Abstract
Background:
Gastroparesis is a common complication after lung transplantation, characterized by delayed gastric emptying that causes nausea, vomiting, and abdominal distension. It is often severe, refractory to medical therapy, and may require surgical intervention. This condition can lead to respiratory complications such as microaspiration and obliterative bronchiolitis. Gastric per-oral endoscopic myotomy (G-POEM) has emerged as a promising treatment for refractory cases.
Methods:
This multicenter retrospective study included post-lung transplant patients who underwent G-POEM for medically refractory gastroparesis at four U.S. tertiary centers. The primary outcome was clinical response, defined as a ≥1-point improvement in the Gastroparesis Cardinal Symptom Index (GCSI).
Results:
Fifty-eight patients (mean age 53.8 ± 12.0 years; 32 female) underwent G-POEM at a median of 12.5 months post-transplant. Gastroparesis was diagnosed at a median of 4.8 months post-transplant, with severe to very severe delayed gastric emptying in 47 of 52 patients based on gastric emptying studies. Fourteen patients (24.1%) were dependent on a gastrojejunostomy tube at baseline. On follow-up, 9 of 13 patients with available data were able to discontinue tube feeds and tolerate a regular diet. All procedures were technically successful. Clinical success was achieved in 73% of patients, with no intraprocedural or postprocedural complications. Follow-up gastric emptying studies were available in 36 patients, of whom 29 showed improvement or normalization.
Conclusions:
This study demonstrates that G-POEM is a safe and effective treatment for refractory gastroparesis in lung transplant recipients and represents a viable option for this complex patient population, warranting further studies to confirm long-term outcomes.
This is a visual representation of the abstract.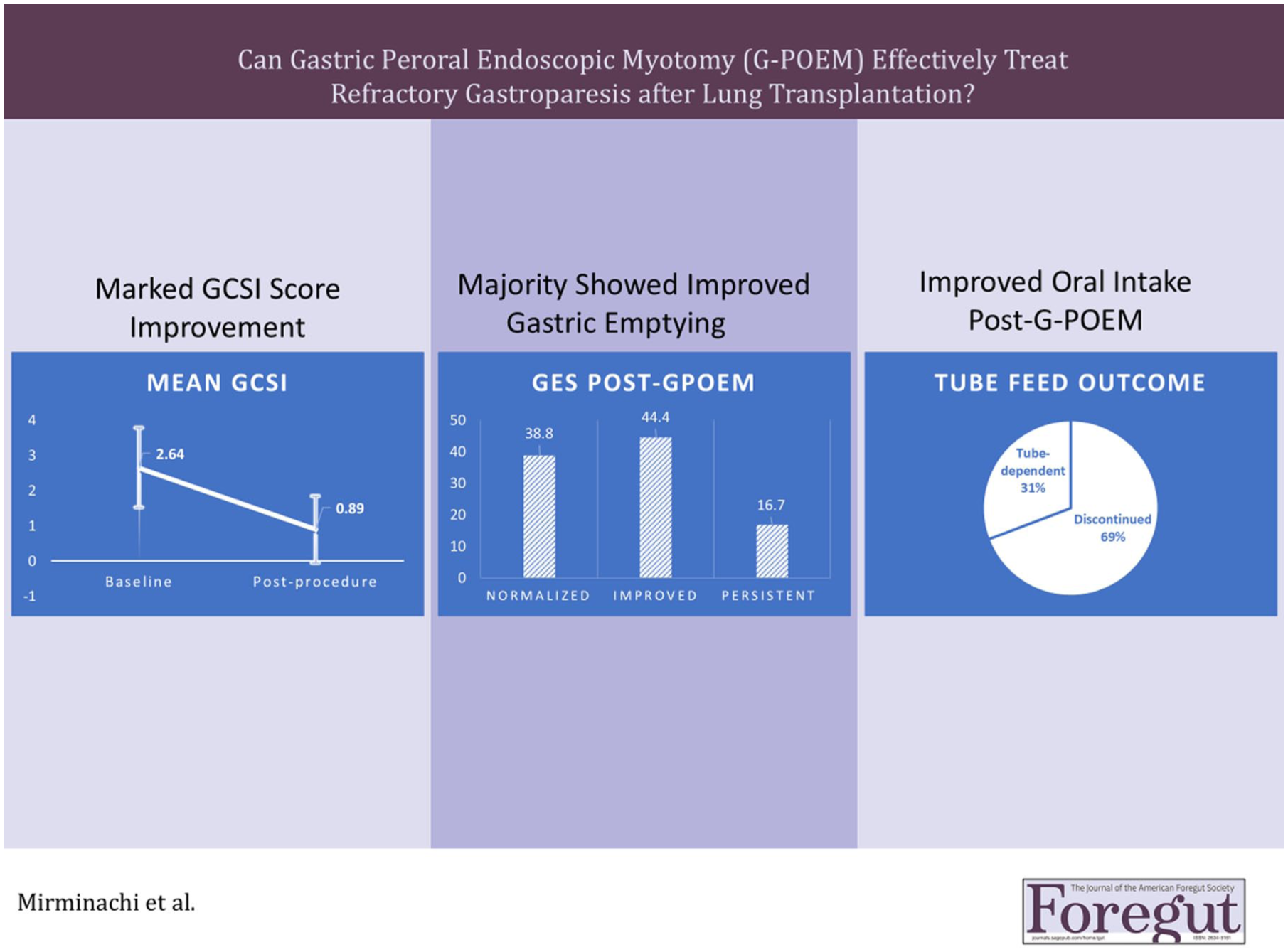
Keywords
Key Learning Points
G-POEM achieved a high rate of clinical response in lung transplant patients with refractory gastroparesis.
No intraprocedural or postprocedural complications were reported, confirming its safety profile.
Given its efficacy and safety, G-POEM may merit earlier consideration in management, though long-term studies are needed to assess its impact on transplant outcomes.
Introduction
Gastroparesis is a well-known complication in patients undergoing lung transplantation, with reported prevalence rates ranging from 23% to 91% following lung transplantation.1,2 Proposed mechanisms include intraoperative vagal nerve injury and the postoperative use of immunosuppressive therapies, both of which can impair gastrointestinal motility and contribute to the development of esophageal dysmotility and gastroparesis.3-5 This complication is of particular concern in lung transplant recipients, as it may increase the risk of gastroesophageal reflux disease (GERD), which can compromise pulmonary hygiene and promote microaspiration. Repeated microaspiration is a known contributor to the development of bronchiolitis obliterans syndrome (BOS), a major cause of chronic graft dysfunction and mortality in this population.6,7 Since GERD is an established risk factor for BOS, early recognition and management of gastroparesis in the postoperative period is critical to reducing the risk of graft rejection and chronic lung allograft dysfunction (CLAD).
Initial management of gastroparesis typically includes lifestyle modification and pharmacologic therapy with prokinetic agents. For patients who remain refractory to medical therapy, interventions such as botulinum toxin injection at the pylorus or placement of enteral feeding tubes may be considered. Gastric peroral endoscopic myotomy (G-POEM) has emerged as a minimally invasive option for patients with refractory gastroparesis. While small observational studies explore the role of G-POEM in post lung-transplant (post-LTx) gastroparesis, data remain limited.
The aim of this study was to evaluate the safety and efficacy of G-POEM in lung transplant recipients with refractory gastroparesis. To our knowledge, this is the largest multicenter study to date investigating the role of G-POEM in this unique and high-risk patient population.
Materials and Methods
Study Design and Setting
This retrospective, multicenter study was conducted between December 2022 and May 2025 across four academic and high-volume transplant centers: University of Pittsburgh Medical Center, Stanford University, UVA Health and Indiana University. Each center has established expertise in advanced endoscopy and transplant care. This study was approved by the University of Pittsburgh Institutional Review Board (24060076), and the requirement for informed consent was waived given the retrospective design.
Patient Selection and Inclusion Criteria
Patients with refractory gastroparesis following lung transplantation, confirmed by delayed gastric emptying on scintigraphy, who underwent G-POEM and had at least 3 months of follow up were included. Clinical response was defined as either complete resolution of gastroparesis symptoms or an improvement in the Gastroparesis Cardinal Symptom Index (GCSI) score by more than 1 point at follow up. Patients were excluded if they had less than 3 months of follow up or lacked documented symptom outcomes. Demographic characteristics (age, sex), clinical history, procedural characteristics and follow up data were collected for all eligible patients.
Data Collection
Data were extracted from electronic medical records (EMRs) and procedure logs, with patient-completed surveys scanned into the EMR. Collected variables included baseline demographics and transplant history, gastric emptying study (GES) results and severity of gastroparesis procedural details (duration, POEM approach, primary closure method), and outcome measures such as technical success, clinical response (eg, Gastroparesis Cardinal Symptom Index [GCSI] improvement), adverse events, hospital length of stay, and need for reintervention. Gastroparesis severity was defined based on gastric emptying scintigraphy and the percentage of retention at 4 hours as follows: grade 1 (mild), 11%-15%; grade 2 (moderate), 16%-35%; grade 3 (severe), 36%-50%; and grade 4 (very severe), >50%.
G-POEM Procedure
All G-POEM procedures were performed under general anesthesia by endoscopists specializing in third space endoscopy. The G-POEM technique involved four standardized steps: (1) making a submucosal incision after submucosal lifting, (2) creating a submucosal tunnel to fully expose the pyloric sphincter on both the gastric and duodenal sides, (3) performing a pyloromyotomy extending 1 to 2 cm proximally, either as a single incision or as two separate cuts, and (4) closing the mucosal entry using through-the-scope clips or endoscopic suturing. Peri-procedural care before and after G-POEM including antibiotic prophylaxis, diet advancement and follow up protocols was tailored to individual patients and varied across institutions.
Outcomes Measures
Outcome measures included technical success and clinical response, defined as a ≥1-point improvement in the GCSI. Additionally, GES results, adverse events, hospital length of stay, and the need for reintervention were recorded.
Statistical Analysis
Continuous variables were expressed as mean ± standard deviation, while categorical variables were presented as number (percentage). Statistical analyses were performed SPSS 18.
Results
Patient Population
Fifty-eight patients (mean age 53.8 ± 12.0 years; 32 female) underwent G-POEM for refractory gastroparesis following lung transplantation and were included in the analysis. All patients had received a lung transplant between 2015 and 2023 (Table 1).
Clinical Characteristics of Lung Transplant Patients Undergoing Gastric Peroral Endoscopic Myotomy (G-POEM) for Refractory Gastroparesis.
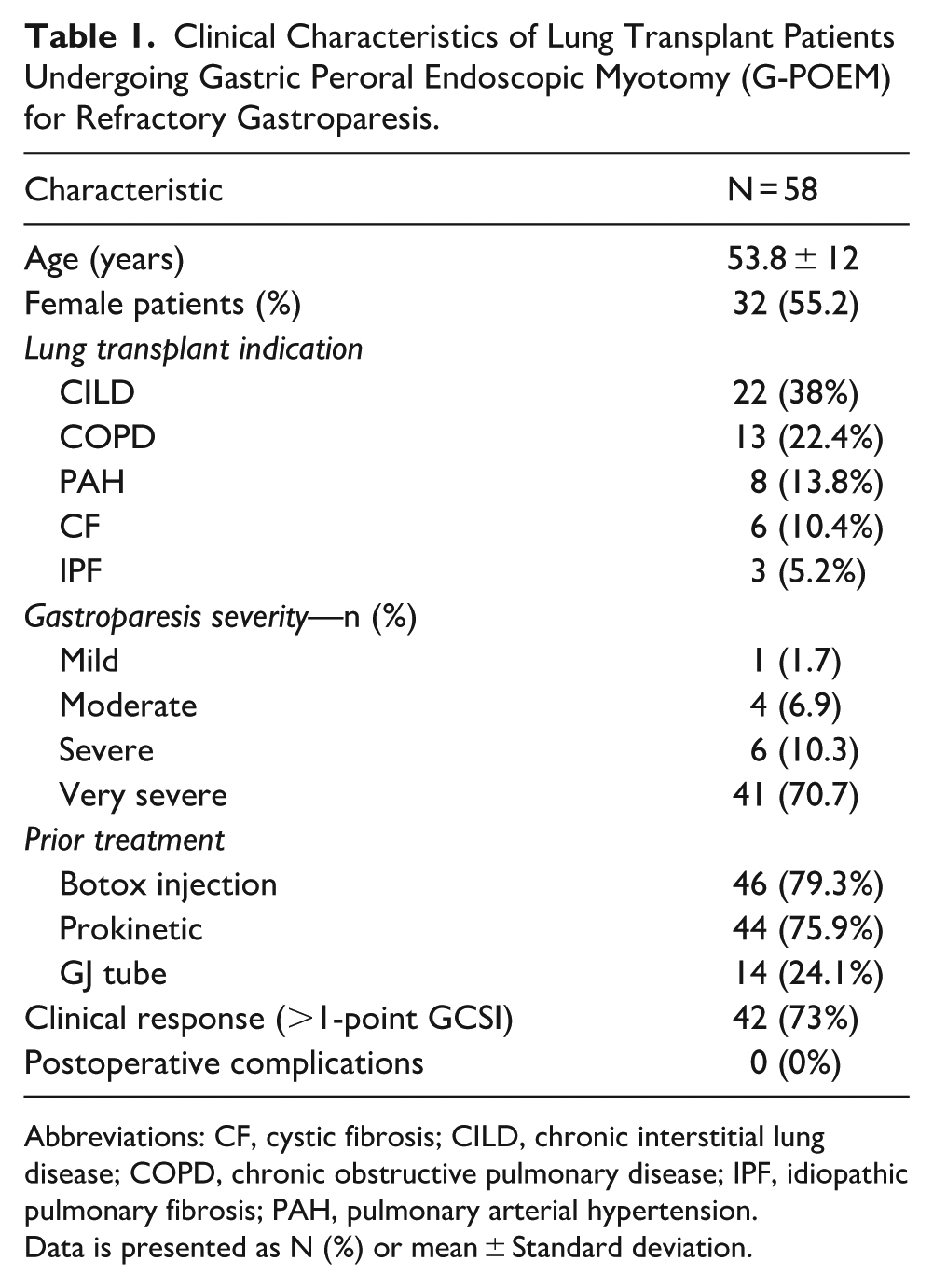
Abbreviations: CF, cystic fibrosis; CILD, chronic interstitial lung disease; COPD, chronic obstructive pulmonary disease; IPF, idiopathic pulmonary fibrosis; PAH, pulmonary arterial hypertension.
Data is presented as N (%) or mean ± Standard deviation.
Baseline Characteristics
Gastroparesis was diagnosed at a median of 4.8 months post-transplant, with a mean baseline GCSI score of 2.64 ± 1.13. At the time of G-POEM evaluation, 44 patients were receiving prokinetic therapy. Prior interventions included botulinum toxin injection in 46 patients and feeding tube placement in 14.
Baseline GES was available for 52 patients, with a mean 4-hour retention of 68.2% ± 22.9%. Daily PPI use was reported in 50 patients (86.2%). Nine patients underwent pre-procedural pH testing, of whom 4 (44.4%) had abnormal DeMeester scores.
Procedural Details
G-POEM was performed at a median of 12.5 months after transplantation. At the time of the procedure, five patients were on aspirin, two on DOACs, and two on warfarin; Anticoagulants were appropriately interrupted and resumed post-procedure, while aspirin was continued.
Technical success was achieved in all cases. The mean total procedure time was 44.4 ± 25.4 minutes. Ten of 58 patients underwent G-POEM through the lesser curvature approach. The mucosal incision measured 17.1 ± 6.5 mm, the submucosal tunnel length 43.5 ± 15.9 mm, and the myotomy length 9.2 ± 3.5 mm. Full-thickness myotomy was performed in all patients, and mucosal closure was achieved using endoscopic suturing or hemoclips.
No intraprocedural bleeding occurred. All but three patients required at least overnight monitoring, with a mean length of stay of 2.4 ± 1.5 days, primarily for observation or unrelated indications.
Clinical Outcomes
Clinical success was observed in 73% of patients. No intraprocedural or delayed complications were reported. The mean GCSI score decreased significantly from 2.64 ± 1.13 at baseline to 0.89 ± 0.95 following G-POEM (Figure 1). Prokinetic use dropped from 63.8% before the procedure to 12% (seven patients) after. There was no statistically significant association between response to botulinum toxin injection and clinical response to G-POEM (Fisher exact test,
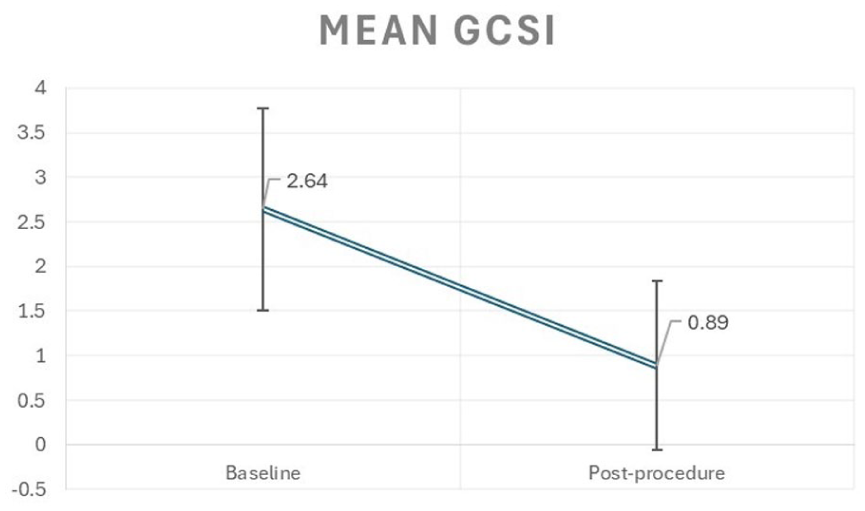
Change in Gastroparesis Cardinal Symptom Index (GCSI) score before and after G-POEM.
Follow-up GES was available in 36 patients (62%). Fourteen patients (38.8%) achieved normalization, 16 (44.4%) showed improvement, and six (16.7%) continued to have abnormal retention (Figure 2). Clinical response occurred in 71% of patients with improvement or normalization on GES compared with 60% of those without radiographic improvement; however, this difference was not statistically significant (
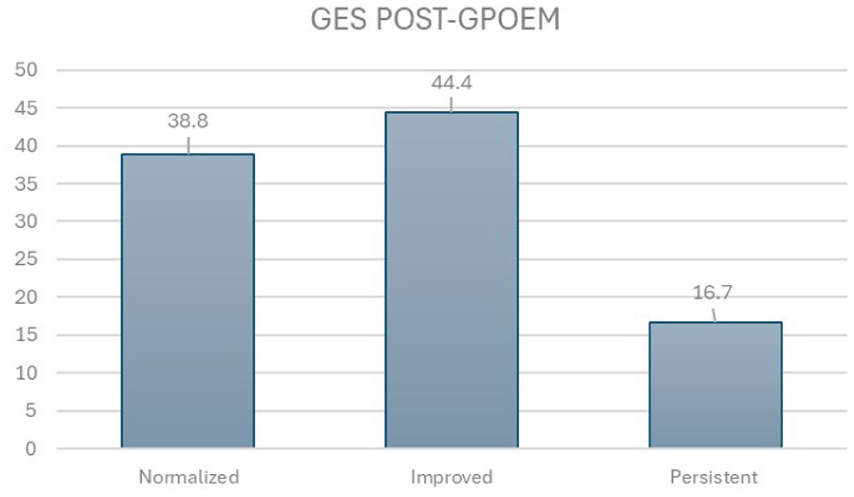
Follow-up gastric emptying study (GES) outcomes after G-POEM.
At the last follow-up, 45 patients were still receiving PPI therapy. Follow-up pulmonary function tests were available for 18 patients. The median interval between G-POEM and the most recent pulmonary evaluation was 92 days (IQR 27-155). The median predicted FEV1% was 84.5 (IQR 60.2-108) pre-G-POEM and 88 (IQR 63.5-107.5) post-G-POEM. Similarly, the median predicted FVC% was 66 (IQR 54-79) before the procedure and 81 (IQR 65-97.75) after G-POEM. Notably, none of the patients demonstrated a decline in pulmonary function compared with baseline.
Discussion
Our multicenter study demonstrates that gastric peroral endoscopic myotomy (G-POEM) is both safe and effective in managing refractory gastroparesis in patients following lung transplantation. A notable finding was that nearly one-quarter of patients were dependent on gastrojejunostomy (G-J) tube feeding at baseline, and approximately 70% of these individuals were able to discontinue tube feeds and transition to an oral diet after G-POEM. This degree of nutritional recovery has important implications for improving functional status and quality of life in lung transplant recipients, who often face substantial morbidity from nutritional compromise. 8 Furthermore, almost 80% of our cohort had previously undergone intra-pyloric botulinum toxin injection without meaningful benefit, underscoring that G-POEM can provide durable improvement even in patients refractory to other pylorus-directed therapies. The mean interval between lung transplantation and G-POEM was approximately 8 months, suggesting that earlier use of this intervention may help reduce morbidity and facilitate recovery.
Our findings are consistent with prior reports. In a multicenter study of 20 lung transplant recipients with refractory gastroparesis, clinical success was achieved in 85% of cases, with gastric emptying study (GES) improvement in 75% of patients with follow-up testing. 9 These results are comparable to those in our cohort and reinforce the reproducibility of G-POEM efficacy in this unique and complex patient population. One important difference was the pattern of proton pump inhibitor (PPI) use. In that study, all patients were on PPI therapy before G-POEM, which decreased to 25% afterward. In contrast, in our cohort, baseline PPI use was 97% and decreased only to 77.5% post-procedure, with most patients continuing daily therapy. The absence of post-G-POEM pH testing in our cohort limits assessment of reflux outcomes. This highlights the importance of objective reflux evaluation, particularly in lung transplant recipients where acid reflux may adversely affect pulmonary hygiene, allograft function, and risk of rejection. Beyond these cohorts, pooled data further support G-POEM efficacy. A meta-analysis of 104 patients across four studies reported an 83% clinical success rate, corroborating its benefit in refractory gastroparesis. 10
Interestingly, nearly 17% of patients in our study continued to demonstrate delayed gastric emptying despite G-POEM. This likely reflects the heterogeneity of gastroparesis pathophysiology, as not all patients have pyloric dysfunction or elevated pyloric pressure as the primary driver of their symptoms. These findings underscore the need to better distinguish patients with pylorus-driven disease from those with diffuse motility impairment, as the former group is more likely to benefit from G-POEM.
The principal strength of our study is that it represents the largest multicenter investigation of G-POEM in lung transplant recipients reported to date and demonstrates that the procedure can be performed safely and effectively across diverse practice settings. Importantly, no procedure-related complications were observed, further supporting its feasibility in this complex patient population.
Several limitations must be acknowledged. The relatively short follow-up, with gastric cardinal symptom index (GCSI) scores and pulmonary function data limited to 3 months, limits assessment of the durability of response and the long-term impact of G-POEM on lung function and graft-related outcomes. Reflux was not systematically evaluated using objective testing, and measures of bile reflux were not available, limiting evaluation of reflux-related complications in this population. Additionally, the retrospective design, small sample size, and absence of key measures such as quality of life assessments introduce potential selection bias and uncontrolled confounding. Finally, Lack of standardized post-procedural protocols across centers may also have contributed to heterogeneity in outcomes.
Conclusions
In conclusion, G-POEM achieved a high rate of clinical response in lung transplant recipients with refractory gastroparesis, with no reported procedure-related complications. Given its favorable safety and efficacy profile, G-POEM should be considered earlier in the management algorithm for this high-risk population. Future prospective studies with larger cohorts and longer follow-up are needed to confirm these findings and clarify the impact of G-POEM on nutritional status, quality of life, and lung transplant function.
Footnotes
Ethical Considerations
The ethics committee of the University of Pittsburgh waived the need for ethics approval and patient consent for the collection, analysis and publication of the retrospectively obtained and anonymized data for this non-interventional study (approval: 24060076).
Author Contributions
Babak Mirminachi contributed to the conception and design of the study, investigation and data curation as well as drafting the article. Lizeth Cifuentes, Abel Joseph, Christopher Farid and Hashem Albunni contributed to the investigation and data curation. Joo Ha Hwang, Andrew Li, Alexander Podboy, Mohammad Al-Haddad, Chadi A. Hage and Albert Ha provided critical revision of the article for important intellectual content. Sultan Mahmood contributed to the conception and design of the study and provided critical revision of the article for important intellectual content. All authors gave final approval of the version to be published.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Joo Ha Hwang has served as a consultant for Olympus, Boston Scientifc Corporation (BSC), Medtronic, FujiFilm, EndoRobotics, Lumendi, Neptune and Erbe Endoscopy. The other authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Use of Artificial Intelligence
No artificial intelligence (AI) was used in the preparation of this manuscript.
