Abstract
Purpose:
The purpose of this study was to describe adaptations and participant characteristics and engagement in family-focused diabetes self-management education (DSME) before and during a large-scale disruption in health care access and research participation, which prompted a pivot to virtual DSME.
Methods:
The study was conducted at a federally qualified health center (FQHC) serving a predominantly low-socioeconomic status Hispanic community. Two hundred twenty-two adults with type 2 diabetes (85% Hispanic) receiving care from the FQHC enrolled with a support person (SP); dyads were randomized to community health worker (CHW)-led dyad-focused Family Support for Diabetes Health Action (FAM-ACT) or patient-focused DSME. Survey, health record, and session data were compared between those enrolled before (n = 77) versus during the disruption (n = 145).
Results:
In hybrid (virtual+in person) DSME, CHWs prioritized group discussion and shorter sessions emphasizing participants’ personal health goals and social-emotional concerns. Enrollment was lower after versus before switching to hybrid (23% vs 30% recruited). Those with less complex diabetes and preferring Spanish enrolled at higher rates during hybrid offerings. Overall, patient DSME attendance slightly decreased during versus before hybrid implementation (mean –0.3 sessions/6) but increased in FAM-ACT patients (mean +0.3 sessions/6) and SPs (mean +0.5 sessions/6). During hybrid programs, patients choosing virtual attendance were more often female, living with children, have food insecurity and difficulty prioritizing diabetes over other demands.
Conclusions:
Group DSME delivered via hybrid sessions maintained participant engagement during a large-scale disruption in health care access by addressing language, health and social needs, life demands, and technological barriers.
Trial registry:
The underlying trial was registered with www.clinicaltrials.gov (NCT03812614, 01/18/2019).
From March 2020 through May 2023, the coronavirus (COVID)-19 pandemic and consequent social distancing regulations significantly disrupted health care access and delivery for people with diabetes. During the first year of the pandemic, outpatient visits related to care and management of chronic conditions were reduced by 10% and by 17% for diabetes specifically. 1 Two-thirds of health care providers in an international survey felt that these changes had a moderate or severe effect on health care utilization among patients with chronic disease, with adults with diabetes the most affected. 2
Diabetes self-management education and support (DSME) is an evidence-based solution to support adults with diabetes in their self-management 3 and consistently leads to improved short-term diabetes outcomes. 4 DSME programs complement medical care for diabetes by helping patients identify and overcome challenges to self-management and empowering them with personalized diabetes-management information and skills. However, DSME has been limited in its reach to adults with diabetes in general 5 and even more to people from low-socioeconomic status (SES) and minoritized communities. 6 Although DSME could be an effective way to support adults with diabetes during a health care disruption, it is typically delivered in person in individual or group sessions and so was especially challenging to deliver during the pandemic.
To address barriers to in-person health care, providers rapidly adopted telehealth visits for managing chronic disease.1,7,8 Some DSME programs were delivered virtually (eg, via telehealth or meeting platforms) prior to the pandemic and were shown to have high patient satisfaction and be effective at improving glycemic control. 9 Yet even after widespread uptake of telemedicine in general during and after 2020 and increases in access to medical care for some adults with type 2 diabetes (T2DM), 10 access to DSME among adults with T2DM remained poor. 11 It is not clear how patients with T2DM are able and choose to engage with virtual DSME if it is offered.
From 2019 to 2023, we conducted a trial of individual versus family-focused DSME at a federally qualified health center (FQHC) serving a primarily Hispanic, low-SES community. Dyads of adult FQHC patients with T2DM and a family or friend “support person” (SP) were enrolled. The start of the COVID-19 pandemic necessitated adaptation of the DSME programs to virtual delivery, providing an opportunity to examine how a disruption to health care access and pivoting to virtual DSME impacted how adults with T2DM from a historically underserved group and their supporters enrolled and engaged in DSME. The objective of the present exploratory study is to describe how we adapted our DSME programs for virtual delivery, compare characteristics of those enrolling before and during the pandemic and their engagement in DSME before and after program adaptations, and describe benefits of and challenges to DSME participation during the pandemic in participants’ own words. Ultimately, we hope to shed light on how virtual options might help improve DSME reach, how virtual DSME can be adapted for those most likely to engage, and how adapting DSME delivery might help mitigate the negative impacts of future health care disruptions.
Methods
Setting and Participants
The trial protocol and interventions were developed using a community-based participatory research approach in partnership with an FQHC in southeast Michigan that serves a primarily Spanish-speaking, low-resource community. 12 The FQHC’s patient population reflects the local community and is 79% Hispanic, 10% non-Hispanic Black, 4% non-Hispanic White, and 7% other. Eleven percent of FQHC patients live below the poverty line. Over 33% of patients are uninsured, 46% use Medicaid, 7% use Medicare, and 8% use private insurance. During the COVID-19 pandemic, the FQHC made efforts to serve general health and pandemic-related needs of the community. This included opening to essential in-person care as early as possible, proactive outreach to patients missing appointments or other essential care (including diabetes tests and care), and outdoor clinics to obtain COVID tests and vaccinations.
Eligible participants were recruited as dyads comprised of 1 adult FQHC patient with T2DM (patient) and an SP. Patients were eligible if they were 21 to 75 years of age, had an A1C ≥7.5% in the past 6 months, and planned to receive care from the FQHC for the next year. SPs could be any family member or friend who was not the patient’s paid caregiver, ≥21 years of age, and able to attend DSME sessions in person or remotely if invited. See Deverts et al 12 for full inclusion and exclusion criteria.
Recruitment, Screening, and Enrollment
Participants were recruited between September 2019 and December 2022, with a several-month pause between March 2020 and February 2021 due to pandemic-related restrictions on in-person research and disruptions to FQHC staff and functions. Recruitment procedures have been described in detail. 12 Briefly, potentially eligible patients were identified via review of the FQHC electronic health record (EHR) or introduced to study staff by their FQHC provider during a clinic visit. Patients identified via EHR were mailed a letter about the study and then called by study staff within 3 days (if the patient did not opt out) and screened for eligibility. Interested eligible patients provided contact information for a family member or friend who was involved in their diabetes care. Patients also were scheduled for their initial study visit, where they gave consent and completed baseline assessments. Seventy-seven dyads enrolled before the pause (prepandemic) and 145 after recruitment resumed (during pandemic).
Program Design and Pandemic Adaptations
Dyads were randomized to Family Support for Diabetes Health Action (FAM-ACT, dyad-focused DSME) or traditional individual patient-focused DSME (I-DSME). Both programs were designed in collaboration with community health workers (CHWs), who ensured all materials were culturally relevant and included content that addressed the needs of adults with T2DM in the local community. The programs also were offered in Spanish and English and delivered by bilingual CHWs. Patients in both programs were invited to take part in an initial introductory (intro) visit with a CHW, 6 CHW-led group DSME sessions, and twice-monthly CHW care management calls (CHW calls). FAM-ACT SPs were directly invited to take part in the program, but I-DSME SPs were allowed to attend if they chose to do so. FAM-ACT SP participation in sessions and calls was encouraged but not required. DSME sessions were conducted in a regular rotation every 2 weeks, with Spanish and English offered on alternate weeks. Participants had 7 months to complete the 6 sessions. Session content was based on American Diabetes Association guidelines for DSME 13 and included healthy eating, physical activity, diabetes medications, and preventing diabetes complications. The sessions also guided patients in setting SMART (specific, measurable, achievable, relevant, time-specific) 14 goals related to the session content. FAM-ACT dyads received additional information designed specifically for SPs, including helpful SP roles for supporting each session topic, strategies for communicating with patients about diabetes, tips for weekly patient-SP talks about diabetes, and approaches SPs could use to help the patient set and work on SMART goals.
CHW-led DSME sessions originally were delivered in an in-person group setting at the FQHC, using the Conversation Map Program (Health Interactions, LLC). Conversation Maps are evidence-based, 3-foot by 5-foot “maps” depicting situations related to the DSME topic being covered. Accompanying facilitator guides are designed to encourage discussion as the group responds to situations depicted in the map. At in-person sessions, CHWs would display the map on a table or wall, invite attendees to view the map together, and encourage discussion while using the guide to prompt them on key topics. Sessions were 60 to 90 minutes, with 30 minutes added for FAM-ACT dyads to cover SP-focused content. Details on session content have been published. 12 CHWs would contact patients between sessions as needed to review patients’ progress on their goals and guide them in setting new goals or identifying next steps for goals they had yet to reach. FAM-ACT dyads were encouraged to attend calls together so they could set goals as a team and include the SP in SMART action plans.
Several efforts were made to facilitate participants’ engagement in DSME. These included reminder calls before DSME sessions, offering 1 evening session per week, and CHW “office hours” during weeks when no sessions were offered to give participants an opportunity to catch up on information they may have missed. FAM-ACT patients and SPs could attend sessions on different days or at the same time but via a different modality. The FQHC offered transportation to onsite in-person sessions when needed.
Adaptations
After March 2020, in-person research activities were limited, health care access reduced, and health threats heightened, especially for people with diabetes. To continue the study while ensuring participant and study staff safety, several modifications were made to the programs (Table 1). The most notable were adapting the intro and DSME sessions for synchronous online delivery (eg, Zoom) and consolidating the intervention from 2 phases over 12 months to a combined phase lasting 6 months.
Adaptations to FAM-ACT Study Recruitment and Delivery in Response to the COVID-19 Pandemic 12
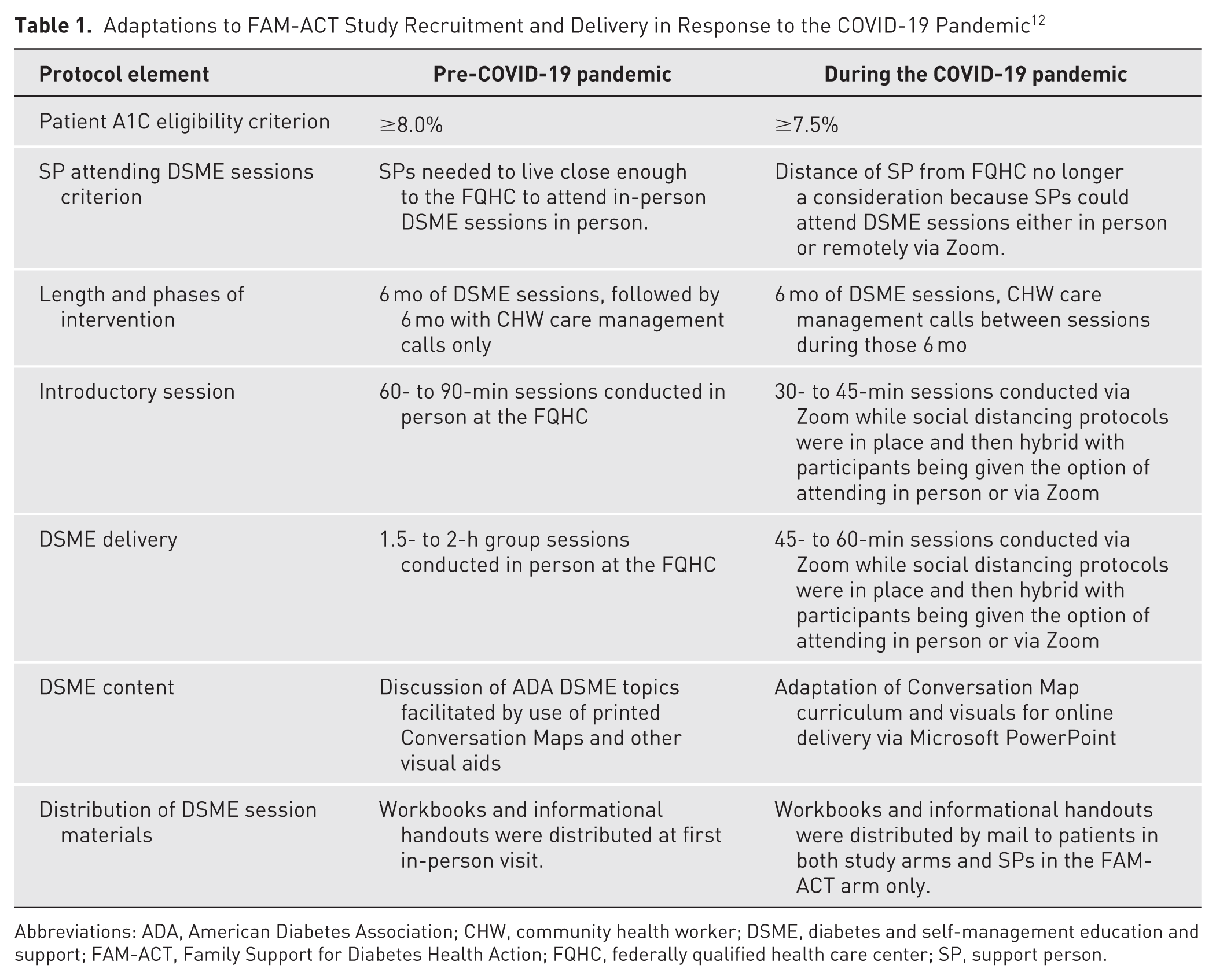
Abbreviations: ADA, American Diabetes Association; CHW, community health worker; DSME, diabetes and self-management education and support; FAM-ACT, Family Support for Diabetes Health Action; FQHC, federally qualified health care center; SP, support person.
Transition to a virtual intervention option
In-person sessions were replaced by “virtual” sessions that participants could attend via Zoom. Only the virtual option was offered for 9 months (February-September 2021). After in-person meeting restrictions were lifted, hybrid sessions were offered that allowed participants to attend group sessions at the FQHC or via Zoom, with in-person and virtual attendees able to interact. Patients and SPs could attend via different modalities. Bilingual study staff helped participants install virtual meeting apps before sessions and navigate them during the sessions.
Several adaptations were made to the intervention to facilitate virtual delivery.
DSME presentation and group facilitation
CHWs used presentation software to display slides containing images relevant to the session topics. Onscreen visuals were used in place of physical teaching aids to ensure a comparable experience for participants attending sessions virtually and in-person, respectively.
Intro and DSME session length
To prevent “Zoom fatigue,” the intro visit was reduced to 30 to 45 minutes and individual DSME sessions to 45 to 60 minutes. CHWs reduced session length without removing essential content by dropping some discussion questions from the original program and eliminating redundancies in session lesson plans.
DSME materials distribution
Prepandemic, participants were oriented to study workbooks and given DSME handouts at in-person visits. During pandemic, materials were mailed to participants ahead of sessions.
Intervention duration
The intervention was originally delivered in 2 parts over 12 months, with the 6 DSME sessions during the first 6 months and twice-monthly CHW calls during the latter 6 months. The pandemic-related recruitment pause did not permit sufficient time to both recruit the target sample size and have all participants complete the intervention. 12 Thus, intervention phases were consolidated so DSME sessions and CHW calls occurred over one 6-month period.
Measures
Enrollment rates
Enrollment rate was calculated as the number of randomized patients divided by the total number of patients who were approached about the study via the aforementioned recruitment methods.
Patient and SP measures
Self-report data were collected by surveys administered by bilingual research assistants at screening and at the baseline visit. 12
Demographic measures included age, sex/gender, race, ethnicity, preferred language (Spanish or English), education, working status, and whether the patient lived with a spouse/partner.
Diabetes measures included self-reported insulin use and baseline fingerstick A1C (Bayer DCA 2000®+, Bayer Diagnostics, USA).
Diabetes distress in patients and SPs was assessed using the Problem Areas in Diabetes (PAID)-5 for People With Diabetes and the PAID-5 for Family Members, respectively. 15 Using a 5-point scale (0 = not a problem, 4 = serious problem), respondents rated how much 5 negative emotional responses to diabetes had been a problem for them in the past 6 months (range, 0 to 20; higher scores = greater distress). Scores ≥8 suggest distress that may warrant further evaluation.
Patient diabetes self-efficacy was assessed using the Self-Efficacy for Managing Chronic Diseases Scale. 16 Patients used a 10-point scale to rate how confident they were in performing diabetes self-management behaviors. Summary scores were calculated by taking the mean of the items (range, 1 to 10; higher scores = greater self-efficacy). SPs rated their self-efficacy for helping the patient with diabetes management using an adapted version of the same scale. For analysis, scores were dichotomized at the median (patients, <8 vs ≥8; SPs, <9 vs ≥9).
Patient food insecurity was assessed with the Hunger Vital Sign. 17 The scale is comprised of 2 yes/no items asking whether in the past 6 months respondents have run out of food or worried about running out of food. A positive response to either item is a positive screen for food insecurity.
Current importance of diabetes was assessed with a single item. 18 Patients and SPs used a 5-point scale to indicate their agreement with the following statement: “I have more important things in my life than diabetes (helping patient with their health care) to take care of now.” Responses were analyzed in 3 categories (strongly agree/agree, neutral, disagree/strongly disagree).
Patient activation was assessed using the Patient Activation Measure (PAM)-10. 19 Patients and SPs used a 4-point scale (0 = strongly agree, 3 = strongly disagree) to rate 10 items on their confidence in handling health-related matters. The PAM is scored by summing the items and then using a proprietary algorithm to transform raw total scores to a 0 to 100 scale. This metric is then reduced to a 4-level categorical variable that can be interpreted as follows: 1, disengaged and overwhelmed; 2, becoming aware but still struggling; 3, taking action and gaining control; and 4, maintaining behaviors and pushing further. Due to low numbers, levels 1 and 2 were combined for these analyses.
Self-rated health was assessed using the SF-1 item (general health: excellent, very good, good, fair, or poor) 20 and was dichotomized (excellent/very good/good vs fair/poor).
At the follow-up assessment, study research assistants asked participants this open-ended question: “In what ways, if any, did the COVID-19 pandemic affect how you participated?” At the time point this question was added, approximately 30% of patient participants had already completed their follow-up assessment and so did not have the opportunity to respond.
Analytic Approach
Two sets of exploratory analyses were performed. The first (N = 222) compared participants from dyads enrolled before (N = 77) and during (N = 145) the pandemic. The second (N = 91) compared participants from dyads enrolled during the pandemic who chose to attend DSME sessions in person only and those who chose to attend at least 1 virtual session. Analyses were bivariate, with participant characteristics in each group described with proportions and means with standard deviations. To assess the magnitude of differences between groups, standardized differences (SDiff)21,22 were calculated. SDiff characterizes differences in size by dividing the between-group difference in means or proportions by the expected variability (ie, average SD across groups). It provides a scale- and sample size-independent measure of between-group imbalance, making it suitable for comparing small subgroups and overreliance on P values. SDiff >0.1 was considered a more than negligible difference and >0.25 a moderate difference.21,22 Analyses were performed using IBM SPSS Statistics software (version 28.0.1.1). Open-ended question responses were transcribed by bilingual study staff and then analyzed for thematic content using editing analysis style. 3
For reporting (see supplement), we used the STROBE reporting guideline 23 to draft this article and the STROBE checklist 24 when editing.
Results
Enrollment Rates Before and During Pandemic
Two hundred twenty-two (N = 222) dyads comprised of an adult with T2DM and an SP enrolled in the study. Enrollment was higher prepandemic (30%) than during pandemic (23%, SDiff = 0.17). The most common reason for ineligibility in both time periods was inability to identify an SP (65% pre vs 68% during). Among those contacted and eligible, the most common reason for declining was not having time to participate (pre, 66% [92/142] vs during, 53% [229/436]; SDiff = 0.25). The second most common reason was “lack of interest,” which increased substantially during the pandemic (pre, 17% [24/142] vs during, 36% [157/436]; SDiff = 0.45).
Participant Characteristics Pre Versus During the COVID-19 Pandemic
Patient Enrollee Characteristics
As shown in Table 2, patients enrolled during pandemic were slightly younger (SDiff = 0.22) and more likely to identify as Hispanic (SDiff = 0.54) and prefer Spanish to English (SDiff = 0.33). They also were less likely to have graduated high school (SDiff = 0.20), more likely to be homemakers (SDiff = 0.17), and equally likely to be women and live with children. Those enrolled during pandemic also were less likely at baseline to use insulin (SDiff = 0.43), had less diabetes distress (SDiff = 0.27), and scored higher on self-efficacy for managing diabetes (SDiff = 0.29).
Baseline Characteristics of Patients Enrolled Before (Prepandemic) and After the Start of the COVID-19 Pandemic (During Pandemic)
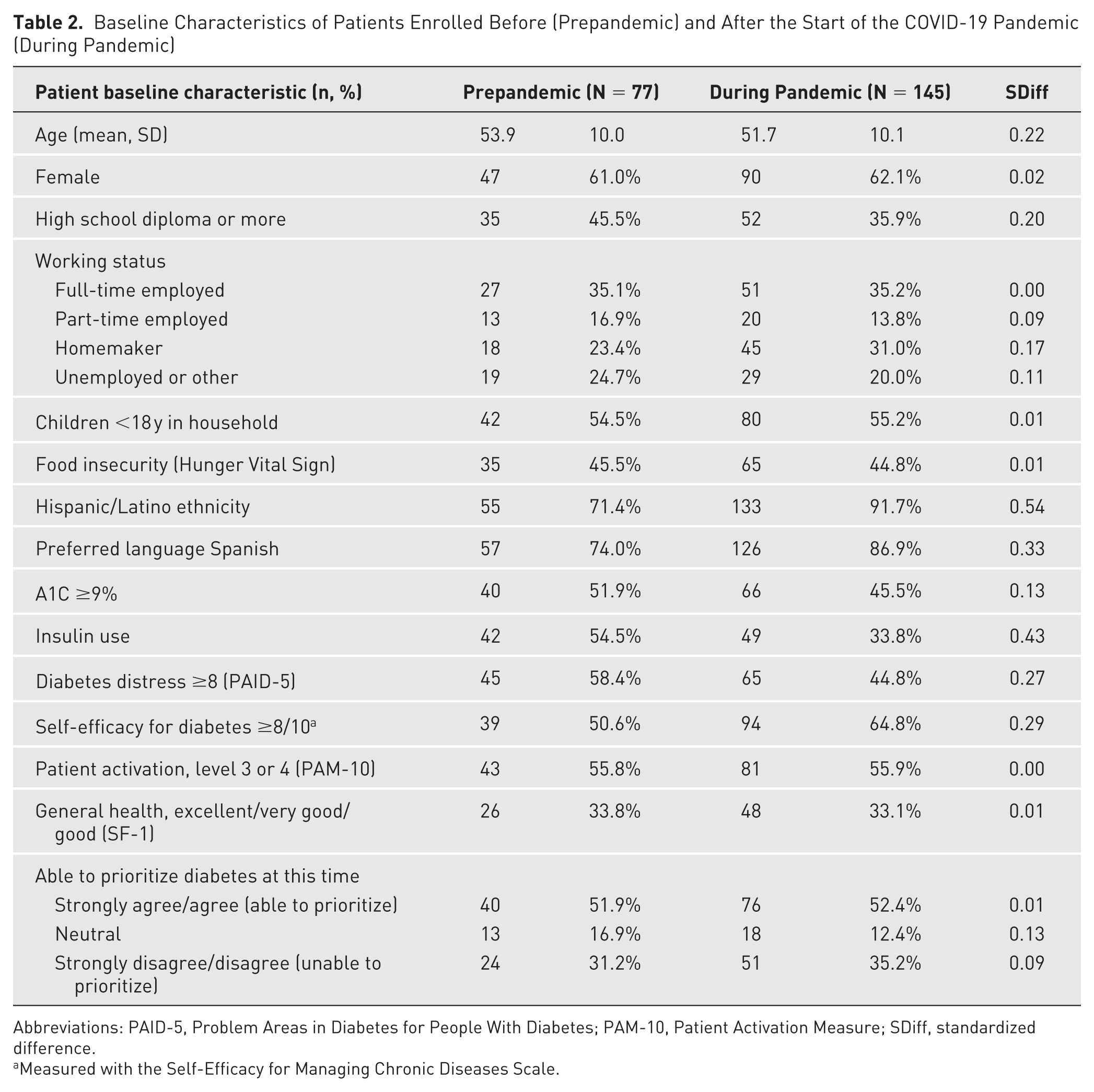
Abbreviations: PAID-5, Problem Areas in Diabetes for People With Diabetes; PAM-10, Patient Activation Measure; SDiff, standardized difference.
Measured with the Self-Efficacy for Managing Chronic Diseases Scale.
SP enrollee characteristics
As shown in Table 3, SPs enrolled during pandemic were younger (SDiff = 0.20) and more likely to identify as Hispanic (SDiff = 0.44) and prefer Spanish to English (SDiff = 0.34). SPs enrolled during pandemic were more likely to be employed part-time (SDiff = 0.24) and be homemakers (SDiff = 0.16) and were less likely to be unemployed (SDiff = 0.27). They were less likely to have diabetes or prediabetes (SDiff = 0.17) and scored lower on patient activation (SDiff = 0.40). They reported less distress about the patient’s diabetes (SDiff = 0.23) but were more likely to feel that they currently were unable to prioritize the patient’s diabetes in the face of competing demands (SDiff = 0.17).
Baseline Characteristics of Support Persons (SPs) Enrolled Before (Prepandemic) and After the Start of the COVID-19 Pandemic (During Pandemic)
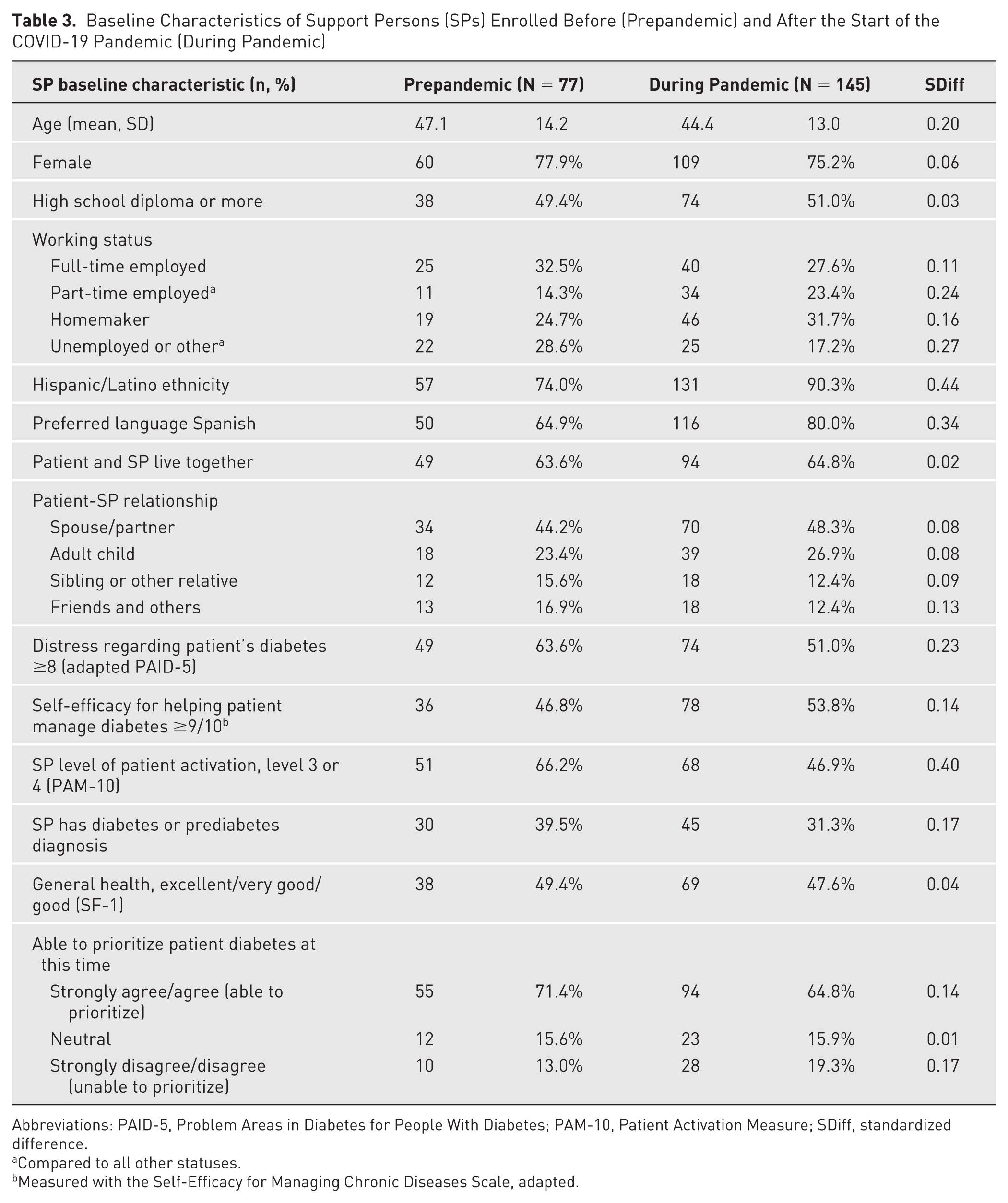
Abbreviations: PAID-5, Problem Areas in Diabetes for People With Diabetes; PAM-10, Patient Activation Measure; SDiff, standardized difference.
Compared to all other statuses.
Measured with the Self-Efficacy for Managing Chronic Diseases Scale, adapted.
Education session attendance pre vs during pandemic
Patients who enrolled prepandemic attended on average 0.3/6 more education sessions than patients enrolled during (Supplemental Figure S1). This difference can be attributed to lower attendance among patients in the I-DSME arm (prepandemic mean = 4.6, SD = 2.24, n = 38 vs during pandemic mean = 3.6, SD = 2.33, n = 72; SDiff = 0.44). By comparison, attendance rates for patients in the FAM-ACT arm did not differ by enrollment period (pre, n = 39, mean = 3.4, SD = 2.71 vs during, n = 73, mean = 3.7, SD = 2.29; SDiff = 0.12. Average SP DSME session participation increased from 2.3/6 sessions pre to 2.8/6 sessions during pandemic (FAM-ACT arm only).
CHW care management call completion
Patients enrolled during pandemic were less likely to complete CHW calls (55% vs 78%, SDiff = 0.50) and completed fewer calls compared to those enrolled prepandemic (SDiff = 0.69). This finding remained when during pandemic calls were compared to prepandemic calls completed only during the first 6 months of the intervention, when patients still were taking classes (SDiff = 0.25). This trend was consistent across study arms (Figure 1).
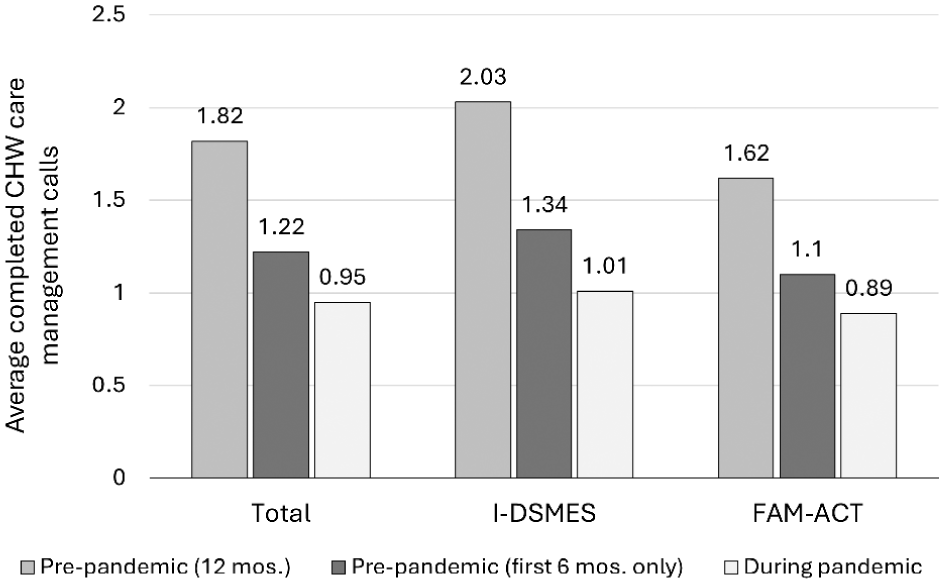
Care management call completion by study arm and enrollment relative to the start of the COVID-19 pandemic. Patients enrolled prepandemic received calls over 12 months of participation, whereas those enrolled during pandemic received calls over 6 months.
Participant views
Eighty-six percent (124/145) of patients and 82% of SPs (183/222) answered open-ended questions about how the pandemic affected their study participation. Content analysis revealed 5 themes. First, some participants described being afraid to go to the clinic due to negative health impacts of COVID-19. Second, some mentioned that quarantining made it more logistically difficult to participate because they were not allowed to attend in-person sessions at the FQHC. Third, some participants remarked that having a virtual option made it easier to participate not just during pandemic but in other situations as well (eg, while traveling). Fourth, both patients and SPs felt the pandemic made it more difficult for them to communicate with one another due to social distancing or illness. Fifth, patients described life circumstances related to the pandemic (eg, having to stay home with children) making it more difficult to attend DSME sessions (see Table 4 for example comments).
Open-Ended Responses Related to How the Pandemic Affected Participants’ Study Participation
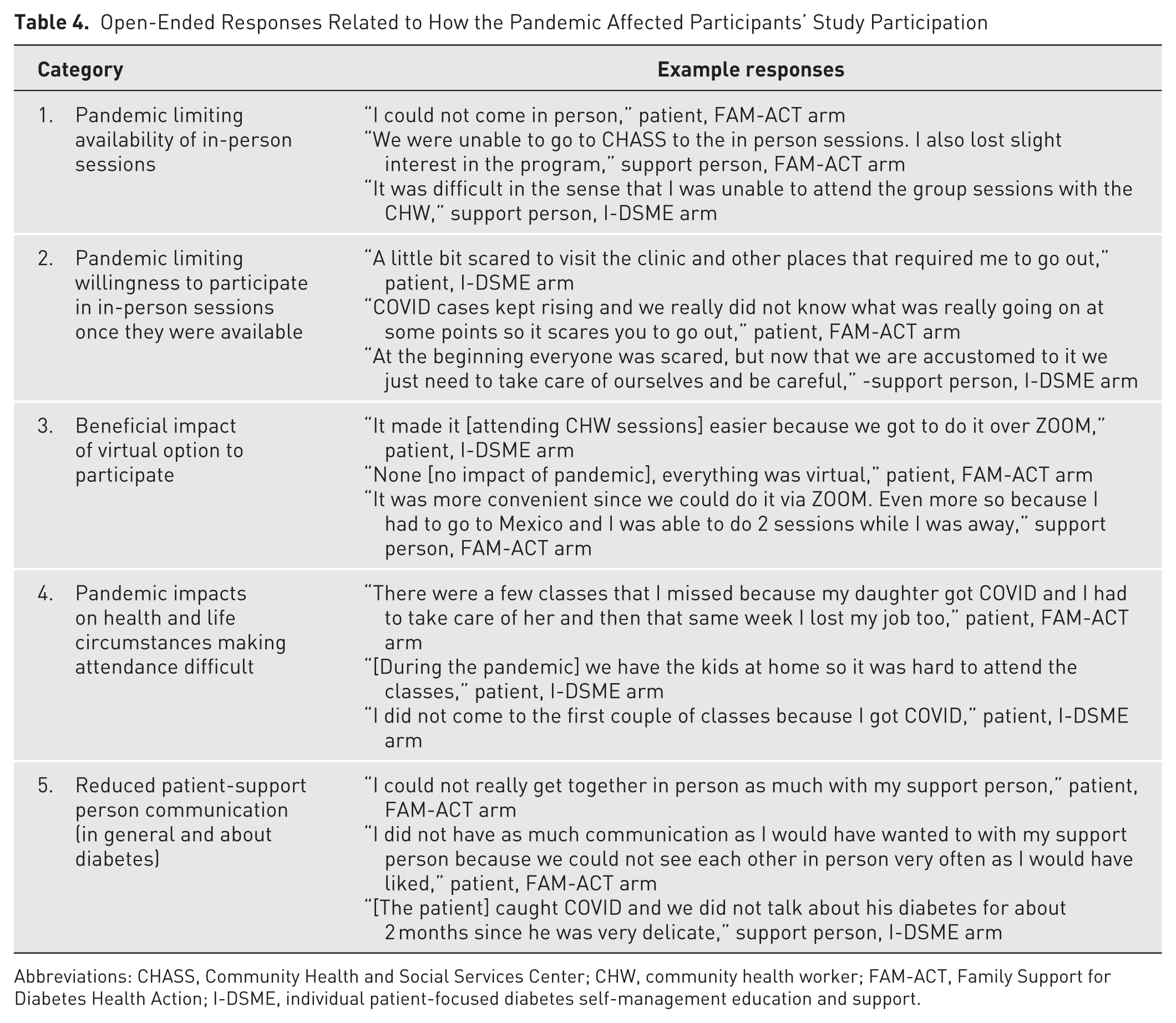
Abbreviations: CHASS, Community Health and Social Services Center; CHW, community health worker; FAM-ACT, Family Support for Diabetes Health Action; I-DSME, individual patient-focused diabetes self-management education and support.
DSME session attendance, in person only versus any virtual
Ninety-one of 145 patients enrolled during pandemic had the option of attending sessions in person or virtually, with 84 patients (92%) completing at least 1 session via either mode. Of these, 58% (n = 49) attended virtually and 42% (n = 35) in person only. Of the 43 FAM-ACT patients who could attend via either mode, 65% (n = 28) attended at least 1 session virtually compared to 51% (n = 21) of the 41 I-DSME patients (SDiff = 0.29). However, FAM-ACT patients attending in person only completed more sessions (in person only, mean = 4.3, SD = 2.4 vs any virtual, mean = 3.7, SD = 2.1; SDiff = 0.27), and I-DSME patients attending virtually completed more sessions (any virtual, mean = 4.2, SD = 1.9 vs in person only, mean = 3.4, SD = 2.5; SDiff = 0.36).
Forty-two (89.4%) of the 47 FAM-ACT SPs given the option to attend in person or virtually completed at least 1 session. Of these, 64% (n = 27) attended at least 1 virtual session and 35% (n = 15) in person only (SDiff = 0.62). SPs attending in person only completed more sessions than SPs who attended any virtual sessions (in person only, mean = 3.13, SD = 2.36 vs any virtual, mean = 2.70, SD = 1.98; SDiff = 0.20).
Characteristics of those attending in-person versus virtual sessions
Patients who attended virtual sessions were younger (SDiff = 0.30) and more likely to be female (SDiff = 0.37), identify as Hispanic (SDiff = 0.29), have graduated high school (vs less than high school; SDiff = 0.24), live with children (SDiff = 0.28), and screen positive for food insecurity (SDiff = 0.24). They also were less likely to use insulin at baseline (SDiff = 0.22), score higher on diabetes distress (SDiff = 0.36), and report worse general health (SDiff = 0.23). Patients attending virtual sessions also more often felt they currently were unable to prioritize diabetes in the face of competing demands (SDiff = 0.22; Supplemental Table S1). SPs who attended any virtual sessions were less likely to be the patient’s spouse or partner (SDiff = 0.33) and more likely to be the patient’s adult child (SDiff = 0.30) and to live with the patient (SDiff = 0.13). SPs attending any virtual sessions were less likely to have been diagnosed with diabetes or prediabetes (SDiff = 0.25; Supplemental Table S2).
Discussion
The present study describes how enrollment and engagement in DSME changed for adults with T2DM and family supporters from a predominantly Hispanic community during the COVID-19 pandemic. We found that the disruption to health care access was associated with decreased but still steady enrollment in DSME. Shifting from solely in-person to virtual/hybrid DSME offered benefits related to ease of access, including supporters, and feeling safe and did not diminish DSME participation. The community-partnered approaches to outreach and transition to virtual DSME described here were successful at reaching patients of this FQHC located in a community hard hit economically and medically by the pandemic. Thus, these methods might be used by others to increase DSME reach to diverse participants and to leverage DSME to mitigate negative effects of future disruptions to diabetes health care delivery.
Despite the pandemic disruption, we were able to continue enrolling patient-SP dyads, albeit at a slightly lower rate (30% prepandemic vs 23% during). Factors that may have contributed to our success in maintaining enrollment include the FQHC’s pandemic outreach efforts, prior relationships of study staff and CHWs with the community, our transition to a flexible virtual DSME format, and perceived importance of managing diabetes to stay healthy in the face of potential COVID-19 infection. We previously surveyed a group of patient participants in this study about their experiences managing diabetes early in the pandemic. Many patients reported both increased worry about diabetes and difficulty accessing medical care, 25 which in combination may have incentivized patients to seek ways to maintain their health through self-management. Not having an SP to participate was the most common reason for patient ineligibility both pre and during pandemic. While highlighting the difficulty of recruiting dyads to these kinds of programs, this finding also suggests that the pandemic did not exacerbate the problem.
Patients enrolling during pandemic had less severe diabetes management challenges at baseline, such as less insulin use and less diabetes distress. This aligns with prior studies that found lower insulin use in patients using telemedicine compared to in-person specialty care for T2DM. 26 SPs enrolling during pandemic were also less likely to have been diagnosed with prediabetes or diabetes than those enrolling prepandemic. These trends may have been due to the awareness of the greater severity of COVID-19 illness for people with or at risk for diabetes, prompting attention by all in this group to healthy lifestyle behaviors. This may also have been due to perceived difficulty accessing healthy food and medications (as reported in our early pandemic patient survey) 25 and participants’ desire to find ways to address these challenges. Because all people with diabetes or at risk for diabetes 27 can benefit from DSME and healthy lifestyle education, this was a welcome change but required those delivering DSME to address a wider range of DSME and support needs. Future programs offering DSME during health care disruptions and virtual T2DM care may want to devote additional recruitment efforts to those with more complex diabetes. 11
Patients and SPs who identified as Hispanic and preferred speaking Spanish were more likely to enroll during the pandemic. This shift may have been due to pandemic outreach efforts by the FQHC, including culturally tailored information and services provided in Spanish and English. Language-concordant care is associated with greater trust and satisfaction among persons with limited English proficiency.28,29 Early in the pandemic, FQHC clinic CHWs called patients with diabetes to help them connect with general health care and behavioral health and social resources (eg, food banks, rent assistance programs). This outreach by language-concordant CHWs may have provided reassurance to Spanish-speaking FQHC patients in particular amid the personal and economic effects of the pandemic experienced by this community. Using a community-partnered, codesign approach to adapting DSME and research study outreach during times of uncertainty may boost the ability to understand community impacts and meet evolving participant needs.
Although DSME attendance dropped during pandemic, patients on average still were attending more than half of the sessions. This continued attendance despite pandemic conditions could be attributed in part to participants having the option to attend virtually. While the virtual option was popular, however, 40% of patients preferred to attend DSME in person only when that option again became available. Several participants commented on the appeal of interacting with other adults with T2DM and SPs, suggesting this aspect of the programs may have incentivized some to participate. The “peer support” benefits of group DSME are well established, 30 especially as relates to navigating day-to-day challenges managing diabetes, which worsened during the pandemic. In-person groups may have appealed especially to those trying to reestablish a sense of community after months of isolation. During large-scale disruptions to health care, finding ways to safely bring together people with similar health concerns could boost motivation and benefits to participation. 30
CHW care management call completion was lower for patients enrolled during pandemic relative to those enrolled before it. This pattern may have resulted from the reduced group DSME session length for both in-person and virtual sessions during pandemic. CHWs reported that with shorter sessions, patients attending in person were more likely to stay after class to discuss personal health goals and progress than discuss them in a separate call. This observation suggests that shorter group sessions with time for brief 1:1 discussions with DSME leaders, a format similar to “shared medical appointments,” 31 might promote greater engagement. Future programs and studies affected by a disruption or change may benefit from monitoring early trends in program engagement and working with partners and participants to adjust approaches early if potentially important shifts are occurring.
We found that FAM-ACT patients who preferred to attend in person completed more sessions than those attending virtual sessions, and this may be due in part to differences in patient characteristics between those who chose one modality versus the other. Other studies indicate that adults who are younger, female, and Black are more likely to use telemedicine for diabetes specialty and primary care.26,32 Here, those choosing virtual sessions were also slightly younger on average and more often were female. They were also more likely to live with children, have food insecurity, be less likely to rate their overall health as good, and felt less able to prioritize diabetes over other demands. In a prior study of this sample, we found that those with food insecurity also perceived less general social support. 33 These findings suggest that the virtual option may have appealed more to those with competing demands and less enabling resources and may be better able to engage people in those situations in DSME. Our providing bilingual “virtual tech support” before and during DSME sessions likely facilitated participants’ ability to maintain virtual participation.
Finally, we found that offering DSME virtually increased session attendance by patients’ SPs and by patients in the FAM-ACT (dyad-focused) arm. We previously found in this sample that patients with participating SPs were better able to maintain their own participation. 34 We also found that SPs who were patients’ adult children more often attended virtually. Our study required patients with T2DM to enroll with an SP. In nonstudy settings, DSME programs could encourage patients to invite supporters to participate, which may promote continued patient engagement. However, some patients reported that the pandemic made communication with their SPs difficult in general and about diabetes specifically.
Strengths and Limitations
This study was well suited for describing changes in FQHC patient and SP characteristics and participation in DSME during a large-scale disruption in health care access and shift from in-person to virtual DSME. The generalizability of the findings, though, is limited by the sample being derived from a single FQHC. Also, patients were required to enroll with an SP, which may have created a bias in the type of person willing and able to participate. Limited data were available for FQHC patients who declined to participate. The study design used for this report is quasi-experimental, limiting causal inference. Analyses were primarily descriptive, focusing on observed associations rather than formal statistical testing. Confounders and contextual changes during the study may have influenced the results.
Conclusions
Our experiences delivering DSME to a historically underserved community during a pandemic-related disruption in health care access suggest that adults with T2DM in this community and their supporters were highly motivated and able to participate in virtual DSME and when safe to do so, in any form of group DSME that was offered during this time. Adaptations helped preserve the patient-centered nature of DSME in both modalities and allowed participants to better blend group DSME with personalized individual support. Virtual access was facilitated by dedicated staff “tech support” before and during virtual sessions. Availability of virtual sessions facilitated engagement by SPs and those with competing demands. Future DSME programs could improve their reach and engagement using similar strategies.
Supplemental Material
sj-docx-1-tde-10.1177_26350106261432172 – Supplemental material for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons
Supplemental material, sj-docx-1-tde-10.1177_26350106261432172 for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons by Denise J. Deverts, Margaret F. Zupa, Edith C. Kieffer, Gretchen A. Piatt, Michele Heisler, Felix Valbuena, Stephanie Gonzalez, Claudia Guajardo, Jonathan G. Yabes, Christina Lalama and Ann-Marie Rosland in The Science of Diabetes Self-Management and Care
Supplemental Material
sj-docx-2-tde-10.1177_26350106261432172 – Supplemental material for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons
Supplemental material, sj-docx-2-tde-10.1177_26350106261432172 for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons by Denise J. Deverts, Margaret F. Zupa, Edith C. Kieffer, Gretchen A. Piatt, Michele Heisler, Felix Valbuena, Stephanie Gonzalez, Claudia Guajardo, Jonathan G. Yabes, Christina Lalama and Ann-Marie Rosland in The Science of Diabetes Self-Management and Care
Supplemental Material
sj-png-1-tde-10.1177_26350106261432172 – Supplemental material for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons
Supplemental material, sj-png-1-tde-10.1177_26350106261432172 for Transition to Virtual Diabetes Self-Management Education Delivery in the Setting of Health Care Disruption for Adults With Diabetes and Their Support Persons by Denise J. Deverts, Margaret F. Zupa, Edith C. Kieffer, Gretchen A. Piatt, Michele Heisler, Felix Valbuena, Stephanie Gonzalez, Claudia Guajardo, Jonathan G. Yabes, Christina Lalama and Ann-Marie Rosland in The Science of Diabetes Self-Management and Care
Footnotes
Acknowledgements
We would like to acknowledge the adults with diabetes and support persons who took part in the study, federally qualified health center clinic staff, and study team members not included as authors on this article: Gloria Palmisano, Deliana Ilarraza-Montalvo, Daniela Robles-Hernandez, Barbara Garcia-Sauceda, Brianna Betancourt, Michele Nichols, Sophia Garvin, and Glory Koerbel.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) R01 DK116733 and NIDDK P30DK092926. The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication.
Ethical Considerations
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards and received approval from the University of Pittsburgh Institutional Review Board (STUDY20110344, June 24, 2019). Informed consent was obtained from all participants included in the study.
Data Availability
De-identified data from this study are not available in a public archive. De-identified data from this study will be made available (as allowable according to institutional institutional review board standards) by emailing the corresponding author.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
