Abstract
Background:
A cancer diagnosis and its treatment can profoundly disrupt an individual’s life, often prompting a reevaluation of personal goals, relationships, and self-identity. Qualitative research has documented experiences of emotional transformation, altered life priorities, and personal growth in cancer survivors. Many struggle to maintain normalcy while adapting to a reality shaped by the illness. This study is motivated by a critical gap in cancer care, that is, a holistic understanding of patients’ lived experiences in their journey. The study aimed to explore key aspects of cancer patients’ experiences, including disease-related factors, as well as their psychosocial and emotional transitions over time.
Methods:
A qualitative research design was adopted using in-depth interviews (life course transition approach). The study employed a life course perspective to examine the cancer journey across three primary thematic phases: (a) Initial diagnosis—exploring both the negative and positive impacts of receiving a cancer diagnosis; (b) Confinement and restrictions—addressing the emotional and psychological effects following diagnosis, including lifestyle changes and limitations; and (c) Obstacles of the cancer journey—identifying ongoing challenges during treatment and survivorship. Each phase encapsulated a range of biopsychosocial factors (codes), which were categorized as either negative (e.g., deterioration of health, treatment side effects, emotional distress, financial burden) or positive (e.g., support from family, friends, and healthcare providers that foster resilience and coping).
Results:
The study revealed that the cancer journey unfolds in distinct yet interconnected phases starting from diagnosis, and carried through treatment, survivorship, and end-of-life care. Each phase presents a set of unique challenges and thus the corresponding transitions in the life course. Psychosocioeconomic dimensions, particularly social support, stigma, sense of contagion, individual coping mechanisms resilience, role of health insurance have emerged as pivotal in influencing patients’ health trajectories. Importantly, effective communication with healthcare providers and the consistent delivery of patient-centered care facilitate smoother transitions.
Conclusion:
This research highlights the critical role of psychosocial and financial determinants and the importance of phase-to-phase continuity in cancer care. The findings underscore that effective healthcare communication and a patient-centered approach are essential for supporting patients through the evolving complexities of their cancer journey.
Background
A cancer diagnosis and its treatment can significantly disrupt an individual’s life course, prompting a redefinition of goals, relationships, and identity. Qualitative studies reveal themes of personal growth, shifting priorities, and efforts to maintain normalcy. A life course perspective helps illuminate how past experiences and social factors shape the cancer journey, highlighting its transformative nature and the need for targeted support during such critical transitions.
The concept of liminality offers insight into the transitional experiences of cancer patients, capturing the in-between state where individuals are neither their former selves nor fully adjusted to survivorship. 1 Young adults face distinct emotional and social challenges during this critical life stage, including struggles with identity, autonomy, and peer relationships.2,3 For those with incurable cancer, themes like “approaching death,” “preparing to leave,” and “holding on to life” reflect complex emotional transitions. 4 These findings highlight the need for holistic care that addresses both physical and existential dimensions.
Integrating a life course perspective in cancer research calls for methods capturing patients’ evolving, subjective experiences. Qualitative approaches like in-depth interviews and phenomenological analysis uncover how individuals find meaning in illness. For example, Moskalewicz et al. explored “lived time” during chemotherapy in ovarian cancer patients, highlighting the importance of positive emotions and authentic living. 5 Thoresen et al. emphasized patients’ navigation of the liminal space between health and illness and the critical role of social support. 6 Shaffer et al. demonstrated through a dyadic study the intertwined physical and mental health of patients and caregivers, reinforcing the need for holistic, family-centered care. 7
Recent qualitative studies highlight the significance of transitions and trajectories in cancer patients’ experiences. Burton-Jeangros et al. show that a life course perspective captures how early life, and social factors shape health over time. 8 Carr et al. emphasize social support and wellness in older adults. 9 The concept of “biographical disruption” explains how illness alters life paths (Solberg et al. 10 ). Hansen et al. advocate person-centered care that integrates medical events with patients’ values and evolving needs. Life course perspective also involves renegotiating roles within family and society. 11
Solberg et al. highlighted patient experiences of fragmentation and lack of holistic care in standardized cancer pathways, described as feeling “lost in the loop.” 10 Hamilton et al. found that women with genetic cancer risks made health decisions influenced by concerns for family, showing how health trajectories are deeply interconnected. 12 Ratcliff et al. used narrative analysis to reveal the individualized, non-linear nature of cancer recovery, emphasizing the need for personalized survivorship care. 13 Foster and Fenlon applied the Illness Trajectory Framework to stress the critical transition from treatment to survivorship. 14 These studies collectively support the life course perspective’s focus on dynamic, cumulative health trajectories, and the importance of tailored, person-centered care (Carr et al. 9 ).
The life course perspective emphasizes the transitions, trajectories, and contextual factors that shape cancer patients’ experiences and resilience, and thus the center of this paper. This research addresses a key gap in cancer care: the lack of holistic understanding beyond medical treatment, often overlooking emotional, social, and economic challenges. Rooted in a commitment to improving care quality, it advocates for personalized, culturally sensitive, and patient-centered approaches. By exploring the full cancer journey from diagnosis to treatment, survivorship, or end-of-life care, it highlights the need to address not just physical health but also psychological and socioeconomic well-being. It also recognizes the vital roles of healthcare providers, families, and support networks, for example, health insurance in shaping patients’ lives.
Methods
A cross-sectional qualitative study was conducted with a purposive sample of 20 cancer patients, focusing on those who were primary breadwinners. Participants under 28 and those not serving as breadwinners were excluded to ensure consistency and relevance in the data. The rationale behind such criteria are (a) individuals under 28 years old are in their early career, for example, pursuing education, often unmarried, yet to be employed, and have different psychosocial, financial, and family responsibilities, which poses as a different spectrum of coping strategies, socioeconomic support, and quality of life when compared to those over this age bar; (b) the principal focus of cancer survivorship research is to examine the social, financial, and employment-related issues as the impact of the illness among breadwinners, compared to non-breadwinners; (c) breadwinners of 28 years old and above yields a more comparable homogeneous sample than the mixture; and (d) as the study focuses on understanding adult survivorship outcomes, such as job losses, financial hardships, impaired work–life balance, excluding younger non-breadwinning population brings more relevance in the study.
The study explored key aspects of cancer patients’ experiences through three sections: demographics, medical history, and life transitions. The first gathered basic details (e.g., age, gender, education, family financial status) are used to profile participants. The second captured disease-related data, including cancer type, stage, time since diagnosis, treatment, and remission status. The third examined life transitions, focusing on health impacts, physical functioning, financial confidence, daily routine changes, relationship dynamics, challenges, shifting priorities, economic strain, and social engagement, highlighting the psychosocial and emotional dimensions of their journey. Additional questions explored life before and during treatment, changes over time, support received (both professional and financial), and advice for others going through similar transitions. These insights aimed to offer a holistic view of the medical and psychosocial challenges and transformations experienced by cancer patients.
Data analysis
Data analysis was conducted alongside data collection. It took interpretivist–constructivist epistemological stance, where due recognition had been provided on the experience of the participants from where meaning of cancer survivorship had been socially conceptualized, constructed, contextualized, and presented. Audio-recorded interviews were transcribed and coded line by line to identify categories, meanings, and processes. Focused hybrid (mixture of both inductive and deductive) coding highlighted recurring themes, which were then systematically compared to define their attributes. The rationale behind adopting hybrid coding in survivorship is due to its multivariate nature, culturally shaped, and an evolving change of life expectations in survivors following treatment, which is evident in this paper. While self-concept, role change, and body image refer to ‘deductive coding’, liminal identity, perceived disconnection, and anticipatory uncertainties fall under ‘inductive coding’. Thematic analysis was also used to identify connections and integrate the codes. 15 It helps identifying, analyzing, and interpreting patterns of meanings, that is, the themes across the qualitative dataset of 20 cancer survivors, described in this paper. Thematic analysis helps identify key themes and codes capturing the multifaceted experiences of cancer patients from diagnosis onward, presented as individual models by organizing codes into broader patterns (candidate themes) and in turn clustering the similar codes across the dataset. An example of thematic saturation, here, is codes such as ongoing anxiety due to various biopsychosocial factors, fear of recurrence and its adverse consequences in the future life, especially at the socioeconomic perspective, can be clustered as “living with ongoing anxiety.” The epistemological stance (contextualist-interpretivist-constructivist) fits with Braun and Clarke’s thematic analysis by its essence of constructionism, contextualism, and interpretivism, because the themes are interpreted, that is, meanings are deduced, subjectivity is not eliminated but accommodated, and reality is not taken as a single objective.
Model 1 explores the “immediate emotional and psychological impact” of a cancer diagnosis, highlighting themes such as emotional turmoil, uncertainty, and a reevaluation of priorities. It also addresses the significant economic burden faced by patients, including financial stress, work and income disruption, treatment costs, and insurance challenges. Additionally, the theme of support systems emphasizes the crucial role of family, healthcare teams, and peer networks in helping patients cope with their cancer journey (see Figure 1).

Initial impact of cancer diagnosis and its negative and positive effects.
Model 2 highlights the theme of “Confinement and Social Restrictions,” revealing how treatment-related limitations lead to isolation, strained social activities, and role changes that affect patients’ daily lives. The “Post-Diagnosis Reaction” theme explores evolving emotional responses, information seeking, and coping strategies. Additionally, “Maintain Secrecy” addresses the psychological toll and challenges patients face when deciding whether to disclose their diagnosis (see Figure 2).

Confinement and social restrictions following a cancer diagnosis and its psychosocial effects.
Model 3, “Barrier to Self-Management,” highlights challenges patients face in managing their health, including treatment side effects and physical limitations. This theme underscores the diverse obstacles encountered during the cancer journey and the need for comprehensive support and tailored care to address these complexities (see Figure 3).
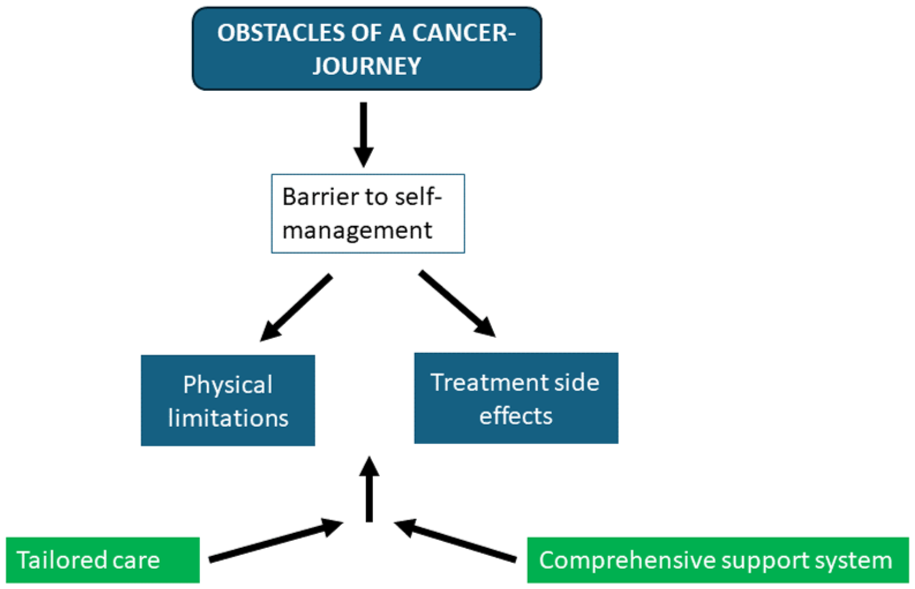
Obstacles of a cancer journey and its driving theme and codes.
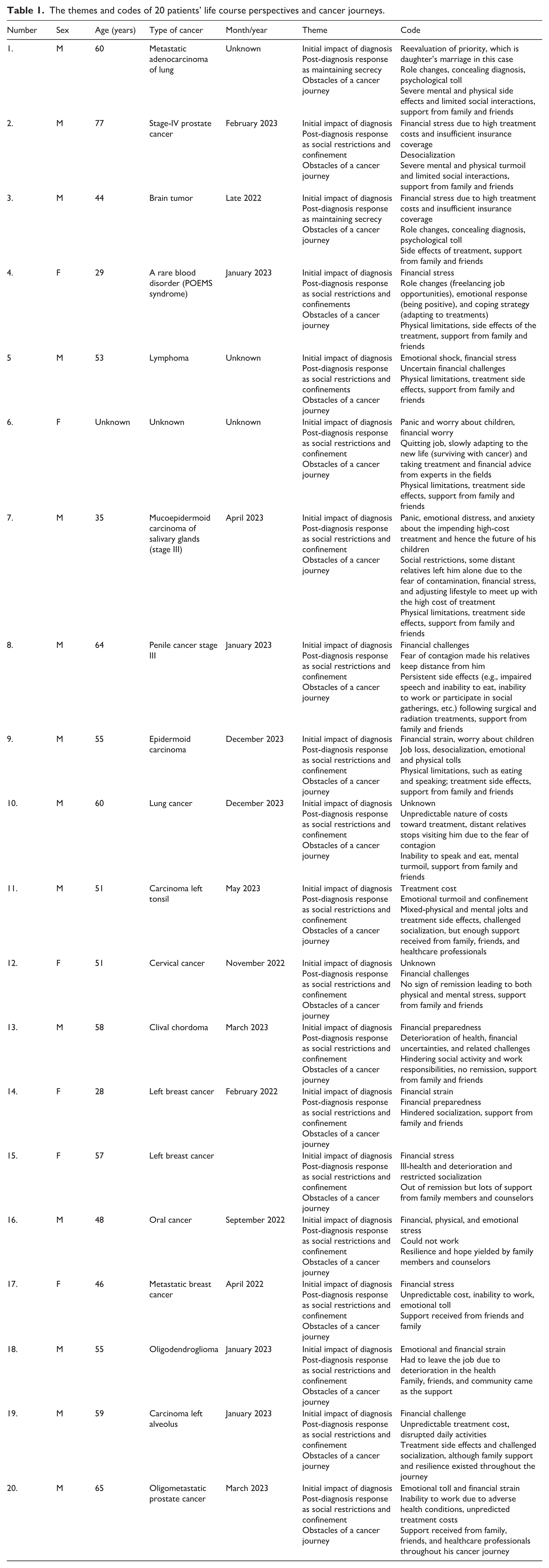
Inclusion and exclusion criteria: The study included participants aged 28 and above who were primary financial providers diagnosed with cancer. Individuals under 28 or not serving as primary breadwinners were excluded to maintain a consistent focus on a specific life stage. Consolidated themes and codes are presented in Table 1.
The themes and codes of 20 patients’ life course perspectives and cancer journeys.
Results
Case study 1: Navigating life transitions: A case study of a 60-year-old Mr. Saw metastatic adeno lung carcinoma
This case study explores the profound life transitions of Mr. Saw, a 60-year-old man from Dhanbad, Jharkhand, diagnosed with Stage-IV metastatic adenocarcinoma of the lung. As the sole breadwinner of his low-middle-class family, Mr. Saw lives with his wife and three children. His elder daughter’s wedding—a long-anticipated moment of joy—coincided with the shocking diagnosis, creating a deeply emotional and complex period in his life.
His illness began with persistent leg pain, initially dismissed as fatigue. A PET-CT scan revealed advanced lung cancer with metastasis, bringing unexpected grief at a time meant for celebration. Struggling to balance deteriorating health and familial responsibilities, Mr. Saw now faces the dual burden of cancer and the emotional weight of organizing a major life event.
Financial strain compounded the situation. With no knowledge of health insurance or available government schemes, Mr. Saw exhausted his fixed deposits—meant for his children’s future—to fund treatment and travel to the Apollo Proton Cancer Centre in Chennai. The ongoing costs have left the family economically fragile and emotionally stressed.
Fearing stigma and wanting to protect the joy of his daughter’s wedding, Mr. Saw and his wife chose to keep his diagnosis private, increasing their emotional burden. Despite the pain and fatigue, he remains actively involved in wedding preparations, often concealing his suffering to maintain a sense of normalcy for his family.
Mr. Saw’s journey reflects the complex interplay of medical, emotional, financial, and social challenges faced by cancer patients. It underscores the urgent need for holistic, patient-centered care that addresses not only treatment but also emotional support and financial counseling. His story calls attention to the importance of empathetic healthcare, greater awareness of medical schemes, and inclusive support systems to help families navigate cancer with dignity and resilience during life-altering transitions.
Case study 2: A businessman’s fight against prostate cancer
Mr. Jain, a 77-year-old businessman from Gurgaon, has been battling Stage-IV prostate cancer since February 2023. The diagnosis has severely affected his physical and mental health, causing persistent fatigue, weight loss, and increasing dependence on his wife for daily activities. The financial strain of his treatment, which has exceeded ₹25 lakhs, has been overwhelming due to inadequate insurance coverage.
While chemotherapy provided some relief from cancer symptoms, radiation therapy introduced challenging side effects such as fatigue, nausea, hair loss, and loss of appetite. These physical hardships, combined with the emotional impact of his diagnosis, have led to feelings of depression and anger.
Throughout this difficult period, Mr. Jain has drawn strength from the unwavering support of his family and friends. Their encouragement and assistance have been crucial in helping him focus on his health. He relies heavily on his wife to manage important tasks, highlighting the essential role of a strong support system in coping with cancer treatment.
The diagnosis has transformed Mr. Jain’s outlook, placing his health as his foremost priority. Despite anticipating future financial difficulties and harboring fears about treatment efficacy, pain, and mounting costs, he remains hopeful, bolstered by his family’s support.
Mr. Jain’s extreme fatigue and weakened immune system have drastically limited his social interactions and diminished his quality of life. The challenges posed by radiation therapy have been especially severe. His experience underscores the critical need for comprehensive health insurance plans to reduce the financial burden on patients.
Mr. Jain’s story highlights the complex physical, emotional, and financial challenges cancer patients face. He advocates for better insurance coverage and government policies and encourages fellow patients to maintain a positive outlook throughout their journey.
Case study 3: Managing life and health: Mr. Kumar’s journey with brain tumor
Mr. Kumar, a 44-year-old resident of Chennai, was diagnosed with a critical brain tumor in late 2022. The illness significantly affected his health, leading to fatigue, persistent pain, and disruption to his daily activities and business. While his condition has improved post-treatment, he still experiences discomfort. Despite this, Mr. Kumar remains cautiously optimistic, rating his health at 8 out of 10 due to partial pain relief.
The absence of health insurance and lack of awareness about government healthcare schemes placed a substantial financial burden on his lower-middle-class family. The family resorted to using savings and selling valuables to cover treatment costs. Initially, misdiagnosis of symptoms like severe headaches and seizures delayed proper care. To shield their children from distress, Mr. Kumar and his wife chose to keep the diagnosis private.
As the sole breadwinner, Mr. Kumar faced overwhelming stress managing treatment costs, household needs, and his children’s education. Their experience revealed the importance of financial preparedness and better access to healthcare-related information. Though surgery brought some relief, side effects such as fatigue and physical limitations have hindered his ability to return to work. He now seeks alternative employment that suits his health condition.
Mr. Kumar’s greatest concerns revolve around ongoing treatment costs, future earning capacity, and his children’s well-being. Social life has been put on hold, and the family continues to struggle with stress, anxiety, and recurring symptoms. Nevertheless, supportive care from doctors and a determined mindset offer him hope.
His case underscores the need for timely diagnosis, better financial counseling, and widespread awareness about available healthcare schemes. Mr. Kumar’s journey reflects the emotional, physical, and financial toll of cancer and highlights the urgent need for holistic, accessible, and patient-centered care systems to support individuals and families through such life-altering transitions.
Case study 4: Living with POEMS syndrome—A young woman’s journey of resilience
A 29-year-old woman from Gurugram was diagnosed with POEMS Syndrome—a rare and complex blood disorder—in January 2023. Though supported by her middle-class family, the illness has severely impacted her physical health, independence, and emotional well-being.
Her symptoms began with numbness and tingling in one foot, progressing to swelling up to the knee and significant loss of mobility. Now dependent on a wheelchair, she rates her current health at 5 out of 10. Daily tasks have become increasingly difficult, and chronic pain has affected her mental health, often leaving her irritable and emotionally drained.
Prior to her diagnosis, she worked as a freelancer and found deep fulfillment in her career. However, her deteriorating condition forced her to pause work, leading to frustration and a sense of purposelessness. Initial treatment costs were covered by insurance, but ongoing care remains financially uncertain. While she is aware of insurance options, navigating them without proper guidance has been challenging. Her family’s income also excludes her from most public health schemes, restricting access to additional support.
Her emotional strength is bolstered by the unwavering care of her parents and the active involvement of close friends during treatments. Yet, becoming increasingly dependent has been difficult for her to accept, affecting her sense of autonomy and self-worth.
Physical therapy has eased some symptoms, offering hope for gradual recovery. However, persistent issues like hyperpigmentation, difficulty walking, and a reduced social life continue to affect her quality of life. Despite these challenges, she remains optimistic and urges others to seek timely medical care. Her journey is one of resilience, underscoring the need for inclusive healthcare for those battling rare and chronic conditions.
Case study 5: Mr. Thambi’s journey through lymphoma—A story of resilience and hope
Mr. Thambi, a 53-year-old resident of Trichy, Tamil Nadu, lived a modest life devoted to his family. His routine was disrupted when he began experiencing persistent back and stomach pain, initially dismissed as minor discomfort. However, as the pain worsened and began affecting his ability to work or manage daily activities, he sought medical attention. A series of diagnostic tests revealed lymphoma, a cancer of the lymphatic system—news that came as a shock to him and his loved ones.
His diagnosis marked the beginning of an emotionally and physically demanding journey. Thambi underwent surgery, chemotherapy, and radiation, each phase bringing intense pain, fatigue, and distressing side effects. These treatments left him dependent on others for basic daily tasks, significantly reducing his independence and quality of life.
With no health insurance and limited knowledge of government schemes, the financial strain was immense. The family relied heavily on savings, which were quickly depleted. The mounting medical bills, paired with uncertainty about outcomes, created overwhelming stress. Yet, amid this hardship, Thambi drew strength from his family’s unwavering care and support, both emotional and financial.
This ordeal reshaped his perspective on life. Priorities shifted from work and material aspirations to health, healing, and family bonding. His social circle narrowed, replaced by moments of introspection and gratitude. Despite the fear and exhaustion, Thambi and his family remained resilient, advocating for early diagnosis and strict treatment adherence.
Thambi’s journey is a testament to the power of familial love, emotional resilience, and perseverance. It highlights the urgent need for accessible, affordable cancer care, and awareness. His story stands as a reminder that even in the face of life-altering illness, hope, strength, and solidarity can pave the path to healing.
Case study 6: Navigating the journey of cancer treatment: A story of Kruthi
Kruthi’s health declined rapidly over 2 months, following 6 months of persistent headaches she initially dismissed as work-related stress. A previous doctor’s visit had found nothing alarming, offering her brief reassurance. However, escalating symptoms—sudden weight loss, extreme fatigue, and difficulty in movement—forced her to leave her job and pursue further medical evaluation. The cancer diagnosis came as a shock, triggering fear, anxiety, and deep concern for her children and the mounting costs of treatment.
While Kruthi had some financial safeguards through insurance and savings, the cost of ongoing care remained substantial. Her family had to make lifestyle and budgetary adjustments to accommodate medical expenses. Radiation therapy helped reduce the size of the tumor, but she continues to face serious side effects, including severe pain, memory lapses, and limited mobility, all of which have significantly impacted her ability to function day-to-day and engage socially.
Emotionally and physically, the journey has been exhausting. Yet, Kruthi draws strength from her family’s constant support and the compassionate care of her healthcare providers. Regular consultations and open communication with her insurance company have helped ease some stress, although the lack of professional financial counseling has left gaps in managing long-term care planning.
Her perspective on life has shifted dramatically. Once career-driven, Kruthi now values her health and family above all. She has become a strong advocate for early detection and preventive care, particularly for her children. She urges others not to ignore persistent symptoms and to seek specialist advice promptly.
Kruthi’s journey reflects the challenges of battling cancer and the transformative power of support, resilience, and timely care. Her story underscores the urgent need for affordable, accessible cancer services, and holistic support systems that address both medical and emotional well-being.
Case study 7: Mr. Thange’s battle with Stage-III Mucoepidermoid
Mr. Thange, a 35-year-old engineer from Thane, Maharashtra, was diagnosed with Stage-III Mucoepidermoid Carcinoma of the salivary gland in April 2023. His illness began with a painless lump in the jaw, initially mistaken for a throat infection. Rapid deterioration followed—significant weight loss, fatigue, and reduced mobility—disrupting his work and daily life.
He underwent major surgery and proton therapy, which brought limited symptom relief. Severe side effects, including difficulty speaking and eating, left him dependent on family support for basic activities. Rating his condition a 6 out of 10, he acknowledged occasional improvement but continued to suffer from pain and functional challenges.
The financial toll was significant. With a modest monthly household income of ₹35,000, even with some savings and insurance, the family struggled to meet rising medical costs. Unpredictable treatment expenses demanded strict budgeting and lifestyle sacrifices, placing long-term planning out of reach.
Emotionally, his parents provided unwavering care, and friends offered moral support. However, fear and stigma led some extended relatives to withdraw, intensifying his sense of isolation. Counseling services at the hospital proved vital in managing anxiety and strengthening his emotional resilience.
A former smoker, Mr. Thange now regrets his past habits and is determined to prioritize recovery and his child’s future. Though the tumor has shown signs of shrinking, persistent symptoms—pain, weakness, and impaired speech—continue to affect his quality of life. He is currently on medical leave, uncertain about resuming work.
His story underscores the importance of early medical intervention, emotional support, and financial preparedness. Mr. Thange’s journey is a testament to resilience in the face of adversity and highlights the pressing need for accessible cancer care and awareness of lifestyle-related risks.
Case study 8: Coping with penile cancer: Prasanth’s journey
Prasanth, 64, from Vellore, Tamil Nadu, was diagnosed with Stage-III penile cancer in January 2023. With only secondary schooling, he supports a household of four living on ₹50,000 a month from two earners. The first warning—a painless lump in his mouth and jaw—was mistaken for a throat infection. Within weeks, he struggled to swallow, shed weight, and grew too weak to move easily.
Surgery followed by radiation has yielded uneven results. The tumor burden has lessened, and pain has eased, yet relentless side effects—slurred speech, raw throat, and an inability to enjoy solid food—still erode his quality of life. He scores his condition a cautious 6 out of 10. Although insurance and savings cushion expenses, the open-ended costs of travel, follow-up scans, and special nutrition have forced the family to trim non-essentials and dip into savings.
Emotional scaffolding has proved as important as clinical care. His elderly parents, his wife, and close friends remain constants, attending appointments and celebrating minor victories. Some relatives, frightened by stigma, have drifted away, a quiet hurt he chooses not to dwell on. Hospital-run counseling sessions have given him practical coping tools—guided breathing, journaling, goal setting—and help steer dark thoughts toward manageable tasks.
Coming from a small village, the jargon of oncology once terrified him, but months of consultations have made him an informed, assertive participant in his care. He rues decades of tobacco use, convinced it played a part in his diagnosis. His advice is simple: heed lingering symptoms, seek expert help early, lean on your circle, and cultivate resilience. Cancer, he says, tests finances, body, and spirit, yet with timely treatment, community support, and personal resolve, hope survives.
Case study 9: Managing epidermoid carcinoma: Ms. Kirthi’s journey
Ms. Kirthi, a 55-year-old postgraduate and former bank clerk from Tirupati, Andhra Pradesh, was diagnosed with Epidermoid Carcinoma in December 2023. Despite a monthly family income of 1 lakh, the financial strain has been significant since he stopped working in December 2022. His health has deteriorated since the diagnosis, with symptoms including a painless lump in his mouth and jaw, difficulty swallowing, and eventual significant weight loss and fatigue. He rated his condition as 6 out of 10 due to intermittent pain and side effects from the treatment, which have severely affected his ability to speak and eat.
Kirthi has experienced a decline in strength and mobility, making daily activities challenging. Financial management has been difficult, despite using insurance and savings, as the unpredictable nature of medical expenses poses a constant concern. Support from his parents and friends has been crucial, though extended family from his rural village has distanced themselves. The emotional and physical toll of the disease and treatment has required significant emotional support, especially after his speech and food intake were affected post-surgery.
The treatment process has also impacted on his economic stability, necessitating lifestyle adjustments. Although there is hope from radiation treatment and surgery, ongoing side effects have left him dependent on others and unable to participate in social activities or continue his job. Throughout his journey, he has faced emotional distress, fear for his children’s future, and challenges in social interactions and work responsibilities. Support from healthcare professionals and counseling sessions has helped him manage these difficulties. Kirthi’s advice to others is to seek medical consultation promptly, educate themselves about their condition, and maintain a positive mindset. His experience highlights the importance of early intervention and emotional and financial support in managing life with cancer.
Case study 10: Navigating the challenges of lung cancer treatment
Mr. Manjunath, a 60-year-old farmer from Secunderabad, Andhra Pradesh, was diagnosed with lung cancer in December 2023. His symptoms began with a painless lump in the mouth and jaw, causing difficulty swallowing and eating—initially mistaken for a throat infection. However, his condition quickly worsened, leading to sudden weight loss, fatigue, weakness, and reduced mobility. A PET-CT scan confirmed the diagnosis, and he now rates his health as 6 out of 10, struggling with fluctuating pain and side effects such as impaired speech and difficulty eating.
Once an active, independent farmer, Mr. Manjunath now depends on others for basic daily tasks. The loss of stamina and autonomy has deeply affected his sense of self. Despite these challenges, he remains determined to fight the disease and regain stability.
Financially, the burden has been heavy. Although initial expenses were covered through insurance and savings, ongoing treatment, medication, and travel costs have strained the family’s resources. With Mr. Manjunath unable to work, lifestyle adjustments and tighter budgets have become necessary.
Emotional support from his parents and close friends has been crucial. While some extended family members distanced themselves due to stigma and misconceptions, his core support network provided unwavering care and encouragement. Counseling services at the hospital have also helped him manage anxiety, fear, and emotional exhaustion.
Regretting his occasional smoking history, which he suspects contributed to his illness, Mr. Manjunath now focuses on managing his health, supporting his family, and repaying friends who helped financially. He continues to cope with lingering effects of surgery and radiation, including fatigue, pain, and limited speech.
His journey highlights the importance of early diagnosis, health education, and a strong support system. He urges others to take symptoms seriously and seek timely care, emphasizing resilience and hope amid illness.
Case study 11: Mr. Agarwal diagnosed with carcinoma left tonsil
Mr. Agarwal, a 51-year-old male from Kolkata, was diagnosed with carcinoma left tonsil in May 2023. Despite his higher secondary education, his health deteriorated rapidly, experiencing difficulty swallowing and eating due to a painless lump in his mouth and jaw. His daughter described his overall health at a 6 out of 10 during treatment, noting a decline in physical performance, including weakness and weight loss. Financial management became challenging, despite family support, as the treatment’s unpredictability strained their budget, impacting their economic stability.
The diagnosis not only affected Mr. Agarwal’s physical health but also strained his emotional well-being and family relationships. Facing the fear of the unknown and the financial burden of treatment, Mr. Agarwal’s priorities shifted toward securing his family’s future. The treatment’s side effects further restricted his social activities, leaving him unable to engage in gatherings or fulfill work responsibilities.
While the treatment journey brought hardships, there were moments of hope and support. Despite setbacks, Mr. Agarwal found solace in the care provided by healthcare professionals and the emotional support from loved ones. Access to counseling sessions at the hospital offered valuable guidance, helping the family navigate through the challenges. Looking ahead, Mr. Agarwal emphasized the importance of seeking support, consulting healthcare professionals, and maintaining a positive mindset in facing similar transitions. Overall, Mr. Agarwal’s journey underscores the multifaceted impact of cancer diagnosis on individuals and their families, highlighting the need for holistic support systems and financial assistance to manage the transition effectively.
Case study 12: Navigating cancer’s challenges of Ms. Dua
Ms. Dua, a 51-year-old woman from Andaman and Nicobar, was diagnosed with Carcinoma Cervix in November 2022. Despite undergoing surgery and chemotherapy, she continues to battle the disease without remission. Her health has deteriorated significantly, with persistent pain and difficulty eating or swallowing, severely impacting her daily life. Alongside the physical challenges, the financial strain from ongoing medical expenses adds to her stress, highlighting the complex burdens cancer places on patients and their families.
Ms. Dua’s illness has also affected her personal relationships, though she finds strength in the steadfast support of her husband and close friends. Their encouragement provides crucial emotional solace amid her struggles, illustrating the vital role of social support in coping with serious illness. Beyond her health, Ms. Dua faces uncertainty about her ability to work and participate in social activities due to treatment side effects and overall weakness. This situation reflects the wider societal impact of cancer, affecting economic stability and social engagement.
Amid these difficulties, counseling sessions have become a refuge for Ms. Dua, offering emotional support and a safe space to express fears and anxieties. Such holistic care addresses not only physical symptoms but also the emotional and psychological needs of cancer patients. Ms. Dua’s journey underscores the resilience needed to navigate cancer’s challenges and emphasizes the importance of comprehensive support systems. Integrating medical treatment with emotional and financial assistance is essential to help patients like Ms. Dua manage the multifaceted impacts of cancer and improve their quality of life during this arduous journey.
Case study 13: Understanding cancer’s impact through life—Mr. Gupta
Mr. Gupta, a 58-year-old from Bhilwara, Rajasthan, was diagnosed with Clival Chordoma in March 2023. Despite treatments like surgery and chemotherapy, he remains out of remission, facing numerous challenges that extend beyond his health. Mr. Gupta’s health has deteriorated since his diagnosis, experiencing pain, difficulty swallowing, and significant weight loss. His son reflects on the impact of his father’s declining health, highlighting the financial strain imposed by medical expenses.
The family’s reliance on insurance and savings underscores the unpredictable nature of medical costs, prompting them to prioritize financial preparedness. Mr. Gupta’s illness not only affects him physically but also strains his relationships and limits his ability to work. Support from family and friends plays a crucial role in navigating these challenges, offering emotional sustenance amidst the turmoil. However, Mr. Gupta’s condition continues to pose obstacles, hindering his social activities and work responsibilities.
Despite the setbacks, Mr. Gupta finds solace in counseling sessions, which provide valuable emotional support and guidance. These sessions serve as a lifeline, helping the family cope with the uncertainties brought about by Mr. Gupta’s illness. Reflecting on his journey, his son emphasizes the importance of seeking support and maintaining a positive outlook in the face of adversity. He encourages others facing similar challenges to prioritize their health, seek medical guidance, and lean on their support networks for assistance. In essence, Mr. Gupta’s story illustrates the multifaceted impact of cancer on individuals and their families, underscoring the need for comprehensive support systems to navigate the complex transitions brought about by illness.
Case study 14: Navigating cancer’s challenges: Sindhu’s journey
Sindhu P, a 28-year-old scientist from Kancheepuram, Tamil Nadu, was diagnosed with left breast carcinoma in February 2022. Despite undergoing surgeries, chemotherapy, and radiation therapy, she remains out of remission, facing numerous hurdles along the way. Since her diagnosis, Sindhu’s health has deteriorated, experiencing pain, difficulty swallowing, and significant weight loss. Her father reflects on the impact of her declining health, highlighting the financial strain imposed by medical expenses.
The family’s reliance on insurance and savings underscores the unpredictability of medical costs, prompting them to prioritize financial preparedness. Sindhu’s illness not only affects her physically but also strains her relationships and limits her ability to work. Support from family and friends plays a crucial role in navigating these challenges, offering emotional sustenance amidst the turmoil. However, Sindhu continues to face obstacles, hindering her social activities and work responsibilities.
Despite the setbacks, Sindhu finds solace in counseling sessions, which provide valuable emotional support and guidance. These sessions serve as a lifeline, helping the family cope with the uncertainties brought about by Sindhu’s illness. Reflecting on her journey, one of relative emphasizes the importance of seeking support and maintaining a positive outlook in the face of adversity. He encourages others facing similar challenges to prioritize their health, seek medical guidance, and lean on their support networks for assistance. In essence, Sindhu’s story illustrates the multifaceted impact of cancer on individuals and their families, underscoring the need for comprehensive support systems to navigate the complex transitions brought about by illness.
Case study 15: Sudha’s cancer journey: Navigating challenges
Sudha S, a 57-year-old graduate from Velachery, Chennai, Tamil Nadu, faced a life-altering diagnosis of Left Breast Carcinoma in February 2022. Despite undergoing surgeries, chemotherapy, and radiation therapy, she remains out of remission, battling through pain, difficulty swallowing, and significant weight loss.
Financial strains imposed by medical expenses add to the family’s burden, despite relying on insurance and savings. The impact extends beyond the physical realm, affecting Sudha’s relationships and ability to work. However, the unwavering support of family and friends serves as a source of strength amidst adversity.
Anand, Sudha’s son, reflects on the challenges faced during her treatment, emphasizing the importance of seeking support and maintaining a positive outlook. Counseling sessions offer invaluable emotional support, aiding the family in coping with the uncertainties brought about by Sudha’s illness.
Despite setbacks, Sudha’s journey highlights moments of resilience and hope. As she continues her treatment, the support of healthcare professionals and loved ones enables her to navigate the challenges with greater fortitude. In conclusion, Sudha’s story underscores the multifaceted impact of cancer on individuals and their families, emphasizing the need for comprehensive support systems to navigate the complex transitions brought about by illness.
Case study 16: Mr. Kumar’s cancer journey: Navigating challenges
Mr. Kumar, a 48-year-old from Dhenkanal, Odisha, was diagnosed with Oral Cancer in September 2022. As his daughter Anjali recounts, the journey has been fraught with challenges, impacting every aspect of their lives. Financial constraints, compounded by Kumar’s inability to work as a salesperson since August 2022, have placed a significant strain on the family. Despite relying on insurance and savings, managing medical expenses remains an ongoing concern. The toll on Kumar’s health has been profound, with symptoms including difficulty swallowing, jaw pain, and fatigue. These physical struggles have been accompanied by emotional distress and fears about the future, exacerbated by the financial burden of treatment. Throughout this ordeal, the unwavering support of family and friends has been a beacon of hope. Their encouragement and assistance helped Mr. Kumar navigate the darkest moments of his illness. As Mr. Kumar continues his treatment journey, there are glimpses of progress amid the challenges. Each radiation therapy session brings temporary relief, but the road to recovery remains arduous. Anjali emphasizes the importance of seeking support and maintaining a positive mindset during such trying times. Access to counseling sessions has been invaluable, providing emotional guidance and practical assistance in managing the complexities of Kumar’s illness. In conclusion, Kumar’s story serves as a reminder of the resilience of the human spirit in the face of adversity. Through love, support, and a determination to persevere, he and his family are confronting the challenges of cancer with courage and hope.
Case study 17: Ms. Naren’s cancer journey
Ms. Naren, a 46-year-old from West Mumbai, Maharashtra, was diagnosed with Metastatic Breast Cancer in April 2022. As her husband Aalok recounts, the journey has been a rollercoaster of emotions and challenges that have deeply impacted their lives. Financial strains, coupled with Ms. Naren’s inability to work since April 2022, have added immense pressure to their family of two. Despite relying on insurance and savings, managing the escalating medical expenses remains a daunting task, highlighting the unpredictability of cancer treatment costs.
Ms. Naren’s health has deteriorated significantly since the diagnosis, with symptoms ranging from difficulty swallowing to fatigue and weight loss. These physical hardships, compounded by the emotional toll of the disease, have tested their resilience and strength as a couple. Throughout this trying time, the unwavering support of family and friends has been a source of comfort and strength.
As Ms. Naren continues her treatment journey, there are glimmers of hope amidst the challenges. Each session brings temporary relief, but the journey to remission is fraught with uncertainties and setbacks. Aman emphasizes the importance of seeking support and staying positive in the face of adversity. Access to counseling sessions has been invaluable, providing emotional guidance and practical assistance in managing the intricacies of Mr. Naren’s illness. In conclusion, Mr. Naren’s journey underscores the resilience of the human spirit in the face of adversity. Through love, support, and a determination to persevere, she and Aman are confronting the challenges of cancer with courage and hope.
Case study 18: Mr. Pal’s diagnosed with oligodendroglioma cancer journey
Mr. Pal, a 55-year-old from Guwahati, Assam, was diagnosed with Oligodendroglioma in January 2023. Since then, his family, led by his daughter, has grappled with the emotional and financial toll of his illness. Financial strain intensified when Mr. Pal had to stop working in January 2023. Despite relying on insurance and savings, managing medical expenses has been overwhelming, adding to their stress during an already challenging time.
Mr. Pal’s health has rapidly declined, with symptoms like difficulty swallowing and jaw pain worsening. Despite occasional relief, treatment side effects have left him unable to eat or speak normally, profoundly impacting his daily life. Navigating relationships has been complex, with some relatives offering unwavering support while others distanced themselves.
Friends have been a source of distraction and comfort during Mr. Pal’s treatment journey, providing much-needed emotional support. Despite the hardships, the family finds solace in the moments of relief brought by treatment, clinging to hope for better days ahead. Through love, resilience, and the support of their community, they navigate the uncertainties of cancer with strength and determination.
Case study 19: Navigating Choudhary cancer treatment challenges
Mr. Choudhary, a 59-year-old resident of Pune, Maharashtra, began a difficult journey after being diagnosed with Carcinoma of the left alveolus in January 2023. His diagnosis brought immense physical, emotional, and financial strain on his family, particularly his son who recounted their shared experience. Mr. Choudhary’s health declined rapidly—difficulty swallowing, significant weight loss, and constant weakness severely impacted his ability to perform daily tasks and maintain social connections.
Financially, the family relied on insurance and savings, but the unpredictable nature of treatment expenses created ongoing anxiety. Despite some support from friends and extended family, they often felt overwhelmed, struggling to balance care responsibilities with financial planning. Mr. Choudhary’s treatment, including surgery and therapy, was accompanied by persistent side effects that limited his mobility and speech, further affecting his work and daily routine.
Amid these challenges, counseling sessions provided a crucial source of emotional strength. These sessions helped Mr. Choudhary and his family process their fears, manage stress, and regain a sense of control in the midst of uncertainty. They learned the value of staying informed, seeking emotional support, and approaching the illness with resilience and a positive mindset.
Mr. Choudhary’s story highlights the dual burden of cancer—medical and financial—and the essential role of mental health support. His journey reflects the strength families must summon when faced with a serious illness. It underscores the importance of accessible emotional counseling, financial planning, and community awareness to support individuals through such taxing times. Through perseverance and family solidarity, Mr. Choudhary continues to face his illness with determination and hope.
Case study 20: Challenges and insights from Mr. Kapur’s cancer treatment journey
Mr. Kapur, a 65-year-old resident of Delhi, was diagnosed with oligometastatic prostate cancer in March 2023, setting off a deeply challenging journey for him and his family. His daughter-in-law shares their experience, highlighting the emotional and financial toll that came with his diagnosis. Despite a comfortable monthly household income of ₹4–5 lakhs and existing insurance coverage, the family struggled with the unpredictability of medical costs—particularly as Mr. Kapur’s declining health forced him to stop working.
His illness brought a gradual but steady decline in physical health, marked by fatigue, pain, and difficulty swallowing. These symptoms disrupted daily life and added emotional strain to the family. The financial burden grew with each passing month, as treatment costs, specialist consultations, and travel expenses added up. Even with insurance and savings, the uncertainty around the long-term nature of care posed significant stress, forcing the family to reevaluate their spending and future planning.
She emphasizes the crucial role of emotional support from close relatives and friends, which provided much-needed relief during their darkest moments. While the journey was riddled with fear, doubt, and concern for the future, the family drew strength from the empathy of healthcare professionals and the resilience they nurtured together.
Mr. Kapur’s case exemplifies the multilayered challenges of cancer care—where financial uncertainty, emotional distress, and health complications intertwine. His story is a testament to the strength families must summon to endure such trials and highlights the importance of early planning, emotional resilience, and strong social support in navigating the cancer journey with dignity and hope.
However, Table 1 is a much elaborative summary of 20 Indian cancer survivors. Table 2 highlights the insights gathered from Table 1 through a crisp cross-case comparison based on four important constructs, for example, age, gender, cancer type, social context, and socioeconomic role. Furthermore, a cross-thematic synthesis is recognized into three higher order categories, for example, Economic disruption, Relational care, and Stigma or secrecy with interpretive subthemes.
Cross-case comparative insights.

The ‘cross-case thematic synthesis’ is recognized into three higher order categories, for example, Economic disruption, Relational care, and Stigma or secrecy with interpretive subthemes. These are discussed below:
Economic disruption
Subthemes:
Financial burden and treatment: Seventeen out of 20 participants reported severe financial stress owing the high cost of treatment, insufficient insurance coverage, and loss of income diminishing self-worth (e.g., Cases 2, 7, 13, and 20).
Unemployment and role redefinition: Quitting jobs or role modifications can be seen in Cases 4, 6, and 18.
Socioeconomic inequality: It leads to both inequality in accessing healthcare and financial structure (Cases 13 and 14).
This work reveals that the economic disruption affects the structural “backbone,” of breadwinners’ socioeconomic identity as cancer not only imposes a stupendous burden of medical cost but also redefines such complex identity involving psychology as well. It adversely transforms self-perceived worth from a “provider to the family” to “dependent of the family.” The inadequacy or absence of formal financial protection measures amplifies vulnerability and thus shapes subsequent coping behaviors of the breadwinners in their journey with cancer.
Relational care and social support network
Subthemes:
Family as the core support system: Participants acknowledged emotional, financial, and logistic support from their families. It was noted that spouses and children provided both caregiving and moral strength, while relatives often managed treatment logistics (Cases 10, 15, 20).
Peer and professional support: Although less frequently mentioned, counselors and healthcare professionals offered meaningful reassurance, helping patients accept the illness and rebuild confidence (Cases 15, 16).
Reciprocity and emotional resilience: Support was not passive, and many participants expressed reciprocal care, finding motivation to endure treatment for the sake of their families (Cases 1, 7).
Relational care emerged as the psychosocial buffer countering the balancing the impact of cancer as a disease and its treatment, as evident from this study. Family and community engagement helped sustain emotional survival and anchored to the reconstruction of post-diagnosis identity. However, reliance on informal networks underscores the lack of structured survivorship care in the healthcare system.
Stigma-based social withdrawal and secrecy and its psychosocial impacts
Subthemes:
Concealment and fear of contagion: Many participants (Cases 1, 3, 7, 8, 10) concealed their diagnosis to avoid social stigma, such as being perceived as “contagious” or “unclean,” resulting into social withdrawal.
Gendered patterns of secrecy: Men, especially older breadwinners, were more likely to hide their condition due to masculine ideals of strength and self-reliance. Women, on the other hand, adopted a more relational approach, which was focused on protecting family reputation.
Desocialization and isolation: Limited mobility and treatment side effects (speech or eating difficulty) further reinforced physical and emotional isolation (Cases 8, 9, 10).
In this paper, stigma and secrecy demonstrate how cultural narratives of illness intersect with social identity. Concealment served as both a protective and restrictive strategy. It falsely shields patients from being judged at the cost of social connectedness. The persistence of contagion myths underscores a public health gap in cancer awareness, which is a concerning. Together, they (i) depict cancer survivorship as a cycle of disrupted normality, or sometimes as a neo-normal stage of life, (ii) relational negotiation, and (iii) social reconstruction within constrained structural contexts. Survivorship thus becomes not only a medical outcome but a process of social reorientation in the face of economic and cultural adversities.
From a cancer survivorship and life course journey perspective, the Caring Life-Course Theory (CLCT) provides a valuable framework to conceive how care practices, relationships, and self-care attitude evolve over time as a psychosocial mechanism of survivorship and life course in cancer patients. 15 CLCT offers care as a mixed dynamic process embedded within the broader life course, shaped by transitions such as diagnosis, treatment, recovery, and long-term survivorship in breadwinners diagnosed with cancer. It highlights the dynamics of survivors’ capacities to give as well as receive care, and the shift in response to changing health, social, and economic circumstances around them. In India, there are additional crucial parameters, for example, debt, job loss, work disruption, and social stigma qualifies the survivorship further.
Summarily, for cancer survivors, CLCT helps understand how care biographies, such as personal histories of being cared for and caring for others intersect with relational networks and psychosocial support systems as noticed in this study. This perspective underscores survivorship merely not as a static endpoint but a continuing process of adaptation, resilience, and renegotiation of care roles across different life phases. The work of Lawless et al. describes how the CLCT helps scan the roles of self-care trajectories in self-care behavior, which is unfolded over time in men with prostate cancer, which reinforces the role of CLCT in cancer survivorship journey. 16
Summary of findings and recommendations
The research revealed that the cancer journey involves distinct phases—diagnosis, treatment, survivorship, and end-of-life care, each with unique challenges. Psychosocial factors like social support, coping, and resilience play key roles in shaping patients’ health trajectories. Effective healthcare communication and patient-centered care are vital for facilitating smoother transitions across these phases. Table 3 showcases an age-group wise (in an ascending order) summary of sociodemographic and cancer types. In this table, “distribution” denotes the mean age with the corresponding sample standard deviations and its “contribution” in percentage in this sample. While cases 1–4, 7–9, and 20 belong to the middle class, no definitive financial information is available for cases 5, 6, 10–19 except for the financial strains due to high cost of diagnostics and treatment and an unknown future.
Summary of sociodemographic and clinical diversity in the sample—Age-wise and cancer types.

Group A is a socioeconomic and psychological jolt to their primary bread-earners in the family. It is also a major jolt to their savings to meet up the treatment cost, which is often exuberant. Group B seems to be the sole financial support for their entire family and hence the financial constraints are maximum. However, case of 13, son has been financially impacted to meet up father’s treatment costs. It is also worth noting that the propensity of cancer is maximally clustered in the age of 50s in this sample. Group C is not well-delineated in terms of age, socioeconomic status, and cancer type as the patient does not want to divulge above information to the interviewer. Although it adds knowledge to the survivorship study, it mostly poses itself as an outlier in the sample data. Stigma due to social constraints, such as belief of contagion is noted in all the cases as evident in Table 3. It is also important to note that the overall ratio of cancers in males and females is 7:13, that is, males suffer close to double the number of females. This is an important observation in Indian context as males are the primary breadwinners in the society.
This paper emphasizes that cultural and contextual insights on cancer survivorship that must move beyond acknowledging stigma and secrecy to offer a more systematic and holistic discussion of the gender norms, cultural narratives, and socioeconomic inequalities. It shapes how individuals disclose and cope with their illness. In the Indian sociocultural context, fears of contagion (due to lack of awareness and knowledge), moral judgment (e.g., effect of an evil or curse), and the threat of social exclusion (cancer apartheids). Some root causes are financial toxicity, rural-urban divide, disparities in diagnostics and treatment, uneven implementation of cancer prevention program, such as Human Papillomavirus (HPV) prevention through vaccination, and a widening research gap due to paucity of local research, clinical trial, and high-quality meaningful data collection. The outcome often is an overlap with entrenched gender expectations. The feminine ideology (case numbers 4, 6, 9, 12, 14–16) upholds being modest, dedicated to familial duty, and more family-centric actions.
On the other hand, masculine ideals of strength, stoicism, and financial responsibility are to influence experiences of survivorship in cases 1–3, 5, 7, 8, 10, 11, 13, and 17–20. In India, these constructs are further compounded by the regressive dynamism of economic class and caste-based disparities that determine the level of access to information and thus influence the grade of awareness, especially accessing and utilizing of various healthcare resources and supportive networks, for example, insurance provided by the government bodies. Situational findings such as fear of contagion or social pressure to maintain a façade of strength within these broader frameworks help illuminate how cancer survivorship is not merely a biomedical journey, but a deeply social and culturally mediated self-evolving process as evident in cases 1, 3, 7, 8, and 10.
Cultural and contextual insights on cancer survivorship can be linked to the literature on financial toxicity and stigma measurement in South Asian socioeconomic context. It strengthens both scholarly relevance and policy usefulness. Financial toxicity includes out-of-pocket costs, lost income, and insurance gaps. These interact with stigma and secrecy, shaping when and how patients disclose diagnosis, pursue care, or draw a red line on their social networks. Masculine norms that valorize breadwinning tend to conceal illness to avoid perceived economic and reputational loss. Integrating validated stigma-measurement tools adapted for South Asian settings and refining them to capture caste/class, gendered expectations, and family-level consequences evident a better reflection on living realities. This base created on a culturally informed evidence enables policies that go beyond clinical funding to include social protection through intending and implementing income support, job protections, reduction of stigma at the community level, caregiver-centered financial counseling, and health insurance rendered financial assistant to meet up the diagnostics and treatment costs, which are substantial in most of the cases. Designing interventions through this cultural lens ensures the insurance and its support system address relational and biographical care needs to help the survivors manage the sudden financial jolt as and when the cancer is first diagnosed. Putting together, assisting role changes, help preserve social and professional dignity, and maintain livelihoods might be the need of the hour rather than treating survivorship as solely a medical problem in a robust and holistic social support system.
As evident, liminality in cancer survivorship refers to the transitional and often ambiguous phase that individuals experience between illness and wellness, marking a threshold state within the broader life course journey. After diagnosis and treatment, almost all survivors, presented in this work, frequently inhabit an “in-between” space, which is overlap of no longer acutely ill but not fully restored to their pre-cancer identity or health, as noted in all the cases. This liminal phase has disrupted temporal and social continuity, challenging notions of normalcy, control, and self. Survivors may navigate shifting roles within families, workplaces, and communities, while grappling with lingering physical symptoms, emotional uncertainty, financial burden due to cost of long treatment, and existential reevaluation.
Viewed through a life course lens, their liminalities underscore how cancer reconfigures one’s biographical trajectory, creating pauses, detours, and reorientations that shape future aspirations and sense of agency. It also highlights the relational dimension of survivorship, especially how care networks, healthcare systems, and social expectations mediate one’s movement through liminal spaces toward renewed meanings of health, identity, and belonging. Thus, liminality serves as a powerful conceptual bridge linking the embodied, temporal, and relational dimensions of living with and beyond cancer. This research also offers valuable insights for developing targeted interventions and support systems tailored to cancer patients’ needs at different stages. Healthcare providers can customize care plans, while policymakers and institutions can use the findings to improve care quality. The study highlights the importance of a holistic approach that addresses the psychosocial aspects of the cancer experience. Overall, this research makes a significant contribution to oncology by using a life course perspective to qualitatively explore cancer patients’ health transitions and trajectories. It provides valuable insights that can improve cancer care practices and enhance the well-being of patients and their families.
A key achievement of this project is recognizing the cancer journey as a complex, non-linear process with distinct phases—diagnosis, treatment, survivorship, and end-of-life care. Understanding these stages is vital for tailoring care to patients’ specific needs at each point. The research highlights psychosocial factors—social support, coping strategies, and patient resilience—as key influences on cancer trajectories. This underscores the need for healthcare providers to adopt a holistic, patient-centered approach addressing both medical and psychosocial aspects of care.
This project emphasizes the interplay of medical, psychosocial, and temporal factors in shaping cancer patients’ experiences. Its findings offer a foundation for developing more effective, compassionate cancer care that improves patients’ lives.
The project holds theoretical and practical significance by deepening understanding of psychosocial and life course perspectives in cancer care, extending existing theories on the complex factors shaping patients’ healthcare experiences.
Practically, this project provides the Apollo Proton Cancer Center and similar organizations with deeper insights into cancer patients’ challenges, enabling more patient-centered, comprehensive care. It informs improved communication, support systems, and tailored interventions, enhancing care quality and patient well-being. Researchers and clinicians are encouraged to adopt a multifaceted, holistic approach to develop more effective, patient-focused care.
The limitations of the study lie on its attempt to maintain homogeneity of the data by recruiting only breadwinners whose ages are 28 years or above. It disallows the perspectives lying with the excluded group of survivors. Elderly dependents are also excluded. It limits the study to capture the longitudinal perspective of life course journey in a holistic manner.
Cancer care should start with immediate emotional support and counseling. Financial burdens must be eased through assistance programs and insurance coverage. Financial burden plays a crucial role in cancer cases by raising the apprehension about the future, affecting the survivorship strategy largely where a holistic and non-judgmental insurance policy can play an important role. For example, there are clauses within the insurance terms and conditions that not only reduce the settlement amount but also decline the claim.17,18
The paper takes the opportunity to recommends a reform in the insurance segment through a two-pronged holistic approach—(a) CLCT-informed strategies such as “know your client” based on their profile, social network, and self-care assessments to mine actionable points including the “pre-existing condition” clause, and following this roadmap (b) a much-personalized care can be provided by the social workers and nurses by improving interpersonal communication, help patients accessing the designated specialist hospitals, monitor treatment cycles, generate awareness among the caregivers and the social network of the patients regarding stigma and belief of contagion, and (c) taking care of the costs involved for diagnostics and treatment empathetically through insurances and public healthcare system. Thus, this paper proposes a unified though multipronged approach to adhere to the best practices of cancer survivorship as suggested by Kitson et al. 19 Strengthening social support through family, peers, and patient communities is a vital step to reduce isolation or being felt isolated in the survivorship journey. Continuous emotional care and compassionate communication are essential for informed decisions. Support for managing diagnosis disclosure and tailored self-management tools should empower patients at every stage of his/her cancer survivorship journey from the life course perspective involving its several trajectories.
Supplemental Material
sj-docx-1-pcr-10.1177_26323524251412831 – Supplemental material for From diagnosis to survivorship: Exploring health trajectories of cancer patients in India through a life course perspective
Supplemental material, sj-docx-1-pcr-10.1177_26323524251412831 for From diagnosis to survivorship: Exploring health trajectories of cancer patients in India through a life course perspective by Sanghamitra Sahu, Gyan Chandra Kashyap, Chandini Divakar and Subhagata Chattopadhyay in Palliative Care and Social Practice
Footnotes
Acknowledgements
The authors would like to acknowledge the medical superintendent and assistant manager of the Apollo Proton Cancer Centre (APCC) for the support provided during the survey. The authors would like to acknowledge all individuals who participated in the survey.
Ethical considerations
Ethical approval has been obtained from the Medical Superintendent and Quality Office-Assistant Manager of Apollo Proton Cancer Centre (APCC).
Consent to participate
Informed consent was obtained from all individual participants involved in the study.
Consent for publication
Informed content was obtained from all individual participants to use the information in anonymized form in academic and scientific publications, reports, or presentations related to this research study.
Author contributions
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
This study is based on primary data collected by the first author. The qualitative information will be made available to the journal upon request, if required.
Supplemental material
Supplemental material for this article is available online:
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
