Abstract
Background:
Posterior glenoid bone loss occurs in more than two-thirds of patients with posterior glenohumeral instability, with 14% to 22% having greater than subcritical bone loss (13.5%), a marker for potential need for bony augmentation versus soft tissue-only procedures. Several techniques are described to augment either the version or volume of the glenoid surface including osteotomies, autograft transfers, and allograft tibia transfers.
Indications:
Arthroscopic-assisted allograft distal tibia bone block augmentation to the posterior glenoid is indicated for revision posterior instability procedures with posterior bone loss and in primary cases of posterior instability with critical bone loss.
Technique Description:
Arthroscopic posterior glenoid reconstruction with allograft distal tibia and posterior labral repair in the lateral position is presented. This technique uses standard instrument sets and requires no patient repositioning. The preplanned tibial bone block is prepared on a back table either prior to, or concurrently with, arthroscopic procedure. After creation of high posterior portal and standard anterior portal, a sucker-shaver and burr are used to create a perpendicular edge for apposition of the allograft tibia. The bone block is introduced through a longitudinal incision and underdelivered to the prepared surface under the liberated labrum. The articular surface of the graft and glenoid are aligned and cannulated screws are used to compress the bone block against the native glenoid. The posterior labral tissue is then mobilized over the graft and repaired to the native glenoid.
Results:
Arthroscopic distal tibial allograft augmentation for posterior bone loss restored stability and function in a small cohort of patients. Patients reported improved stability in the immediate postoperative course, with restoration of motion by 2 months. Push-ups, pull-ups, and return to full active duty without restrictions is allowed at 6 months postoperatively. Imaging at 3 months postoperatively has shown excellent graft healing.
Discussion:
The benefits of allograft tibia augmentation for posterior instability with glenoid bone loss include an anatomic joint surface restoration including articular cartilage, lack of donor site morbidity, and a minimally invasive approach. When performed arthroscopically, this technique permits concurrent posterior labral repair and anatomic reconstruction.
This is a visual representation of the abstract.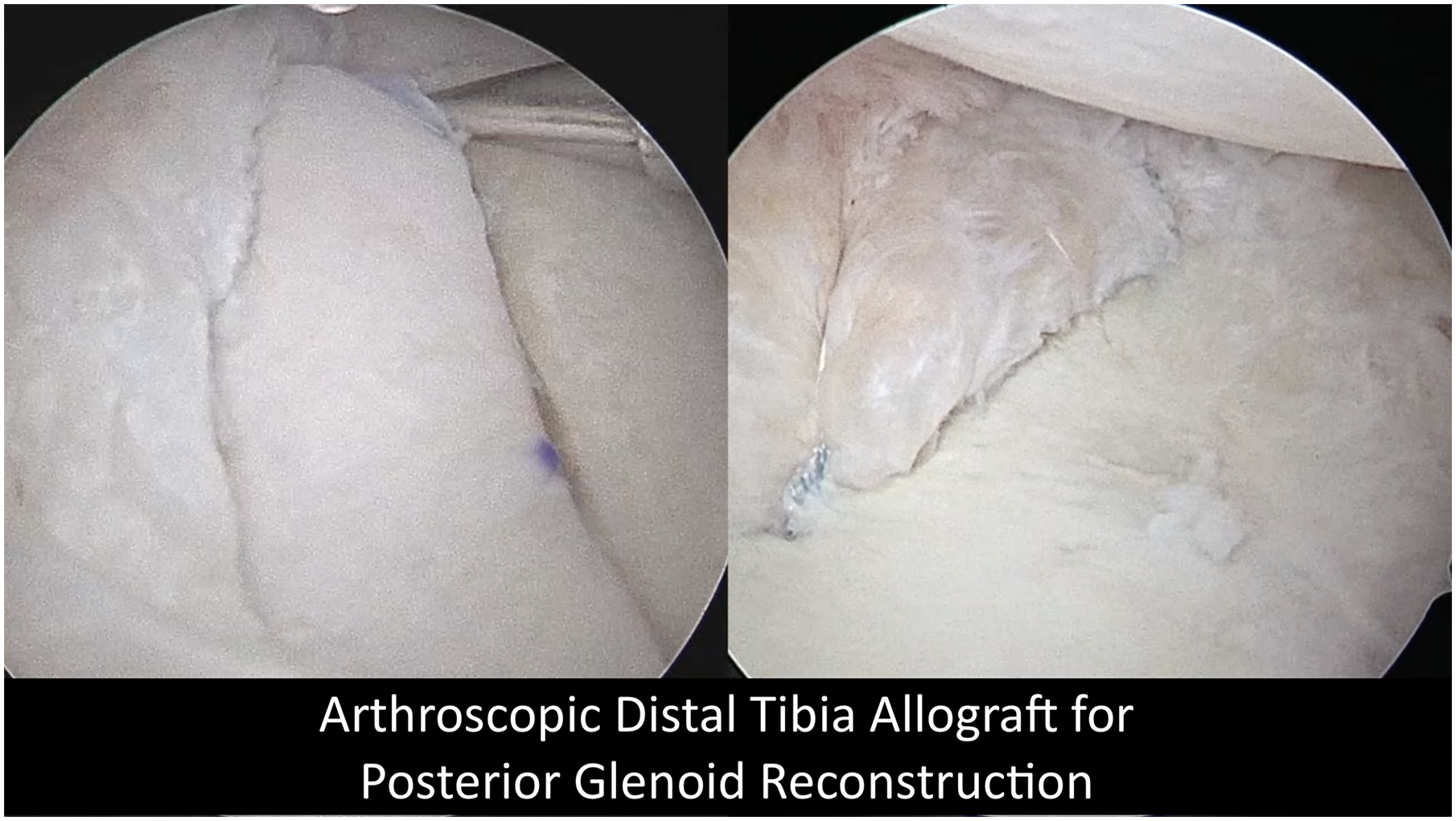
Keywords
Video Transcript
This is Dr Jon Dickens from Walter Reed National Military Medical Center. This technique was developed in combination with Drs LeClere and Kilcoyne and our expert orthopedic team of Drs Hoyt and Riccio. In this video, we are presenting our technique of arthroscopic distal tibia allograft (DTA) for the treatment of recurrent posterior instability in the setting of posterior glenoid bone loss (pGBL). We have no relevant disclosures.
This case is a 32-year-old man with recurrent posterior instability that has failed 2 prior posterior labral repairs. X-rays shown here demonstrate significant pGBL. Computed tomography (CT) demonstrates combined 16% pGBL and posterior retroversion. This is best demonstrated on the 3D model which we obtain for preoperative planning on all posterior glenoid augmentation cases. Posterior instability and pGBL has been considered to be relatively uncommon although it may be more prevalent than previously recognized, with between 15% and 20% of all shoulder stabilizations involving the posterior labrum. Measurable pGBL greater than 5% may be present in as many as 69% of posterior instability cases, and 14% to 22% will have pGBL greater than 13.5%.
Patients with this substantial bone loss are more likely to fail arthroscopic stabilization and less likely to return to previous function following soft tissue procedures. Multiple osseous augmentation procedures have been described, which can assist with increasing anteversion or creating greater posterior contact area, including osteotomies, autograft iliac crest, and allograft distal tibia.
Allograft distal tibia is an appealing graft as it is similar in curvature to the glenoid articular surface, resurfaces posterior bone loss with articular cartilage, restores native glenohumeral contact pressures, and avoids the morbidity of autograft harvest. Traditionally, described osteotomy procedures and posterior bone augmentation procedures have been performed with an open approach to the posterior aspect of the glenohumeral joint. Difficult surgical exposures, limited visibility, depth of the surgical field, and potential neurovascular complications have led to decreased enthusiasm for posterior glenoid bone augmentation. Recently, arthroscopic techniques have gained favor.
In this video, we demonstrate our technique for arthroscopic-assisted distal tibial bone block allograft transfer followed by a posterior Bankart repair to create an extra-articular graft position. The current indication for this procedure is failed arthroscopic posterior labral repair in the setting of pGBL >13.5% and primary complaints of instability. Those patients with advanced glenohumeral arthritis, pain as a primary complaint, multidirectional instability in the setting of hyperlaxity are the most common contraindications.
Our basic equipment and set up is provided here. We prefer to use the Latarjet glenoid guide. A ¾-inch malleable or sleds are useful for graft delivery. We currently use a fresh, never frozen, DTA. Similar to the DTA graft preparation for anterior bone loss, the posterolateral aspect of the incisura is used. The width of the graft is determined based on our planed glenoid preparation and bone loss; however, it is generally 10-mm wide, 20-mm from superior to inferior, and 11-mm deep. We use the 10° scarf cut jig. The 4-mm drill is over-reamed to prepare the graft for later fixation. The contour of the articular surface can be confirmed based on the sizing jigs. The graft is then pulse lavage and soaked in platelet rich plasma (PRP).
We perform this procedure in the lateral decubitus position. The standard posterior viewing portal is high and outside to optimize access for posterior glenoid preparation. The accessory posterior lateral portal is created at the end of the case for posterior labral repair and our glenoid delivery portal is made slightly more medial and in line with the posterior glenoid to optimize screw trajectory.
Viewing the left shoulder in the lateral decubitus position from the anterior superior portal, the prior labral repair sutures are removed and glenoid preparation completed from the high-lateral posterior portal. It is important to create a perpendicular and smooth posterior glenoid recipient surface that ensures adequate depth. We use a longitudinal posterior incision for guide and graft delivery. We prefer to access and deliver the sizing block medial to the capsule and labrum so as not to damage the posterior capsular labral structures. We use a spinal needle to ensure location medial to native labrum. We have also found this facilitates screw placement when performed in the lateral decubitus position.
After confirmation of final sizing, the final graft is delivered. We use a polydioxanone suture looped through the graft and offset guide to aid in security if the graft needs to be readjusted. The lip of this guide fits securely onto the glenoid and the shorter cannulated drill guides do not interfere with graft placement. Guide wires are used to provide preliminary fixation followed by a 2.75-mm cannulated drill. Screw depths are measured and 3.75-mm cannulated screws are placed with sequential tightening. Use of the 3D-printed model for preoperative planning can assist in determining appropriate screw length. Final graft security is checked. Posterior capsular labral tissue may not be amendable for repair depending on tissue quality. If a posterior capsular labral repair is desired, an accessory posterolateral portal is created. We prefer soft tissue repair when possible and may use up to 3 anchors depending on the tissue quality.
Postoperatively, patients are maintained in an abduction sling for 6 weeks. We start Codman exercises immediately. Early scapular control is initiated in the first 2 weeks and full active range of motion is achieved by 8 weeks. Return to full pushups and pull ups is achieved at 6 months. Final x-rays are shows here. High quality reports of short- or long-term clinical outcomes are currently lacking for this and other posterior glenoid bone augmentation procedures; however, results in small series appear promising.
Footnotes
Submitted March 2, 2021; accepted March 10, 2021.
Each author certifies that his or her institution approved the human protocol for this investigation and that all investigations were conducted in conformity with ethical principles of research. All of the authors are employees of the US Government. This work was prepared as part of their official duties. Title 17 U.S.C.§105 provides that “Copyright protection under this title is not available for any work of the United States Government.” Title 17 U.S.C. §101 defined a US Government work as a work prepared by a military service member or employees of the US Government as part of that person’s official duties. The contents of this publication are the sole responsibility of the author(s) and do not necessarily reflect the views, opinions, or policies of Uniformed Services University of the Health Sciences (USUHS), the Department of Defense (DoD), or the Departments of the Army, Navy, or Air Force. Mention of trade names, commercial products, or organizations does not imply endorsement by the US Government.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
