Abstract
Background
Subglottic stenosis (SGS) is a complex medical condition marked by airway narrowing. Studies implicate gastroesophageal reflux disease as a potential contributing factor for SGS, however the diagnostic standard and pathogenesis are unknown. This study sought to characterize esophageal structure and function in patients with SGS using multimodal diagnostic testing to address gaps in the current understanding of esophageal involvement in this population.
Methods
We performed a retrospective single-center review of adults with SGS who underwent esophageal evaluation at a tertiary referral center between January 2014 and June 2024. Patients were included if they had laryngoscopically-confirmed SGS and completed esophageal function test(s) including esophagogastroduodenoscopy (EGD), high-resolution manometry (HRM), esophageal pH testing, and/or barium esophagram. Demographics, SGS characteristics, and esophageal test results were analyzed descriptively.
Results
Among 72 patients (mean age 54.3 years; 87.5% female), most (41.7%) had idiopathic SGS. Esophageal symptoms were reported in 91.7% of patients. Abnormal findings were identified by at least one modality in over half of cases: EGD (53.6%, most commonly hiatal hernia), HRM (53.8% abnormal), pH testing (52.9% abnormal acid exposure), and barium esophagram (62.5% abnormal, including dysmotility and intraesophageal reflux). Notably, 58.8% of patients with normal EGD demonstrated abnormalities on subsequent esophageal function testing.
Conclusions
Esophageal abnormalities were highly prevalent in patients with SGS. These findings suggest that a low threshold for comprehensive esophageal evaluation is warranted in patients with SGS. Future studies should evaluate whether targeted esophageal interventions improve SGS outcomes.
This is a visual representation of the abstract.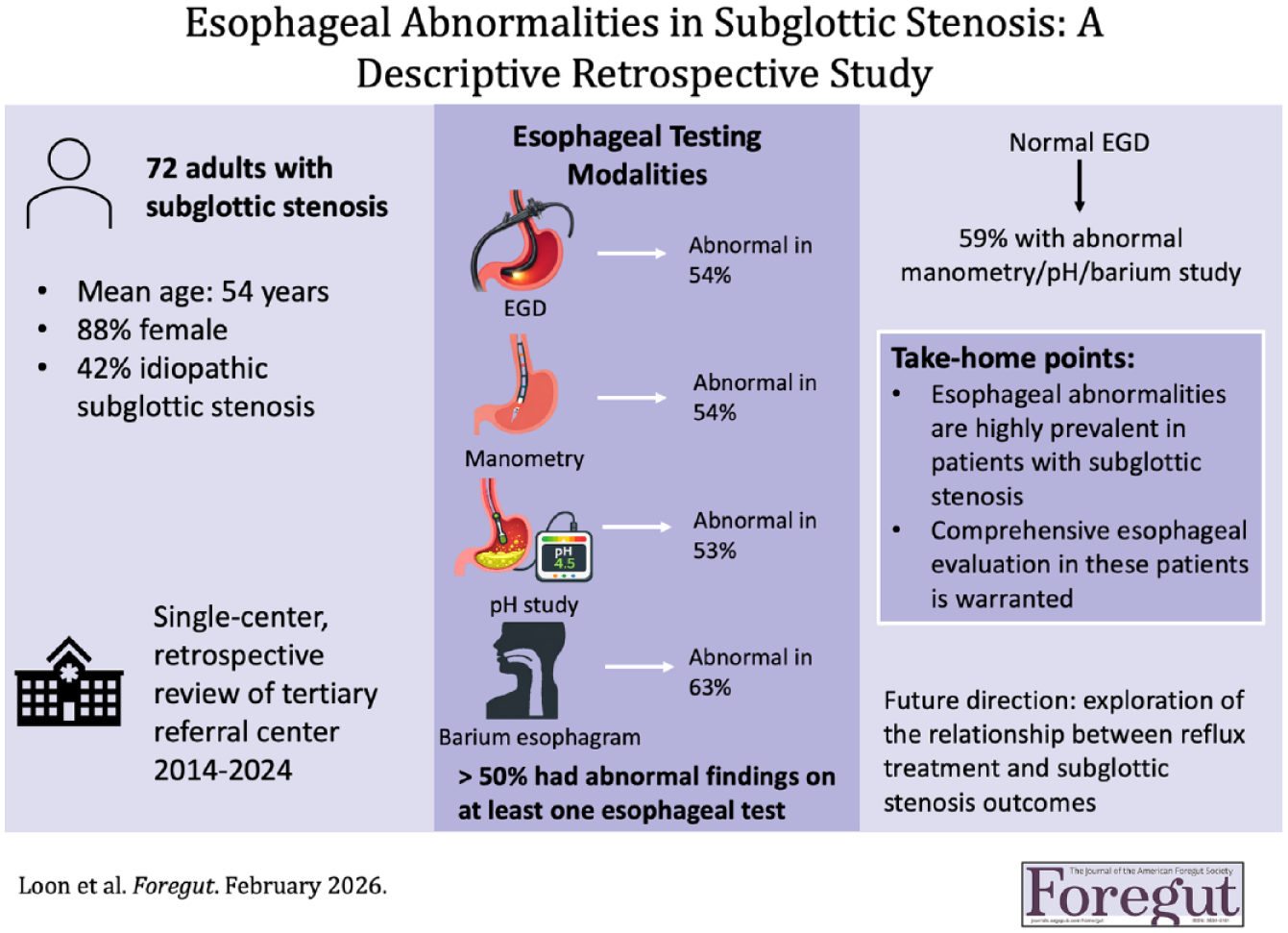
Get full access to this article
View all access options for this article.
