Abstract
Background:
There are multiple ways of reconstructing the medial patellofemoral ligament (MPFL), including dynamic techniques that fix the graft to the adductor magnus tendon. We present this technique associated to an increasingly common surgery used as adjuvant in some patients with patellar instability, lateral retinaculum lengthening.
Indications:
Recurrent patellar dislocation with medial laxity and lateral tightness/lateral tilt.
Technique Description:
This is double bundle MPFL reconstruction with anterior tibialis tendon allograft. Both autograft or allograft may be used, with a minimum length of 15 cm. The graft is fixed to the proximal third of the patella, passing as a sling under the adductor magnus tendon where it is fixed with sutures and returns to the patella. The patellar fixation includes a 10 to 15 mm deep and 4 to 4.5 mm diameter tunnel in the proximal third with suture stitches to the soft tissues in the entrance of the tunnel, plus an anterior periostic tunnel for the second bundle in the proximal third of the patella fixed with suture stitches. Meanwhile, the lateral retinaculum is incised longitudinally into a superficial and deep layer, in order to lengthen it the desired length.
Results:
The expected outcome of the procedure is to have a stable patellofemoral joint, with patients that gain the lost function and may return to sport without recurrence of patellar dislocation.
Discussion/Conclusion:
This is a simple, cheap, and reproducible technique that corrects both medial laxity and lateral tightness for patients with recurrent patellar dislocation.
This is a visual representation of the abstract.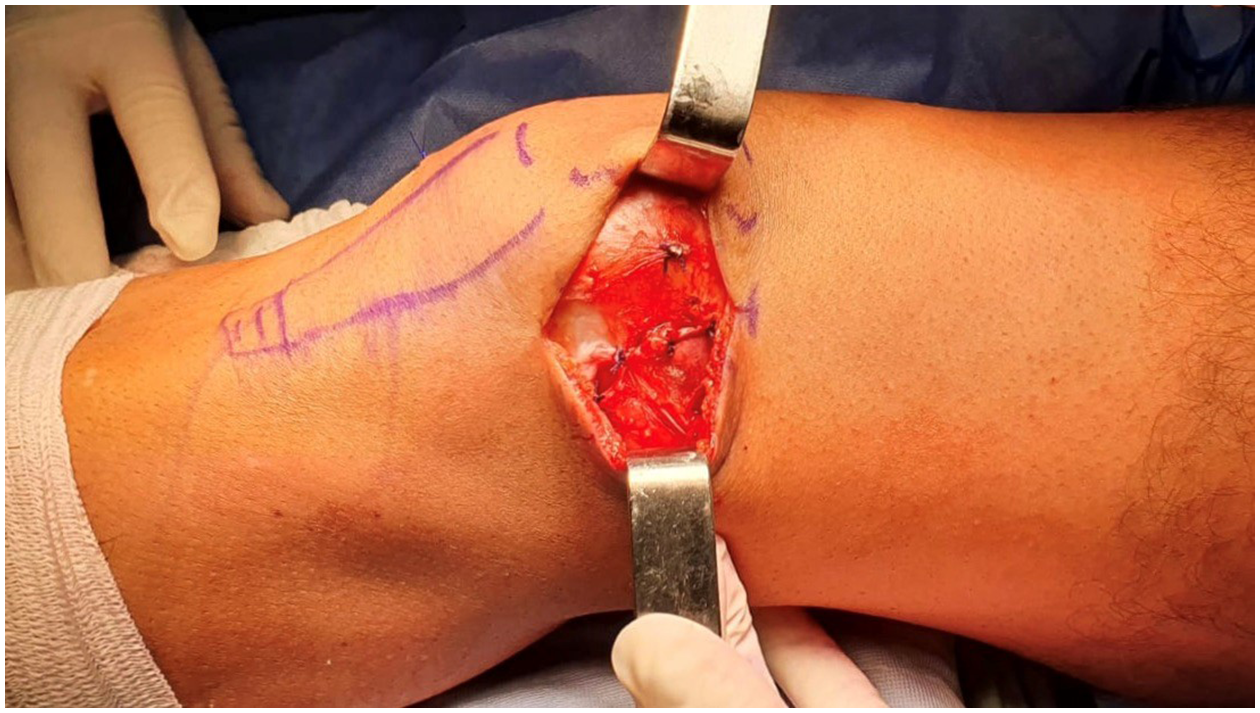
Video Transcript
There are multiples techniques to reconstruct the medial patellofemoral ligament (MPFL). We present a technique with 2 bundles, using anterior tibialis allograft, with soft tissue fixation in the patella in a bone tunnel and periostic tunnel, and soft tissue fixation in the femoral side, in a sling to the adductor magnus tendon. The indication is recurrent patellar dislocation associated to medial laxity and lateral tightness or lateral tilt. It is not indicated if there is lateral laxity.
In the video, we have a 22-year-old male patient with recurrent patellar dislocation in his right knee. He presented with mild effusion, complete range of movement, positive apprehension test, and negative J sign. This was the ideal indication, a patient with lateral tilt of the patella, lateral displacement of 2.5 quadrants and medial displacement of 0.5 quadrant. There was no malalignment or torsional deformities. The x-rays showed appropriate alignment, with mild trochlear dysplasia and patellar height in the upper limit of the normal range. Axial x-rays showed lateral tilt and magnetic resonance imaging (MRI) confirmed a shallow trochlea. Tibial tubercle (TT) and trochlear groove (TG) distance was 10 mm. These elements from the physical examination and images are key for the preoperative planning.
Under general anesthesia, with the patient in supine position, and after placing the tourniquet, we mark the patellar limits and test the movement in quadrants of the patella on either side. The ideal patient for this type of surgery has medial laxity of soft tissue structures and a tight lateral retinaculum.
The first incision is on the lateral border of the patella, longitudinal, approximately 5 cm in length. The dissection is gentle to expose the lateral retinaculum without damaging its fibers.
After identifying the lateral retinaculum, we dissect medially through this plane to have access to the medial border of the patella and use this same incision for the medial patellofemoral ligament reconstruction. The lateral retinaculum has to be separated from the subcutaneous tissues until it can be properly visualized, including the attachment to the iliotibial band. Following, the superficial and deep layers of the lateral retinaculum are separated. The first step is incising longitudinally the superficial layer with a scalpel just lateral to the patella. You may also use the scissors to dissect between the 2 layers. These layers should be separated very carefully to avoid breaking through any of them. The separation should be extended proximally and distally. This technique can be used regardless of patellar height and can be associated to tibial tuberosity osteotomies or trochleoplasty.
Finally, you have a clear separation of the 2 layers and you may incise the deep layer longitudinally, approximately 15 mm lateral from the initial incision, depending on how much you plan to lengthen. We usually preserve the capsular tissue under both layers. You can see how the original length of the retinaculum can be now modified as much as you have planned, depending on where you are suturing the flap to the superficial layer and the deep layer.
Now, the medial side of the patella is prepared, dissecting its proximal half. Next a guide pin is placed on the footprint of the MPFL, between the proximal and middle third of the patella, crossing it from medial to lateral. Fluoroscopy can be used to check the position of the guide pin. Care should be taken to avoid the articular surface.
Then, a 4.0-mm cannulated drill is used to make a 10 to 15–mm deep tunnel. A passing suture is left in this tunnel for passing the allograft latter on. Next, the femoral incision is localized over the adductor tubercle, slightly posterior to the medial epicondyle. A 2.5-cm longitudinal incision is performed, dissecting through the fascia that covers the adductor magnus tendon. Once the tendon has been identified, you pass a suture around it, as close as possible to the bone insertion, in order to fix it as close as possible to its anatomical insertion.
Then from the patellar incision, layer 2 for the medial soft tissues is identified and 2 passing sutures are passed through this layer. Later, these sutures will help to pass the 2 bundles of the allograft through layer 2, first toward the adductor tendon and then back to the patella.
The anterior tibialis tendon allograft is prepared mixing it with saline and vancomycin to decrease risk of infection. One of its ends should pass through the 4.0-mm tunnel in the patella, where it is passed and fixed to the periosteum and soft tissues surrounding the tunnel entrance. Then, the allograft is passed toward the adductor tendon, going around it and then back to the patella. The graft is fixed to the adductor magnus tendon with a single nonabsorbable stitch with the knee at 40° of flexion, with the graft tight, only enough to have it straight and avoid overconstraint to the patella from the medial side. The graft is returned now through the same layer 2 plane to the patella. Finally, we create a soft tissue tunnel through the anterior periosteum of the proximal third of the patella to fix the second bundle of the MPFL, with the knee between 30° and 40° of flexion, which is the flexion where it is most tensioned.
Next, the lateral retinaculum with the desired lengthening is sutured, around 10 to 15 mm with the knee at 40° of flexion, aiming for a medial displacement of the patella between 1 and 1.5 quadrants. At the end of the surgery, you can see how the medial displacement has increased and the lateral displacement decreased, with a patella that is stable in both directions.
Regarding potential complications, you do not want to drill through the articular cartilage of the patella. Then, you have to be sure of the direction of the guide pin, checking for its exit point in the lateral side. Using fluoroscopy will help to avoid this problem, especially for the first cases. Another potential complication is to incise the lateral retinaculum in all its width when splitting the superficial and deep layers. For this, you may create a flap from the superficial or posterior layer to complete the lengthening.
The postoperative management for the first days includes a soft bandage to promote some movement, partial weight bearing, movement as tolerated, and isometric strengthening. One month after, the patient should be able to do full weight bearing, at least 90° of knee flexion, proprioceptive, and strengthening exercises. Full range of movement is aimed between the first and second month, and return to sports after 4 to 6 months.
The adductor sling technique, has shown very good functional outcomes and low recurrence of dislocation, as reported in the case series of Arendt, who originally described this kind of technique with semitendinosus or gracilis graft. There are other similar ways of doing a MPFL reconstruction in the soft tissues, for skeletally immature patients or adults. Sillanpää et al showed that a tenodesis can be made with the adductor magnus tendon to the patella. Gomes compared the sling with the adductor tendon transfer finding similar good results in function, with no recurrence in either group and higher return to sport for the sling group. This type of MPFL reconstruction has shown to be very similar to the native ligament in terms of patellar contact pressures in a finite element model, and has shown very good functional results, similarly to an anatomical technique. Meanwhile, the lateral retinacular lengthening has shown less medial instability, less quadriceps atrophy, and better clinical outcomes at 2 years compared with lateral retinacular release.
Footnotes
Submitted January 31, 2021; accepted April 11, 2021.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
