Abstract
Herpes zoster (HZ) or shingles is an acute and self-limiting viral infection caused due to reactivation of varicella zoster virus. The virus remains latent in the ganglionic neurons, and during states of reduced cell-mediated immunity, as in the elderly and immunocompromised, the virus reactivates and travels along the nerve fibres peripherally. The result is a painful vesicular rash, which should typically be localised to a single dermatome and not cross the midline. In some cases, however, the infection may have a varied and atypical presentation, including disseminated HZ, multidermatomal or bilateral HZ, glioma and acute cerebral angiitis. A prompt diagnosis and early initiation of antiviral therapy can prevent the occurrence of postherpetic neuralgia and neurological sequelae, and also enable early disease resolution.
We report the case of a 27-year-old man with severe HZ infection of all the divisions of the trigeminal nerve. A robust knowledge of such atypical disease presentations would enable improved patient outcomes.
Background
Herpes zoster (HZ) is a common self-limiting infection characterised by a unilateral vesicular eruption. It is caused by the varicella zoster virus, which remains latent in the sensory ganglia and is reactivated with ageing or immunosuppression. 1 The condition has an incidence of 3-5/1,000-person years in Europe, North America and Asia, subsequently increasing with age. 3
We report a case of a patient with multiple vesicular eruptions over the face accompanied by pain. The patient had no identified risk factors contributing to the atypical presentation despite the lesions being characteristic of HZ. The case demonstrates the fact that common diseases can present in an atypical manner and highlights the importance of having knowledge of such atypical presentations in order to initiate treatment at the earliest and avoid significant complications.
Case Presentation
A 27-year-old truck driver presented with complaints of high-grade fever for 1 week, followed by multiple, painful rashes on the face and painful oral ulcers. The patient revealed a history of chickenpox as a child and childhood asthma, which has since resolved.
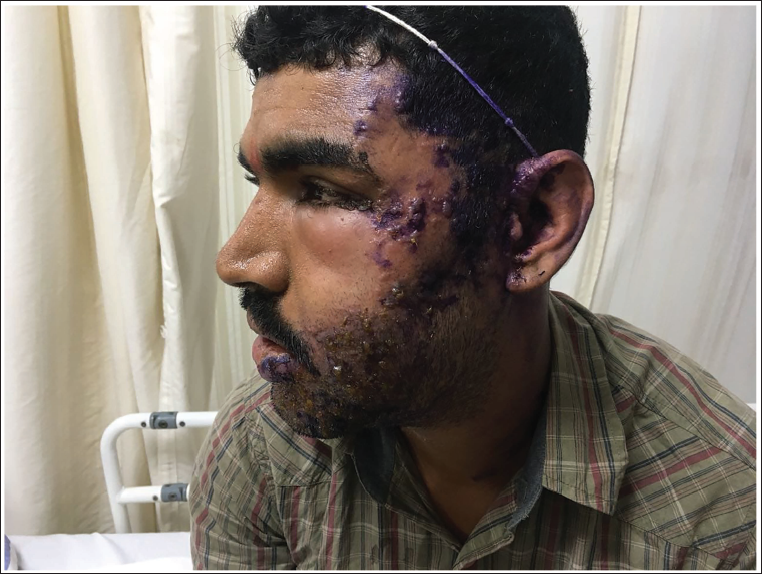
On examination, he was normotensive with a blood pressure (BP) of 120/70 mmHg, a pulse rate of 78 bpm and afebrile. Local examination revealed clusters of fluid-filled vesicles with surrounding redness over the left side of the face (Figure 1), not crossing the midline, also involving the ear and the jaw. Multiple ulcers were noted over the left buccal mucosa and the left half of the tongue (Figure 2). On examination of the eyes, congestion was noted in both eyes. Similar lesions were not found on any other site of the body on detailed examination. Other systemic examinations proved unremarkable.
Clusters of Vesicles Over the Left Side of the Face Including the Ear.
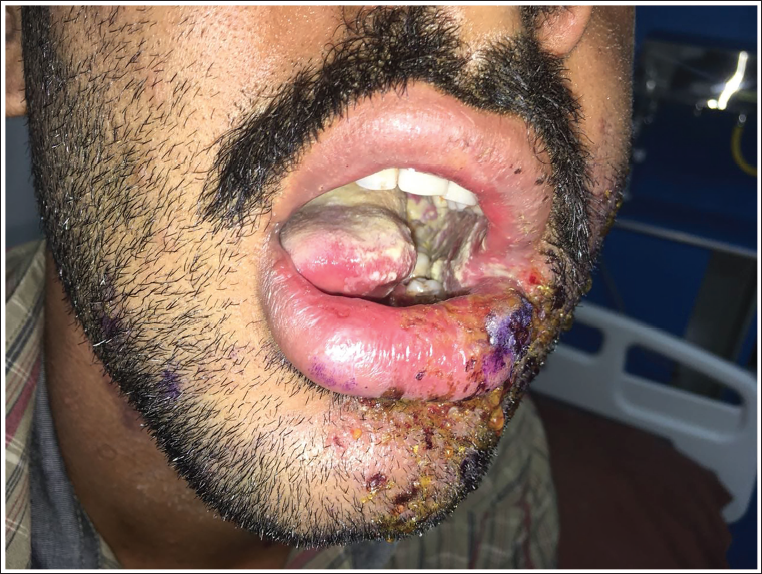
Multiple Lesions Present Over the Left Half of the Lower Lip and Intraoral Ulcers Over the Left Buccal Mucosa and Tongue.
Investigations
Routine haematological and serological investigations that were done for the patient were within normal limits, and any underlying cause for immunosuppression was ruled out. Complete blood counts were within normal limits, and peripheral smear examination showed monocytosis.
Diagnosis
In the context of the history provided, with the clinical findings of multiple vesicles present over the left half of the face, not crossing the midline, in a dermatomal distribution with no evidence of facial palsy, a diagnosis of HZ of the complete dermatomal distribution of the trigeminal nerve was made.
Treatment
Patient was initiated on oral antivirals (tablet Valacyclovir 1 g once daily for 1 week), with IV antibiotics (injection Cefotaxime 1 g thrice daily and injection Clindamycin 600 mg thrice daily) and oral antifungals (tablet Fluconazole 100 mg once daily) for prophylaxis against secondary bacterial and fungal infections, respectively, and topical moisturisers. Tablet Pregabalin 75 mg twice daily was started to provide adequate analgesia, and subsequently tapered to once daily after a week.
Patient improved symptomatically and was discharged. On follow-up after 1 week, the patient reported marked clinical improvement with a reduction in pain and no fresh vesicles being noted.
Discussion
Varicella zoster virus causes two distinct clinical diseases. Varicella (chickenpox) is the primary infection, and its recurrence results in a unilateral vesicular eruption referred to as HZ (shingles), commonly in the elderly and immunocompromised host.
These eruptions most commonly involve the thoracic and lumbar dermatomes. Disease onset is typically heralded by pain within the affected dermatome, preceding the appearance of lesions by 2–3 days. This is followed by the development of vesicular lesions, which may coalesce to form bullae. Lesions usually evolve over 3–5 days, and the entire disease course spans approximately 10–15 days. The condition characteristically involves a single dermatome corresponding to one dorsal root or cranial sensory ganglion.
Disseminated zoster is seen in immunocompromised patients and involves three or more dermatomes, and usually arises on a background of some underlying skin disease such as eczema or atopic dermatitis. It is defined as >20 skin lesions beyond the primary or adjacent dermatomes, according to a clinical trial by Whitley et al. 4 It is estimated to occur in 2%-5% of all HZ infections.
Another rare presentation of HZ is HZ duplex unilateralis or bilateralis, which has an incidence of less than 0.1% and refers to HZ occurring in two, noncontiguous, widely separated dermatomes. 5
Disseminated enteroviral infections may also cause widespread distal vesicular lesions. However, these rashes are usually morbilliform with a haemorrhagic component rather than vesicular or vesiculopustular, involving the palms, oropharynx and soles.
Unusual cutaneous manifestations in addition to HZ ophthalmicus include involvement of the maxillary or mandibular branch of the fifth cranial nerve, which results in intraoral involvement with lesions over the palate, tonsillar fossa, roof of the mouth and tongue.
The most significant manifestations of HZ are the associated acute neuritis and postherpetic neuralgia, which are uncommon in young people. Rare manifestations include cerebral angiitis, which follows zoster ophthalmicus. HZ has been recognised as a frequent infection in human immunodeficiency virus (HIV)-infected hosts, occurring in 8%-11% of patients. 6
While HZ is usually self-limiting, the early administration of antivirals, ideally within 72 h of the development of skin lesions, and symptomatic treatment results in a significant reduction in morbidity. Acyclovir (800 mg, 5 times a day/7 days), famciclovir (500 mg, 3 times a day/7 days) and valacyclovir (1 g, 3 times a day/7 days) are effective antivirals.
According to a review article published by Wareham et al., the inclusion of oral prednisolone in treatment has been shown to reduce the pain, quicken the healing of lesions, with earlier recovery to daily activities. 7 Therefore, steroids may be considered in elderly patients with significant pain without any contraindication to steroids. The use of steroids with acyclovir in acute idiopathic facial palsy is also advised. However, they have failed to show a demonstrable effect in the management of postherpetic neuralgia.
According to a review article by Koshy et al., the incidence of HZ is 3-5/1,000-person years in Europe, North America and Asia, with an increased incidence of 6-8/1,000-person years by age 60, with the incidence higher at 12/1,000-person year by 80 years of age. 3
A study by di Legami et al. had demonstrated an increased incidence of hospitalisation for HZ in patients with advancing age. A higher incidence of HZ among immunocompromised individuals is seen compared to the healthy population, according to various studies. 8
HZ, initially thought to not recur more than once in an individual, is now estimated to recur in 5.7% of immunocompetent people, with a higher risk in the immunocompromised population, according to a study by Yawn et al. 9 This demonstrates that, though rare, HZ can occur in immunocompetent individuals and needs to be considered in order to ensure favourable patient outcomes.
Learning Points
Herpes is an extremely common medical condition. While HZ is classically seen in the immunocompromised and elderly, cases of recurrent and multidermatomal HZ have been described even in immunocompetent patients.
Early detection and prompt initiation of antivirals aid in recovery and minimise the risk of the development of complications like postherpetic neuralgia, which can be difficult to effectively manage.
Footnotes
Authors Contribution
BA and NVD were the main contributors to the concept, design of the report and critically revised the final draft of the article. SS, TS and MAM collated the case report data from the patient records and drafted the article. All authors critically revised and approved the final manuscript for publication.
Declaration of Conflicting Interests
The authors declared no conflict of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval and Informed Consent
The ethical consent was obtained from the Institutional Ethics Committee. Written informed consent has been obtained from the next of kin for the publication of this case.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
