An osteotomy is performed using an oscillating saw and completed with an osteotome to harvest the bone block, leaving the conjoint tendon intact. Soft tissue is cleared from the graft, and it is predrilled/measured. We use a subscapularis splitting technique to access the joint and expose the anterior glenoid. All bony surfaces are prepared. We drill into the glenoid at the premeasured offset. The graft is provisionally fixed into place with K wires, then secured with 2 parallel cannulated screws. The capsule is repaired to make the graft extraarticular. The subscapularis split is repaired in addition to standard closure.
Results:
The Latarjet procedure is very successful for restoring stability. Rates of recurrent dislocation range from 0% to 10% across various studies, and revision rates are as small as 3%. This is much lower than those seen following soft tissue stabilization, particularly in high-risk patient populations. Patient reported outcomes show good function and high rates of return to sport. Complication rates are generally higher, with some studies reporting up to 25% incidence. Musculocutaneous and axillary nerve injuries may occur, and graft overhang can lead to glenohumeral arthritis. Certain complications are unique to the procedure, including graft lysis, coracoid fracture, nonunion, and hardware issues.
Discussion/Conclusion:
The Latarjet procedure is very useful in cases of anterior glenohumeral instability with significant glenoid bone loss or following failed soft tissue stabilization. Its utilization may continue to grow in future years as technique innovations develop and surgical indications expand.
This is a visual representation of the abstract.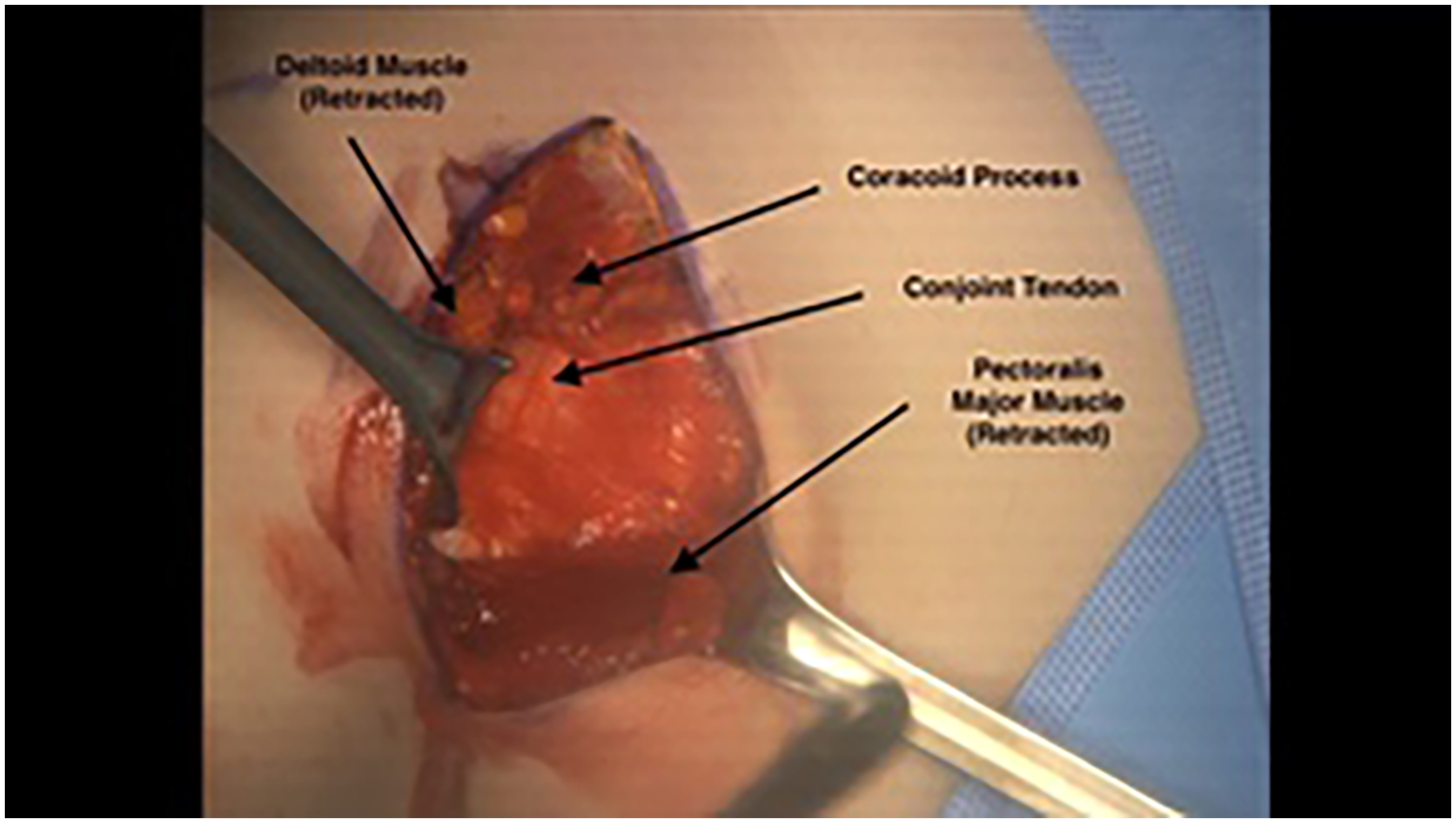
Video Transcript
Open shoulder stabilization: the Latarjet procedure. Presented by the authors below in the Sports Medicine division at the Ohio State University in Columbus, Ohio.
There are no relevant disclosures or conflicts of interest.
A representative case is presented. This involves a 20-year-old man who was a college football player. He suffered a traumatic anterior shoulder dislocation that was initially treated nonoperatively. After recurrent dislocations over several years, he presented to our clinic. His physical examination is notable for full range of motion and strength of the affected shoulder. He was neurovascularly intact with positive apprehension test and no generalized ligamentous laxity.
Preoperative imaging is shown here. Radiographs were largely unremarkable other than a small Hill–Sachs lesion. The axial CT as well as the 3D reconstruction show anterior glenoid bone loss of roughly 25%. See the pertinent references for more detail on how this calculation was performed.
At this point, the options available to this patient are conservative management including therapy and activity modification. For surgery, we can consider arthroscopic versus open Bankart repair, but this will have a high rate of reoccurrence. Bony procedures are possible as well including glenoid autograft/allograft or a coracoid transfer (also known as the Latarjet procedure).
In high-risk patient populations, nonoperative and arthroscopic management have high rates of reoccurrence. This patient meets nearly all criteria with his young age <20 years, male sex, contact athlete, and glenoid and humeral sided bone loss. Bony procedures provide an extra element of stability. The Latarjet procedure has traditionally been used when glenoid bone loss exceeds 20% to 25% or when soft tissue stabilization surgeries have failed. However, indications have slowly been expanding in recent years.
Some contraindications for the Latarjet procedure include uncontrolled seizures. The retained conjoint tendon attachment can lead to catastrophic failure if firing too forcefully. Instability due to irreparable rotator cuff tears would be better served with other procedures, and the Latarjet is not used with instability in the setting of prior arthroplasty. There are high failure rates seen among voluntary dislocators and with microinstability as well. Given the degree of his bone loss, as well as his high-risk patient characteristics, this patient elected to proceed with the Latarjet procedure.
For preoperative planning, some important equipment to have available include a sagittal saw, osteotomes, burrs, and a standard open shoulder set. We elect to use 4.0 mm cannulated screws rather than solid. Each has its risks and benefits, with cannulated screws having slightly higher risk of hardware failure but they allow for more K-wire trajectory control and minimize graft migration. The literature has shown increased failure rates with 1 screw versus 2 and with divergent rather than parallel trajectory.
Patients are offered an interscalene block preoperatively. We use a modified beach-chair setup using an arm positioner as seen here. The upper extremity is prepped and draped in a standard sterile fashion.
For the procedure, we use a standard deltopectoral approach to the shoulder. We begin by identifying the coracoid process and drawing out our planned incision as seen here. Incision is made through skin and carried through subcutaneous tissues using a combination of blunt dissection and electrocautery. For brevity’s sake, we will largely skip this well-known approach in this video and highlight the key portions of the procedure beyond that.
Seen here is the superficial interval. The cephalic vein is retracted laterally along with the deltoid muscle. The pectoralis major muscle is retracted medially to expose the conjoint tendon, which is composed of the short head of the biceps as well as the coracobrachialis.
The lateral border of the conjoint tendon is identified, and sharp dissection is used to elevate the clavipectoral fascia. Here you can see us completing that interval with Metzenbaum scissors. Shoulder abduction and external rotation can improve visualization here.
The lateral dissection is completed by detaching the coracoacromial ligament superiorly. We leave a 1-cm cuff of tissue for later repair.
Next, we detach the pectoralis minor tendon medially. The dissection should stay along bone. Shoulder adduction and internal rotation will further protect the musculocutaneous nerve during this portion. We then place a curved retractor medially.
Our standard is to use a 2-cm graft, so we will mark that level out from the distal tip as seen here. A larger graft is better if possible, but it is important to ensure that you stay anterior to the coracoclavicular ligaments when choosing your osteotomy site.
We avoid using an osteotome alone especially in larger, more muscular patients where getting the appropriate angle can be difficult. The osteotomy is started with an oscillating saw. We use a nitrous hose for more control, and the cut is finished with an osteotome.
Grab the coracoid with a kocher clamp, and use a bovie to separate it from its soft tissue attachments posteriorly. Make sure to leave the conjoint tendon intact distally. This will maintain the vascularity of the graft. In addition, the conjoint tendon provides a sling effect, adding a soft tissue component to the so-called triple effect of glenohumeral stability that the Latarjet procedure provides.
Next, we will prepare the graft. The inferior surface of the coracoid is exposed. An oscillating saw is used to remove a small sliver of bone to flatten it, a bovie is used to clear off any remaining soft tissue, and a high-speed burr is used to create a bleeding bony surface that promotes healing.
The coracoid drill guide is placed into appropriate position grasping medial and lateral. The guide allows 2 parallel 3.2-mm drill holes to be placed centrally and separated by 1 cm. Make sure to protect your soft tissues while drilling. The pilot holes are measured with depths noted for steps later on.
To ensure flush graft placement, the offset is measured from the center of each drill hole to the lateral coracoid edge, which will be aligned with the articular surface of the glenoid in later steps.
Electrocautery is used to clear off the superior edge drill holes for easier screw placement down the road. The graft is released and tucked away.
Next, we proceed to the glenohumeral joint exposure. This is done in external rotation to place the subscapularis tendon on stretch. We use a subscapularis split approach. Benefits include less fat atrophy and greater strength preservation compared with the alternative tenotomy technique. However, visualization can be limited through this small exposure, so great care needs to be taken to ensure correct graft placement.
The superior and inferior borders of the muscle are palpated. The split should be through the intersection of the inferior and middle fibers (around the inferior 1/3 line). We start by marking out the incision with a bovie and then proceeding with a knife. The plane is developed bluntly.
A Gelpi retractor opens the interval, and a broad Hohmann retractor is placed along the anterior glenoid neck to gain exposure.
The capsular incision should be about 1 cm medial to the glenoid rim to leave enough length for later reattachment. We make our incision in the superomedial corner. After that, a tag stitch is placed for traction.
A Fukuda retractor is placed laterally inside the split. With this exposure, the superficial retractors can be removed as visualization should be adequate at this point. We then complete the capsulotomy with a bovie. Aggressive inferior dissection or prolonged retraction should be avoided to minimize risk of axillary nerve palsy.
A rongeur is used to remove any remaining soft tissue from the anterior glenoid neck. Then, after placement of a superior retractor, a burr can stimulate bony bleeding for potential healing. No major bone stock should be removed during these steps. This completes the glenohumeral exposure.
A guide is used based on the offset measured earlier on the coracoid graft. The guide will be aimed roughly 10° medially to ensure there is no screw penetration into the joint. This fits into the safe zone of the suprascapular nerve as well.
The bottom hole is drilled first. This is taken through the posterior cortex. The guide is removed, and the distance is measured.
The coracoid graft is retrieved. It is inserted onto a K wire, which is threaded into the drilled hole. We aim to cover roughly from the 2 o’clock to the 5 o’clock position on the glenoid face. As mentioned previously, we use the originally described technique with the prepared inferior surface of the coracoid in direct contact with the glenoid neck.
A cannulated 4.0-mm screw with a washer is inserted over the guidewire based on the measured depth. This is added to the premeasured thickness of the coracoid graft.
We have found that the superior screw is consistently 2 mm shorter than the inferior screw, so we do not measure this time. The process is repeated. Longer screws (especially superior) are shown to increase the risk of suprascapular nerve injury at the spinoglenoid notch.
To prevent malrotation, we will sequentially tighten each screw and hold the graft in place. You must avoid overtightening the screws as well to avoid damage to the graft.
Once both screws are tightened, the K wires may be removed. This completes the graft placement portion of the procedure. The lengthening of the articular arc represents the bony portion of the glenohumeral stability triple effect. Ensure that there is a smooth joint surface with no overhang to minimize the risk of future glenohumeral arthritis.
The closure is extremely important in this case as well, because many of these patients will have a patulous capsule from repetitive dislocations. To set optimal tension, the arm is adducted and at roughly 45° of external rotation. The previously tagged capsule is shifted superiorly and medially and attached to the coracoacromial ligament. This ligament effect provides the third and final component of the triple blocking effect of the Latarjet procedure.
The capsule is also sutured into the native glenoid. This is a modification of the originally described procedure that makes the graft an extra-articular structure. This avoids any potential abrasive contact between the graft and the humeral head articular cartilage.
Retractors are removed, and the subscapularis split is reapproximated with heavy braided suture. Standard closure is carried out after this point.
The patient’s postoperative imaging is shown here. He is doing well and progressing as expected postoperatively.
The traditional critique of the Latarjet procedure has been higher complication rates, ranging from 10% to 25% based on the study. Rates of residual apprehension, stiffness, and reoccurrence are rare compared with soft tissue stabilization. Coracoid fractures are an unusual but devastating complication seen in the early postoperative period. Some complications are expected with any bony fixation such as graft nonunion, graft lysis, and hardware issues. Uniquely, overhang of the graft has been shown to lead to glenohumeral arthritis. Rates are low and most cases are self-limited, but musculocutaneous and axillary nerve palsies can occur at different points during the procedure. Proper surgical technique can mitigate these risks.
With the subscapularis split technique, patients are placed into our institution’s accelerated protocol. In the first 4 weeks, we prohibit all active motion and passive internal rotation/adduction/extension to protect the graft. Rehabilitation in weeks 4 to 6 works to regain full motion. Weeks 7 to 12 are focused on strengthening. Patients are allowed to progress back to full activities of daily living in weeks 12 to 16.
Refer to our institution’s website or the above protocol for more information.
Patients can get back to noncontact sports at 4 months. Contact sports, including heavy lifting or bench press, can start at 6 months. Patients can begin light throwing at 4 months with a goal of return to full competition by 9 months.
Outcomes of the Latarjet procedure are generally very successful. Patient reported outcomes and functional scores are high. Rates of return to play approach 80%. Rates of reoccurrence are 5% to 10% with revision rates as low as 3%. The Latarjet procedure leads to less reoccurrence, less reoperation, better functional outcomes, and less range of motion loss in external rotation when compared with soft tissue stabilization. Some key points to make about indications as well are that outcomes after first time and recurrent dislocations are equivalent. However, a Latarjet procedure following a failed arthroscopic surgery leads to worse functional outcomes and more postoperative pain compared with a primary Latarjet.
References are shown below. A link to our institution’s standardized rehabilitation protocol is included as well.
Footnotes
Submitted September 24, 2021; accepted October 16, 2021.
One or more of the authors has declared the following potential conflict of interest or source of funding: G.L.C. received education payments from Smith & Nephew; received a grant from Arthrex; received travel and lodging payments from Medwest Associates; and received food and beverage payments from Zimmer Biomet. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
